Impact of Endometriosis on Pregnancy and Delivery- A Retrospective Cohort Study
Impact of Endometriosis on Pregnancy and Delivery- A Retrospective Cohort Study
Sebastian D. Schäfer*, Moritz Berkenkamp, Martin Götte, Ralf Schmitz, Ludwig Kiesel
University Hospital Münster, Department of Gynecology and Obstetrics, Münster, Germany
*Corresponding Author: Sebastian D. Schäfer, MD PhD University Hospital Münster, Department of Gynecology and Obstetrics Albert-Schweitzer-Campus 1, Building A1, 48149 Münster, Germany
Received: 19 August 2022; Accepted: 15 September 2022; Published: 20 September 2022
Article Information
Citation: Sebastian D Schäfer, Moritz Berkenkamp, Martin Götte, Ralf Schmitz, Ludwig Kiesel. Impact of Endometriosis on Pregnancy and Delivery- A Retrospective Cohort Study. Obstetrics and Gynecology Research 5 (2022): 187-193.
View / Download Pdf Share at FacebookAbstract
Objective: To clarify if endometriosis, especially deep infiltrating endometriosis (DE), in our cohort is associated with increased risk of obstetric complications.
Material and Methods: Single center, retrospective analysis of consecutive cases (endometriosis laparoscopically removed and child wish) vs. consecutive controls (endometriosis laparoscopically excluded and child wish), from 2009 until 2016. Calculation of pregnancy rate. Analysis of mode of delivery and complications using Clavien-Dindo-classification. Analysis of DE using ENZIAN classification. Comparison also with controls from the literature. Statistical analysis: t-test (p < 0.050) and 95% Confidence Interval (CI).
Results: Inclusion of 501 out of 973 cases vs. 291 out of 789 controls. Pregnancy rate: cases 57.5% vs. controls 60.7%. Vaginal delivery: more in cases if natural conception (62% vs. 46.7% if ART, p=0.009). Cesarean section: if pregnancy by ART more secondary Cesarean section in cases (32% vs 20.8%; p=0.040). Miscarriage: more in controls (34.9% vs 27.6%; p=0.038). Complications: Clavien Dindo I and II more in cases (I: 43.3% vs. 32.5%, p=0.005; II: 29.7% vs. 21.0%, p=0.010). Clavien Dindo III and IV not increased. During pregnancy: more bleeding (p=0.005), early uterine contractions (p=0.012), cervical insufficiency (p=0.042), and tendency to more pre-eclampsia (p=0.080) in cases. During delivery: more bleeding (p=0.007), vaginal tear (p=0.009), pubic diastasis (p=0.022), prolonged labor (p=0.011), less episiotomy (p=0.002) in cases. During puerperium: more bleeding (p=0.022), infectious complications (p=0.007) in cases. DE: more cases of severe bleeding and abnormal cardiotocography leading to secondary caesarean section. Adenomyosis: slightly increased risk of secondary cesarean section (38.6% vs 27.7%, p=0.1). Cases vs control groups from the literature: more placenta praevia (p=0.042), placental abruption an
Keywords
Endometriosis; Pregnancy; Delivery complications; ENZIAN; Clavien-Dindo; Deep infiltrating endometriosis; Adenomyosis
Endometriosis articles Endometriosis Research articles Endometriosis review articles Endometriosis PubMed articles Endometriosis PubMed Central articles Endometriosis 2023 articles Endometriosis 2024 articles Endometriosis Scopus articles Endometriosis impact factor journals Endometriosis Scopus journals Endometriosis PubMed journals Endometriosis medical journals Endometriosis free journals Endometriosis best journals Endometriosis top journals Endometriosis free medical journals Endometriosis famous journals Endometriosis Google Scholar indexed journals Pregnancy articles Pregnancy Research articles Pregnancy review articles Pregnancy PubMed articles Pregnancy PubMed Central articles Pregnancy 2023 articles Pregnancy 2024 articles Pregnancy Scopus articles Pregnancy impact factor journals Pregnancy Scopus journals Pregnancy PubMed journals Pregnancy medical journals Pregnancy free journals Pregnancy best journals Pregnancy top journals Pregnancy free medical journals Pregnancy famous journals Pregnancy Google Scholar indexed journals Delivery complications articles Delivery complications Research articles Delivery complications review articles Delivery complications PubMed articles Delivery complications PubMed Central articles Delivery complications 2023 articles Delivery complications 2024 articles Delivery complications Scopus articles Delivery complications impact factor journals Delivery complications Scopus journals Delivery complications PubMed journals Delivery complications medical journals Delivery complications free journals Delivery complications best journals Delivery complications top journals Delivery complications free medical journals Delivery complications famous journals Delivery complications Google Scholar indexed journals ENZIAN articles ENZIAN Research articles ENZIAN review articles ENZIAN PubMed articles ENZIAN PubMed Central articles ENZIAN 2023 articles ENZIAN 