Cervical Cancer Screening Practice using Smear Test Method in the Northwestern Algeria
Article Information
Leila Isràa Boukabene, Zoulikha Masmoudi, Mustapha DIAF*
Department of Biology, Faculty of Natural and Life Sciences, Djillali Liabes University, Sidi-bel-Abbes, Algeria
*Corresponding author: Mustapha DIAF, Department of Biology, Faculty of Natural and Life Sciences, Djillali Liabes University, Sidi-bel-Abbes, Algeria
Received: 03 January 2020; Accepted: 17 January 2020; Published: 20 January 2020
Citation:
Leila Isràa Boukabene, Zoulikha Masmoudi, Mustapha DIAF. Cervical Cancer Screening Practice using Smear Test Method in the Northwestern Algeria. Archives of Internal Medicine Research 3 (2020): 061-068.
View / Download Pdf Share at FacebookAbstract
Background and objective: Cervical cancer is a major public health burden, in Algeria; it represents the second most common cancer in women. The main factor leading to invasive cervical cancer is the lack of Pap smear practice. The aim of the present study is to evaluate the cervical cancer screening activities by cervical smears in the northwestern region of Algeria.
Methods: a retrospective study was performed from 2015 to 2017 in the Wilaya of Sidi-Bel-Abbès, the northwest region of Algeria. A total of 266 cervicovaginal smears were collected during the study period.
Results: among the 266 cervical smears performed during the study period; 69.54% were first cervical smears, 22.55% were performed for the second time and 7.89% for the 3rd. The highest rate was recorded in 2017. The most represented age groups for the first cervical smear were [35-39 years], [40-44 years] and [45-49 years]. The cervical smears adequate for the interpretation were the majority whether for the first, the second or the third cervical smears. However, cervical smears not satisfactory for interpretation represented lower rates. Out of all the samples, 17.85% of the cervical smears carried out in 2015, 46.59% in 2016 and 18.40% in 2017 were normal. Moreover, no presence of intra-epithelial lesions has been reported. Epithelial abnormalities of low grade were observed on 3.4% of 1st and 2nd cervical smears done in 2016 and on 0.8% of 1st and 1.6% of 2nd smears performed in 2017. The most frequent recommendations were to redo cervical smears during the 6 months following the previous test; 35.71% in 2015, 47.67% in 2016 and 57.25% in 2017. However, performing a colposcopy or biopsy ware the less frequent as recommendations.
Conclusion: Cervical cancer occupies the second position of female cancers in Algeria. Its screening reaches a limited rate of target female populat
Keywords
Cervical cancer, Pap smear, Screening, Wilaya of Sidi-Bel-Abbès
Cervical cancer articles Cervical cancer Research articles Cervical cancer review articles Cervical cancer PubMed articles Cervical cancer PubMed Central articles Cervical cancer 2023 articles Cervical cancer 2024 articles Cervical cancer Scopus articles Cervical cancer impact factor journals Cervical cancer Scopus journals Cervical cancer PubMed journals Cervical cancer medical journals Cervical cancer free journals Cervical cancer best journals Cervical cancer top journals Cervical cancer free medical journals Cervical cancer famous journals Cervical cancer Google Scholar indexed journals Pap smear articles Pap smear Research articles Pap smear review articles Pap smear PubMed articles Pap smear PubMed Central articles Pap smear 2023 articles Pap smear 2024 articles Pap smear Scopus articles Pap smear impact factor journals Pap smear Scopus journals Pap smear PubMed journals Pap smear medical journals Pap smear free journals Pap smear best journals Pap smear top journals Pap smear free medical journals Pap smear famous journals Pap smear Google Scholar indexed journals Screening articles Screening Research articles Screening review articles Screening PubMed articles Screening PubMed Central articles Screening 2023 articles Screening 2024 articles Screening Scopus articles Screening impact factor journals Screening Scopus journals Screening PubMed journals Screening medical journals Screening free journals Screening best journals Screening top journals Screening free medical journals Screening famous journals Screening Google Scholar indexed journals Wilaya of Sidi-Bel-Abbès articles Wilaya of Sidi-Bel-Abbès Research articles Wilaya of Sidi-Bel-Abbès review articles Wilaya of Sidi-Bel-Abbès