Utilization of Cellulose Nanocrystals (CNC) Biopolymer Nanocomposites in Ophthalmic Drug Delivery System (ODDS)
Article Information
Jonathan Tersur Orasugh1,2*, Soumyadip Dutta1, Diphankar Das1, Jyotishka Nath1, Chandrika Pal1, Dipankar Chattopadhyay1,2*
1Department of Polymer Science and Technology, University of Calcutta, West Bengal, India
2Centre for Research in Nanoscience and Nanotechnology, Acharya Prafulla Chandra Roy Sikhsha Prangan, University of Calcutta, Kolkata, India
*Corresponding Authors: Jonathan Tersur Orasugh (JTO) and Dipankar Chattopadhyay (DC), Department of Polymer Science and Technology, University of Calcutta, 92 A.P.C. Road, Kolkata-700 009, West Bengal, India
Received: 26 July 2019; Accepted: 09 August 2019; Published: 20 August 2019
Citation:
Jonathan Tersur Orasugh, Soumyadip Dutta, Diphankar Das, Jyotishka Nath, Chandrika Pal, Dipankar Chattopadhyay. Utilization of Cellulose Nanocrystals (CNC) Biopolymer Nanocomposites in Ophthalmic Drug Delivery System (ODDS). Journal of Nanotechnology Research 1 (2019): 075-087.
View / Download Pdf Share at FacebookAbstract
Undeniably drug delivery systems (DDSs) engaged take part in controlling the drug pharmacological effect along with the pharmacokinetic profile with respect to the drug release rate, the site, bioavailability and then the side-effect. Different procedures for visual medication conveyance have been reportedly considered; from fundamental strategies aimed at improving the accessibility of medications; consistency enhancers and mucoadhesives help sedate maintenance and entrance enhancers advance medication transport into the eye. The utilization of drug loaded CNC nanoengineered smart gels enabled medications can be better put where they are required for sustained release of the drugs with straightforward conveyance. Advancements in visual inserts give a way to conquer the physical obstructions that generally forestalled compelling treatment. Advancements are being worked on permitting long term tranquillized conveyance from solitary DDSs: these devices permit the release of the loaded drugs even up to 25 h. Future improvements could lead to the nanoengineering of CNC based drug loaded ODDS with excellent ophthalmic DDSs.
Keywords
Ophthalmic, Drug delivery, Polymer, Nanocomposite, Cellulose nanocrystals
Ophthalmic articles Ophthalmic Research articles Ophthalmic review articles Ophthalmic PubMed articles Ophthalmic PubMed Central articles Ophthalmic 2023 articles Ophthalmic 2024 articles Ophthalmic Scopus articles Ophthalmic impact factor journals Ophthalmic Scopus journals Ophthalmic PubMed journals Ophthalmic medical journals Ophthalmic free journals Ophthalmic best journals Ophthalmic top journals Ophthalmic free medical journals Ophthalmic famous journals Ophthalmic Google Scholar indexed journals Drug delivery articles Drug delivery Research articles Drug delivery review articles Drug delivery PubMed articles Drug delivery PubMed Central articles Drug delivery 2023 articles Drug delivery 2024 articles Drug delivery Scopus articles Drug delivery impact factor journals Drug delivery Scopus journals Drug delivery PubMed journals Drug delivery medical journals Drug delivery free journals Drug delivery best journals Drug delivery top journals Drug delivery free medical journals Drug delivery famous journals Drug delivery Google Scholar indexed journals Polymer articles Polymer Research articles Polymer review articles Polymer PubMed articles Polymer PubMed Central articles Polymer 2023 articles Polymer 2024 articles Polymer Scopus articles Polymer impact factor journals Polymer Scopus journals Polymer PubMed journals Polymer medical journals Polymer free journals Polymer best journals Polymer top journals Polymer free medical journals Polymer famous journals Polymer Google Scholar indexed journals Nanocomposite articles Nanocomposite Research articles Nanocomposite review articles Nanocomposite PubMed articles Nanocomposite PubMed Central articles Nanocomposite 2023 articles Nanocomposite 2024 articles Nanocomposite Scopus articles Nanocomposite impact factor journals Nanocomposite Scopus journals Nanocomposite PubMed journals Nanocomposite medical journals Nanocomposite free journals Nanocomposite best journals Nanocomposite top journals Nanocomposite free medical journals Nanocomposite famous journals Nanocomposite Google Scholar indexed journals Cellulose nanocrystals articles Cellulose nanocrystals Research articles Cellulose nanocrystals review articles Cellulose nanocrystals PubMed articles Cellulose nanocrystals PubMed Central articles Cellulose nanocrystals 2023 articles Cellulose nanocrystals 2024 articles Cellulose nanocrystals Scopus articles Cellulose nanocrystals impact factor journals Cellulose nanocrystals Scopus journals Cellulose nanocrystals PubMed journals Cellulose nanocrystals medical journals Cellulose nanocrystals free journals Cellulose nanocrystals best journals Cellulose nanocrystals top journals Cellulose nanocrystals free medical journals Cellulose nanocrystals famous journals Cellulose nanocrystals Google Scholar indexed journals technologist articles technologist Research articles technologist review articles technologist PubMed articles technologist PubMed Central articles technologist 2023 articles technologist 2024 articles technologist Scopus articles technologist impact factor journals technologist Scopus journals technologist PubMed journals technologist medical journals technologist free journals technologist best journals technologist top journals technologist free medical journals technologist famous journals technologist Google Scholar indexed journals biocompatibility articles biocompatibility Research articles biocompatibility review articles biocompatibility PubMed articles biocompatibility PubMed Central articles biocompatibility 2023 articles biocompatibility 2024 articles biocompatibility Scopus articles biocompatibility impact factor journals biocompatibility Scopus journals biocompatibility