2024 articles ENZIAN Scopus articles ENZIAN impact factor journals ENZIAN Scopus journals ENZIAN PubMed journals ENZIAN medical journals ENZIAN free journals ENZIAN best journals ENZIAN top journals ENZIAN free medical journals ENZIAN famous journals ENZIAN Google Scholar indexed journals Clavien-Dindo articles Clavien-Dindo Research articles Clavien-Dindo review articles Clavien-Dindo PubMed articles Clavien-Dindo PubMed Central articles Clavien-Dindo 2023 articles Clavien-Dindo 2024 articles Clavien-Dindo Scopus articles Clavien-Dindo impact factor journals Clavien-Dindo Scopus journals Clavien-Dindo PubMed journals Clavien-Dindo medical journals Clavien-Dindo free journals Clavien-Dindo best journals Clavien-Dindo top journals Clavien-Dindo free medical journals Clavien-Dindo famous journals Clavien-Dindo Google Scholar indexed journals Deep infiltrating endometriosis articles Deep infiltrating endometriosis Research articles Deep infiltrating endometriosis review articles Deep infiltrating endometriosis PubMed articles Deep infiltrating endometriosis PubMed Central articles Deep infiltrating endometriosis 2023 articles Deep infiltrating endometriosis 2024 articles Deep infiltrating endometriosis Scopus articles Deep infiltrating endometriosis impact factor journals Deep infiltrating endometriosis Scopus journals Deep infiltrating endometriosis PubMed journals Deep infiltrating endometriosis medical journals Deep infiltrating endometriosis free journals Deep infiltrating endometriosis best journals Deep infiltrating endometriosis top journals Deep infiltrating endometriosis free medical journals Deep infiltrating endometriosis famous journals Deep infiltrating endometriosis Google Scholar indexed journals Adenomyosis articles Adenomyosis Research articles Adenomyosis review articles Adenomyosis PubMed articles Adenomyosis PubMed Central articles Adenomyosis 2023 articles Adenomyosis 2024 articles Adenomyosis Scopus articles Adenomyosis impact factor journals Adenomyosis Scopus journals Adenomyosis PubMed journals Adenomyosis medical journals Adenomyosis free journals Adenomyosis best journals Adenomyosis top journals Adenomyosis free medical journals Adenomyosis famous journals Adenomyosis Google Scholar indexed journals Reproductive Techniques articles Reproductive Techniques Research articles Reproductive Techniques review articles Reproductive Techniques PubMed articles Reproductive Techniques PubMed Central articles Reproductive Techniques 2023 articles Reproductive Techniques 2024 articles Reproductive Techniques Scopus articles Reproductive Techniques impact factor journals Reproductive Techniques Scopus journals Reproductive Techniques PubMed journals Reproductive Techniques medical journals Reproductive Techniques free journals Reproductive Techniques best journals Reproductive Techniques top journals Reproductive Techniques free medical journals Reproductive Techniques famous journals Reproductive Techniques Google Scholar indexed journals puerperium articles puerperium Research articles puerperium review articles puerperium PubMed articles puerperium PubMed Central articles puerperium 2023 articles puerperium 2024 articles puerperium Scopus articles puerperium impact factor journals puerperium Scopus journals puerperium PubMed journals puerperium medical journals puerperium free journals puerperium best journals puerperium top journals puerperium free medical journals puerperium famous journals puerperium Google Scholar indexed journals neonatal outcome articles neonatal outcome Research articles neonatal outcome review articles neonatal outcome PubMed articles neonatal outcome PubMed Central articles neonatal outcome 2023 articles neonatal outcome 2024 articles neonatal outcome Scopus articles neonatal outcome impact factor journals neonatal outcome Scopus journals neonatal outcome PubMed journals neonatal outcome medical journals neonatal outcome free journals neonatal outcome best journals neonatal outcome top journals neonatal outcome free medical journals neonatal outcome famous journals neonatal outcome Google Scholar indexed journals
Article Details
Introduction
While symptoms of endometriosis often improve during pregnancy, there seems to be an increased risk of adverse pregnancy outcome [1-4]. Assisted Reproductive Techniques (ART), which are often necessary because of endometriosis-associated infertility, constitute a risk factor for complications during pregnancy [5]. The aim of this study was to analyse the reproductive outcome of women with endometriosis who received treatment at our certified expert endometriosis center, compared to controls with surgically excluded endometriosis from the same period suffering from sterility. Additionally the outcome of our endometriosis cases was compared with data of healthy controls available from the literature.
