IgG titers Decline Post-Vaccination with BNT6112b2 in an Italian Dental Team
Livia Barenghi1*, Francesco Romano2, Garagiola Umberto1, Francesco Spadari1
1Department of Biomedical, Surgical and Dental Sciences, University of Milano, Milan, Italy
2European Institute of Medical Studies (EIMS), New Building of Saint Martin, Schembri Street, Hamrun HMR1541, Malta
*Corresponding Author: Livia Barenghi, Department of Biomedical, Surgical and Dental Sciences, University of Milano, Milan, Italy
Received: 18 October 2021; Accepted: 26 October 2021; Published: 28 October 2021
Article Information
Citation:
Livia Barenghi, Francesco Romano, Garagiola Umberto, Francesco Spadari. IgG titers Decline Post-Vaccination with BNT6112b2 in an Italian Dental Team. Dental Research and Oral Health 4 (2021): 074-084.
View / Download Pdf Share at FacebookAbstract
The occupational risk of dental health care workers for COVID-19 is a burning issue. Currently, the long-lasting efficacy of the induced immunity from SARS-CoV-2 vaccination is largely unknown. Our aim is to study the RDB-IgG response after 1, 4, and 7 months from complete vaccination with BNT6112b2 in an Italian dental team. All 13 dental health care workers (3 men and 10 women) working in a private dental office were enrolled in the frame of scheduled controls for occupational safety. All dental health care workers were aged less than 60 yrs old; the mean age (±DS) was 41.23±9.63 yrs; 2/13 had one medical condition associated with a higher risk of developing severe illness from COVID-19, but none of DHCW were affected with the disease. Antigen tests on nasal swab in detecting the SARSCoV-2 were always negative from December 2020 to September 2021. Any symptoms commonly attributed to COVID-19 were not reported. The vaccination with BNT6112b2 was done on them with two doses according to the authorization protocol. Some female dental health workers (4/13) seem to be non-responders or slightly responders and reported associated pathologies (obesity, hypertension). 7 months after the second dose of vaccine, the RDB-IgG antibodies against SARS-CoV-2 have reduced significantly (94%; P < 0.001) compared to levels 1 month after. More knowledge on occupational risk and on vaccine efficacy in dental health care workers, stringent adoption of standard precautions, and, perhaps, the vaccine boost or new mucosal vaccines seem to be the main strategy in facing COVID-19 pandemic.
Keywords
COVID-19, Infection, Vaccination, Safety, Workers, Dentistry
COVID-19 articles; Infection articles; Vaccination articles; Safety articles; Workers articles; Dentistry articles
COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals Infection articles Infection Research articles Infection review articles Infection PubMed articles Infection PubMed Central articles Infection 2023 articles Infection 2024 articles Infection Scopus articles Infection impact factor journals Infection Scopus journals Infection PubMed journals Infection medical journals Infection free journals Infection best journals Infection top journals Infection free medical journals Infection famous journals Infection Google Scholar indexed journals Vaccination articles Vaccination Research articles Vaccination review articles Vaccination PubMed articles Vaccination PubMed Central articles Vaccination 2023 articles Vaccination 2024 articles Vaccination Scopus articles Vaccination impact factor journals Vaccination Scopus journals Vaccination PubMed journals Vaccination medical journals Vaccination free journals Vaccination best journals Vaccination top journals Vaccination free medical journals Vaccination famous journals Vaccination Google Scholar indexed journals Dentistry articles Dentistry Research articles Dentistry review articles Dentistry PubMed articles Dentistry PubMed Central articles Dentistry 2023 articles Dentistry 2024 articles Dentistry Scopus articles Dentistry impact factor journals Dentistry Scopus journals Dentistry PubMed journals Dentistry medical journals Dentistry free journals Dentistry best journals Dentistry top journals Dentistry free medical journals Dentistry famous journals Dentistry Google Scholar indexed journals dental articles dental Research articles dental review articles dental PubMed articles dental PubMed Central articles dental 2023 articles dental 2024 articles dental Scopus articles dental impact factor journals dental Scopus journals dental PubMed journals dental medical journals dental free journals dental best journals dental top journals dental free medical journals dental famous journals dental Google Scholar indexed journals IgG levels articles IgG levels Research articles IgG levels review articles IgG levels PubMed articles IgG levels PubMed Central articles IgG levels 2023 articles IgG levels 2024 articles IgG levels Scopus articles IgG levels impact factor journals IgG levels Scopus journals IgG levels PubMed journals IgG levels medical journals IgG levels free journals IgG levels best journals IgG levels top journals IgG levels free medical journals IgG levels famous journals IgG levels Google Scholar indexed journals
