Atlantoaxial Rotatory Instability in a Down Syndrome Patient with Aberrant Vertebral Artery Anatomy
Micah W Smith1*, Daniel R Romano2
1Ortho Northeast, Fort Wayne, Indiana, USA
2Indiana University School of Medicine, Indianapolis, USA
*Corresponding Author: Micah W Smith, Ortho Northeast 5050 N. Clinton Street, Fort Wayne, IN 46825, USA
Received: 12 April 2019; Accepted: 25 April 2019; Published: 07 May 2019
Article Information
Citation:
Micah W Smith, Daniel R Romano. Atlantoaxial Rotatory Instability in a Down Syndrome Patient with Aberrant Vertebral Artery Anatomy. Journal of Spine Research and Surgery 1 (2019): 16-22.
DOI: 10.26502/fjsrs.2687-8046003
View / Download Pdf Share at FacebookAbstract
Atlantoaxial instability (AAI) is a common deformity in Down syndrome (DS). Although often inconsequential, AAI can progress to atlantoaxial rotatory subluxation (AARS). In patients with DS, concomitant AAI often necessitate surgical fusion, but successful stabilization in this population can be challenging due to high complication rates. A 14-year-old male with DS presented with a 3-month history of spontaneous AARS. After failed closed reduction, the parents consented to surgical stabilization. Preoperative planning revealed a high-riding vertebral artery and thin C2 lamina; therefore, C1-C4 segmental posterior instrumented fusion was performed, resulting in a successful reduction maintained at 12 months’ follow-up. The development of rigid fixation for the treatment of AARS has improved fusion rates in children with DS. However, vascular and osseous anomalies in this population often dictate extension of the fusion constructs beyond C1 and C2. Careful preoperative planning is a prerequisite to safe and solid fixation.
Keywords
<p>Down syndrome, Vertebral artery, Atlantoaxial rotatory subluxation, Atlantoaxial instability</p>
Article Details
Abbreviations:
ADLs-activities of daily living; AAI-atlantoaxial instability; AARS-atlantoaxial rotatory subluxation; DS-Down syndrome; PICA-posterior inferior cerebellar artery
1. Introduction
Down syndrome (DS) is a constellation of signs and symptoms caused by trisomy 21, the most common viable chromosomal abnormality, with 1 in every 733 live births [1]. In addition to intellectual disability and characteristic morphologic features, individuals with DS exhibit a predisposition to many chronic medical conditions, including gastrointestinal disorders, cardiac defects, early-onset Alzheimer’s disease, hypothyroidism, and musculoskeletal problems [2, 3]. Of the latter, atlantoaxial instability (AAI), present in 10-30% of those with DS, has perhaps the most serious sequelae [1, 2].
In DS, AAI may be the consequence of os odontoideum, intrinsic ligamentous laxity, and/or ligament damage secondary to chronic inflammation [1]. Although often subclinical, AAI progresses to symptomatic subluxation in 1-2% of individuals with DS [3]. Children with DS are especially predisposed to atlantoaxial rotatory subluxation (AARS) due to the relative ligamentous laxity, inconspicuous facet joints, large heads, and small stabilizing muscles of children [4, 5]. Therefore, patients with DS commonly present with symptomatic subluxation between the ages of 5 and 15 years [2]. Initial treatment is conservative, but surgical stabilization is recommended for refractory subluxation, progressive neurologic deterioration, and/or unstable deformity, as in os odontoideum [1, 5, 6, 7]. Here, we present the case of an adolescent with DS and AARS in which abnormal osseous and vascular anatomy necessitated an extension of the fusion construct caudally to C4.
2. Case Report
A 14-year-old male with DS presented to our spine service 3 months after awaking with cervical pain. He developed a cock robin posture and was initially treated by a chiropractor without resolution of pain or posturing. Eventually, he was no longer able to complete activities of daily living (ADLs) without pain and sought further medical care. AARS was diagnosed on imaging (Figure 1), and we admitted the patient for skeletal traction using Gardner-Wells tongs. Closed reduction was attempted over the course of 4 days, but despite partial radiographic improvement, the deformity could not be completely reduced.
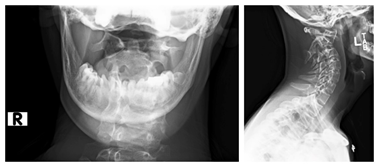
Figure 1: Preoperative cervical radiographs illustrating C1/C2 rotatory subluxation in both odontoid (Left) and lateral (Right) views.
