Can Ultrasound Reduce the Rate of Negative Testicular Exploration in Suspicious Acute Scrotum; A 5-Year Experience in A District Hospital
Article Information
Ahmed Gendia1*, S. Tariq Cheema2, Yousaf Tanveer3
1General surgery registrar, Cavan General Hospital, Cavan, Ireland
2General surgery consultant, Cavan General Hospital, Cavan, Ireland
3General surgery senior house officer, Cavan General Hospital, Cavan, Ireland
*Corresponding Author: Dr. Ahmed Gendia, General surgery registrar, Cavan General Hospital, Cavan, Ireland
Received: 07 August 2020; Accepted: 31 August 2020; Published: 01 October 2020
Citation: Ahmed Gendia, S. Tariq Cheema, Yousaf Tanveer. Can Ultrasound Reduce the Rate of Negative Testicular Exploration in Suspicious Acute Scrotum; A 5-Year Experience in A District Hospital. Archives of Nephrology and Urology 3 (2020): 097-103.
View / Download Pdf Share at FacebookAbstract
Objective: To retrospectively outline findings of testicular exploration in patients with suspicious acute scrotum and to compare the outcomes between exploration with and without US as a preoperative diagnostic tool.
Methods: A retrospective analysis of patients underwent scrotal exploration from Jan2014 till Dec 2018 in our hospital was conducted. The data were divided into exploration with preoperative ultrasound (US group) and exploration without preoperative US (non-US group).
Results: 47 patients (mean age 14-years) were explored during the 5-year period. The most common finding was torsion Cyst of Morgagni (34%, 16/47). True torsion was found in 27.6% (13/47) with 3 unsalvageable testes. Torsion rates were higher in patients who underwent US (7/14, 50%) than exploration without US (6/33, 18.1%). Time delay between two groups showed no statistical difference (p-value >.05). Also, US showed 70% sensitivity and 100% Specificity regarding torsion testis.
Conclusion: Based on our numbers, negative exploration can be reduced with the help of US as a diagnostic tool for torsion. However, until further studies with larger populations and definitive pathway regarding ultrasound are commenced, we recommend urgent exploration as the standard intervention in dealing with suspicious acute scrotum.
Keywords
Torsion testis; Testicular torsion; Testicular exploration; Ultrasound; Doppler
Torsion testis articles, Testicular torsion articles, Testicular exploration articles, Ultrasound; Doppler articles
Torsion testis articles Torsion testis Research articles Torsion testis review articles Torsion testis PubMed articles Torsion testis PubMed Central articles Torsion testis 2023 articles Torsion testis 2024 articles Torsion testis Scopus articles Torsion testis impact factor journals Torsion testis Scopus journals Torsion testis PubMed journals Torsion testis medical journals Torsion testis free journals Torsion testis best journals Torsion testis top journals Torsion testis free medical journals Torsion testis famous journals Torsion testis Google Scholar indexed journals Testicular torsion articles Testicular torsion Research articles Testicular torsion review articles Testicular torsion PubMed articles Testicular torsion PubMed Central articles Testicular torsion 2023 articles Testicular torsion 2024 articles Testicular torsion Scopus articles Testicular torsion impact factor journals Testicular torsion Scopus journals Testicular torsion PubMed journals Testicular torsion medical journals Testicular torsion free journals Testicular torsion best journals Testicular torsion top journals Testicular torsion free medical journals Testicular torsion famous journals Testicular torsion Google Scholar indexed journals Testicular exploration articles Testicular exploration Research articles Testicular exploration review articles Testicular exploration PubMed articles Testicular exploration PubMed Central articles Testicular exploration 2023 articles Testicular exploration 2024 articles Testicular exploration Scopus articles Testicular exploration impact factor journals Testicular exploration Scopus journals Testicular exploration PubMed journals Testicular exploration medical journals Testicular