Ischemic Stroke; A Severe Complication In Patients Admitted To Resuscitation
Zelmat SA1*, Bouabida D2, Bellalaoui I3, Zaoui C4, Boucherite E3, Mazour F5
1Lecturer A in intensive care anesthesia, EHU d´Oran, Oran, Algeria
2Department of Pediatrics, EHU d´Oran, Oran, Algeria
2Department of Obstetrics and Gynecology, EHU d´Oran, Oran, Algeria
4Faculty of Medicine, EHU d´Oran, Oran, Algeria
5Resuscitation anesthesia specialty, EHU d´Oran, Oran, Algeria
*Corresponding Author: Zelmat Setti Aouicha, Lecturer A in intensive care anesthesia, EHU d´Oran, Resuscitation anesthesia specialty, Oran, Algeria
Received: 09 November 2020; Accepted: 19 November 2020; Published: 01 February 2021
Article Information
Citation: Zelmat SA, Bouabida D, Bellalaoui I, Zaoui C, Boucherite E, Mazour F. Ischemic Stroke; A Severe Complication In Patients Admitted To Resuscitation. Obstetrics and Gynecology Research 4 (2021): 026-033.
View / Download Pdf Share at FacebookAbstract
Stroke is a real public health problem because of its incidence and morbimortality. Ischemic stroke (AVCI) accounts for 80% of strokes. It is the third leading cause of overall mortality in industrialized countries, after heart disease and cancer, and the leading cause of physical disability acquired. The objective of our study was to describe the clinical characteristics, and factors of Cardiovascular Risk (LRIF) and the factors associated with death in patients admitted for stroke (AVCI) and them in a resuscitation ward.
Methods: Retrospective study over a 12-month period (between January 1, 2018 and January 1, 2019), conducted in the medical-surgical emergency room.
Results: A total of 147 strokes: 110 AVCI (84%). The age of the patients included in the study ranged from 49 to 77 years. The average age was 66 years - 10.9 years, 75% of AVCI occurring after 65 years. Sex divided into 47 women (42.72%). And 63 men (57.28%). Ischemic strokes: The main vascular risk factors three risk factors: severe high blood pressure (0.007), diabetes (0.05) and emboligenic heart disease (0.017). Other risk factors found are tobacco (13.09%), obesity (10.7%), dyslipidemia (08.3%), alcohol (7.1%). 17, 8% of patients had a history of formed stroke or TIA (Table 1). The onset of neurological symptomatology was brutal in 70% (77 patients). The clinical examination at admission found consciousness disorders with a NIHSS score of 5 to 15 in 45.54% of cases (49 patients). 23 patients (20.9%) had a NIHSS score of 15 and 39 patients (35.45). Para clinical cardiac evaluation (ECG, Echocoeur) objective a complete arrhythmia by atrial fibrillation (AC/FA) in 11.4% of cases, left atrial hypertrophy in 40% of cases and left ventricular hypertrophy in 89% of cases. The length of hospitalization in resuscitation ranged from 1 to 46 days with an average of 13.4 days (-10.1). Among the 110 patients 22 died or (20%). Three risk factors associa
Keywords
<p>Ischemic stroke</p>
Article Details
1. Introduction
1.1 Definition
Stroke is a sudden onset focal neurological deficit (onset in less than 2 minutes) in relation to a brain parenchyma lesion by heart attack or hemorrhage secondary to a cerebral vascular pathology of arterial or venous origin the first cause of acquired motor impairment in the adult.The third leading cause of death after cardiovascular disease and cancer. On distinguish 2 type of stroke 1 stroke [1, 2, 3, 4]. schemic (85% of cases) composed of
- Transient ischemic infarction and
- ischemic infarction consisting of
And hemorrhagic stroke (15% of cases)
- Bleeding in the brain
- Cerebral thrombophlebitis
1.2 Gravity scores
1.2.1 NIHSS Score:
Minor stroke: NIHSS 1-4
Major stroke: NIHSS 5-15
Severe stroke: NIHSS top 15
Allows:
- Quantify neurological deficit.
- Assess the initial severity of patients.
If the NIHSS score is 15: there is a high probability of having a poor prognosis in 3 months.
1.2.2Glascow score: A severe stroke is a stroke whose SCORE of NIHSS -15 AND GLASCOW-lt; 9.
1.2.3Risk Factors: [5] The risk factors for IVUS differ from those of hemorrhagic strokes, although some of them are common both.It is classic to separate riskfactors into modifiable and non-modifiable factors.
1.3 Non-modifiable risk factors
Non-modifiable risk factors are generally common between AVCI and hemorrhagic.
