Recurrent Pregnancy Loss (RPL): An overview
Shehnaz Sultana, Pratibha Nallari, Venkateshwari Ananthapur*
Institute of Genetics and Hospital for Genetic Diseases, Osmania University, Telangana, India
*Corresponding author: Dr. Venkateshwari Ananthapur, Institute of Genetics and Hospital for Genetic Diseases, Osmania University, Begumpet, Hyderabad-500016, Telangana, India
Received: 04 June 2020; Accepted: 17 July 2020; Published: 18 August 2020
Article Information
Citation:
Shehnaz Sultana, Pratibha Nallari, Venkateshwari Ananthapur. Recurrent Pregnancy Loss (RPL): An overview. Journal of Women’s Health and Development 3 (2020): 302-315.
DOI: 10.26502/fjwhd.2644-28840038
View / Download Pdf Share at FacebookAbstract
Recurrent pregnancy loss (RPL) is defined as two or more pregnancies losses occurring before 20 weeks of gestation and affecting 1-3% of the couples. Chromosomal abnormalities, uterine defects, thrombophilia, immunological factors, endocrine and metabolic factors are the known risk factors involved in the causation of recurrent pregnancy loss in 50% of the cases. However, remaining 50% of the recurrent pregnancy loss cases are unexplained. A lot of research is going on in the area of recurrent pregnancy loss globally and the results are inconsistent due to study designs, sample size, ethnicity etc. The present review took an insight into the overall risk factors involved in the causation of explained recurrent pregnancy loss to help the researchers to identify the origin of pregnancy loss and to provide best investigation and treatment strategy for women with recurrent pregnancy loss.
Keywords
<p>Antiphospholipid syndrome, Chromosomal abnormalities, Genetics, PCOS, Thrombophilia, Uterine defects</p>
Article Details
1. Introduction
Recurrent pregnancy loss (RPL) is defined as two or more pregnancy losses occurring prior to 20 weeks of gestation in 1–3% of couples [1]. Pregnancy loss or miscarriage is the spontaneous process which occurs before the foetus reaches its viability, which includes all pregnancy losses occurring from the time of conception to 24 weeks of gestation. Primary recurrent pregnancy loss is defined as the pregnancy loss without a previous ongoing pregnancy beyond 24 weeks of gestation, whereas secondary recurrent loss is an episode of pregnancy loss after one or more previous pregnancies progressing beyond 24 weeks of gestation. Pregnancy is confirmed by the presence of beta human chorionic gonadotropin (BHCG) hormone in serum or urine. Non visualized pregnancy loss includes biochemical pregnancy loss and resolved and treated pregnancies of unknown location which occurs after 6 weeks of gestation, where an ultrasound examination is done only after complete expulsion of the embryo and trophoblast or else no ultrasound was done after heavy bleeding. In case earlier ultrasound scan is done then it is termed as clinical miscarriage. Ectopic, molar pregnancies and implantation failures are excluded from the definition of recurrent pregnancy loss, whereas pregnancy loss after spontaneous conception and assisted reproductive treatment (ART) are included in the definition of recurrent pregnancy loss. Recurrent early pregnancy loss (REPL) is defined as the loss of two or more pregnancies occurring before 10 weeks of gestation. Recurrent pregnancy loss affects approximately 1 to 2% of women taking into consideration three consecutive pregnancy losses occurring before 20 weeks of gestation. A prevalence of 0.8 to 1.4% was reported when only clinical miscarriages that is pregnancy losses confirmed by ultrasound scan are taken into consideration, including biochemical losses increased the prevalence from 2 to 3%. The known risk factors for RPL are advanced female age, previous pregnancy losses, parental structural chromosomal abnormalities, uterine anomalies, endocrine disturbances, antiphospholipid syndrome (APS) and inherited thrombophilia. Life style and obesity also play an important role in recurrent pregnancy loss. In spite of lot of research done in the area of RPL only in 50% of the cases the known cause is identified. Still in majority of the cases a known cause for RPL is unknown. Recurrent pregnancy loss has a significant psychological and emotional impact on couples. The present review helps the researchers to identify the different origins of pregnancy loss and to provide best investigation and treatment strategy for women with recurrent pregnancy loss.
2. Aetiologies of RPL
2.1 Chromosomal abnormalities
Chromosomal abnormalities both structural and numerical are the most common cause of recurrent pregnancy loss and constitutes 50% of the cases. Balanced translocations are the most common parental abnormality found in 3-5% of RPL cases followed by reciprocal translocation which affects non-homologous chromosomes and Robertsonian translocations which involves acrocentric chromosomes. In 5 % of the couples with recurrent pregnancy loss one of the them carries a balanced chromosomal rearrangement. The other karyotypic abnormalities includes ring chromosomes, deletions, duplications and mosaicism. A retrospective cohort study reported abnormal parental karyotypes in 1.9% individuals (n=20432) with recurrent pregnancy loss referred for genetic testing [2]. In a study of 795 couples with two or more pregnancy losses, 3.5% couples showed chromosomal abnormalities and subsequent miscarriage rate was higher in carrier couples [3]. Another cohort study reported lower birth rate in carrier couples compared to women with normal karyotype [4]. Majority of the subsequent pregnancy losses occurs in the carriers of reciprocal translocations and inversions compared to Robertsonian translocations. Aneuploidy is one of the important causes of sporadic and recurrent pregnancy loss which increases with female age. Meiotic non-disjunction in oogenesis leads to autosomal chromosomal aneuploidies whereas, meiotic spermatogenesis leads to sex chromosome aneuploidies. Chromosomal analysis of sperm showed numerical abnormalities. Embryos showing abnormal karyotype are aborted due to implantation failure or other mechanisms interfering with normal placental growth. Chromosomal abnormalities affect placental morphology, histology, hormones, protein secretions and shows decreased cell proliferation in vascular smooth muscles and increased apoptosis, which leads to impaired vascular development and recurrent pregnancy loss. Parental karyotyping can be recommended for recurrent pregnancy loss couples after individual risk assessment based on genetic history.
