Physical Rehabilitation Based on International Classification of Functioning, Disability and Health (ICF) Model of a Child with Arthrogryposis Multiplex Congenita
Faruq Ahmed1, Zannatul Mawa2, Mohammad Nazmul Hasan2, Suria Akter1, Md Shujayt Gani2, Chowdhury Muhsinin Mosharofy Aroshi2
1William & Marie Taylor School, Centre for the Rehabilitation of the Paralysed (CRP), Dhaka, Bangladesh
2Departments of Physiotherapy, Centre for the Rehabilitation of the Paralysed (CRP), Savar, Dhaka, Bangladesh
*Corresponding Author: Faruq Ahmed, MSc.PT, Senior Clinical Physiotherapist, Department of Physiotherapy, Centre for the Rehabilitation of the Paralysed (CRP), Dhaka, Bangladesh, [https://orcid.org/0000-0003-0239-0113]
Received: 09 November 2022; Accepted: 15 November 2022; Published: 06 December 2022
Article Information
Citation: Faruq Ahmed, Zannatul Mawa, Mohammad Nazmul Hasan, Suria Akter, Md Shujayt Gani, Chowdhury Muhsinin Mosharofy Aroshi. Physical Rehabilitation Based on International Classification of Functioning, Disability and Health (ICF) Model of a Child with Arthrogryposis Multiplex Congenita. Journal of Pediatrics, Perinatology and Child Health 6 (2022): 502-508.
View / Download Pdf Share at FacebookAbstract
Background: Arthrogryposis Multiplex Congenita (AMC) is a condition used to portray inborn contractures with at least two different body limbs behind a general predominance of 1 out of 3000 at live births. The aim of the study was to provide information about appropriate physical rehabilitation protocol using ICF model for the child with AMC.
Case Description: The reported case for the study was 13 years old girl born with suffering from AMC. During pregnancy period mother had history of malnutrition and prolong labour pain was present and child had deformity at different joints. Child was not able to sit properly except modified cross sitting, stand or walk due to deformities. Patient had no history of operation and serial plaster casts for this deformed condition. She was residential students and attended the inclusive school where he participated in a regular special education program. He took routine based individual physiotherapy, occupational therapy and hippotherapy intervention. The Child and her mother gave consent and agreed to participate in this observational case report study for 12 months. Purposive sampling technique was applied considering the inclusion and exclusion criteria. The research was carried out between July 2021 and June 2022. Measurement tools were used ICF model, prone positioning time, passive ROM and muscle strength. This article enlightens rehabilitation treatment strategies for child with AMC.
Conclusion: Physical therapy of AMC children ought to be multi-focused, continual and holistic. Early way to deal with physiotherapist limits the complexity following AMC. Early physiotherapy treatments can help in delaying the early requirement of surgical management during formative age.
Keywords
<p style="text-align:justify">Physical therapy, Rehabilitation, Arthrogryposis Multiplex Congenita</p>
Article Details
Introduction
Arthrogryposis Multiplex Congenita (AMC) is a non-progressive disorder constituted by numerous prenatal jointcontractures [1]. It is a phrase used to characterize various contractures occurring at birth in at least two body segments with an estimated rate of 1 in 3000 newborns [2]. AMC, which is acronym for numerous curved joints [3], has been recognized as an abnormality since birth. It is a series of congenital disorders with restricted mobility resulting the joints are fixed in flexion or extension direction [4]. Although the contractures are not progressive, they may affect and impede flexibility in mobility, self-care, and daily living activities [5]. This calls for early, comprehensive rehabilitation that includes splinting, strengthening exercises, and range of motion training [6,7].