exploration free journals Testicular exploration best journals Testicular exploration top journals Testicular exploration free medical journals Testicular exploration famous journals Testicular exploration Google Scholar indexed journals Ultrasound articles Ultrasound Research articles Ultrasound review articles Ultrasound PubMed articles Ultrasound PubMed Central articles Ultrasound 2023 articles Ultrasound 2024 articles Ultrasound Scopus articles Ultrasound impact factor journals Ultrasound Scopus journals Ultrasound PubMed journals Ultrasound medical journals Ultrasound free journals Ultrasound best journals Ultrasound top journals Ultrasound free medical journals Ultrasound famous journals Ultrasound Google Scholar indexed journals Doppler articles Doppler Research articles Doppler review articles Doppler PubMed articles Doppler PubMed Central articles Doppler 2023 articles Doppler 2024 articles Doppler Scopus articles Doppler impact factor journals Doppler Scopus journals Doppler PubMed journals Doppler medical journals Doppler free journals Doppler best journals Doppler top journals Doppler free medical journals Doppler famous journals Doppler Google Scholar indexed journals �colour Doppler sonography articles �colour Doppler sonography Research articles �colour Doppler sonography review articles �colour Doppler sonography PubMed articles �colour Doppler sonography PubMed Central articles �colour Doppler sonography 2023 articles �colour Doppler sonography 2024 articles �colour Doppler sonography Scopus articles �colour Doppler sonography impact factor journals �colour Doppler sonography Scopus journals �colour Doppler sonography PubMed journals �colour Doppler sonography medical journals �colour Doppler sonography free journals �colour Doppler sonography best journals �colour Doppler sonography top journals �colour Doppler sonography free medical journals �colour Doppler sonography famous journals �colour Doppler sonography Google Scholar indexed journals acute scrotum articles acute scrotum Research articles acute scrotum review articles acute scrotum PubMed articles acute scrotum PubMed Central articles acute scrotum 2023 articles acute scrotum 2024 articles acute scrotum Scopus articles acute scrotum impact factor journals acute scrotum Scopus journals acute scrotum PubMed journals acute scrotum medical journals acute scrotum free journals acute scrotum best journals acute scrotum top journals acute scrotum free medical journals acute scrotum famous journals acute scrotum Google Scholar indexed journals Ultrasound articles Ultrasound Research articles Ultrasound review articles Ultrasound PubMed articles Ultrasound PubMed Central articles Ultrasound 2023 articles Ultrasound 2024 articles Ultrasound Scopus articles Ultrasound impact factor journals Ultrasound Scopus journals Ultrasound PubMed journals Ultrasound medical journals Ultrasound free journals Ultrasound best journals Ultrasound top journals Ultrasound free medical journals Ultrasound famous journals Ultrasound Google Scholar indexed journalsArticle Details
1. Introduction
Testicular torsion is a relatively common cause of acute scrotal pain which accounts for approximately up to 15% of acute scrotal disease in children [1] and up to 25% in early adolescents [2]. It remains a difficult differential which require proper management, as delay in intervention can comprise organ preservation and cosmetic outcome [3]. More dramatically, it can lead to impairment in hormonal and fertility functions [4, 5], with nearly 80% and 100% infarction of torted testes after 10 h and 24 h since the onset of pain respectively [3]. Urgent Testicular exploration remains the definitive management of scrotal pain with suspicion of torsion, as the primary objective of surgery is to avoid testicular loss [6]. However, it’s debatable that with the advances in Doppler US studies, unnecessary interventions can be avoided [8]. The purpose of this study is to report the outcomes of scrotal exploration in a district hospital setting, and to outline our experience in utilization of Ultrasound imaging as a pre-operative investigation.
