Un Unbelievable Intradural Extramedullary Metastasis from a Uterine Leiomyosarcoma: The First Case and Review of Literature
Marinaccio M1, Giannoccaro A1, Marzullo A2, d’Amati A2, Messina R3, de Gennaro L3, Cicinelli E1, Mastronardi M1
1 Interdisciplinary Department of Medicine, AOU Consorziale Policlinico, Bari, Italy
2 Department of Emergency and Organ Transplantation, Section of Pathology, University of Bari “Aldo Moro”, 70124 Bari, Italy.
3 Division of Neurosurgery, Department of Translational Biomedicine and Neurosciences (DiBraiN), University “Aldo Moro” of Bari, Bari, Italy, UE
*Corresponding Author: Marco Marinaccio, Interdisciplinary Department of Medicine, University Medical School of Bari, Apulia, Italy.
Received: 23 March 2023; Accepted: 28 March 2023; Published: 04 May 2023
Article Information
Citation: Marinaccio M, Giannoccaro A, Marzullo A, d’Amati A, Messina R, de Gennaro L, Cicinelli E, Mastronardi M. Un unbelievable intradural extramedullary metastasis from a uterine leiomyosarcoma: the first case and review of literature. Obstetrics and Gynecology Research. 6 (2023): 139-142.
View / Download Pdf Share at FacebookAbstract
Uterine leiomyosarcoma is a rare malignancy with poor prognosis that occurs during pre- and peri-menopause. Metastatic spread in uterine leiomyosarcoma is common, but intradural spinal cord metastases is a very rare event, and, for this reason, there is no standard treatment. We report the case of a 58-years-old woman with onset symptoms related to intradural extramedullary metastasis and no gynecological signs. She underwent dorsal laminectomy followed by chemotherapy with gemcitabine and docetaxel and radiotherapy. Although she is suffering from a very serious illness, she is currently in good general condition. Some studies believe that the mutation of HRD and BRCA will be a therapeutic target in the future
Keywords
<p>Uterine Leyomiosarcoma, Intradural Metastasis, Chemotherapy</p>
Article Details
1. INTRODUCTION
Uterine leiomyosarcoma represents only 1% of all uterine malignancies, but implies a poor prognosis in most cases. It often occurs during pre- and peri-menopause, with an annual diagnosis range from 2.0 to 12.8 per 1000 reproductive-age women. Based on the literature, the FDA reported that 1 in 352 women have unsuspected uterine sarcoma while undergoing surgery for presumed benign leiomyoma [2]. The relative rarity of this kind of neoplasm together with its pathological diversity, poses a challenge in defining a good management. Signs and symptoms of leiomyosarcoma include abnormal vaginal bleeding (56%), palpable pelvic mass (54%) and pelvic pain (22%) [3].
Survival rates depend on the stage of disease at diagnosis. The five-year survival rate is 50-55% for stage I and 8-12% for stage II-IV [4].
2. CASE REPORT
The patient is gravida 3, para 2; BMI 26.3 kg/m2. Absence of risk factors for inherited malignancies. Her clinical history was significant for episodes of AUB from August 2021, but US examination was inconclusive. In September 2021 she suffered from paraesthesia of the lower limbs and, for this reason, she was admitted to the neurosurgery ward and underwent spinal MRI showing the presence of intradural extramedullary pathological tissue inside the spinal canal at levels T2-T4 and S1. (Fig.1).
She underwent dorsal laminectomy extended from D2 to D4, under general anesthesia, performed with the aid of piezosurgery. Piezosurgery technology improves posterolateral exposure of the lesion and it is less invasive, thanks to the “cold cut” with reduced heat development and reduced bone necrosis. Once the lamina was bilaterally removed, the extradural lesion appeared wrapped around the spinal cord, causing a wide compression on the dorsal surface of the dural sac. A piecemeal resection was favored by curettes and ultrasound aspirator, in order to obtain a progressive decompression of the spinal cord. The same procedure was repeated at level S1, where the spinal MRI showed a second lesion. At the end, a significant decompression of the dural sac was obtained (Fig.2).
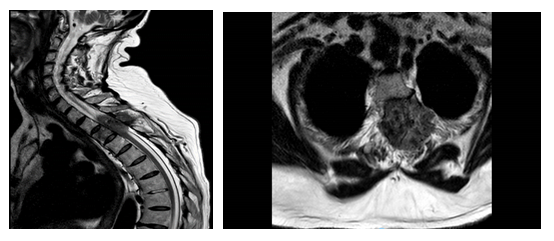
Fig 1: Preoperative spinal MRI. Sagittal and axial T2 weighted images, showing an intradural extramedullary lesion at level T2-T4. The lesion infiltrates the spinal canal posterolaterally on the left side, originating from the paravertebral tissue
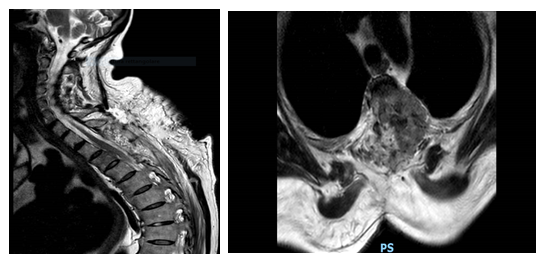
Fig 2: Postoperative spinal MRI. Sagittal and axial T2 weighted images showing the laminectomy at level T2-T4 with decompression and riexpansion of the spinal cord.