2.2 Anatomical abnormalities
Recurrent pregnancy loss in 19% of the women is due to uterine defects, which consists of both acquired and congenital. Septate uterus is the most common congenital uterine abnormality associated with spontaneous miscarriage. Congenital uterine malformations are well established in recurrent pregnancy loss. Congenital Mullerian tract malformations include septate uterus, bicorporeal uterus with normal cervix (AFS bicornuate uterus), bicorporeal uterus with double cervix (AFS didelphic uterus) and hemi-uterus (AFS unicornuate uterus). Uterine malformations prevalence is higher in women with recurrent pregnancy loss history. A higher prevalence of miscarriage is reported in women with congenital uterine malformations. Women with septate uterus and bicornuate uterus showed increased probability of pregnancy loss in first trimester, whereas women with arcuate uterus, septate uterus and bicornuate uterus showed pregnancy loss in second trimester [5]. Acquired uterine malformations such as submucous myomas, endometrial polyps and uterine adhesions are prevalent in pregnancy loss women, though the clinical relevance is still not established. A study reported 12.9% of acquired defects, 7% congenital defects and 0.6% of both congenital and acquired defects among 113 recurrent pregnancy loss women [6]. Uterine fibroids were reported in 8.2% of recurrent pregnancy loss women [7].
2.3 Thrombophilia
Thrombophilia is a hereditary or acquired condition that predisposes women with recurrent pregnancy loss to venous thromboembolism.
2.3.1 Hereditary thrombophilia: The role of genetic thrombophilia in women with recurrent pregnancy loss have been evaluated and assumed it to be a causing factor for recurrent pregnancy loss and other reproductive complications, which includes Factor V Leiden mutation, Prothrombin mutation, Protein C, Protein S and Antithrombin deficiency and MTHFR mutation. Factor V Leiden mutation (1691G→A) renders factor V resistant to cleavage by activated protein. Studies on Factor V Leiden mutation showed a significant association between (F5c.1691G>A) genotype and recurrent pregnancy loss. Carriers of Factor V Leiden mutation were more likely to have a subsequent loss compared to non-carriers [8]. Prothrombin encoding gene mutation 20210G→A mutation increases plasma concentrations of prothrombin and risk of thrombosis. Studies has reported a significant association between prothrombin mutation and recurrent pregnancy loss [9]. MTHFR gene mutation 677C→T a thermolabile variant can cause hyperhomocysteinemia and associated with recurrent pregnancy loss [10].
2.3.2 Acquired thrombophilia: Antiphospholipid Syndrome (APS) an autoimmune condition, which is an acquired thrombophilia accounts for 5-20% of recurrent pregnancy loss. Antiphospholipid antibodies damages trophoblast and leads to impaired trophoblast mediated functions like spiral artery formation, secretion of growth factors, human chorionic gonadotrophin (hCG), early apoptosis of trophoblasts and abnormal inflammatory response resulting in impaired pregnancy support. Lupus anticoagulant (LA), anticardiolipin antibodies (ACA, IgG and IgM), and β2 glycoprotein I antibodies (aβ2GPI, IgG and IgM) are antiphospholipid antibodies associated with thrombosis.
2.4 Immunological factors
2.4.1 Human leukocyte antigen (HLA): HLA influences immune reactions, HLA studies in recurrent pregnancy loss is divided into three different types. 1) HLA allele compatibility between partners with recurrent pregnancy loss, 2) HLA allele prevalence in recurrent pregnancy loss women and 3) HLA-C and G alleles studies in partners with recurrent pregnancy loss. Initially it was thought that increased HLA compatibility between partners would decrease the probability of mother to produce blocking antibodies that protect against foetal rejection. According to a meta-analysis allele sharing in HLA-A, B and C loci was not found with various frequencies in recurrent pregnancy loss and controls, but HLA-DR locus was significantly increased [11]. Allo-immune factors such as absence of maternal blocking antibodies and HLA sharing at A, B, C and DR loci by couples might be related with increased risk of miscarriage [12]. HLA-DRB1*03 allele was more often found to be significant in recurrent pregnancy loss women [13]. A study showed a significant increase in activating and decrease in inhibitory KIRs in women with recurrent pregnancy loss [14]. Soluble HLA-G polymorphisms modulate NK cytotoxicity and cytokine secretion at the foetal maternal interface in recurrent pregnancy loss. Low plasma soluble HLA-G levels might be associated with homozygosity of HLA-G 14bp insertion in HLA-G gene. HLA-G 14bp insertion frequency was found be significantly increased in recurrent pregnancy loss women [15]. Anti-HY antibodies are directed against male-specific minor histocompatibility (HY) antigens expressed on most or all nucleated male cells. Live birth rate in women negative for anti-HY antibodies is more compared to women positive for anti-HY antibodies [16]. However, further studies are needed for confirmation.