Material and Methods
All surgical endometriosis cases from our department from the period 2009 until 2016 were identified from patient records. As an internal control group, patients from the same period undergoing laparoscopy because of infertility during which endometriosis was excluded, were equally identified from patient records. Both groups received similar questionnaires by mail asking patients to report on any additional treatment regarding endometriosis as well as infertility, occurring pregnancies, mode of delivery and complications during pregnancy, delivery and puerperium. Those patients not responding to the questionnaires were offered a telephone interview if they gave their consent. The possible specific influence of deep infiltrating endometriosis (DE) rated using the ENZIAN classification [6,7] for better understanding of the severity of DE cases, on pregnancy and its outcome was analysed. The Clavien-Dindo-classification was used to describe the complications reported [8-10]. Cesarean sections were not considered a complication or surgical intervention in the sense of the Clavien-Dindo-classification. There was no analysis of fetal or neonatal outcome performed in the study.
Statistical Analysis
IBM SPSS Statistics version 25 (IBM Corporation, New York, NY, USA) was used and differences were calculated using the t-test. The reproductive outcome was calculated as relative risk for cases and controls using 95% Confidence Interval (CI). A value of p<0.050 was considered statistically noticeable for every statistical analysis.
Ethical approval
The local ethics committee “Ethikkommission der Ärztekammer Westfalen-Lippe und der Medizinischen Fakultät der Westfälischen Wilhelms-Universität”, approved of the study (Ethical approval number 2016-076-f-S, dated 13 September 2016). Written informed consent was obtained from all participants. The study was performed in accordance with the Declaration of Helsinki.
Results
Cases and internal Controls
2.764 cases were identified. 973 out of those had a child wish. 501 patients could be reached by questionnaire or telephone (51.5%). 472 patients were lost to follow-up (48.5%). 414 women were included (Figure 1). 238 cases experienced 343 pregnancies.
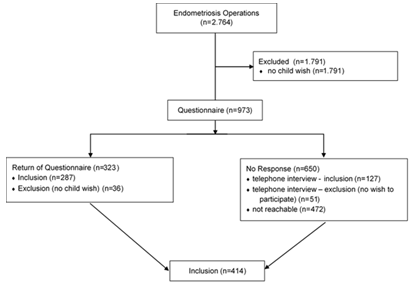
Figure 1: Description of endometriosis cases.
789 controls were identified. 252 women could be reached by questionnaire or telephone (31.9%). 33 controls declined participation. 537 controls were lost to follow up (68.1%). 219 women were included. 193 pregnancies were reported in 131 controls.
Pregnancy rate and outcome
Patient characteristics, pregnancy rate and pregnancy outcome are reported in table 1. Median age when giving birth and relative number of pregnancies were similar in cases and controls. Secondary caesarean sections were more frequent in cases achieving pregnancy by ART (p=0.04). Birth by primary caesarean section seemed to be more frequent in controls as well as generally in case of conception by ART but these differences were not statistically noticeable (p=0.202 / p=0.092). Natural birth was similar between groups but it was more frequent in cases with natural conception as well as controls with ART (p=0.009). Miscarriage rate was higher in patients from the control group (p=0.038), especially in the subgroup with natural conception (p=0.011).
