Young South Asians with ST-Elevation Myocardial Infarction (STEMI) – Outcomes, Clinical and Angiographic Profiles
Salik ur Rehman1*, Aysha Almas2, Aisha Siddiqui3, Sania Sabir Sethi4, Safia Awan3, Aamir Hameed Khan5
1Department of Cardiology, Aga Khan University Hospital, Karachi, Pakistan
2Associate Professor of Medicine, Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan
3Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan
4Research Assistant, Department of Medicine, Aga Khan University Hospital, Karachi, Pakistan
5Professor of Cardiology, Section of Adult Cardiology, Aga Khan University Hospital, Karachi, Pakistan
*Corresponding author: Salik ur Rehman, MBBS, FCPS (Cardiology), Instructor, Adult Cardiology, Aga Khan University Hospital, Karachi, Pakistan
Received: 26 July 2021; Accepted: 03 August 2021; Published: 09 August 2021
Article Information
Citation:
Salik ur Rehman, Aysha Almas, Aisha Siddiqui, Sania Sabir Sethi, Safia Awan, Aamir Hameed Khan. Young South Asians with ST-Elevation Myocardial Infarction (STEMI) – Outcomes, Clinical and Angiographic Profiles. Archives of Internal Medicine Research 4 (2021): 200-211.
View / Download Pdf Share at FacebookAbstract
Background: Why STEMI in young South Asians (SAs) has more adverse outcomes compared to elder population is underexplored. We conducted this study to learn about common risk factors, disease patterns and prognostic factors in this population.
Methods: It was an observational study from 2013-2019 done at the Aga Khan University Hospital, Karachi, Pakistan, a tertiary care hospital. Patients aged <45 years who presented with their first episode of ST elevated Myocardial Infarction (STEMI) and who underwent Primay PCI were included. Patients with previous MI or revascularization were excluded. Details of risk factors, lesion complexity and outcomes were noted. Main outcome measures were: • Primary outcome of 30 day All-cause mortality • Secondary outcomes: (a) Composite of Shock/CPR/VT/Vfib, (b) Ejection fraction <35%, (c) Delayed discharge >5 days
Results: Of a total of 1207 patients, only 165 patients (13%) were <45 years old. Common risk factors included male gender 90.3%, n=149, obesity in 48.3%, n=69, history of tobacco in 45%, n=74 and positive family history in 48.4%, n=80. LAD was the culprit in 77.0%, n=127 with Single vessel disease (SVCAD) in 68%, n=112. Primary outcome of 30 day All-cause mortality was seen in 3.6%, n=6 patients. Secondary outcomes: (i) Composite of Shock/CPR/VT/Vfib was seen in 12%, n=20 associated to initial SBP <110 mmhg (OR 4.1, 95% CI 1.2-13.4) or heart failure (OR 3.5, 95% CI 1.0-12.6). (ii) Ejection fraction <35% was seen in 29%. n=48 associated to anterior infarction (OR 5.0, 95% CI 1.8-13.5), Time to hospital (TTH) >4 hours (OR 2.6, 95% CI 1.0-6.7) and heart failure (OR 5.1, 95% CI 1.7-15.4). (iii) Delayed discharge >5 days was seen in 27.3%, n=45 associated to TTH >4 hours (OR 3.8, 95% CI 1.3-11.2), the Composite of Shock/CPR/VT/VF (OR 6.4, 95% CI 1.9-21.6) and HTN (OR 2.1, 95% CI 1.0-5.2).
Conclusion: <
Keywords
<p>Young, ST-elevation Myocardial Infarction, South Asian</p>
Article Details
1. Introduction
Ischemic Heart disease (IHD) is the commonest causeof deathsglobally. In 2016, Cardiovascular diseases (CVD) constituted 31% of all global deaths with 85% due to heart attack and stroke combined. However, deaths due to CVDs occur primarily in Low- and middle-income countries (LMIC) [1]. In 2013, nearly 40% of all deaths in South Asia occurred due to CVDs where there were 125.7 deaths for every 100,000 individuals [2]. This can be attributed to delayed identification and treatment of risk factors, insufficient health facilities and poverty [1]. Whereas there is vast data for IHD in the elder, data focusing on the clinical features, risk factors and outcomes in young patients is lacking.
Most studies have used an age of 40 to 45 years to define "young" patients with coronary artery disease (CAD) as they have less traditional risk factors, have Single vessel disease (SVCAD) and a favorable prognosis [3]. South Asian (SA) ethnicity is itself a risk factor for Premature Coronary Artery Disease (PMCAD) with adverse outcomes [4]. Whereas mortality from CAD has improved in elder patients who are treated for risk factors, the incidence of death in young patients is static likely due to a high burden of unidentified and unaddressed risk factors and increasing prevalence of diabetes mellitus (T2DM), obesity, and hypertension (HTN) in developed countries [5]. As CAD prevention guidelines primarily address the traditional risk factors, they underestimate risks particular to the young population resulting in a static death incidence.
