Negative Pressure Wound Therapy in Surgical Wounds - A Single Centre Experience
Article Information
Mohammad Imtiaz1*, Chijioke Ikechi2, A K Shrestha3, Ankur Shah4
1Consultant emergency and colorectal surgery EKHUFT, Department of General Surgery, William Harvey Hospital Ashford, East Kent Hospitals University NHS Trust, UK
2Registrar General Surgery, EKHUFT NHS, Department of General Surgery, William Harvey Hospital Ashford, East Kent Hospitals University NHS Trust, UK
3Consultant emergency and colorectal surgery EKHUFT, Department of General Surgery, William Harvey Hospital Ashford, East Kent Hospitals University NHS Trust, UK
4Consultant emergency and hepatobiliary surgery EKHUFT, Department of General Surgery, William Harvey Hospital Ashford, East Kent Hospitals University NHS Trust, UK
*Corresponding Author: Mohammad Imtiaz, Consultant emergency and colorectal surgery EKHUFT, Department of General Surgery, William Harvey Hospital Ashford, East Kent Hospitals University NHS Trust, UK
Received: 02 September 2020; Accepted: 14 September 2020; Published: 16 September 2020
Citation: Mohammad Imtiaz, Chijioke Ikechi, A K Shrestha, Ankur Shah. Negative Pressure Wound Therapy in Surgical Wounds - A Single Centre Experience. Journal of Surgery and Research 3 (2020): 329-338.
View / Download Pdf Share at FacebookAbstract
Background: Negative pressure wound therapy (NPWT) is a therapeutic technique using suction pump to promote healing of wound. It can be used in a variety of surgical wounds. The aim of the study was to evaluate the outcome of NPWT in different types surgical wounds in a district general hospital (DGH)with a view to identify the complete healing rate of surgical wound and complication rate of using this technique.
Method: A retrospective review on prospectively-collected data of 102 patients was conducted from January 2018 to September 2019. Demographic data, diagnosis, comorbidities, indications for the application of NPWT, duration of therapy were recorded. Outcome included rate of complete healing and complications. The exclusion criteria were patients from other non-general surgical specialties and patients with bed sores.
Result: 102 patients (M: F 40:62) with a median age of 61 (30-96) years were included in the study. Median Body Mass Index (BMI) of patients was 27(19.2-44). 26.4%, 63% and 11.8% had a BMI less than 25, between 25-35 and above 35 respectively. The NPWT application was mostly (71.5% n= 73) used for anterior abdominal. Wound dimensions revealed a median length of 8 cm (range 3-20) and median width of 5cm (range 1-31). 98(96.1%) patients had complete healing and four patients (3.9%) had recorded complications.
Conclusion: From our experience, the use of NPWT achieved excellent complete healing rate with a very low complication rate. We can conclude that NPWT is a very useful, safe and effective technique to manage surgical wounds.
Keywords
Negative pressure wound therapy; Skin and soft tissue Infection( SSI)
Negative pressure wound therapy articles, Skin and soft tissue Infection( SSI) articles
Negative pressure wound therapy articles Negative pressure wound therapy Research articles Negative pressure wound therapy review articles Negative pressure wound therapy PubMed articles Negative pressure wound therapy PubMed Central articles Negative pressure wound therapy 2023 articles Negative pressure wound therapy 2024 articles Negative pressure wound therapy Scopus articles Negative pressure wound therapy impact factor journals Negative pressure wound therapy Scopus journals Negative pressure wound therapy PubMed journals Negative pressure wound therapy medical journals Negative pressure wound therapy free journals Negative pressure wound therapy best journals Negative pressure wound therapy top journals Negative pressure wound therapy free medical journals Negative pressure wound therapy famous journals Negative pressure wound therapy Google Scholar indexed journals Skin and soft tissue Infection articles Skin and soft tissue Infection Research articles Skin and soft tissue Infection review articles Skin and soft tissue Infection PubMed articles Skin and soft tissue Infection PubMed Central articles Skin and soft tissue Infection 2023 articles Skin and soft tissue Infection 2024 articles Skin and soft tissue Infection Scopus articles Skin and soft tissue Infection impact factor journals Skin and soft tissue Infection Scopus journals Skin and soft tissue Infection PubMed journals Skin and soft tissue Infection medical journals Skin and soft tissue Infection free journals Skin and soft tissue Infection best journals Skin and soft tissue Infection top journals Skin and soft tissue Infection free medical journals Skin and soft tissue Infection famous journals Skin and soft tissue Infection Google Scholar indexed journals wound dehiscence articles wound dehiscence Research articles wound dehiscence review articles wound dehiscence PubMed articles wound dehiscence PubMed