Bilateral Xanthogranulomatous Pyelonephritis due to Staphylococcus Schleiferi: An Uncommon Presentation
Leonardo Rene Aguilar-Rivera¹, Raúl Alberto Jiménez-Castillo¹, Miguel Ángel Zamora-López¹, Itzel Aracely Ortiz Meza², Ulises Longoria-Estrada³, Emma Purón González4, Lilia Rizo-Topete1,5 *
1Internal Medicine Department, Hospital Universitario, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León, México. Reumathology service, Hospital Civil de Guadalajara, Mexico
2Pathology Department, Hospital Universitario, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León, México. Reumathology service, Hospital Civil de Guadalajara, Mexico
3Radiology Department, Hospital Universitario, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León, México. Reumathology service, Hospital Civil de Guadalajara, Mexico
4Fray Antonio Alcalde, Hospital Universitario, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León, México. Reumathology service, Hospital Civil de Guadalajara, Mexico
5Nephrology Service, Hospital Universitario, Universidad Autónoma de Nuevo León, Monterrey, Nuevo León, México. Reumathology service, Hospital Civil de Guadalajara, Mexico
*Corresponding Author: Lilia María Rizo Topete MD, Profesor del Departamento de Medicina Interna y Servicio de Nefrología Facultad de Medicina y Hospital Universitario “Dr. José Eleuterio Gonzalez”, Universidad Autónoma de Nuevo León Av. Francisco I. Madero y Av. Gonzalitos s/n, Colonia Mitras Centro. Monterrey, N.L. México C.P. 64460, Tel. +52 8180297718
Received: 02 August 2021; Accepted: 09 August 2021; Published: 19 August 2021
Article Information
Citation: Leonardo Rene Aguilar-Rivera, Raúl Alberto Jiménez-Castillo, Miguel Ãngel Zamora-López, Itzel Aracely Ortiz Meza, Ulises Longoria-Estrada, Emma Purón González, Lilia Rizo-Topete. Bilateral Xanthogranulomatous Pyelonephritis due to Staphylococcus Schleiferi: An Uncommon Presentation. Archives of Nephrology and Urology 4 (2021): 115-123.
DOI: 10.26502/anu.2644-2833042
View / Download Pdf Share at FacebookAbstract
Xanthogranulomatous pyelonephritis (XGP) describes a rare infectious disease with a destructive granulomatous process. The literature contains few cases of bilateral XGP and no cases due to Staphylococcus schleiferi; we diagnosed it with the advance at imaging and bacterial identification systems technology. This is a case of a 22-year-old female at our emergency department complaining of abdominal pain, nausea, emesis, dyspnea of 3 weeks. Medical history included Chronic Kidney Disease (CKD) treated with Peritoneal dialysis and history of recurrent urinary tract infection. On examination, we found signs of septic shock and suprapubic tenderness. No flank or renal mass found on examination. Tomography (CT) scan showed bilateral kidney enlargement with pyelocaliceal dilatation due to stones obstructing ureteral union; presence of gas on left kidney´s renal pelvis and an abscess in the posterior pararenal space. We diagnosed Bilateral XGP and emphysematous pyelitis, initiated board-spectrum antibiotic and perform urgent right nephrostomy and left nephrectomy. The urinary, blood and renal tissue culture identified pathogenic agents (Escherichia coli and Staphylococcus schleiferi) and antibiotic treatment was de-escalated. After two weeks of treatment, she recovered of an acute on chronic renal failure (ACRF) remaining with 24ml/min/1.73m2 of GFR (stage IV of CKD) and was discharged from hospital.
Keywords
<p>Xanthogranulomatous Pyelonephritis; Emphysematous pyelitis; Staphylococcus schleiferi</p>
Article Details
1. Introduction
Xanthogranulomatous pyelonephritis is a chronic pyogenic infection of renal parenchyma resulting in its destruction and replacement with a mixed inflammatory infiltrate. It represents less than 1% of chronic renal infections - accounting for 6/1000 surgically proven cases of chronic pyelonephritis- and befalls all ages. In the adult population, women are more affected than men (1:2.5-4) and it is associated with diabetes and immunosuppression [1-4].