The histological analysis revealed the presence of multiple malignant mesenchymal nodules, infiltrating the vertebral bone and the paravertebral soft tissues (Fig.3). The neoplasm was hypercellular and composed of fascicles of malignant smooth cells and numerous zones of necrosis (Fig.4), The cells showed elongated shape, abundant eosinophilic cytoplasm, a high mitotic index (>20/10HPF) and marked nuclear atypia (Fig.5).
Immunohistochemistry revealed positivity for smooth muscle actin (Fig.6) and a very high proliferative index (>90%), calculated with Ki67 staining (Fig.7).
According to the patient’s medical history and to the histological features, a diagnosis of leiomyosarcoma metastasis was made.
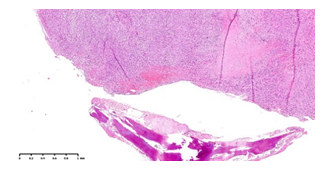
Fig 3: Malignant mesenchymal neoplasm, in close proximity to the bone (HE, 2.5x)
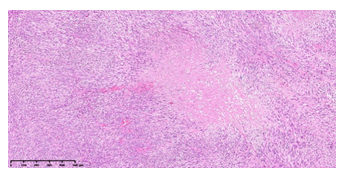
Fig 4: Fascicles of malignant smooth cells, waving around a zone of tumoral necrosis (HE, 10x)
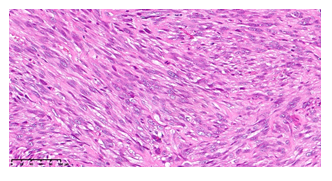
Fig 5: Neoplastic cells showing marked nuclear atypia and many mitoses, some of them atypical (HE, 20x)
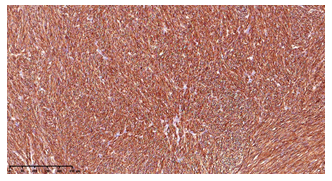
Fig 6: Neoplastic cells showing intense and diffuse positivity for SMA (10x)
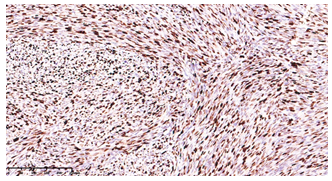
Fig 7: Very high proliferative index, assessed with Ki67 (10x)
Later she performed total body CT that highlighted “voluminous inhomogeneous solid formation of probable heterologous nature of uterine origin with a diameter of 11x8.5 cm which marks the bottom of the bladder. In both lungs nodular formations with random distribution of probable heterologous nature. In the subcutis of the anterior wall of the left pelvis and in the right inguinal area two solid nodular formations with a maximum diameter of 18 mm”
Due to this imaging finding we decided to offer the patient chemotherapy with gemcitabine and docetaxel. The patient underwent six cycles of therapy until February 2022.
In January 2022 the patient underwent a total body CT scan which documented in correspondence with the aforementioned surgery site “in the left paramedian area presence of solid tissue that undergoes enhancement after contrast and involves the peduncles and transverse processes of D2, D3 and D4 vertebrae with the relative ipsilateral costovertebral joints. The same affects the ipsilateral apicodorsal parietal pleura, extends into the vertebral canal and is to be referred to disease recurrence. Further solid tissue is present at level D11-D12. Apparent slight reduction of the known uterine lesion. Two solid nodal formations in the subcutaneous tissue at the right frontal level which are to be referred to secondarisms”.
In March 2022 the patient then underwent radiotherapy for consolidation after laminectomy and, after radiotherapy, she underwent removal of the neoformations of the scalp. Histological examination of these lesions showed "dual secondary cutaneous and subcutaneous localization of well differentiated leiomyosarcoma".
In May 2022 a control CT scan was performed which showed stability of the disease. The patient was then offered to resume chemotherapy with gemcitabine and docetaxel.
Another CT scan was performed in July 2022 which showed an increase in the number and volume of secondary lesions for which the patient underwent chemotherapy with epirubicin.
In November 2022 another CT scan showed an increase in uterine mass which caused hydronephrosis for which the patient underwent ureteral stent placement.
An MRI of the spine was also performed which showed an increase in spinal lesions for which the patient underwent two sessions of radiotherapy.