PubMed articles Wilaya of Sidi-Bel-Abbès PubMed Central articles Wilaya of Sidi-Bel-Abbès 2023 articles Wilaya of Sidi-Bel-Abbès 2024 articles Wilaya of Sidi-Bel-Abbès Scopus articles Wilaya of Sidi-Bel-Abbès impact factor journals Wilaya of Sidi-Bel-Abbès Scopus journals Wilaya of Sidi-Bel-Abbès PubMed journals Wilaya of Sidi-Bel-Abbès medical journals Wilaya of Sidi-Bel-Abbès free journals Wilaya of Sidi-Bel-Abbès best journals Wilaya of Sidi-Bel-Abbès top journals Wilaya of Sidi-Bel-Abbès free medical journals Wilaya of Sidi-Bel-Abbès famous journals Wilaya of Sidi-Bel-Abbès Google Scholar indexed journals human papillomavirus articles human papillomavirus Research articles human papillomavirus review articles human papillomavirus PubMed articles human papillomavirus PubMed Central articles human papillomavirus 2023 articles human papillomavirus 2024 articles human papillomavirus Scopus articles human papillomavirus impact factor journals human papillomavirus Scopus journals human papillomavirus PubMed journals human papillomavirus medical journals human papillomavirus free journals human papillomavirus best journals human papillomavirus top journals human papillomavirus free medical journals human papillomavirus famous journals human papillomavirus Google Scholar indexed journals female health articles female health Research articles female health review articles female health PubMed articles female health PubMed Central articles female health 2023 articles female health 2024 articles female health Scopus articles female health impact factor journals female health Scopus journals female health PubMed journals female health medical journals female health free journals female health best journals female health top journals female health free medical journals female health famous journals female health Google Scholar indexed journals cervical smears articles cervical smears Research articles cervical smears review articles cervical smears PubMed articles cervical smears PubMed Central articles cervical smears 2023 articles cervical smears 2024 articles cervical smears Scopus articles cervical smears impact factor journals cervical smears Scopus journals cervical smears PubMed journals cervical smears medical journals cervical smears free journals cervical smears best journals cervical smears top journals cervical smears free medical journals cervical smears famous journals cervical smears Google Scholar indexed journals Life Sciences articles Life Sciences Research articles Life Sciences review articles Life Sciences PubMed articles Life Sciences PubMed Central articles Life Sciences 2023 articles Life Sciences 2024 articles Life Sciences Scopus articles Life Sciences impact factor journals Life Sciences Scopus journals Life Sciences PubMed journals Life Sciences medical journals Life Sciences free journals Life Sciences best journals Life Sciences top journals Life Sciences free medical journals Life Sciences famous journals Life Sciences Google Scholar indexed journals Biology articles Biology Research articles Biology review articles Biology PubMed articles Biology PubMed Central articles Biology 2023 articles Biology 2024 articles Biology Scopus articles Biology impact factor journals Biology Scopus journals Biology PubMed journals Biology medical journals Biology free journals Biology best journals Biology top journals Biology free medical journals Biology famous journals Biology Google Scholar indexed journals cervical smear test articles cervical smear test Research articles cervical smear test review articles cervical smear test PubMed articles cervical smear test PubMed Central articles cervical smear test 2023 articles cervical smear test 2024 articles cervical smear test Scopus articles cervical smear test impact factor journals cervical smear test Scopus journals cervical smear test PubMed journals cervical smear test medical journals cervical smear test free journals cervical smear test best journals cervical smear test top journals cervical smear test free medical journals cervical smear test famous journals cervical smear test Google Scholar indexed journals
Article Details
1. Introduction