Several challenges exist in its diagnosis and treatment which have been difficult to overcome. The clinician must distinguish this disease from other entities to define the appropriate surgical management [1-3, 5]. As well, in 40% of the cases, the pathogenic agent remains unknown making it difficult to narrow the antibiotic coverage [1, 2, 6]. XGP usually affects one kidney but a few (sixteen) case reports have described patients with bilateral XGP, making a therapeutic challenge [7]; the decision between conservative, partial or complete nephrectomy and antibiotic therapy is based on case individualization by the clinicians. Finally, it is an insidious disease that can lead to end-stage renal disease and its mortality rate exceeds 40% [8]. We present the case of a patient with bilateral XGP in whom a rare etiologic agent was isolated from renal tissue culture through matrix-assisted laser desorption ionization-time of flight (MALDI-TOF).
2. Case Report
A 22-year-old female at our emergency department; referred progressive pain in the left iliac fossa and hypogastrium moderate intensity, anemic syndrome, nausea, emesis, dyspnea for the last 3 weeks; associated with weight loss (15 kg) over 1 year. She denied pneumaturia, genitourinary symptoms, and hematuria. Medical history included Chronic Kidney Disease (CKD) with hemodialysis four sessions/week for 9 months and change to peritoneal dialysis 3 months after delivery, nonadherence since then; transfusion 4 years ago for anemia; recurrent urinary tract infection. She denied other medical comorbidities or surgical history.
On examination she was tachycardic 115 beats/min, blood pressure 60/40 mmHg, tachypneic 27 breath/min, temperature was 37.8 °C, 45 Kg, 1.55 meters; pale, moderate to severe suprapubic tenderness without rebound, without costovertebral angle tenderness. Her complete blood count included a hemoglobin concentration of 2.11 g/dl, a leucocytosis of 51.4x109 /L and neutrophil count of 46.6x109 /L; a platelet count of 523.0x109 /L, albumin 1.4 g/dL, AST 26 UI/L, ALT 17 UI/L, TB 0.5 mg/dL. Urine analysis: density 1.012, pH 8, proteins 100 mg/dL, leukocyte esterase 500 leucocytes/uL, erythrocytes 10/field, leucocytes 100/field, observations: abundant bacteria, negative urinary culture. An abdominal Computer Tomography (CT) with contrast demonstrated the presence of gas on the renal pelvis and the destruction granulomatous process of parenchyma thus suggesting bilateral XGP and emphysematous pyelitis. (Figure 1)
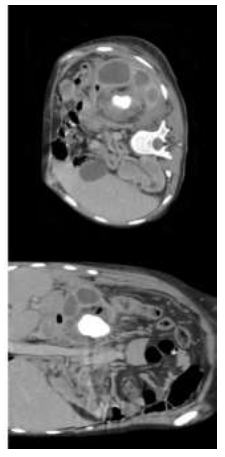
Figure 1: Contrast CT scan.
Bilateral XGP and retroperitoneal abscess: bilateral kidney enlargement with pyelocaliceal dilatation due to stones obstructing ureteral union, thinning of its cortex, perfusion defects, enhancement of urothelium, scar areas and heterogeneity in its density.
Right kidney: sagittal axis 12.1 cm, coronal axis 5.8 cm. Left kidney: sagittal axis 12.5 cm, coronal axis 7.3 cm, a coralliform stone, presence of gas on left kidney´s renal pelvis. Abscess: Irregular collection at posterior pararenal space including psoas and iliac muscles.
The patient was treated with IV crystalloids, red blood cell transfusion, and broad-spectrum antibiotics. Urgent right nephrostomy and left nephrectomy were performed sending tissue for culture and the left kidney to pathology evaluation. Renal tissue culture isolated Escherichia coli sensible to ampicillin and gentamicin; and Staphylococcus schleiferi sensible to clindamycin and erythromycin. Results from histopathology corroborated the diagnosis (Figure 2) and two weeks later she recovered from an acute on chronic renal failure, she was discharged from the hospital with 24ml/min/1.73m2. of GFR (stage IV of CKD).
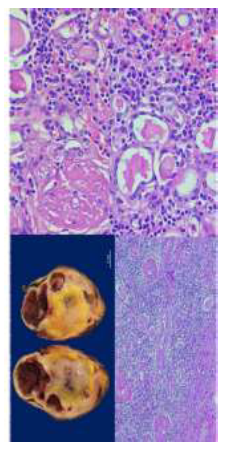
Figure 2: Anatomopathological kidney.
Macroscopic: Solid cystic cut surface with a reddish parenchyma with a hemorrhagic appearance and yellowish nodules. In addition to 3 pelvic calculi. Microscopic: Inflammatory infiltrate characterized by inconspicous netrophiles, linfocytes, plasmatic cells and abundanted foamy macrophages.
