Granulomatous Mastitis: Manifestation of Primary Sarcoidosis Masquerading as Tubercular Mastitis
Richmond Ronald Gomes1*
1Associate Professor, Medicine, Ad-din Women’s Medical College Hospital, Dhaka, Bangladesh
*Corresponding Author: Dr. Richmond Ronald Gomes, Associate Professor of Medicine, Ad-din Women’s Medical College Hospital, Dhaka, Bangladesh
Received: 22 June 2021; Accepted: 28 June 2021; Published: 30 June 2021
Article Information
Citation:
Richmond Ronald Gomes, Granulomatous Mastitis: Manifestation of Primary Sarcoidosis Masquerading as Tubercular Mastitis. Fortune Journal of Rheumatology 3 (2021): 4-10.
View / Download Pdf Share at FacebookAbstract
Sarcoidosis is a multisystem disease of unknown etiology that affects young to middle aged adults, characterized by granuloma formation in various tissues, most commonly the lungs, lymphatics, skin and eyes. Involvement of the breast in sarcoidosis is rare. The breast is involved in less than 1% of cases and can be defined into three subsets, including granulomas localized to the breast, referred to as breast sarcoidosis. Breast can be either a primary or a secondary site of presentation. Breast sarcoidosis often mimics carcinomas at clinical examination. It may present with systemic findings such as erythema nodosum, arthritis, and uveitis, and unlike typical sarcoidosis, commonly manifests during pregnancy. We report a case of breast Sarcoidosis in a 35-year-old lady presenting as recurrent breast abscess with polyarthralgia. On histology, it was characterized by non-caseating giant cell granulomas. Differential diagnoses included idiopathic granulomatous mastitis, tuberculosis, fungal infection, cat-scratch disease, and sarcoid-like reactions to cancer. She was started anti tubercular therapy but responded poorly. Further clinical and laboratory investigations were consistent with a diagnosis of sarcoidosis. Specifically, serum levels of angiotensin-converting enzyme (ACE) were elevated. The patient received treatment with corticosteroid and immunosuppressive, methotrexate and is presently asymptomatic. Breast involvement by sarcoidosis, although rare, should be considered when dealing with granulomatous lesions of the breast.
Keywords
<p>Granulomatous disease; Sarcoidosis; Granuloma; Tuberculosis; Corticosteroid</p>
Article Details
1. Introduction
Sarcoidosis is an idiopathic multisystem inflammatory granulomatous disorder comprised of epithelioid and multinucleated giant cells with little necrosis. It affects young to middle aged adults, with a higher incidence in women. It usually invades the lungs with fibrosis [1-3], and may also involve lymph nodes, skin, liver, spleen, eyes, phalangeal bones, and parotid glands, but it is rare to find an isolated extra pulmonary disease (less than 10% of patients). The diagnosis is based on typical radiological manifestations supported by histological evidence, in particular thoracic radiograms, associated with clinical examination and an elevated serum angiotensin-converting enzyme (ACE) level, a pathognomonic feature of sarcoidosis. Exclusion of other granulomatous diseases is necessary. Sarcoidosis of the breast is rare. It occurs in less than 1% of cases and in differential diagnosis may be potentially considered as a malignancy [4–6]. We report a middle-aged lady with recurrent breast abscess with granulomatous inflammation of the breast as a first clinical manifestation of primary sarcoidosis masquerading as tubercular mastitis.