PubMed journals biocompatibility medical journals biocompatibility free journals biocompatibility best journals biocompatibility top journals biocompatibility free medical journals biocompatibility famous journals biocompatibility Google Scholar indexed journals bio-system articles bio-system Research articles bio-system review articles bio-system PubMed articles bio-system PubMed Central articles bio-system 2023 articles bio-system 2024 articles bio-system Scopus articles bio-system impact factor journals bio-system Scopus journals bio-system PubMed journals bio-system medical journals bio-system free journals bio-system best journals bio-system top journals bio-system free medical journals bio-system famous journals bio-system Google Scholar indexed journals biomimitic alikeness articles biomimitic alikeness Research articles biomimitic alikeness review articles biomimitic alikeness PubMed articles biomimitic alikeness PubMed Central articles biomimitic alikeness 2023 articles biomimitic alikeness 2024 articles biomimitic alikeness Scopus articles biomimitic alikeness impact factor journals biomimitic alikeness Scopus journals biomimitic alikeness PubMed journals biomimitic alikeness medical journals biomimitic alikeness free journals biomimitic alikeness best journals biomimitic alikeness top journals biomimitic alikeness free medical journals biomimitic alikeness famous journals biomimitic alikeness Google Scholar indexed journals zero-dimensional articles zero-dimensional Research articles zero-dimensional review articles zero-dimensional PubMed articles zero-dimensional PubMed Central articles zero-dimensional 2023 articles zero-dimensional 2024 articles zero-dimensional Scopus articles zero-dimensional impact factor journals zero-dimensional Scopus journals zero-dimensional PubMed journals zero-dimensional medical journals zero-dimensional free journals zero-dimensional best journals zero-dimensional top journals zero-dimensional free medical journals zero-dimensional famous journals zero-dimensional Google Scholar indexed journals
Article Details
1. Introduction
Bioderived polymers, also known as biopolymers are the polymers derived from plants (polysaccharides, like-cellulose, chitosan, guar gum and chitin, etc.) and animals (proteins, like-collagen, gelatin, etc.) which have been conventionally utilized/examined by scientists/technologist into diverse applications in biomedical field extending from edible and non-edible packaging, medicated drug delivery systems and tissue regeneration [1-23] owing to their biomimitic alikeness when contrasted and compared with the extracellular matrix (ECM) tissues, biocompatibility, easily accessible, cheap, and non toxicity [24-26]. Moreover, these polymers upon cyto-degradation within the bio-system framework generates cyto-friendly end-products [20, 27].
Biopolymer nanocomposites are a kind of composite which comprises of a biopolymer or bio-copolymer matrix framework reinforced/loaded up using nanocrystals/nanofillers/nanoparticles [23]. These nanoparticles have at least one of their dimensions within the range of 1-100 nm in addition to its novel properties. These nanoparticles/fillers are categorized into zero-dimensional nanoparticles (metal oxides/clusters), one-dimensional nanoparticles (nanotubes or nanofibres), two-dimensional nanoparticles (layered materials, for example, layered silicates or nanoclays) and three-dimensional (zeolites). The benefits of nanocomposite materials in contrast with customary composites are their superior thermal, mechanical and hindrance/barrier properties at low reinforcement levels [23, 28, 29], in addition with better recyclability, transparency, UV blockage, and lightweight [23].
Cellulose is one of the most abundantly available biomaterial and highly involved in research studies on earth [30]. Currently, cellulose-based nanomaterials like CNC are a rising class of nanomaterials with some appealing properties: which are isolated from sustainable crude raw materials (cellulose or lignocellulose) at comparatively low cost with certain attractive properties like - biodegradability, biocompatibility, phenomenal mechanical strength, high water absorption ability, and high surface area. CNCs have been explored for its various potential applications in biopolymer nanocomposites for sustained drug delivery, tissue scaffolding, tin films, rheology modifiers for hybrid films, aerogels, reinforcement in hydrogels, artificial blood vessels, food additives, and wound dressings [20, 22, 31, 32].
These words CNC is used to depict highly crystalline rice shaped or needle-like form of nanocellulose derived from cellulosic or lignocellulosic materials, like jute, ramie, sisal, cotton, sugar beet pulp, wood pulp, etc through controlled acid/enzymic hydrolysis, and advanced mechanical/chemo-mechanical treatment [20, 22, 31-33]. CNCs are also frequently referred to as cellulose whiskers, cellulose nanowhiskers, or cellulose nanoparticles [9, 12, 20, 33, 34]. Evidently, the kind of drug delivery systems (DDSs) chosen for drug administration takes part in controlling the drug pharmacological impact with the pharmacokinetic profile concerning the drug release rate, the site, bioavailability and also the side effects. A productive/effective DDS affirms exact and accurate bioavailability within the required duration [26]. The drug concentration at the favorable site should be over the minimal effective concentration (MEC) and below the minimal toxic concentration (MTC) for the avoidance of any intricate complications. The DDS, and dosing, adapted for the drug administration is imperatively crucial for fulfillment of the required concentration [26]. In the last hundreds of decades, human advancements and evolution have successfully used chemical substances for different fields including cosmetics and medical purposes. In the same manner, substances utilized specifically for eye treatment have been used in ophthalmic medication for ocular diseases [3].
