Stress Induced Right Ventricular Diastolic Dysfunction in Non-severe Chronic Obstructive Pulmonary Disease - the Role of Oxidative Stress and Inflammation
Article Information
Zheina Cherneva1*, Dinko Valev2, Vania Youroukova3, Radostina Cherneva3
1Medical Institute of the Ministry of Internal Affairs, Sofia, Bulgaria
2University First Multiple Clinic for Active Treatment, Sofia, Bulgaria
3Medical University Sofia, University Hospital for Respiratory Diseases “St. Sophia”, Sofia, Bulgaria
*Corresponding Author: Zheina Cherneva, Medical Institute of the Ministry of Internal Affairs, bul. General Skobelev 79, Sofia, Bulgaria
Received: 14 August 2020; Accepted: 24 August 2020; Published: 28 August 2020
Citation: Zheina Cherneva, Dinko Valev, Vania Youroukova, Radostina Cherneva. Stress Induced Right Ventricular Diastolic Dysfunction in Non-severe Chronic Obstructive Pulmonary Disease - the Role of Oxidative Stress and Inflammation. Cardiology and Cardiovascular Medicine 4 (2020): 460-480.
View / Download Pdf Share at FacebookAbstract
Background: Oxidative stress and inflammation have been implicated in the pathogenesis of diastolic dysfunction (DD) and are both present in chronic obstructive pulmonary disease (COPD). Our aim was to evaluate the role of 8-isoprostane, prostaglandin E2 and resistin for stress induced right ventricular DD (RVDD) in non-severe COPD.
Methods: 104 patients with non-severe COPD (FEV1>50%) and preserved left ventricular ejection fraction >50% underwent cardio-pulmonary exercise testing (CPET). Echocardiography was performed before CPET and 1-2 minutes after peak exercise. Peak E/e’ ratio>6 was a marker for stress RVDD. To measure urine concentration of 8-isoprostanes, prostaglandine-E2 and plasma resistin levels mass spectrometry and ELISA were applied.
Results: Patients were divided into two groups: with (82) and without stress RVDD (22). In subjects with and without RVDD the levels of 8-isoprostane were (30.78 vs 30.41μmol/l/cre, p-0.847); prostaglandin E2 - (49.73 vs 62. 19 μmol/l/cre, p-0.014); resistin plasma levels (18.91 vs 5.47ng/ml, p-0.027). Resistin and prostaglandine E2 correlated to stress RV E/e’, but were not independent indices for it. RAVI (cut-off 20.55 ml/m2; sensitivity 86%; specificity 86%), RVWT (cut-off 5.25 mm; sensitivity 100%; specificity 63%) and RV E/A at rest (cut-off 1.05; sensitivity 79.7%; specificity 90.5%) independently predicted stress RV E/e’ with the accuracy of 92%.
Conclusions: Patients with stress RVDD demonstrate similar levels of oxidative stress. Prostaglandine E2 may have protective role in RV remodeling, while resistin plasma levels contribute to RVDD pathogenesis. RAVI, RVWT, RV E/A and RV E/e’ ratio at rest may be used as independent predictors for stress RVDD.
Keywords
Inflammation; Oxidative stress; Stress echocardiography; Heart failure with preserved ejection fraction; Chronic obstructive pulmonary disease
Article Details
Abbreviations:
COPD: Chronic obstructive pulmonary disease; DD: Diastolic dysfunction; RVDD: Right ventricular diastolic dysfunction; CPET: Cardio-pulmonary exercise testing; CV: Cardio-vascular; LVDD: Lef ventricular diastolic dysfunction; RAVI: Right atrium volume index; RVWT: Right ventricle wall thickness; AT: Acceleration time; PASP: Pulmonary arterial systolic pressure; PAP: Pulmonary arterial pressure; TAPSE – Tricuspidal annular plane systolic excursion; DH: Dynamic hyperinflation; FRC: Functional residual capacity; TLC: Total lung capacity; EELV: End-expiratory lung volume; HRAM: High Resolution Accurate Mass; RELM: Rodent resistin-like molecules; ROS: Reactive oxidative species; MRC: Medical research council; O2 pulse: Oxygen pulse; VE: Minute ventilation; RER: Respiratory exchange ratio; V'O2: Oxygen consumption; VE/VCO2 slope: Ventilatory efficiency
Introduction
Cardio-vascular (CV) comorbidity in COPD is assumed as “cardio-pulmonary continuum” rather than being attributed to shared risk factors. Cardio-respiratory interactions are not restricted to certain structural, haemodynamic, vascular or genetic parameters and both disease states are related with oxidative stress and systemic inflammation [1,2].
Contemporary investigational methods demonstrate that COPD patients have small RV dimensions and RV hypertrophy-factors, predisposing to right ventricular diastolic dysfunction (RVDD) [3-6]. RVDD is an early sign of pulmonary vasculopathy and precedes the clinical/echocardiographic manifestation of pulmonary hypertension [7-9]. Right ventricular dysfunction and pulmonary vessel impairment may be essential contributors for dyspnea and limited physical activity even in non-severe forms of COPD [10,11].
RVDD detection is thus essential for the early diagnosis of pulmonary vasculopathy in COPD management and physical activity improvement. The simultaneous performance of stress-echocardiography and cardio-pulmonary exercise testing may provide timely detection of RVDD in COPD patients with exertional dyspnoea.
Oxidative stress and inflammation in addition to intrathoracic and haemodynamic pressure oscillations have been assumed as leading factors for both right and left ventricular diastolic remodeling in COPD. Assuming this we set the following aims: 1) to detect the frequency of stress RVDD - in non-severe COPD patients, free of overt cardiovascular pathology who complain of exertional dyspnea; 2) to establish which echocardiographic parameters at rest may be predictors for stress RVDD; 3) to establish which inflammatory (resistin, prostaglandine E2) and oxidative stress (8-isoprostane) markers are predictors for stress RVDD.
Materials and Methods
Patients and Study Protocol
It was a prospective study that was performed in 224 clinically stable outpatients, diagnosed with COPD at the University Hospital for Respiratory Diseases “St. Sophia”, Sofia. Only 163 of them met the inclusion criteria: The inclusion criteria are: 1) non-severe COPD (post bronchodilatator FEV1/FVC<70%; FEV1/ > 50%); 2) preserved left ventricular systolic function LVEF>50%; 3) lack of overt cardiovascular disease; 4) exertional dyspnea. All the subjects had exertional dyspnoea, but a total of 104 patients (64 men, 40 women; mean age of 62.9±7.5 years) were considered eligible, assuming the exclusion criteria. The recruitment period was between May 2017-April 2018, and was approved by the local Ethical Committee (protocol 5/12.03.2018). All the patients signed informed consent before their participation. They were preliminary acquainted with the aim of the study, its scientific value and the potential presentation of data at different forums.