AMC has a multi factorial and sporadic etiology. Reduced fetal movements may be the most relevant factor [8]. It depends on the kind of inheritance mitochondrial, X-linked, autosomal recessive, or autosomal dominant [9]. AMC's etiology is complicated. The following causes of AMC can be categorized: neuropathy, alteration of muscle structure or function, anomaly of connective tissue, space restriction, maternal illnesses, and reduced intrauterine or prenatal vascularity [10]. As a result of the mother's tiny uterus, it could happen because of joint restriction during fetal growth. The disease can be classified into two primary kinds, neurological or myopathic issues, and the majority of patients experience neurological symptoms [1]. Extrinsic and intrinsic factors, such as prenatal abnormalities, contribute to AMC [9]. For the purpose of differential diagnosis, AMC can be split into three basic groups: illnesses that primarily affect the limbs, those that also affect a few other body regions, and those that also entail dysfunction of central nervous system [11].
The international classification of functioning, disability, and health (ICF) focuses on the links between a person's body structures and functions, activity limitation, participation restriction, personal, and environmental element, in order to maximize function and reduce disability [12]. In a study published by Elfassy et al. (2019) recently child with AMC claimed that their environment, such as the home, school, and community, has an impact on their capacity to participate in meaningful activities and responsibilities [13]. The aim of the study was to provide information about appropriate physical rehabilitation protocol using ICF model for the child with AMC.
Case Presentation
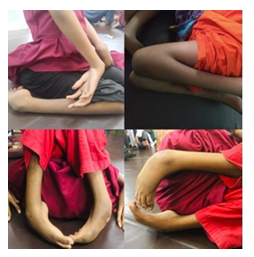
The reported case for the study was 13 years old girl born with suffering from AMC. During pregnancy period mother had history of malnutrition and prolong labour pain was present and child had deformity at different joints. At the time of birth patient had limited joint ROM at cervical spine, both upper limb and lower limb and bilateral Congenital Talipes Equino Varus (CTEV). Child both wrist, hip, knee joint was in flexed position. Child ankle joint was inverted and planter flexed position. Child was not able to sit properly except modified cross sitting, stand or walk due to deformities. Patient had no history operation and serial plaster casts for this deformed condition. Her vision, hearing and cognition status was good.
She was residential students and attended the inclusive school where he participated in a regular special education program. She had weakness of both upper limbs and lower limbs. During the course of the trial, the child used modified wheelchair as assistive device though she needed help to propel wheelchair. She took routine based individual physiotherapy, occupational therapy and hippotherapy intervention. Physiotherapy treatment was directed towards maintenance of range of motion in all joints, strengthening of weak muscles as well as gait training. Occupational therapy was provided for performing smoothly the activity of daily livings and further plan for vocational program according to her conditions.
Ethical Approval
A subject for this case study was recruited from an inclusive school. Approval was obtained from the selected school and from the parent’s willingness to participate in this study. The Child and her mother agreed to participate in this observational case report study for 12 months. Mother also consented for her child and photograph to be published; her face is blocked out for anonymity.
Methods & Materials
The study was conducted in the inclusive school named “William & Marie Taylor School” of CRP. A single subject with repeated-measures design was utilized for evaluation of outcome. Purposive sampling technique was applied considering the inclusion and exclusion criteria. Only participant was selected who matched the criteria specially who are medically diagnosed as AMC. The research was carried out between July 2021 and June 2022. The study was started after the acceptance of protocol; following which data collection was started after getting consent and the study period was over after the submission of the final report.
Eligibility Criteria for Case
Inclusion criteria included enrolled had a medical diagnosis of AMC. She had the consent from parents or guardians, the child is able to follow simple directions, and the child ages between 5 and 14 years. Exclusion criteria were follows severe behavioral and cognitive problems, and had a fever or infection at the time of the initial evaluation.
Outcome measurement
Using a Goniometer, the passive ROM of each joint was measured for the study. A good tool with excellent validity and reliability is Goniometer [14,15]. The baby was kept in the prone position to measure the baby's prone tolerance and restriction was counted by crying or feeling uneasy. Muscle strength is measured using the Modified Oxford Grade scale. In order to maximize function and reduce disability, the international classification of functioning, disability, and health (ICF) emphasizes the interaction between a person's body structures and functions, activity limitation, participation restriction, personal, and environmental elements [12]. The quality and reliability of the acquired data were once more validated. In order to relate variables to the study's objectives, appropriate statistical analysis, calculation, and testing were done.