2.4.2 Cytokines: TNF-α is a known marker for systemic inflammation, increased levels of TNF-α increases the risk of miscarriage in recurrent pregnancy loss women. High TNF-α and TNF-α/IL10 ratios characterize women with euploid compared to aneuploid miscarriages. Secondary recurrent pregnancy loss women had higher levels of TNF-α in early pregnancy compared with primary recurrent pregnancy loss women [17]. Th1 cells expressing intracellular TNF-α in peripheral blood lymphocytes and TNF-α/IL-10 Th-cell ratio was significantly increased in recurrent pregnancy loss compared to controls [18]. Polymorphisms of cytokine genes influence the production of cytokines. Cytokine function changes depending on the length of gestation. Mitogen stimulated lymphocytes in women with recurrent pregnancy loss with further miscarriages produced more TNF-α than women who gave birth [19].
2.4.3 Antinuclear antibodies (ANA): Antinuclear antibodies (ANA) are directed against various components of
the cell nuclei, usually detected in autoimmune diseases. Increased levels of antinuclear antibodies were found in recurrent pregnancy loss. Prevalence of antinuclear antibodies in recurrent pregnancy loss women with new miscarriage is more compared to women who gave birth [20].
2.4.4 Natural killer cells (NK cells): Natural killer cell investigations in recurrent pregnancy loss is done by flow-cytometric analysis or tests of NK cell cytotoxicity of peripheral blood lymphocytes before or during pregnancy from pre-pregnancy endometrial biopsies or decidual tissue from miscarriages and terminated pregnancies.CD56+ NK cells percentage in peripheral blood cells taken before pregnancy is higher in recurrent pregnancy loss women compared to controls [21]. Sometimes previous successful pregnancy can induce permanent changes in lymphocyte subsets including NK cells. Majority of the studies found increased NK cell cytotoxicity in blood samples of women before pregnancy with a history of recurrent pregnancy loss [21]. A study reported reduced NK cytotoxicity in recurrent pregnancy loss women compared to controls [22]. Study found higher frequency of CD56+ NK cells in recurrent pregnancy loss [23]. Other immunological abnormalities include anti-HLA antibodies, celiac disease serum markers, anti-sperm antibodies and immune biomarkers such as IL2 receptor levels and anti-protein Z.
2.5 Endocrine and metabolic factors
Thyroid, diabetes and polycystic ovarian syndrome (PCOS) are the conditions associated with an increased risk of miscarriage, the mechanisms thought to be involved are insulin resistance, hyperinsulinemia, hyperandrogenaemia, or increased plasminogen activator inhibitor-1 activity.
2.5.1 Thyroid dysfunction: Thyroid hormones are very crucial for foetal development, thyroid hormone disorders and increased thyroid peroxidase antibodies (TPO-Ab) levels disturbs folliculogenesis, spermatogenesis, embryogenesis and fertilization supporting an important role in pregnancy loss.
Hyperthyroidism: The percentage of hyperthyroidism also called as Graves disease in pregnant women is 0.1-0.4%, which often leads to pregnancy complications such as sporadic pregnancy loss, pre-eclampsia, preterm delivery and congestive heart failure.
Hypothyroidism: Hypothyroidism prevalence was higher in recurrent pregnancy loss women compared to controls based on serum triiodothyronine (T3), thyroxine (T4) and thyroid stimulating hormone (TSH) levels.
Isolated hypothyroxinaemia: Normal female TSH concentration in conjunction with FT4 concentrations in the lower 5th or 10th percentile of the reference range is called as isolated hypothyroxinaemia. Isolated hypothyroxinaemia has been associated with an increased risk of obstetric complications and child neurocognitive impairment.
Thyroid autoantibodies: Thyroid peroxidase autoantibodies (TPOAb) are more relevant in recurrent pregnancy loss compared to antibodies against the thyroid gland. TPOAb prevalence in women of reproductive age is 8-14%. Majority of the women with TPOAb is euthyroid, although it predisposes to hypothyroidism. A meta-analysis reported an association of TPOAb and recurrent pregnancy loss [24].
2.5.2 Polycystic ovary syndrome (PCOS) and Insulin metabolism: Pregnancy complications such as gestational diabetes, pre-eclamptic toxaemia, pregnancy-induced hypertension and probably pregnancy loss are associated with polycystic ovarian syndrome. Obesity, hyperinsulinemia, LH hypersecretion, hyperandrogenism, and thrombophilia are the factors associated with polycystic ovarian syndrome and pregnancy loss and also may be the factors responsible for uncertainty of association between them. Fasting insulin (FI), fasting glucose (FG), the fasting glucose to insulin ratio (FG/FI), and insulin resistance (IR) are the markers frequently used to assess insulin metabolism in women with recurrent pregnancy loss. Insulin resistance was calculated in idiopathic recurrent pregnancy loss and fertile controls with no pregnancy losses and reported a significance between insulin resistance and recurrent pregnancy loss [25]. Higher levels of maternal serum fructosamine a known marker for glycemic control was reported in recurrent pregnancy loss women [26].