The following exclusion criteria were considered: 1) left ventricular ejection fraction (LVEF) <50%; 2) left ventricular diastolic dysfunction at rest more than first grade; 3) presence of echocardiographic criteria of pulmonary hypertension (systolic pulmonary arterial pressure > 36 mmHg, maximum velocity of the tricuspid regurgitation jet > 2.8 m/s; 4) valvular heart disease; 5) documented cardiomyopathy; 6) severe uncontrolled hypertension (systolic blood pressure >180 mmHg and diastolic blood pressure >90 mmHg); 7) atrial fibrillation or malignant ventricular arrhythmia; 8) ischaemic heart disease; 9) anaemia; 10) diabetes mellitus; 11) cancer; 12) chronic kidney disease; 13) recent chest or abdominal surgery; 14) recent exacerbation (during the last three months); 15) recent change (during the last three months) in medical therapy.
Procedures
Pulmonary Function Testing
All the subjects underwent preliminary clinical examination which included chest X-ray, spirometry, electrocardiogram, echocardiography. Those eligible for the study performed spirometry and exercise stress test. They were performed on Vyntus, Cardio-pulmonary exercise testing (Carefusion, Germany) in accordance with ERS guidelines [12]. Only patients with mild/ moderate airway obstruction (FEV1 >50%) were selected.
Dynamic Hyperinflation (DH)
Body plethysmography (residual volume (RV), functional residual capacity (FRC), total lung capacity (TLC)) was performed on (Vyntus, body plethysmograph, CareFusion, Germany) using European and American Thoracic Society guidelines [12]. Changes in operational lung volumes were derived from measurements of dynamic inspiratory capacity (IC), assuming that total lung capacity (TLC) remained constant during exercise [13,14]. This has been found to be a reliable method of tracking acute changes in lung volumes [13-15]. IC was measured at the end of a steady-state resting baseline, at 2 min intervals during exercise, and at end exercise. End-expiratory lung volume (EELV) was calculated from IC maneuvers at rest, every 2 minutes during exercise and at peak exercise (Vyntus).In these maneuvers, after EELV was observed to be stable over 3-4 breaths, subjects were instructed to inspire maximally to TLC. For each measurement, EELV was calculated as resting TLC minus IC, using the plethysmographic TLC value. Dynamic IC (ICdyn) was defined as resting IC minus IC at peak exercise [16]. Dynamic hyperinflation (DH) was defined as a decrease in IC from rest of more than 150 mL or 4.5% pred at any time during exercise [16].
Stress Test Protocol – Cardio-Pulmonary Exercise Testing (CPET)
All the patients underwent symptom limited incremental exercise stress test following the guidelines [17]. A continuous ramp protocol was applied. After two minutes of unloaded pedaling (rest phase-0W), a three minute warm-up phase (20W) followed. The test phase included 20W/2min load increments. Patients were instructed to pedal with 60-65 rotations per minute. Patients’ effort was considered to be maximal if two of the following criteria emerged: predicted maximal HR is achieved; predicted maximal work is achieved; ’VE/’VO2 >45, RER >1.10 as recommended by the ATS/ACCP [18]. A breath-by-breath analysis was used for expiratory gases evaluation. ’VO2 (mL/kg/min), ’VCO2 (L/min), ‘VE (L/min) and PetCO2 (mm Hg) were collected continuously at rest and throughout the exercise test. Peak values of oxygen consumption and carbon dioxide production were presented by the highest 30-second average value, obtained during the last stage of the exercise test. Peak respiratory exchange ratio was the highest 30second averaged value between ’VO2 and ’VCO2 during the last stage of the test. Resting PetCO2 was the 2-minute averaged value in the seated position prior to exercise, while the peak value was expressed as the highest 30-second average value obtained during the last stage of the exercise test. Ten-second averaged ’VE and VCO2 data, from the initiation of exercise to peak, were used to calculate the ’VE/’VCO2 slope via least squares linear regression. It has been shown to produce clinically optimal information compared with derivations excluding data past the respiratory compensation point [19]. ‘VE/’VCO2 slope was calculated as a linear regression function using 10-s averaged values and excluding the non-linear part of the relationship after the respiratory compensation point where nonlinear rise in ’VE occurred relative to ’VCO2 in the presence of decrease of end-tidal pressure of CO2. As the study group consisted of COPD patients a dual approach for the measurement of the anaerobic threshold (AT) was applied. Both V-slope method and the ventilatory equivalents method for ‘VO2 and ’VCO2 were used. The modified Borg scale was applied for peak dyspnea and leg discomfort.
Echocardiography Methods
Echocardiography included the generally applied approaches of M-mode, two-dimensional and Doppler echocardiography. Routine structural and haemodynamic indices of both chambers were measured following the guidelines [20,21]. The systolic function of the left ventricle (LV) was defined by Simpson’s modified rule. The diastolic function of both ventricles was evaluated by the E/A ratio and the average E/e’ ratio at rest. As a more precise approach for diastolic dysfunction detection, tissue Doppler analysis was used. We used e’ value as the average of medial and the lateral measurements for the mitral annulus. The peak of the average E/e’ ratio >15 was considered as a marker for stress induced left ventricular diastolic dysfunction (LVDD).
The dimensions of the right ventricle were assessed from the long-axis parasternal and apical four chamber view [22]. Tricuspid annular plane systolic excursion (TAPSE) and S-peak velocity were analysed for RV systolic function evaluation. Right ventricular wall thickness (RVWT) was measured in end-diastole. Systolic pulmonary arterial pressure was calculated by Bernoulli equation and by the acceleration time (AT) [22,23]. Right atrium volume index (RAVI) was measured at right ventricle end-systole by Simpson’s modified rule. The peak of the average E/e’ ratio >6 was considered as a marker for stress induced RVDD. Stress induced RV diastolic dysfunction was considered if stress induced E/e’ ratio >6. All parameters were measured at end-expiration and in triplicate during different heart cycles [23].
Laboratory Assays
Approximately 7 mL of venous blood was obtained from all cases. Blood samples were centrifuged immediately after collection and isolated plasma was stored in vials at –80°C until assayed. Resistin was measured by commercial kits, following the procedure protocol. Resistin was determined by an ELISA kit (RayBio_Human Resistin ELISA Kit) Protocol (Cat#:ELH-Resistin-001). The intra- and interassay coefficients of variation in this assay kit ranged from 10 to 12%. Plasma resistin levels were measured in ng/ml.