Central articles wound dehiscence 2023 articles wound dehiscence 2024 articles wound dehiscence Scopus articles wound dehiscence impact factor journals wound dehiscence Scopus journals wound dehiscence PubMed journals wound dehiscence medical journals wound dehiscence free journals wound dehiscence best journals wound dehiscence top journals wound dehiscence free medical journals wound dehiscence famous journals wound dehiscence Google Scholar indexed journals skin grafts articles skin grafts Research articles skin grafts review articles skin grafts PubMed articles skin grafts PubMed Central articles skin grafts 2023 articles skin grafts 2024 articles skin grafts Scopus articles skin grafts impact factor journals skin grafts Scopus journals skin grafts PubMed journals skin grafts medical journals skin grafts free journals skin grafts best journals skin grafts top journals skin grafts free medical journals skin grafts famous journals skin grafts Google Scholar indexed journals crohn’s disease articles crohn’s disease Research articles crohn’s disease review articles crohn’s disease PubMed articles crohn’s disease PubMed Central articles crohn’s disease 2023 articles crohn’s disease 2024 articles crohn’s disease Scopus articles crohn’s disease impact factor journals crohn’s disease Scopus journals crohn’s disease PubMed journals crohn’s disease medical journals crohn’s disease free journals crohn’s disease best journals crohn’s disease top journals crohn’s disease free medical journals crohn’s disease famous journals crohn’s disease Google Scholar indexed journals diabetes-associated chronic leg wounds articles diabetes-associated chronic leg wounds Research articles diabetes-associated chronic leg wounds review articles diabetes-associated chronic leg wounds PubMed articles diabetes-associated chronic leg wounds PubMed Central articles diabetes-associated chronic leg wounds 2023 articles diabetes-associated chronic leg wounds 2024 articles diabetes-associated chronic leg wounds Scopus articles diabetes-associated chronic leg wounds impact factor journals diabetes-associated chronic leg wounds Scopus journals diabetes-associated chronic leg wounds PubMed journals diabetes-associated chronic leg wounds medical journals diabetes-associated chronic leg wounds free journals diabetes-associated chronic leg wounds best journals diabetes-associated chronic leg wounds top journals diabetes-associated chronic leg wounds free medical journals diabetes-associated chronic leg wounds famous journals diabetes-associated chronic leg wounds Google Scholar indexed journals Microdeformation articles Microdeformation Research articles Microdeformation review articles Microdeformation PubMed articles Microdeformation PubMed Central articles Microdeformation 2023 articles Microdeformation 2024 articles Microdeformation Scopus articles Microdeformation impact factor journals Microdeformation Scopus journals Microdeformation PubMed journals Microdeformation medical journals Microdeformation free journals Microdeformation best journals Microdeformation top journals Microdeformation free medical journals Microdeformation famous journals Microdeformation Google Scholar indexed journals healing wound articles healing wound Research articles healing wound review articles healing wound PubMed articles healing wound PubMed Central articles healing wound 2023 articles healing wound 2024 articles healing wound Scopus articles healing wound impact factor journals healing wound Scopus journals healing wound PubMed journals healing wound medical journals healing wound free journals healing wound best journals healing wound top journals healing wound free medical journals healing wound famous journals healing wound Google Scholar indexed journals intestinal fistula articles intestinal fistula Research articles intestinal fistula review articles intestinal fistula PubMed articles intestinal fistula PubMed Central articles intestinal fistula 2023 articles intestinal fistula 2024 articles intestinal fistula Scopus articles intestinal fistula impact factor journals intestinal fistula Scopus journals intestinal fistula PubMed journals intestinal fistula medical journals intestinal fistula free journals intestinal fistula best journals intestinal fistula top journals intestinal fistula free medical journals intestinal fistula famous journals intestinal fistula Google Scholar indexed journals
Article Details
Introduction
Wound infection is the most common postoperative complication that includes surgical site infections (SSIs), seroma or hematoma and wound dehiscence. This leads to prolonged healing time, increased cost and decrease in quality of life [1]. It can also lead to incisional hernia formation and delay the commencement of adjuvant chemotherapy or interventions [2]. The risk factors for wound infection includes emergency surgery especially in the setting of sepsis, obesity, poor nutritional status, a history of smoking, diabetes [3].