2.5.3 Prolactin deficiency: Prolactin is an essential hormone for female reproduction and plays an important role in maintaining corpus luteum function and progesterone secretion. Prolactin levels were associated with an increased risk of miscarriage in subsequent pregnancy in unexplained recurrent pregnancy loss women [27]. Prolactin assessment is done to known ovulatory dysfunction.
2.5.4 Ovarian reserve testing: Taking advanced maternal age into consideration diminished ovarian reserve could be a causative factor for recurrent pregnancy loss. Measurement of follicular stimulating hormone (FSH), estrogen (E2), inhibin B, and anti-Mullerian hormone (AMH) are used for the assessment of ovarian reserve, whereas ultrasound is done to determine antral follicle count (AFC) and ovarian volume. Ovarian reserve was assessed in women with unexplained recurrent pregnancy loss history and compared with fertile controls. FSH levels were higher in recurrent pregnancy loss women, whereas the levels of AMH were lower. Higher levels of diminished ovarian reserve were observed in women with recurrent pregnancy loss [28]. Low levels of AMH and oestradiol were observed in women with unexplained recurrent pregnancy loss [29].
2.5.5 Luteal phase insufficiency: Progesterone is very crucial for secretory transformation of endometrium that allows implantation and maintenance of early pregnancy. Luteal phase insufficiency is a condition where insufficient progesterone exposure to maintain a regular secretory endometrium and allowed for normal implantation and growth. Several endocrinopathies, stress, PCOS and prolactin disorders cause luteal phase insufficiency. Luteal phase defect defined as midluteal was higher among recurrent pregnancy loss women compared to fertile controls [30].
2.5.6 Androgens: Elevated androgen levels are associated with retardation of endometrial development in luteal phase and assessed as a possible cause for recurrent pregnancy loss. Testosterone and androstenedione levels were higher in recurrent pregnancy loss women compared to fertile controls. Testosterone levels were higher in unexplained recurrent pregnancy loss women compared to multiparous women.
2.5.7 Vitamin D: Vitamin D deficiency is one of the risk factors for gestational diabetes and preeclampsia. Decreased vitamin D level were associated with the increased prevalence of antiphospholipid antibody, antinuclear antigen antibody (ANA), anti-ssDNA, and anti-thyroid peroxidase antibody (TPOAb), and with higher peripheral blood CD19+ B and CD56+ NK cell levels and NK cytotoxicity in women with recurrent pregnancy loss. A study reported immune regulatory effects of vitamin Don NK cell cytotoxicity, cytokine secretion and degranulation [31]. Lower expression of Vitamin D Receptor and 25-hydroxyvitamin D3-1α-hydroxylase has been observed in recurrent pregnancy loss women compared to normal pregnant women.
2.5.8 Luteinizing hormone (LH): Luteinizing hormone with high concentrations in the early to mid-follicular phase has been associated with an increased prevalence of pregnancy loss in both PCOS and without PCOS.
2.5.9 Hyperhomocysteinemia: Elevated plasma levels of homocysteine (Hcy) is called as Hyperhomocysteinemia (HHcy), it is one of the risk factors for venous thromboembolism and pregnancy complications such as neural tube defects, pre-eclampsia and placental abruption. Higher levels of homocysteine were observed in women with recurrent pregnancy loss and unexplained infertility. A study reported homocysteine as a significant risk factor for recurrent pregnancy loss [32]. Geographical and ethnic variation plays an important role in genetic pathways of homocysteine metabolism.
2.6 Genetics and RPL
Genetic disorders constitute about 25% of the known causes of recurrent pregnancy loss, which involves both parental and foetal genetic profile. Sporadic and recurrent pregnancy loss occurs due to the presence of genetic abnormalities in the conceptus. By analysing the foetal tissue, it is possible to known whether the early pregnancy loss is due to genetically abnormal foetus. Chromosomal anomalies are one of the most important genetic cause of recurrent pregnancy loss followed by gene copy numbers variation, single gene defect, single nucleotide polymorphism, abnormal micro-RNA expression, and many other genetic and epigenetic factors. Genetic studies of recurrent pregnancy loss help to identify DNA and RNA-based markers exhibiting direct predictive value to a couple’s risk to experience recurrent pregnancy losses and to capture the gene and protein expression profiles, pathways, and net- works involved in recurrent pregnancy loss. Array CGH is a better technique which is in current use. Next generation sequencing (NGS) is a new technique which is not fully used for genetic analysis of pregnancy tissue but in future it may be helpful. Genetic studies carried out in recurrent pregnancy loss shows inconsistency due to differences in study design, definitions of RPL and control group, focus on RPL women instead of couples or placenta, low statistical power due to small sample size, ethnic difference in risk variants.
