Bone Marrow Metastatic Prostate Cancer Representing Itself With Deep Anemia
Aktas Yasin1* , Karamik Kaan1 , Mehmet Salih Boga1 , Yildirim Senay2 , Islamoglu Ekrem1 , Ates Mutlu1
1Health Sciences University Antalya Training and Research Hospital Department of Urology, Antalya, Turkey
2Health Sciences University Antalya Training and Research Hospital Department of Pathology, Antalya, Turkey
*Corresponding Author: Aktas Yasin, Health Sciences University Antalya Training and Research Hospital Department of Urology, Antalya, Turkey, Tel: +90-05373425596; E-mail: aktas.yasin.007@hotmail.com
Received: 16 July 2019; Accepted: 08 August 2019; Published: 02 September 2019
Article Information
Citation:
Aktas Yasin, Karamık Kaan, Mehmet Salih Boga, Yıldırım Senay, Islamoglu Ekrem, Ates Mutlu. Bone Marrow Metastatic Prostate Cancer Representing Itself With Deep Anemia. Archives of Nephrology and Urology 2 (2019): 062-066.
DOI: 10.26502/anu.2644-2833010
View / Download Pdf Share at FacebookKeywords
<p>Metastatic prostate cancer; Bone marrow aspiration; PSA; Bone marrow metastasis; Anaemia</p>
Article Details
1. Case Report
A 70-year-old male patient admitted to physiotherapy doctor with complaint of intermittent lower back pain lasting 2 months. Routine tests related to lower back pain such as hemogram, C-Reactive Protein (CRP), sedimentation rate and lumbosacral radiography were requested. The test results were as follows haemoglobin 7.7 g/dl, hematocrit 23.5%, platelets 132 000 /mm3, white blood cell 4500/mm3, sedimentation rate 140 mm/h, alkaline phosphatase (ALP) 146 U/L, lactate dehydrogenase (LDH) 258 U/L, calcium 8.1 mg/dl. Lumbosacral radiography indicated increased sclerosis and thinning of the cortex. These results showed that the patient had deep anaemia and low platelet count. Then, the patient was referred to the internal specialist. Primary or secondary bone marrow malignancy was thought on first assessment. Therewith, all tests on haematological malignancy and tumoral markers which included PSA, CA 15.3, CA125, CEA, JAK2 mutation, immunofixation electrophoresis, serum protein electrophoresis, immunoglobulins, bone marrow flow cytometer, bone marrow aspiration and biopsy, were requested. Among them PSA level and bone marrow biopsy took attention. Total PSA value were 2833 ng/ml and pathological investigation of bone marrow biopsy identified that carcinoma infiltration in the glandular pattern, in neoplastic cells were positive with PanCk, PSA (Figure 1).
Findings were consistent with bone marrow metastasis of prostate adenocarcinoma. Other haematological malignancies and tumoral markers were normal. Later, the patient was consulted to urology and after initial evaluations, 12 core needle transrectal ultrasound guided prostate biopsy was performed. Pathology report revealed a prostate adenocancer with Gleason score 4+3 in six cores positive of twelve fragments. Tumour rate was between 50%-100% in positive cores. Bone scintigraphy was performed for clinical staging and it was compatible with extensive bone metastasis (Figure 2). These results were discussed in urology-oncology council and patient was conducted chemotherapy and radiotherapy. Medical oncology began a docetaxel chemotherapy regimen with maximum androgen blockade (MAB) and denosumab for bone lesions. Radiation oncology also began radiation therapy for bone lesions. Patients current PSA and haemoglobin were 0.04 ng/ml and 10.1 g/dl, respectively. The patient is still on oncological follow-up. Written informed consent was obtained from the patient for their anonymized information to be published in this article.
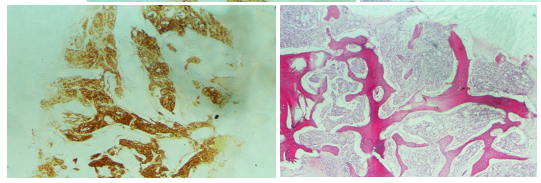
Figure 1: Histopathological findings (A) PSA immunohistochemical staining of the metastatic tumoral tissue (magnification, ×40). (B) Hematoxylin and eosin staining of the bone marrow. Tumoral glands infiltrated marrow distance (magnification, ×40).
