Vomiting as the Sole Manifestation of Congenital Diaphragmatic Hernia in an 8-Month-Old Infant
Article Information
Sylwester Gerus1*, Marcin Rasiewicz1, Katarzyna Wielgos3, Sonia Nogalska2, Dariusz Patkowski1
1Department of Pediatric Surgery and Urology, Wroclaw Medical University, Wroclaw, Poland
2Wroclaw Medical University, Wroclaw, Poland
3Department of Pediatrics, Voivodeship Specialist Hospital, Wroclaw, Poland
*Corresponding Author: Sylwester Gerus, Department of Pediatric Surgery and Urology, Wroclaw Medical University, Wroclaw, Poland
Received: 30 December 2019; Accepted: 11 January 2020; Published: 25 January 2020
Citation:
Sylwester Gerus, Marcin Rasiewicz, Katarzyna Wielgos, Sonia Nogalska, Dariusz Patkowski. Vomiting as the Sole Manifestation of Congenital Diaphragmatic Hernia in an 8-Month-Old Infant. Journal of Pediatrics, Perinatology and Child Health 4 (2020): 001-006.
View / Download Pdf Share at FacebookKeywords
Congenital diaphragmatic hernia, Digestive system
Congenital diaphragmatic hernia articles, Digestive system articles
Article Details
1. Introduction
Congenital diaphragmatic hernia is a birth defect that occurs in 1 out of 2000-3000 born-alive infants [1] and consists in a displacement of internal organs towards the chest due to a defect in the diaphragm. In most cases, it is a unilateral defect that occurs on the left side without the presence of a hernial sac. The symptoms appear shortly after birth, usually in the respiratory and circulatory systems. In 5-25% of the cases [2-5], the symptoms of congenital diaphragmatic hernia occur after the neonatal period. In such case, the defect is referred to as late-presenting congenital diaphragmatic hernia. Its symptoms are not characteristic and may take an acute or chronic form occurring mostly in the respiratory and digestive systems, which can lead to wrong or late diagnoses.
2. Case Report
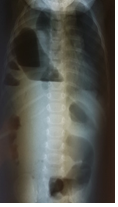
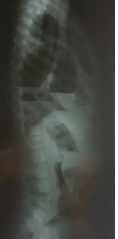
An 8-month-old girl was admitted to the pediatric ward of the Voivodeship Hospital in Wroclaw as she was repeatedly vomiting gastric contents with no other worrying symptoms. The medical history stated that she had been born at term, in a good general condition and had not suffered from any serious illnesses to date. The symptoms occurred suddenly several hours before admission. After admission, the patient’s state was moderate, the abdomen was soft, slightly sunken, moderately painful on the whole surface, with no pathological resistance and without peritoneal symptoms. Slight symptoms of dehydration were also noted. In laboratory tests (blood count, GPT, GOT, creatinine, ionogram, CRP), apart from slightly higher levels of CRP (7.9 mg/l where the norm is <6 mg/l) no deviations from the norms were found. While in hospital, the patient was subfebrile and vomited gastric contents containing fresh blood several times. As bleeding in the upper part of the digestive system was suspected, the girl was transferred to the Pediatric Surgery and Urology Clinic of Wroclaw Medical University for consultation and possible further treatment. She was brought to the emergency department at night. She was sleepy and in a moderate general condition. Physical examination proved the abdomen to be soft, with no pathological resistance and moderately painful below the chest. The skin bore no signs of dehydration and the mucosa of the oral cavity was normal. Due to diminished vesicular sound on the right side of the chest and the suspicion of obstruction of the digestive system, X-rays of the chest and the abdominal cavity were taken in a standing position and abdominal and pleural cavity ultrasound scans were performed as well. The ultrasound scan showed no deviations from the norm (both pleural cavities were described as having no pathological contents), however, the chest X-ray (in the anteroposterior and lateral projection, Figure 1 and Figure 2) showed distended small bowel loops in the area of the right side of the chest with fluid levels.