Article Details
1. Introduction
As Tamim recently stated, “Occupational health professionals have a unique and key role at the interface between work and health”, but their decisions are not always trouble-free in dental settings [1]. The Coronavrus Disease 2019 (COVID-19) risk on dental health care workers (DHCW) and dental patients is a burning issue, based on contradictory and largely unknown evidence [2-5]. It is unclear how the interplay among SARS-CoV-2, host, social behaviour, specific dental procedures and then the worker and environmental contamination by droplets and aerosol, affects infection risk. The rate of COVID-19 in a population seeking oral healthcare reflects the community positivity rate, including a considerable percentage of asymptomatic and afebrile patients [6]. SARS-CoV-2 dispersion parameter, named k, is small, and SARS-CoV-2 transmission, has been highly over-dispersed and propelled by the super-spreading of events. This means that 10–20% of cases cause 80% of secondary infections, and asymptomatic cases are nearly impossible to identify by triage in dental settings [7]. In addition to respiratory apparatus and vascular system, SARS-CoV-2 also resides in oral cavities, saliva, crevicular fluid and dental biofilm, and also influences oral microbiome and different oral manifestations [8]. Currently, it seems that aerosol and fomite contamination do not contributed substantially to transmission [2]. Nevertheless, DHCW work near to, or inside the oral cavity, while avoiding aerosol generating procedures (AGP), is a real tiring job in dentistry.
In general, vaccination has been considered the best defense in the hierarchy of infection prevention control (IPC) and against human error during infection prevention [9]. Vaccination against SARS-CoV-2 generally induces systemic immune responses with dominant IgG responses, while natural infection induces both systemic and mucosal immune responses. Vaccination, with traditional, viral vector, protein and RNA based vaccines, is promising in terms of bringing the COVID-19 pandemic to an end, mainly by lowering the risk of symptomatic COVID-19 and the most serious and deadly consequences of the virus. Vaccine ability to limit viral transmission between individuals is less well understood [10].
Evidence from prospective cohorts of 3,950 health care workers (HCW), shows that with full immunization (14 days after second dose), mRNA vaccine was 90% effective against SARS-CoV-2 infections, regardless of symptom status [11]. 14 weeks after complete vaccination with BNT6112b2 (Pfizer/BioNTech) vaccine, 2.6% of the Israeli HCW had breakthrough COVID-19 infections (BCI), 67% of which were mild, and 33% of which were asymptomatic [12]. Among fully vaccinated HCW, the occurrence of BCI was correlated with neutralizing antibody titers during the peri-infection period. Male sex, older age, and hospitalization for COVID-19 have been associated with increased antibody response, while obesity, arthritis and some drugs with reduced antibody response. Antibody titers induced by natural coronavirus infection have been reported to wane over time. Unfortunately, the duration of the induced immunity from SARS-CoV-2 vaccination is largely unknown after many months [13]. Little evidence has been reported on long-lasting efficacy of COVID-19 mRNA vaccines, but it is indicative of a rapid decline of spike antigen specific serum IgG (<23% peak levels within 80 days of the initial shot) in four HCW [14].
Therefore, we investigated the induced immunity in a sample of DHCW, where the occupational risk was homogeneous, by the strict adoption of standard precautions [2].
2. Methods
2.1 Study place and enrolment
This study was conducted in a private dental office (Centro Odontoiatrico del dr. V. Romano, Piazza Castelnuovo 26A, 90141 - Palermo, Italy) located in Sicily, under the guidelines of occupational risk according to Italian Law (mainly Law 81/08), rules, regulations, and local guidance and specific recommendation for COVID-19 prevention in dental offices [15]. The study protocol was approved by the internal board for occupational risk (including the occupational physician), according to Italian Law and health data protection (EU General Data Protection Regulation). DHCW (2 dentists, 8 dental nurses, 2 receptionists) were included after a written informed consent. The study was carried out from January 2021 to September 2021. During dental cares, administrative work and instrument and environmental decontamination, the dental office strictly adopted the up-to-date guidance by CDC and the Italian recommendation [2,15]. In Sicily, the epidemiologic trend of COVID-19 showed three main peaks on 20 November 2020, 14 January, 14 April and 25 August 2021, with respectively 1634,1867, 1542 and 1491 new cases/daily and 40,38,20 and 9 deaths/daily for about 4.9 million of inhabitants (mean age =44,4 yrs) [16]. As of 5 September 2021, the total cases and death were respectively 281000 and 6435 for about 4.9 million of inhabitants.