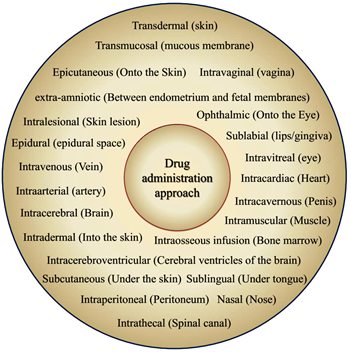
Figure 1: The scheme showing different drug administration approaches.
The delivery/administration of drug entities have been allegedly reported to be epidural (epidural space) [35], Intracerebral (Cerebrum-direct injection into the brain) [36], Intracerebroventricular (Cerebral ventricles of the brain) [37], epicutaneous (Onto the Skin) [38], Intradermal (Into the skin) [39], Subcutaneous (Under the skin) [40], Intralesional (Skin lesion) [41], Nasal (Nose) [42], Inhalational (anesthetics), Intravenous (vein) [43], Intraarterial (artery) [44], Intramuscular (Muscle) [45], Intracardiac (Heart) [46], Intraosseous infusion (Bone marrow) [47], Intrathecal (Spinal canal) for spinal anesthesia [48], Intraperitoneal (Peritoneum) [49], Intracavernous (via penis) [50], Intravaginal delivery (via vagina) [51], extra-amniotic (administration Between endometrium and fetal membranes) [52], Transdermal (via intact skin) [10, 23, 53], Transmucosal (Through the mucous membrane) [54], Sublingual (beneath the tongue) [55], and Sublabial (Between the lips and gingival) [56] as depicted in Figure 1. Ophthalmic medication transport system presents noteworthy troubles for pharmaceutical and therapeutic sciences. Visual diseases are muddled to treat, and visual structures ought to be protected, non-unfavorably susceptible for the patient and sterile. Topical structures address 90% of the stepped detailing. This review adopts a multidisciplinary strategy to the thought of the feasibility and potential utilization of CNC based polymer nanocomposites in the advancement of ophthalmic drug delivery systems (ODDS).
2. Cellulose Nanocrystals (CNC)
Cellulose (as structurally depicted in Figure 2) is the richest available bio-polymer on the planet. In cotton fibre, it is accessible in its unadulterated form and in jute, ramie, flax, wood, bombax, and other lignocellulose sources it is with a blend of lignin and hemicelluloses [9, 12]. Cellulose is a polydispersed linear polymer of poly-(1, 4)- D-glucose units [9, 20, 23], the base unit consists of two chair form molecules of glucose balanced by 180° that is displayed in Figure 1. Nanocellulose can be extensively classified into cellulose nanocrystals, nanofibres or bacterial cellulose (CNC/CNF/BC) with minimum any one of its dimensions ranging between 5-100 nm. Nanocrystalline cellulose precious stones (cellulose nanocrystals) is the smallest in dimension and most crystalline type of nanocellulose [9, 56].
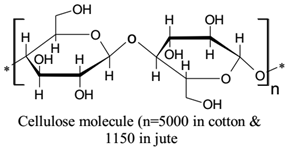
Figure 2: The molecular structure of a cellulose polymer with cellobiose is the smallest repeating unit in the polymer.
2.1 Sources and synthesis of CNC
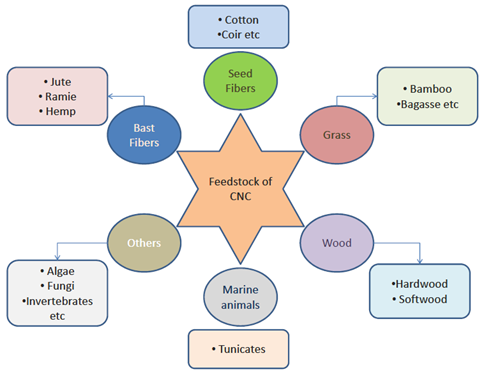
Figure 3: Sources of CNC.
The extraction of CNC mostly incorporates processes like cryocrushing, high-pressure homogenization, grinding, refining and chemical processes such as acid hydrolysis, steam explosion, enzymic hydrolysis [2, 6, 7, 59-63]. The various strategies are briefly shown in the Figure 3.
2.2 Properties of CNC
Nanocellulose stands out amongst other nanomaterials, as it is one of the most preferred nanomaterial for being lightweight, stable, extremely tough, having high mechanical strength, high UV resistance and furthermore it has phenomenal barrier properties [12, 23]. Nanocellulose has a density of 1.3/cm3 as reported [13]. The tensile strength of nanocellulose/CNC is more significant than that of Kevlar and steel [11, 13-16]. CNC possess length scope of 89 ? 250 nm (from lignocelluloses or celluloses) or ? 100 nm up to more than several ?m (for bacteria, tunicates, and algae source) having thickness of 5 ? 77 nm. Nanocellulose can be isolated into amorphous and crystalline domains by controlled degeneration procedure like acid hydrolysis resulting into crystalline domains with an elastic modulus of 150 GPa, which is very higher than that of the S-glass (85 GPa) and aramid fibers (65 GPa). These nanocrystals forms gels in water that shows shear-thinning and thixotropic behavior. CNC has a lot of ?OH groups on its surface, which participates in the development of inter and intra molecular hydrogen bonds between parallel chains and also within the same chain [11, 14-16]. CNC has a high affinity to water which is strong because of the surface covered ?OH groups. It forms highly viscous dispersions at low concentration. Removal of water from nanocelluloses, like, CNC at room temperature or above, usually results in the development of -H-H-bonds between the neighboring CNC. This gives the development of firmly close-packed mesh like fiber network arrangement which is generally irreversible and is commonly referred as hornification [15].
