Diode Laser in the management of Oral Sub-mucous Fibrosis: A Case Report
Vaishali Jamdade*, 1, Anshuman Jamdade2, Amrita Agarwal3, Nilesh D Pardhe4
1Senior Lecturer, Department of Oral and Maxillofacial Surgery, Mahatma Gandhi Dental College and Hospital, Jaipur
2Professor and Head, Department of Oral Medicine and Radiology, Mahatma Gandhi Dental College and Hospital, Jaipur
3Senior Lecturer, Department of Oral Medicine and Radiology, Mahatma Gandhi Dental College and Hospital, Jaipur
4Independent Researcher in Dentistry, Former Head - Dept of Oral & Maxillofacial Pathology, Mahatma Gandhi Dental College and Hospital, Jaipur
*Corresponding author: Nilesh D Pardhe, Former Professor & Head of Department, Oral & Maxillofacial Pathology, Mahatma Gandhi Dental College, Jaipur, India.
Received: 11 October 2021; Accepted: 19 October 2021; Published: 26 October 2021
Article Information
Citation: Vaishali Jamdade, Anshuman Jamdade, Amrita Agarwal, Nilesh D Pardhe. Chondrosarcoma of the Posterior Mandible: A Case Report. International Journal of Applied Biology and Pharmaceutical Technology 12 (2021): 415-419.
View / Download Pdf Share at FacebookAbstract
Etiology of oral submucous fibrosis (OSMF) is not fully understood, henceforth treated unsatisfactorily. Generally surgical treatment aims to reopen mouth. Surgery includes relieving fibrous bands followed by grafting to prevent re-fibrosis. Different surgical techniques are used to improve the condition of the patient. Each technique has its own advantage and disadvantages. Lasers application in OSMF is not much studied. In our case, laser (Diode) fibrotomy had an excellent result with satisfactory mouth opening and no recurrence until the last follow up.
Keywords
<p>Oral submucous fibrosis, Diode Laser, Laser Surgery, Fibrotomy</p>
Article Details
1. Introduction
Oral submucous fibrosis (OSMF) is defined as “An insidious chronic disease affecting any part of the oral cavity and sometimes the pharynx. It is always associated with juxta-epithelial inflammatory reaction followed by fibroelastic changes of the lamina propria with epithelial atrophy leading to stiffness of the oral mucosa and causing trismus and inability to speak”[1].
OSMF is a pre-malignant condition with high risk of malignant transformation, particularly oral squamous cell carcinoma. OSMF is more prevalent in Indian sub-continent.
Various treatment modalities like medical, surgical and physical therapy either single or in combination are used. Each technique has its own limitations. Surgical treatment includes incising and relieving fibrous bands and reconstruction of defects using local or distant skin or oral mucosal grafts or muscular flaps like temporalis or temporalis fascia transferor buccal fat pad. Studies on lasers in the management of OSMF are very limited.
The purpose of this paper is the use of Diode laser in the treatment of OSMF in order to find out its merits and demerits.
2. Case report
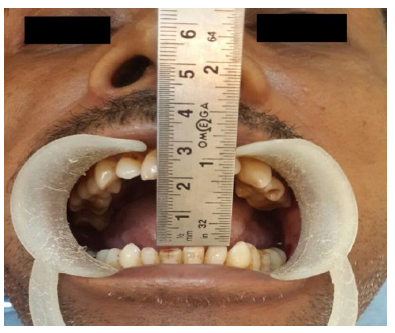
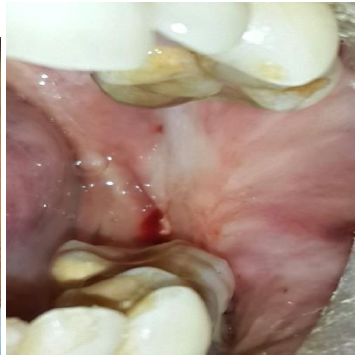
A 42 year old male reported with progressive painless reduction in mouth opening since last two year. Patient had history of gutkha (mixture of areca nut, tobacco and slaked lime) chewing habit for about 10 years. Mouth opening (Inter-incisal distance) was less than two centimeter (Fig. 1). Mucosal blanching and fibrotic bands were palpated prominently in left buccal mucosa (Fig. 2). Patient was diagnosed as having grade III OSMF according to Khanna et al [2].Patient was informed about the risk associated with the condition. Laser fibrotomy using Diode laser in left buccal mucosa was planned under local anesthesia.