Application of Negative Pressure Wound Therapy (NPWT) is an effective way to manage both open and chronic wounds including large and deep clean wounds, open abdominal wounds, skin grafts, open fractures, pressure ulcers [4]. It involves the application of sub atmospheric pressure to a healing wound. Usually, 50mm Hg to 125mmHg pressure is used. There are several mechanisms postulated to the efficacy of NPWT. It decreases seroma formation in a wound and stimulates angiogenesis and granulation. It also generates a hypoxic environment in a wound, resulting in the upregulation of inflammatory cytokines, which stimulates wound healing [5].
NPWT was first introduced in 1997 [6]. There are several studies that showed its effectiveness in reducing the SSI rate and promoting wound healing [7-9]. Cochrane review showed that in comparison with wound dressing, NPWT reduces the healing time in case of diabetic foot [10]. It has been widely practiced in the NHS. NPWT is delivered by skilled and dedicated specialist tissue viability nurses in both in-patient settings and community settings. However, the actual clinical efficacy, financial burden and complexity of its use with introduction of newer devices and components have always been controversial because of lack of robust high quality clinical effectiveness trials [11,12]. The aim of the study was to evaluate the safety and effectiveness of NPWT on surgical wounds in a district general hospital (DGH).The primary end point was incidence of complete wound healing. Secondary end point was complication rate.
Methodology
It was a retrospective review of prospectively collected data. There were 102 patients included in our study over a period of 21 months from January 2018 to September 2019. Data were collected from patients records and hospital electronic data base. Patient demographics including Body Mass Index (BMI), diagnosis, comorbidities, indications for the application of NPWT, duration of therapy and adverse events including those related and unrelated to the treatment process were collected. Other variables like wound characteristics such as anatomical site, dimensions, type and primary operation including etiology and NPWT related variables such as duration, pressure, type (continuous vs intermittent) were recorded. All adult patients with general surgical wounds not amenable for simple wound dressing were included in the study. The NPWT was performed by experienced doctors and trained nurses.
Results
A total of 102 patients were included in the study. The Male to female ratio in the study was 40:62. The median age of patients was 61 (30-96) years (Table 1).
The majority (61.7%, n=63) of the patients were overweight or obese with BMI in the range of 25-35 and 11.8% (n=12) with a BMI above 35. This was followed by 26.4%(n=27) with a normal BMI. However, there was no direct correlation between BMI and requirement or complication related to NPWT.
ASA score was recorded in relation to the patient comorbidities and showed that the majority (81.3%) were either ASA II (33.3%, n= 34) or III (48%, n= 49).
Etiology of NPWT was postoperative abdominal surgery in the majority of the sample (n=73) with wound located over anterior abdominal wall making up 71.5% of the study population. Of these, majority were surgical site infection (n=68) and five patients received NPWT as a method of temporary abdominal closure (n=5). Other etiologies included post examination under anesthesia of anorectum with abscess drainage (n=17), pilonidal sinus surgery (n=10), one perineal abscess (n=1) and an extensive perineal debridement for Fournier’s gangrene (n=1).
The wound size revealed a median length of 8 cm (range 3-20) and median width of 5 cm (range 1-31). Application of NPWT was initially done either in theatre following an operation (36.2% n=37) or later on in ward (63.7% n=65)
The total duration of NPWT varied between patients with a median value of 21.5 days (range 2-120).
The majority (96.1%, n= 98) of the wounds healed completely as expected requiring no further intervention. Complete healing was defined as 100% skin epithelialization without the need for further drainage or dressing However, there were only four documented complications which mandated abandoning NPWT. Three patient had a minor complication of skin irritation/ contact dermatitis due to the dressing material which and was treated conservatively and NPWT discontinued while another patient who had a background of crohn’s disease developed an intestinal fistula following the application of NPWT. However, it wasn’t determined if the fistula was already present or the NPWT was the cause of it, but NPWT was discontinued, the patient was managed conservatively and the fistulae healed consequently. One patient had an extensive perineal debridement for Fournier’s gangrene. The patient was subsequently transferred to a plastic team for skin grafting. He had initial NPWT prior to grafting and had a good outcome (Figure 1,2 &3).
None of our patients developed infection and sepsis, foam retention in the wound, tissue adherence, bleeding or severe pain.
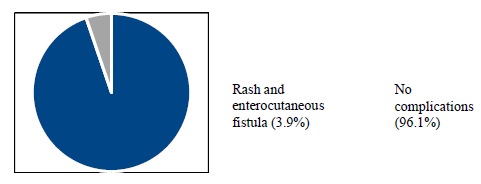
Figure 1: Pie chart showing complications.