Mean age of onset of CAD in SAs is much younger (53 years) compared to European figures of 63 [6]. This correlates with the mean age of 52.2 years for patients presenting with acute coronary syndromes (ACS) in Pakistan [7]. MI at a young age can have serious effects on one’s mental health, working capability, and socioeconomic status and it can effect multiple dependents. As the data is scarce, in-depth research into this will help in designing better preventive measures and impact outcomes. We, therefore, designed this study to describe the risk factor profile in patients <45 years of age with acute MI who require urgent coronary intervention. Additionally, we will also comment on the anatomy of the coronary lesions and outcomes in this young patient population.
2. Methods
We conducted an observational study from January 2013 to December 2019 at the Aga Khan University Hospital (AKUH), Karachi, Pakistan. All patients were admitted with the first presentation of STEMI, aged 18 to 45 years and who underwent emergent Coronary Angiography (CAG) with/without Percutaneous Coronary Intervention (PCI). Data were extracted using Health Information Management System (HIMS) using the ICD 10 Version 2019 diagnosis code 121.0-121. Patients with history of MI, revascularization or stroke or who were dialysis-dependent were excluded. Ethical exemption from ethical review committee at AKUH was obtained. Information was collected for risk factors, outcomes, and coronary anatomy on pre-designed data collection form.
2.1 Risk factors for CAD
Data for risk factors including obesity, T2DM, HTN, smoking, family history of Prematue Coronary Artery Disease (FHx-PMCAD) and lipid profile was collected. Those with an HbA1c between 5.7-6.4% were classified as pre-diabetic and those with a known history or HbA1c values >6.5% were grouped as diabetics [8]. FHx-PMCAD was deemed positive if a parent, sibling, or a first-degree relative had CAD (<55 years for males and <65 years for females) or there was a history of sudden cardiac death (SCD) [9]. HTN was defined as SBP >140/90 mmHg or patients with a known history of HTN or taking antihypertensive medicines [10].
Tobacco use was counted as positive if the patient was a former or current smoker or used chewable tobacco [11]. Obesity was defined as per the Asian cut-off value of a BMI of >27.5 kg/m2 [12]. LDL-C levels >150 mg/dl and LDL-C/HDL-C ratio >2.7 were considered elevated on presentation with ACS as they correlate well with increased risk of stent thrombosis, target lesion revascularization, and MACE [13, 14].
2.2 Coronary angiography (CAG)
Patients undergoing CAG that included at least one expert interventional cardiologist were included. At our center, eyeballing method is used to estimate the percentage, morphology, and length of the coronary lesion. Coronary vessels with stenosis >50% were counted as significant and counted as diseased. Any stenosis <50% was classified as non-obstructive [15]. Diseased vessels were classified as one vessel disease (SVCAD), two-vessel disease (2VCAD), or three vessel disease (3VCAD). Each vessel was sub-classified as either a proximal segment or mid to distal segment based on the origin of major branches, the first septal in case of Left Anterior Descending (LAD), the Right ventricular marginal (RV marginal) in case of Right Coronary Artery (RCA), and first Obtuse marginal (OM1) in case of the Left Circumflex (LCx). An isolated diseased major branch (first diagonal or obtuse marginal) deemed necessary to revascularize was counted as branch vessel disease and classified along with the proximal segments of the vessels i.e. proximal LAD and proximal LCx respectively.
2.3 Outcomes
Data were collected to look for the primary outcome of All-cause mortality within 30 days after STEMI or related to the immediate consequences of STEMI, whether in-hospital or in a subsequent hospital visit. Data was also collected for variables such as Cardiogenic shock (CS), Cardio-pulmonary resuscitation (CPR), Ventricular Tachycardia (VT) or Ventricular Fibrillation (VF), need for temporary pacing, invasive ventilation, and Ejection fraction (LVEF) on a transthoracic echocardiogram (TTE). CS was defined as the presence of systolic blood pressure (SBP) <90mmHg for at least 30 minutes and/or need for one or more vasopressor agents to maintain SBP >90 mmHg in the absence of hypovolemia or sepsis along with a clinical presentation of ACS [16]. Secondary outcomes included patients with a (i) composite outcome of CS/CPR, VT, or VF, (ii) initial LVEF <35% on TTE, or (iii) delayed length of stay (LOS) up to 5 days or more.
