DE-T1 on the Blastocyst obtained Rate and Live Births Rates in Women Receiving IVF-ET Treatment
Hui Shao1, 2*, Yoji Yamaguchi1, Toshiaki Nozaki1, Li Bai1, Xi Dong3, Dongzi Yang4, Shuang Jiao5, Junko Otsuki2, 6, Shoji Kokeguchi2, Masahide Shiotani2
1Department of research, Tokujun Co., Ltd., Hyogo, Japan
2Hanabusa Women’s Clinic, Kobe, Japan
3Zhongshan Hospital, Fudan University, Shanghai, China
4Sun Yat-Sen Memorial Hospital, Sun Yat-Sen University, Guangzhou, China
5China Academy of Chinese Medical Sciences, Beijing, China
6Assisted Reproductive Technology Center, Okayama University, Okayama, Japan
*Corresponding author: Hui Shao, Department of research, Hanabusa Women’s Clinic, Tokujun Co., Ltd., Kobe, Hyogo, Japan
Received: 02 February 2022; Accepted: 09 February 2022; Published: 21 March 2022
Article Information
Citation:
Hui Shao, Yoji Yamaguchi, Toshiaki Nozaki, Li Bai, Xi Dong, Dongzi Yang, Shuang Jiao, Junko Otsuki, Shoji Kokeguchi, Masahide Shiotani. DE-T1 on the Blastocyst obtained Rate and Live Births Rates in Women Receiving IVF-ET Treatment. Journal of Women’s Health and Development 5 (2022): 069-080.
DOI: 10.26502/fjwhd.2644-28840078
View / Download Pdf Share at FacebookAbstract
Background: Our objective was to retrospectively analyze the influence of DE-T1, a type of amino-polysaccharide extracted from dandelions, on the rates of blastocysts obtained and live births in women undergoing IVF-ET treatment.
Methods: This was a retrospective cohort study, conducting a total of 1014 patients over the age of 30, who received IVF treatment at Hanabusa Women’s clinic from Aug. 1, 2012 to Feb. 29, 2020. The patients were divided into two groups, based on their own choice regarding DE-T1 supplementation, which is available as over the counter medicine at the Clinic. The two groups’ overall rates of blastocysts obtained were compared and the rates of blastocysts obtained in patients with different ages and Anti-Mullerian hormone (AMH) levels were also compared using an Intention-to-treat (ITT) analysis. Among the patients who completed embryo transfers (ET), the live birth rate was compared between the supplementation group and the non-supplementation group using a Chi-squared test.
Results: The blastocyst obtained rate in the supplementation group was 75.98%, which was significantly higher than that of 57.28% in the non-supplementation group (P=2.4×10-9). The blastocyst obtained rate across the range of ages in the supplementation group were significantly higher than those of the non-supplementation group (≥30 and <35 years of age: 90.97% vs 74.32%, P=0.001;≥35 and <40 years of age: 82.40% vs 69.79%, P= 0.010; ≥40 and <43 years of age: 72.90% vs 52.11%, P=0.002; ≥43 years of age: 53.29% vs 22.95%, P= 5.7×10-5). The blastocyst obtained rate for both AMH levels in the supplementation group were significantly higher than those of the non-supplementation group (AMH≤1.1: 56.47% vs 40.44%, P=0.002; AMH> 1.1: 88.48% vs 71.08%, P=2.52×10-7). The live birth rate of the supplementation group was significantly higher than that of th
Keywords
<p>DE-T1, Fertility, Blastocyst obtained Rate, Live Birth Rate, AMH</p>
Article Details
1. Introduction
Due to social development, there has been an increase in delayed marriage and childbearing among women. It is well known that women's fertility declines with age [1]. With an increase in infertility among women, assisted reproductive technologies (ARTs) are being used more widely than ever. The assisted reproductive health care industry requires the collection of a large number of mature oocytes, and gonadotropins (Gns) are in common use. Many women of advanced reproductive age and women with poor ovarian functionality suffer from poor ovarian responses, and therefore do not respond adequately to Gns. They cannot produce high quality ovum by means of superovulation treatment, while the cultivation of high quality blastocysts, impre-gnation and childbirth are also out of reach. Consequently, obtaining mature oocytes and the successful cultivation of embryos, especially blast-ocysts, is vitally important to in vitro fertilization and embryo transfer (IVF-ET).