2.6.1 Single nucleotide polymorphisms (SNPs): Single nucleotide polymorphisms (SNPs) are the most common genomic variations where a single nucleotide is replaced at a specific position in the DNA. SNPs contributes to several diseases including recurrent pregnancy loss. Immune tolerance, inflammation, maternal metabolism and blood coagulation influencing genes are the most common candidate genes studied in recurrent pregnancy loss. Endothelial nitric oxide synthase (eNOS) gene plays an important role in uterine and placental angiogenesis, SNPs of this gene may alter the gene expression leading to recurrent pregnancy loss. Methylation of DNA is most important for gametogenesis and continuation of pregnancy. DNA methyltransferase 3B (DNMT3B) and DNMT3A-448A > G in the 3A promoter region are the common SNPs in recurrent pregnancy loss [33]. SNPs in the promoter region of matrix metalloproteinase-2 (MMP2) and matrix metalloproteinase-9 (MMP9) genes are associated with recurrent pregnancy loss which plays an important role in cell proliferation, apoptosis, and angiogenesis. Cytotoxic T-lymphocyte-associated antigen 4 (CTLA4) gene has a regulatory function and plays a role in the immune tolerance of the maternal-foetal interface. Abnormal expression of this protein is due to the SNPs of the promoter region and exon-1, which might be the key factor for recurrent pregnancy loss. The balance between pro-inflammatory and anti-inflammatory cytokines is very important for successful pregnancy. Interleukin-10 (IL-10) and Toll-like receptors are the anti-inflammatory cytokines most important for embryonic implantation and development, SNPs of these genes may affect their expression and leads to recurrent pregnancy loss. Tumour necrosis factor-alpha (TNF-α) is an inflammatory cytokine that balances several body functions which includes coagulation, angiogenesis, and endothelial functions. Studies have shown that SNPs in the promoter region of the (TNF-α) gene as one of the genetic risk factors for recurrent pregnancy loss [34]. Thrombophilia-associated factor (Leiden factor) mutation, factor II (prothrombin) G20210Amutation and MTHFR C667T variant encoding the methylene tetrahydrofolate reductase enzyme with reduced activity are one of the polymorphisms involved in recurrent pregnancy loss. Chromosome microarray and next generation sequencing are the recent technologies which helps in genome wide screening of SNPs. Recent studies are focusing on the role of genes involved in the functioning of placenta which carries maternal and paternal gene copies instead of mere maternal factors.
2.6.2 Micro-RNA (miRNA) expression: MicroRNAs (miRNAs) are the endogenous and short noncoding molecules transcribed from DNA, plays an important role in gene expression. A single miRNA regulates the expression of multiple genes and different miRNAs can regulate a particular gene. Micro RNAs are involved in several regulatory pathways such as cell growth, differentiation, development. Placenta-specific levels of miRNA expression are important for foetal growth and development. Recent studies showed the role of differential miRNA expression in adverse pregnancy’s [35, 36]. The expression of HLA-G gene was modulated by a 3’ UTR polymorphism exhibiting allele-specific affinity to microRNA smiR-148a, miR-148b, and miR-152and consequent differential mRNA degradation and translation suppression processes [37]. Increased risk of recurrent pregnancy loss was associated with SNPs in pre-miR-[38]. Placenta-specific miRNAs are capable of crossing placental barrier and detectable in maternal plasma, altered profile of several miRNAs has been shown in pregnancy complications.
2.6.3 Epigenetics: Epigenetics regulate, govern and control gene expression which is an important factor for placental development. CpG methylation in DNA, histone modifications in chromatin and non-coding regulatory RNAs are included in epigenetics. Placental epigenome consists of active temporal dynamics that changes epigenetic marks over course of pregnancy. Studies have been carried out on altered placental epigenetics in foetal growth disturbances, preeclampsia and gestational diabetes [39] but studies showing the role of aberrant epigenetic profiling in recurrent pregnancy loss are limited. Increased skewed X-chromosome inactivation (XCI) in women with recurrent pregnancy loss was reported [40]. A study showed XCI association with maternal age and foetal karyotype [41]. Study carried out in hCG beta-subunit coding CGB5 showed monoallelic expression of maternal alleles and hemi methylated gene promoters providing the evidence for the association of methylation allelic polymorphism with pregnancy loss [42]. Methyltransferase(G9aMT) and methylated histone(H3-K9) expressions were lower in decidual/endometrial tissue of recurrent pregnancy loss with unknown aetiology [43]. Abnormal methylation is observed in APC and imprinted PEG3 in chorionic villus samples of abortions and stillbirths [44].
2.6.4 Preimplantation genetic testing (PGT): Preimplantation genetic testing for aneuploidy (PGT-A) previously called as preimplantation genetic screening (PGS) or preimplantation diagnosis of aneuploidy (PGD-A) is a potential treatment proposed for recurrent pregnancy loss where an IVF cycle creates embryos which are biopsied and screened for chromosomal anomalies prior to implantation. An alternative to prenatal diagnosis is preimplantation genetic testing for monogenic/single gene defects (PGT-M) and chromosomal structural rearrangements (PGT-SR) previously PGD which avoids termination of pregnancy in couples with risk of genetic disorders risk. Miscarriage rate was reduced with PGD (PGT-SR) [45]. Couples with translocations opted for PGD (PGT-SR) after genetic counselling.