2.2 Vaccination with BNT6112b2
The regional heath government of Sicily prioritised DHCW for COVID-19 vaccination early, since January 2021. We underline that only on 21 December 2021, did the European Commission grant market authorization for EU-wide use for the vaccine Comirnaty, developed by BioNTech and Pfizer, named BNT6112b2, to prevent COVID-19 in people from 16 years of age. The vaccination with BNT6112b2 was done on DHCW with two doses according to the authorization protocol. The first dose of vaccination was administered from the 9th of January 2021 to the 12th of February 2021, and after 3 weeks, the second dose was administered, from the 30th of January to the 6th of March. As of August 28, 70.88% (equal to 3 million people) of the resident population in Sicily received at least one dose of the anti-COVID-19 vaccine, while 61.71% (over 2.6 million) were completely immunized (i.e. received both doses or the single Janssen dose).
2.3 Analytical methods
Diagnostic analyses were carried out in a highly specialized laboratory (Locorotondo Labs S.R.L. via G. Carducci n.3, 90141 Palermo; https://www.locorotondolabs.it/), authorised by the Sicily Region in accordance with the methods and procedures agreed upon with the National Reference Laboratory of the Istituto Superiore di Sanità. Analyses were performed at 1, 4 and 7 months after the second dose of vaccine.
2.4 IgG Immunoassay
IgG (sCOVG) antibodies to SARS-CoV-2 were evaluated by Atellica® IM* assay (Siemens, Germany). This test was authorized for emergency use by the FDA, for use by authorized laboratories. It is a chemiluminescent immunoassay intended for qualitative and semi-quantitative detection of IgG antibodies to SARS-CoV-2 in human serum and plasma (lithium heparin), using the Atellica IM Analyzer. The Atellica IM* assay detects IgG antibodies to the S1 RBD antigen, known to be an important component of the spike (S)-protein. The analytic performance (Positive percent agreement =95,58%; negative percent agreement=99-90%) from the manufacturer seems in line with real clinical performance [17,18]. RBD-based antibody tests are appropriate for testing at 6-8 months after SARS-CoV-2 infection. The sensitivity of Siemens tests was similar 4-10 weeks and 6-8 months after infection [18]. The analytical reference value is > 1 (U/mL).
2.5 SARSCoV-2 antigen test
SARSCoV-2 antigen was evaluated by immunoassay (Panbio™ COVID-19 Ag Rapid Test Device) on nasal swabs at 1, 4 and 7 months. The Panbio™ COVID-19 Ag test (Abbot, USA) has a specificity of 100% and a sensitivity of 93.8% (for subjects with Ct values ≤ 30) among asymptomatic subjects, representing a viable alternative to RT-PCR when molecular testing is not readily available or too expensive. Mutations in the more transmissible forms of SARS-CoV-2 virus are located far from the target regions of the Abbott COVID-19 tests and should not pose a threat to assay performance and our study.
2.6 Statistical methods and software
Statistical analyses were performed using Excel software version 97-2003 for Windows software. The means of IgG levels after 1, 4 and 7 months days were compared by using Paired T Test. All tests were considered significant if P-value was ≤0.05.
3. Results
All DHCW of the dental office were enrolled. There were 13 (3 men and 10 women) enrolled DHCW (Table). All DHCW aged less than 60 years old; the mean age (±DS) was 41.23±9.63 yrs; 2/13 had a medical condition associated with higher risk of developing severe illness from COVID19, but none of DHCW were affected with COVID-19.