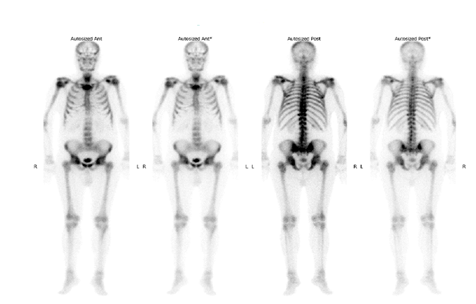
Figure 2: Findings compatible with extensive bone metastasis, The lesion in the manubrium sterni was observed in a lytic-sclerotic manner leading to cortical irregularity.
2. Discussion
The United States Preventive Services Task Force (USPSTF) has advised against the use of PSA for screening purposes [3]. Nevertheless, with declining rates of PSA testing, there has been an increased incidence of metastatic prostate cancer in the United States. The incidence of low-risk prostate cancer decreased from years 2007 to 2013 to 37% less than that of 2004. Conversely, the incidence of metastatic prostate cancer increased to 72% between 2007-2013 more than that of 2004. The greatest increase in metastatic prostate cancer was seen in men aged 55-69 years. Patients at these ages thought to most benefit from prostate cancer screening and early definitive treatment [4]. We can recognize patients with prostate cancer owing to PSA screening in the early stages and we can treat them. Nevertheless, patients with no urological complaints and patients who did not admit to the urology before or did not have PSA screening can be presented with advanced disease.
Bone involvement by solid tumours can be diagnosed on CT, MRI or bone scan. It is very rare to detect non-hematologic malignancy while examining the bone marrow biopsy. Detection of bone marrow metastatic deposits is important to determine the stage of the malignancy, chemotherapeutic response, prognosis and follow up [5]. Hypercalcemia, bone pain, raised the level of ALP and LDH, unexplained cytopenias and lytic or sclerotic bony lesions on radiology suggest bone marrow metastasis.
3. Conclusion
Declining use of the PSA test has been associated with an increased incidence of metastatic prostate cancer. Prostate cancer is a slowly developing malignancy but untreated cases can present symptoms of advanced disease such as bone pain, spinal cord compression, fatigue, depression, obstruction, weight loss, constipation and anaemia. We must systematically evaluate patients and keep in mind possibilities malignancy. We should be convincing, informative against patients. It should not be forgotten that prostate cancer is diagnosed at an early stage 5-years relative survival rate for local stage is almost 100% and for distant stage is 28%.
Conflicting Interests
The Author(s) declare(s) that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Informed Consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Ethical Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Contributorship
AY wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript
Acknowledgements
The authors would like to thank the anonymous reviewers for their comments on an earlier version of the manuscript, which have led to significant changes to the final manuscript.
References
- Daniyal M, Siddiqui ZA, Akram M, et al. Epidemiology, Etiology, Diagnosis and Treatment of Prostate Cancer. Asian Pac J Cancer Prev 15 (2014): 9575-9578.
- Leitzmann MF, Rohrmann S. Risk factors for the onset of prostate cancer: age, location, and behavioural correlates. Clinical Epidemiology 4 (2012): 1-11.
- Moyer Screening for prostate cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med 157 (2012): 120-134.
- Weiner AB, Matulewicz RS, Eggener SE, et al. Increasing incidence of metastatic prostate cancer in the United States (2004-2013). Prostate Cancer and Prostatic Diseases 19 (2016): 395-397.
- Mishra P, Das S, Kar R, et al. Non-hematopoietic malignancies metastasising to the bone marrow: A 5-year record based descriptive study from a tertiary care centre in South India. Indian J Cancer 51 (2014): 30-34.


 Impact Factor: * 3.3
Impact Factor: * 3.3 Acceptance Rate: 73.59%
Acceptance Rate: 73.59%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 