Arterial Hypertension Secondary to Renal Artery Stenosis in a Child: Diagnosis and Management, a Case Report
Isadora Langoni Amorim Barbosa1*, Tayenne do Vale Cabral¹, Mariana Carraro², Mariana Castro Loureiro Borges e Curi³
1Fellow in Pediatrics, Hospital de Clínicas da Universidade Federal do Triângulo Mineiro, Brazil
2Pediatric Cardiologist, Cardiovascular Unit, Hospital de Clínicas da Universidade Federal do Triângulo Mineiro, Brazil
3PhD. Pediatric Rheumatologist, Pediatric Unit, Hospital de Clínicas da Universidade Federal do Triângulo Mineiro, Brazil
*Corresponding author: Isadora Langoni Amorim Barbosa, Rua Isoldino Correa nº75, Bairro Vila Maria Helena – Uberaba/Minas Gerais – Brazil
Received: 01 June 2021; Accepted: 16 June 2021; Published: 25 June 2021
Article Information
Citation: Isadora Langoni Amorim Barbosa, Tayenne do Vale Cabral, Mariana Carraro, Mariana Castro Loureiro Borges e Curi. Arterial Hypertension Secondary to Renal Artery Stenosis in a Child: Diagnosis and Management, a Case Report. Archives of Clinical and Biomedical Research 5 (2021): 385-390.
View / Download Pdf Share at FacebookAbstract
Arterial hypertension (AH) in children up to 13 years old is defined as systolic blood pressure, diastolic blood pressure, or both above the 95th percentile for their age, sex, weight, and height by percentile. In children older than 13, it is defined by values greater than or equal to 130 × 80 mmHg. A diagnosis of Takayasu's arteritis is only established as set forth in the EULAR/PRINTO/PRES diagnostic criteria (2008) the mandatory criterion is an angiography of the aorta and its main branches or of the pulmonary arteries showing an aneurysm, dilatation, stenosis, occlusion, or thickening of the vessel wall, while discarding other possibilities. Additionally, at least one of these minor criteria must be present pulse deficit or claudication; blood pressure (BP) discrepancy in any of the four limbs; cardiac or arterial murmurs, systemic arterial hypertension; and acute-phase laboratory reactions (erythrocyte sedimentation rate > 20 mm or C-reactive protein above the reference value). To highlight the importance of BP evaluation in pediatric outpatient clinics, aiming for an early diagnosis to allow rapid management and a reduction of morbidity and mortality in pediatric patients. A previously healthy 8-year-old girl developed AH associated with headache and arthralgia. A diagnostic investigation was conducted, concluding that the AH was secondary to a stenosis of a renal artery, with a probable differential diagnosis of Takayasu's arteritis. An early and adequate clinical conduct causes an impact in reducing the morbidity and mortality of pediatric patients diagnosed with arterial hypertension and in maximizing their chances of recovery.
Keywords
<p>Arterial hypertension; Pediatrics; Takayasu arteritis; Renal artery stenosis; Diagnosis; Management</p>
Article Details
1. Introduction
Arterial hypertension (AH) in childhood has become an important global public health problem in recent decades [1-4]. This is very often due to late diagnoses caused by blood pressure (BP) not being measured in pediatric medical appointments, although it should be measured in all children over 3 years old at least once a year [4]. The 2017 guidelines of the American Academy of Pediatrics (AAP) and those (2016) of the European Society of Hypertension (ESH) define AH in children up to 13 years old as the presence of systolic blood pressure (SBP), diastolic blood pressure (DBP), or both above the 95th percentile for the child’s age, sex, weight, and height by percentile. In children older than 13 years, AH is defined by values greater than or equal to 130 × 80 mmHg. In both age ranges, three or more BP measurements on different occasions are required to establish a diagnosis [1-4].
The causes of AH may be primary or secondary [1]. Primary causes are associated with children over 6 years old with a positive family history for AH and excess weight or obesity [1-3]. Secondary causes are more common in children and adolescents, and their main agents are kidney diseases (39%–74%) and renovascular disorders (12%–13%) [1, 5-6]. In these cases, clinical pictures of children with severe AH stand out, often associated with lesions of target organs. These cases require investigation [1]. Among renovascular causes, renal artery stenosis is responsible for the highest proportion of cases, and most cases are caused by fibromuscular dysplasia. However, attention is required for differential diagnoses such as vasculites (Takayasu's arteritis), moyamoya disease, and congenital vascular anomalies [5-6]. The process of diagnosis of secondary AH in children and adolescents is still a significant challenge. The rarity of the cases and their complex diagnosis and management demonstrate that there are still many scientific gaps to fill [6].
Treatment of Takayasu's arteritis should be started as early as possible, aiming at a rapid control of the vascular inflammatory process to prevent the progression of vascular damage and the consequent development of stenoses, aneurysms, and ischemic and thrombotic complications [7]. Considering these facts, this study aims to highlight the importance of BP evaluation in pediatric outpatient clinics, aiming for an early diagnosis to allow rapid management and a reduction of morbidity and mortality in pediatric patients.