2.4 Statistical analysis
Data analysis was performed by using SPSS version 22.0. Chicago. Continuous variables were calculated as mean ± (SD), and categorical variables were presented as counts and percentages. To evaluate the association between outcome variables and demographic and related factors, exploratory variables including an anterior infarction, SBP <110, Time to hospital (TTH) >4 hours on presentation to the emergency unit, pre-PCI fibrinolysis, gender, obesity, positive FHx-PMCAD, tobacco use, T2DM or history of HTN were used. A chi-square -test was used to compare categorical variables and a student t-test was used for continuous variables. Odds Ratios (OR) and their 95% confidence intervals (CI) were estimated using Logistic Regression. All p-values were two-sided and considered as statistically significant if < 0.05.
3. Results
Out of 1207 patients, 165 patients (13%) patients were <45 years old and fulfilled the inclusion criteria. Out of these, 90.3% (n=149) patients were male and only 9.7% (n=16) patients were female. The mean age in this population was 39.5 years (SD 5.1).
3.1 Risk factors
Nearly half of the patients (n=69, 48.3%) were obese and had a BMI of (> 27.5 kg/m2) and a significant proportion was overweight (38%). Data for BMI was missing for 22 patients. Similarly, nearly half of the patients had a positive FHx-PMCAD (n=80, 48.4%) or history of tobacco use (n=74, 45%). Baseline characteristics and risk factors in young STEMI patients (<45 years) are shown in Table 1.Of all these patients, 2.4% of patients (n=4) had chronic kidney disease but were non-dialysis dependent. Nearly 8.5% (n=14) patients received fibrinolysis before arriving at our center. Data for lipids were present only for a third of patients (n=49). Three patients presented in their early twenties and had a history of cocaine, hyperhomo-cysteinemia, or pheochromocytoma respectively.
3.2 Coronary anatomy
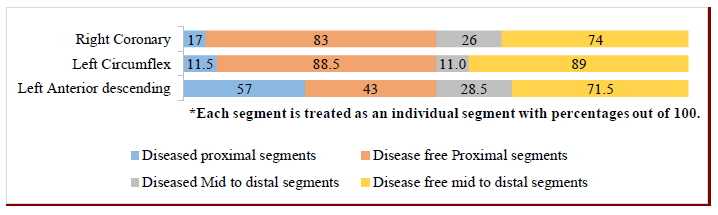
Less than two-third patients (n=102, 62%) had Anterior infarction of which a third (n=39) had extensive anterio-lateral STEMI. A third of patients (n=62, 37.2%) presented with inferoposterior or inferolateral infarction. A minority (1.8%, n=3) presented with lateral STEMI. More than two-third patients (n=112, 68%) had SVCAD followed by 2VCAD in 23% (n=38) and 3VCAD in a minority (n=13, 8%). Nearly three-fourths (n=127, 77%) had lesions in LAD. Right coronary artery (RCA) was the second most involved vessel in 37.3% (n=61) followed by Left Circumflex (LCx) in 23.6% (n=39) cases. Each proximal or distal segment was assigned a disease percentage out of the total number of patients i.e. 165 (Figure 1). Isolated branch vessel disease was present in only five patients, that also in the OM1 requiring PCI. They were classified as ‘proximal LCx.’ Only six patients (3.6%) had Left Main (LM) or LM equivalent disease. Around 93% (n=154) patients received revascularization via PCI. The mean length of stents placed in proximal LAD was 25 (+ 8.4) mm with a mean diameter of 3.1 (+ 0.5) mm. Nearly 4.2% (n=7) patients underwent revascularization via emergent CABG. Only 3 patients underwent medical therapy either due to STEMI from a small branch that was non-significant or excess thrombus burden for which, the patient was put on oral anticoagulation.
3.3 Outcomes
A primary outcome of all-cause mortality was observed in nearly 3.6 % of the patients (n=6). In the secondary outcomes, the composite of CS, CPR, VT, or VF was seen in 12% (n=20) whereas less than a third of patients (n=48, 29%) had LVEF <35%. Similarly, 27.3% patients (n=45) were discharged on or after the fifth day of the indexed admission. Patients with history of HTN (OR 2.1, 95% CI 1.0-5.2) or T2DM (OR 2.5, 95% CI 1.0-6.7) were at borderline risk to have increased length of stay even after adjustment for other comorbids and gender (Table 2). Patients with heart failure symptoms on presentation requiring diuresis were at a borderline risk for the composite outcome (OR 2.6, 95% CI 1.0-7.8) whereas those with initial SBP <110 mmhg were at a higher risk (OR 3.4, 95% CI 1.1-9.8) (Table 3). Similarly, patients with heart failure symptoms were also at risk for LVEF <35% (OR 5.1, 95% CI 1.7-15.4). Also Anterior location of STEMI was a risk factor for LVEF <35% (OR 5.0, CI 1.8-13.5). TTH > 4 hours imparted a borderline risk (OR 2.6. 95% CI 1.0-6.7) for LVEF <35% but was significantly associated to LOS >5 days (OR 3.8, 95% CI 1.3-11.2). Patients who had the composite outcomes of shock/CPR/VT or VF were at a higher risk of LOS >5 days (OR 6.4, 95% CI 1.9-21.6) but with a wide confidence interval after adjustment for other predictors. (Table 3). Only 4 patients were lost to follow-up. Two patients had stent thrombosis and presented within a week of PCI. A minority (7.9%, n=13) required invasive mechanical ventilation. Temporary pacing was required by 4.2% (n=7) of patients. None of our patients suffered from a periprocedural stroke.