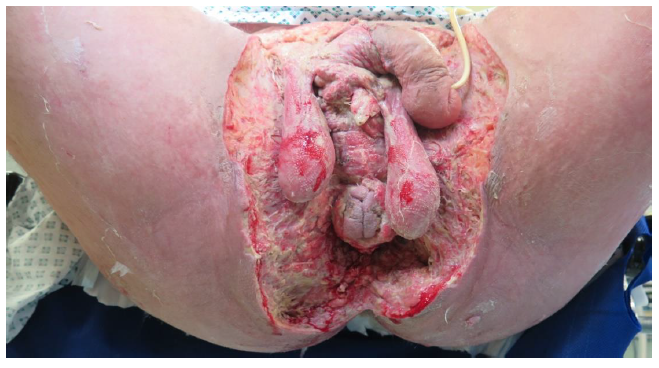
Figure 2: Patient presented with severe sepsis and hyperglycaemia and on catheterization, it was noted that the scrotal skin was erythematous and that the scrotum had doubled, in size within a 24-hour period. Urgent CT which confirmed Fournier’s gangrene as was suspected. Radical debridement of scrotum and perineum following Fournier’s gangrene with formation of a sigmoid colostomy was done [13].
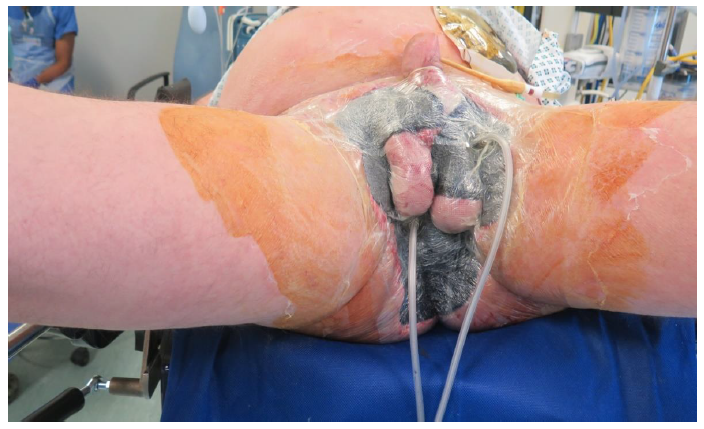
Figure 3: NPWT with drains in situ and pressure of about 125mmhg [13].
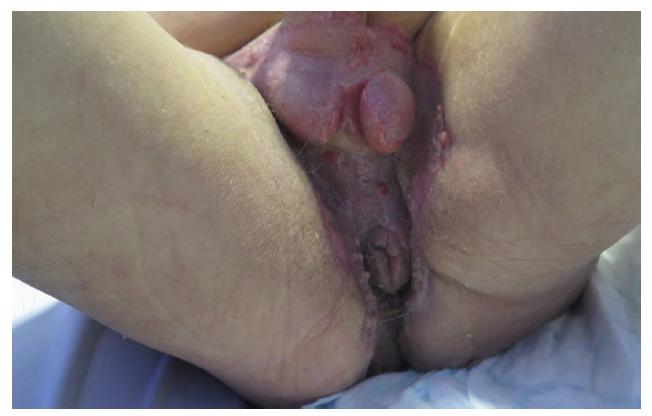
Figure 4: Post vac dressing and skin grafting outcome. A total of 43 days treatment with good wound healing [13].
|
Variables |
Values |
|
Total Number of Patients |
102 |
|
Patient Characteristics |
|
|
Male |
40 |
|
Female |
62 |
|
Median Age in years |
61 (30-96) |
|
BMI |
|
|
<25 |
27(26.4%) |
|
25-35 |
63(61.7%) |
|
>35 |
12(11.8%) |
|
ASA grade |
|
|
ASA-I |
19(18.6%) |
|
ASA –II |
34(33.3%) |
|
ASA-III |
49(48%) |
|
Surgery |
|
|
Laparotomy (abdominal wound) |
73 |
|
Pilonidal Sinus Surgery |
10 |
|
Perineal abscess and extensive perineal debridement |
2 |
|
Post Examination under anesthesia and Incision and Drainage of Abscess (Perianal Region.) |
17 |
|
Wound Characteristics |
|
|
Median Length in cm |
8 (3-20) |
|
Median Width |
5 cm (1-31) |
|
VAC Therapy |
|
|
Continuous |
102 |
|
Complications |
4 (3.9%) |
|
Median Duration |
21.5 days (range 2-120). |
Table 1: Following table summarizes the different variables considered in the study.