Furthermore, it aims to encourage the scientific community to discuss the best approach to these cases. This article will discuss these issues by reporting a case of secondary hypertension successfully treated.
2. Objective
To highlight the importance of BP evaluation in pediatric outpatient clinics, aiming for an early diagnosis to allow rapid management and a reduction of morbidity and mortality in pediatric patients.
3. Methods
The information contained in this clinical case description was obtained through clinical and procedure record review and interview.
4. Case Report
A female child, 8 years and 7 months old, student, sought assistance at HC-UFTM, accompanied by her mother, reporting “high BP” measured at home. After observation of AH by the family, the child was evaluated in other medical clinics, where the increased BP was confirmed. The patient also complained of recurrent headaches for over a year, as well as myalgia episodes, but these symptoms and the BP were never investigated. The mother reported that the child had undergone laboratory tests earlier, and that those tests were normal, but this was only a verbal report and the actual medical reports were not presented.
The patient was referred to the HC-UFTM outpatient clinic by a public emergency clinic. The physical examination showed moderate changes in the patient’s general condition. She was crying, complaining of abdominal pain, with normal skin perfusion, hydrated but with thick saliva. No cyanosis, jaundice, or fever was present. The heart rate was 116 bpm; the pulse was palpable on all four limbs, but appeared to be weaker on the feet than on the wrists. BP in both arms, both standing and in decubitus: 160 × 110 mmHg. The abdomen had reduced bowel sounds and was painful on diffuse palpation, but showed no signs of peritonitis.
The patient was referred to the Pediatric Emergency Room for hospitalization and better investigation of the case. During the investigation, an alteration of flow velocity was observed in the renal arteries. Echocardiography showed no signs of aortic coarctation, but electrocardiography evidenced left ventricular overload. Captopril 25 mg every 12 hours (1.6 mg/kg/day) was prescribed, associated with a strict control of diuresis and BP, and a low-sodium diet. A computed tomography angiography (CTA) of the abdomen showed a stenosis in the right renal artery. During hospitalization, the patient's BP remained high, and it was decided to increase the dose of captopril to 25 mg every 8 hours (2.5 mg/kg/day) and to start with hydrochlorothiazide 25 mg once daily (0.8 mg/kg/day). After the medication management, the patient's BP remained below the 90th percentile, with significant improvement.
In addition, a preliminary diagnosis of Takayasu's arteritis was made and an investigation for this diagnosis was started, with a CTA of the chest performed to rule out other causes of stenosis. The implantation of a stent was indicated. The patient was discharged from the hospital with BP levels appropriate for her age, and was prescribed captopril 25 mg every 8 hours (2.5 mg/kg/day), hydrochlorothiazide 25 mg/day (0.8 mg/kg/day), and acetylsalicylic acid 100 mg/day.
The patient later returned to the HC-UFTM Pediatric Emergency Room to undergo an angioplasty of the right renal artery with a 3.5 mm balloon, without complications. A biopsy was not possible. She evolved with blood pressure levels under control. Methotrexate 15 mg/m2 once a week was started to control Takayasu's arteritis. This therapy is still under way in pediatric outpatient clinics.
5. Discussion
The presently reported case shows a clinical picture of systemic arterial hypertension (SAH). At the first sporadic measurement, the patient in this report presented a BP of 160 × 80 mmHg, which remained high at up to 170 × 110 mmHg. At no time did BP reach values lower than 140 × 60 mmHg, and this consistently high BP was associated with recurrent headaches for more than one year, at least once a week.
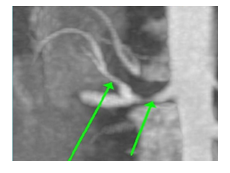
SAH in the pediatric age group, as well as in adults, may have primary or secondary causes. According to the Brazilian Society of Pediatrics, children and adolescents with SAH are usually asymptomatic. Some of them may present headache, irritability, and sleep disorders. In the present case, the patient's AH was investigated as being due to a secondary cause. These causes are more common in children and adolescents, and their leading agents are renal diseases (39%–74%) and renovascular diseases (12%–13%). However, during hospitalization, the patient started complaining of arthralgia in the knees, without signs of inflammation or effusion of the joints. Considering this patient’s clinical picture, it was chosen to perform a CTA of the abdomen and pelvis, which evidenced a 70%–80% stenosis in the right renal artery, 0.5 cm from its emergence and for a length of 0.3 cm. Downstream of this stenosis, a right upper polar renal artery emerged, and it also had a 50%–60% stenosis (Figure 1).
Figure 1: Angiotomografy of the abdomen and pelvis. Stenosis between 70-80%, for an extension of 0.3 cm in the right renal artery, 0.5 cm from its emergence. After stenosis, there is an emergence of a right upper polar renal artery, which also presents a stenosis between 50-60%. Consider possibility of vasculitis of medium-caliber vessels.