3. Ophthalmic Drug delivery systems (ODDS)
Serendipity has always been an important aspect of great scientific endeavors. Mankind has witnessed several serendipitous discoveries and inventions throughout its evolutionary phase. In this context a brief account of the evolution of drug delivery and its evolutionary timeline has been disinterred while segueing into ODDS. A focused assay of the role of CNC in these domains is the essence of this section. The major face off to the progress in traditional eye drops formulations with the desire to treat eye illness is effective bioavailability of the drugs at the drug target for a long time period, with negligible or no side effects, enhanced patient adherence etc. for diseases such as diabetic retinopathy, glaucoma. In these perspective, key advances in sustained delivery of loaded drugs to the eye is the utilization of using invasive delivery systems, such as intravitreal implants and drug suspensions.
Biopolymers (natural/synthetic) such as cellulose, methylcellulose, hydroxylpropyl methylcellulose, PVA, PLA, hyaluronic acid, guar gum, chitosan, etc. demonstrate valuable viscosity enhancing characteristics in polymer based ophthalmic drug formulations aimed at enhanced bioavailability [3, 20, 24]. The solution of these macromolecules with water results in the formation of viscoelastic hydrogels having evident potential as carriers in drug delivery and other biomaterials application [24]. The swelling properties, chemical properties and structural morphology of the these gels to a great extent controls the release mechanism of the drugs loaded in this systems [20, 25]. The resistance of polymer based ophthalmic drug delivery devices such as CNC-polymer based ODDS formulations to lacrimal drainage when residing in the lower conjunctival cul-de-sac of the eye is very important in ODDS though it has an initial blurring of vision of the patient. Visual medication conveyance is hampered by the physiological hindrances introduced by the eyes [20]. These incorporate squinting and wash out by tears, nasolacrimal waste, ineffective misfortunes and impermeability of the cornea [3, 20]. The use of polymer based CNC composites, or their hybrids is very promising in the field of ODDS although awareness on the novel properties of CNC in this respect is not know by many researcher, scientist or technologist working in this field. There is much room for the synthesis, study, and application of CNC based ODDS for advanced ocular application.
4. Polymeric Hydrogels based on CNC Polymer Composites (PC) in ODDS
There has been a limited study performed for potential application of novel CNC in ODDS which may be due to lack of information on its excellent properties as rheology modifiers in hydrogels. Dilution and drainage from the eye are the major causes of the poor bioavailability of ophthalmic solutions which can be overcome by using CNC based in situ-forming ODDS prepared from smart polymers (polymers that exhibit reversible phase transitions) [20]. Qinghua Xu and co-workers developed a nanocomposite hydrogel based on cellulose nanocrystal (CNC) and chitosan (CS) which are the two most abundant natural polymers and studied the drug release performance of the composite in controlled delivery of theophylline [21]. In the process, they first oxidized CNC using periodate treatment to obtain dialdehyde nanocellulose (DACNC). Then, they crosslinked chitosan using DACNC (as both the matrix and crosslinker) in different weight ratios, to fabricate CNC/CS composites. Also, an extra advantage of using DACNC is that, it is nontoxic in nature as compared to glutaraldehyde which is commonly used but is toxic in nature hence, can be used in biomedical application without any complexity. They found that there was an increase in swelling ratio of the composite, which was probably due to decline of crosslinking density [21]. Also, the pH responsive hydrogel gave different bioavailability at different pH. They achieved bioavailability of 85% and 23% in gastric pH of 1.5 and in intestinal fluids which has pH of 7.4 respectively, due to swelling ratio of the hydrogels loaded with drug which differed under different pH values. These CNC/CS hydrogel showed application potential as a theophylline carrier which can be potentially used in biosensors and ODDS [21].
In another study, Ahlen et al. developed nanoparticle loaded hydrogel based contact lenses and explored its potential for the ODDS. They developed two potential contact lens platforms for ODDS by integrating chitosan-poly (acrylic acid) nanoparticles into polyvinyl alcohol (PVA) hydrogels and in situ gelled nanoparticles and cellulose nanocrystals (CNC) in PVA lenses. The nanoparticles were shown to disintegrate in a physiological 0.2 mM concentration of lysozyme resulting from the hydrolysis of the chitosan chains by lysozyme. A drug prolong release over 28 hours? period was observed after incorporation of the nanoparticles in the composite lenses [19]. They revealed from their study that the nanoparticle-CNC-PVA lenses showed even greater potential for extended drug release [19] which they attributed to the particles leaching from the swelling PVA-network during the incubation period. These researchers also observed that the in situ gelation between the nanoparticles and cellulose nanocrystals were preventing the leaching by interlocking the particles to the CNC, and causing the gel to become immobilized in the PVA-network [19]. They concluded that the material showed countless possibilities in designing novel controlled drug release ocular lenses [19] along with the possibility of developing an enzyme-triggered ocular drug delivery system.