Cervical cancer remains a public health problem in developing countries. According to the latest data of GLOBOCAN 2018, the cervical cancer is the fourth leading cause of cancer and death from all cancers in women worldwide [1]. Furthermore, the International Agency for Research on Cancer (IARC), estimated the global incidence of cervical cancer at 570,000 new cases per year in 2018, more than 80% of which occur in developing countries [1]. In Algeria cervical cancer is the second most common cancer among women [2], with an estimated incidence of 15.1 per 100,000 women per year, and therefore represents a serious public health problem in Algeria [3]. For this reason, the Ministry of Health and Population in Algeria have set up a national screening program for this cancer since 2001. Cervical cancer affects women with sexual activity and occurs most often in multiparous women between 40 and 50 years of age [4]. This cancer depends on several factors: the human papillomavirus, the earliness of the first sexual intercourse, the multiplicity of sexual partners, the parity, the oral contraception use, tobacco and the inadequacy of gynecological surveillance of women [5]. This female health problem is characterised by a slow progression and the existence of numerous curable lesions before the invasive stage, the treatment of which in principle makes the development of cancer impossible [6]. To do so, they must be detected early using a screening test, which is the Papanicolaou test (Pap) also known as cervical smears or smear test [7].
The Pap test has the advantage of being inexpensive and simple to carry out [8]. It should be offered systematically to all women who have had sexual activity. It should be started early in sexually active women before the age of 25. After three negative smears a year apart, the recommended rate is one smear every three years [9]. The aim of this work is to evaluate the activities of cervical cancer screening activities by cervical smears in the "Wilaya of Sidi-Bel-Abbès", northwestern Algeria. The study was carried out during a period of three years (from 2015 to 2017).
2. Methods
This is a retrospective study performed over a period of three years (from 2015 to 2017) concerning two hundred and sixty six cervical smears carried out at the level of the Public Hospital Establishment (PHE) "DAHMANI Slimane" located in the Wilaya of Sidi-Bel-Abbès, the northwest region of Algeria. The source of information is based on quarterly evaluation reports of cervical cancer screening activities. Data analysis were processed and performed manually using the Statistical Package for Social Sciences® (SPSS, version 24.0) and the Microsoft Excel 2013 program.
3. Results
A set of 266 cervical smears were counted during the period of our study (three years) among them; 69.54% were first cervical smears, 22.55% were performed for the second time and 7.89% for the 3rd (Figure. 1). The analysis carried out on the entire studied population has shown that the smear rate made in 2017 was higher (56.39%) compared to previous years; 2016 and 2015 with 33.08% and 10.52%, respectively. The age groups most represented for the first cervical smear were the age groups of [40-44 years] in 2015, [40-44 years] and [45-49 years] in 2016 and [35-39 years] and [40-44 years] in 2017 (Table. 1). While, for the other cervical smears (2nd and 3rd), the older age groups were the most represented. In Figure 2 are summarized the cervical smears qualities. In general, during the study period, the smears adequate for the interpretation were the majority whether for the first, the second or the third cervical smears. However, cervical smears not satisfactory for interpretation represented lower rates of about 3.57% for the first cervical smear in 2015, 3.40% in 2016 and 3.33% in 2017. The cytological observed results are reported in Table 2. Out of all the samples, 17.85% of the cervical smears carried out in 2015, 46.59% in 2016 and 18.40% in 2017 were normal. Moreover, no presence of intra-epithelial lesions due to Trichomonas, mycosis, herpes, bacteria and Chlamydia has been reported. Epithelial abnormalities of low grade were, however, observed on 3.4% of 1st and 2nd cervical smears done in 2016 and on 0.8% of 1st and 1.6% of 2nd smears performed in 2017. Based on the cytological results, the attending physician make recommendations that are illustrated on Table 3. The most frequent recommendations were to redo cervical smears during the 6 months following the previous test; 35.71% in 2015, 47.67% in 2016 and 57.25% in 2017. However, performing a colposcopy or biopsy ware the less frequent as recommendations.