Posterior fusion was recommended over continued traction, and after a discussion of the risks and benefits, the parents consented. Preoperative work-up revealed a high-riding course of the vertebral artery through C2, precluding safe placement of C2 pedicle screws (Figure 2-Left). Safe placement of C2 translaminar screws was also prevented due to a thin-only 1-2 mm-C2 lamina composed entirely of cortical bone (Figure 2-Right). Intraoperatively, the Gardner-Wells tongs were replaced with a 3-pronged Mayfield head clamp to attempt closed reduction under neurological monitoring, but the dislocation still proved irreducible.
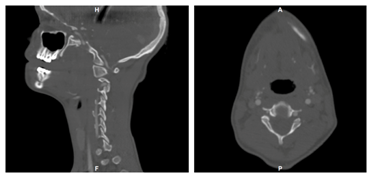
Figure 2: Preoperative computed tomography angiogram revealing a high-riding vertebral artery in sagittal cut (Left) and a thin C2 lamina in axial cut (Right).
A standard posterior approach was then performed from C1-C3. Of note, after blunt dissection of the fascia, the posterior aspect of the spinal cord could be visualized through a large interspinous space. The C1/C2 joint was identified, and granulation-type soft tissue was removed. A clamp was then used to complete the reduction by pulling the C1 arch to the C2 lamina. Fluoroscopy confirmed both complete reduction and acceptable rotation (Figure 3-Left). Neurological monitoring remained stable, and the Mayfield clamp was momentarily loosened to ensure no stretch on neurological elements. The anatomy of C1 allowed good screw placement, but without the ability to safely place screws in C2, and with a large quadrilateral construct fusing C1-C3, it was decided intraoperatively to provide segmental instrumentation with screws in C1, C3, and C4 (Figure 3-Right). Bicortical structural iliac crest allograft was molded to C1 and around the C2 spinous process in a pantaloon-fashion and then secured around the rods.
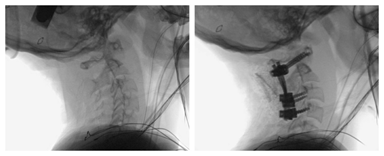
Figure 3: Intraoperative fluoroscopy demonstrating complete reduction (Left) and fixation with a rigid segmental construct (Right).
After surgery, the patient was placed in an Aspen collar for 6 weeks, primarily to remind him of his limitations, as he was eager to return to his normal activities. His postoperative course was uneventful, with complete resolution of both cervical pain and cock robin posturing. Radiographic analysis revealed that reduction was maintained at 12 months’ follow-up (Figure 4).
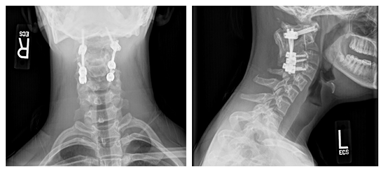
Figure 4: 12-month postoperative cervical radiographs demonstrating sustained reduction and solid arthrodesis in both anterior (Left) and lateral (Right) views.
3. Discussion
The atlantoaxial joint is the site of approximately 60% of the 180° of axial rotation that occurs at the level of the cervical spine [8]. This mobility is possible because of nearly-horizontal facet joints that do little to limit motion [8]. As a result, stability of the atlantoaxial joint is dependent on osseous stops and ligamentous tethers, namely the anterior arch of atlas, dens, and transverse and alar ligaments [1, 2, 5]. Due to the unique biomechanics of the atlantoaxial joint, subluxation of the facets occurs during normal axial rotation, but this natural subluxation is tightly controlled, with little variance among individuals [7, 8]. In its pathologic counterpart, this tight control is lost, and the atlas and axis interact abnormally during axial rotation [8]. The resulting condition, AARS, typically presents as painful torticollis with the so-called cock robin posture and can progress to myelopathy with paresis, ataxia, and/or urinary retention [5, 7-11] Progression from instability to subluxation is precipitated by surgery, infection, and trauma but may be idiopathic in up to one-fourth of cases [8]. The most common initial treatment for AARS is a cervical collar in combination with analgesics [7]. The success of these conservative measures and others, such as halter traction and muscle relaxers, is highly dependent on early diagnosis and intervention, and closed reduction is often possible in patients presenting within 1 month of onset [5, 7]. Rotatory subluxations that persist for over 1 month are less amenable to conservative treatment, and those that persist for 2-3 months or longer are considered chronic [6, 7].