3. Laser Surgical Technique
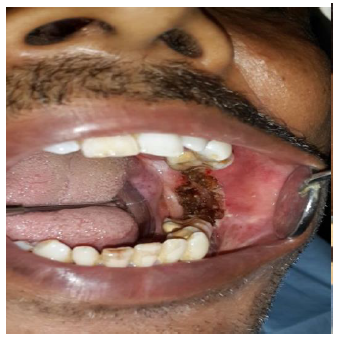
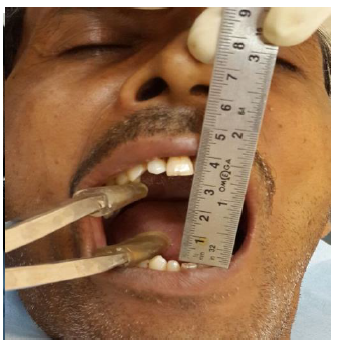
2% lignocaine with adrenaline 1: 80000 dilution infiltrated all over posterior and middle part of left buccal mucosa. First, the buccal mucosa was incised transversely fromedges of retromolar triangle anterirolyalong the occlusal plane using 1 watt power with intermittent contact mode for sharp incision. Laser tip introduced through open mucosa and then laser machine started to cut fibrous bands in order to prevent epithelial collateral damage. Fibrotomy was carried out depending upon the spread using 3 watt with continuous contact mode (Fig. 3). Simultaneously, Heister’sjaw opener was used for separating cut bands to open the mouth. Interincisal distance of 3.4 cm was achieved immediately after release of bands (Fig. 4).
Patient was advised for mouth opening exercises (using wooden sticks) from the 1st post-operative daywith frequency of 4-5 times with duration of half an hour. Patient was advised to increase frequency and duration of exercises and to continue same forminimumof 6-8 months in order to prevent relapse.Patient was recalled after 2, 4 weeks and then after 6 months. Complete epithelial coverage took place after 3 weeks.6 months post-operative inter-incisal distance was 3.2 cm. Elasticity of left buccal mucosa was much improved.
Discussion
No definite treatment has been suggested for OSMF. Blade surgery includes incision and release of bands but has a high recurrence from contracture. Therefore, various surgical grafts have been suggested not only to cover the raw area but to prevent post-surgical contracture.
Tongue flaps are bulky and require an additional surgery for detachment [2], can cause dysphasia, disarticulation and post-operative complications of instability and dehiscence [3]. Palatal flaps have drawbacks of limited donor size and fail to reach posteriorly [4]. Results with skin grafting to cover the denuded areas have been disappointing [5]. Split skin graft showed some degree of relapse due to contracture of the graft [6]. The survival of full thickness skin grafts is questionable [2]. Main limitation of buccal fat pad is its limited size and requires additional coverage for anterior defect. [7, 8]. Buccal fat pad shrink in olders, precluding its use. Nasolabial flaps cannot be extended sufficiently to cover the larger defects; they also cause facial scar, orocutaneous fistula, dehiscence and often hair bearing [5].Its main drawback is an esthetically compromising extra-oral scar [9, 10]. Diode Laser with follow-up physiotherapy is effective to reduce trismus in OSMF; is less expensive, less hospital stay and less follow up as compared to other surgical methods [11, 12]. ErCr: YSGG (Erbium Chromium Yttrium Scandium Gallium Garnet) laser surgery is effective and safe in the treatment of OSMF [13]
Diode laser is a portable hand piece delivers rays through a fiber-optic cable that can reach to relatively inaccessible area. Its cutting depth is less than 0.01 mm, thus controlled cutting is possible without damaging deeper structure. It seals smaller blood and lymphatic vessels, allowing excellent visibility and minimizes the chances of post-operative bleeding and edema.