2.6.5 Male factors: Till now it is considered recurrent pregnancy loss is caused due to female anomalies which contributes to only 50-60% of recurrent pregnancy loss and male factors are not taken into consideration. Male factor such as sperm quality and sperm DNA fragmentation has been related to recurrent pregnancy loss. Male semen quality, occupational exposure and lifestyle effect on recurrent pregnancy loss was examined by semen analysis. Semen from recurrent pregnancy loss group men showed reduced viability, normal morphology and progressive sperm motility and a higher percentage of DNA damaged sperm. Risk of recurrent pregnancy loss increased when smoking, drinking and occupational exposure to environmental factors were added. Several studies recommended for the assessment of male factors such as sperm quality, occupational exposure and lifestyle habits such as smoking, alcohol consumption in recurrent pregnancy loss couples along with female factors [46, 47]. A study reported differences in abnormal sperm chromatin integrity and low sperm concentrations in infertile recurrent pregnancy loss couples, whereas lower percentage of normal morphology was detected in recurrent pregnancy loss couples [48]. Recent studies addressing the role of male factors in recurrent pregnancy loss are focusing on genetic defects such as Y chromosomal deletions, chromatin integrity and DNA damage. Men with high sperm DNA damage showed increased rates of miscarriages compared to men with low sperm DNA damage [49]. Sperm DNA fragmentation shows detrimental effect on pregnancy outcome and miscarriages. Increased sperm DNA fragmentation was observed in couples who experienced recurrent pregnancy loss after natural conception. Males from recurrent pregnancy loss couples are advised to prevent sperm DNA damage caused by unhealthy lifestyles.
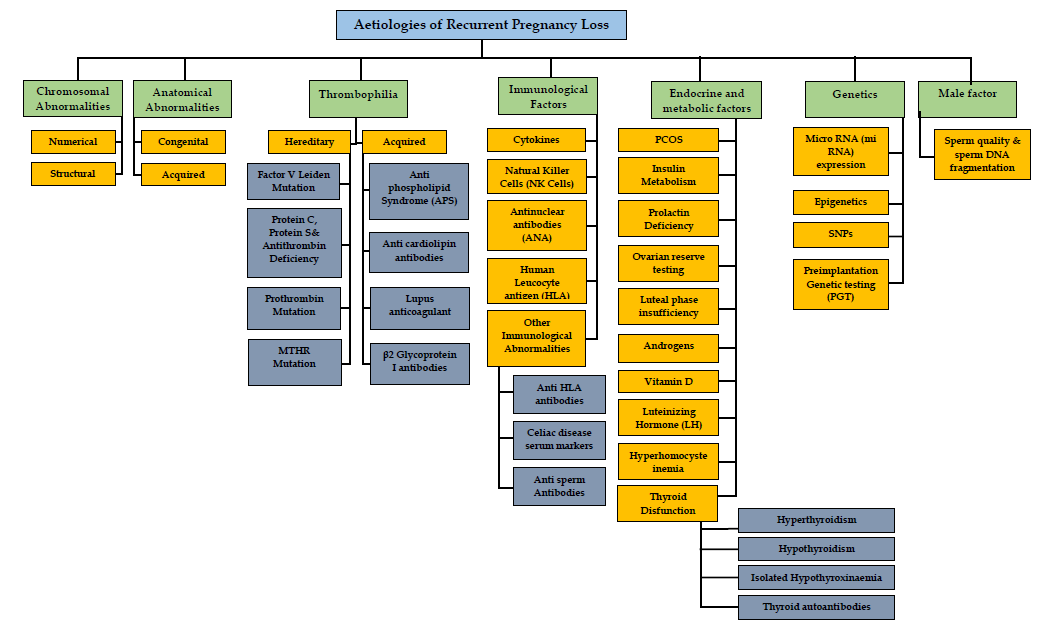
Figure 1: shows the various aetiological factors involved in the causation of recurrent pregnancy loss.
3. Conclusion
Recurrent pregnancy loss should be investigated taking into consideration of the complete clinical history of the couples including known risk factors and their life style habits, which will help the clinician to provide evidence-based treatment to couples to achieve a successful pregnancy. Further research is recommended in the area of unexplained recurrent pregnancy loss to find out the possible underlying patho physiological and genetic mechanisms. Genetic counselling is recommended for the couples with known genetic defects to improve the future care in the recurrent pregnancy loss scenario.
Acknowledgements
Dr. Shehnaz Sultana would like to thank Department of Science and Technology (DST) for funding the project under Women Scientist Scheme (WOS-A).
Conflict of Interest
None of the authors have conflict of interest.
References
- ESHRE guideline ’Recurrent Pregnancy Loss’. ESHRE Early Pregnancy Guideline Development Group Version 2.0 (2017).
- Barber JC, Cockwell AE, Grant E, Williams S, Dunn R, Ogilvie CM. Is karyotyping couples experiencing recurrent miscarriage worth the cost?. Bjog 117 (2010): 885-888.
- Flynn H, Yan J, Saravelos SH, Li TC. Comparison of reproductive outcome, including the pattern of loss, between couples with chromosomal abnormalities and those with unexplained repeated miscarriages. J ObstetGynaecol Res 40 (2014): 109-116.
- Sugiura-Ogasawara M, Aoki K, Fujii T, Fujita T, Kawaguchi R, Maruyama T, et al. Subsequent pregnancy outcomes in recurrent miscarriage patients with a paternal or maternal carrier of a structural chromosome rearrangement. J Hum Genet 53 (2008): 622-628.
- Venetis CA, Papadopoulos SP, Campo R, Gordts S, Tarlatzis BC, Grimbizis GF. Clinical implications of congenital uterine anomalies: a meta-analysis of comparative studies. Reprod Biomed Online 29 (2014): 665-683.
- Jaslow CR, Kutteh WH. Effect of prior birth and miscarriage frequency on the prevalence of acquired and congenital uterine anomalies in women with recurrent miscarriage: a cross-sectional study. FertilSteril 99 (2013): 1916-1922.