The patient was diagnosed with late-presenting congenital diaphragmatic hernia with the obstruction of the digestive system and was admitted to a ward. Intravenous fluids were administered, the blood group was determined and the patient was prepared for surgery, which was performed in general anesthesia several hours later. It was decided that diagnostic laparoscopy would be performed. The patient was placed on her back. A 5-mm optical port was inserted through the navel and another two 3.5-mm trocars were placed in the left umbilical region and midepigastrium. The operating table was slightly lifted on the side of the head and on the right side, which caused the liver to move and reveal the right side of the diaphragm. In order to gain access to the diaphragm’s defect, which was located in the posterolateral area, liver ligaments were dissected. The distended small bowel loops were moved from the right pleural cavity. Having moved the intestines, an optical port was inserted into the pleural cavity, where the presence of fluids was discovered and the presence of a part of the right lower pulmonary lobe, which could have been responsible for the presence of pulmonary sequestration, was noted. The fluid was suctioned and the defect in the diaphragm of the approximate size of 3 × 1.5 cm was closed by means of single non-absorbable sutures. Neither the chest nor the abdominal cavity was drained. No direct postoperative complications occurred. Feeding started the day after the surgery and was well-tolerated. A chest X-ray showed no abnormalities in the diaphragm or lungs. The patient was discharged from hospital on the third day after the surgery. Chest tomography was performed in ambulatory conditions in order to rule out the suspected pulmonary sequestration. The scan showed no abnormalities in the lung tissue and the hemidiaphragm silhouette was also correct.
At present, the girl remains under the control of the pediatric surgery clinic, develops properly and does not show any worrying symptoms in the respiratory or digestive systems.
3. Discussion
Congenital diaphragmatic hernia is a birth defect, which is most frequently diagnosed in the first days after birth and in most cases occurs on the left side [1]. However, in approximately 5-25% of the cases [2-5], or even in 45% according to some authors [6], the infants diagnosed with the defect are one month old and older. It is then referred to as late-presenting congenital diaphragmatic hernia. A high percentage of the patients diagnosed with the defect after the neonatal period has been described by Elhalaby in rural areas of Egypt and may be related to the high mortality rate among infants with congenital diaphragmatic hernia [6]. A characteristic feature of the described type of diaphragmatic hernia, as opposed to the type diagnosed directly after birth, is a low frequency of concurrent defects, which may be an argument supporting the claim that these two types of diaphragmatic hernia are caused by different pathogenetic factors [2, 3, 7]. It is also assumed that the prognoses in late-presenting congenital diaphragmatic hernia are good and that this type is characterized with a much lower mortality rate than in the case of the defect occurring in the neonatal period: according to relevant studies, the mortality rate in this group of patients is approximately 3.8%. In both types of diaphragmatic hernia, the defect was located on the left side (79.4% vs. 20.6%) in the posterolateral area. The male to female ratio was approximately 2:1 [1, 2, 4].
As opposed to congenital diaphragmatic hernia occurring in the neonatal period, whose main symptom is respiratory insufficiency, older children present a wide array of symptoms that are not pathognomonic for this defect. The patients may show no symptoms (approx. 10% of the patients), present acute or chronic symptoms that are most often related to the respiratory system (coughing, frequent infections, whizzing, dyspnea and symptoms of respiratory insufficiency) and the digestive system (nausea, vomiting, abdominal pain and constipation) or their combination [2, 8]. Therefore, it happens that children with late-presenting congenital diaphragmatic hernia are diagnosed with and treated for other more common diseases that share the same symptoms, which may delay the proper diagnosis and treatment and result in complications, including death. In the case of diaphragmatic hernia occurring on the right side in one-third of patients, especially the ones younger that one year, the symptoms occur mostly in the respiratory system. The older the patient the more frequently the symptoms include abdominal pain, constipation as well as vomiting, and they are more often chronic. It is most probably connected with the presence of the diaphragm preventing the intestines from moving to the pleural cavity, which happens in the case of younger children. As opposed to the left-side hernia, acute symptoms occur less frequently [2, 8, 9]. The our patient experienced sudden vomiting of gastric contents, moderate abdominal pain and symptoms of dehydration. The parents arrived at the emergency department suspecting an intestinal infection and the consulting pediatrician asked for a surgical consultation in order to rule out an obstruction of the digestive system caused by herniation or acute appendicitis. A physical examination showed no deviation from the correct condition, apart from moderate abdominal pain and diminished vesicular sound on the right side. In laboratory tests, apart from slightly higher levels of CRP in the serum, no deviations from the norms were found, as was the case with an ultrasound scan of the abdominal and pleural cavities (both pleural cavities were described as containing no fluids or air). Only a chest X-ray image showed distended bowel loops in the right pleural cavity. This situation confirms the reports of other authors, who claim that late-presenting congenital diaphragmatic hernia constitutes a challenge, since the patient is older and the symptoms are not characteristic, which leads few doctors to consider the presence of congenital diaphragmatic hernia. A patient’s examination does not differ from the regular algorithm: case history, a physical examination and then additional (laboratory and imaging) tests. Measuring the levels of inflammatory parameters may confirm an infective background of the symptoms. Among imaging tests, the most frequently performed are X-rays and ultrasound scans of the chest and abdominal cavity. Neither of them is expensive and they are both routine test that are available in most pediatric and surgical centers. Additionally, an ultrasound scan does not expose patients to radiation and should be the first-choice examination. According to the data described by Bag?aj, chest X-rays make it possible to diagnose late-presenting congenital diaphragmatic hernia only in 49% of the patients, whereas 25% of them are diagnosed with pneumonia, lung tissue malformations, pleural empyema and dehiscence of the diaphragm [2, 10, 11]. Ultrasound scans of the chest and abdominal cavity, however, make it possible to examine lung tissue and evaluate diaphragm mobility and continuity as well as relations between various organs. In case of further diagnostic uncertainties, it is recommended to perform computer tomography of the abdominal cavity and the chest.