Tests on nasal swabs in detecting the SARSCoV-2 spike antigen were always negative from December 2020 to September 2021. The SARS CoV-2 Antigen Test is adequate for screening asymptomatic individuals. No symptoms commonly attributed to COVID-19 were reported. Temporary lay-offs of DHCW were in line with previous years, and were not caused by, or attributed to COVID-19. The vaccination with BNT6112b2 was done on DHCW with two doses according to the authorization protocol. The vaccine immunity response, by RBD-IgG level, is reported in Figures 1,2 and Table 1.
We don’t have RDB-IgG level of three DHCW at four months. After 4 months of the second dose of vaccine, the mean antibody level against SARS-CoV-2 is significantly reduced (80%; P < 0.001) compared to levels 1 month after (Table). After 7 months of the second dose of vaccine, the mean antibody level against SARS-CoV-2 is significantly reduced (94%; P < 0.001) compared to levels 1 month after (Table). Our data is in line with 50% reduction of anti-RBD antibodies and anti-trimeric spike IgG in HCW, three months after the first dose [19]. The exponential decay calculated by mean RBD-IgG levels at 1,4,7 months (R2=0.985), follows the formula y=308,9e-1,41x. The half life of IgG is 36 days and 47 days, calculated between 1-4 months and 4-7 months, respectively. Four DHCW (signed with 2,4,8,11) seem to be non-responders or slightly responders and reported associated pathologies (obesity, hyperthension) (Figure 1); however, they continued to work in the dental office without problems during this study. Only one female (DHCW n° 5) reported contact with someone with suspected or confirmed COVID-19 infection, and needed to quarantine during the study. She was not never diseased or asymptomatic, but her antibodies levels were the highest, being 163,88, 44.11 and 16.46 U/mL respectively at 1, 4 and 7 months after complete vaccination. It is known that prior SARS-CoV-2 exposure is independently associated with higher IgG levels, after vaccination in HCW [20].
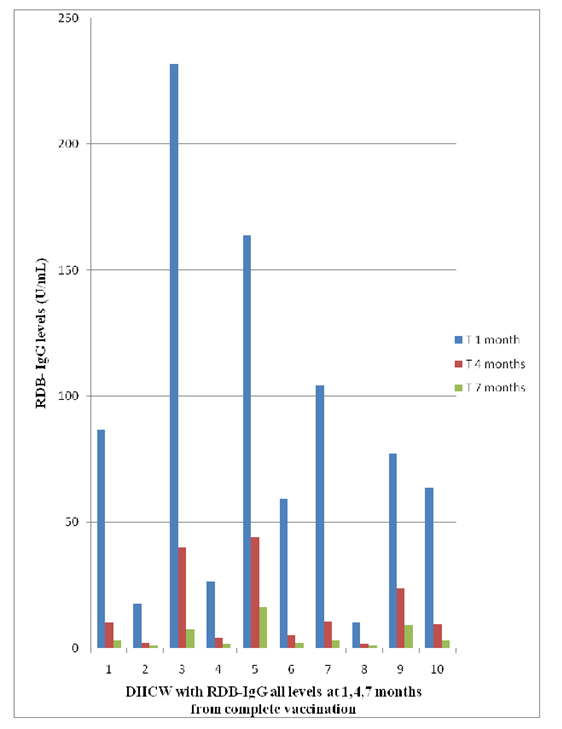
Figure 1: RDB-IgG levels in 10 DHCW at 1,4, 7 months after 2nd dose of vaccine BNT6112b2.
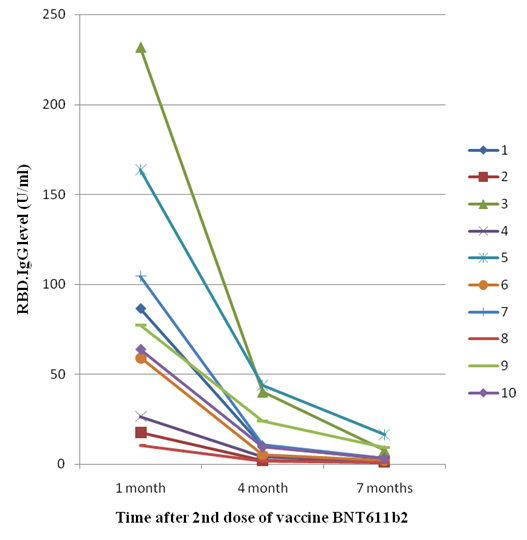
Figure 2: RDB-IgG levels in 10 DHCW at 1,4, 7 months after 2nd dose of vaccine BNT6112b2.