Dandelion (Taraxacum mongolicum Hand.-Mazz.) has been used as a traditional herb by the Chinese and other ancient cultures for centuries. The chemical composition of dandelion has become a hot topic for research in recent years. It has been reported that dandelion polysaccharide has efficacious properties, as an antioxidant, anti-free-radical, in the protection of the liver, for hypoglycemic activity, for promoting growth factor secretion, antitumorigenesis and more [2-6]. DE-T1 is a type of amino-polysaccharide extracted from dandelions. Our previous in vitro studies confirmed that it could promote the growth of granular cells, inhibit the apoptosis of granular cells, and regulate the balance of female hormones [7-8]. Shawkea T-1 (Tokujun Co., Ltd), with the essential component DE-T1, is an assisted reproductive supplement which has been used in Japan for 23 years, and for over 9 years in China.
In this study, we aimed to retrospectively analyze the influences of DE-T1, combined with ovulation stim-ulants, on the blastocyst obtained rate and the live birth rates, to investigate if DE-T1 supplementation would have had an impact on the blastocyst obtained rates and the live birth rates of women receiving IVF-ET treatment. This study was approved by the Institutional Review Board (IRB) of Hanabusa Women’s Clinic (approval number: 2021-09).
2. Materials and Methods
2.1 Study design
This was a retrospective cohort study aiming to investigate the clinical outcome to DE-T1 supple-mentation. Patients were free to choose whether to take DE-T1 oral solution. Patients who chose to purchase and take Shawkea T-1, containing the essential ingredient DE-T1, were assigned to the supplementation group. Patients who chose not to take DE-T1 were assigned to the non-supplemen-tation group. The rates of blastocysts obtained and the live birth rates of both groups were analyzed. The effect modifiers included age and Anti-Mullerian hormone (AMH) value.
2.2 Setting and case recruitment
All infertility patients from China who received IVF treatment at Hanabusa Women's Clinic (Kobe, Japan) for IVF-ET treatment, between Aug. 1, 2012 and Feb. 29, 2020 were subjected for the analyses. They were aged 30 or above. There was no restriction regarding the cause of their infertility, including complaints such as ovarian dysfunction, polycystic ovary syndrome, uterine leiomyoma, adenomyosis, fallopian tube blockage, and basic diseases. Thorough informed consent, in which all patients were informed that their clinical data might be used for future medical research, was obtained from all of the patients. All of the patients agreed to the collection and analysis of their data [9]. Only patients with incomplete general information and patients who conceived naturally during the treatment period were excluded from this study. Patients whose embryos were transported to other institutions or provinces were excluded from the analysis of live birth rates.
2.3 Interventions
The supplementation group took Shawkea T-1 (a brown liquid with a smoky taste, batch number: 6120801011-6200929064, manufactured by Tokujun Co., Ltd, address: 4-2-15 Gokodori, Chuo-ku Kobe city, Hyogo, Japan) containing the essential component DE-T1 (an amino-saccharide extracted from dandelions). Patients aged between 30 and 34 years took 300ml (100ml per bag) daily. Patients aged between 35 and 40 years took 400ml daily. Patients aged over 40 years took 500ml daily. Data regarding DE-T1 administration, including the administration period and the administration dose of each patient in the administration group were obtained by telephone follow-up with medical assistants and the purchase of records provided by Tokujun Co., Ltd. The median (Q25, Q75) duration of administration among the 712 patients in the administration group was 5 (3, 7) months. All treatments and embryo culturing were performed by Hanabusa Women’s Clinic’s team of embryologists and IVF physicians. No fixed course of supple-mentation or treatment was set for the participants of this study. All patients were able to choose whether to have multiple oocyte retrieval and ET cycles during the observation period, in accordance with their individual outcomes in terms of oocyte retrieval, embryo culturing and transplantation. Frozen embryo transplants were conducted for all patients in this study. This reduced both potential research biases as well any disturbance to ovarian stimulation, serum hormone levels, or the endometrial factors involved in fresh embryo cycles by means of artificial endometrial cycle preparation.