Discussion
Negative pressure wound therapy is safe and it accelerates wound healing. There is sufficient evidence to justify its use in the treatment of diabetes-associated chronic leg wounds [14]. Its efficacy has been proven for acute as well as chronic wounds, including those of vascular and diabetic origin [15]. We also know from the data that, NPWT in critically ill patients with open abdomen improves outcome [16].
The way NPWT works is complex and not all of its aspects are yet completely understood. It is postulated that there are four primary effects and several secondary effects. Primary mechanism of action includes macrodeformation, microdeformation, fluid removal and environmental control of the wound. In macrodeformation, the suction draws the wound edges together depending on the mobility of the surrounding tissue [17]. Microdeformation streches the cells, which inturn facilitates division and proliferation [18]. It also creates an insulated warm and moist environment and remove fluid from surrounding oedematous tissue [19]. There are also secondary effects that helps in wound heling by NPWT. These include granulation tissue formation, cell proliferation, modulation of inflammation , upregulating neurotransmitter and bacterial levels [20].
Thre is cochrane review of 45 studies to assess the benefit of NPWT in comparision to standard wound therapy for wounds healing by primary intention [21].
The review concluded that, there is slight increase in benefit of NPWT in comparision with standard wound therapy in wounds healing by primary intention. There is no additional benefit in terms of outcome like mortality, total rate of complication, length of hospital stay, pain and health related quality of life.
With regards to wound healing by secondary intention, there is also cochrane review [22] which assessed the effects of negative pressure wound therapy (NPWT) on the healing of surgical wounds healing by secondary intention in any care setting. Only two studies with 69 participants were included in this review. The authors concluded that there is currently no stringent RCT evidence available regarding the clinical effectiveness of NPWT in the treatment of surgical wounds healing by secondary intention. It remain largely uncertain whether NPWT gives any potential benefit in case of wound healing by secondary intention.
Our data showed that NPWT is very effective in healing wound by secondary intention. >96% of our cases healed completely.
Previous report [23] showed that, although NPWT promotes excellent wound healing, several complications can occur with its use like bleeding, pain and infection. Its long term use may be associated with decrease life quality, increase anxiety, and malnutrition. In our study, only four patients (3.9%) developed complications. Three patient had a minor complication of skin irritation due to the dressing material. All of them were treated conservatively and NPWT discontinued. One patient, who had a background of crohn’s disease developed an intestinal fistula following the application of NPWT. The therapy was discontinued and the fistula healed by its own.
Our study has limitations. It is retrospective, observational study with single centre experience. There was no comparision with other modalities of wound therapy to conclude its significant benefit. There was no long term follow up data to comment on patient reported outcome like cosmesis, cost analysis or quality of life.
To overcome the potential bias, we need large, multicentre RCTs with a long term follow up.
Conclusion
Our study showed the use of NPWT gives satisfactory results in laparotomy and perianal wound. It also accelerates healing of wound related with pilonidal disease operation. Its advantages include accelerated wound healing times, reduce risk of infection, reduce the number of dressing changes while increase blood flow to the wound area with simultaneously drawing out excess fluids. There was low complication rate recorded in our study. NPWT therapy can also be used easily in the community with set up of good community support network.
It is clear that NPWT is very helpful in many different clinical situations. It is a versatile treatment method that has provided effective treatment for different wounds. As wounds are heterogeneous in nature, using NPWT for their treatment is not a simple and straightforward process. Each patient will have different needs and this will have to be taken into account when planning on the treatment.
With more research into NPWT, new and innovative ways may be discovered in which they can be used, and the effectiveness of current treatments will undoubtedly increase.
Acknowledgements
Specialist nurse Sally Wilson for her involvement with managing NPWT wound in the wards.
She also presented a paper on this during the nurses forum and the regional surgical evening.
Conflict of interest
The Author(s) have no conflict of interest to disclose.
References
- Zimlichman E, Henderson D, Tamir O, et al. Health care-associated infections: a meta-analysis of costs and financial impact on the US health care system. JAMA Intern Med 173 (2013): 2039-2046.
- Smith RL, Bohl JK, McElearney ST, et al. Wound infection after elective colorectal resection. Ann Surg 239 (2004): 599-605.
- Taylor GD, Kirkland TA, McKenzie MM, Sutherland B, Wiens RM. The effect of surgical wound infection on postoperative hospital stay. Can J Surg 38 (1995): 149-153.