|
Parameter |
With endometriosis (n=414*) |
Without endometriosis (n=219**) |
p-value |
|
Patients with pregnancies (n) |
238 (57.5%) |
133 (60.7%) |
0.214 |
|
Total pregnancies (n) |
343 |
193 |
0.34 |
|
Pregnancies per patient |
1.44 |
1.45 |
/ |
|
Median age when giving birth (years) |
34.4 |
34.8 |
0.562 |
|
Ongoing pregnancies |
31 |
7 |
|
|
Primary caesarean section (n) |
39 (11.4%) |
25 (13.0%) |
0.202 |
|
-natural conception (n) |
12 (6.6%)§ |
8 (8.7%)§ |
/ |
|
- ART (n) |
27 (14.1%)§ |
17 (16.8%)§ |
/ |
|
Secondary caesarean section (n) |
69 (20.1%) |
29 (15.0%) |
0.111 |
|
- natural conception (n) |
29 (15.9%) |
14 (15.2%) |
/ |
|
- ART (n) |
40 (20.8%) |
15 (14.9%) |
0.04 |
|
Natural birth (n) |
124 (36.2%) |
67 (34.7%) |
0.34 |
|
-Natural conception (n) |
67 (36.8%)# |
28 (30.4%)$ |
/ |
|
- ART (n) |
57 (29.7%)# |
39 (38.6%)$ |
/ |
|
Interruption (n) |
11 (3.2%) |
3 (1.6%) |
0.112 |
|
- Natural conception (n) |
5 (2.7%) |
2 (2.2%) |
/ |
|
- ART (n) |
6 (3.1%) |
1 (1.0%) |
/ |
|
Miscarriage (n) |
100 (29.2%) |
69 (35.8%) |
0.038 |
|
- Natural conception (n) |
51 (28.0%) |
41 (44.6%) |
0.011 |
|
- ART (n) |
49 (25.5%) |
28 (27.7%) |
/ |
Table 1: Patient characteristics, pregnancy rate and pregnancy outcome (*: total: n=414; natural conception: n=182; ART: n=192; **: total: n=219; natural conception: n=92, ART: n=101; §: ART both groups vs. natural conception both groups: p=0.092; #: cases natural conception vs. cases ART: p=0.009; $: controls natural conception vs. controls ART: p=0.009).
Complications
In cases during pregnancy bleeding (15.2% vs 7.0%, p = 0.005), early uterine contractions (9.5% vs 3.9%, p = 0.012) and cervical insufficiency (5.7% vs 2.3%, p = 0.042) were increased. In addition, there was a trend towards more pre-eclampsia (3.8% vs 1.6%; p = 0.080). During labour the risk of vaginal tear (7.2% vs 2.3%, p = 0.009), bleeding (2.3% vs 0%, p = 0.007) and pubic diastasis (1.5% vs 0%, p = 0.022) was increased. During puerperium bleeding (1.5% vs 0%; p=0.022), scar infections (2.3% vs 0%; p =0.007), as well as fever (0.8% vs 0%; p=0.078) and total number of complications were increased. Complications according to Clavien-Dindo-classification are reported in Table 2.
|
Clavien-Dindo-Grade |
Endometriosis (n=374) |
Controls (n=200) |
p-value |
|
I |
162 (43.3%) |
65 (32.5%) |
0.005 |
|
II |
111 (29.7%) |
42 (21%) |
0.01 |
|
III |
53 (14.2%) |
39 (19.5%) |
n.s.n. |
|
IV |
0 |
0 |
/ |
|
V |
0 |
0 |
/ |
|
During pregnancy |
|||
|
Vaginal bleeding |
40 (15.2%) |
9 (7%) |
0.005 |
|
Early uterine contractions |
25 (9.5%) |
5 (3.9%) |
0.012 |
|
Cervical insufficiency |
15 (5.7%) |
3 (2.3%) |
0.042 |
|
Diabetes |
12 (4.6%) |
7 (5.4%) |
n.s.n. |
|
Pre-eclampsia |
10 (3.8%) |
2 (1.6%) |
n.s.n. |
|
Rupture of amniotic membrane |
8 (3%) |
6 (4.7%) |
n.s.n. |
|
Placenta praevia |
8 (3%) |
1 (0.8%) |
n.s.n. |
|
Hypertension |
6 (2.3%) |
3 (2.3%) |
n.s.n. |
|
Placental insufficiency |
4 (1.5%) |
1 (0.8%) |
n.s.n. |
|
During labour |
|||
|
Pathological cardiotocography |
25 (9.5%) |
9 (7%) |
n.s.n. |
|
Vaginal tear |
19 (7.2%) |
3 (2.3%) |
0.009 |
|
Green amniotic fluid |
14 (5.3%) |
5 (3.9%) |
n.s.n. |
|
Perineal rupture of unknown degree |
14 (5.3%) |
8 (6.2%) |
n.s.n. |
|
Perineal rupture II° |
8 (3%) |
10 (7.8%) |
n.s.n. |
|
Bleeding |
6 (2.3%) |
0 (0%) |
0.007 |
|
Prolonged labour |
5 (1.9%) |
9 (7%) |
0.011 |
|
Perineal rupture III° |
4 (1.5%) |
2 (1.6%) |
n.s.n. |
|
Breech presentation |
4 (1.5%) |
4 (3.1%) |
n.s.n. |
|
Pubic diastasis |
4 (1.5%) |
0 (0%) |
0.022 |
|
Occipito posterior presentation |
1 (0.4%) |
5 (3.9%) |
n.s.n. |
|
Episiotomy |
1 (0.4%) |
9 (7%) |
0.002 |
|
During puerperium |
|||
|
Scar infection |
6 (2.3%) |
1 (0.8%) |
0.007 |
|
Curettage |
4 (1.5%) |
5 (3.9%) |
n.s.n. |
|
Bleeding |
4 (1.5%) |
0 (0%) |
0.022 |
Table 2: Complications according to Clavien-Dindo-classification and details on complications (n>3; nsn: not statistically noticeable).