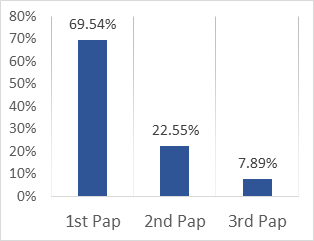
Figure 1: Distribution of all smears test made during the study period.
|
|
2015 |
2016 |
2017 |
||||||
|
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
|
|
< 30 years |
7.14 |
0.0 |
0.0 |
3.40 |
0.0 |
0.0 |
8.0 |
1.33 |
0.0 |
|
30-34 years |
7.14 |
0.0 |
0.0 |
11.36 |
2.27 |
1.13 |
8.0 |
2.0 |
0.0 |
|
35-39 years |
14.28 |
0.0 |
0.0 |
4.54 |
5.68 |
1.13 |
14.66 |
2.66 |
0.66 |
|
40-44 years |
21.42 |
7.14 |
0.0 |
13.63 |
3.40 |
1.13 |
14.66 |
4.66 |
0.66 |
|
45-49 years |
3.57 |
3.57 |
0.0 |
15.90 |
3.40 |
2.27 |
4.66 |
2.0 |
0.66 |
|
50-54 years |
14.28 |
3.57 |
0.0 |
5.68 |
2.27 |
2.27 |
10.66 |
5.33 |
3.33 |
|
55-59 years |
3.57 |
3.57 |
3.57 |
3.40 |
1.13 |
4.54 |
4.66 |
3.33 |
0.0 |
|
³ 60 years |
7.14 |
0.0 |
0.0 |
9.09 |
2.27 |
0.0 |
4.0 |
3.33 |
0.66 |
|
Total |
78.54 |
17.85 |
3.57 |
67.0 |
20.42 |
12.47 |
69.3 |
24.64 |
5.97 |
Pap: The Papanicolaou test (cervical smear test)
Table 1: Distribution of the performed smears test by patients’ age group.
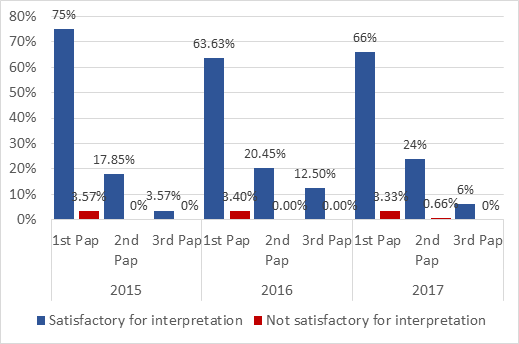
Figure 2: Distribution according to smear test quality.
|
|
2015 |
2016 |
2017 |
|||||||
|
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
1st Pap (%) |
2nd Pap (%) |
3rd Pap (%) |
||
|
Absence of intraepithelial lesion or malignancy signs |
Normal |
10.71 |
7.14 |
0.0 |
30.68 |
6.81 |
9.09 |
13.6 |
4.0 |
0.8 |
|
Non-specific inflammation |
67.85 |
10.71 |
3.57 |
30.68 |
12.50 |
3.40 |
54.4 |
20.0 |
4.8 |
|
|
Trichomonas |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Mycosis |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Herpes |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Bacteria |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Chlamydia |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Chemotherapy |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Radiotherapy |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Epithelial cell abnormality |
ASC-US |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
ASC-H |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Low grade |
0.0 |
0.0 |
0.0 |
3.40 |
3.40 |
0.0 |
0.8 |
1.6 |
0.0 |
|
|
High grade |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Squamous cell carcinoma |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
AGC |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
AGC lesion |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
AIS |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Endocervical adenocarcinoma |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Endometrial adenocarcinoma |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Other |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
0.0 |
|
|
Total |
78.56 |
17.85 |
3.57 |
64.76 |
22.71 |
12.49 |
68.8 |
25.6 |
5.6 |
|
ASC-US: Atypical Squamous Cells of Undetermined Significance; ASC-H: Atypical Squamous Cell Evocating High Grade Lesion; AGC: Atypical Glandular Cells; AIS: Adenocarcinoma in Situ; Pap: The Papanicolaou test (cervical smear test).
