Underdiagnosed Pulmonary Artery Thrombosis and Pulmonary Embolism in Rheumatic Heart Disease
Article Information
Lei Pu1,2, Yingjie Zhang1,2, Yaxiong Li1,2, Yingnan Yang1,2*
1Department of Cardiovascular Surgery, Yan'an Affiliated Hospital of Kunming Medical University, Kunming, Yunnan, PR China
2Cardiovascular Surgery Institution of Yunnan, Kunming, Yunnan, PR China
3Key Laboratory of Cardiovascular Disease of Yunnan Province, Kunming, Yunnan, PR China
*Corresponding Author: Yingnan Yang, Department of Cardiovascular Surgery, Yan'an Affiliated Hospital of Kunming Medical University, Kunming, Yunnan, PR China
Received: 10 March 2019; Accepted: 13 March 2019; Published: 16 March 2019
Citation: Lei Pu, Yingjie Zhang, Yaxiong Li, Yingnan Yang. Underdiagnosed Pulmonary Artery Thrombosis and Pulmonary Embolism in Rheumatic Heart Disease. Cardiology and Cardiovascular Medicine 3 (2019): 030-033. This
View / Download Pdf Share at FacebookAbstract
Pulmonary embolism is a life-threatening acute cardiovascular disease and not easy to make an immediate diagnosis in clinical arena. A 46-year-old female with underdiagnosed pulmonary artery thrombus and pulmonary embolism in rheumatic heart disease, the patient’s presentation, diagnostic procedure and successful treatment are presented.
Keywords
Pulmonary artery thrombus; Pulmonary embolism; Rheumatic heart disease
Article Details
1. Clinical Case
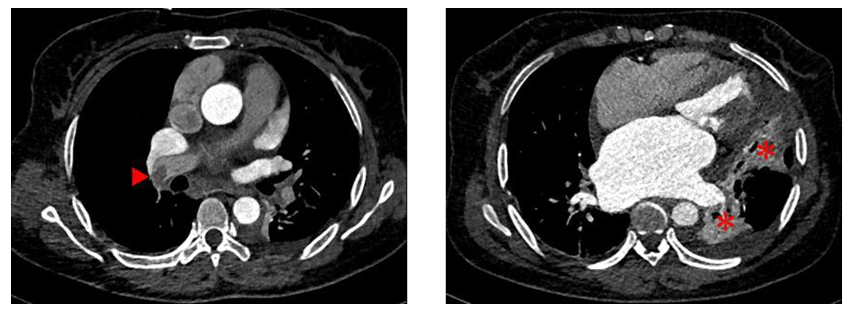
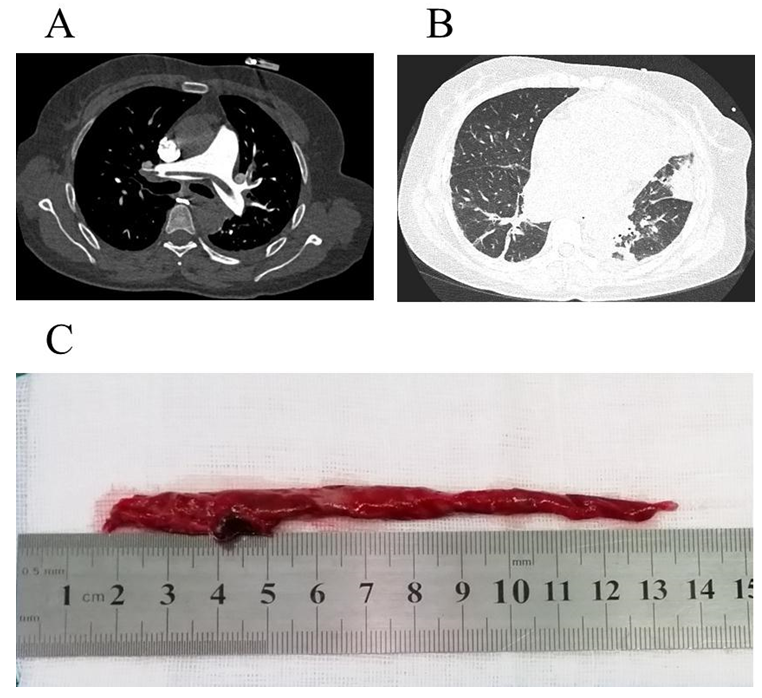
A 46-year-old female presented with a 24-hour history of sustained left epigastrium ache, accompanied with abdominal distension, cough, short of breath, and severe lower extremity edema. The initial diagnosis and treatment were concentrated in gastro-enteritis at rural health center for 7 days. However, the mentioned symptoms were non-significantly relieved. Subsequently, she was admitted to local tertiary hospital and diagnosed with rheumatic heart disease (RHD). After 10 days of pharmacological treatment (diuresis and inotropic medications), she was been referrals to our department. Physical examination exhibited the patient was in poor general condition, blood pressure of 90/60 mmHg, pulse rate of 106 beats per minute, respiratory rate of 32 breaths per minute with 92% oxygen saturation of blood on oxygen therapy (1 L/ml)?with typical malar flush and mild cyanotic lips, pulmonary auscultation showed crackles and lower breath sounds in left lung, cardiac auscultation indicated arrhythmic and mild-diastolic murmur at the apical region, engorgement of the jugular vein and moderate lower extremity edema. The diuretic and inotropic treatment was continued. Transthoracic echocardiography (TTE) confirmed moderate rheumatic mitral valve stenosis and regurgitation, moderate aortic valve regurgitation, moderate tricuspid regurgitation and significantly decreased left ventricular ejection fraction (40%). The estimated pulmonary artery systolic pressure was 60 mmHg. After that, coronary computed tomography angiography revealed normal coronary artery, filling defect of distal right pulmonary artery and atelectasis (Figure 1). Finally, pulmonary artery thrombus (PTA) and PE were detected by computed tomography pulmonary angiography (CTPA), the PTA was riding on the pulmonary bifurcation (Figure 2A). Pulmonary infarction was synchronously detected (Figure 2B). Furthermore, the D-dimer testing was 65.37 μg per litre. Deep venous thrombosis was excluded with ultrasonography and cancer was ruled out with computed tomography scan. The patient experienced urgent cardiopulmonary bypass assisted cardiac surgery and pulmonary embolectomy. The PAT was removed via an incision of pulmonary artery (Figure 2C). The patient was quickly recovered and discharged with oral anticoagulation on the 15th day postoperative.