2. Methods and Materials
Cavan General hospital is a regional hospital in county Cavan, Ireland. No urology service is available in the hospital. However, Acute scrotal pain is managed by on-call general surgeons. Testicular Ultrasound is utilized only in working hours (9 am till 5 pm). All acute scrotal pain presented before 5 pm were urgently imaged utilizing a special pathway to avoid any delay. But after 5 pm, the decision of acute scrotal management is only dependent on clinical findings. All patients underwent scrotal exploration for acute scrotum from January 2014 to December 2018 were included in this study. The hospital database and the operative theatre log books were screened for included data. Patient with abscess, trauma, elective settings and non-acute causes were excluded. Patients records were retrospectively reviewed and audited by AG and YT. Data collected included; Age, presenting time, time to US and intervention, weather preoperative ultrasound was performed or not and intraoperative findings. The data were analysed and categorized into 2 groups, Us group and Non-US group. Follow up wasn’t included in this study.
Due to the limitation of sample size in both groups, Z test couldn’t be applied regarding the positive and negative exploration results. However, comparison between the time needed to operate between US and Non-US group was done by T test using hypothesis testing with significance level 0.05(α).
3. Results
In the 5-year period, 47 patients underwent urgent scrotal exploration for acute scrotal pain, mean age was 14 years (5-35 years) with 43% of patients in the age group (11-15 years) (Figure 1). The most common finding was torsion cyst of Morgagni (16/47, 34%) and testicular torsion (13/47, 27.6%). Three patients of the 13 with torsion required orchidectomy for gangrenous testes. Normal findings and epididymitis/orchitis presented 17% (8/47) and 11% (5/47) respectively, 3 cases of epidydimal cyst and 2 cases were small hydrocele (Table 1).
The 47 cases were further categorised to Non-US group (33/47) and US group (14/47) (Figure 2) according to preoperative application of ultrasound doppler; In Non-Us group (33), mean time between primary assessment and exploration was 4 hours, the most common finding was torted cyst of Morgagni (15/33, 45.5%). Six patients (18%) in this group had a finding of torsion testes; 5 viable torsion and 1 gangrenous. Unremarkable finding was found in 6 cases (18%) while 4 had epididymitis/orchitis, one epididymal cyst and one hydrocele.
On the other hand, the most common finding in the US group was testicular torsion (7/14, 50%), 2 of them were unviable and required orchidotomy. US conformed the torsion in all 7 cases. 3 cases underwent exploration with suspicious blood flow in colour doppler, but the results were negative (2 normal and 1 hydrocele). Another 4 negative explorations, with Ultrasound proved normal vascularity and other finding, showed 2 epididymal cysts, 1 epididymitis, and 1 torted Morgagni. Average time needed to operate on this groups was 5 hours from presenting to the emergency department.
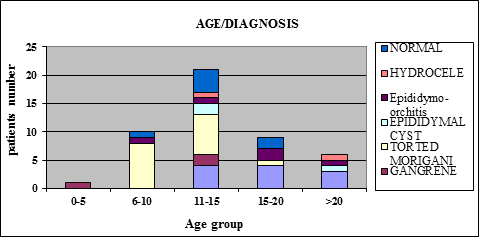
Figure 1: Showing age group and diagnosis.
|
Finding |
US group (n=14) |
Non-US group (n=33) |
Total |
||||
|
n |
% |
n |
% |
n |
% |
||
|
Positive Result |
Torsion |
5 |
35.7% |
5 |
15.1% |
10 |
21.2% |
|
Gangrene |
2 |
14.3% |
1 |
3% |
3 |
6.4% |
|
|
+ve Total |
7 |
50% |
6 |
18.1% |
13 |
27.6% |
|
|
Negative Results |
Torted morgagni |
1 |
7% |
15 |
45.5% |
16 |
34% |
|
Normal |
2 |
14.3% |
6 |
18.2% |
8 |
17% |
|
|
Epididymitis/orchritis |
1 |
7% |
4 |
12.1% |
5 |
10.6% |
|
|
Epididymal Cyst |
2 |
14.3% |
1 |
3% |
3 |
6.4% |
|
|
Hydrocele |
1 |
7% |
1 |
3% |
2 |
4.2 |
|
|
-ve Total |
7 |
50% |
28 |
81.8% |
37 |
78.7% |
|
|
Total |
14 |
33 |
47 |
||||
Table 1: Overall, Non-US and US group outcomes.