High Resolution Accurate Mass (HRAM) of 8-isoprostane and prostgalndine E2
Approximately 20 mL of urine was obtained from all cases the levels of 8-isoprostane and prostgalndine E2 in urine samples were determined by HRAM (high resolution accurate mass) mass spectrometry on LTQ Orbitrap® Discovery (ThermoScientific Co, USA) mass spectrometer, equipped with Surveyor® Plus HPLC system and IonMax® electrospray ionization module. The analyses were carried out by stable isotope dilution method in negative ionization mode using HESI II (heated electrospray ionization) source type. The concentration and purification of 8-isoprostane and prostgalndine E2 from urine samples was processed by affinity sorbent (Cayman Chemical, USA), following the producer’s protocol with some modification. The urinary 8-isoprostane and prostgalndine E2 levels were standardized to the levels of urinary creatinine. Creatinine was measured applying the enzyme method - Creatinine plus version 2 Cobas Integra (Roche). Results are given in pg/mkmol/creatinine.
Statistical Analysis
Descriptive statistics was used for demographic and clinical data presentation. The Kolmogorov-Smirnov test was used to explore the normality of distribution. Continuous variables were expressed as median and interquartile range when data was not normally distributed and with mean ±SD if normal distribution was observed. Categorical variables were presented as proportions. Data were compared between patients with and without RVDD. An unpaired Student’s t test was performed for normally distributed continuous variables. Mann-Whithney-U test was used in other cases. Categorical variables were compared by the χ2 test or the Fisher exact test. Receiver operating characteristic (ROC) curves were constructed. ROC analysis was performed to test RV echocardiographic parameters at rest that may accurately distinguish between stress RV E/e’>6 or <6. Regression analysis was also applied with the echocardiographic indices, as qualitative parameters, using their cut-off values. Univariable regression analysis was performed to assess which echocardiographic, CPET parameters and biomarkers (resistin, prostglandine E2 and 8-isoprostanes) are associated with stress RV E/e’>6. Multivariable logistic regression analysis by using a forward stepwise approach detected the signi?cant independent predictors of stress RV E/e’>6. Predictive models were constructed. Age, sex, height, weight (BMI), FEV1, ICdyn, were specifically included as co-variates.
In all cases a p value of less than 0.05 was considered significant as determined with SPSS® 13.0 Software (SPSS, Inc, Chicago, Ill) statistics® 13.0 Software (SPSS, Inc, Chicago, Ill) statistics.
Results
Demographic and Clinical Data
Subjects enrolled in the study were Caucasians at a mean age of 62.50±8.5 years and a body mass index of 27.26±6.92kg/m2. They were divided into two groups-subjects with stress induced right ventricular diastolic dysfunction-78% (82/104) (COPD-RVDD), and those without stress induced diastolic dysfunction 22% (22/104), (COPD -no RVDD). There was no statistically significant difference regarding the demographic and clinical parameters between the two groups (Table 1).
|
Patients w/o stress RVDD (22) |
Patients with stress RVDD (82) |
p-value |
|
|
Demographic data |
|
||
|
Age, year, |
60.00 ± 8.00 |
65.00 ± 9.00 |
0.143* |
|
Male:Female gender, n |
14:8 |
50:32 |
0.298 † |
|
Current smokers, n (%) |
17(77%) |
45(55%) |
0.341 † |
|
Former smokers, n (%) |
3 (14%) |
19 (23%) |
0.235 † |
|
Non-smokers, n (%) |
2(9%) |
18 (22%) |
0.272 † |
|
Packet-year |
26.52 (23.46-30.43) |
32.11(28.82-36.13) |
0.176 † |
|
Body mass index, kg/m2 |
28.00 (25.25-30.5) |
26.52 (22.72-30.61) |
0.981? |
|
Respiratory function |
|
|
|
|
FVC, l/min |
2.05 (2.11-3.73) |
2.21 (1.71-2.93) |
0.491? |
|
FEV 1, l/min |
1.60 (1.15-2.42) |
1.52 (1.14-1.75) |
0.207? |
|
FEV1/FVC % |
65.50 (54.81-68.82) |
62.59 (46.57-66.79) |
0.218? |
|
mMRC |
1.55 ±0.73 |
1.42±0.68 |
0.065? |
|
Acid-base balance |
|||
|
Ph |
7.44 (7.42-7.46 |
7.43(7.41-7.45 |
0.093? |
|
O2 , mmHg |
67.20 (63.56-71.68) |
70.6 (63.2-74) |
0.126? |
|
CO2, mmHg |
34.73 (31.27-39.21) |
35.7 (32.5-40) |
0.811? |
|
Sat, % |
94.75 (92.67-95.0) |
95.00 (93.9-95.5) |
0.069? |
|
CPET parameters |
|||
|
Peak Load , W |
86.66 (78.65-94.76) |
73.08 (68.93-83.16) |
0.039? |
|
Peak VE, l/min |
41.1 (32.12-48.17) |
39.07 (31.89-48.32) |
0.025? |
|
PeakV'O2, ml/min/kg |
14.30 (12.6-16.15) |
13.40(15.77-12.55) |
0.121? |
|
RER |
1.05 (0.98-1.18) |
1.08 (1.01-1.19) |
0.503? |
|
PeakO2 pulse ml/min/kg |
9.51 (9.02-13.1) |
7.92(6.27-9.84) |
0.027? |
|
Peak VE/VCO2 slope |
34.11 (33.78-36.89) |
36.98 (34.26-38.91) |
0.016? |
|
GOLD stages |
|||
|
GOLD I, n (%) |
13 (59%) |
40 (49%) |
0.141? |
|
GOLD II, n (%) |
9 (41%) |
42 (51%) |
0.095 ? |
|
Dynamic hyperinflation |
|||
|
ICdyn>150ml |
7 (32%) |
57 (69%) |
0.049? |
|
ICdyn<150ml |
15(68%) |
25(31%) |
0.042? |
|
Biomarkers |
|||
|
Urine 8-isoprostane, µmol/l/cre |
30.41 ±3.74 |
30.78 ±3.25 |
0.847? |
|
Urine prostaglandin E2, µmol/l/cre |
62.19 ±4.35 |
49.73 ±3.42 |
0.014? |
|
Plasma resistin, ng/ml |
5.47±2.52 |
18.91±3.32 |
0.027? |
Table 1: Anthropometric, clinical, cardio-pulmonary parameters and biomarkers of the patients with and w/o stress RVDD
*Unpaired t test; ?Mann-Whitney U test; †chi square test; § Abbreviations: RVDD – right ventricular diastolic dysfunction; mMRC – medical research council; O2 pulse – oxygen pulse; VE – minute ventilation; RER – respiratory exchange ratio; V'O2 – oxygen consumption; VE/VCO2 slope – ventilatory efficiency; •p<0.05 between patients with and w/o RVDD.