2.3.1 Main outcome measures:
- The blastocyst obtained rate for both groups. The proportion of patients who obtained at least one blastocyst by the end of the observation period was calculated for each group. The blastocyst obtained rate = the number of patients who obtained at least one blastocyst at the end of the observation period/the total number of patients in the group × 100%.
- The live birth rates of both groups. The proportion of patients who delivered a liveborn infant at ?28 weeks’ gestation was calculated for each group following the conclusion of their treatment. The live birth rate = the number of patients who delivered a liveborn infant at the end of the observation period/the total number of patients who had embryos transferred in the group × 100%.
2.3.2 Secondary outcome measures:
- The blastocyst obtained rate of different age groups. All patients were divided into the following age groups: ≥30 to <35 years, ≥35 to <40 years, ≥40 to <43 years, and ≥43 years. The blastocyst obtained rate for each age range in the administration group and the control group were compared.
- The blastocyst obtained rate in relation to different AMH values. All patients were grouped according to their AMH levels (AMH≤1.1 and AMH>1.1). The blastocyst obtained rates of patients with these two different AMH values were compared, between the administration group and the control group.
2.4 Statistical methods
Patients who stopped treatment or were lost to follow-up during the observation period were also considered as effective cases in the calculation of outcome statistics and data analysis. Intention-to-treat (ITT) analysis was used in the analysis of the results. Data was analyzed using IBM SPSS Statistics for Windows, Version 23.0 (IBM Co., Armonk, NY, USA). Continuous variables were expressed as mean ± SD, if data was normally distributed. Data not normally distributed was presented using the median (Q25, Q75). Categorical variables were expressed as counts and percentages. Data regarding patients’ age was represented by “mean ± SD”, and an independent sample t test was used to determine statistical significance. Data on patients’ AMH levels was represented by [median (Q25, Q75)], and non-parametric tests were used to determine statistical significance. Frequencies and percentages were used to calculate the blastocyst obtained rate and the live birth rate, and the Chi-square test was used to determine statistical significance. Two-tailed p-values less than 0.05 were considered statistically significant.
3. Results
Data from 1014 Chinese female patients who received IVF-ET treatment at Hanabusa Women’s Clinic was analyzed in this study. 712 patients were assigned to the supplementation group, and 302 patients were assigned to the non-supplementation group. 231 patients completed embryo transfers. Of these, 186 were from the supplementation group, while 45 were from the non-supplementation group. With the exception of those patients who had their embryos transported to other institutions or provinces, there were several main reasons why some patients did not have embryo transfers, as follows: 1) Some patients preferred to gather more embryos at a younger age prior to starting embryo transfers, to thus improve the success rate of ensuing embryo transfers, rather than proceeding to embryo transfer imme-diately upon the conclusion of one stimulation cycle. 2) Some patients opted to take several months to reach optimum physical condition, prior to comm-encing embryo transfer. 3) Some patients failed to produce high quality embryos for transfer. During the observation period from Aug. 1, 2012 to Feb. 29, 2020, a medical assistant followed up on the treatment process by means of monthly telephone calls. There was no significant difference in the baseline characteristics of the participants between the administration and control groups (Table 1).
