A Case of Recurrent Massive Secondary Postpartum Haemorrhage following Caesarean Section Due to the Eroded Left Uterine Artery Sealed by Laparoscopic Bipolar Coagulation
Ramkrishna Purohit*, Jay Gopal Sharma, Devajani Meher
Department of Obstetrics and Gynaecology, Purohit General Hospital, Odisha, India
*Corresponding Author: Ramkrishna Purohit, Director, Department of Obstetrics and Gynaecology, Purohit General Hospital, Shakti Nagar, Bargarh, pin-768028, Odisha, India
Received: 12 January 2022; Accepted: 23 January 2022; Published: 31 January 2022
Article Information
Citation:
Ramkrishna Purohit, Jay Gopal Sharma, Devajani Meher. A Case of Recurrent Massive Secondary Postpartum Haemorrhage following Caesarean Section Due to the Eroded Left Uterine Artery Sealed by Laparoscopic Bipolar Coagulation. Obstetrics and Gynecology Research 5 (2022): 054-058.
View / Download Pdf Share at FacebookAbstract
Background: Recurrent massive secondary postpartum haemorrhage (PPH) due to uterine wound dehiscence with uterine artery erosion following LSCS causes management challenges.
Case: Primiparous of 26 years had three recurrent episodes of severe PPH within 37 days after LSCS. Hysteroscopy visualized features of uterine scar dehiscence on the left angle side and excluded other causes of PPH after the 2nd episode on the 24th day and found bleeding through the wound gap. Laparoscopy after 3rd episode on 37th day revealed bleeding eroded left uterine artery. Bipolar coagulation of the left uterine artery sealed bleeding and conserved the uterus.
Conclusion: Recurrent massive PPH may occur from uterine artery erosion following LSCS scar dehiscence. Abdominal sonography, a quick hysteronscopy, and an emergency laparoscopic bipolar seal of the eroded uterine artery can serve the purpose of minimally invasive surgery in a stable patient.
Keywords
<p>Recurrent Massive Secondary Post-partum Haemorrhage, Uterine Scar Dehiscence, The Role of Hysteroscopy, Postpartum Uterine Artery Erosion, Laparoscopic Coagulation of Eroded Uterine Artery</p>
Article Details
1. Introduction
Secondary postpartum haemorrhage (PPH) following caesarean section (CS) occurs one in 365 cases. Common causes are the retained products of concept-tion, subinvolution of placental site and endometritis, etc. Massive life-threatening secondary PPH due to uterine wound dehiscence after lower segment caesa-rean section (LSCS), and because of uterine artery erosion is rare [1]. The diagnostic difficulty of such cases increases morbidity and delays definitive inter-vention. We, present here with a case of recurrent (three times) massive secondary PPH within 37 days after LSCS where a hysteroscopy helped us to detect bleeding through the left angle of the uterine scar from the eroded left uterine artery, and was managed laparoscopically.
2. The Case
A 26-year primiparous woman was presented to our hospital in an emergency on the 24th day after CS in a state of haemorrhagic shock. She was afebrile, her blood pressure was not recordable. There was infla-mmation and induration of the abdominal wall skin scar. Vaginal wall had no tear or trauma. About 100cc of blood clot was removed from vagina during the speculum examination. However, there was no fresh haemorrhage from the vaginal or cervical canal at the time of examination. LSCS was indicated for failed progress of labour. She was discharged from the hospital on the fifth post-operative day after uneventful recovery. She gave history of a similar episode of severe vaginal bleeding on 20th day (first episode) after LSCS. She responded to conservative management with intravenous fluids, blood trans-fusion and antibiotics in another local hospital. The bleeding stopped following the management, and she went home after a day.
On bimanual vaginal examination, uterus was well involuted, external cervical os was patulous. There was tenderness in fornices. Transabdominal ultra-sound showed an empty uterine cavity and cervical canal. There was a hypoechoic area of broad ligament suggesting oedema measuring 2.5cm beside the left angle of the CS scar. The right angle of the LSCS scar did not show any hypoechoic oedematous area. She was resuscitated with intravenous fluid and blood transfusion. Broad-spectrum antibiotics were started. We continued watchful conservative management as there was no active bleeding. Blood investigation showed leucocytosis (TLC - 12800/mm3) with predominant neutrophils, severe anaemia with hemoglobin-5.4Gm%, normal Platelet- 290 thousand/ ml and raised CRP level-10.6mg/L.