There was no substantial distinction between the patients with and without stress RVDD, regarding the incidence of GOLD stages. Mild COPD was found in 40 (49%) of the patients with stress RVDD vs 13 (59%) in those without RVDD. Moderate COPD was met in 42 (51%) of the patients with stress RVDD vs 9 (41%) in those without. Most of the patients without stress RVDD were with mild COPD-13 (59%); moderate COPD demonstrated 9 (41%) of them; in patients with stress RVDD the GOLD stages were almost evenly distributed – mild forms of COPD showed 40 (49%) of the patients vs 42 (51%) with moderate COPD.
Dynamic Hyperinflation
Although none of the patients in the studied group demonstrated static hyperinflation, 64 (62%) showed DH. There is a predominance of hyperinflators – 69% among the patients with stress RVDD in comparison to those without – 32% (p-0.049). In contrast, non-hyperinflators were the majority (68%) of the subjects without stress RVDD; (31%) of the patients with stress RVDD were also non-hyperinflators (p-0.042) (table 1).
Markers for Inflammation and Oxidative Stress
8-isoprostane levels did not differ between the two groups–patients with and without RVDD (30.78 vs 30.41µmol/l/cre, p-0.847). Resistin plasma levels were higher in patients with RVDD, compared to those without, (18.91 vs 5.47 ng /ml, p-0.027 ). Urine concentrations of prostaglandin E2 were higher in subjects without RVDD vs those with (62.19 vs 49.73 µmol/l/cre; p-0.014 ) (table 1). Resistin and prostaglandine E2 correlated to stress RV E/e’, but were not an independent predictors for it (table 4).
RV Parameters
The echocardiographic characteristics are detailed in Table 2.
|
Patients w/o stress RVDD (22) |
Patients with stress RVDD (82) |
p-value |
|
|
LV structural parameters |
|||
|
TDD, mm |
51 (49.5-56.5) |
51 (48-54) |
0.536* |
|
TSD,mm |
34 (32-39) |
33 (31-35) |
0.473* |
|
TDV, ml |
122.5 (115-157) |
121(107.5-139) |
0.616* |
|
TSV, ml |
45 (41-69) |
44 (38-50) |
0.481* |
|
Septum, mm |
12.00 (11-12.75) |
12.00 (11-13) |
0.526* |
|
PW, mm |
12.00 (11.25-2.75) |
12.00 (11-13) |
0.403* |
|
LV functional parameters at rest |
|||
|
E/A ratio |
0.78 (0.76-0.83) |
0.84 (0.75-1.21.) |
0.201* |
|
E/e' aver ratio |
6.96 (6.27-8.33) |
6.66 (5.63-8.1) |
0.317* |
|
LV functional parameters after exercise stress test |
|||
|
LVEF, %, Simpson |
65.00(60-66) |
61.00 (67-65) |
0.421* |
|
E/A ratio |
1.22 (0.88-1.37) |
1.71 (1.5-2.00) |
0.041* |
|
E/e' aver |
8.12 (7.25-10) |
17.14 (14.66-18.39) |
0.036* |
|
RV structural parameters |
|||
|
RAVI, ml/m2 |
16.55 (15.81-7.54) |
22.27 (20.65-23.85) |
0.024* |
|
RWT, mm |
5.00 (4.12-5.00) |
6.50 (6.00-7.00) |
0.038* |
|
RV diameter parasternal, mm |
28 (26.5-30) |
28 (26-30) |
0.438* |
|
RV basal, mm |
35 (35.5-39) |
38 (36-39) |
0.526* |
|
RV med, mm |
23 (22-25.75) |
27 (25.5-29) |
0.645* |
|
RV functional parameters at rest |
|||
|
E/A ratio |
0.83 (0.76-1.16) |
0.71 (0.66-0.83) |
0.532* |
|
E/e' aver |
5.47 (4.56-5.69) |
4.54(3.33-5.22) |
0.641* |
|
S peak velocity, cm/s |
15 (15-16) |
15 (15-16) |
0.897* |
|
AT, msec |
170 (165-180) |
170(160-180) |
0.615* |
|
sPAP, mmHg |
25.00 (23-27) |
28.00 (25-30) |
0.908* |
|
RV functional parameters after exercise stress test |
|||
|
E/A ratio |
1.28 (1.14-1.5) |
1.37 (1.22-1.52) |
0.887* |
|
E/e' aver |
6.92 (5.46-8.00) |
11.25 (9.00-13.33) |
0.039* |
|
S peak velocity, cm/s |
15 (13-16) |
14 (14-15) |
0.842* |
|
AT, msec |
162.5(155-170) |
110(95-115) |
0.039* |
|
sPAP, mmHg |
32.00 (30-33.75) |
38.00 (35-40) |
0.043* |
*Mann-Whitney U test;† Abbreviations: RVDD – Right ventricular diastolic dysfunction
Table 2: Echocardiographic parameters of the patients with and w/o RVDD
The median right ventricular basilar diameter was 38mm (35-39), right ventricular systolic function - S’ peak velocity 16m/s (15-16) and TAPSE – 22mm (21-24) were within normal limits. Median RAVI was at the upper limit of normal 19.47ml/m2 (21.38-23.61); Median RVWT – 6.5mm (6-7) with approximately 53% of subjects demonstrating evidence of right ventricular hypertrophy. None of the subjects had evidence of right atrial and ventricular enlargement. The pulmonary artery systolic pressure was estimated in all subjects -27mmHg (25-30) and was not elevated at rest.
Fourteen percent (15/104) of the patients demonstrated right ventricular diastolic dysfunction at rest (E/e’>6). Stress-induced myocardial velocities (E/e’>6), measured 1-2 minutes after peak load were higher in (82/104) - 78% of the patients in comparison to the rest (22/104) - 22%. Sixty-seven percent of the patients (67%) demonstrated stress-induced elevation of the systolic pulmonary arterial pressure (baseline 26.50±3.75mmHg; after CPET 35.00±4.38mmHg). There was not a significant difference between the two groups regarding functional (systolic and diastolic) parameters of the RV at rest. In contrast, right atrial (RA) geometry was distinctive. The mean values of RAVI in the group without stress-induced RVDD were significantly lower (16.55±1.72ml/m2) in comparison to the group with RVDD (22.27±3.19ml/m2). The same is observed regarding right wall thickness (RWT). In subjects without stress-induced RVDD, RWT was lower (5.00±0.87mm) in comparison to those with stress-induced diastolic dysfunction (6.50±1.00mm). The functional parameters that were distinctive between the groups were the AT and sPAP, measured at peak stress (Table 2).