|
Description |
Patients (n=165) and percentages |
|
Mean Age (SD) |
39.5 (+ 5.1) |
|
Males |
149 (90.3%) |
|
Mean BMI (SD) (kg/m2) |
27.9 (+ 5.7) |
|
Obese (BMI >27.5 kg/m2) * |
69 (48.3%) |
|
Overweight [BMI (kg/m2) 23-27.5]** |
54 (38%) |
|
History of Tobacco use |
74 (45%) |
|
Positive family history |
80 (48.4%) |
|
Elevated sugars |
60 (36%) |
|
-Prediabetes |
22 (13.3%) |
|
-Diabetes |
38 (23%) |
|
Mean Random blood sugar (mg/dl) |
161.5 (+ 82.4) |
|
Hypertension |
51 (31 %) |
|
Pre-PCI fibrinolysis |
14 (8.5%) |
|
LDL-C >150 (mg/dl)*** |
17.6 % |
|
LDL-C/HDL-C ratio >2.7*** |
80.0 % |
* Cutoff for obesity in South Asian population
** Cutoff for overweight in South Asian Population
*** Data was present only for a third of the subjects (n=49)
Table 1: Baseline characteristics and risk factors in young STEMI patients (<45 years).
|
Composite outcome |
LVEF<35% |
LOS >5 days |
||||
|
(Shock, CPR, VT/VF) |
||||||
|
Co-morbids |
Unadjusted OR(95 % CI) |
Adjusted* OR(95 % CI) |
Unadjusted OR(95 % CI) |
Adjusted* OR(95 % CI) |
Unadjusted OR(95 % CI) |
Adjusted* OR(95 % CI) |
|
Obesity |
1.0 (0.5-2.1) |
1.0 (0.5-2.1) |
1.1 (0.6-1.9) |
1.1 (0.6-2.0) |
0.5 (0.3-1.0) |
0.5 (0.3-1.0) |
|
Hypertension |
2.0 (0.7-5.6) |
2.0 (0.7-5.6) |
1.0 (0.4-2.3) |
1.0 (0.4-2.3) |
2.1 (1.0-5.1) |
2.1 (1.0-5.2) |
|
DM |
1.7 (0.5-5.2) |
1.8 (0.5-5.5) |
0.9 (0.4-2.4) |
0.8 (0.3-2.2) |
2.7 (1.0-7.1) |
2.5 (1.0-6.7) |
|
Tobacco |
2.1 (0.8-6.0) |
2.1 (0.7-6.0) |
0.5 (2.4-1.2) |
0.6 (0.2-1.4) |
1.0 (0.3-2.1) |
1.0 (0.3-2.3) |
|
Family history |
0.4 (0.1-1.0) |
0.4 (0.1-1.0) |
0.7 (0.3-1.5) |
0.7 (0.3-1.5) |
0.3 (0.1-1.0) |
0.3 (0.1-1.0) |
*adjusted for gender
Table 2: Associations of risk factors with Composite outcome, reduced Ejection fraction <35% or LOS >5 days.