The patient is currently receiving pazopanib chemotherapy. She is in good clinical condition and continues to perform physiotherapy to strengthen the lower limbs and back.
3. REVIEW FROM LITERATURE
The literature search was conducted using Medline / PUBMED (key words: uterine leyomiosarcoma AND intradural, extramedullary, spinal, cord, dura, meningeal); review conducted according to the “PRISMA statement” from the date of the foundation (1960) [8].Eighty articles from 1976 to 2022 were retrieved from database search. The first screening by abstract excluded 69 articles non-focused on metastases of uterine leiomyosarcoma to the spine and spinal cord. From the remaining 13 articles we excluded 9 papers in which metastases to the vertebrae were reported. A total of 2 patients with extramedullary/extradural and intramedullary are described in the included papers.
Table 1: The two patients with extramedullary/extradural and intramedullary
4. DISCUSSION
Standard treatment in localized disease is abdominal hysterectomy. Bilateral salpingo-oophorectomy and lymphadenectomy have no proven value in leiomyosarcomas and high-grade undifferentiated sarcomas [5]. Preservation of the ovarian function may be an option for premenopausal women with stage I disease [6]. In metastatic disease, the role of surgery depends on the patients’ general conditions, the extent of disease and treatment goals. Pulmonary metastasectomy is performed with good results [7].
Metastatic spread in leiomyosarcomas is common, usually to lungs, liver, brain and bones, but metastasis to spinal cord is a very rare event [9].
Leiomyosarcoma metastases to spinal column can be extra spinal as well as intraspinal but rarely penetrate the dura (9). In this case, as often happens, the onset symptoms were related only to the metastatic localization. In fact, our patient underwent neurosurgery in order to obtain vertebral decompression and histological diagnosis.
Cases of intradural spinal cord metastases from a leiomyosarcoma are a very rare event, in fact very few similar cases are reported in literature and, for this reason, there is no standard treatment. The main treatment is surgical decompression and resection, followed by adjuvant radiation therapy and chemotherapy (doxorubicin/ifosfamide, docetaxel/gemcitabine) depending on the stage and the features of the tumor [10]. Our patient underwent radiation therapy and chemotherapy because of the advanced stage of the disease, with development, however, of numerous side effects. She also benefitted from physiotherapy.
Recent molecular biology studies have highlighted that HRD and BRCA mutations may be the most promising therapeutic target for uterine leiomyosarcomas, but the question is still a source of study [11].
REFERENCES
- Juhasz-Böss I, Gabriel L, Bohle R, M, Horn L, C, Solomayer E, -F, Breitbach G, -P: Uterine Leiomyosarcoma. Oncol Res Treat 2018; 41: 680-686.
- Mao J, Pfeifer S, Zheng XE, Schlegel P, Sedrakyan A. Population-Based Estimates of the Prevalence of Uterine Sarcoma Among Patients With Leiomyomata Undergoing Surgical Treatment. JAMA Surg. 2015; 150(4): 368-370.
- Kaur K, Kaur P, Kaur A, Singla A. Uterine leiomyosarcoma: A case report. J Midlife Health. 2014 Oct;5(4): 202-204.
- Omar M. Salazar, Margaret E. Dunne, The role of radiation therapy in the management of uterine sarcomas, International Journal of Radiation Oncology*Biology*Physics, Volume 6, Issue 7, 1980, Pages 899-902.
- Reichardt P. The treatment of uterine sarcomas. Ann Oncol. 2012 Sep;23 Suppl 10:x151-157.
- El-Khalfaoui, K., du Bois, A., Heitz, F., Kurzeder, C., Sehouli, J., & Harter, P. (2014). Current and future options in the management and treatment of uterine sarcoma. Therapeutic advances in medical oncology, 6(1); 21–28.
- Amant F, Lorusso D, Mustea A, Duffaud F, Pautier P. Management Strategies in Advanced Uterine Leiomyosarcoma: Focus on Trabectedin. Sarcoma. 2015; 2015: 704124.
- Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009 Jul 21; 339: b2700.
- Tan LA, Kasliwal MK, Nag S, O'Toole JE. A rare intramedullary spinal cord metastasis from uterine leiomyosarcoma. J Clin Neurosci. 2013 Sep; 20(9): 1309-1312.
- Shirzadi A, Drazin D, Shirzadi N, Westhout F, Drazin N, Fan X, Acosta FL. Metastatic Leiomyosarcoma to the Spine Complicated With Thrombocytopenia. World J Oncol. 2012 Aug;3(4):182-186.
- Asano H, Isoe T, Ito YM, et al. Status of the Current Treatment Options and Potential Future Targets in Uterine Leiomyosarcoma: A Review. Cancers (Basel). 2022; 14(5): 1180. Published 2022 Feb 24.


 Impact Factor: * 3.2
Impact Factor: * 3.2 Acceptance Rate: 76.63%
Acceptance Rate: 76.63%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 