1.3.1 Age:It is the most powerful: after age 55, the risk of stroke doubles every.
1.3.2 Sex:[6] Male does not appear to be a major factor in the occurrence of a stroke unlike coronary heart disease, but the data are divergent.However, the incidence of stroke is higher in men than in women.However, because of the higher life expectancy for women, the absolute number of strokes is higher for women than for men.
1.3.3 Ethnic factors:Have also been identified.For example, the Manhattan registry showed twice as high an incidence of IC and CI in individuals of African and Hispanic descent as among Caucasians In addition, the incidence of HFCs is higher among Asian.Socio-economic and cultural factors may be responsible for differences in the prevalence of risk factors observed in these populations, as well as genetic variations that have yet to be identified. A paternal or maternal family history of strokedoubles therisk.Apart from the rare monogenic diseases, there may be complex interactions with sex, unexplained by conventional genetic transmission.For example, women with a transient IC or ischemic accident (TIA) were more likely to have a maternal than paternal history of stroke, while in men, maternal and paternal history had the same prevalence.
1.4 Changeable risk factors
1.4.1 Cerebral infarction: [7] High blood pressure and metabolic factors: High blood pressure (HTA) is the most common risk factor found in CI patients.The relationship between blood pressure and stroke risk exists from the blood pressure values of 115/75 mm Hg (systolic/diastolic), and it is loglinerary.Indeed, each increase in systolic blood pressure of 20 mm Hg or diastolic blood pressure of 10 mm Hg is associated with a doubling of the risk of stroke, regardless of age.
1.4.2 Type 2 diabetes: [8] Is a well-established risk factor for AVCI that increases the risk by a factor ranging from 1.8 to 6.
1.4.3 Hyper cholesterolemia:[9] HDL cholesterol is a very high protein fraction, especially ApoA1.There is an inverse relationship between HDL cholesterol levels and IC risk that may be higher in atherosclerosis-related accidents.
1.5 The role of tobacco and alcohol [10, 11]
- A meta-analysis of 32 studies showed that smokers had a nearly two-fold risk of IC.
- A meta-analysis of 35 observational studies showed that regular alcohol consumption greater than 60 g per day is associated with an increased risk of IC.
1.6 Contraception and hormone replacement therapy [12]
The role of female hormones in the occurrence of cerebrovascular pathology has also been studied.Thus, oral contraception is associated with an increased risk of ICwith a relative risk of between 2 and 4. For example, the risk of cerebral infarction due to atrial fibrillation also increases significantly with age, from 1.5% in subjects aged 50 to 59 to 23.5% in the 80-89age group.
2. Materials and Methods
2.1 Type and study period
This is aretrospective, descriptive study, conducted in the medical and surgical emergency room (UMC) over a 12-month period (January 2018 and January 2019).
2.2 Inclusion criteria
Being hospitalized during the UMC study period for an ischemic stroke defined according to WHO criteria.
2.3 Exclusion criteria
- TransitionalIschemic Accident
- Hemoragic Stroke
- Aneurological deficit in relation to a head injury or a brain tumor or other cause.
2.4 Variables studied
Sociodemographic (age, sex,), risk factors clinics at
admission (NIHSS score, glascow scores), hospitals (hospital duration, complication, management), prognostics.
2.5 Data analysis and application of statistical tests
Descriptive data analysis is based on transforming variables: by grouping using either coding or conditional transformations for tabulation and analysis.
2.5.1 Univariate analysis: The descriptive analysis of the variables is done by calculating the frequencies, central tendency or dispersion characteristics: the mean (m), the median (me), the variance (σ2), standard deviation (σ) as well as the determination confidence intervals (95% CI) around the mean, and the median (me) for the risk α = 0.05 for the quantitative variables. Determination of frequencies and confidence intervals for qualitative variables. The confidence interval around the mean is presented by the Standard Deviation around the mean (mean ± SD).
2.5.2 Bivariate analysis: It is used to find the association between two independent variables, or between a dependent variable (to be explained) and other independent (explanatory) variables. The tests used are: the ?² test for independence or homogeneity, corrected by YATES, the exact test by FISHER, the KRUSKALL-WALLIS test for two groups, with the determination of the significance levels. STUDENT's test for two independent samples and analysis of variance (ANOVA) were used for the comparison of variables continuing. For the bivariate analysis, the comparison of interrupts variables between groups was carried out by non-parametric tests, the conformity and homogeneity test for the search for statistical associations between two qualitative variables; Fisher's exact nonparametric test for comparison of small groups. We used Pearson's correlation tests to estimate the relationship between two quantitative variables. A relationship is considered significant.