|
Clinical Predictors |
Composite of Shock/CPR/VT or VF |
EF<35% |
|||
|
Unadjusted OR(95 % CI) |
Adjusted* OR(95 % CI) |
Unadjusted * OR(95 % CI) |
Adjusted OR(95 % CI) |
||
|
Anterior STEMI |
1.0 (0.3-2.9) |
1.0 (0.3-3.2) |
4.6 (1.7-12.4) |
5.0 (1.8-13.5) |
|
|
TTH >4hours |
1.0 (0.3-2.9) |
1.4 (0.4-4.6) |
2.6 (1.1-6.3) |
2.6 (1.0-6.7) |
|
|
SBP<110 mmhg |
3.4 (1.1-9.8) |
4.1 (1.2-13.4) |
1.5 (0.5-4.3) |
1.6 (0.5-5.0) |
|
|
Heart failure symptoms |
2.6 (1.0-7.8) |
3.5 (1.0-12.6) |
4.3 (1.6-11.7) |
5.1 (1.7-15.4) |
|
|
Pre-hospital thrombolysis |
0.9 (0.1-5.2) |
0.9 (0.1-6.0) |
0.9 (0.2-3.6) |
0.9 (0.2-4.0) |
|
|
*Adjusted for gender, risk factors including obesity, positive FHx-PMCAD, tobacco consumption, T2DM and HTN. |
|||||
|
Clinical Predictors |
Length of stay (LOS) 5 days or more |
||||
|
Unadjusted OR(95 % CI) |
Adjusted** OR(95 % CI) |
||||
|
Anterior STEMI |
1.39 (0.5-3.1) |
1.5 (0.5-3.9) |
|||
|
TTH >4hours |
3.9 (1.5-10) |
3.8 (1.3-11.2) |
|||
|
SBP<110 mmhg |
1.0 (0.6-4.7) |
2.1 (0.7-6.8) |
|||
|
Heart failure symptoms |
1.0 (0.3-3.0) |
1.0 (0.3-3.4) |
|||
|
Pre-hospital thrombolysis |
1.2 (0.3-5.0) |
0.7 (0.1-3.1) |
|||
|
Composite of CPR/VT/VF |
6.7 (2.3-19.4) |
6.4 (1.9-21.6) |
|||
**Adjusted for gender, risk factors including obesity, positive FHx-PMCAD, tobacco consumption, T2DM and HTN.
Table 3: Associations of clinical predictors with Composite outcome, reduced Ejection fraction <35% or LOS >5 days.
4. Discussion
This was an observational study recruitng young STEMI patients. Majority were male, obese, tobacco users, and with positive FHx-PMCAD. Anterior STEMI was the commonest presentation with Proximal LAD involvement and SVCAD as the commonest pattern. Overall mortality was found to be 3.6%. Studies show a prevalence of 1.2% of CAD in young patients however, prevalence in young SAs may vary from 5% to 10% [6]. SAs with IHD are more likely to have male gender, complex coronary disease, and anterior infarction [17]. The landmark study by Salim Yusuf conducted in 52 countries showed that risk factors responsible for PMCAD are smoking, HTN, T2DM and obesity [18]. The reason for higher obesity is the use of high cholesterol diet and lack of physical activity in addition to lack of facilites, sedentary lifestyle and lack of awareness about risk factors leading to a lack of health-seeking behavior at an early age [19, 20]. Tobacco use, whether smoked or chewed is also quite prevalent in Asia with mean age of smoking initiation a little later than 20 years [21]. It significantly increases the risk of all-cause mortality in young adults and cessation can reduce risk [22]. Given the high burden of tobacco products in an LMIC, cost-effective and evidence-based interventions are critical to avoid future risk [23]. FHx-PMCAD as a risk factor can be attributed to genetic causes such as dysfunctional and lower levels of HDL-C, and higher Lipoprotein (a) concentrations [18, 24]. Further research regarding the inheritance patterns and ways to intervene is still required. Traditional risk factors like T2DM and HTN are less prevalent in young patients however, the INTERHEART study showed a higher prevalence of T2DM, increased waist-hip ratio, and increased ApoB100/ApoA-I ratio in young SAs compared to other ethnicities [18]. This demands immediate screening and preventive measures at a much younger ages. High LDL-C/HDL-C ratio i.e. >2.7 has been associated with higher rates of target lesion revascularization (TLR), stent thrombosis (ST), and MACE in ACS patients receiving DES. Moreover, LDL-C levels as high as >150 mg/dl on presentation with ACS also predict microvascular injury [13]. In one study, as high as 50% of the patients presenting with ACS had a high LDL-C/HDL-C ratio >2.7 [14]. In our study, nearly 80% of the patients had elevated LDL-C/HDL-C ratios.
The proximal segments of the coronary arteries form a bridging zone between elastic and muscular artery types such that these segments are more likely to develop foam cell lesions and lipid core plaque [25]. Foam cell lesions are already present in childhood and adolescent ages [26]. Also, a hemodynamic basis might be responsible for the development of atherosclerotic plaques in proximal segments [27]. At young ages, SVCAD with LAD involvement is the commonest pattern that can be explained partly by dynamic compression of the septal perforators with disturbed blood flow in the adjacent LAD segment favoring atherosclerosis [27]. Followed by LAD, the disease appears to cluster in the RCA and lastly the LCx [28]. This same pattern of disease was also determined by a few studies done in SAs in addition to the fact that SAs were more likely to have complex (Type B or C) disease [29]. International studies have shown a favorable prognosis in young patients with mortality rates as low as 1.6% at 30 days rising to 2.7% per year. In contrast, young SAs have higher in-hospital mortality, as high as 2.8% as do SA immigrants [30]. Although our study showed a 30 day mortality in only 3.6% (n=6), it was still higher compared to international data. This might be explained by higher risk factor clustering at young ages, lack of protective factors like exercise and healthy diet and lack of awareness about risk factors and symptoms for CAD in addition to a deficiency of appropriate health facilities [31].