Evaluation criteria according to ICF Model
In accordance with the ICF (International Classification of Functioning, Disability, and Health) parameters and physiotherapist treatment recommendations that physical therapy care for individuals with AMC often include gentle joint manipulation and massage application consisting of stroking, kneading, picking up and rolling applications, removable splint management for knees and feet to help allow regular muscle movement [16]. Additionally, orthosis procedure can help children with AMC walk and be more independent [17], by preserving muscular tension and strengthening the child's muscles, particularly the quadriceps, hip extensors, rotator cuff muscles, and deltoid anterior, middle, and posterior part, serratus anterior and trapezius muscles [9,16]. It commences a neck, pectoral, elbow, wrist, and finger flexor muscle stretching program for the family to do at home, encourages active muscle use to prevent immobility, and stretches joint and muscle contractures. Stretching is advised daily three to five times with 3-4 repetitions per session, and holding every stretch for 30 seconds [18]. Other treatment modalities in physical therapy for children with AMC include hydrotherapy, hippotherapy, training in the use of assistive devices including a gait instructor, walker, crutches, orthosis, dynamic strengthening of the trunk, and ambulation independently or with an assistive device [16,18].
Presenting ICF model with the case
|
HEALTH CONDITION Arthrogryposis Multiplex Congenita Disease |
||||||
|
BOBY STRUCTURE /FUNCTION (IMPAIRMENTS) |
ACTIVITY (TASKS) |
PARTICIPATION |
||||
|
Abilities |
Limitations |
Abilities |
Restrictions |
|||
|
Reduced ROM of both UEs, LEs & spine |
Eating, writing & dressing UEs with supervision |
Decreased movement of all 4 limbs, |
Schooling & participating in cultural program using wheelchair |
Problem in Transferring |
||
|
Environmental |
||||||
|
Internal |
External |
|||||
|
+ |
- |
+ |
- |
|||
|
Motivated with education & rehabilitation |
Less interest & motivation in grooming |
Good social skill Get support from teachers & therapists |
Accessibility |
|||
Physical intervention AMC, as an uncommon condition, should be used to a integrated, comprehensive therapy approach in every sphere [19]. Rehabilitation should begin as soon as feasible with the fullest team led by a rehabilitation professional, should include physiotherapists, orthotists, nurses, clinical psychologists, counselors, and occupational therapy [10]. To promote joint mobility, physiotherapy procedures such massages and articular mobilization techniques, stretching exercises, corrective kinesio taping, serial cast, and mobilization of the foot using the ponseti method are utilized [20].
Physical therapy goals of a AMC child included increasing joint range of motion (ROM), preventing muscular tightness, and promoting neurosensory and motor development [21]. Patel (2021) asserts that soft massage techniques like kneading, stroking, picking up, and rolling can improve joint mobility. Muscle stretching was applied of 30 seconds hold for thrice a day on each stretch position. Ligaments, capsules, and tendons were released gently by mobilization. Each joint receives 10 repetitions of passive ROM exercises [21].
In order to promote neuro sensory motor development, Patel (2021) states that stimulation of the sucking and rooting reflexes, graded sensory stimulation, visual tracking of musical and lighting toys, various auditory and verbal cues, prone positional awareness, positional treatments, facilitatory rolling, kinesio taping for adjustment, and psychotherapy to the parents were all crucial components of therapy sessions [21]. In this case study, after rehabilitation, an increase in the range of motion of the upper extremity and lower extremities.