Figure 1 shows the main flow and results of this study. The blastocyst obtained rate of the supplementation group was significantly higher than that of the control group (P<0.05). Furthermore, the blastocyst obtained rates of the supplementation group of different ages and AMH levels were all significantly higher than those of the non-supplementation group (P<0.05) (Table 2). The live birth rate of the supplementation group was significantly higher than that of the non-supplementation group (P<0.05) (Table 3). Raw data are available as Supplementary Tables 1, 2 and 3.
|
Parameters |
Administration group |
Control group |
P value |
||
|
N |
N |
||||
|
Age (years) (mean ± SD) |
712 |
38.5 ± 4.6 |
302 |
38.2 ± 4.8 |
0.41 |
|
≥30 and <35 |
155 |
32.2 ± 1.4 |
74 |
32.0 ± 1.5 |
0.10 |
|
≥35 and <40 |
250 |
37.0 ± 1.4 |
96 |
36.5 ± 1.4 |
0.16 |
|
≥40 and <43 |
155 |
41.0 ± 0.8 |
71 |
41.0 ± 0.6 |
0.82 |
|
≥43 |
152 |
44.5 ± 1.7 |
61 |
45.0 ± 1.8 |
0.16 |
|
Patients received ET |
186 |
36.1 ± 4.0 |
45 |
36.2 ± 3.9 |
0.84 |
|
AMH (ng/ml) [Median (Q 25, Q75)] |
712 |
1.60 (0.68, 2.92) |
302 |
1.26 (0.50, 2.89) |
0.11 |
|
≤1.1 |
278 |
0.47 (0.20, 0.80) |
136 |
0.41 (0.12, 0.78) |
0.20 |
|
>1.1 |
434 |
2.56 (1.74,3.90) |
166 |
2.64 (1.70,4.42) |
0.58 |
|
Patients received ET |
186 |
2.46 (1.46,4.18) |
45 |
2.50 (1.19,4.87) |
0.91 |
|
Partner’s age (years) (mean ±SD) * |
711 |
41.0 ± 6.9 |
295 |
40.8 ± 7.3 |
0.72 |
|
Stimulation cycle |
1523 |
690 |
|||
|
39.86% |
38.99% |
0.70 |
|||
|
Mild ovarian stimulation |
60.14% |
61.01% |
|||
Note: *,One case in the administration group and 7 cases in the control group lacked their partners’ information
Table 1: Baseline characteristics in administration group and control group.
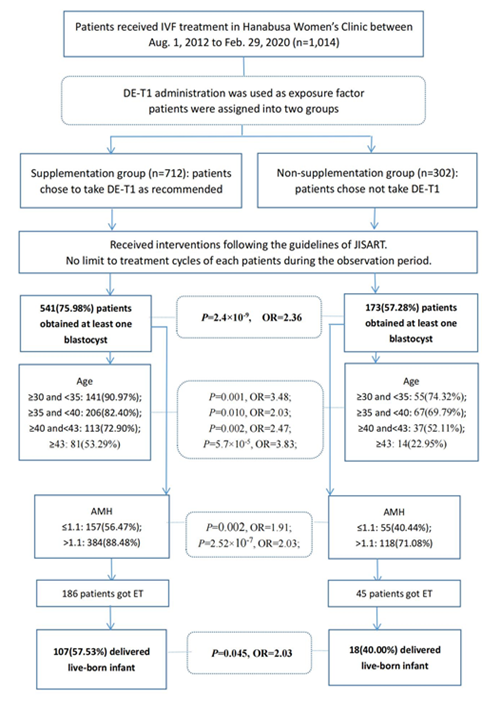
Figure 1: Flow chart and main results of the study.
|
Toal |
Administration group |
Control group |
P -value |
OR |
||
|
N |
Cases obtained Blastocyst (%) |
N |
Cases obtained Blastocyst (%) |
|||
|
712 |
541 (75.98) |
302 |
173 (57.28) |
2.4×10-9 |
2.36 |
|
|
Age (years) |
||||||
|
≥30 to <35 |
155 |
141 (90.97) |
74 |
55 (74.32) |
0.001 |
3.48 |
|
≥35 to <40 |
250 |
206 (82.40) |
96 |
67 (69.79) |
0.010 |
2.03 |
|
≥40 to <43 |
155 |
113 (72.90) |
71 |
37 (52.11) |
0.002 |
2.47 |
|
≥43 |
152 |
81 (53.29) |
61 |
14 (22.95) |
5.7×10-5 |
3.83 |
|
AMHa (ng/ml) |
||||||
|
≤1.1 |
278 |
157 (56.47) |
136 |
55 (40.44) |
0.002 |
1.91 |
|
>1.1 |
434 |
384 (88.48) |
166 |
118 (71.08) |
2.52×10-7 |
3.12 |
Table 2: Comparison of blastocyst obtained rates between the two groups.
|
Group |
N |
Cases delivered live-born infant (%) |
P -value |
OR |
|
Administration group |
186 |
107 (57.53) |
0.045 |
2.03 |
|
Control group |
45 |
18 (40.00) |
Table 3: Comparison of the live birth rate between the two groups.