LV Parameters
Our patients were with normal LV dimensions and had preserved LV systolic function table 2. LV wall thickness was 12mm (11-13). 62% of the subjects demonstrated evidence of left ventricular hypertrophy. In the group with stress-RVDD 67% (55/82) had LVH; in the group without stress-RVDD 45% (10/22) had LVH. If we compare the prevalence of LVH in patients with and without stress-RVDD, no statistically significant difference (p – 0.408) could be established. The left atrial and ventricular dimensions were within normal limits.
Only 30% of the patients had LV diastolic dysfunction at rest (average E/e’>8) and the remaining 70% were with normal LV diastolic function at rest. In the group with stress-RVDD 33% (27/82) had LV diastolic dysfunction at rest; in the group without stress-RVDD 18% (4/22) had LV diastolic dysfunction at rest. Regarding LVDD at rest no statistically significant difference between stress-RVDD/ without stress-RVDD groups was detected (p – 0.458).
A total of sixty-seven percent (67%) of all the patients had left diastolic dysfunction during exercise (E/e’>15). No significant difference in both structural and functional parameters of the LV at rest may be discerned between the patients with and without stress induced RVDD (Table 2). Statistically significant difference is present in: LV stress E/A, LV stress E/e’ (Table 2).
Right Heart Structural Abnormalities and Stress RVDD
ROC analysis was performed in order to assess the predictive value of the right heart structural parameters that are usually measured in clinical practice and the stress induced RVDD (stress E/e’ >6). Results are shown in (Table 3).
|
Area under the curve |
95% CI |
Cut-off value |
Sensitivity |
Specificity |
|||||
|
RV basil diameter, mm |
0.75 |
0.69-0.81 |
35.5 |
63% |
71% |
||||
|
RVWT, mm |
0.66 |
0.66-0.77 |
5.25 |
100% |
63% |
||||
|
RAVI, ml/m2 |
0.91 |
0.84-0.97 |
20.55 |
86.36% |
86.11% |
||||
|
E/A ratio at rest |
0.90 |
0.83-0.96 |
1.05 |
79.7% |
90.5% |
||||
|
E/e’ ratio at rest |
0.64 |
0.52-0.75 |
5.10 |
74.7% |
61.9% |
||||
|
TAPSE, mm |
0.70 |
0.58-0.82 |
21.62 |
68% |
61% |
||||
|
PASP, mmHg |
0.66 |
0.55-0.78 |
18.78 |
55% |
81% |
||||
|
AT, msec |
0.65 |
0.54-0.76 |
145 |
50% |
75% |
||||
Table 3: Receiver operating characteristic curve analysis using RV echocardiographic parameters at rest to identify subjects with an stress RV E/e’>6
Abbreviations: RVDD – right ventricular diastolic dysfunction; RAVI – right atrium volume index; RVWT – right ventricle wall thickness; AT – acceleration time; PASP –pilmonary arterial systolic pressure; TAPSE – tricuspidal annular plane systolic excursion.
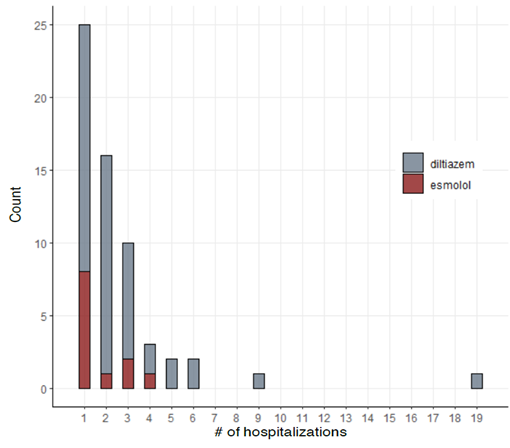
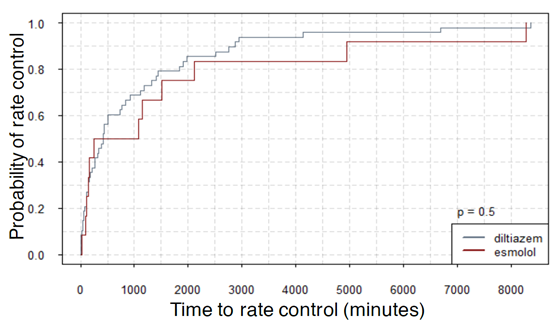
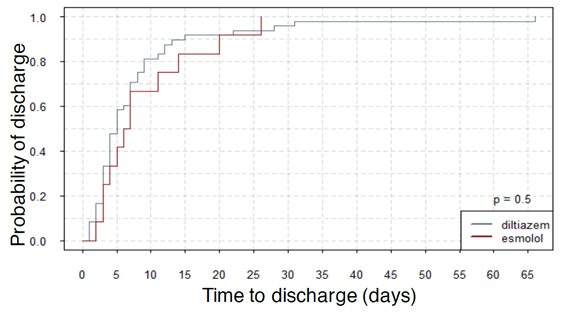
RAVI and RVWT seem to be the parameters that have the best sensitivity and specificity. A cut- off value of 20.55 ml/m2 for RAVI may discriminate the patients with stress RVDD with a sensitivity of 86.36% and specificity 86.11%; E/A ratio at rest (cut-off 1.05) discriminates stress RVDD patients with sensitivity 79.7%; specificity 90.5%. RVWT of 5.25 mm is discriminative with a sensitivity 100% and specificity 63%. ROC curves are presented in Figure1, Figure 2 and Figure 3.
To assesss the association between LV structural (septum and posterior wall thickness) and functional parameters (LV E/A, LV E/e’ at rest; LV E/A, LV E/e’ after stress) and stress induced RVDD, univariate regression analysis was performed (table 4).