CS and Sudden Cardiac Arrest (SCA) are known poor predictors after STEMI. Studies have quoted that nearly 5% of young STEMI patients present with cardiogenic shock and 1.7% and 0.3% of patients might present with VT and VF [30, 32]. Risk factors such as elder age, ischemia time, anterior infarction or shock index can predict the occurrence of CS [33]. However, all these studies have included patients from all age groups and might not be a true representation of the young subgroup. Our study found that patients with initial SBP <110 mmHg and signs and symptoms of heart failure had borderline elevated risk for the composite outcome. Low admission SBP is known to be a predictor of short term mortality as well as CS. Initial SBP between 130 to 140mmHg correlate with the lowest event rates [34]. Also, signs and symptoms of heart failure predict the development of CS and other adverse outcomes and initial aggressive therapy might be preventive [35]. Patients with Severe LV dysfunction have increased risk of mortality. SCD-HeFT and MADIT-II trials showed mortality benefit of Implantable Cardioverter Defibrillator (ICD) in patients with an LVEF <35% around 90-days after revascularization for primary prevention [36, 37]. Elder age, increased TTH, proximal occlusion and multivessel stenosis are predictors of reduced LVEF in ACS patients and may also dictate mortality. TTH >5hours is known to predict LV dysfunction regardless of the coronary vessel involved likely due to impaired microcirculation that causes extensive myocardial ischemia, injury and infarction along with a higher risk of cardiac complications [38]. Our study found the anterior location of infarction, TTH >4 hours, or heart failure symptoms requiring diuresis to be independently associated to EF<35% after adjustment of other factors.
Low-risk patients may be safely discharged early which is cost-effective and adds to the benefits of PPCI [39]. Not much data is available focusing on predictors of delayed discharge in young patients, modification of which might be cost-effective. Patients with HTN are more likely to develop CS and hence may be at risk of increased LOS [34]. This can be due to greater endothelial injury in addition to the fact that HTN usually co-exists with other CV risk factors [40]. Similarly, patients with a TTH >4 hours or who develop CS/CPR/VT/VF maybe more likely to stay up to 5 days or more due to more myocardial damage [38].
4.1 Strength and limitations
To the best of our knowledge, this is the first study that has addressed the outcomes of young Pakistani patients with STEMI with a significant sample size. However, there are several limitations. This was a single-center observational study and the results may not be generalizable with some residual confounders including dietary patterns, medications and exercise status, effecting the clinical outcomes. Patients who died before receiving revascularization could not be included. Significant data on lipid profiles was missing which is why it was not included in the regression analysis. Also, this study lacks the long-term outcomes of this population due to a limited follow-up. Due to the fewer number, this study was limited in delineating predictors for mortality. In terms of secondary outcomes, this study was able to identify the relationship with some variables like TTH, anterior infarction, SBP<110 mmHg, and heart failure symptoms, however, larger studies with adequate sample size and power are further required to testify and expand on these impressions.
5. Conclusion
In conclusion, STEMI in young patients is not uncommon and SAs have increased mortality. Obesity, positive FHx-PMCAD, and tobacco use are common risk factors and SVCAD involving the LAD is the most common CAG finding. Various factors such as anterior infarction, delayed presentation, initial SBP, and heart failure symptoms may help stratify these patients.
Declarations
Ethics approval and consent to participate: Ethical exemption from Ethical Review Committee (ERC) at the Aga Khan University Hospital (AKUH) was obtained (ERC number 5438-Med-ERC-18) in accordance with declaration of Helsinki. The committee waived the need of informed consent for the study.
Consent for publication:
Not applicable.
Availability of data and materials:
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
Competing interests:
The authors declare that they have no competing interests.
Authors contributions:
All authors were involved in reviewing the manuscript. Dr. Salik ur Rehman Iqbal (SR), Dr. Aysha Almas (AA), Dr. Aisha Siddiqui (AS) and Dr. Aamir Hameed Khan (AHK) participated in writing the main manuscript text. AS, SR and SS were involved in data collection. AS, SR, SS and Safia Awan were involved in preparing figures and tables for the study.
Funding:
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Acknowledgments:
I would like to acknowledge Javeriah Khan for providing the most accurate patient records and also Nobel Joseph who made it possible to recruit files for data collection.
