The Frequency of Acquired and Age-Related Tracheal Deformations: a Retrospective Study of CT Scan Findings
Article Information
Altman Edward1, Rappaport Rudolf2, Kroitoro Simona3, Barak Michal4*
1Senior Surgeon, Department of General Surgery, the Galilee Medical Center, Nahariya, Israel
2Senior Radiologist, Department of Radiology, Bnai Zion Medical Center, Haifa, Israel
3Senior Radiologist and Head of CT scan Unit, Department of Radiology, Bnai Zion Medical Center, Haifa, Israel
4Assistant Professor and Senior Anaesthesiologist, Department of Aanesthesiology, Rambam Health Care Campus, and the Bruce Rappaport Faculty of Medicine, Technion-Israel Institute of Technology, Haifa, Israel
*Corresponding Author: Dr. Michal Barak, Department of Anaesthesiology, Rambam Health Care Campus, Haifa 31096, Israel
Received: 21 May 2019; Accepted: 28 May 2019; Published: 03 June 2019
Citation: Altman Edward, Rappaport Rudolf, Kroitoro Simona, Barak Michal. The Frequency of Acquired and Age-Related Tracheal Deformations: a Retrospective Study of CT Scan Findings. Anesthesia and Critical Care 1 (2019): 23-28.
View / Download Pdf Share at FacebookAbstract
Background: Changes of the anatomy of the trachea occur during aging and as a result of a large goiter, cardiac or pulmonary diseases and smoking. These changes may cause difficulties in endotracheal intubation.
Methods: In this retrospective study, we analyzed the frequency of acquired deformations, as seen in chest CT scan of 200 adult patients. The radiographic findings were studied, as well as the patients’ demographic variables and co-morbidities.
Results: Acquired deformation of the trachea was found only in patients that were older than 50 years. In 117 patients 50 to 90 year-old three types of deformations were found: “S-shape” trachea in 83 patients (71%), horizontal left main bronchus with wide angle main carina in 24 patients (20.5%) and saber-sheath trachea in 10 patients (8.5%).
Conclusions: Acquired deformation of the trachea is frequent in patients older than 50. Studying the patient’s chest CT scan may assist the physician in performing endotracheal intubation cautiously and safely.
Keywords
Trachea, Endotracheal intubation, Acquired tracheal deformation, Double lumen tube
Trachea articles Trachea Research articles Trachea review articles Trachea PubMed articles Trachea PubMed Central articles Trachea 2023 articles Trachea 2024 articles Trachea Scopus articles Trachea impact factor journals Trachea Scopus journals Trachea PubMed journals Trachea medical journals Trachea free journals Trachea best journals Trachea top journals Trachea free medical journals Trachea famous journals Trachea Google Scholar indexed journals Endotracheal intubation articles Endotracheal intubation Research articles Endotracheal intubation review articles Endotracheal intubation PubMed articles Endotracheal intubation PubMed Central articles Endotracheal intubation 2023 articles Endotracheal intubation 2024 articles Endotracheal intubation Scopus articles Endotracheal intubation impact factor journals Endotracheal intubation Scopus journals Endotracheal intubation PubMed journals Endotracheal intubation medical journals Endotracheal intubation free journals Endotracheal intubation best journals Endotracheal intubation top journals Endotracheal intubation free medical journals Endotracheal intubation famous journals Endotracheal intubation Google Scholar indexed journals Acquired tracheal deformation articles Acquired tracheal deformation Research articles Acquired tracheal deformation review articles Acquired tracheal deformation PubMed articles Acquired tracheal deformation PubMed Central articles Acquired tracheal deformation 2023 articles Acquired tracheal deformation 2024 articles Acquired tracheal deformation Scopus articles Acquired tracheal deformation impact factor journals Acquired tracheal deformation Scopus journals Acquired tracheal deformation PubMed journals Acquired tracheal deformation medical journals Acquired tracheal deformation free journals Acquired tracheal deformation best journals Acquired tracheal deformation top journals Acquired tracheal deformation free medical journals Acquired tracheal deformation famous journals Acquired tracheal deformation Google Scholar indexed journals Double lumen tube articles Double lumen tube Research articles Double lumen tube review articles Double lumen tube PubMed articles Double lumen tube PubMed Central articles Double lumen tube 2023 articles Double lumen tube 2024 articles Double lumen tube Scopus articles Double lumen tube impact factor journals Double lumen tube Scopus journals Double lumen tube PubMed journals Double lumen tube medical journals Double lumen tube free journals Double lumen tube best journals Double lumen tube top journals Double lumen tube free medical journals Double lumen tube famous journals Double lumen tube Google Scholar indexed journals Computed tomography articles Computed tomography Research