|
Time after the 2nd dose |
1 month |
4 months |
7 months |
|
|
Number of DHCW |
13 |
10 |
13 |
|
|
Age (mean±SD) |
41.23±9.63 yrs |
|||
|
Sex (F/M) |
10/3 |
7/3 |
10/3 |
|
|
Age (mean±SD) of females |
42±8.37 |
|||
|
Age (mean±SD) of males |
38.3±14.87 |
|||
|
RBD-IgG level (mean ± SD) (U/mL) |
83.16±62.859 |
15.17±14.789 |
4.96±4.416 |
|
|
P value |
P . |
|||
|
RDB-IgG level at 7 months vs 1 month |
0.000725 |
|||
|
RDB-IgG level at 4 months vs 1 month |
0.003419 |
|||
|
RDB-IgG level at 7 months vs 4 month |
0.017893 |
Table 1: Characteristics of the enrolled DHCP and vaccine immunity response after two doses of vaccine BNT6112b2, by RBD-IgG level
6. Discussion
Vaccination and the application of standard precautions are the two main preventive measures against COVID-19 for DHCW. The challenges are open because the rate of infection is the highest in DHCW, at 26% , while in HCW it’s at 14.5%. These figures are respectively about 5 and 3 fold higher than the local population [5] or significant [4]. The estimated incidence rate ratio against any SARS-CoV-2 infection and asymptomatic or symptomatic/contact SARS-CoV-2 infection was 0.16 (0.10-0.25 95% CI) in vaccinated hospital employers (HE) compared to those not vaccinated HE [21]. The cumulative incidence of positive tests for symptoms or known exposure is 5-fold lower in vaccinated HE, compared to unvaccinated HE. By mathematical modeling, the transmission probability of corona virus was estimated to be between 0 and 99,4% in three different dental scenarios, and driven mainly by patient infectiousness, indoor air quality, and slightly limited by respiratory protection [22]. Despite the fact that the pandemic led to unprecedented attention on infection prevention (IP), we have to underline that: a) different National Laws and European guidelines on IP often raise differing levels of awareness, and operational choice in UE [23]; lapses, errors, and the use of counterfeit products (mainly PPE, hand sanitizer products, “gray market” disinfectants) were frequent even before COVID-19 [24]. International guidelines (USA CDC, UK NHS etc) continue to recommend the application of standard IP measures, and in particular the use of a filtering facepiece respirator (N95, FFP). That said, data from a 6-month longitudinal study from June to November 2020, shows that only about 60% of dentists always wore FFP and eye protection by performing AGP. Additionally, the extended use (no change every patients) of respiratory protection is adopted by 75% of dentists [3]. During AGP, the evidence-based recommendation to use air turbine at 60-80 rpm to avoid aerosol production is largely unknown. DHCW are considered fully vaccinated 2 weeks after their second dose in a 2-dose series, such as the Pfizer or Moderna vaccines. Post-dose 2, BNT162b2 vaccine efficacy (VE) in preventing COVID-19 (ClinicalTrials.gov number, NCT04368728), peaked at 96.2% during the interval from 7 days to <2 months post-dose 2, and then showed an average decline of ~6% every 2 months [25].
Long term vaccine efficacy is very important for DHCW occupational safety and for establishing the "levels of protection" determined by FDA approved clinical laboratory assays, even if at present, the CDC does not recommend measuring post vaccination titers for COVID-19. Data by different analytical methods, antigen target, and intra-individual immune response have contributed to an unclear picture around this topic.
Here, we show the spike RBD-IgG response to BNT162b2 vaccine in a homogeneous sample of DHCW, with concurrent antigen test negative for COVID-19 from nasal swabs (Figure 1,2 and Table). RBD-IgG level dropped by 94 % after 7 months. As expected, IgG decrease by vaccination is higher than the roughly 10-20% of the maximum concentration observed 1 year after the natural infection [26]. We evaluated serum anti–RBD IgG because of antibodies against SARSCoV-2 spike and receptor binding domain (RBD) are known to decline moderately over 8 months after infection, according to several other reports [27,28], and have an estimated half life (t1/2) of 83 days (95% CI: 62 to 126 days) [27]. In healthy volunteers, a decrease in anti-RBD antibody after its peak in "2nd dose" group was significant only on
In convalescent plasma donors, the antibody decay is bi-phasic, with a more pronounced decrease during the first 6 months following the onset of symptoms. The antibodies half life for spike-RDB and nucleocapisde are respectively 62, and 47 days at a 0-6 months interval following symptom onset, while at 212 and 100 days at
6 months or more, following symptom onset [30]. Our data after vaccination (Figure 2), shows an increased exponential decay of RdB-IgG and shorter t1/2: 36 and 47 days calculated between 1-4 months and 4-7 months, respectively.