Another group of researchers have demonstrated an in vitro sustained release of pilocarpine hydrochloride (PL) from poloxamer (PM) modified CNC with enhanced rheological and overall properties for ODDS [20]. These authors reveal that the transport phenomenon of all the PM and its nanocomposite hydrogels was anomalous transport while the critical gelation concentration of PM reduced from 18% (w/v) to 16.6% (w/v) with the addition of different CNC% (w/v). They also showed from their report that the addition of different CNC% (w/v) in PM for the engineered nanocomposite hydrogels led to excellent sustained release of the PL up to more than 20 hrs [20]. They observed that the in vitro drug release was best explained by the first-order equation which showed the highest linearity (r2>0.981) for all the CNC-nanocomposites [20].
Yet in an interesting work investigated by Katarzyna Zubik et al., on thermo-responsive hydrogels containing poly (N-isopropylacrylamide) (PNIPAAm), reinforced with CNC by means of both covalent and non-covalent interactions with it [64]. They synthesized the nanocomposite material via free-radical polymerization without any additional cross-linkers. Variation in properties of PNIPAAm-CNC hybrid hydrogels change with dosage of CNC was reported also showing declined thermal stability of the hydrogels with increasing CNC content64. Also, it was observed that the rheological parameters such as elastic and viscous moduli of hydrogels increased with the higher amounts of CNC addition, representing stronger mechanical properties of the hydrogels, which supports the hypothesis that after incorporation of CNC the hydrogel exhibit superior structural integrity. Their work showed that the thermoresponsive behavior of PNIPAAm-CNC hybrid hydrogels, the volume phase transition temperature (VPTT) in the range of 36 to 39°C, which is close to normal human body temperature [64]. A study on drug loading and release properties of the prepared hydrogels was also conducted for wound dressing purposes and metronidazole, an antibiotic and antiprotozoal often used for skin infections, was used as a target drug for study. The hydrogels performed well and showed decent drug-loading capacity at ambient temperature and a burst drug release, which was followed by slow and sustained release at 37°C. Their results suggested that the developed CNC based hydrogels stand out as a promising material for application in ophthalmic drug delivery system (ODDS) and injectable hydrogels for wound dressing [64].
5. Preparation Techniques of CNC based Nanocomposite Hydrogel
From the available methods for the preparation of NC based ophthalmic gels (OG) the most preferred one, is the one which is carried out using the conditions for the fabrication of gels from the polymer matrix. Considering an example, wherein a solvent containing DMSO with water in the ratios of 80:20, 70:30 and 60:40 was used by Tummala et al., [65] these were then heated at 100°C along with constant stirring for 2 h. The synthesis of the nanocomposite hydrogel was done with the addition of nanocellulose gel which was weighed equivalent to 30 mg dry weight of the PVA solutions. It was then kept for stirring at 100°C for about an hour until it was homogeneous and transparent solution. It was then casted into polypropylene molds which were followed by gelling at -20°C for the entire day and then it was dialyzed in distilled water for two more days. The storage was done in distilled water for any further characterizations.
6. Kinetics of Drug release in CNC based Ophthalmic Formulations
A group of swelling controlled drug delivery systems includes drug-loaded hydrogel-based devices along with OG. It is assumed that the swelling of the polymer is a result of interaction between hydrophilic polymer chains with water. As a result of interaction between the absorbed water and the hydrogel polymer drop the hydrogel turns into a rubbery kind of material, this phenomena occurs due to decrease in Tg temperature of the polymer. As a result of this interaction the absorbed water molecules within the gel structure will dissolve the trapped drug inside the device.66 Controlling of this phenomenon depends mainly on three driving forces which are the penetrant concentration gradient, the polymer stress gradient, and the osmotic forces involved in it. Considering cellulose based hydrogels which are also known as swelling controlled drug delivery devices, there has been anomalous transport system reported by Serra et al. whereas Dewan et al. came up with the Fickian diffusion/transport mechanism in case of the hydrophilic devices used for hydrogel drug delivery systems [3, 67, 68]. It is concluded that the drug release kinetics particularly for hydrophilic hydrogels is often identified by an intermediate between the Fickian diffusion and case II transport.
Currently taking into consideration, the kinetics of release of NC based ophthalmic systems is quite rare or nearly negligible. Although, the only report accessible is based on methylcellulose (MC) based ophthalmic medication discharge device which can prove to be envisioning the mechanism of drug discharge from NC based ophthalmic frameworks [3]. A discovery made by Dewan and co revealed that MC was efficient in reducing the critical gelation concentration from 18% to 17% (wt/v) and the gelation temperature of poloxamer from 34°C to 28°C. Additionally, it was also identified that the release mechanism of the formulation system is often pursued by the Fickian diffusion only [3], and also it was dependent on the molecular weight of MC employed in formulations; greater the molecular weight of MC better-sustained drug release of the device was observed. Also, there were some other close cellulose derivatives reported, like thermally triggered transitions of hydroxypropylcellulose [68] and methylcellulose [3], carboxymethyl cellulose [69], poly(vinyl alcohol)/methylcellulose [68], Carbopol/HPMC [70], and hyaluronic acid-methylcellulose [71].