3. Discussion
XGP represents a diagnostic and a treatment challenge, especially in bilateral affectation. Earlier diagnosis and treatment improves prognosis in order to preserve kidney function. XGP portrays a vague clinical picture, which manifests unilateral in 92% of the cases -left kidney (70%), right kidney (30%)-or bilateral (8%) [2-4, 8-10]. XGP infiltrates tissue in two ways: focal (8-16%) or diffuse (84-92%) [1-3, 8-10]. Focal lesions mimic renal tumors (Wilms, renal carcinoma, malakoplakia) or infections (renal abscess, renal tuberculosis, infects renal cystic disease); the diffuse lesions can involve adjacent organs (solid organs, bowels, great vessels) [2, 9].
3.1 Pathogenesis
Previous researches imply a multifactorial process: Urinary tract obstruction with or without calculi (Clinic entities as ureteropelvic junction syndrome, ureteropelvic duplication, and chronic interstitial nephritis); renal ischemia, lymphatic obstruction, venous occlusion and hemorrhage; abnormalities in the lipids metabolism, abnormal immune response (pregnancy, diabetes mellitus, rheumatoid arthritis); ineffective treatment of urosepsis, recurrent urinary tract infection (a subacute inflammatory reaction) and destructive infections and collection of foamy cells- that leads from acute kidney injury to renal failure or azotemia (rare because of the compensatory function of the opposite kidney) [1-3, 6, 9, 11].
3.2 Etiology
Proteus spp. and E. coli cause 60% of infections; 40% of the cases remain unknown. In the minority of cases Staphylococcus aureus, group B Streptococcus, Candida, Klebsiella, and Bacteroides appear in cultures [1, 2, 6]. Staphylococcus schleiferi is known to cause skin and soft tissue infection, device infection, meningitis, brain empyema, osteomyelitis, and bacteremia but not reported so far as a cause of pyelonephritis [12, 13]. S. schleiferi as an uro-pathogen represents the 0.7% of urinary tract infection -none of them were pyelonephritis [14]. This is the first case description of Staphylococcus schleiferi pyelonephritis infection in a human patient. Any isolates of this bacterium in human beings should be presumed to be pathogenic unless proven otherwise.
3.3 Diagnostic
XGP is a difficult entity because only 16.7-46.2% is diagnosed preoperatively [1-3, 5]. The presentation may vary depending on age: The pediatric population clinically complains about systemic illness symptoms (62%), abdominal pain (60%), pyrexia (53%), and urinary tract infection (53%) [4]; whereas adults manifest as fever and flank pain, presentation respects laterality and affects also predominantly one kidney.
In a adults the sintomatology could be different and confuse, sometimes asintomatyc laboratory test shows ESR>30 (57-87%), pyuria (63-87%), anemia (41-86%), thrombocytosis (80%), and leukocytosis (41-71%); urine culture isolates micro-organisms in 56 to 70% of samples [2, 3, 8, 9, 10] and has an 83% concordance between positive urines and intraoperative cultures; Imaging helps establish a correct diagnosis, define extrarenal extension, and facilitate planning surgical management [15]. Some features suggest XGP such as: Hydronephrosis (90.9%), renal calculus (72%), pyonephrosis (45.5%), cortical renal atrophy (45.5%), intraparenchymatous collection (45.5%), abscess (36.4%) and perinephric fat accumulation (18.2%) [2].
Ultrasonography is unable to distinguish between focal and diffuse variants and sonographic findings are unspecific to XGP; it also detects 73-83% of significant renal abnormalities requiring urologic treatment. The classical triad of XGP is unilateral renal enlargement, no or little function, and large stone (usually staghorn) in the renal pelvis [2, 6, 8-10]. Focal XGP is impossible to differentiate from a renal abscess or necrotic renal cell carcinoma (RCC) [2] .
CT is ideal for presurgical evaluation of the extension, complications (abscess and fistula), and diffuse disease. CT shows poor or no excretion of contrast into the collecting system, and multiple focal low-attenuation (-10 to +30 HU) which are xanthoma collections and dilated calyces; bright enhancement of the rims of the collections due to inflammatory hypervascularity; calculi, hydronephrosis, kidney enlargement, with parenchyma destruction, administration of contrast enhancement a ring around the granulation tissue. Classic CT is the “bear paw sing” [1, 8, 16].