2. Case Report
A 35-year-old woman, not known to have diabetes, hypertension or bronchial asthma presented at 36 weeks of her 3rd pregnancy to her local obstetrician with a painful, red swelling in her right breast for 7 days. A breast ultrasound showed right breast abscess. Drainage of breast abscess was done, and she was treated with cephalosporin and flucloxacillin. Pus for culture failed to reveal growth of any organism. One month later, she again developed painful swelling in her right breast, new onset weakness, arthralgias and myalgias, so severe that she needed a walker for ambulation. Repeat ultrasonography revealed abscess in her right breast without any localized lymph node involvement. She also had a mild non-productive cough but denied fevers, chills, oral ulcers, dry mouth, shortness of breath, hemoptysis, chest pain, gastrointestinal symptoms, or hematuria. She was otherwise in good health. Her only medications included iron and calcium. There was no family history of autoimmune disease. She denied any recent travel, previous tuberculosis or contact with patients with active tuberculosis. She was vaccinated as per immunization schedule. Drainage of abscess was done; pus and tissue were sent for culture and sensitivity and histopathology, respectively. She was started meropenem with linezolid. Pus for culture revealed no growth. Histopathology revealed non caseating granuloma. Considering erythema nodosum and histopathology report she was discharged with anti-tubercular therapy (ATT).4 weeks after starting ATT, she again presented with same kind of painful right breast swelling. This time, she also developed polyarthralgia, red tender nodules on legs. On physical examination, she was afebrile but tachycardic with heart rate ranging from 100-110. Her lungs were clear to auscultation, and there was non-pitting edema of her legs to the knees. She did not have joint redness, tenderness or swelling and muscle strength was normal. On skin examination, she had a 6 x 7 cm indurated, tender, red mass in her right breast (Figure 1) as well as red tender subcutaneous nodules on her anterior legs (Figure. 2).
She had a normal complete blood count (CBC) and complete metabolic profile (CMP). Her C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) were highly elevated at 79 and 60, respectively. Further autoimmune serologies (ANA, dsDNA, nRMP/SM, SS-A, SS-B, Scl-70, Jo-1, histones, ribosomal P-proteins, and centromere) were negative. Chest radiograph (CXR) and CT chest did not show consolidation, fibrosis, or lymphadenopathy. Breast ultrasound showed right breast abscess. Drainage of breast abscess was done for third time.Swab and tissue cultures for bacterial, fungal and mycobacterial organisms were negative. Breast tissue biopsy showed non-caseating granulomas (Figure 3).
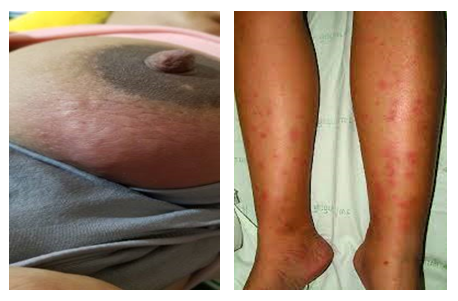
Figure. 1 and 2: showing red indurated right breast mass compatible with abscess and red subcutaneous nodules over anterior legs (erythema nodosum) respectively.
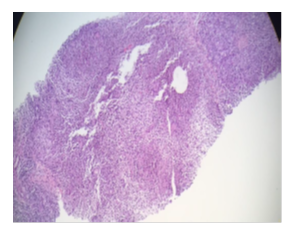
Figure 3: Histopathology of breast tissue showing non caseating granuloma.
The patient was diagnosed with sarcoidosis with a presentation of erythema nodosum, arthralgias, granulomatous mastitis not responding to ATT. The level of ACE in the sera was significantly elevated (126 U/l, normal range 20–70); the serum calcium concentration was at the upper level (2.50 mmol/l, normal range 2.14–2.53).
Once the diagnosis was confirmed the patient was treated with a standard dose corticosteroid therapy (1 mg/kg/day) with methotrexate 10 mg once weekly, with a gradual reduction in dosage. Remission of the disease was achieved and confirmed by a control breast Ultrasonography and repeat serum ACE (16U/L) revealing no signs of relapse, and 1-year follow-up results.
3. Discussion
Sarcoidosis is a chronic granulomatous disease that predominantly affects the intrathoracic organs. Only a few cases with a primary presentation of this disease in the breast tissue have been reported [7]. Sarcoidosis must be included in differential diagnosis of breast malignancy. Our patient presented with breast involvement of sarcoidosis, which is rare. Breast involvement in sarcoidosis is classified into three categories: sarcoidosis patients with breast cancer, breast cancer patients showing sarcoidosis-like breast reactions, and sarcoidosis patients with breast granulomas, which is referred to as breast sarcoidosis [8], the latter presentation of breast sarcoidosis is rare and accounts for less than 1% of cases of breast involvement of sarcoidosis. A total of 51 cases of breast sarcoidosis have been reported with approximately one quarter (23%) as the initial presentation [9]. In those 51 cases, the mean age of onset was 48 years, and the most frequent presentation is of a palpable mass concerning for breast cancer. Diagnosis is achieved by core biopsy revealing non-caseating granulomas, without evidence of adjacent malignancy. Numerous reports of idiopathic granulomatous mastitis, occurring most frequently in parous young women between the ages 30-40, usually within a few years after giving birth or during pregnancy exist [10]. In some of these patients, extra-mammary findings including erythema nodosum, arthralgias and episcleritis have been reported and these may represent a form fruste of sarcoidosis [11]. Though sarcoidosis is typically reported to be rare in pregnancy, reports of idiopathic granulomatous mastitis occurring during pregnancy are likely presentations of breast sarcoidosis, and thus the prevalence of sarcoidosis in pregnancy may be underestimated [12].