articles Computed tomography review articles Computed tomography PubMed articles Computed tomography PubMed Central articles Computed tomography 2023 articles Computed tomography 2024 articles Computed tomography Scopus articles Computed tomography impact factor journals Computed tomography Scopus journals Computed tomography PubMed journals Computed tomography medical journals Computed tomography free journals Computed tomography best journals Computed tomography top journals Computed tomography free medical journals Computed tomography famous journals Computed tomography Google Scholar indexed journals S-shape trachea articles S-shape trachea Research articles S-shape trachea review articles S-shape trachea PubMed articles S-shape trachea PubMed Central articles S-shape trachea 2023 articles S-shape trachea 2024 articles S-shape trachea Scopus articles S-shape trachea impact factor journals S-shape trachea Scopus journals S-shape trachea PubMed journals S-shape trachea medical journals S-shape trachea free journals S-shape trachea best journals S-shape trachea top journals S-shape trachea free medical journals S-shape trachea famous journals S-shape trachea Google Scholar indexed journals
Article Details
1. Introduction
The anatomy of the trachea may be anomalous due to congenital, physiologic or pathologic reasons [1-3]. The diseases affecting the trachea can be categorized into focal or diffuse diseases. Tracheobronchial strictures, such as post-intubation stenosis and tracheobronchial neoplasms are regarded as focal diseases, whereas tracheobronchomegaly, tracheomalacia, are examples of diffuse diseases. Cardiac and pulmonary diseases may cause changes in tracheal anatomy, as well as goiter, smoking and aging [1, 3]. In addition to anatomical changes, there are dynamic changes of the tracheal following anesthesia and relaxation [4]. Tracheal anatomy has great importance in procedures as tracheal intubation and ventilation [5, 6]. Casual, thoughtless intubation of anomalous trachea may result in tracheal tear and mortality, especially when introducing large devices as the double-lumen endotracheal tube [7, 8].
Computed tomography (CT) is the best non-invasive method for evaluation of tracheal lesions [9, 10]. In this study, we retrospectively analyzed chest CT scan of adult patients, in order to find the frequency of acquired tracheal anomalies in our population and its correlation with demographic variables and co-morbidities.
2. Patients and Methods
This study was conducted in Bnai-Zion Hospital, Haifa, after acquiring the institution’s Ethic Committee approval. It is a retrospective study of 200 adult patients, aged 40-90 years, who underwent chest CT scan in our hospital. Data that was analyzed: patient’s age, gender, main disease, co-morbidity, smoking, geometric parameters of trachea and its main bifurcation and bronchi and other pulmonary findings.
2.1 Statistical analysis
Comparison of quantity characteristics between possible reasons for deformation were performed by Anova, Kruskal Wallis test, independent sample t-test, Wilcoxon rank sum test. The decision of choosing among those tests were done according to the number of the groups which was compared, group size and shape of the data distribution. For qualitative data correlation, Chi square test or Fisher's exact test were used. The choice between those tests was done according to pre-assumptions of these tests. P value less 5% was considered significant.
3. Results
Two hundred patients were included in this study, 105 female and 95 male patients. Among 83 patients 40-49 year old no tracheal deformation was detected. This group was not included in the data analysis. In 117 patients 50 to 90 year-old three types of tracheal and main bronchi deformations were found: “S-shape” trachea in 83 patients (71%) (Figure 1), horizontal left main bronchus with wide angle main carina in 24 patients (20.5%) (Figure 2) and saber-sheath trachea in 10 patients (8.5%) (Figure 3).
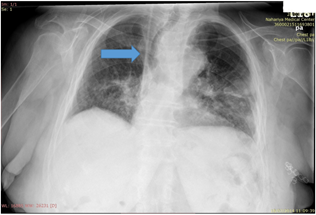
Figure 1: Chest x-ray of a patient with S-shape trachea (blue arrow shows the trachea).
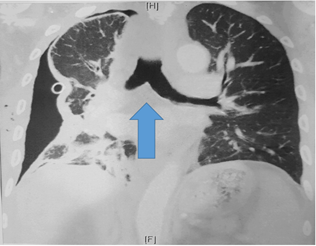
Figure 2: Chest CT scan of horizontal left main bronchus with wide angle main carina (blue arrow at the carina angle).
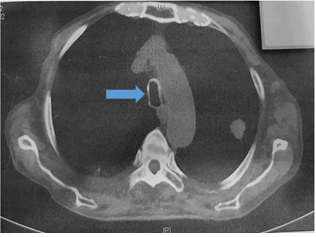
Figure 3: Chest CT scan of a saber sheath trachea (blue arrow shows the trachea).
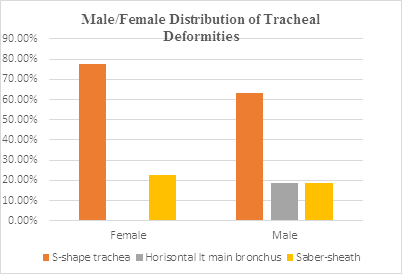
Figure 4: The distribution of acquired tracheal deformity between male and female patients.
Saber sheath trachea was detected in male patients only, while S-shape trachea was predominantly female (Figure 4).
No significant correlation was found between the patient’s age and deformity (p=0.92). Regarding co-morbidities: all the patients with saber sheath trachea had COPD, 54 of the patients with S-shape trachea (74%) had cardiovascular disease. Horizontal left main bronchus with wide angle main carina was not correlated to co-morbidities.