7. Challenges and the Future of Bio CNC PC DDS
CNC based ODDS nanocomposites systems are structures composed of macromolecules for instance chitosan, cellulose, guar gum, their nanoparticles (nanofibers, nanorods, or nanostructures), and nanocomposites with themselves and other polymeric matrices. The use of nanoparticles such as CNC is advantageous because of their biomimetic structures which resemble biological living tissues having excellent cell adherence ability. Furthermore, the exploit of liquid CNC crystalline phases in hydrogels allows the development of self-assembled hierarchical structures that mimetic to ECM of living organisms for the engineering of bionanomaterials for advance applications. There is still much room for the marketing, pharmaceutical, and clinical application this system. In spite of their limitations, the utilization of nontoxic, biodegradable, sustainable, and biocompatible renewable materials such as CNC based composite materials continue as focus of contemporary research studies cut across every niche in biomaterial. CNC PC nanocomposites have shown great potentials for engineering new advanced ODDSs for effective delivery of drugs for increased bioavailability. However, there are no research publications or practical utilization of even the few reports on CNC PC ODDS at the moment. There is fervent need for more studies in this area.
8. Conclusion
Apparently, there are limited research on CNC-polymer based ophthalmic formulations for ODDS which calls for urgent research into the utilization of the novel properties of CNC such as its ability to increase the gel strength, enhance sustained delivery of drugs via hydrophilic interaction of the -OH groups on the surface of CNC to the polymer and CNC to the drugs along with enhanced gel strength and reduced gel dissolution rate.
Acknowledgement
Soumyadip Dutta and Diphankar Das wish to express their profound gratitude to the Department of Polymer Science and Technology, and the Centre for Research in Nanoscience and Nanotechnology (CRNN), University of Calcutta for availing them with this golden opportunity. Jonathan Tersur Orasugh acknowledges the Centre for Research in Nanoscience and Nanotechnology (CRNN), Department of Polymer Science and Technology, and Department of Jute and Fibre Technology, Institute of Jute Technology, the University of Calcutta for supporting his research work.
References
- Kumbar SG, Toti US, Deng M, et al. Novel mechanically competent polysaccharide scaffolds for bone tissue engineering. Biomed Mater 6 (2011): 065005.
- Michell AJ. Wood cellulose-organic polymer composites. Comp Asia Pac, Adelaide, Australia 89 (1989): 19-21.
- Dewan M, Bhowmick B, Sarkar G, et al. Effect of methyl cellulose on gelation behavior and drug release from poloxamer based ophthalmic formulations. Int J Bio Macro 72 (2015): 706-710.
- Paakko M, Ankerfors M, Kosonen H, et al. Enzymatic Hydrolysis Combined with Mechanical Shearing and High-Pressure Homogenization for Nanoscale Cellulose Fibrils and Strong Gels. Biomacromolecules 8 (2007): 1934-1941.
- Dutta K, Das B, Orasugh TJ, etal. Bio-derived cellulose nanofibril reinforced poly(N-isopropylacrylamide)-g-guar gum nanocomposite: An avant-garde biomaterial as a transdermal membrane. Polymer 135 (2018): 85-102.
- Iwamoto S, Nakagaito AN, Yano H. Optically transparent composites reinforced with plant fiber-baed nanofibers. Appl Phy A: Mat Sci Proc 89 (2007): 461-466.
- Nakagaito AN, Yano H. The effect of morphological changes from pulp fiber towards nano-scale fibrillated cellulose on the mechanical properties of high-strength plant fiber based composites. Appl Phy A-Mat Sci Prog 78 (2004): 547-552.
- Orasugh JT, Saha RN, Rana D, et al. Jute cellulose nano-fibrils/hydroxypropylmethylcellulose nanocomposite: A novel material with potential for application in packaging and transdermal drug delivery system. Ind Crop Prod 112 (2018b): 633-643.
- Orasugh JT, Saha RN, Sarkar G, et al. Synthesis of methylcellulose/cellulose nano-crystals nanocomposites: Material properties and study of sustained release of ketorolac tromethamine. 188 (2018c): 168-180.
- Sarkar G, Orasugh TT, Saha RN, et al. Cellulose nanofibrils/chitosan based transdermal drug delivery vehicle for controlled release of ketorolac tromethamine. New J Chem 41 (2017): 15312-15319.
- Kolakovic R, Peltonen L, Laukkanen A, et al. Nanofibrillar cellulose films for controlled drug delivery. J Pharm Biopharm 82 (2012): 308-315.
- Wustenberg T. Cellulose and Cellulose Derivatives in the Food Industry. 1st Wiley-VCH Verlag GmbH and Co. KGaA (2015): 91-142.
- Orasugh JT, Saha NR, Sarkar G, et al. A facile comparative approach towards utilization of waste cotton lint for the synthesis of nanocrystalline cellulose crystals along with acid recovery. Int J Bio Macro 109 (2018a): 1246-1252.
- Cao X, Ding B, Yu J, et al. Cellulose nanowhiskers extracted from TEMPO-oxidized jute fibers. Carbohyd Polym 90 (2012): 1075-1080.
- Barbash VA, Yaschenko OV, Shniruk OM. Preparation and properties of Nanocellulose from Organosolv Straw Pulp. Nanoscale Res Let 12 (2017): 241.
- Diniz J, Gil MH, Castro J. Hornification: its origin and interpretation in wood pulps. Wood Sci Tech 37 (2004): 489-494.
- Kolakovic R, Peltonen L, Laukkanen A, et al. Evaluation of drug interactions with nanofibrillar cellulose. Europ J Pharm Biopharm 85 (2013): 1238-1244.
- Siro I, Plackett D. Microfibrillated cellulose and new nanocomposite materials: a review. Cellulose 17 (2010): 459-494.