Sarcoidosis is an idiopathic multi system disease of unknown etiology characterized by the formation of granulomas in various tissues, most commonly the lungs, lymphatic tissue, skin, and eyes. The prevalence ranges from 4.7-63 in 100,000, and is more common in women, and in African Americans [13]. The pathogenesis is largely unknown but is thought to be due to an exaggerated immune response to unidentified antigens, either through an autoimmune phenomenon, or as reaction to underlying infection, including possibly mycobacteria. The inflammatory response is characterized by up regulation of Th1 CD4+ cells, causing increased production of IL-2, IFN-gamma, and TNF-alpha, with resultant epithelioid granuloma formation [14].
Clinical manifestations of sarcoidosis vary based on degree and location of tissue involvement. Lung disease is seen in approximately 90% of patients with sarcoidosis [15]. Lymphatic involvement is also common, and typically presents with bilateral hilar lymphadenopathy. Skin disease is seen in 30% of patients, and histologic specific lesions include papules, nodules, plaques, or subcutaneous nodules due to granuloma formation in the skin [16]. Nonspecific lesions include erythema nodosum. Bilateral ankle arthritis can be seen in 7-28% of patients [17].
Sarcoidosis is diagnosed by clinical and radiological presentation, evidence of non-caseating granulomas on histology, and lack of evidence for other diseases [17]. As a diagnosis of exclusion, other granuloma-forming conditions, including infections (most commonly tuberculosis or fungal disease), occupational or environmental induced granulomas, drug-induced granulomas and other idiopathic granulomatosis should be considered and excluded [13].
Diagnostic work-up in patients with sarcoidosis includes a thorough history and physical examination. If any cutaneous lesions are present, skin biopsy should be performed. Laboratory studies can include a CBC, CMP (to evaluate for renal or liver involvement), ESR and ACE level. Elevated ACE levels are seen in 60% of patients with sarcoidosis and can be used to monitor disease activity. Internal organ involvement should be screened for with an ophthalmology evaluation, chest X-ray, pulmonary function tests, and EKG. Treatments for sarcoidosis are most commonly employed with oral corticosteroids. Other treatments that can be effective include immunosuppressive agents such as methotrexate, azathioprine, leflunomide, cyclophosphamide, mycophenolate mofetil; TNF-alpha suppressants such as pentoxyfilline, thalidomide, and TNF-alpha inhibitors; and anti-inflammatory antimicrobial agents such as antimalarials and tetracycline derivatives [13].
In our case, ultrasonography also revealed breast abscess. Although not specific, some reported cases suggested MRI as a method of choice for the diagnosis of breast sarcoidosis [18]. As biopsy is a specific method for this diagnosis, pathohistological verification of breast tissue should always be made. The assessment of serum ACE activity, another specific test essential in diagnostics of primary sarcoidosis, also confirmed our findings.
In the differential diagnosis we excluded collagenous disorders by performing an ANA test. This test included antibodies against dsDNA, nRMP/SM, SS-A, SS-B, Scl-70, Jo-1, histones, ribosomal P-proteins, and centromere. All yielded negative results. Furthermore, other chronic granulomatous diseases such as idiopathic granulomatous mastitis, fungal infections and foreign body reactions had to be excluded [7, 19]. Idiopathic granulomatous mastitis is characteristic for the postpartum period, and it is characterized with panlobulitis associated with micro abscesses, ductal damage, and ductal inflammation [19]. No micro abscesses and ductal damage were present in our histopathology findings. Fungal infection was excluded by negative microscopic findings. Biopsy showed no foreign body reaction.