- Saravelos SH, Yan J, Rehmani H, Li TC. The prevalence and impact of fibroids and their treatment on the outcome of pregnancy in women with recurrent miscarriage. Hum Reprod 26 (2011): 3274-3279.
- Bradley LA, Palomaki GE, Bienstock J, Varga E, Scott JA. Can Factor V Leiden and prothrombin G20210A testing in women with recurrent pregnancy loss result in improved pregnancy outcomes?: Results from a targeted evidence-based review. Genet Med 14 (2012): 39-50.
- Gao H, Tao FB. Prothrombin G20210A mutation is associated with recurrent pregnancy loss: a systematic review and meta-analysis update. Thromb Res 135 (2015): 339-346.
- Chen H, Yang X, Lu M. Methylenetetrahydrofolate reductase gene polymorphisms and recurrent pregnancy loss in China: a systematic review and meta-analysis. Arch GynecolObstet 293 (2016): 283-290.
- Beydoun H, Saftlas AF. Association of human leucocyte antigen sharing with recurrent spontaneous abortions. Tissue Antigens 65 (2005): 123-135.
- Evaluation and treatment of recurrent pregnancy loss: a committee opinion. FertilSteril 98 (2012): 1103-1111.
- Kruse C, Steffensen R, Varming K, Christiansen OB. A study of HLA-DR and -DQ alleles in 588 patients and 562 controls confirms that HLA-DRB1*03 is associated with recurrent miscarriage. Hum Reprod 19 (2004): 1215-1221.
- Vargas RG, Bompeixe EP, Franca PP, Marques de Moraes M, da GracaBicalho M. Activating killer cell immunoglobulin-like receptor genes' association with recurrent miscarriage. Am J Reprod Immunol 62 (2009): 34-43.
- Fan W, Li S, Huang Z, Chen Q. Relationship between HLA-G polymorphism and susceptibility to recurrent miscarriage: a meta-analysis of non-family-based studies. J Assist Reprod Genet 31 (2014): 173-184.
- Nielsen HS, Wu F, Aghai Z, Steffensen R, van Halteren AG, Spierings E, et al. H-Y antibody titers are increased in unexplained secondary recurrent miscarriage patients and associated with low male: female ratio in subsequent live births. Hum Reprod 25 (2010): 2745-2752.
- Piosik ZM, Goegebeur Y, Klitkou L, Steffensen R, Christiansen OB. Plasma TNF-alpha levels are higher in early pregnancy in patients with secondary compared with primary recurrent miscarriage. Am J Reprod Immunol 70 (2013): 347-358.
- Lee SK, Na BJ, Kim JY, Hur SE, Lee M, Gilman-Sachs A, et al. Determination of clinical cellular immune markers in women with recurrent pregnancy loss. Am J Reprod Immunol 70 (2013): 398-411.
- Kruse C, Varming K, Christiansen OB. Prospective, serial investigations of in-vitro lymphocyte cytokine production, CD62L expression and proliferative response to microbial antigens in women with recurrent miscarriage. Hum Reprod 18 (2003): 2465-2472.
- Cavalcante MB, Costa FD, Araujo Junior E, Barini R. Risk factors associated with a new pregnancy loss and perinatal outcomes in cases of recurrent miscarriage treated with lymphocyte immunotherapy. J Matern Fetal Neonatal Med 28 (2015): 1082-1086.
- Souza SS, Ferriani RA, Santos CM, Voltarelli JC. Immunological evaluation of patients with recurrent abortion. J Reprod Immunol 56 (2002): 111-121.
- Tuckerman E, Laird SM, Prakash A, Li TC. Prognostic value of the measurement of uterine natural killer cells in the endometrium of women with recurrent miscarriage. Hum Reprod 22 (2007): 2208-2213.
- Thangaratinam S, Tan A, Knox E, Kilby MD, Franklyn J, Coomarasamy A. Association between thyroid autoantibodies and miscarriage and preterm birth: meta-analysis of evidence. BMJ 342 (2011): d2616.
- Ispasoiu CA, Chicea R, Stamatian FV, Ispasoiu F. High fasting insulin levels and insulin resistance may be linked to idiopathic recurrent pregnancy loss: a case-control study. Int J Endocrinol (2013): 576926
- Romero ST, Sharshiner R, Stoddard GJ, Ware Branch D, Silver RM. Correlation of serum fructosamine and recurrent pregnancy loss: Case-control study. J ObstetGynaecol Res 42 (2016): 763-768.
- Li W, Ma N, Laird SM, Ledger WL, Li TC. The relationship between serum prolactin concentration and pregnancy outcome in women with unexplained recurrent miscarriage. J ObstetGynaecol 33 (2013): 285-288.
- Atasever M, Soyman Z, Demirel E, Gencdal S, Kelekci S. Diminished ovarian reserve: is it a neglected cause in the assessment of recurrent miscarriage? A cohort study. FertilSteril 105 (2016): 1236-1240.
- Pils S, Promberger R, Springer S, Joura E, Ott J. Decreased Ovarian Reserve Predicts Inexplicability of Recurrent Miscarriage? A Retrospective Analysis. PLoS One 11 (2016): e0161606.
- Li TC, Spuijbroek MD, Tuckerman E, Anstie B, Loxley M, Laird S. Endocrinological and endometrial factors in recurrent miscarriage. Bjog 107 (2000): 1471-1479.