Influence of deep infiltrating Endometriosis and Adenomyosis
Women with DE (ENZIAN A, B, C) were compared to patients without DE. 213 pregnancies in patients with DE were identified and compared to 81 pregnancies in patients without DE but suffering from endometriosis. While the probability of natural birth was similar (54.2% vs 53.57%), more women without DE were in need of a secondary caesarean section (39.3% vs. 23.7%; p=0.02). In half of these cases, this was due to multiple birth and obstructed or prolonged labour. Women with DE however were more likely to suffer from severe bleeding (16.1% vs 4.6%, p=0.07) resulting in a secondary caesarean. This was often associated with disorders affecting the placenta like placenta praevia, placental insufficiency or placental abruption, while women without DE in need of a secondary caesarean reported only one case of placental abruption (12.9% vs 4.55%, p=0.13). Primary caesarean sections were more frequently chosen as the mode of delivery for women with DE (20.61% vs 7.14%, p<0.01). Also abnormal cardiotocography was more likely in women with DE even if this difference was only a trend (12.4% vs 7.14%, p=0.12). Abnormal cardiotocography was statistically noticeably more often the reason for a secondary caesarean section (38.71% vs 13.64%, p=0.01) in patients with DE.
There was a trend towards a higher rate of miscarriage in women with DE (29.1% vs 24.69%, p=0.22). There was no difference in rate of secondary caesarean section among patients with ENZIAN B vs. patients with ENZIAN A or C (20.6% vs. 23.7%, p = 0.357). The pregnancy outcomes of women with adenomyosis were compared to women with endometriosis at other locations. Age of women at birth (34.2 vs 34.4 years; p=0.54), pregnancy duration (38.4 vs. 39.0 weeks, p=0.212) and miscarriage rate (28.8% vs. 27.2%, p = 0.398) were similar. Secondary caesarean section occurred slightly more often (38.6% vs. 27.7%; p=0.1) in case of adenomyosis. Women with adenomyosis gave birth by vaginal delivery in only 40.9% of cases. Women with ENZIAN A and C (n=71) did not show more lacerations under delivery, nor were they more likely to suffer from perineal laceration (12.7% vs 12.8%; p = 0.488) nor labial tear (9.9% vs 10.3; p =0.463). 58 women with ENZIAN FB endometriosis of the bladder reported natural delivery in 33.3% (lowest between endometriosis groups) and birth by secondary caesarean section in 38.9% (highest between the groups). Miscarriage rate was similar to other endometriosis subgroups (27.6% vs 28.0%; p =0.468).