Table 2: Smears test results for the three years of the study.
|
|
2015 |
2016 |
2017 |
|
Pap smear in 6 months (%) |
35.71 |
47.67 |
57.25 |
|
Pap smear in 1 year (%) |
21.42 |
47.67 |
14.50 |
|
Pap smear in 3 years (%) |
0.0 |
0.0 |
3.05 |
|
Pap smear post treatment (%) |
0.0 |
1.16 |
18.32 |
|
To redo as soon as possible (%) |
42.85 |
0.0 |
4.58 |
|
HPV test (%) |
0.0 |
0.0 |
0.0 |
|
Colposcopy (%) |
0.0 |
2.32 |
1.52 |
|
Biopsy (%) |
0.0 |
1.16 |
0.76 |
|
Endocervical curettage (%) |
0.0 |
0.0 |
0.0 |
|
Total (%) |
100 |
100 |
100 |
HPV: Human Papillomavirus
Table 3: Recommendations based on the smear test results.
4. Discussion
Early detection of cervical cancer is a prevention strategy that has proven effective in the fight against this disease [10]. In most countries, it is based on making a cervical smear [11]. In Algeria, the screening of cervical cancer by cervical smear (Pap test) is available in public health facilities since 2001. The screening practice was individual, left to the initiative of the doctor or the patients. However, a majority of women think that their behaviour regarding the practice of Pap smear test depends on those of health professionals. The absence of recommendations from the latter implies the non-practice of cervical smear. This dependence vis-à-vis health professional is still observed developing courtiers’ societies [4]. The present work was conducted to evaluate the activities of malignant cervical lesions screening by cervical smears in the "Wilaya of Sidi-Bel-Abbès", northwestern Algeria. In our study, very low rates of women undergo this test regularly. However, it has been shown that the incidence of cervical cancer can decrease by more than 90% if all women aged 25 to 65 receive a cervical smear every three years [12]. In our series, the age groups (35-39), (40-44) and (45-49) years represent the most successful groups. This agrees with the results of Boublenza et al. West of Algeria and El Gnaoui In Morocco [13, 14]. A remarkable increase from 2015 (with only 28 cervical smear) to 2017 (with 150 cervical smear) was noted in our investigation. This increase is the result of a relatively large awareness of cervical cancer screening initiated in Algeria and in the Wilaya of Sidi-Bel-Abbès where the essential recommendations were to benefit all women from cervical smear screening every 5 years after two negative smears, from the age of 25. During the three years of the study, the vast majority of the smears studied were of satisfactory quality for interpretation. The non-specific inflammation was the most common sing in our study population and the remaining smears were normal. However, we did not revealed presence of intra-epithelial lesions due to Trichomonas, mycosis, herpes, bacteria and Chlamydia. All the same, when studying epithelial cell abnormalities, the low-grade lesions were observed in 3.4% of the first and the second cervical smear in 2016 and in 0.8% and 1.6%, respectively, in the 1st and the 2nd cervical smears in 2017. Our findings are similar to those of Nahet at al. (2015) [2] and Mahé et al. (2007) [15]. Based on the smear test results, the physicians took several decisions; a surveillance check is recommended, if this is the first smear to be performed, a second smear at one year is required, but if it is a smear in a woman already followed, a check at 3 years is necessary. The 3-year interval is generally recommended between each two cervical smears. However, most countries outside the USA and Canada use 3 or 5 years intervals [16]. The frequencies of colposcopy and biopsy. According to Karimi-Zarchi et al. (2015), these two techniques provide higher levels of accuracy, sensitivity, specificity, and negative predictive value than cervical smear test in identifying pre-malignant lesions [17]. Though, the cervico-vaginal smear remains an effective, rapid and less expensive diagnostic tool for the initial evaluation of the cervix and for the detection of precancerous and inflammatory cervical lesions.