3. Result
147 strokes: 110 AVCI (84%)(Figure 1). The age of the patients included in the study ranged from 49 to 77 years.The average age was 66 years - 10.9 years (Figure 2) 75% of AVCI occurring after 65 years. Patients with AVCI are divided into 47 women (42.72%)and 63 men (57.28%) (Figure 3).
3.1 Risk factors
The three main vascular risk factors: severe high blood pressure (P-0.007), diabetes (P -0.05) and emboligen heart disease (P-0.017). Other risk factors were in descending order: tobacco (13.09%), obesity (10.7%), dyslipidemia (08.3%), alcohol (4.1%). 17, 8% of patients had a history of formed stroke or TIA (Table 2).
3.2 TIA :transient ischemic attack
3.2.1 The neurological examination has admission: The clinical examination at admission found consciousness disorders with a NIHSS score of 5 to 15 in 45.54% of cases (49 patients).23 patients (20.9%)had a NIHSS score of 15, and a score of NIHSS-lt; 5 in 39 patients (35.45%)(Figure 4).
3.2.2 The cardiac assessment has admission: Para clinical cardiac evaluation (electrocardiogram and echocoeur) objective a complete arrhythmia by atrial fibrillation (AC/FA) in 11.4% of cases, left atrial hypertrophy in 40% of cases and left ventricular hypertrophy in 79% of cases(Figure 5).
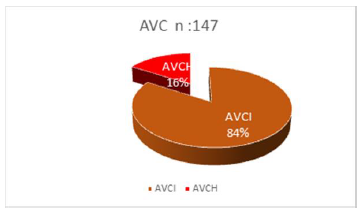
Figure 1: Distribution of patients by type of stroke.
|
Age range |
Staff |
% |
|
More than 35 |
82 |
75 |
|
75 and Under |
28 |
25 |
|
Total |
110 |
100 |
Table 1: Breakdown of Patients by Age Group.
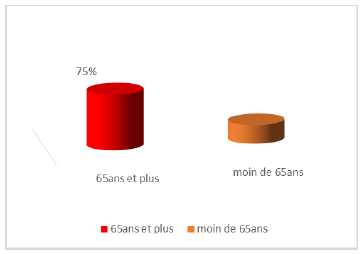
Figure 2: Distribution of patients by age.
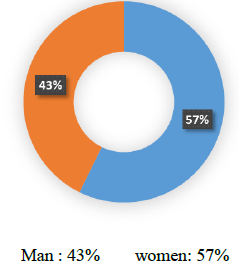
Figure 3: Distribution of patients by sex.
|
Risk factors |
% |
|
History of TIA or TIA |
17,8 |
|
Tobacco |
13,09 |
|
Obesity |
10,7 |
|
Dyslipidemia |
8,3 |
|
Alcohol |
4,1 |
Table 2: Risk Factors.
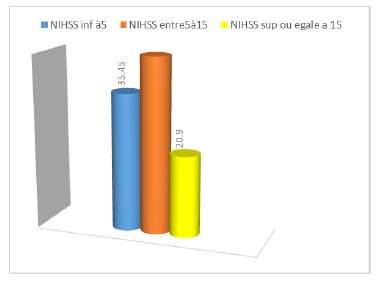
Figure 4: Percentage of Patients by NIHSS Score.
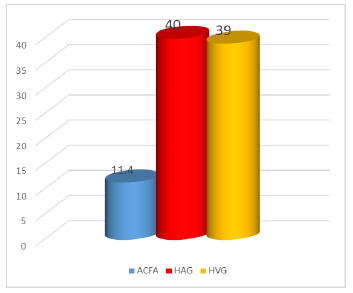
Figure 5: Percentage of patients by cardiac assessment at admission.
4. Discussion
4.1 Age
According to the literature, Elderly people are particularly vulnerable to stroke when atrial fibrillation
is present [13], the frequency of strokes after 65 years
is tripled [14, 15], this agrees with our study.
4.2 Sex
The incidence of DALY was also higher in men than in
women, according to the literature [16, 17]. the majority
of studies were in favor as well as a female preponderance with ratios between 0.82 and 0.97 [18].
4.3 Risk factors
The main risk factors of our study were significant:
arterial hypertension, diabetes, cardiac embolism, for others the risk factors considered significant in several studies that we did not find such as, tabas, obesity, dyslipidemia, and alcohol. Hypertension as the main risk factor is described everywhere [19, 20].
4.4 Mortality rate
In our study, the mortality was 20%. This is consistent with most studies which have reported that the disparity in this rate is significant around the world with figures ranging from 10 to 30% [1]. Three risk factors associated with the poor prognosis: NHISS - 15 (p - 0.0001), anisocoria (p - 0.006) and long stay in intensive care (p - 0.013) our results are consistent with the literature because several authors have observed that: Anisocoria is considered to be a potentially fatal bad factor reflecting brain engagement [16, 19]. The most reliable neurological parameter of mortality is the NIHSS awareness score by the NIHSS score. Indeed [21].