In the case of our patient, the ultrasound scan of the abdominal cavity and the chest showed no abnormalities. Thus, if an X-ray of the chest had not been performed or only an X-ray of the abdominal cavity had been performed, the patient would have been sent back to the pediatric ward and treated conservatively. That is why we suggest performing at least two imaging tests of the abdominal cavity and the chest in the case of patients differentially diagnosed with diaphragmatic hernia. Late-presenting congenital diaphragmatic hernia is an indication to urgent surgical treatment after the patient has been properly prepared. Access through the abdominal cavity is preferable [12]: laparotomy or laparoscopy, depending on the level of experience of the medical center or the operator. Owing to this type of access, it is possible to evaluate the organs removed from the pleural cavity and assess the peritoneal cavity. In the case of our patient, a laparoscopy was performed with the use of 5- and 3.5-mm trocars, which resulted in a good cosmetic effect and less pain after the surgery. Laparoscopy also made it possible to insert an optical port to the pleural cavity in order to assess lung tissue.
As mentioned earlier, late-presenting congenital diaphragmatic hernia is a defect whose postsurgical course and prognoses are described as good. Our patient left the pediatric surgery ward on the third day after the surgery, remains under the control of the pediatric surgery clinic, develops properly and does not show any symptoms of recurrence of diaphragmatic hernia in imaging tests.
4. Conclusions
Late-presenting congenital diaphragmatic hernia is a rare defect with different clinical pictures, a high possibility of misdiagnosis during imaging tests and the occurrence of complications in the case of a lack of correct diagnosis, which should be taken into consideration in the differential diagnosis of the patients presenting non-characteristic clinical symptoms, especially after one month of age.
References
- Keijzer R, Puri P. Congenital diaphragmatic hernia. Semin. Pediatr Surg 19 (2010): 180-185.
- Bag?aj M. Late-presenting congenital diaphragmatic hernia in children: a clinical spectrum. Ped Surgery Int 20 (2004): 658.
- Butler MW, Stolar CJH, Altman RP. Contemporary management of congenital diaphragmatic hernia. World J Surg 17 (1993): 350-355.
- Newman BM, Afshani E, Karp MP, et al. Presentation of Congenital Diaphragmatic Hernia Past the Neonatal Period. Arch Surg 121 (1986): 813-816.
- Mei-Zahav M, Solomon M, Trachsel D, et al. Bochdalek diaphragmatic hernia: not only a neonatal disease. Arch Dis Child 88 (2003): 532-535.
- Elhalaby EA, Abo Sikeena MH. Delayed presentation of congenital diaphragmatic hernia. Ped Surgery Int 18 (2002): 480.
- Holder AM, Klaassens M, Tibboel D, et al. Genetic factors in congenital diaphragmatic hernia. Am J Hum Genet 80 (2007): 825-845.
- Kitano Y, Lally KP, Lally PA. Congenital Diaphragmatic Hernia study group: Late-presenting congenital diaphragmatic hernia. J Pediatr Surg 40 (2005): 1839-1843.
- Chang SW, Lee HC, Yeung CY, et al. A Twenty-year Review of Early and Late-presenting Congenital Bochdalek Diaphragmatic Hernia: Are They Different Clinical Spectra. Pediatr Neonatol 51 (2010): 26-30.
- Baglaj M, Dorobisz U. Late-Presenting Congenital Diaphragmatic Hernia in Children: A Literature Review. Pediatric Radiology 35 (2005): 478-488.
- Kim DJ, Chung JH. Late-presenting congenital diaphragmatic hernia in children: the experience of single institution in Korea. Yonsei Med J 54 (2013): 1143-1148.
- Cigdem M, Onen A, Otcu S, et al. Late Presentation of Bochdalek-Type Congenital Diaphragmatic Hernia in Children: A 23-Year Experience at a Single CenterSurg Today 37 (2007): 642.


 Impact Factor: * 3.8
Impact Factor: * 3.8 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 