The chosen method for checking vaccine-immune response is adequate. In addition, RBD-binding antibodies are commonly referred to as "neutralizing" antibodies, since binding to the virus precludes its attachment and the entry into the host cell. Low titers of S-specific IgG and neutralizing antibody have been hypotized markers of breakthrough infection [31]. The quantitative values of antibodies against the RBD of the S-Protein of SARS-CoV-2 showed a good correlation to virus neutralization titers (Spearman’s r=0.843, 95%CI: 0.785- 0.885, p<0.0001) [32] and are expected to be suitable for monitoring the humoral immune response to vaccination with BNT162b2 vaccine. Pfizer reported that the BNTl62b2, which encoded the full-length stabilized S glycoprotein, elicited dose-dependent SARS-CoV-2 neutralizing antibody titers comparable or higher than those elicited by a defined panel of convalescent SARS-CoV-2 serum samples, and is also effective against Delta and Kappa variants [33]. When neutralising antibodies alone are insufficient, reinfection with SARS-CoV-2 can be limited by non-neutralising antibodies and T cells [34].
The main limitation of our study was the small size population, mainly of the female sex; nevertheless, the sample is very homogeneous for the occupational risk and the restricted age range of DHCW. In addition, it lacks of neutralization studies, mucosal IgA response, and T-cell response studies, that would have needed a very specialized laboratory and high cost. Unfortunately, the predictive power of circulating RBD IgG for assessing T cell memory was poor, so any speculation should be worrisome [27].
Conclusion
In conclusion, more knowledge is needed to evaluate the long-term VE because of the following factors:
- it is known that in nonhuman primates, even low circulating neutralizing (antibody titers 1:20) were associated with a substantial degree of protection against COVID-19.
- it is largely unknown the degree to which mucosal antibodies, including salivary highly effective secreted dimeric antibodies, elicited by vaccines can prevent infection [10]. Adenovirus-vectored vaccines seem to be potentially less effective than the mRNA vaccines.
- after SARS-CoV-2 infection, the immune system seems to produce around 50% lower amounts of IgG and IgA in women compared to men; this has been related to the higher risk of adverse COVID-19 outcome in men through a stronger (inflammatory) response.
- the immunological memory depends not only on antibodies, but also on the cellular immunity (memory B cells, memory CD4+ T cells, and/or memory CD8+T cells) [35]. RDB-specific CD8+ and S-specific IgG+ memory cells have been found to be involved in VE at long term, that is approximately 7 months after natural infection [36]. Nevertheless, specific memory B cells are extremely scarce even after vaccination [19,26,37]. But, recent data shows that two months after the second dose of BNT162b2 vaccine, specific antibody levels decline, but highly specific memory B cells continue to increase, thus predicting a sustained protection from COVID-19 [19].
The current strategy for facing COVID-19 outbreak is based on more knowledge of occupational risk, and of vaccine efficacy in DHCW, and the stringent adoption of standard precautions [1-5,9]. A vaccine boost, with intramuscular SARS-CoV-2 vaccines, should be taken into consideration, especially for more vulnerable and non responder DHCW. Infection after vaccination may be caused by the lack of local preventive immunity because of the absence or low levels of mucosal IgA [19]. The new generation mucous vaccines, are in various stages of development and very interesting for dentistry. They could effectively block the transmission of SARS-CoV-2 by the oral epithelial cells and oral mucosa [8] and there, generate antibodies and cellular immunity within the oral mucosa and saliva [10], and then reduce the danger caused by AGP.
Acknowledgments
The authors would like to thank Dr Maté Jarai (PhD, Creative Writing Ma Creative Writing Bachelor in Philosophy), for English language revision and Dr Marco Grassini (Degree in Statistical) for statistical analysis.