In magnetic resonance imaging, T1-weighted MRI shows a hyperintense appearance of included cavitary borders, with hypointense cavitary fluid and perirenal strands. T2-weighted images are isointense in cavitary borders with hyperintensity in cavitary fluid and hypointensity in perirenal strands depending on the number of foamy macrophages [2, 16].
A definitive diagnosis is based on the histopathologic analysis of the kidney [4]. Macroscopically, we can find enlarged kidneys with hydronephrosis, pelvic calculi or equivalent obstruction; single or multiple yellow to orange nodules; central necrosis with abscess formation, the involvement of perinephric fat, diffuse cortical scarring with effacement of the normal renal architecture, and cortical atrophy. In severe cases, gross destruction extends into the perinephric tissues and adrenal glands [2]. Microscopically, the examination shows granulomatous mixed inflammatory infiltrates (xanthomatous histiocytes with foamy cytoplasm, neutrophils, lymphocytes, plasma cells, and multinucleated giant cells) with fibrosis and cholesterol clefts in renal parenchyma and perirenal soft tissue in severe cases. Tubulopathy among renal tubular atrophy, tubular dilatation, and focal squamous metaplasia of the urothelium, microabscesses, lymphoid aggregates with germinal center formation, and spindle cell proliferation [2]. Cytokeratin, epithelial membrane antigen, and CD68 immunohistochemistries can help in the differential diagnosis. Xanthomatous cells and macrophages stains positive for a1-antitrypsin, CD68, lysozyme and vimentin; and negative for smooth muscle actin, desmin, and epithelial markers. Renal cell carcinoma is usually positive for CD10 and epithelial membrane antigen; vimentin can stain positive for both [2].
During the diagnostic approach two benign closely related entities must be considered: malakoplakia and megalocytic interstitial nephritis. The hallmark of both lesions is the periodic acid–Schiff diastase-positive material in the cytoplasm of the histiocytes; XGP is characterized by periodic acid-schiff stain negative [2, 6].
3.4 Treatment
Chronic complicated infections require prompt decompression; 12% of cases of presumed to be simple pyelonephritis require emergent urologic intervention [8]. Conservative management with antibiotics fails to treat the underlying process [9]. Antibiotics must be initiate before surgical to control the infectious process and avoid sepsis complications, -which occur in >50% of patients- and continues for 1 to 2 weeks postoperatively [1, 5, 8, 17].
The treatment method depends on the infiltration lesions. In the case of a diffuse form or difficult differentiation from malignant renal mass, the treatment is to remove all the inflammatory mass including nephrectomy. In focal lesions further renal parenchymal destruction can be prevented by partial nephrectomy [3].
Gold-standard therapy is complete nephrectomy, especially when patients present severe lumbar pain, recurrent urinary tract infections, or renovascular hypertension, like in our case. Partial nephrectomy can be successfully performed as intermediate steps in treatment [1, 18]. Nephrostomy before nephrectomy facilitates surgery, obtaining of cultures and the access to de the kidney at the time of surgery [1]. The laparoscopic technique has a 16% conversion to open technique because of vascular and adjacent organ injuries [18] Successful reports cases from conservative treatment (bilateral cases, focal lesion, or high-risk surgery) describe 2 months of antibiotic schemes with follow-up ultrasonography [3, 8, 10, 17].
3.5 Prognosis
Mortality and morbidity rate exceeds 40% and 23-33% in undecompressed cases, respectively. Among the complications described in the literature stands out contralateral kidney hypertrophy 75%, abscess formation 18% (psoas abscess and paranephric abscess), renal failure 3% (amyloid in the long term) and fistula (nephrocutaneous or nephrocolonic). Other complications described are emphysematous pyelonephritis and ischemic colitis involving transverse and descending colon by compression of a large mass. In the long term, it increases the risk of urinary tract infections, hypertension and it is associated with transitional cell carcinoma of the renal pelvis and Renal cell carcinoma [2, 4, 8, 9].
The absence of guidelines leads to a lack of optimal antimicrobial selection, duration, and timing of surgery. Analysis of literature led us to a successful result and this builds evidence supporting clinical indications for conservative treatment with bilateral XGP.
There are several limitations inherent to this report. We ignore the source of bacterial infection and histology confirmation of XGP in the contralateral kidney. However, we confirmed the diagnosis and demonstrated the benefits of multidisciplinary care and clinical research teams. The complexity of this case makes it unique, and as far as we know it is the first case of a Staphylococcus schleiferi pyelonephritis infection in a human patient. Also, it´s one successful conservative treatment in a bilateral XGP.