4. Discussion
4.1 The main outcomes of this study
With the continuous development of ARTs, blastocyst culture has become more widely used. Meta-analysis has shown that when an equal number of embryos are transferred in a fresh IVF cycle, the probability of both live birth and clinical pregnancy is significantly higher if the embryo transfer is performed at the blastocyst stage rather than at the cleavage stage. This has been found to apply particularly to live birth rates [10]. Another unselected patient cohort study also concluded that the cumulative live birth rate per oocyte collection cycle is higher for blastocyst-stage transfers, as compared to cleavage-stage transfers [11]. It was found that IVF outcomes might be improved by performing blastocyst-stage transfers as compared to cleavage-stage transfers. The embryo selection and implantation processes improve with blastocyst stage transfers, while there is a demonstrable decline in multiple gestations [12-16]. Several explanations have been proposed for the superiority of blastocyst-stage transfers in improving implantation rates [13], and the transfer of blastocysts has become the first choice of an increasing number of patients and reproductive medical centers.
In this study, the blastocysts obtained rate for the supplementation group was 75.98%, which was significantly higher than 57.28%, for the non-supplementation group (OR=2.36, P< 0.001). Given that live birth is the ultimate aim of ARTs, and the defining goal of each patient, the live birth rate was used as one of the main outcomes in this study. The live birth rate of the supplementation group was significantly higher than that of the non-supplementation group (P < 0.05). This indicates that DE-T1 could improve not only the outcome for blastocyst culturing, but also the outcome of the pregnancy itself.
4.2 The influences of DE-T1 on patients of differing ages and AMH levels
Studies have shown that the non-separation of meiosis chromosomes increases with age. This, in turn, leads to an increase in aneuploidy and sponta-neous abortion rates in early embryos [17-18]. The most common resulting abnormality has been found to be autosomal trisomy, which is caused by an abnormal arrangement of the chromosomes and the composition of the spindle matrix during meiosis in elderly female oocytes [18]. A 2013 study concluded that both the aneuploid rate and the no-euploid embryo rate rose in a mathematically predictable way with age [1].
In this study, we enrolled patients from 30 to 46 years of age. Considering the influence of age and AMH on blastocyst formation in IVF treatment, we further observed the influence of DE-T1 on patients of different age groups (≥30 to <35 years; ≥35 to <40 years; ≥40 to <43 years of age and ≥43 years of age), and different AMH levels (AMH ≤ 1.1ng/ml and AMH > 1.1ng/ml). Our results showed that the blastocyst obtained rates of the supplementation group with differing ages and AMH levels were all significantly higher than those of the non-supplementation group (P < 0.05). These results suggest that women of differing ages and AMH values could all benefit from DE-T1 supplementation
during IVF treatment.
4.3 The mechanisms of DE-T1 on reproduction health
Follicular dysplasia has long been considered as one of the main causes of infertility. The causes of follicular dysplasia infertility are various. Congenital ovarian dysplasia, premature ovarian failure or ovarian lesions, excessive obesity or wasting, irregu-lar menstruation and heredity, are the common risk factors [19]. A variety of drugs have solved the problem of ovulation disorder in recent years, but this kind of treatment has anti-hormonal influences and can lead to the depletion of estrogen levels [20]. The aforesaid anti-hormonal effects could inhibit endo-metrial DNA synthesis and cause a decrease in endometrial receptivity, while the depletion of estrogen levels could lead to increased cervical viscosity, which is not conducive to sperm passage. Therefore, any long-term use of ovulation promoting drugs tends to lower pregnancy rates and increase early abortion rates [21-22]. The Follicle-Stimulating Hormone (FSH) receptor is the only receptor present in granular cells. Our previous studies have confirmed that DE-T1 could increase the activity of FSH receptors on the surface of ovarian granulosa cells [7].