- Wafaa S, Elseoud A, Hassan LM, et al. Chitosan nanoparticles/cellulose nanocrystals nanocomposites as a carrier system for the controlled release of repaglinide. Int J Biol Macromol 111 (2018): 604-613.
- Ahlen M, Tummala KG, Mihranyan A. Nanoparticle-loaded hydrogels as a pathway for enzyme-triggered drug release in ophthalmic applications. Int J Pharm 536 (2018): 73-81.
- Orasugh JT, Sarkar G, Saha NR, et al. Effect of cellulose nanocrystals on the performance of drug loaded in situ gelling thermo-responsive ophthalmic formulations. Int J Bio Macro 124 (2019): 235-245.
- Xu Q, Ji Y, Sun Q, et al. Fabrication of Cellulose Nanocrystal/Chitosan Hydrogel for Controlled Drug Release. Nanomaterials 9 (2019): 253.
- Orasugh JT, Saha NR, Sarkar G, et al. A facile comparative approach towards utilization of waste cotton lint for the synthesis of nano-crystalline cellulose crystals along with acid recovery. Int J Bio Macro 109 (2018a): 1246-1252.
- Orasugh JT, Saha RN, Rana D, et al. Jute cellulose nano-fibrils/hydroxypropylmethylcellulose nanocomposite: a novel material with potential for application in packaging and transdermal drug delivery system. Ind Crop Prod 112 (2018b): 633-643.
- Shahwal VK. Ocular drug delivery: an overview. Int J Biomed Adv Res 2 (2011): 167-187.
- Nazar H, Roldo M, Fatouros DG, et al. Hydrogels in mucosal delivery. Ther Deliv 3 (2012): 535-555.
- Prausnitz MR, Gill HS, Park JH. Modified Release Drug Delivery. In Eds.: Rathbone MJ Hadgraft J, Roberts MS, et al. New York: Informa Healthcare (2008).
- Mkedder I, Travelet C, Durand-Terrasson A, et al. Preparation and enzymatic hydrolysis of nanoparticles made from single xyloglucan polysaccharide chain. Carbohydr Polym 94 (2013): 934-939.
- Wang B, Sain M. Dispersion of soybean stock?based nanofiber in a plastic matrix. Polym Int 56 (2007): 538-546.
- Henriette MC Azeredo, Luiz Henrique C Mattoso, Roberto J Avena?Bustillos, et al. Nanocellulose Reinforced Chitosan Composite Films as Affected by Nanofiller Loading and Plasticizer Content. J Food Sci 75 (2010): 1.
- Domingues AMR, Manuela E Gomes, Reis LR. The Potential of Cellulose Nanocrystals in Tissue Engineering Strategies. Biomacromolecules 15 (2014): 2327-2346.
- Plackett DV, Letchford K, Jackson JK, et al. A review of novel cellulose as a novel vehicle for drug delivery. Nord Pulp Pap Res J 29 (2014): 105-118.
- Dong S, Cho HJ, Lee YW, et al. Synthesis and Cellular Uptake of Folic Acid-Conjugated Cellulose Nanocrystals for Cancer Targeting. Biomacromolecules 15 (2014): 1560-1567.
- Moon RJ, Martini A, Nairn J, et al. Cellulose nanomaterials review: structure, properties and nanocomposites. Chem Soc Rev 40 (2011): 3941-3994.
- Tuman KJ, McCarthy RJ, March RJ, et al. Effects of epidural anesthesia and analgesia on coagulation and outcome after major vascular surgery. anesth analg 73 (1991): 696-704.
- McKeran RO, Firth G, Oliver S, et al. A potential application for the intracerebral injection of drugs entrapped within liposomes in the treatment of human cerebral gliomas. J Neur Neur Psych 48 (1985): 1213-1219.
- Goudas LC, Langlade A, Serrie A, et al. Acute decreases in cerebrospinal fluid glutathione levels after intracerebroventricular morphine for cancer pain. Anesth Analg 89 (1999): 1209-1215.
- Ohlsen L, Englesson S, Evers H. An anaesthetic lidocaine/prilocaine cream (EMLA) for epicutaneous application tested fpr cutting split skin grafts. J Plast Surg Hand Surg 19 (1985): 201-209
- Rangaka MX, Wilkinson KA, Seldon R, et al. Effect of HIV-1 infection on T-Cell-based and skin test detection of tuberculosis infection. Am J Respir Crit Care Med 175 (2007): 514-520.
- Pickup JC, Keen H, Parsons J, et al. Continuous Subcutaneous Insulin Infusion: An Approach To Achieving Normoglycaemia. Brit Med J 1 (1978): 204-207.
- Layton AM, Yip J, Cunliffe WJ. A comparison of intralesional triamcinolone and cryosurgery in the treatment of acne keloids. Br J Dermatol 130 (1994): 498-501.
- Graf P, Hallen H, Juto JE. Benzalkonium chloride in a decongestant nasal spray aggravates rhinitis medicamentosa in healthy volunteers. Clin exp allergy 25 (1995): 395-400.
- Buchman AL, Dubin MD, Moukarzel AA, et al. Choline deficiency: a cause of hepatic steatosis during parenteral nutrition that can be reversed with intravenous choline supplementation. Hepatology 22 (1995): 1399-1403.
- Kaku Y, Yonekawa Y, Tsukahara T, et al. Superselective intra-arterial infusion of papaverine for the treatment of cerebral vasospasm after subarachnoid hemorrhage. J Neurosurg 77 (1992): 842-847.