|
Univariable regression analysis |
p-value |
OR |
95% CI |
|
Ventilatory parameters |
|||
|
FEV1, l |
0.78 |
2.01 |
0.86-3.87 |
|
ICdyn, l |
0.04 |
5.29 |
2.68-9.18 |
|
LV parameters |
|||
|
Septum, mm |
0.67 |
1.98 |
1.62-2.86 |
|
LVPWT, mm |
0.81 |
2.17 |
1.93-4.49 |
|
E/A ratio at rest |
0.94 |
0.99 |
0.80-1.23 |
|
E/e’ ratio at rest |
0.99 |
1.89 |
1.59-1.99 |
|
E/A ratio after stress |
0.04 |
1.54 |
1.00-2.35 |
|
E/e’ ratio after stress |
0.00 |
4.07 |
1.75-12.47 |
|
RV parameters |
|||
|
RV basilar diameter, mm |
0.00 |
1.48 |
1.23-1.78 |
|
RVmedian diameter, mm |
0.00 |
1.83 |
1.38-2.48 |
|
RVWT, mm |
0.74 |
0.98 |
0.78-1.02 |
|
RAVI, ml/m2 |
0.00 |
3.82 |
2.04-7.14 |
|
E/A ratio at rest |
0.00 |
19.73 |
18.52-21.01 |
|
E/e’ ratio > 5.1 at rest |
0.03 |
4.79 |
1.73-13.24 |
|
TAPSE, mm |
0.37 |
21.56 |
1.20-38.91 |
|
S peak velocity, m/s |
0.33 |
0.73 |
0.55-0.97 |
|
PASP, mmHg |
0.12 |
0.70 |
0.07-75.08 |
|
AT, msec |
0.49 |
2.39 |
0.20-28.67 |
|
Biomarkers |
|||
|
Resistin, ng/ml |
0.02 |
0.81 |
0.51-1.31 |
|
PG E2 , µmol/l/cre |
0.04 |
0.70 |
0.34-1.07 |
|
Multivariable regression analysis |
|||
|
E/e’ ratio > 5.1 at rest |
0.02 |
9.03 |
1.32-63.73 |
|
RAVI, ml/m2 |
0.00 |
2.27 |
1.40-3.68 |
Table 4: Logistic regression analysis between ventilatory and echocardiographic parameters and stress RV E/e’
Abbreviations: FEV1 – Forced Expiratory Volume in 1 sec; ICdyn – dynamic hyperinflatio; RVDD – right ventricular diastolic dysfunction; LV left ventricle; RV – right ventricle; LVPWT – left ventricular posterior wall thickness; RVWT – right ventricular wall thickness; RAVI – right atrium volume index; AT – acceleration time; PASP –pulmonary arterial systolic pressure; AT – acceleration time; TAPSE – tricuspidal annular plane systolic excursion; PG E2 – prostaglandine E2.
This was also performed with the RV structural parameters and their selected cut-off values. From all the variables only the cut-off value of rest RV E/e’>5.1 is statistically significant and clinically applicable with the odd ratio for stress-RVDD – 4.79; (95% CI - 1.73-13.24). If we apply univariate regression analysis with the echocardiographic measurements as quantitative parameters the RV basilar and median diameter, RAVI, rest RV E/e’ ratio, stress LV E/A, stress LV E/e’, may be used as predictors (table 4). The RV E/A ratio showed the highest odds ratio 19.73; (95% CI – 18.52-21.01); followed by RAVI - odds ratio 3.82; (95% CI–2.04-7.14). In multivariate regression analysis with a forward step approach RAVI and rest RV E/e’>5.1 remained independent predictors for stress-RVDD. The combination of these two variables predicts stress-RVDD with the accuracy of 92%. This association was independent of LV diastolic dysfunction (LV E/A at rest; LV E/e’ at rest; stress LV E/A; stress LV E/e’), lung function (FEV1), ICdyn, age, sex, and BMI, taken as covariates.
Discussion
The major findings of our study are: 1) 78% of the patients with non-severe COPD have stress induced RVDD, while only 14% show RVDD at rest; 2) The cut-off values RAVI, RVWT and RV E/A ratio at rest have good sensitivity and specificity for stress RV E/e’> 6; 3) RAVI, RV E/A and RV E/e’>5.1 are independent predictors of stress RVDD in multivariate regression analysis; 4) prostaglandine E2 and resistin correlate to RV E/e’>6, but none of them is an independent predictor for it.
Cor pulmonale is classically assumed as the major cardio-vascular manifestation of COPD but subclinical RV abnormalities may be found even in mild form of the disease [24,25]. MRI shows that invasive pulmonary arterial pressure (PAP) measurement delays the diagnosis of lung vascular pathology in the general population and in COPD patients [8,9,26,27].
We support this notion, showing that exercise exertion in non-severe COPD patients facilitates the detection of right ventricular-arterial decoupling. According to our knowledge this is the first study in non-severe COPD patients without pulmonary arterial hypertension at rest that evaluates the functional state of the RV under stress conditions. Although only a small proportion of patients have RVDD (14%) at rest, after symptom limited incremental stress protocol 78% show signs of RVDD. Both functional (RV E/e’ and RV E/A) and structural parameters (RAVI, RVWT, RV basilar and median diameter) may serve as echocardiographic predictors for stress RVDD in non-severe COPD without PAH at rest. These echocardiographic parameters correlate to stress RV E/e’ ratio in univariate regression analysis.
We confirm the concept of “cor pulmonale parvus’’ [28-31]. Our COPD patients have small RV dimensions, RV hypertrophy and RVDD at rest. RVDD is an early sign of pulmonary vasculopathy and precedes the clinical/echocardiographic manifestation of pulmonary hypertension [27,32]. Non-severe COPD patients with normal PAP at rest probably experience excessive haemodynamic PAP changes during exertion They may gradually result in RV structural changes, that may precede the clinical manifestation of RV dysfunction, and may, thus, be more sensitive for exercise induced pulmonary haemodynamic abnormalities. Physical exertion, however, undoubtedly facilitates the dynamic assessment of diastoling filling pressures. These may be normal at rest, but often augment abnormally during exercise [27,32]. Thus, stress RVDD detection may help the diagnosis of a specific COPD phenotype which is associated with reduced exercise capacity.
In addition to intrathoracic and haemodynamic pressure oscillations during physical exertion, oxidative stress and inflammation have been assumed as leading factors for both right and left ventricular diastolic remodeling [33-35]. Despite this, according to our results none of the inflammatory and oxidative stress markers is an independent predictor for it.
Systemic inflammation in COPD leads to elevated IL-6, TNF-α, hsCRP levels, which increase E-selectin, VCAM, endothelial reactive oxygen species and attenuate nitric oxide availability in the coronary microvasculature [36]. These biochemical reactions stimulate collagen deposition and myocardial stiffness [36].
Indeed, in our study resistin plasma levels correlated to stress RV E/e’>6. Resistin has been associated with vascular damage and increased cardiovascular morbidity [37-40]. It is implicated in the development of insulin resistance, hypertension and left diastolic dysfunction in the general population of patients. Several small studies have reported that circulating resistin levels are increased in human obesity and diabetes, although not all studies have been consistent [39,40]. Resistin and rodent resistin-like molecules (RELM) α are mechanistically critical to pulmonary hypertension (PH) etiology in lungs. However, it is still unclear whether these molecules are activated in cardiac myocytes and whether they can directly induce the PH-associated cardiac dysfunction and remodeling. Lin et al, prove that Resistin/RELMα are the pathogenic driver in the development of right cardiac dysfunction and maladaptive RV remodeling [41]. This confirms the findings that targeting resistin signaling modulates cardiac inflammation and metabolism. It constitutes a therapeutic target for PH. Resistin blockade with human therapeutic antibodies efficaciously prevented and reversed the proliferative pulmonary vascular remodeling, maladaptive RV remodeling and impaired RV function in an experimental PH. Lin et al, successfully established that the anti-hResistin neutralizing antibodies are novel therapy for PAH and the associated RV failure in an animal model [42]. Our findings also support the current notion. Although plasma resistin levels are not independently associated with stress RVDD, they correlate to stress RV E/e’ ratio.