To clarify the diagnosis, an echocardiography examination was performed, and it showed no evidence of aortic coarctation. The same examination did show slight left ventricular hypertrophy, a 55% ejection fraction, and a slight increase in myocardial thickness, and electrocardiography evidenced left ventricular overload. As explained above, considering the clinical picture, it was chosen to investigate the differential diagnosis of Takayasu's arteritis. This is a type of primary, chronic systemic vasculitis, classified as a granulomatous vasculitis, with a predominance of large-caliber vessel involvement. It affects predominantly the thoracic and abdominal aorta (60% to 90% of cases) and their main branches. Sometimes, it also affects the renal, subclavian, carotid, and pulmonary arteries, causing segmental stenosis, occlusion, thrombosis, dilatation, and aneurysms in the vessels involved.
A diagnosis of Takayasu's arteritis is only established as set forth in the 2008 diagnostic criteria by the European Alliance of Associations for Rheumatology (EULAR), the Paediatric Rheumatology International Trials Organisation (PRINTO), and the Paediatric Rheumatology European Association (PRES). The mandatory EULAR/PRINTO/PRES criterion is an angiography of the aorta and its main branches or of the pulmonary arteries showing an aneurysm, dilatation, stenosis, occlusion, or thickening of the vessel wall, while discarding other possibilities. Additionally, at least one of the following minor criteria must be present: pulse deficit or claudication; BP discrepancy in any of the four limbs; cardiac or arterial murmurs, systemic arterial hypertension; and acute-phase laboratory reactions (erythrocyte sedimentation rate > 20 mm or C-reactive protein above the reference value). However, the patient in the current report presented arterial hypertension, a slight cardiac murmur, and an abdominal CTA showing a stenosis of the right renal artery.
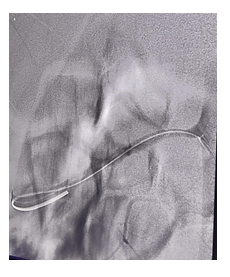
Renovascular hypertension due to renal artery involvement may be refractory to medical treatment and is recognized as an important prognostic factor and a cause of premature death. Although renal artery revascularization surgery shows long-term effectiveness, endovascular treatment should be preferred as an initial approach. In the present case, it was chosen to perform a dilatation of the right renal artery with a 3.5mm balloon. After the procedure, normal BP levels were obtained with satisfactory blood flow through the right artery (Figure 2).
Based on scientific evidence and considering the importance of an early start of treatment for the prognosis of Takayasu's arteritis, methotrexate 15mg/m² once a week was prescribed. Corticosteroids should be started early as first-line drugs, either orally or in the form of intravenous pulse therapy, although there is no sustained response with their use alone. The relevance of the treatment must be emphasized, as Takayasu’s arteritis is a disease with high morbidity and mortality.
6. Conclusion
An early and adequate clinical conduct provided to pediatric patients diagnosed with arterial hypertension causes an impact in reducing morbidity and mortality, and in maximizing the chances of recovery. Identifying the cause of hypertension in pediatric care is extremely important, and according to the literature, the measurement of blood pressure in children and adolescents should become routine in daily practice. It is one of the measures of basic health care and may be useful in preventing complications in the early phase of life.
References
- Göknar N, Çaliskan S. New guidelines for the diagnosis, evaluation and treatment of pediatric hypertension. Turk Pediatri ARS 55 (2020): 11-222.
- Luber E, Agabiti-Rosei E, Cruickshank JK, et al. European Society of Hypertension Guidelines for the management of high blood pressure in children and adolescents. J Hypertens 34 (2016): 1887-1920.
- Flynn JT, Kaelber DC, Baker-Smith CM, et al. Subcommittee on Screening and Management of High Blood Pressure in Children. Clinical Practice Guideline for Screening and Management of High Blood Pressure in Children and Adolescents. Pediatrics 140 (2017): e20171904.
- Bresolin NL, Sylvestre LC, Kaufman A, et al. Hipertensão arterial na infância e adolescência. Manual de orientação da Sociedade Brasileira de Pediatria. SBP 2 (2019): 1-25.
- Sak M, Gökçe I, Çiçek N, et al. Renal artery stenosis presenting with resistant hypertension in children and adolescents: A report of five cases. Turk J Nephrol 29 (2020): 242-246.
- Novriyanti MD, Pabuti A, Amelin F. Hypertension due to renal artery stenosis. Jurnal Kesehatan Andalas 8 (2019): 262-267.
- Silva CAA, Hilário MOE, Fonseca AR, et al. Arterite de Takayasu na faixa etária pediátrica: uma causa frequente de hipertensão arterial e redução de pulsos arteriais. Manual de orientação da Sociedade Brasileira de Pediatria. SBP 11 (2019 -2021): 1 -7.
- Kinjo H, Kafa A. The results of treatment in renal artery stenosis due to Takayasu disease: comparison between surgery, angioplasty, and stenting. A monocentrique retrospective study 36 (2015):161-167.


 Impact Factor: * 5.6
Impact Factor: * 5.6 Acceptance Rate: 74.36%
Acceptance Rate: 74.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 