Discussion
According to this study, endometriosis was not associated with increased caesarean section rates overall compared to internal controls, a group made up of patients with infertility and surgically excluded endometriosis. In subgroup analyses, there was a trend in favour of internal controls who conceived by ART regarding primary caesarean sections, as well as a statistically noticeable difference in favour of cases who conceived by ART regarding secondary caesarean sections. This group also had a statistically noticeable decrease in probability of natural delivery. Miscarriages occurred more frequently in internal controls. Further subgroup analysis showed that this effect might be mainly due to controls conceiving naturally. This group would typically include patients suffering from habitual abortions. Endometriosis was associated with increased risks during pregnancy, delivery and puerperium. Complications were mainly Clavien Dindo I or II categories in case of endometriosis. Clavien Dindo IV and V complications did not occur. DE in general was not associated with an increased risk of miscarriage, delivery by secondary caesarean section or obstetric complications when compared to other types of endometriosis. Adenomyosis and bladder endometriosis were associated with a slightly increased risk of secondary caesarean section compared to other types of endometriosis. The return rate for the questionnaire was good in the endometriosis group (51.5 %) and acceptable in the control group (31.9 %). Compliance might have been higher in the endometriosis group because this study was performed at a tertiary referral center for endometriosis. All cases were diagnosed, treated and classified by a specialist, which is a strong point of this study. The answers given by the patients however could not always be verified by analysing original medical documents. Especially symptoms like pain, nausea and even bleeding might be underreported as these were considered common symptoms in pregnancies by some and were therefore not always understood to be noteworthy. Pregnancy rate was similar in patients with endometriosis and controls. While Sharma et al found this similarity only in patients with endometriosis under the age of 35, in this study all age groups showed pregnancy rates comparable to controls [11]. Lin et al [12] showed an increased risk of placenta praevia in pregnant women with endometriosis, which is also reflected in our study`s endometriosis group. While placental abruption was not associated with endometriosis in the Chinese study, our survey reported 2 women with endometriosis with placental abruption, while none of the control group were affected. However, the numbers were too small for statistical analysis. As the control group of this study is a selected population group of patients suffering from infertility without endometriosis which therefore does not represent healthy controls, we also compared the results of cases to healthy control groups available from the literature which can be seen as representative of the general population. In this study miscarriage rate was highest in internal controls who conceived naturally. A possible explanation might be the occurrence of habitual abortions within this group. Miscarriage rate was noticeably lower for women with endometriosis compared to internal controls in this study. Compared to the equivalent age group of pregnant women in Denmark between 1978-1992 the risk of miscarriage in this study was noticeably higher for women suffering from endometriosis (12.4% vs. 27.6%, p<0.001) [13]. The relative risk was calculated at 2.23 (1.84-2.70). A Japanese cohort study suggests a much lower relative risk of 1.24 (1.20-1.29, 95% CI) [1]. This might be due to cases originating from a tertiary referral center which could mean that more severe cases were included. The rate of secondary caesarean sections in internal controls who conceived by ART showed a trend towards being lower than in the endometriosis group overall. This is probably not due to fewer complications, but rather the consequence of the trend towards a higher rate of primary caesarean sections due to increased expectancy of complications, as meta-analyses show an increased risk for obstetric and perinatal complications in this group [14]. The risk for a secondary caesarean section seems to be noticeably higher in patients with endometriosis than in the average population in Germany (29.7% vs 15.9% p<0,001) [15], while there was no statistically noticeable difference in the number of planned caesarean sections (16.8% vs 15.4%, p=0.283). This contradicts a Swedish survey stating that the adjusted odds ratio (OR) of pre-labour caesarean sections is 1.64 (1.54-1.75, 95% CI), whereas the OR for emergency caesarean sections was only 1.18 (1.10-1.27, CI 95%) [16]. However, the rate of emergency caesarean sections in Sweden is only 8.6 % and therefore the lowest out of the 31 European countries analysed in the study by Macfarlane et al, while the rate is at 15.9% in Germany [17]. This suggests that a caesarean section is indicated much faster in Germany than in Sweden, the patient characteristics differ between the countries or guidelines lead to a different kind of management. The higher rate of emergency caesarean sections may indicate that there were more unforeseen complications in this group. This supports recent data according to which adverse pregnancy outcomes and obstetrical complications are more common in women suffering from endometriosis [18,19]. While, statistically, women with endometriosis were more likely to suffer from Clavien-Dindo I and II complications, more severe complications, which needed surgical, endoscopic or radiological intervention (Clavien-Dindo III), were not increased. This might be due to the fact that more severe complications were too rare to be detected in this study. DE classified using the ENZIAN classification was analysed separately from other forms of endometriosis. Miscarriage rate was slightly increased in DE compared to other forms of endometriosis and occurred more frequently than in the general