The other inflammatory marker that significantly differed between both groups was prostaglandin E2. In contrast to resistin, it has been described as beneficial in cardiac remodeling after ischaemic injury [43,44]. Our data supports this notion. Urine levels of prostaglandin E2 are higher in the group without stress RVDD. Urine levels of prostaglandin E2 did not show good sensitivity and specificity to distinguish the two patients with stress RVDD from those without. Our results, regarding urine prostaglandin E2 and plasma resistin levels should be validated in larger cohorts and their pathogenetic mechanisms should be further explored.
In addition to systemic inflammation, oxidative stress in COPD may also disturb calcium transport and myocardial relaxation [45]. Reactive oxidative species (ROS) are generated under inflammatory or hypoxic conditions. They stimulate endothelin secretion and decrease NO/prostacyclin synthesis [46]. The endothelial damage, caused by oxidative stress, affects both coronary, systemic and pulmonary vessels and exerts multifaced mechanisms, that contribute both to right (RVDD) and left ventricular diastolic dysfunction (LVDD) [47]. Though we applied a well-validated method and marker for oxidative stress – urine 8-isoprostanes, we did not detect substantial difference in its concentrations between COPD subjects with/without RVDD. Neither a correlation between urine 8-isoprostanes and stress RV E/e’ was found.
Study Limitations
The main limitations of this study are: 1) the relatively small sample size; 2) COPD patients experience enhanced pressure swings during the respiratory cycle and measurements were performed at the end of expiration, which may influence the results; 3) we do not have invasive measurement of sPAP; 4) measurements were acquired in the early recovery period (approximately 2 min) after symptom-limited exercise. The timeline of changes of the pulmonary and intrathoracic pressures during the brief time interval from peak exercise to their measurement in early recovery is not well known and underestimation is possible.
Conclusion
There is a high prevalence of stress induced RVDD in non-severe COPD patients with exertional dyspnea, free of overt cardiovascular disease. Patients with stress RVDD demonstrate similar levels of oxidative stress. Prostaglandine E2 may have protective role in RV remodeling, while resistin plasma levels contribute to RVDD pathogenesis. None of these biomarkers may be applied as a predictor for stress RVDD in clinical practice. In contrast, the echocardiographic parameters - RAVI, RVWT, RV E/A and RV E/e’ ratio at rest independently predict stress RVDD.
Acknowledgements
We give our acknowledgements to professor Vukov, who performed the statistical analysis.
Ethical Statement
Ethics approval for the study protocol was received from the Ethics Committee of the Medical University, Sofia protocol 5/12.03.2018. There were no external funding sources for this study.
Disclosure
All the authors state no conflict of interests and leave the copyright of the article if accepted.
References
- Trinkmann F, Saur J, Borggrefe M, et al. Cardiovascular Comorbidities in Chronic Obstructive Pulmonary Disease (COPD)—current considerations for clinical practice. Journal of Clinical Medicine 8 (2019): 69.
- Ukena C, Mahfoud F, Kindermann M, et al. The cardiopulmonary continuum systemic inflammation as ‘common soil’of heart and lung disease. International Journal of Cardiology 145 (2010): 172-176.
- Grau M, Barr RG, Lima JA, et al. Percent emphysema and right ventricular structure and function: the multi-ethnic study of atherosclerosis-lung and multi-ethnic study of atherosclerosis-right ventricle studies. Chest 144 (2013): 136-144.
- Kawut SM, Poor HD, Parikh MA, et al. Cor pulmonale parvus in chronic obstructive pulmonary disease and emphysema: the MESA COPD study. Journal of the American College of Cardiology 64 (2014): 2000-2009.
- Barr RG, Bluemke DA, Ahmed FS, et al. Percent emphysema, airflow obstruction, and impaired left ventricular filling. New England Journal of Medicine 362 (2010): 217-227.
- Kubota Y, Asai K, Murai K, et al. COPD advances in left ventricular diastolic dysfunction. International Journal of Chronic Obstructive Pulmonary Disease 11 (2016): 649.
- Gan CT, Holverda S, Marcus JT, et al. Right ventricular diastolic dysfunction and the acute effects of sildenafil in pulmonary hypertension patients. Chest 132 (2007): 11-17.
- Stevens GR, Garcia-Alvarez A, Sahni S, et al. RV dysfunction in pulmonary hypertension is independently related to pulmonary artery stiffness. JACC: Cardiovascular Imaging 5 (2012): 378-387.
- Sanz J, Kariisa M, Dellegrottaglie S, et al. Evaluation of pulmonary artery stiffness in pulmonary hypertension with cardiac magnetic resonance. JACC: Cardiovascular Imaging 2 (2009): 286-295.
- Mitzner W. Emphysema: a disease of small airways or lung parenchyma?. The New England Journal of Medicine 365 (2011): 1637.
- Aaron CP, Hoffman EA, Lima JA, et al. Pulmonary vascular volume, impaired left ventricular filling and dyspnea: the MESA Lung Study. PloS One 12 (2017): e0176180.
- Miller MR, Hankinson JA, Brusasco V, et al. Standardisation of spirometry. European Respiratory Journal 26 (2005): 319-338.
- O'donnell DE, Lam MI, Webb KA. Measurement of symptoms, lung hyperinflation, and endurance during exercise in chronic obstructive pulmonary disease. American Journal of Respiratory and Critical Care Medicine 158 (1998): 1557-1565.
- O'donnell DE, Revill SM, Webb KA. Dynamic hyperinflation and exercise intolerance in chronic obstructive pulmonary disease. American Journal of Respiratory and Critical Care Medicine 164 (2001): 770-777.
- Stubbing DG, Pengelly LD, Morse JL, et al. Pulmonary mechanics during exercise in normal males. Journal of Applied Physiology 49 (1980): 506-510.
- Yan S, Kaminski D, Sliwinski P. Reliability of inspiratory capacity for estimating end-expiratory lung volume changes during exercise in patients with chronic obstructive pulmonary disease. American Journal of Respiratory and Critical Care Medicine 156 (1997): 55-59.