We performed hysteroscopic evaluation 48 hours after conservative treatment with an aim to find other causes of PPH like a retained piece of placenta, endometritis, scar dehiscence, slough, etc. Hyster-oscope entered easily into the uterine cavity without a need for cervical dilatation. The tip of the 30-degree hysteroscope was directed towards the posterior wall of the uterus during insertion to avoid the fragile LSCS scar. Hysteroscopy showed smooth uterine cavity, pale appearing endometrium without any tear or space- occupying lesion or endometritis. During withdrawal of the telescope, the anterior wall of the cervix showed multiple loose loops of vicryl suture hanging in one place (Figure 1) to the left side of the midline of the LSCS scar. Also, there was a thin string of blood clots of the recent bleeding hanging along the loops of vicryl suture on the left side (Figure 1). The upper end of the clot was there inside the LSCS wound gap. Hysteroscopic diagnosis of sloughing of edges of incision on the left side of uterine scar was made. In view of no active bleeding throughout the admission periods, we took the traditional decision to continue with the conservative treatment. The patient recovered and went home after 5 days.
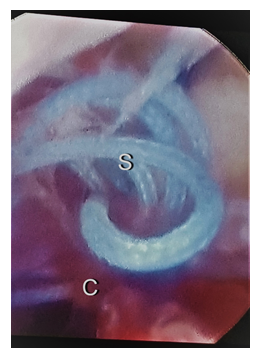
Figure 1: Hysteroscopy picture showing crumpled loops of vicryl suture (S)with blood clots( C ) on the left angle of the LSCS scar.
On the 37th day after the caesarean section, she again presented in emergency with the third episode of vaginal bleeding. The patient was apprehensive about her concern. Her blood pressure measured 120/80mm of Hg, the pulse of 96/min. The patient was in stable condition. During speculum examination, about 200cc of blood clot came out of the vagina. Again, there was no active bleeding from the cervix. The patient was treated with a plasma expander and intravenous fluids. Her transabdominal ultrasono-graphy had similar oedematous features to that of the previous one after 2nd episode of bleeding. We strongly suspected the source of recurrent bleeding was from the left uterine artery erosion following uterine scar dehiscence and decided to proceed with emergency laparoscopy, and laparotomy as when required. She signed the informed consent for operative laparoscopy, emergency laparotomy and if needed, for a hysterectomy. Under anaesthesia, we tried a quick hysteroscopy as the patient had no active vaginal bleeding and was in stable condition. The hysteroscopy found a clear uterine cavity, the clot and blood were seen clearly at the LSCS wound dehiscence.
Laparoscopy showed no intraperitoneal adhesions, bleeding, or pus. The uterus was well involuted. The previous incision on uterovesical peritoneum was opened by blunt dissection using Maryland forceps. Surprisingly, there was complete dehiscence of the uterine incision on the left side and the dehiscence was extending into the broad ligament beyond the left uterine artery. Firm clot of about 10ml was aspirated from the left angle of incision. Clot removal caused fresh bleeding from the left uterine artery. The pressure was used to stop bleeding. Sloughing of the left angle created a gap of about 2.5 cm between the upper and lower uterine edges of the incision. But there was no bleeding from the edges of the uterine wound or from other tissues except the left uterine artery. Ascending branch of the left uterine artery was barely exposed, eroded at multiple sites and stretched in the gap between upper and lower margins of the uterine wound. The artery had three separate bleeding holes along its exposed trunk and were the sources of recurrent massive postpartum haemorrhage. Bleeding was directly ejecting into the lower uterine cavity and flowing into the cervical canal. There was no sacculation or pseudoaneurysm of the left uterine artery. The right angle of LSCS incision was well healed and the right uterine artery was unexposed. Then, the exposed trunk of the left uterine artery was grasped by laparoscopic Babcock’s forceps and was coagulated by bipolar energy (45 watts) to stop bleeding [2]. The coagulated artery trunk was not divided. Sutures were avoided fearing a cut-through.