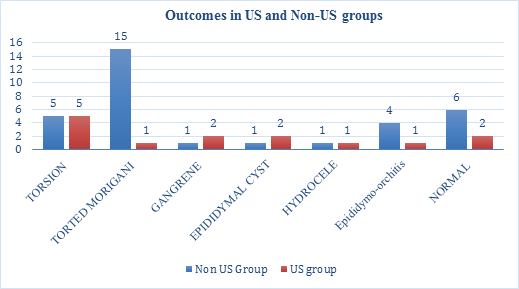
Figure 2: Outcomes in US and Non-Us groups.
4. Discussion
Testicular torsion results from twisting of spermatic cord and its content which leads to inadequate blood supply to testis, annual incidence of this surgical problem is 3.8 per in 100,000 males younger than 18 [9]. It has a bimodal peak, in neonates and around puberty [1]. Torsion pain is usually acute and severe and may lead to vomiting; and rarely presents with acute abdomen rather than scrotal pain [10]. The duration of the torsion can influence the clinical features, and may include swelling and induration of the surrounding skin. The testis is usually tender and may be high riding, the cord can be thickened and twisted or anteriorly located epididymis [6]. Also, cremasteric reflex is usually absent is patients with torsion which can help in distinguish it from other causes of acute scrotal pain [11].
The first line of imaging to testicular vascularity is colour Doppler sonography (CDS) [8, 12]. It can outline size, shape, echogenicity and perfusion of both testes. Also, it helps to evaluates the relative absence or decrease of blood flow in the affected testis in compared with the healthy one [12]. However, the time needed to perform imaging can increase testicular ischemia and thereby decrease testicular savage [13]. Additionally, Radionuclide studies can be used to evaluate acute scrotum, it can differentiate epididymitis “hot spots” from torsion testis “cold spots” [14]. However, availability, time, and radiation made Ultrasound the investigation of choice.
Urgent surgical intervention is recommended for acute pain with suspicion of torsion without the delay of ultrasound [6, 15, 16]. The critical time to needed to salvage the organ was reported at about 4-6 hours for 360 degree torsion [17]. The affected testis should be untwisted, warmed and fixed, contralateral orchiopexy should be performed regardless of the viability of the affected testicle due to increase the risk of contralateral torsion especially with bell clapper testis [18]. Orchiectomy is performed if the testis is unsalvageable [6, 18].
The acute scrotum in our hospital has two different pathways due to the limitation of availability of imaging. If the patient presented within working hours (9 am to 5 pm) testicular Us would be performed. Moreover, if presentation time is after 5 pm history and clinical examination would be the main indicator for exploration. In our study, torsion of testicular appendage was the most common overall cause of acute scrotum leading to exploration with 16 (34%) out of 47 patients. It was also reported to be the most common cause for scrotal pain in paediatrics with 50-70% of cases[19, 20]. In Addition, our study showed a significant difference between the 2 groups regarding the true torsion numbers. True torsions in the patient who underwent ultrasound and exploration was 50% and only 18 % in patients who underwent exploration without US. Also, numbers from our study showed that US had Sensitivity 70% Specificity 100% which is nearly similar to reported ones [7].
A recent meta-analyses on 2116 patient , which outlined the role of ultrasound in investigating testicular torsion in adult patients , showed that ultrasound can be an effective investigation testicular torsion and acute scrotal pain in adults with Overall diagnostic sensitivity was 0.86 [95% confidence interval (CI) 0.79–0.91] and specificity was 0.95 (95% CI: 0.92–0.97) [7]. However, none of the study included were randomized [7]. The meta-analysis results were significantly higher than those reported paediatric patients due to the presumption that adult patients are more cooperative during the exam. Ultrasound has been reported to fail to identify intratesticular flow in approximately half of paediatric patients [21]. False-negative US results can also occur during incomplete torsion and spontaneous detorsion. In these situations, repeating of ultrasound should be considered. However, a time delay could jeopardise organ savage [22].