population. In case of DE miscarriage rate in this study was 29.1% compared to 19.7% in the general population [24]. More obstetrical complications were reported in women with DE, especially severe bleeding associated with disorders of the placenta like placenta praevia, placental insufficiency or placental abruption, while women without DE only rarely reported placental anomalies. As a consequence abnormal cardiotocography as the reason for a secondary caesarean section was more frequent in cases with DE. This might also explain the increased probability of primary caesarean sections in patients with DE. In contrast to the results of a study conducted by Allerstorfer et al., which showed a higher rate of caesarean sections for women with ENZIAN A or C endometriosis compared to ENZIAN B [19], we found no differences between these groups. There may be many reasons for this finding. One of them might be that breech presentation (3.6%) and obstructed labour (4.7%) only occurred in women without DE in our study. Other studies suggest that the incidence of obstructed labour in the general population is even higher than stated by the women without DE in this study (8.9% vs 4.7%) [20]. This might also be due to underreporting in the study because of the study design. Miscarriage rate for patients with adenomyosis was similar to that of patients with DE but higher than in the general population (28.8% / 29.1% vs 19.7%) [24]. Secondary caesarean section was necessary more often in patients with adenomyosis. Women with adenomyosis had a significantly decreased probability of vaginal spontaneous delivery as opposed to the average German population as reported in the literature (40.9% vs 70.4%, p-value <0.01) [23]. Leyendecker et al [21] suggest that adenomyosis is a result of a dysfunction of the endometrial-subendometrial unit. As this disease can affect all myometrial uterine muscle layers this may increase the risk for obstructed labour. While prolonged labour occurred in 4.4% (n=2) of the cases of adenomyosis and only 1.5% (n=3) of the cases with endometriosis in other locations the numbers are too small to draw definitive conclusions. As endometriosis of the uterus seems to increase the risk of complications during labour it may seem obvious that endometriosis of the rectovaginal space / vagina and the rectum may increase the risk of perineal laceration and bowel complications. However, women with endometriosis in these locations were not reported to suffer from lacerations more often than other women with endometriosis, suggesting that endometriosis does not generally weaken the tissue in this cohort. Patients with bladder involvement had the lowest rate of spontaneous delivery compared to other groups with DE. Reported reasons were mainly cardiotocographic anomalies and obstructed labour. Numbers for miscarriage were similar to the average woman with endometriosis. While bladder endometriosis did not seem to have a negative impact on early pregnancies, this might have changed with uterine growth leading to more direct contact with bladder endometriosis. Other studies show that pregnancy outcome is favourable after removal of bladder endometriosis [22].
Limitations of this study mainly are due to limited sample size, retrospective design of the study, data collection being dependent of patient participation, response rate, the internal control group suffering from infertility and possibly differing surgical techniques between the surgeons involved.
Conclusion
This study shows that women with endometriosis and adenomyosis have a higher risk of miscarriage and caesarean section compared to published controls from the general population. This however varies depending on the location of endometriosis lesions. Especially women with adenomyosis, who also suffer from prolonged labour, are often in need of a caesarean section. The risk for placenta praevia and placental abruption seemed to be higher in case of endometriosis and even more so in DE than in the average population. The risk for bleeding during all stages of pregnancy and delivery was much higher for women suffering from endometriosis. Also early uterine contractions and cervical insufficiency occurred noticeably more often. According to the Clavien-Dindo classification severe complications did not occur more often during the pregnancy of women with endometriosis, however mild to moderate complications were more likely to happen. DE of the rectovaginal space, the vagina and the rectum did not seem to increase the risk of severe lacerations during vaginal delivery. Counselling of endometriosis patients with regard to pregnancy and delivery is recommended. Patients should have access to specialized centers of care also with regard to pregnancy and delivery as increased risks are reported. Recommendations regarding mode of delivery should not exclude vaginal delivery in case of DE.
Authors' contributions
SDS: Protocol/project development, Data collection and management, Data analysis, Manuscript writing/editing
MB: Data collection, Data analysis, Manuscript writing/editing
MG: Data analysis, Manuscript writing/editing
RS: Data analysis, Manuscript writing/editing
LK: Data analysis, Manuscript writing/editing
Conflict of interest statement
SDS, MB, MG and RS declare no competing interest. LK reports personal fees from Ferring Pharmaceuticals A/S, personal fees from MITHRA Pharmaceuticals SA, personal fees from Novartis Pharma GmbH, personal fees from palleos healthcare, personal fees from abbvie, personal fees from Actavis Group, personal fees from AstraZeneca, personal fees from Gedeon Richter, personal fees from Dr. Kade/Besins, personal fees from Pantarhei, personal fees from Roche Pharma AG, personal fees from Shionogi, personal fees from Exeltis, outside the submitted work.
Acknowledgements
All authors confirm that the corresponding author Sebastian Daniel Schäfer, MD PhD and the co-author Mr. Moritz Berkenkamp contributed equally to this work
References
- Harada T, Taniguchi F, Onishi K, et al. Obstetrical Complications in Women with Endometriosis: A Cohort Study in Japan. PLOS ONE (2016): 168-476.