4. Discussion
The main result of this study was the finding of frequent acquired tracheal malformation in patients 50 year old and older. While S-shape trachea and wide main carina are detectable on standard chest x-ray exam, the saber sheath malformation is not, and chest CT scan is required for its diagnosis. The patients with saber sheath trachea were found to have COPD, while S-shape trachea was found in patients with cardio-vascular disease. Acknowledging the possibility of tracheal anomaly is significant if tracheal intubation is planned, especially in case the endotracheal tube is massive and long as the double-lumen tube.
The procedure of endotracheal intubation is extremely frequent. However, it may carry the risk of tracheal trauma, such as tear or rupture [11-13]. Post-intubation tracheal injury is a potentially fatal complication. Several factors may increase the risk for complication: repetitive attempts of intubation, emergency situations, intubation of a neonate, patient with a tracheal pathology, or when using large endotracheal tubes, as the double lumen tube [7, 8, 12-14]. The double-lumen tube is to be placed in the left main bronchus, thus the intubator has to rotate the tube to the left [15, 16]. In case of S-shape trachea, where the trachea curve is to the right, a rotation to the left may tear it. By being familiar with the tracheal anatomy, the injury may be prevented.
An important weakness of this study relies on its design as a retrospective study. Indeed, a prospective study may have a more robust result. Another problem was the study population that was younger than 50 years, where no tracheal deformity was found and was not included in the data analysis. However, this finding teaches us that patients younger than 50 are at lower risk for acquired tracheal deformity and intubation may be with reduced risk of complications. In the group of patients 50 year old and more, no significant correlation was found between patient’s age and deformity. This finding may be different in a larger group of patients.
5. Conclusions
Patient 50 year-old or older may have a required tracheal deformity. In patients with a non-linear trachea, intubation carries a risk of injuring the trachea. When planning to intubate such a patient, it is advised to become familiar with the tracheal anatomy, for a safe and cautious endotracheal intubation.
Acknowledgments
None
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Ethics Approval and Consent to Participate
The study was approved by the institutional local Ethic Committee.
Competing Interest
The authors declare that they have no competing interests.
References
- Lawrence DA, Branson B, Oliva I, et al. The wonderful world of the windpipe: a review of central airway anatomy and pathology. Can Assoc Radiol J 66 (2015): 30-43.
- Tsao TC, Shieh WB. Intrathoracic tracheal dimensions and shape changes in chronic obstructive pulmonary disease. J Formos Med Assoc 93 (1994): 30-34.
- Nygaard M, Hilberg O, Rasmussen F, et al. Tracheal collapsibility in adults is dynamic over time. Respir Med 146 (2019): 124-128.
- Herway ST, Benumof JL. The tracheal accordion and the position of the endotracheal tube. Anaesth Intensive Care 45 (2017): 177-188.
- Garstang JS, Bailey DM. General anaesthesia in a patient with undiagnosed "saber-sheath" trachea. Anaesth Intensive Care 29 (2001): 417-420.
- Asai T, Shingu K. Airway management of a patient with tracheal stenosis for surgery in the prone position. Can J Anaesth 51 (2004): 733-736.
- Tezel C, Okur E, Baysungur V. Iatrogenic tracheal rupture during intubation with a double-lumen tube. Thorac Cardiovasc Surg 58 (2010): 54-56.
- Marchese R, Mercadante S, Paglino G, et al. Tracheal stent to repair tracheal laceration after a double-lumen intubation. Ann Thorac Surg 94 (2012): 1001-1003.
- Acar T, Bayraktaroglu S, Ceylan N, et al. Computed tomography findings of tracheobronchial system diseases: a pictorial essay. Jpn J Radiol 33 (2015): 51-58.
- Kligerman S, Sharma A. Radiologic evaluation of the trachea. Semin Thorac Cardiovasc Surg 21 (2009): 246-254.
- Miñambres E, Burón J, Ballesteros MA, et al. Tracheal rupture after endotracheal intubation: a literature systematic review. Eur J Cardiothorac Surg 35 (2009): 1056-1062.
- Sternfeld D, Wright S. Tracheal rupture and the creation of a false passage after emergency intubation. Ann Emerg Med 42 (2003): 88-92.
- Fan CM, Ko PC, Tsai KC, et al. Tracheal rupture complicating emergent endotracheal intubation. Am J Emerg Med 22 (2004): 289-293.
- Wei JL, Bond J. Management and prevention of endotracheal intubation injury in neonates. Curr Opin Otolaryngol Head Neck Surg 19 (2011): 474-477.
- Pappin JC. The current practice of endobronchial intubation. Anaesthesia 34 (1979): 57-64.
- McGrath B, Tennuci C, Lee G. The History of One-Lung Anesthesia and the Double-Lumen Tube. J Anesth Hist 3 (2017): 76-86.

 Impact Factor: * 2.1
Impact Factor: * 2.1 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 