After achieving complete haemostasis, edges of incisions after minimal debridement were closed in a single full -thickness layer using interrupted vicryl suture no 1(Ethicon). Inj. Meropenem (1Gm) was administrated 12 hourly for 5 days. The patient continued scanty blood tint discharge vaginally from inflamed and oedematous tissues for 5 days and was discharged from the hospital on the 6th post-operative day. She was followed 6 weeks later with no fresh complaints. The patient resumed her normal menstruation 3 months after laparoscopy. Thereafter, she did not experience recurrence of severe uterine bleeding.
3. Discussion
This is the first case in our obstetrics practice of 22 years. Recurrent episodes of massive secondary PPH following uterine wound dehiscence like the present case had been reported by previous studies [1, 3-6]. Massive haemorrhage occur usually from uterine artery leaks [1, 3-5]. Erosion of the arterial wall due to infection may occur without an aneurysm [7]. Remission due to different haemostasis mechanisms in between 2 episodes of massive haemorrhage gives a false impression of complete recovery, and delays diagnosis and definitive treatment. The main risk factor associated with infection and weakening of the arterial wall is previous surgical trauma [8] among others like underlying arterial pathology, foreign body, intimal disruption, and endothelial cell (EC) dysfunction, etc. The sloughing out of the left angle of the CS scar compared to the right angle in this case, caused tension and tearing of the bare weak ascending branch of the uterine artery. All cases having infection of the abdominal wound and uterine wound do not suffer from uterine wound dehiscence and massive PPH. Sloughing of uterine wound margins rarely happens due to infection [9]. The uterine wound dehiscence could be detected by MRI. A pelvic angiogram would have detected and occluded by uterine artery embolization the leaks from the uterine artery in a hemodynamically stable patient in the same sitting [3]. Bare exposed uterine artery erosion was the culprit of severe secondary PPH in this case. Alternatively, in the present case, abdominal sonography, a quick hysteroscopy, and an emergency laparoscopic bipolar seal of uterine artery could serve the purpose of minimally invasive surgery in a stable patient. In the present case, lapa-roscopic bipolar coagulation of the uterine artery successfully stopped bleeding and helped to conserve the uterus like that of uterine artery embolization [1, 4, 5].
4. Conclusion
Recurrent massive PPH may occur from uterine artery erosion following LSCS scar dehiscence. Abd-ominal sonography, a quick hysteroscopy, and an emergency laparoscopic bipolar seal of the uterine artery can serve the purpose of minimally invasive surgery in a stable patient.
Acknowledgement
The woman whose story was reviewed in this case report had provided written consent for its pub-lication
References
- Sengupta Dhar R, Misra R. Postpartum Uterine Wound Dehiscence Leading to Secondary PPH: Unusual Sequelae.Case Rep Obstet Gynecol 2012 (2012): 154685.
- Ram Krishna Purohit. Purohit technique of vaginal hysterectomy: a new approach 110 (2003): 1115-1119.
- Suja Varghese, Nandini Gokulam, Sheika Al Abri. Uterine Artery Embolization in Postpartum Hemorrhage: A Case Report. Oman Med J 27 (2012): e033.
- Ahmet Ozgur Yeniel, Ahmet Mete Ergenoglu, Ali Akdemir. Massive Secondary Postpartum Hemorrhage with Uterine Artery Pseudoan-eurysm after Cesarean Section. Case Rep Obstet Gynecol 2013 (2013): 285846.
- Dasari P, Maurya DK, Mascarenhas M. Uterine artery pseudoaneurysm: a rare cause of secondary postpartum haemorrhage following caesarean section. BMJ Case Rep (2011).
- Barahmeh S, Edwan SH. Secondary post-partum haemorrhage with uterine artery pseudoaneurysm after caesarean section, managed with uterine artery embolization. S Afr J Obstet Gynaecol 23 (2017): 28-30.
- Jamaan T, Raedecke J, Kayser C. Septic Bleeding of the Common Carotid Artery Following Total Thyroidectomy: An Atypical Complication.Case Rep Med 2010 (2010): 953282.
- Christopher J, Abularrage MD, Robert S. Extracranial infected carotid artery aneurysm. Journal of Vascular Surgery 50 (2009): 1484-1486.
- Rivlin ME, Carroll CS, Morrison JC. Infectious necrosis with dehiscence of the uterine repair complicating cesarean delivery: a review. Obstet Gynecol Surv 59 (2004): 833-837.


 Impact Factor: * 3.2
Impact Factor: * 3.2 Acceptance Rate: 76.63%
Acceptance Rate: 76.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 