- Khorana N, Pullagurla MR, Dukat M, et al. Stimulus effects of three sulfur-containing psychoactive agents. Pharmacol Biochem 78 (2004): 821-826.
- Lindner KH, Haak T, Keller A, et al. Release of endogenous vasopressors during and after cardiopulmonary resuscitation. Heart 75 (1996): 145-150.
- Rosetti VA, Thompson BM, Miller J, et al. Intraosseous infusion: an alternative route of pediatric intravascular access. Ann Emerg Med 14 (1985): 885-888.
- Watterson J, Toogood I, Nieder M, et al. Excessive spinal cord toxicity from intensive central nervous system-directed therapies. Cancer 74 (1994): 3034-3041.
- Karl DN, Zbylut JT. The peritoneal dialysis system. Perit Dial (1989): 13-27.
- Brock G, Tu LM, Linet OI. Return of spontaneous erection during long-term intracavernosal alprostadil (Caverject) treatment. Urology 57 (2001): 536-541.
- Martinez MF, Adams GP, Kastelic JP, et al. Induction of follicular wave emergence for estrus synchronization and artificial insemination in heifers. Theriogenology 54 (2000): 757-769.
- Gustavii B. Studies on the mode of action of intra-amniotically and extra-amniotically injected hypertonic saline in therapeutic abortion. Acta Obstet Gynecol Scand 52 (1973): 2-22.
- Stapleton JA, Russell MA, Feyerabend C, et al. Dose effects and predictors of outcome in a randomized trial of transdermal nicotine patches in general practice. Addiction 90 (1995): 31-42.
- Hernandez SH, Nelson LS. Prescription drug abuse: insight into the epidemic. Clin Pharmacol Ther 88 (2010): 307-317.
- Patel NK, Panchol SS. An overview on: sublingual route for systemic drug delivery. Int J Res Pharm Biomed Sci 3 (2012): 913-923.
- Koren I, Tuvia H, Rappaport ZH,et al. Endoscopic transnasal transsphenoidal microsurgery versus sublabial approach for the treatment of pituitary tumors: endonasal complication. Laryngoscope 109 (1999): 1838-1840.
- Helbert W, Cavaille JY, Dufresne A. Thermoplastic nanocomposites filled with wheat straw cellulose whiskers. Part I: Processing and mechanical behavior. Polym Comp 17 (1996): 604-611.
- Cheriana BM, Leao AL, Ferreira de Souza S, et al. Isolation of nanocellulose from pineapple leaf fibres by steam explosion Carbohyd. Polym 81 (2010): 720-725.
- Wang B, Sain M. Dispersion of Soybean stock-based nanofibre in a plastic matrix. Polym Int 56 (2007): 538-546.
- Bhatnagar A, Sain M. Processing of cellulose nanofiber-reinforced composites. J Reinf Plas Comp 24 (2005): 1259-1268.
- Qua EH, Hornsby PR, Sharma HSS, et al. Preparation and characterisation of cellulose nanofibres. J Mat Sci 46 (2011): 6029-6045.
- Kumar A, Negi YS, Choudhary V, et al. Characterization of Cellulose Nanocrystals Produced by Acid-Hydrolysis from Sugarcane Bagasse as Agro-Waste. J Mat Phys Chem 2 (2014): 1-8.
- Klemm D, Kramer F, Moritz S, et al. Nanocelluloses: a new family of nature-based materials. Angew Chem Int Ed 50 (2011): 5438-5466.
- Zubik K, Singhsa P, Wang Y, et al. Thermo-Responsive Poly(N-Isopropylacrylamide)-Cellulose Nanocrystals Hybrid Hydrogels for Wound Dressing. Polymers 9 (2017): 119.
- Tummala GK, Joffre T, Lopes VR, et al. Hyperelastic Nanocellulose-Reinforced Hydrogel of High Water Content for Ophthalmic Applications. ACS Bio Sci Engin 2 (2016): 2072-2079.
- Almeida H, Amaral MH, Lobao P, et al. Applications of poloxamers in ophthalmic pharmaceutical formulations: an overview. Exp Opin Drug Del 10 (2013): 1223-1237.
- Serra L, Dome'nech J, Peppas AN. Drug transport mechanisms and release kinetics from molecularly designed poly(acrylic acid-g-ethylene glycol) hydrogels. Biomaterials 27 (2006): 5440-5451.
- El-Naggar MWA, Sennaa MM, Mostafa AT, e al. Radiation Synthesis and Drug Delivery Prpperties of Interpentrating Networks (IPNS) Based on (Vinyl alcohol)/methyl cellulose Blend Hydrogels. Int J Bio Macro 102 (2017): 1045-1051.
- Kono H. Characterization and properties of carboxymethyl cellulose hydrogels crosslinked by polyethylene glycol. Carbohyd Polym 106 (2014): 84-93.
- Wu C, Qi H, Chen W, et al. Preparation and evaluation of a Carbopol/HPMC-based in situ gelling ophthalmic system for puerarin. Yakugaku Zasshi 127 (2007): 183-191.
- Mayol L, De Stefanoa D, De Falcoa F, et al. Effect of hyaluronic acid on the thermogelation and biocompatibility of its blends with methyl cellulose. Carbohydr Polym 112 (2014): 480-485.

 Impact Factor: * 1.2
Impact Factor: * 1.2 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 