5. Conclusion
Cervical cancer, although it is one of the easiest cancers to prevent, still occupies the second position of female cancers in Algeria, so there remains a major public health problem where its screening reaches a limited rate of target female population, at a late age, result confirmed by the present retrospective study.
References
- Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68 2018): 394-424.
- Nahet A, Boublenza L, Hassaine H, et al. Étude rétrospective de l’évaluation des activités de dépistage des lésions précancéreuses du col de l’utérus dans une région du sud d’Alger entre 2008 et 2011. J Afr Cancer 7 (2015): 168-172.
- Hammouda D, Muñoz N, Bouhadef A, et al. Épidémiologie de l’infection à papillomavirus humain en Algérie Eurocancer. John Libbey Eurotext (2008): 163-166.
- Watfa Beiruthy I, Sassine Kazan R. Étude corrélationnelle sur les facteurs prédictifs de la pratique du test de dépistage du cancer du col utérin chez les femmes fréquentant les centres médico-sociaux à Zahlé (Liban). Revue Francophone Internationale de Recherche Infirmière 2 (2016): 31-40.
- Delcroix M, Du Masgenet B. Gynécologie obstétrique. Paris: Vigot (1996): 467.
- Duport N. Données épidémiologiques sur le cancer du col de l’utérus. Institut de veille sanitaire. DIADEIS Paris (2008): 5-11.
- Monsonego J. Infections à papillomavirus état des connaissances, pratiques et prévention vaccinale. Springer France, Paris (2006): 3-178.
- Camus E, Heim N, Nisand I. Soins infirmières en maternitéet aux personnes atteintes d’affections gynécologiques. Paris: Masson (2003): 49.
- Fernandez H. Traité de gynécologie. Paris: Médecine-Sciences, Flammarion (2005): 350-359.
- Gustafsson L, Pontén J, Zack M, et al. International incidence rates of invasive cervical cancer after introduction of cytological screen- ing. Cancer Causes Control 8 (1997): 755-763.
- Fahey MT, Irwig L, Macaskill P. Meta-analysis of Pap Test Accuracy. Am J Epidemiol 141 (1995): 680-689.
- Boulanger JC, Gondry J. De la bonne pratique du dépistage du cancer du col utérin. Ref Gynecol Obstet 4 (1996): 75-84.
- Boublenza L, Moulessehoul S, Beldjillali H, et al. Analyse des activités de dépistage du cancer du col de l’utérus dans une région de l’ouest Algérien entre 2007 et 2011. J Afr Cancer 5 (2013): 11-15.
- El Gnaoui N, Saile R, Benomar H. Le frottis cervicovaginal un test incontournable dans le dépistage des lésions du col de l’utérus. J Afr Cancer 2 (2010): 9-13.
- Mahé C, Cocqueel F, Garnier A. État des lieux du dépistage du cancer du col utérin en France. Institut National du Cancer (2007).
- Dickinson J, Tsakonas E, Conner Gorber S, et al. Recommendations on screening for cervical cancer. CMAJ 185 (2013): 35-45.
- Mojgan Karimi-zarchi, Leila Zanbagh, Alireza Shafii, et al. Comparison of Pap Smear and Colposcopy in Screening for Cervical Cancer in Patients with Secondary Immunodeficiency. Electron Physician 7 (2015): 1542-1548.


 Impact Factor: * 3.6
Impact Factor: * 3.6 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 