4. Conclusion
In conclusion, XGP is a significant cause of morbidity and mortality for the patients affected. Although unilateral affection is the most common way of XGP, bilateral affection is out of any guideline of treatment. The preferred management if total nephrectomy, although it represents great morbidity for the patient. The report emphasizes the importance of diagnosis and analyzes an individualized treatment. Future studies and analysis of cases are indicated to direct an evidence-base guideline for XGP.
Declaration of Interest
None.
Funding Source
None.
References
- Ramos LD, de Moraes Lima M, de Carvalho M, et al. Emphysematous and xanthogranulomatous pyelonephritis: Rare diagnosis. Brazilian J Infect Dis 14 (2010): 374-376.
- Li L, Parwani AV. Xanthogranulomatous Pyelonephritis. Arch Pathol Lab Med 135 (2011): 671-674.
- Kim SW, Yoon B Il, Ha US, et al. Xanthogranulomatous pyelonephritis: Clinical experience with 21 cases. J Infect Chemother 19 (2013): 1221-1224.
- Stoica I, O’Kelly F, McDermott MB, et al. Xanthogranulomatous pyelonephritis in a paediatric cohort (1963-2016): Outcomes from a large single-center series. J Pediatr Urol 14 (2018): 169.e1-169.e7.
- Morales C, Opazo V, Bassa C, et al. Xanthogranulomatous pyelonephritis: A case report. Urol Case Reports 19 (2018): 65-66.
- Yueh P, Lee LM, Wen YC, et al. Well surgical outcome of malakoplakia and xanthogranulomatous pyelonephritis which presented in the same patient: A case report and literature review. Urol Case Reports (2019): 101052.
- Yacoubi S El, Ziouziou I, Zizi M, et al. case Pyélonéphrite xanthogranulomateuse bilatérale focale: à propos d ’ un cas 8 (2014): 666-669.
- Gibbons R, Leonard N, Magee M, et al. Xanthogranulomatous Pyelonephritis: A Complicated Febrile Urinary Tract Infection Detected by Point-of-Care Ultrasound in the Emergency Department. J Emerg Med 55 (2018): e1-e4.
- Çaliskan S, Özsoy E, Kaba S, et al. Xanthogranulomatous pyelonephritis. Arch Iran Med 19 (2016): 712-714.
- Ho CI, Wen YK, Chen ML. Xanthogranulomatous pyelonephritis successfully treated with antibiotics only. J Chinese Med Assoc 71 (2008): 643-645.
- El-Asmar JM, Ghanem R, Ghandour R, et al. Postpartum xanthogranulomatous pyelonephritis: A case report. Case Reports Women’s Heal 22 (2019): e00112.
- Yarbrough ML, Hamad Y, Burnham CA, et al. Closing the Brief Case: Bacteremia and Vertebral Osteomyelitis Due to Staphylococcus schleiferi. J Clin Microbiol 55 (2017): 3309-3310.
- Swe T, Naing AT, Baqui AAMA, et al. Methicillin-resistant Staphylococcus schleiferi subspecies coagulans infection in a patient with hepatocellular carcinoma. J Investig Med High Impact Case Reports 4 (2016): 1-3.
- Öztürkeri H, Kocabeyoglu O, Yergök YZ, et al. Distribution of coagulase-negative staphylococci, including the newly described species Staphylococcus schleiferi, in nosocomial and community acquired urinary tract infections. Eur J Clin Microbiol Infect Dis 13 (1994): 1076-1079.
- Stoica I, Muntean A, McDermott MB, et al. Xanthogranulomatous pyelonephritis: The conundrum of a calcified kidney. J Pediatr Surg Case Reports 52 (2020): 101347.
- Garrido-Abad P, Rodríguez-Cabello MÁ, Vera-Berón R, et al. Bear paw sign: Xanthogranulomatous pyelonephritis. J Radiol Case Rep 12 (2018): 18-24.
- Chow J, Kabani R, Lithgow K, et al. Xanthogranulomatous pyelonephritis presenting as acute pleuritic chest pain: a case report. J Med Case Rep 11 (2017): 1-5.
- Peña PA, Torres-Castellanos L, Patiño G, et al. Minimally invasive nephrectomy for inflammatory renal disease. Asian J Urol 2019 (xxxx).


 Impact Factor: * 3.3
Impact Factor: * 3.3 Acceptance Rate: 73.59%
Acceptance Rate: 73.59%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 