Laser induced coagulum cover the surface, therefore eliminates the need for grafts. Tissue coagulation acts as dressing, decreases pain and risk of infection. We experienced laser is cause more collateral damage especially of epithelium compared to blade surgery. This may be due to its inherent property of coagulation or of misdirected usage. Therefore, wound healing delayed because of secondary epithelization, takes around 3 to 4 weeks. But fortunately that provide more time for active mouth opening exercise in order to prevent contracture during healing. Studies supporting our observation stated that laser causes 0.5 mm of tissue shrinkage compared to 3 mm with a Bard-Parker blade [14]. In our case, we found 2 mm reduction in mouth opening after 6 months. This could be caused either by secondary healing orre-fibrosis.
Conclusion
Diode laser was safe and effective in managing a grade III OSMF case. However, we need a larger study with long term follow-up especially in advanced cases to evaluate its true efficacy.
Acknowledgement
:None
Conflict of Interest:
None
References
- Pindborg JJ, Sirsat SM. Oral submucous fibrosis. Oral Surg Oral Med Oral Pathol 22 (1966): 764–79.
- Khanna and Andrade NN. “Oral submucous fibrosis”: a new concept in surgical management – Report of 100 cases”. Int J Oral Maxillofac Surg 24 (1995): 433-439.
- Kavarana NM, Bhathena HM. Surgery for severe trismus in submucous fibrosis. Br J Plast Surg 40 (1987): 407–9.
- Lee JT, Cheng LF, Chen PR, Wang CH, Hsu H, Chien SH, Wei FC. Bipaddled radial forearm flap for the reconstruction of bilateral buccal defects in oral submucous fibrosis. International Journal of Oral & Maxillofacial Surgery 36 (2007): 615-619.
- Borle RM, Borle SR. “Management of oral submucous fibrosis: a conservative approach,” Journal of Oral andMaxillofacial Surgery 49 (1991) 788–791.
- Mehrotra D, Pradhan R, and Gupta S, “Retrospective comparison of surgical treatment modalities in 100 patientswith oral submucous fibrosis,” Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology and Endodontology 107 (2009): e1–e10.
- Agarwal D et al. Management of Oral Submucosal Fibrosis with Fibrous Release and Defect coverage with Buccal Pad of Fat and Collagen Sheeth. National Journal of Medical and Dental Research 1 (2012): 14-18.
- Paissat DK: Oral submucous fibrosis. International Journal of Oral Surgery 10 (1981): 307-312.
- Borle RM, Nimonkar PV, Rajan R: Extended nasolabial flaps in the management of oral submucous fibrosis. The British journal of Oral & Maxillofacial Surgery 47 (2009): 382-385.
- Bande CR, Datarkar A, Khare N. Extended nasolabial flap compared with the platysma myocutaneous muscle flap for reconstruction of intraoral defects after release of oral submucous fibrosis: a comparative study. British Journal of Oral and Maxillofacial Surgery 51 (2013): 37-40.
- Talsania JR, Shah UB, Shah AI, Singh NK. Evaluated the efficacy of Laser with follow-up physiotherapy to reduce trismus in OSMF. Indian Journal of Otolaryngology & Head & Neck Surgery 61 (2009): 22-25.
- Babaji H, Anuradha, Nagaraj A, Veena G. Diode Lasers for Oral Submucus Fibrosis – An Experimental Study. J Dent and Med Sci 13 (2014): 04-09.
- Chaudhary Z, Verma M, Tandon S. Treatment of oral submucous fibrosis with ErCr: YSGG laser. Indian J Dent Res 22 (2011).
- Pumphrey DW. Creating the esthetic anterior implant. Lecture presented at Hinman Dental Meeting (2004).


 Impact Factor: * 3.0
Impact Factor: * 3.0 Acceptance Rate: 76.32%
Acceptance Rate: 76.32%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