Timing of exploration plays a critical role in testicular salvage, in our series, the exact time of pain onset wasn’t recorded. However, average time between presenting to our hospital and exploration in both groups showed no significant difference (p>.05) with 4 hours in Non-US group and 5 hours US group. Additionally, only 3 patients had unviable testes out of 10 torsions, those 3 presented late to hospital, and it was mostly related to the children embarrassment to express their complains to their parents.
In a study of 209 scrotal explorations, the overall rate of testicular salvage was 75%. This rate dramatically decreases to 25% after 16 hours of torsion [23]. Another study outlined the significant impact of duration of presenting testicular pain and organ savage; It showed that Delay in exploration of beyond 12 h from onset of pain resulted in preserving only (33%) 5 out 15 patients with torsion [3].
Another limitation of our study is follow up, In our practice follow up is usually done by family doctor, however none of our patient reported postoperative complication which needed review or admission by our surgical team. In literature, the clear outcome of long-term effect of testicular torsion is not reported on adequate population. A study on 23 patients with detorsion and fixation reported no pain or discomfort during follow up. Also, analysis of 6 sperm samples of those patients showed; one normal, 3 pathological and 2 doubtful [24]. Another study 53 cases with torsion showed a significant association of loss of testicular tissue with increase of preoperative time. Also, sex hormones were significantly higher with a longer time of torsion [25]. On the other hand, study on 63 cases, with follow up period ranged from 6 months to 4 years, reported no significant difference in semen quality or hormones levels when compared with the normal individual of same age [26].
Mandatory scrotal exploration remains the recommended pathway for acute scrotum without the delay needed for US study. However, this pathway leads to a large number of negative results. Hence, increase morbidity and operative risks, expenses and loads on hospitals [27]. Negative exploration was reported in wo retrospective studies on 119 and 73 patients who underwent exploration for acute scrotum, showed 65% and 70% negative results respectively and authors in both studies recommended urgent exploration when dealing with suspicious acute scrotum [28, 29]. In our study overall negative exploration was 72% and 50% in patients underwent ultrasound preoperatively. These negative results showed that the dilemma of whether we should continue on immediate surgical intervention for acute scrotum with the suspicion of torsion, or should we rely on US for definite diagnosis. More studies are required to outline the role of ultrasound as a definite diagnostic tool in the management of acute suspicious scrotal pain.
5. Conclusion
Acute scrotum is an urgent surgical emergency that requires proper management. Also, scrotal exploration remains the recommended intervention to avoid testicular loss. However, with the advances of US doppler scan, unnecessary exploration can be avoided. More studies should be conducted to test the role of ultrasound in future planning of surgery. Also follow up studies are advised so we can have a better understanding of the outcome of torsion on fertility.
Statement of Ethics
Ethical approval was exempted by the national ethical committee as it was approved by local ethical committee for auditing by Cavan hospital. Waiver of consents was applied in this study as the nature of the retrospective study.
Disclosure
There were No Conflicts of interests between authors.
Funding
No Funding was received for this article.
Author Contributions
Ahmed Gendia; main data collection and analysis, writing of the manuscript; S. Tariq Cheema; Supervision of the research; Yousaf Tanveer; co-data collection and analysis.
References
- Sharp VJ, Kieran K, Arlen AM. Testicular Torsion: Diagnosis, Evaluation, and Management. Am Fam Physician 88 (2013): 835-840.
- Gunther P, Rubben I. The acute scrotum in childhood and adolescence. Dtsch Arztebl Int 109 (2012): 449-457.
- Patrlck J. Dunne, Testlcular Torslon: Tlme Is The Enemy. Aust. N.Z. J. Surg 70 (2000): 441-442.