- Porpora MG, Tomao F, Ticino A, et al. Endometriosis and pregnancy: a single institution experience. Int J Environ Res Public Health 17 (2020): 401-402
- Kobayashi H, Kawahara N, Ogawa K, et al. A relationship between endometriosis and obstetric complications. Reprod Sci 27 (2020): 771-778
- Farland LV, Prescott J, Sasamoto N, et al. Endometriosis and Risk of adverse pregnancy outcomes. Obstet Gynecol 134 (2019): 527-536
- Mani S, Ghosh J, Lan Y, et al. Epigenetic changes in preterm birth placenta suggest a role for ADAMTS genes in spontaneous preterm birth. Hum Mol Gen 81 (2019): 84-95.
- Tuttlies F, Keckstein J, Ulrich U, et al. ENZIAN-Score, eine Klassifikation der tief infiltrierenden Endometriose. Zentralbl Gynakol 127 (2005): 275-282.
- Haas D, Oppelt P, Shebl O, et al classification. Does it correlate with clinical symptoms and the rASRM score? Acta Obstet Gynecol Scand 92 (2013): 562-566
- Clavien P, Sanabria J, Strasberg S. Proposed classification of complications of surgery with examples of utility in cholecystectomy. Surgery 111 (1992): 518-526
- Dindo D, Demartines N, Clavien P. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240 (2004): 205-213.
- Clavien P, Barkun J, de Oliveira M, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250 (2009): 187-196.
- Sharma S, Roy Choudhury S, Bathwal S, et al. Pregnancy and live birth rates are comparable in young infertile women presenting with severe endometriosis and tubal infertility. Reprod Sci 27 (2020): 1340-1349
- Lin H, Leng J, Liu J, Lang J. Obstetric outcomes in Chinese women with endometriosis: a retrospective cohort study. Chin Med J 128 (2015): 455-458.
- Nybo Andersen A, Wohlfahrt J, Christens P, Olsen J. Maternal age and fetal loss: population based register linkage study. BMJ 320 (2000): 1708-1712.
- Pandey S, Shetty A, Hamilton M, et al. Obstetric and perinatal outcomes in singleton pregnancies resulting from IVF/ICSI: a systematic review and meta-analysis. Hum Reprod Update 18 (2012): 485-503.
- Macfarlane A, Blondel B, Mohangoo A, et al. Wide differences in mode of delivery within Europe: risk?stratified analyses of aggregated routine data from the Euro-Peristat study. BJOG 123 (2015): 559-568.
- Stephansson O, Kieler H, Granath F, Falconer H. Endometriosis, assisted reproduction technology, and risk of adverse pregnancy outcome. Hum Reprod 24 (2009): 2341–2345
- Conti N, Cevenini G, Vannuccini S, et al. Women with endometriosis at first pregnancy have an increased risk of adverse obstetric outcome. J Mat Fet Neonat Med 28 (2015): 1795-8000
- Glavind MT, Forman A, Arendt LH, et al. Endometriosis and pregnancy complications: a Danish cohort study. Fertil Steril 107 (2017): 160-166.
- Allerstorfer C, Oppelt P, Enzelsberger S H, et al. Delivery after Operation for Deeply Infiltrating Endometriosis. BioMed Res Int (2016).
- Ranjana S A. Incidence, causes and feto-maternal outcomes of obstructed labour in a tertiary health care centre. IJRCOG 6 (2017): 2817-2821.
- Leyendecker G, Kunz G, Noe M, Herbertz M, Mall G. Endometriosis: a dysfunction and disease of the archimetra. Hum Reprod Update 4 (1998): 752-762.
- Soriano D, Bouaziz J, Elizur S, et al. Reproductive Outcome Is Favorable After Laparoscopic Resection of Bladder Endometriosis. JMIG (2016): 781-786.
- Federal Statistic Office Germany Press Release #18, 15th of May 2021 https://www.destatis.de/EN/Press/2021/03/PE21_N018_231.html#:~:text=Caesarean%20rate%20almost
%20doubled%20in%20Germany%20since%201991&text=The%20Federal%20Statistical
%20Office%20(Destatis,slightly%20(2018%3A%2029.1%25). - Rossen L M, Ahrens K A, Branum A M. Trends in Risk of Pregnancy Loss Among US Women, 1990-2011. Paediatr Perinat Epidemiol.32 (2018):19-29


 Impact Factor: * 3.2
Impact Factor: * 3.2 Acceptance Rate: 76.63%
Acceptance Rate: 76.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 