In this study, DE-T1 supplementation significantly increased the blastocyst obtained rate in women undergoing IVF treatment. We speculate that the mechanism might be related to an increase in the number of follicular granulosa cells and a delay in the death of granulosa cells, as well as a reduction in sinusoidal cell atresia, thus increasing the quantity of mature ovum cells. Growth hormone (GH) is also involved in many processes of human reproduction [23]. In the process of oocyte development, GH could promote the maturity of oocytes and improve the receptor activity of granulosa cells. Further research has [24] found that the effect of GH on reproduction is mainly caused by promoting the secretion of insulin-like growth factor (IGF), which effectively enhances the activity of granulosa cells. It has been reported that dandelion polysaccharide could increase the activity of IGF related receptors [5]. This may also be a contributing factor in the beneficial impact of DE-T1 on reproductive health.
To analyze the process by which DE-T1 improves live birth rates: firstly, DE-T1 significantly increased the blastocyst obtained rate of the patients in the supplementation group. Thus, the patients had more blastocysts available for ET, and therefore more chance of delivering an infant. Secondly, our previous studies have confirmed that DE-T1 can regulate the activity of multiple receptors in the ovaries and uterus, and balance the secretion of female reproductive hormones, which play a key role in ovum growth, embryo implantation, and fetal development [7-8]. In this way DE-T1 improves the quality of ova during IVF treatment and promotes high-quality fertilized embryos. We hypothesize that the improvement of live birth rates by DE-T1 supplementation was achieved through these two functions: increasing the number of blastocysts obtained and improving the quality of those blastocysts.
4.4 Research design and future prospects
With the increasing application of evidence-based methods in the field of medical research, randomized controlled trials (RCTs) and cohort studies have been widely used in clinical research. Intervention cohort studies are the main source of evidence for causal association, especially when randomized controlled trials are difficult to carry out due to ethical limitations [25-26]. Considering patients' subjective desires regarding their treatment and patient compli-ance, in addition to the need for long-term follow-ups and complicated interventions, we employed the methods of a retrospective cohort study to observe the influence of DE-T1 on the blastocyst obtained rates and live birth rates of women receiving IVF treatment.
We did not take the quantity of oocytes as an observation indicator for this study. As mentioned above, blastocysts are more valuable than oocytes or early embryos. Blastocysts are also acknowledged to be superior in the prediction of the therapeutic effects of any regimen or protocol under study, and in terms of pregnancy outcomes. Furthermore, as this study was a retrospective cohort study, the related influe-ncing factors, such as the oocyte retrieval cycles and the oocyte retrieval protocols of the two groups, were not completely controlled or consistent for either group. Consequently, using the quantity of oocytes as an indicator would have introduced bias and other challenges in the assessment and interpretation of the research outcomes. In this study, we retrieved 4,155 oocytes from 712 patients in the supplementation group, over the course of 1,523 ovarian stimulation cycles, with an average of 2.72 oocytes obtained per cycle. For the non-supplementation group, 1,746 oocytes were collected from 302 patients over 690 cycles, with an average of 2.53 oocytes obtained per cycle. This evidence was in line with our more long-term clinical observations, suggesting that DE-T1 could improve both the quality and quantity of oocytes. Patients who struggled to attain successful oocyte retrieval and blastocyst culturing generally resorted to several cycles of oocyte retrieval, rend-ering their courses of treatment relatively long. We aim to explore optimal courses of supplementation for patients of differing ages and AMH values in the future, to enable us to prescribe individualized supplementation protocols for each patient.