Although current literature supports fusion for chronic AARS, conservative attempts at reduction are still trialed in these patients, and Park et al. achieved a reduction of a chronic AARS using halter traction and a cervical collar [10, 12, 13, 14]. More recently, Ishii et al. treated 12 cases of chronic AARS using remodeling therapy, a closed reduction protocol, without recurrence [6]. It is worth noting that remodeling therapy is contraindicated in DS, and ultimately, surgical fusion is often needed to resolve AARS in these patients due to underlying AAI [5, 6]. Although Au-Yong et al. reported the successful use of halo traction to reduce AARS in a child with DS, Yamazaki et al. could not achieve closed reduction with a halo vest in an adult with chronic AARS and resorted to open reduction with O-C3 fusion [11, 15]. It is an unfortunate irony that the same factors that predispose DS patients to AAI also produce comparably high rates of nonunion, recurrence, and graft resorption with posterior fusion [1, 2, 16]. The traditional method of posterior wiring with onlay fusion, with complications that commonly include ligation of hypo- or dysplastic C1 arches and graft resorption, is perhaps particularly ill-suited for this population [17, 18]. The introduction of screw-based systems over the past quarter-century has increased fusion rates in children with DS from 40% to 58-95% [1].
First described by Magerl et al. in 1979 as an adjunct to sublaminar wiring, transarticular screws have been successfully used to reduce syndromic AARS [19, 20]. The Harms and Melcher technique-originally consisting of contoured rods secured between C1 lateral mass screws and C2 pedicle screws and since adapted to incorporate pars or laminar screws in C2-has high fusion rates, avoids postoperative halo fixation, and is safe and suitable for children [1, 17, 14]. Authors have reported the safe placement of C1 lateral mass screws, C2 pars screws, C2 pedicle screws, and C2 laminar screws in children with DS [9, 21-23]. However, because of their immature and undersized bones, these patients may require extension of the fusion area beyond C1 and C2, and reports of occipitocervical fusion are not uncommon [9, 21-23]. Vertebral artery anomalies may also necessitate extension of the fusion area [9]. Vertebral artery injury is a serious complication of screw-based fixation, and the anomalous vertebral arteries more common in children with DS are especially susceptible to injury [1, 6, 24, 25]. Deviations from normal anatomy include the persistent intersegmental artery, fenestrated vertebral artery, early posterior inferior cerebellar artery (PICA), and high-riding vertebral artery, which Yeom et al. found at 14.5% of C2 screw insertion sites [24, 25].
For patients with a high-riding course, transarticular and pedicle screws are not safe options [24, 25]. In the present case, safe placement of interlaminar screws was not possible, and thus, extension of the fusion to C4 was required. Although Spennato et al. previously reported extension to C3 due to C2 anatomy that prevented interlaminar screw placement, our case is unique in that the anatomy of the vertebral artery prevented C2 pedicle screw placement as well [14]. Interestingly, Hong et al. recently found that vertebral artery and bony anomalies at the craniovertebral junction are relatively concordant, such that anatomy precluding the safe placement of all C2 screws may not be entirely rare [24].
In summary, we present the case of a DS patient with chronic atlantoaxial rotatory subluxation. This case demonstrates the importance of preoperative planning and imaging to achieve optimal fixation and prevent vascular complications. These complications are more prevalent in patients with DS, but can be minimized with thoughtful planning.
Acknowledgments
The authors report no sources of funding.
Conflicts of interest
The authors report no potential conflict of interest.
References
- Hankinson TC, Anderson RC. Craniovertebral Junction Abnormalities in Down Syndrome. Neurosurgery 66 (2010): 32-38.
- Caird MS, Wills BP, Dormans JP. Down Syndrome in Children: The Role of the Orthopaedic Surgeon. J Am Acad Orthop Surg 14 (2006): 610-619.
- Malt EA, Dahl RC, Haugsand TM, et al. Health and Disease in Adults with Down Syndrome. Tidsskr Nor Laegeforen 133 (2013): 290-294.
- Barcelos AC, Patriota GC, Netto AU. Nontraumatic Atlantoaxial Rotatory Subluxation: Grisel Syndrome. Case Report and Literature Review. Global Spine J 4 (2014): 179-186.
- Kinon MD, Nasser R, Nakhla J, et al. Atlantoaxial Rotatory Subluxation: A Review for the Pediatric Emergency Physician. Pediatr Emerg Care 32 (2016): 710-716.
- Ishii K, Toyama Y, Nakamura M, et al. Management of Chronic Atlantoaxial Rotatory Fixation. Spine (Phila Pa 1976) 37 (2012): 278-285.