In conclusion, breast sarcoidosis is a rare presentation of this systemic disease, especially as a first clinical manifestation. When changes in the breasts are chronic and present as indeterminate masses, biopsy is required for pathohistological verification and accurate diagnosis. Biopsy in association with high serum levels of ACE confirmed our diagnosis of primary breast sarcoidosis. Because of the prompt diagnosis, early corticosteroid therapy with immunosuppressive could be started. Our patient showed improvement and remission of the disease with excellent 1 year follow-up.
4. Conclusion
Breast sarcoidosis has diverse and nonspecific imaging characteristics. Carcinoma must always be excluded by core needle biopsy. Achieving correct diagnosis is mandatory so that adequate corticosteroid and immunosuppressive therapy can be applied as early as possible. A multidisciplinary approach is of utmost importance in the diagnostic workup.
Conflict of Interests
None declared
Funding
None
References
- Aladesanmi OA. Sarcoidosis: An update for the primary care physician. Med Gen Med 6 (2004): 7.
- Prabhakar HB, Rabinowitz BC, Gibbons FK, et al. Imaging features of sarcoidosis on MDCT, FDG PET, and PET/CT. AJR Am J Roentgenol 190 (2008): 1–6.
- Tremblay A, Stather DR, Maceachern P, et al. A randomized controlled trail of standard vs endobronchial ultrasonography-guided transbronchial needle aspiration in patients with suspected sarcoidosis. Chest 136 (2009): 340–346.
- Isley LM, Cluver AR, Leddy RY, et al. Primary sarcoid of the breast with incidental malignancy. J Clin imaging Sci 2 (2012): 46.
- Fiorucci F, Conti V, Lucantoni G, et al. Sarcoidosis of the breast: A rare case report and a review. Eur Rev Med Pharmacol Sci 10 (2006): 47–50.
- Donaldson BA, Polynice A, Oluwole S: Sarcoidosis of the breast: Case report and chart review. Am Surg 61 (1995): 778–780.
- Gisvold JJ, Crotty TB, Johnson RE. Sarcoidosis presenting as spiculated breast masses. Mayo Clin Proc 75 (2000): 293–295
- Lower EE, Hawkins HH, Baughman RP. Breast disease in sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis 18 (2001): 301-306.
- Mona el K, Pascal C, Charley H, et al. Quiz case. Breast sarcoidosis presenting as a metastatic breast cancer. Eur J Radiol 54 (2005): 2-5.
- Altintoprak F, Kivilcim T, Ozkan OV. Aetiology of idiopathic granulomatous mastitis. World J Clin Cases 2 (2014): 852-858.
- Fahmy J, Halabi-Tawil M, Bagot M, et al. Erythema nodosum during the course of idiopathic granulomatous mastitis. Ann Dermatol Venereol 142 (2015): 46-49.
- Hadid V, Patenaude V, Oddy L, et al. Sarcoidosis and pregnancy: obstetrical and neonatal outcomes in a population-based cohort of 7 million births. J Perinat Med 43 (2015): 201-207.
- Valeyre D, Prasse A, Nunes H, et al. Sarcoidosis. Lancet 383 (2014): 1155-1167.
- Kataria YP, Holter JF. Immunology of sarcoidosis. Clin Chest Med 18 (1997): 719-739.
- Sheffield EA. Pathology of sarcoidosis. Clin Chest Med 18 (1997): 741-754.
- Judson MA. Extrapulmonary sarcoidosis. Semin Respir Crit Care Med 28 (2007): 83-101.
- Joint Statement of the American Thoracic Society (ATS) the European Respiratory Society (ERS) the World Association of Sarcoidosis and Other Granulomatous Disorders (WASOG) adopted by the ATS Board of Directors and by the ERS Executive Committee, February 1999. Am J Respir Crit Care Med 160 (1999): 736-755.
- Krause A, Gerber B, Rohde E, et al. Sarcoid tumor of the breast (in German). Zentralbl Gynakol 118 (1996): 299–302.
- Banik S, Bishop PW, Ormerod LP, et al. Sarcoidosisof the breast. J Clin Pathol 39 (1986): 446–448.

 Impact Factor:
* 1.7
Impact Factor:
* 1.7
 Acceptance Rate:
74.36%
Acceptance Rate:
74.36%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