In this study, we observed 1014 cases over an observation period of approximately 8 years. The supplementation group underwent a total of 1523 stimulation cycles. Using real-world research methodologies, we didn’t set any strict inclusion criteria for the participants. In consequence we suggest that the results of this study may more truly reflect the influence of DE-T1 on women with different ages and AMH values who receive IVF-ET treatment. Reproduction is a complex physiological process. The mechanisms by which DE-T1 achieves its multitarget, synergistic influences on the hypothalamus, pituitary glands, ovaries, uterus and other organs requires further study.
5. Conclusions
A retrospective cohort study was conducted to explore the influences of DE-T1 on blastocyst obtained rates and live birth rates of women receiving IVF treatment. Our results showed that DE-T1 could significantly increase both the blastocyst obtained rate and the live birth rate, and furthermore, that women of differing ages and AMH values could all benefit from DE-T1 supplementation.
Declarations
Ethics approval and consent to participate
This study was approved by the Institutional Review Board (IRB) of Hanabusa Women’s Clinic (approval number: 2021-09). Thorough informed consent, in which all patients were informed that their clinical data might be used for future medical research, was obtained from all of the patients. All of the patients agreed to the collection and analysis of their data. All the methods were performed in accordance with relevant guidelines and regulations.
Statement
All the authors confirmed that all methods were performed in accordance with the relevant guidelines and regulations in this research.
Consent for publication
Not applicable
Availability of data and materials
All data generated or analysed during this study are included in this published article and its supplementary information file.
Competing interests
The authors declare that they have no competing interest.
Funding
No funding was obtained for this study.
Authors' contributions
H.S. is the corresponding author and primarily responsible for writing and editing the manuscript. H.S and S. J. wrote the main manuscript text and S. J performed the statistical analyses. Y.Y., T.N. and L.B contributed with data acquisition and reviewing the manuscript text. X.D., D.Y., J.O., S.K., and M.S. contributed with reviews and revisions of the manuscript text. All authors read and approved the final version of the manuscript.
Acknowledgements
We thank all the women who participated in this study.
Supplementary
Here, is the list of supplementary files. Click to download.
References
- Jason M Franasiak, Eric J Forman, Kathleen H Hong, et al. The nature of aneuploidy with increasing age of the female partner: a review of 15,169 consecutive trophectoderm biopsies evaluated with comprehensive chromosomal screening. Fertil Steril 101 (2014): 656-663.
- Yong-Shen Ren, Yao Zheng, Huan Duan, et al. Dandelion polyphenols protect against acetaminophen-induced hepatotoxicity in mice via activation of the Nrf-2/HO-1 pathway and inhibition of the JNK signaling pathway. Chin J Nat Med 8 (2020): 103-113.
- Libo Wang, Tengfei Li, Fangcheng Liu, et al. Ultrasonic-assisted enzymatic extraction and characterization of polysaccharides from dandelion (Taraxacum officinale) leaves. Affiliations expandInt J Biol Macromol 126 (2019): 846-856.
- Liu Q, Zhao H, Gao Y, et al. Effects of Dandelion Extract on the proliferation of rat skeletal muscle cells and the inhibition of a lipopolysaccharide-induced inflammatory reaction. Chin Med J (Engl) 131 (2018): 1724-1731.
- Feng Ren, Kaixuan Wu, Yun Yang, et al. Dandelion polysaccharide exerts anti-angio-genesis effect on hepatocellular carcinoma by regulating VEGF/HIF-1α expression. Front Pharmacol 11 (2020): 460.
- Huijing Guo, Weida Zhang, Ying Jiang, et al. Physicochemical, structural, and biological properties of polysaccharides from dandelion.Molecules 24 (2019): 1485.
- Tong Wang, Bing Xue, Hui Shao, et al. Effect of Dandelion extracts on the proli-feration of ovarian granulosa cells and expression of hormone receptors. Chin Med J (Engl) 131 (2018): 1694-1701.
- Xu Zhi, Ken-Ichi Honda, Koji Ozaki, et al. Dandelion T-1 extract up-regulates reprod-uctive hormone receptor expression in mice. Inter J Molecu med 20 (2007): 287-292.
- Christine Grady, Lisa Eckstein, Ben Berk-man, et al. Broad Consent for Research With Biological Samples: Workshop Conclusions. Am J Bioeth 15 (2015): 34-42.