- Ota K, Dambaeva S, Kim MW, Han AR, Fukui A, Gilman-Sachs A, et al. 1,25-Dihydroxy-vitamin D3 regulates NK-cell cytotoxicity, cytokine secretion, and degranulation in women with recurrent pregnancy losses. Eur J Immunol 45 (2015): 3188-3199.
- Puri M, Kaur L, Walia GK, Mukhopadhhyay R, Sachdeva MP, Trivedi SS, et al. MTHFR C677T polymorphism, folate, vitamin B12 and homocysteine in recurrent pregnancy losses: a case control study among North Indian women. J Perinat Med 41 (2013): 549-554.
- Liu Y, Zheng H, Guo P, Feng S, Zhou X, Ye D, et al. DNA methyltransferase 3A promoter polymorphism is associated with the risk of human spontaneous abortion after assisted reproduction techniques and natural conception. Journal of Assisted Reproduction and Genetics 34 (2017): 245-252.
- Parveen F, Agrawal S. A Study of forty-seven single nucleotide polymorphisms among recurrent miscarriage using classification and regression tree analysis. Am J Reprod Immunol 70 (2013): 529-537.
- Amin-Beidokhti M, Mirfakhraie R, Zare-Karizic S, Karamoddin F . The role of parental microRNA alleles in recurrent pregnancy loss: an association study. Reproductive analysis. European Journal of Obstetrics &Gynecology and Reproductive Biology 215 (2017): 93-100.
- Yang Q, Gu WW, Gu Y, Yan NN, Mao YY, Zhen XX, et al. Association of the peripheral blood levels of circulating microRNAs with both recurrent miscarriage and the outcomes of embryo transfer in an in vitro fertilization process. J Transl Med 16 (2018): 186.
- Tan Z, Randall G, Fan J, Camoretti- Mercado B, Brockman-Schneider R, Pan L, et al. Allele-specific targeting of microRNAs to HLA-G and risk of asthma. Am.J. Hum. Genet 81 (2007): 829-834.
- Hu Y, Liu CM, Qi L, He TZ, Shi-Guo L, Hao CJ, et al. Two common SNPs in pri-miR-125a alter the mature miRNA expression and associate with recurrent pregnancy loss in a Han-Chinese population. RNABiol 8 (2011): 861-872.
- Nelissen EC, vanMontfoort AP, Dumoulin JC, Evers JL. Epigenetics and the placenta. Hum. Reprod 17 (2011): 397-417.
- VandenVeyver IB. Skewed X inactivation in X-linked disorders. Semin.Reprod.Med 19 (2001): 183-191.
- Warburton D, Kline J, Kinney A, Yu CY, Levin B, Brown S. Skewed X-chromosome inactivation and trisomic spontaneous abortion: no association. Am.J. Hum. Genet 85 (2009): 179-193.
- Uuskula L, Rull K, Nagirnaja L, Laan M. Methylation allelic polymorphism (MAP) in chorionic gonadotropinbeta5(CGB5) and its association with pregnancy success. J. Clin.Endocrinol. Metab 96 (2011): E199- E207.
- Fatima N, Ahmed SH, Salhan S, Rehman SM, Kaur J, Owais M, et al. Study of methyltransferase(G9aMT) and methylated histone (H3-K9) expressions in unexplained recurrent spontaneous abortion (URSA) and normal early pregnancy. Mol. Hum. Reprod 17 (2011): 693-701.
- Zechner U, Pliushch G, Schneider E, ElHajj N, Tresch A, Shu- faro Y, et al. Quantitative methylation analysis of developmentally important genes in human pregnancy losses after ART and spontaneous conception. Mol. Hum. Reprod 16 (2009): 704-713.
- Brezina PR, Anchan R, Kearns WG. Preimplantation genetic testing for aneuploidy: what technology should you use and what are the differences? J Assist Reprod Genet 33 (2016): 823-832.
- De Krom G, Arens YH, Coonen E, Van Ravenswaaij-Arts CM, Meijer-Hoogeveen M, Evers JL, et al. Recurrent miscarriage in translocation carriers: no differences in clinical characteristics between couples who accept and couples who decline PGD. Hum Reprod 30 (2015): 484-489.
- Anifandis G, Bounartzi T, Messini CI, Dafopoulos K, Sotiriou S, Messinis IE. The impact of cigarette smoking and alcohol consumption on sperm parameters and sperm DNA fragmentation (SDF) measured by Halosperm ((R)). Arch GynecolObstet 290 (2014): 777-782.
- Jensen TK, Gottschau M, Madsen JO, Andersson AM, Lassen TH, Skakkebaek NE, et al. Habitual alcohol consumption associated with reduced semen quality and changes in reproductive hormones; a cross-sectional study among 1221 young Danish men. BMJ 4 (2014): e005462.
- Zhang L, Wang L, Zhang X, Xu G, Zhang W, Wang K, et al. Sperm chromatin integrity may predict future fertility for unexplained recurrent spontaneous abortion patients. Int J Androl 35 (2012): 752-757.
- Robinson L, Gallos ID, Conner SJ, Rajkhowa M, Miller D, Lewis S, et al. The effect of sperm DNA fragmentation on miscarriage rates: a systematic review and meta-analysis. Hum Reprod 27 (2012): 2908-2917.


 Impact Factor: * 3.4
Impact Factor: * 3.4 Acceptance Rate: 78.89%
Acceptance Rate: 78.89%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 