|
Joints |
Movements |
Pre Rehabilitation |
Post Rehabilitation |
Differences |
|||
|
Right |
Left |
Right |
Left |
Right |
Left |
||
|
Cervical |
Lateral flexion |
20 |
20 |
25 |
25 |
5 |
5 |
|
Rotation |
30 |
30 |
40 |
40 |
10 |
10 |
|
|
Shoulder |
Flexion |
60 |
60 |
75 |
75 |
15 |
15 |
|
Extension |
10 |
10 |
15 |
15 |
5 |
5 |
|
|
Abduction |
40 |
40 |
45 |
45 |
5 |
5 |
|
|
Med rotation |
25 |
25 |
35 |
30 |
10 |
5 |
|
|
Lat rotation |
NT |
NT |
NT |
NT |
0 |
0 |
|
|
Elbow |
Flexion |
90 |
85 |
100 |
100 |
10 |
15 |
|
Extension |
FROM |
FROM |
FROM |
FROM |
0 |
0 |
|
|
Wrist |
Flexion |
25 |
25 |
30 |
30 |
5 |
5 |
|
Extension |
NT |
NT |
NT |
NT |
0 |
0 |
|
|
Fingers |
Flexion |
40 |
40 |
45 |
40 |
5 |
0 |
|
Extension |
FROM |
FROM |
FROM |
FROM |
0 |
0 |
|
|
Hip |
Flexion |
145 |
145 |
145 |
145 |
0 |
0 |
|
Extension |
NT |
NT |
NT |
NT |
0 |
0 |
|
|
Abduction |
15 |
15 |
20 |
20 |
5 |
5 |
|
|
Knee |
Flexion |
145 |
145 |
145 |
145 |
0 |
0 |
|
Ankle |
Planter flexion |
45 |
45 |
45 |
45 |
0 |
0 |
|
Dorsi flexion |
NT |
NT |
NT |
NT |
0 |
0 |
|
*NT (not testable): Hip lateral rotation, shoulder lateral rotation, wrist, hip and knee extension, and ankle dorsiflexion
Table 1: Measuring the passive ROM of before and after rehabilitation.
In the upper extremities and lower extremities, before physical therapy muscle strength was measured Grade-I and Grade-III respectively. After physical rehabilitation muscle strength was measured in upper extremities and lower extremities at Grade-I and Grade-IV respectively.
|
Extremities |
Prime mover |
Pretest |
Post-test |
Differences |
|
Upper extremities |
Elbow flexor (C5) |
I |
II |
Improved |
|
Wrist flexor (C6) |
NT |
NT |
No changed |
|
|
Elbow extensor (C7) |
NT |
NT |
No changed |
|
|
Little finger flexor (C8) |
I |
II |
Improved |
|
|
Finger abduction (T1) |
I |
II |
Improved |
|
|
Lower extremities |
Hip flexor (L2) |
III |
IV |
Improved |
|
Knee extensor (L3) |
NT |
NT |
No changed |
|
|
Ankle dorsiflexor (L4) |
NT |
NT |
No changed |
|
|
Long toe extensor (L5) |
NT |
NT |
No changed |
|
|
Ankle planter flexor (S1) |
NT |
NT |
No changed |
Table 2: Measuring of muscle strength using modified Oxford Grade scale.
The summery of outcome data of prone positioning time, passive ROM, muscle strength and ICF model evaluation were mentioned according baseline assessment and after 12 months interventions.
|
Tools |
Baseline assessment |
Post-test assessment |
|
Prone positioning time |
60 sec (1 minute) |
150 sec (2.5 minutes) |
|
Passive ROM |
Restricted |
Mild increased |
|
Muscle strength |
UEs: Grade-I LEs: Grade-III |
UEs: Grade-II LEs: Grade-IV |
|
ICF Model |
Restricted joint ROM, social participation and transferring |
Improved environment, social participation and transferring |
UEs: Upper extremities, LEs: Lower extremities.
Table 3: Summary of outcome data.
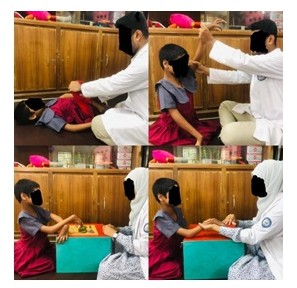
After rehabilitation, our patient has become able to perform fine motor skills such as bilateral use, in hand manipulation, symmetrical use, holding objects, releasing an object, and button fastening with moderate support. After rehabilitation improved gross motor function like rolling, side lying, lying to sitting, modified sitting, wheelchair propel as a mobility purpose with supervision. Child has observed improved brushing, eating with supervision, bathing with mild support, toileting with moderate support and writing with modified independent after rehabilitation.