- Guazzi M, Arena R, Halle M, et al. EACPR/AHA Scientific Statement. 2016 Focused update: clinical recommendations for cardiopulmonary exercise testing data assessment in specific patient populations. Circulation 133 (2016): e694-e711.
- American Thoracic Society; American College of Chest Physicians. ATS/ACCP Statement on cardiopulmonary exercise testing. Am J Respir Crit Care Med. 167 (2003): 211–277.
- Arena R, Myers J, Guazzi M. The clinical and research applications of aerobic capacity and ventilatory efficiency in heart failure: an evidence-based review. Heart Failure Reviews 13 (2008): 245-269.
- Nagueh SF, Smiseth OA, Appleton CP, et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. European Journal of Echocardiography 17 (2016): 1321-1360.
- Lancellotti P, Moura L, Pierard LA, et al. European Association of Echocardiography recommendations for the assessment of valvular regurgitation. Part 2: mitral and tricuspid regurgitation (native valve disease). European Journal of Echocardiography 11 (2010): 307-332.
- Rudski LG, Lai WW, Afilalo J, et al. Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography: endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. Journal of the American Society of Echocardiography 23 (2010): 685-713.
- Galiè N, Humbert M, Vachiery JL, et al. 2015 ESC/ERS guidelines for the diagnosis and treatment of pulmonary hypertension: the Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). European Heart Journal 37 (2016): 67-119.
- Gökdeniz T, Kalayc?o?lu E, Boyac? F, Ayket al. The BODE index, a multidimensional grading system, reflects impairment of right ventricle functions in patients with chronic obstructive pulmonary disease: a speckle-tracking study. Respiration 88 (2014): 223-233.
- Schoos MM, Dalsgaard M, Kjærgaard J, et al. Echocardiographic predictors of exercise capacity and mortality in chronic obstructive pulmonary disease. BMC Cardiovascular Disorders 13 (2013): 84.
- Ben-Yehuda O, Barnett C. Magnetic Resonance Assessment of Pulmonary Artery Compliance. JACC: Cardiovascular Imaging 3 (2009): 296-298.
- Hilde JM, Skjørten I, Hansteen V, et al. Haemodynamic responses to exercise in patients with COPD. European Respiratory Journal 41 (2013): 1031-1041.
- Ford ES, Murphy LB, Khavjou O, et al. Total and state-specific medical and absenteeism costs of COPD among adults aged 18 years in the United States for 2010 and projections through 2020. Chest 147 (2015): 31-45.
- Waschki B, Kirsten A, Holz O, et al. Physical activity is the strongest predictor of all-cause mortality in patients with COPD: a prospective cohort study. Chest 140 (2011): 331-342.
- Guenette JA, Jensen D, Webb KA, et al. Sex differences in exertional dyspnea in patients with mild COPD: physiological mechanisms. Respiratory Physiology & Neurobiology 177 (2011): 218-227.
- Ofir D, Laveneziana P, Webb KA, et al. Mechanisms of dyspnea during cycle exercise in symptomatic patients with GOLD stage I chronic obstructive pulmonary disease. American Journal of Respiratory and Critical Care Medicine 177 (2008): 622-629.
- Hilde JM, Skjørten I, Grøtta OJ, et al. Right ventricular dysfunction and remodeling in chronic obstructive pulmonary disease without pulmonary hypertension. Journal of the American College of Cardiology 62 (2013): 1103-1111.
- Alter P, van de Sand K, Nell C, et al. Airflow limitation in COPD is associated with increased left ventricular wall stress in coincident heart failure. Respiratory Medicine 109 (2015): 1131-1137.
- Funk GC, Lang I, Schenk P, et al. Left ventricular diastolic dysfunction in patients with COPD in the presence and absence of elevated pulmonary arterial pressure. Chest 133 (2008): 1354-1359.
- Maclay JD, McAllister DA, Johnston S, et al. Increased platelet activation in patients with stable and acute exacerbation of COPD. Thorax 66 (2011): 769-774.
- Paulus WJ, Tschöpe C. A novel paradigm for heart failure with preserved ejection fraction: comorbidities drive myocardial dysfunction and remodeling through coronary microvascular endothelial inflammation. Journal of the American College of Cardiology 62 (2013): 263-271.
- Banerjee RR, Rangwala SM, Shapiro JS, et al. Regulation of fasted blood glucose by resistin. Science 303 (2004): 1195-1198.
- Furuhashi M, Ura N, Higashiura K, et al. Circulating resistin levels in essential hypertension. Clinical Endocrinology 59 (2003): 507-510.
- Papadopoulos DP, Makris TK, Krespi PG, et al. Adiponectin and resistin plasma levels in healthy individuals with prehypertension. The Journal of Clinical Hypertension 7 (2005): 729-733.
- Papadopoulos DP, Perrea D, Thomopoulos C, et al. Masked hypertension and atherogenesis: the impact on adiponectin and resistin plasma levels. The Journal of Clinical Hypertension 11 (2009): 61-65.
- Lin Q, Fan C, Skinner J, et al. Therapeutic Effects of the Generated Antibodies Targeting Human Resistin in Pulmonary Hypertension. InD96. Cracking The Cellular Code In Pulmonary Hypertension (2018): pp. A7398-A7398.
- Lin Q, Skinner J, Yang W, et al. Human Resistin Signaling Induces Cardiac Dysfunction in Pulmonary Hypertension. InC105. With All My Heart: Sex, Estrogen, And Right Ventricle In Pulmonary Vascular Disease And Beyond (2020): pp. A6077.
- Degousee N, Fazel S, Angoulvant D, et al: Microsomal prostaglandin E2 synthase-1 deletion leads to adverse left ventricular remodeling after myocardial infarction. Circulation 117 (2008): 1701-1710.
- Gould KE, Taffet GE, Michael LH, et al. Heart failure and greater infarct expansion in middle-aged mice: a relevant model for postinfarction failure. American Journal of Physiology-Heart and Circulatory Physiology 282 (2002): H615-H621.
- Cargill RI, Kiely DG, Lipworth BJ. Adverse effects of hypoxaemia on diastolic filling in humans. Clinical Science 89 (1995): 165-169.
- Paulus WJ, Tschöpe C. A novel paradigm for heart failure with preserved ejection fraction: comorbidities drive myocardial dysfunction and remodeling through coronary microvascular endothelial inflammation. Journal of the American College of Cardiology 62 (2013): 263-271.
- Barbera JA, Peinado VI, Santos S. Pulmonary hypertension in chronic obstructive pulmonary disease. European Respiratory Journal 21 (2003): 892-905.


 Impact Factor: * 3.5
Impact Factor: * 3.5 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 14.80%
Acceptance Rate: 14.80%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 