- Amer SA, Smith J, Mahran A, et al. Double-blind randomized controlled trial of letrozole versus clomiphene citrate in subfertile women with polycystic ovarian syndrome. Hum Reprod 32 (2017): 1631-1638.
- Evangelos G Papanikolaou, Efstratios M Kolibianakis, Herman Tournaye, et al. Live birth rates after transfer of equal number of blastocysts or cleavage-stage embryos in IVF. A systematic review and meta-analysis. Hum Reprod 23 (2008): 91-99.
- De Croo I, Colman R, De Sutter P, et al. Blastocyst transfer for all? Higher cumulative live birth chance in a blastocyst-stage transfer policy compared to a cleavage-stage transfer policy. Facts Views Vis Obgyn 11 (2019): 169-176.
- Bruce S Shapiro, Kevin S Richter, Dee C Harris, et al. Implantation and pregnancy rates are higher for oocyte donor cycles after blastocyst-stage embryo transfer. Fertil Steril 77 (2002): 1296-1297.
- Reh A, Fino E, Krey L, et al. Optimizing ermryo selection with day 5 transfer. Fertil Steril 93 (2010): 609-615.
- Zander-Fox DL, Tremellen K, Lane M. Single blastocyst embryo transfer maintains comparable pregnancy rates to double cleavage-stage embryo transfer but results in healthier pregnancy outcomes. Aust NZJ Obstet Gynaecol 51 (2011): 406-410.
- Evangelos G Papanikolaou, Efstratios M Kolibianakis, Herman Tournaye, et al. Live birth rates after transfer of equal number of blastocyst or cleavage stage embryos in IVF. A systematic review and meta-analysis. Hum Reprod 23 (2008): 91-99.
- Fragility E, Wells D. Aneuploidy in the human blastocys. Cytogenet Genome Res 133 (2011): 149-159.
- Jie Qiao, Zhen-Bo Wang, Huai-Liang Feng, et al. The root of reduced fertility in aged women and possible therapeutic options: current status and future prospects. Mol Aspects Med 38 (2014): 54-85.
- Franck Pellestor, Brigitte Andréo, Françoise Arnal, et al. Maternal aging and chromosomal abnormalities: new data drawn from in vitro unfertilized human oocytes. Hum Genet 112 (2003): 195-203.
- Gadalla M A, Huang S, Wang R, et al. Effect of clomiphene citrate on endometrial thick-ness, ovulation, pregnancy and live birth in anovulatory women: systematic review and meta-analysis. Ultrasound Obstet Gynecol 51 (2018): 64-76.
- Amer SA, Smith J, Mahran A, et al. Double-blind randomized controlled trial of letrozole versus clomiphene citrate in subfertile women with polycystic ovarian syndrome. Hum Reprod 32 (2017): 1631-1638.
- Osamah Batiha, Nour Alhoda Alahmad, Amer Sindiani, et al. Genetics of female infertility: molecular study of newborn ovary homeobox gene in poor ovarian responders. J Hum Reprod Sci 12 (2019): 85-91.
- Magalhães-Padilha D M, Duarte A B G, Araújo V R, et al. Steady-state level of insulin-like growth factor-I (IGF-I) receptor mRNA and the effect of IGF-I on the in vitro culture of caprine preantral follicles. Theriogenology 77 (2012): 206-213.
- Ipsa E, Cruzat VF, Kagize JN, et al. Growth hormone and insulin-like growth factor action in reproductive tissues. Front Endocrinol (Lausanne) 10 (2019): 777.
- BENSON K, HARTZ AJ. A comparison of treatmental studies and randomized, controlled trials. N Engl J Med 342 (2000): 1878-1886.
- Horwitz HR I, Viscoli CM, Clemens JD, et al. Developing improved treatmental methods for evaluating therapeutic effectiveness. Am J Med 89 (1990): 630-638.


 Impact Factor: * 3.4
Impact Factor: * 3.4 Acceptance Rate: 78.89%
Acceptance Rate: 78.89%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 