2. Discussion
PAT has been reported in Eisenmenger syndrome, pulmonary artery aneurysm, pulmonary artery stump and the other disease conditions [1, 2]. According to current diagnostic algorithms of PE, Wells rule and Geneva score [3], the PE should be ruled out in this case. The D-dimer test has been extensively applied in the diagnosis of PE and the age-adjusted D-dimer threshold for non-invasive exclusion of PE has been proposed by Marc Righini and collagues [4]. However, the result of D-dimer testing in this case was 65.37μg per litre. Acute PE is characterized by substantial clinical manifestations which are result from a complex interplay between di?erent organs. In most patients of dyspnea, chest pain, haemoptysis, syncope, and unilateral extremity swelling, PE should be suspected [3]. In this case, the symptoms were variable and nonspecific, included left epigastrium pain, abdominal distension, cough, short of breath, and lower extremity edema were manifested. Parts of these symptoms are overlap with RHD, this is the primary cause of belated diagnosis. Therefore, a high index of clinical suspicion is a critical factor in the establishing diagnosis of PE. The left epigastrium pain might be related to the disturbances in left lower pulmonary circulation and local pleural involvement. In spite of the pharmacological treatment was continued more than 2 weeks, there was not in complete relief of clinical signs and symptoms in this case. These conditions suggested that clinical must consider the possibility of some other disease may combine in this case. Finally, the CTPA confirmed the diagnosis of PTA and PE. Surgical pulmonary embolectomy has been successfully performed before the introduction of medical treatment [3]. The remove of PAT can ameliorate right ventricular dysfunction, lung ventilation-perfusion match and pulmonary hypertension. The mechanism of PAT and PE in RHD patient has not been fully understood. Here, we infer that PAT and PE may result from mitral stenosis related pulmonary hypertension, left atrial blood turbulence and hypercoagulability.
3. Conclusion
This case highlights not only the frequent problem of PE is easily missed diagnosis, but also remind clinicians should maintain a high index of suspicion. We assume that the diagnosis of RHD in this case was an incidental finding and that she did not suffer from PTA, PE and right heart ventricular failure.
Conflict of Interest
None declared
References
- Broberg CS, Ujita M, Prasad S, et al. Pulmonary Arterial Thrombosis in Eisenmenger Syndrome Is Associated With Biventricular Dysfunction and Decreased Pulmonary Flow Velocity. Journal of the American College of Cardiology 50 (2007): 634-642.
- Cha S, Choi K, Shin K, et al. Clinical characteristics of in-situ pulmonary artery thrombosis in Korea. Blood Coagulation and Fibrinolysis 26 (2015): 903-907.
- Konstantinides SV, Torbicki A, Agnelli G, et al. 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism. Eur Heart J 35 (2014): 3033-3069.
- Righini M, Van Es J, Den Exter PL, et al. Age-Adjusted D-Dimer Cutoff Levels to Rule Out Pulmonary Embolism. JAMA 311 (2014): 1117.


 Impact Factor: * 3.5
Impact Factor: * 3.5 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 14.80%
Acceptance Rate: 14.80%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 