- Neal KM, Mohamed AS. Atlantoaxial Rotatory Subluxation in Children. J Am Acad Orthop Surg 23 (2015): 382-392.
- Pang D, Li V. Atlantoaxial Rotatory Fixation: Part 1-Biomechanics of Normal Rotation at the Atlantoaxial Joint in Children. Neurosurgery 55 (2004): 614-625.
- Siemionow K, Chou D. To the Occiput or Not? C1-C2 Ligamentous Laxity in Children with Down Syndrome. Evid Based Spine Care J 5 (2014): 112-118.
- Umebayashi D, Hara M, Nishimura Y, et al. A Morphologically Atypical Case of Atlantoaxial Rotatory Subluxation. J Korean Neurosurg Soc 55 (2014): 284-288.
- Yamazaki M, Someya Y, Aramomi M, et al. Infection-Related Atlantoaxial Subluxation (Grisel Syndrome) in an Adult with Down Syndrome. Spine (Phila Pa 1976) 33 (2008): 156-160.
- Lavelle WF, Palomino K, Badve SA, et al. Chronic C1-C2 Rotatory Subluxation Reduced by C1 Lateral Mass Screws and C2 Translaminar Screws: A Case Report. J Pediatr Orthop 37 (2017): 174-177.
- Park SW, Cho KH, Shin YS, et al. Successful Reduction for a Pediatric Chronic Atlantoaxial Rotatory Fixation (Grisel Syndrome) with Long-Term Halter Traction: Case Report. Spine (Phila Pa 1976) 30 (2005): 444-449.
- Spennato P, Nicosia G, Rapanà A, et al. Grisel Syndrome Following Adenoidectomy: Surgical Management in a Case with Delayed Diagnosis. World Neurosurg 84 (2015): 7-12.
- Au-Yong I, Boszczyk B, Mehdian H, et al. Spontaneous Rotatory Atlantoaxial Dislocation without Neurological Compromise in a Child with Down Syndrome: A Case Report. Eur Spine J 17 (2008): 308-311.
- McKay SD, Al-Omari A, Tomlinson LA, et al. Review of Cervical Spine Anomalies in Genetic Syndromes. Spine (Phila Pa 1976) 37 (2012): 269-277.
- Haque A, Price AV, Sklar FH, et al. Screw Fixation of the Upper Cervical Spine in the Pediatric Population. Clinical Article. J Neurosurg Pediatr 3 (2009): 529-533.
- Jain VK. Atlantoaxial dislocation. Neurol India 60 (2012): 9-17.
- Bahadur R, Goyal T, Dhatt SS, et al. Transarticular Screw Fixation for Atlantoaxial Instability-Modified Magerl’s Technique in 38 Patients. J Orthop Surg Res 5 (2010): 87.
- Herzka A, Sponseller PD, Pyeritz RE. Atlantoaxial Rotatory Subluxation in Patients with Marfan Syndrome. A Report of Three Cases. Spine (Phila Pa 1976) 25 (2000): 524-526.
- Hedequist D, Bekelis K, Emans J, et al. Single Stage Reduction and Stabilization of Basilar Invagination after Failed Prior Fusion Surgery in Children with Down’s Syndrome. Spine (Phila Pa 1976) 35 (2010): 128-133.
- Ito K, Imagama S, Ito Z, et al. Screw Fixation for Atlantoaxial Dislocation Related to Down Syndrome in Children Younger than 5 Years. J Pediatr Orthop B 26 (2017): 86-90.
- Kuroki H, Kubo S, Hamanaka H, et al. Posterior Occipito-Axial Fixation Applied C2 Laminar Screws for Pediatric Atlantoaxial Instability Caused by Down Syndrome: Report of 2 Cases. Int J Spine Surg 6 (2012): 210-215.
- Hong JT, Kim IS, Kim JY, et al. Risk Factor Analysis and Decision-Making of Surgical Strategy for V3 Segment Anomaly: Significance of Preoperative CT Angiography for Posterior C1 Instrumentation. Spine J 16 (2016): 1055-1061.
- Yeom JS, Buchowski JM, Kim HJ, et al. Risk of Vertebral Artery Injury: Comparison between C1-C2 Transarticular and C2 Pedicle Screws. Spine J 13 (2013): 775-785.


 Impact Factor: * 3.123
Impact Factor: * 3.123 Acceptance Rate: 75.30%
Acceptance Rate: 75.30%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 