Competing interests
Until 2018, L. Barenghi had a service agreement with KerrKaVo and was a consultant for DentalTrey il Blog (http://blog.dentaltrey.it/), neither of which gave any input or financial support to the writing of this article. The authors (F Romano, F. Spadari, U. Garagiola) declare that there are no conflicts of interest regarding the publication of this paper.
Funding
The work was supported by the Centro Odontoiatrico del dr. V. Romano (Palermo, Italy) [COVR/01/2021], and the Integrated Orthodontic services srl , Lecco (Italy) [IOS/03/2021].
Contributors
FR conceptualized, planned and run this study. LB wrote the manuscript and prepared figures and the table. All authors contributed to the revision and discussions of the scope of this study and approved the final manuscript.
References
- Tamin J. COVID-19 and vulnerable workers. Occuational Medicine 71 (2021): 161-164.
- Interim Infection Prevention and Control Guidance for Dental Settings During the Coronavirus Disease 2019 (COVID-19) Pandemic.
- Araujo MWB, Estrich CG, Mikkelsen M, et al. COVID-2019 among dentists in the United States. A 6-month longitudinal report of accumulative prevalence and incidence. Journal American Dental Association 152 (2021): 425-433.
- Jungo S, Moreau N, Mazevet ME, et al. Prevalence and risk indicators of first-wave COVID-19 among oral health-care workers: A French epidemiological survey. Plos One 6 (2021): e0246586.
- NHS Grampian. Incident management team formally asks Aberdeen's West End Dental Practice to close following Covid-19 outbreak (2020).
- Palla B, Callahan N. What is the rate of COVI D-19 infection in a population seeking oral health care? J ournal American Dental Association 152 (2021): 448-454.
- Chen PZ, Koopmans M, Fisman D, et al. Understanding why superspreading drives the COVID-19 pandemic but not the H1N1 pandemic. The Lancet Infectious Diseases 21 (2021): 1203-1204 .
- Huang N, Perez P, Kato T, et al. SARS-CoV-2 infection of the oral cavity and saliva. Nature Medicine 27 (2021): 892-903.
- Riva MA, Paladino ME, Paleari A, Belingheri Workplace COVID-19 vaccination, challenges and opportunities. Occuational Medicine 22 (2021): kqab080.
- Mostaghimi D, Valdez CN, Larson HT, et al. Prevention of host-to-host transmission by SARS-CoV-2 vaccines. The Lancet Infectious Diseases 14 (2021): 51473-53099.
- Thomson Mg, Burgess JL, Naleway AL, et al. Interim estimates of vaccine effectiveness of BNT162b2 and MRNA-1273 COVID-19 vaccines in preventing SARS-CoV-2 infection among health care personnel, first responders, and other essential and frontline workers-eight U.S. locations. Morbidity and Mortality Weekly Report (CDC) 70 (2021): 495-500.
- Bergwerk M, Gonen T, Lustig Y, et al. Covid-19 Breakthrough infections in vaccinated health care workers. New England Journal Medicine 28 (2021): NEJMoa2109072.
- How long does protection from a covid-19 vaccine last? (2021)
- Wisnewski AV, Campillo Luna J, Redlich CA. Human IgG and IgA responses to COVID-19 mRNA vaccines. PLoS ONE 16 (2021): e0249499.
- Ministero della salute (Italy). Indicazioni operative per l'attività odontoiatrica durante la fase 2 della pandemia Covid-19 (2020).
- Demografic indices and struttura Sicilia (Indici demografici e Struttura Sicilia-(Italy) (2021).
- Harritshoj LH, Gybel-Brask M, Afzal S,Kamstrup PR, Jorgensen CS, Thomsen MK, et al. Comparison of 16 serological SARS-CoV-2 immunoassays in 16 clinical laboratories. Journal of Clinical Microbiology 59 (2021): e02596-20.
- Kannenberg J, Schnurra C, Reiners N, et al. Sensitivity of SARS-CoV-2 antibody tests with late convalescent sera. Journal of Clinical Virology Plus 1 (2021): 100038.100038.
- Piano Mortari E, Russo C, Vinci MR, et al. Highly specific memorY B cells generation after the 2nd dose of BNT162b2 vaccine compensate for the decline of serum antibodies and absence of mucosal IgA. Cells 10 (2021): 2541.