Discussion
AMC is an uncommon and diverse illness. Children with AMC should be treated using an interdisciplinary approach to problem-solving. Rehabilitation specialists are more worried while treating children with AMC due to the paucity of research on treatment techniques for children with AMC [22]. This case report provides information on rehabilitation strategies for a child with AMC.
The purpose of this type of rehabilitation is to improve the baby's neuro-developmental stimulus and joint range of motion. While reducing the risk of joint dislocation, this modest treatment enables training advancement. Physical treatment is crucial to their independence for kids with AMC. A recent assessment of AMC trials reveals that no literature precisely states the specifics of a given therapy session [22]. In this report, we tried to provide appropriate treatment for the child with AMC.
Studies have been advised for children with an AMC diagnosis, physiotherapy and occupational therapy to improve postural muscular strength, maximal mobility, and motor capacity for age-appropriate tasks. Compensatory devices (splints, adaptive equipment) are necessary if a patient with AMC is unable to hold things, cannot provide residential hygiene, and has eating difficulties [22].
It was intended to minimize knee and hip flexor rigidity with 2 repetitions of 30 seconds stretches to every tightened joint, and with neck stretches, wrist night splints, elbow dynamic splints, prone positioning maintain properly. A case described that elbow flexion limitation was caused by extension contracture [23]. Family training was used in our study as a form of physical therapy to delay the progression through stretching, muscle strengthening, and motor ability facilitation to increase joint range of motion and muscle strength in the extremities.
In a case report that was published, Patel (2021) described the length, frequency, and outcomes of physiotherapy for a baby girl with AMC from the time she was 15 days old until she was 11 months old. They have made sure to increase ROM patency in physiotherapy, to preserve muscular tension, and to promote neuro-sensory development of motor skills in examinations using the ICF framework [21]. In our case study, the aim of the study was to provide information about appropriate physical rehabilitation protocol specially increasing joint ROM, muscle strength, mobility, and fine and gross motor functional ability using ICF model for the child with AMC.
Conclusion
Arthrogryposis multiple congenita is uncommon non-progressive neonatal condition. Although it cannot be cured, the kid can be made as independent as possible by undergoing numerous corrective procedures and receiving physiotherapy. If physical therapy is administered effectively after surgery, the child will eventually have a higher quality of life. It is vital to provide rehabilitation for kids with rare disorders like AMC. It must also assist the child and his or her family to engage in society.
Early physical therapy intervention lowers problems such muscular atrophy, muscular weakness, and contracture. Interventions in physical therapy can postpone the need for surgery in young AMC children. It is necessary to conduct further study to assist establish more uniform guidelines for the rehabilitation of children with AMC.
Compliance with Ethical guidelines:
This article paid attention to all ethical concepts.
Conflict of Interest:
Authors declared that there was no competing of interest.
Funding Information:
Fully self-funded research was done.
Author contribution:
All authors contributed in preparing write up, revising article & giving final approval of the version to be published. Authors consent to accept responsibility for all contents of the tasks.
Acknowledgement:
The authors would like to appreciate the William & Marie Taylor School, Centre for the Rehabilitation of the Paralysed(CRP), Savar, Dhaka, Bangladesh.
References
- Binkiewicz-Glinska A, Sobierajska-Rek A, Bakula S, et al. Arthrogryposis in infancy, multidisciplinary approach: case report. BMC pediatrics (2013) 13: 1-6.
- Bamshad M, Van Heest AE, Pleasure D, et al. Arthrogryposis: a review and update. The Journal of Bone and Joint Surgery. American volume (2009) 91: 40.