- Puri P, Barton D, O'Donnell B. Prepubertal testicular torsion: Subsequent fertility 20 (1986): 598-601.
- Romeo C, et al. Late hormonal function after testicular torsion. Journal of Pediatric Surgery 45 (2010): 411-413.
- Network N.E.M.C. Commissioning guide: management of paediatric torsion London: Royal College of Surgeons of England (2016).
- Ota K, et al. The role of ultrasound imaging in adult patients with testicular torsion: a systematic review and meta-analysis. J Med Ultrason (2001): 2019.
- Remer EM, et al. ACR Appropriateness Criteria (R) acute onset of scrotal pain--without trauma, without antecedent mass. Ultrasound Q 28 (2012): 47-51.
- Zhao LC, et al. Pediatric testicular torsion epidemiology using a national database: incidence, risk of orchiectomy and possible measures toward improving the quality of care. J Urol 186 (2011): 2009-2013.
- Wang F, Mo Z. Clinical evaluation of testicular torsion presenting with acute abdominal pain in young males. Asian Journal of Urology (2018).
- Rabinowitz R. The importance of the cremasteric reflex in acute scrotal swelling in children. J Urol 132 (1984): 89-90.
- Baker LA, et al. An analysis of clinical outcomes using color doppler testicular ultrasound for testicular torsion. Pediatrics 105 (2000): 604-607.
- Nguyen L, et al. Effect of unilateral testicular torsion on blood flow and histology of contralateral testes. J Pediatr Surg 34 (1999): 680-683.
- Amini B, et al. Diagnostic nuclear medicine in the ED. Am J Emerg Med 29 (2011): 91-101.
- Yang C, et al. Acute scrotum in children: an 18-year retrospective study. Pediatr Emerg Care 27 (2011): 270-274.
- Murphy FL, Fletcher L, Pease P. Early scrotal exploration in all cases is the investigation and intervention of choice in the acute paediatric scrotum. Pediatr Surg Int 22 (2006): 413-416.
- Sessions AE, et al. Testicular torsion: direction, degree, duration and disinformation. J Urol 169 (2003): 663-665.
- Bolln C, Driver CP, Youngson GG. Operative management of testicular torsion: current practice within the UK and Ireland. J Pediatr Urol 2 (2006): 190-193.
- Baldisserotto M, et al. Color Doppler Sonography of Normal and Torsed Testicular Appendages in Children. American Journal of Roentgenology 184 (2005): 1287-1292.
- Kass EJ, et al. Do all children with an acute scrotum require exploration? J Urol 150 (1993): 667-669.
- Dudea SM, et al. Doppler applications in testicular and scrotal disease. Med Ultrason 12 (2010): 43-51.
- Sung EK, Setty BN, Castro-Aragon I. Sonography of the Pediatric Scrotum: Emphasis on the Ts—Torsion, Trauma, and Tumors. American Journal of Roentgenology 198 (2012): 996-1003.
- Lewis AG, et al. Evaluation of acute scrotum in the emergency department. J Pediatr Surg 30 (1995): 277-281.
- Krarup T. The Testes After Torsion 50 (1978): 43-46.
- Brasso K, et al. Testicular torsion: a follow-up study. Scand J Urol Nephrol 27 (1993): 1-6.
- Pan F, et al. Emergency treatment of testicular torsion and postoperative follow-up: a 71 case report. J Huazhong Univ Sci Technolog Med Sci 32 (2012): 704-706.
- Agrawal AM, et al. Role of ultrasound with color Doppler in acute scrotum management. Journal of family medicine and primary care 3 (2014): 409-412.
- Tajchner L, et al. Management of the acute scrotum in a district general hospital: 10-year experience. TheScientificWorldJournal 9 (2009): 281-286.
- Naumann D, et al. Heterogeneity in practice during negative scrotal exploration for clinically-suspected testicular torsion 19 (2015).


 Impact Factor: * 2.3
Impact Factor: * 2.3 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 