- Cahill C, Fowler A, Williams LJ. The application of incisional negative pressure wound therapy for perineal wounds: A systematic review. Int Wound J 15 (2018): 740-748.
- Huang C, Leavitt T, Bayer LR, Orgill DP. Effect of negative pressure wound therapy on wound healing. Curr Probl Surg 51 (2014): 301-331.
- Morykwas MJ, Argenta LC, Shelton-Brown EI and McGuirt W. Vacuum-Assisted Closure: A New Method for Wound Control and Treatment: Animal Studies and Basic Foundation. Annals of Plastic Surgery 38 (1997): 553-562.
- O'Leary DP, Peirce C, Anglim B, et al. Prophylactic Negative Pressure Dressing Use in Closed Laparotomy Wounds Following Abdominal Operations: A Randomized, Controlled, Open-label Trial: The P.I.C.O. Trial. Ann Surg. 2017;265(6):1082-1086.
- Sahebally SM, McKevitt K, Stephens I, et al. Negative Pressure Wound Therapy for Closed Laparotomy Incisions in General and Colorectal Surgery: A Systematic Review and Meta-analysis. JAMA Surg 153 (2018): e183467.
- Strugala V, Martin R. Meta-Analysis of Comparative Trials Evaluating a Prophylactic Single-Use Negative Pressure Wound Therapy System for the Prevention of Surgical Site Complications. Surg Infect (Larchmt) 18 (2017): 810-819.
- Liu Z, Dumville JC, Hinchliffe RJ, et al. Negative pressure wound therapy for treating foot wounds in people with diabetes mellitus. Cochrane Database Syst Rev 10 (2018): CD010318.
- Banwell PE, Téot L. Topical negative pressure (TNP): the evolution of a novel wound therapy. J Wound Care 12 (2003): 22-28.
- Gottrup F, Apelqvist J, Price P. Outcomes in controlled and comparative studies on non-healing wounds: recommendations to improve the quality of evidence in wound management. J Wound Care 19 (2010): 239–68.
- Ikechi CO, Mohamed H, Shah A, Wilson S, Pangeni A, Fernandes R, et al. Evaluating the Outcome of Vacuum Assisted Closure of Surgical Wound – A Retrospective Single Centre Review. Clin Surg 4 (2019): 2649.?
- Blume PA, Walters J, Payne W, Ayala J, Lantis J. Comparison of negative pressure wound therapy using vacuum-assisted closure with advanced moist wound therapy in the treatment of diabetic foot ulcers: a multicenter randomized controlled trial. Diabetes Care 31 (2008): 631–6.
- Roberts DJ, Zygun DA, Grendar J, Ball CG, Robertson HL, Ouellet JF, et al. Negative-pressure wound therapy for critically ill adults with open abdominal wounds: a systematic review. The journal of trauma and acute care surgery 73 (2012): 629–639.
- Baxter, Helena; Ballard, Kate. Vacuum-Assisted Closure. Nursing Times 97 (2001): 51–52.
- Orgill DP, Manders EK, Sumpio BE, et al. The mechanisms of action of vacuum assisted closure: more to learn. Surgery 146 (2009): 40-51.
- Saxena V, Hwang CW, Huang S, Eichbaum Q, Ingber D, Orgill DP. Vacuum-assisted closure: microdeformations of wounds and cell proliferation. Plast Reconstr Surg 114 (2004): 1086-1098.
- Morykwas MJ, Simpson J, Punger K, Argenta A, Kremers L, Argenta J. Vacuum-assisted closure: state of basic research and physiologic foundation. Plast Reconstr Surg 117 (2006): 121S-126S.
- Mouës CM, Vos MC, van den Bemd GJ, Stijnen T, Hovius SE. Bacterial load in relation to vacuum-assisted closure wound therapy: a prospective randomized trial. Wound Repair Regen 12 (2004): 11-17.
- Webster J, Scuffham P, Sherriff KL, Stankiewicz M, Chaboyer WP. Negative pressure wound therapy for skin grafts and surgical wounds healing by primary intention. Cochrane Database Syst Rev 18 (2012): CD009261.
- Dumville JC, Owens GL, Crosbie EJ, Peinemann F, Liu Z. Negative pressure wound therapy for treating surgical wounds healing by secondary intention. Cochrane Database Syst Rev 4 (2015): CD011278.
- Li Z, Yu A. Complications of negative pressure wound therapy: a mini review. Wound Repair Regen 22 (2014): 457-461.


 Impact Factor: * 4.2
Impact Factor: * 4.2 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 