Authors information:
Dr. Salik ur Rehman is a Cardiologist currently working as an instructor at the AKUH. He is Fellow of College of Physicians and Surgeons (FCPS) Pakistan in Adult Cardiology. Dr. Aysha Almas is an Internist woking as an Associate Professor at AKUH. She is Fellow of College of Physicians and Surgeons Pakistan (FCPS) in Internal Medicine and did her Masters in Clinical Research from AKU. Further, she obtained her PhD in Medical Science from the Karolinska Institutet, Stockholmes, Sweden. She is also Fellow of American College of Physicians (FACP). Dr. Aisha Siddiqui is working as a Medical officer in the Section of Internal Medicine, AKU. Miss Sania Sabir Sethi is Bachelors in Medical Science. She is currently working as a research Assistant at AKUH. Miss Safia Awan is Masters in Statistics currently working as a Senior Instructor at AKUH. Professor Dr. Aamir Hameed Khan is a Cardiologist and Cardiac Electrophysiologist at AKUH. He is FCPS in Medicine and Cardiology. He is also currently the Cardio-thoracic Service Line chief at the AKUH.
References
- World Health Organization. Cardiovascular diseases (CVDs) (2017).
- Roth GA, Huffman MD, Moran AE, et al. Global and regional patterns in cardiovascular mortality from 1990 to 2013. Circulation 132 (2015): 1667-1678.
- Gulati R, Behfar A, Narula J, et al. Acute Myocardial Infarction in Young Individuals. Mayo Clin Proc 95 (2020): 136-156.
- Ahmed E, El-Menyar A. South Asian ethnicity and cardiovascular risk: the known, the unknown, and the paradox. Angiology 66 (2015): 405-415.
- Wilmot KA, O'Flaherty M, Capewell S, et al. Response to Letter Regarding Article, "Coronary Heart Disease Mortality Declines in the United States From 1979 Through 2011: Evidence for Stagnation in Young Adults, Especially Women". Circulation 133 (2016): e433.
- Aggarwal A, Srivastava S, Velmurugan M. Newer perspectives of coronary artery disease in young. World J Cardiol 8 (2016): 728-734.
- Maqbool H Jafary AS, Mohammad Ishaq, Shaukat Ali Jawaid MA, et al. Profile of Acute Myocardial Infarction (AMI) In Pakistan. Pakistan Journal of Medical Sciences 23 (2007): 485-489.
- American Diabetes A. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes-2020. Diabetes Care 43 (2020): S14-S31.
- Cohen R, Budoff M, McClelland RL, et al. Significance of a positive family history for coronary heart disease in patients with a zero coronary artery calcium score (from the Multi-Ethnic Study of Atherosclerosis). Am J Cardiol 114 (2014): 1210-1214.
- Chobanian AV, Bakris GL, Black HR, et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 289 (2003): 2560-2572.
- Barua RS, Rigotti NA, Benowitz NL, et al. 2018 ACC Expert Consensus Decision Pathway on Tobacco Cessation Treatment: A Report of the American College of Cardiology Task Force on Clinical Expert Consensus Documents. Journal of the American College of Cardiology 72 (2018): 3332-3365.
- Consultation WHOE. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363 (2004): 157-163.
- Reindl M, Reinstadler SJ, Feistritzer HJ, et al. Relation of Low-Density Lipoprotein Cholesterol With Microvascular Injury and Clinical Outcome in Revascularized ST-Elevation Myocardial Infarction. J Am Heart Assoc 6 (2017).
- Zhong Z, Hou J, Zhang Q, et al. Assessment of the LDL-C/HDL-C ratio as a predictor of one year clinical outcomes in patients with acute coronary syndromes after percutaneous coronary intervention and drug-eluting stent implantation. Lipids Health Dis 18 (2019): 40.
- Rosenthal RL. The 50% coronary stenosis. Am J Cardiol 115 (2015): 1162-1165.
- Akhter Z, Hussain S, Aijaz S, et al. Mortality and deciding factors for no revascularization in cardiogenic shock patients; a cross sectional study. JPMA The Journal of the Pakistan Medical Association 69 (2019): 1663-1667.
- Enas EA, Mehta J. Malignant coronary artery disease in young Asian Indians: thoughts on pathogenesis, prevention, and therapy. Coronary Artery Disease in Asian Indians (CADI) Study. Clin Cardiol 18 (1995): 131-135.
- Yusuf S, Hawken S, Ounpuu S, et al. Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 364 (2004): 937-952.
- Horne M, Tierney S. What are the barriers and facilitators to exercise and physical activity uptake and adherence among South Asian older adults: a systematic review of qualitative studies. Preventive medicine 55 (2012): 276-284.