- Fixsen J, Benson M, Fixsen J, et al. Arthrogryposis multiplexcongenita. Childrens Orthopaedicsand Fractures, third Edition (2010) 327-334.
- Rink BD. Arthrogryposis: a review and approach to prenatal diagnosis. Obstetrical & gynecological survey. (2011) 66: 369-377.
- Amor CJ, Spaeth MC, Chafey DH, et al. Use of the Pediatric Outcomes Data Collection Instrument to evaluate functional outcomes in arthrogryposis. Journal of Pediatric Orthopaedics (2011) 31: 293-296.
- Bernstein RM. Arthrogryposis and amyoplasia. JAAOS-Journal of the American Academy of Orthopaedic Surgeons (2002) 10: 417-424.
- Södergård J, Hakamies-Blomqvist L, Sainio K, et al. Arthrogryposis multiplex congenita: perinatal and electromyographic findings, disability, and psychosocial outcome. Journal of Pediatric Orthopedics. Part B. (1997) 6: 167-171.
- Hall JG. Arthrogryposis multiplex congenita: etiology, genetics, classification, diagnostic approach, and general aspects. Journal of Pediatric Orthopedics. Part B (1997) 6: 159-166.
- Greggi T, Martikos K, Pipitone E, et al. Surgical treatment of scoliosis in a rare disease: arthrogryposis. Scoliosis (2010) 5: 1-1.
- Binkiewicz-Glinska A, Wierzba J, Szurowska E, et al. Arthrogryposis multiplex congenital-multidisciplinary care-including own experience. Dev Period Med (2016) 20: 191-196.
- Hall JG. Arthrogryposis multiplex congenita: etiology, genetics, classification, diagnostic approach, and general aspects. Journal of Pediatric Orthopedics. Part B (1997) 6: 159-166.
- World Health Organization. Towards a common language for functioning, disability, and health: ICF. The international classification of functioning, disability and health (2002).
- Elfassy C, Darsaklis VB, Snider L, et al. Rehabilitation needs of youth with arthrogryposis multiplex congenita: Perspectives from key stakeholders. Disability and Rehabilitation. (2020) 42: 2318-2324.
- Norkin CC, White DJ. Measurement of joint motion: a guide to goniometry. FA Davis; (2016).
- Kolber MJ, Hanney WJ. The reliability and concurrent validity of shoulder mobility measurements using a digital inclinometer and goniometer: a technical report. International journal of sports physical therapy (2012) 7: 306.
- Bartonek Å. The use of orthoses and gait analysis in children with AMC. Journal of Children's Orthopaedics. (2015) 9: 437-447.
- Lake AL, Oishi SN. Hand therapy following elbow release for passive elbow flexion and long head of the triceps transfer for active elbow flexion in children with amyoplasia. Journal of Hand Therapy. (2015) 28: 222-227.
- Campbell SK, Palisano RJ, Orlin MN, et al. Physical therapy for children. 4th ed. St.Louis, MO: Elsevier/Saunders (2012): 313-332.
- Sykut-Cegielska J, Bozkowa K. Why the rare diseases becometo be a challenge for medicine of today?Developmental Period Medicine (2015) 19: 401-402.
- Binkiewicz-Glinska A, Sobierajska-Rek A, Bakula S, et al. Arthrogryposis in infancy, multidisciplinary approach: case report. Bmc Pediatrics (2013): 13.
- Patel V. Role of Early Rehabilitation in An Infant with Arthrogryposis Multiplex Congenita: A Case Report with 11 Months of Follow up. Indian Journal of Physiotherapy and Occupational Therapy (2021) 15: 134-140.
- Calisgan E, Akyol B. Current concepts in physiotherapy and rehabilitation protocol for arthrogryposis multiplex congenita: An unusual case report.
- Azbell K, Dannemiller L. A case report of an infant with arthrogryposis. Pediatric Physical Therapy (2015) 27: 293-301.


 Impact Factor: * 4.8
Impact Factor: * 4.8 Acceptance Rate: 69.70%
Acceptance Rate: 69.70%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 