5. Conclusion
Stroke is a major public health problem.Cardiovascular risk factors are dominated by HTA, diabetes and embologenous heart disease. Cardiovascular assessment (ACFA,HAG,HVG) plays an important role in stroke management. Prevention remains the only effective measure.
This prevention must be primary and secondary and involves the prevention of thromboembolic accidents. Anisocoria and depth of consciousness disorder predisposes to fatal evolution of AVCI
Conflict of Interest
The authors do not declare any conflict of interest.
References
- Leys D, Pruvo JP. Stratégie pratique en urgence face à un accident vasculaire cérébral. Encycl Méd Chir neurologie 7 (2002): 01-10.
- Touzé E, Béjot Y. Épidémiologie analytique. In : Bousser MG, Mas JL, eds. Accidents vasculaires cérébraux. Paris: Doin (2009).
- Rothwell PM, Coull AJ, Silver LE, et al. Population-based study of event-rate, incidence, case fatality, and mortality for all acute vascular events in all arterial territories (Oxford vascular study). Lancet 366 (2005): 1773-1783.
- White H, Boden-Albala B, Wang C, et al. Ischemic stroke subtype incidence among whites, blacks, and Hispanics: the Northern Manhattan Study. Circulation 111 (2005): 1327-1331.
- Béjot Y, Touzé E, Osseby GV, et al. Épidémiologie descriptive. In : Bousser MG, Mas JL, eds. Accidents vasculaires cérébraux. Paris: Doin (2009).
- Touzé E, Rothwell PM. Heritability of ischaemic stroke in women compared with men: a genetic epidemiological study. Lancet Neurol 6 (2007): 125-133.
- Lewington S, Clarke R, Qizilbash N, et al. Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 360 (2002): 1903-1913.
- Stegmayr B, Asplund K. Diabetes as a risk factor for stroke. Diabetologia 38 (1995): 1061-1068.
- Sanossian N, Saver JL, Navab M, et al. High-density lipoprotein cholesterol: an emerging target for stroke treatment. Stroke 38 (2007): 1104-1109.
- Shinton R, Beevers G. Meta-analysis of relation between cigarette smoking and stroke. Br Med J 298 (1989): 789-794.
- Reynolds K, Lewis B, Nolen JD, et al. Alcohol consumption and risk of stroke:a meta-analysis. JAMA 289 (2003): 579-588.
- Chan WS, Ray J, Wai EK, et al. Risk of stroke in women exposed to low-dose oral contraceptives: a critical evaluation of the evidence. Arch Intern Med 164 (2004): 741-747.
- Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 22 (1991): 983-988.
- Lopez AD, Mathers CD, Ezzati M, et al. Global and regional burden of disease and risk factors, 2001. Systematic analysis of population health data 367 (2006): 1747-1757.
- Rozec B, Blanloeil Y, Cinotti R, et al. Accidents vasculaires cérébraux postpér-atoires. Ann Fr Anesth Reanim (2011).
- Carpentier F, Mingat J, Hommesl M. Etude épidémiologique des accidents vasculaires cérébraux admis en un an aux urgences médicales. Réanim Soins Intens Med Urg 6(1990): 47-50.
- Hazim A. Prise en charge des accidents vasculaires cérébraux au milieu de réanimation, Hôpital de koughibga. Thèse Doctorat Médecine, Casablanca 143 (2006).
- Garbusinski JM, van der Sande MA, Bartholome EJ, et al. Stroke presentation and outcome in developing countries: a prospective study in the Gambia. Stroke (2005).
- Mihaela Rusinaru. Identification et prévalence des facteurs de risque de l’accident vasculaire cerebral en médecine générale. Enquête rétrospective dans une unité de soins, d’enseignement et de recherché de médecine ambulatoire en lorraine, de 2000 à 2010, et comparaison à l’étude interstroke. Sciences du Vivant [q-bio] (2010).
- Damorou F, Togbossi E, Pessinaba S, et al. Accidents vasculaires cérébraux (AVC) et affections cardio-vasculaires emboligènes. Mali Méd 23 (2008): 33.
- Leys D, Pruvo J.P. Stratégie pratique en urgence face à un accident vasculaire cérébral. Encyclopédie médico-chirurgicale, Neuro-logie, Tome3,17-046-A-50 (2002): 10.


 Impact Factor: * 3.2
Impact Factor: * 3.2 Acceptance Rate: 76.63%
Acceptance Rate: 76.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 