- Almas A, Hameed A, Sultan FA. Knowledge of coronary artery disease (CAD) risk factors and coronary intervention among university students. JPMA The Journal of the Pakistan Medical Association 58 (2008): 553-557.
- National Center for Chronic Disease Prevention and Health Promotion (US) Office on Smoking and Health. The Health Consequences of Smoking—50 Years of Progress. A Report of the Surgeon General (2014).
- Li K, Yao C, Di X, et al. Smoking and Risk of All-cause Deaths in Younger and Older Adults: A Population-based Prospective Cohort Study Among Beijing Adults in China. Medicine 95 (2016): e2438.
- Basu S, Glantz S, Bitton A, et al. The effect of tobacco control measures during a period of rising cardiovascular disease risk in India: a mathematical model of myocardial infarction and stroke. PLoS medicine 10 (2013): e1001480.
- Ahmed ST, Rehman H, Akeroyd JM, et al.
- Premature Coronary Heart Disease in South Asians: Burden and Determinants. Current atherosclerosis reports 20 (2018): 6.
- Dalager S, Paaske WP, Kristensen IB, et al. Artery-related differences in atherosclerosis expression: implications for atherogenesis and dynamics in intima-media thickness. Stroke 38 (2007): 2698-2705.
- Stary HC. Evolution and progression of atherosclerotic lesions in coronary arteries of children and young adults. Arteriosclerosis (Dallas, Tex) 9 (1989): I19-I32.
- Wasilewski J, Niedziela J, Osadnik T, et al. Predominant location of coronary artery atherosclerosis in the left anterior descending artery. The impact of septal perforators and the myocardial bridging effect. Kardiochirurgia i torakochirurgia polska = Polish journal of cardio-thoracic surgery 12 (2015): 379-385.
- Rathod KS, Jones DA, Gallagher S, et al. Atypical risk factor profile and excellent long-term outcomes of young patients treated with primary percutaneous coronary intervention for ST-elevation myocardial infarction. Eur Heart J Acute Cardiovasc Care 5 (2016): 23-32.
- Bilal Mustafa HuR. Angiographic characteristics of premature coronary artery disease in Pakistani population; a prospective cross-sectional study. Rawal Medical Journal 40 (2015): 366-370.
- Sinha SK, Krishna V, Thakur R, et al. Acute myocardial infarction in very young adults: A clinical presentation, risk factors, hospital outcome index, and their angiographic characteristics in North India-AMIYA Study. ARYA Atheroscler 13 (2017): 79-87.
- Joshi P, Islam S, Pais P, et al. Risk factors for early myocardial infarction in South Asians compared with individuals in other countries. Jama 297 (2007): 286-294.
- Ruiz Pizarro V, Palacios-Rubio J, Cruz-Utrilla A, et al. ST-Elevation Myocardial Infarction in Patients </=35 Years of Age. Am J Cardiol 123 (2019): 889-893.
- Acharya D. Predictors of Outcomes in Myocardial Infarction and Cardiogenic Shock. Cardiology in review 26 (2018): 255-266.
- Ma W, Liang Y, Zhu J, et al. Impact of Admission Systolic Blood Pressure and Antecedent Hypertension on Short-Term Outcomes After ST-Segment Elevation Myocardial Infarction: Strobe-Compliant Article. Medicine 94 (2015): e1446.
- Auffret V, Leurent G, Gilard M, et al. Incidence, timing, predictors and impact of acute heart failure complicating ST-segment elevation myocardial infarction in patients treated by primary percutaneous coronary intervention. International journal of cardiology 221 (2016): 433-442.
- Bardy GH, Lee KL, Mark DB, et al. Amiodarone or an implantable cardioverter-defibrillator for congestive heart failure. The New England journal of medicine 352 (2005): 225-237.
- Moss AJ, Zareba W, Hall WJ, et al. Prophylactic implantation of a defibrillator in patients with myocardial infarction and reduced ejection fraction. The New England journal of medicine 346 (2002): 877-883.
- Chen ZW, Yu ZQ, Yang HB, et al. Rapid predictors for the occurrence of reduced left ventricular ejection fraction between LAD and non-LAD related ST-elevation myocardial infarction. BMC cardiovascular disorders 16 (2016): 3.
- Noman A, Zaman AG, Schechter C, et al. Early discharge after primary percutaneous coronary intervention for ST-elevation myocardial infarction. Eur Heart J Acute Cardiovasc Care 2 (2013): 262-269.
- Picariello C, Lazzeri C, Attanà P, et al. The impact of hypertension on patients with acute coronary syndromes. International journal of hypertension 2011 (2011): 563657.


 Impact Factor: * 3.6
Impact Factor: * 3.6 Acceptance Rate: 78.21%
Acceptance Rate: 78.21%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 