- Debes AK, Xiao S, Colantuoni E, et al. Association of Vaccine Type and Prior SARS-CoV-2 Infection With Symptoms and Antibody Measurements Following Vaccination Among Health Care Workers. Journal American Medical Association Intern Med 325 (2021): 2500-2502.
- Tang L, Hijano DR, Gaur AH, et al. Asymptomatic and Symptomatic SARS-CoV-2 Infections After BNT162b2 Vaccination in a Routinely Screened Workforce. Journal American Medical Association Intern Med 325 (2021): 2500-2501.
- Zemouri C, Awad SF, Volgenant CMC, et al. Modeling of the Transmission of Coronaviruses, Measles Virus, Influenza Virus, Mycobacterium tuberculosis, and Legionella pneumophila in Dental Clinics. Journal of Dental Research 12 (2020): 1192-1198.
- Becker K, Gurzawska-Comis K, Brunello G, et al. Summary of European guidelines on infection control and prevention during COVID-19 pandemic. Clinical Oral Implant Research 30 (2021): 12-25.
- Barenghi L, Barenghi A, Di Blasio A. Infection control in dentistry and drug resistant infectious agents: a burning issue. Part 2 (2018).
- Thomas SJ, Moreira Ed, Kitchin N, et al. Safety and Efficacy of the BNT162b2 mRNA Covid-19 Vaccine through 6 Months. The New Engand Journal Medicine (2021).
- Radbruch A, Hyun-Dong Chang A long-term perspective on immunity to COVID. Nature 595 (2021): 359-360.
- Dan JM, Jose Mateus J, Yu Kato Y, et al. Immunological memory to SARS-CoV-2 assessed for up to 8 months after infection. Science 371 (2021): eabf4063.
- Gluck V, Grobecker S, Tydykov L, et al. SARS-CoV-2-directed antibodies persist for more than six months in a cohort with mild to moderate COVID-19. Infection 49 (2021): 739-746.
- Wheeler SE, Shurin GV, Yost M, et al. Differential antibody response to mRNA COVID-19 vaccines in healthy subjects. Microbial Spectroscopy 9 (2021): e0034 l-21.
- Terpos E, Dimitris Stellas D, Rosati M, et al. SARS-CoV-2 antibody kinetics eight months from COVID-19 onset: Persistence of spike antibodies but loss of neutralizing antibodies in 24% of convalescent plasma donors. European Journal Internal Medicine 89 (2021): 87-96.
- Chvatal-Medina M, Mendez-CortinaY, Patino PJ, et al. Antibody Responses in COVID-19: A Review. Frontiers in lmmunology 12 (2021): 633184.
- Irsara C, Egger AE, Prokop W, et al. Clinical validation of the quantitative Siemens SARS-CoV-2 spike lgG assay (sCOVG) reveals improved sensitivity and a good correlation with virus neutralization titers. Clinical Chemistry and Laboratory Medicine 59 (2021): 1453-1462.
- Sahin U, Muik A, Vogler I, et al. BNT162b2 vaccine induces neutralizing antibodies and poly-specific T cells in humans. Nature 595 (2021): 572-577.
- Lu LL, Suscovich TJ, Fortune SM, et al. Beyond binding: antibody effector functions in infectious diseases. Nature Review Immunology 18 (2018): 46-61.
- Klein LS, Pekosz A, Parl H, et al. Sex, age, and hospitalization drive antibody responses in a COVID-19 convalescent plasma donor population. Journal of Clinical Investigation 130 (2020): 614-650.
- Wheatley AK, Juno JA, Wang JJ, et al. Evolution of immune responses to SARS-CoV-2 in mild-moderate COVID-19. Nature Communications 12 (2021): 1162.
- Wang Z, Schmidt F, Weisblum Y, et al. mRNA vaccine-elicited antibodies to SARS-Co V-2 and circulating variants. Nature 592 (2021): 616-623.
- Turner JS, O'Halloran JA, Kalaidina E, et al. SARS-CoV-2 mRNA vaccines induce persistent human germinal centre responses. Nature 596 (2021): 109-113.


 Impact Factor: * 3.1
Impact Factor: * 3.1 Acceptance Rate: 76.66%
Acceptance Rate: 76.66%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 