Factors Associated with the Type of Cesarean Section and the Risk of Postoperative Complications in Greek Women
Evangelia Antoniou*, Eirini Orovou, Maria Iliadou, Angeliki Sarella, Ermioni Palaska, Antigoni Sarantaki, Georgios Iatrakis, Maria Dagla
Department of Midwifery, University of West Attica, Athens, Greece
*Corresponding author: Evangelia Antoniou, Department of Midwifery, University of West Attica, Athens 12243, Greece
Received: 20 February 2022; Accepted: 04 March 2022; Published: 25 March 2022
Article Information
Citation:
Evangelia Antoniou, Eirini Orovou, Maria Iliadou, Angeliki Sarella, Ermioni Palaska, Antigoni Sarantaki, Georgios Iatrakis, Maria Dagla. Factors Associated with the Type of Cesarean Section and the Risk of Postoperative Complications in Greek Women. Journal of Women’s Health and Development 5 (2022): 081-096.
DOI: 10.26502/fjwhd.2644-28840079
View / Download Pdf Share at FacebookAbstract
Background: Cesarean Section was historically performed to save the lives of mothers and infants. Ηowever, in the past decades, a significant increase in Cesarean Section rates have been observed in Greece and worldwide. The purpose of this research was to investigate the contributing factors to the increase in the Cesarean Section rate (emergency and elective) and postoperative complications.
Methods: A total of births in 6 months (August 2019- February 2020) at the University Hospital of Larisa in Greece was collected. The performed analysis included the available socio-demographic and medical information in the medical records and a socio-demographic and medical questionnaire for women with cesarean deliveries. We also analyzed the importance of the variables in cesarean deliveries compared to vaginal deliveries and postoperative complications.
Results: Out of the total number of the included 633 births, the vaginal delivery rate was 42% (n = 268), and the cesarean delivery rate was 58% (n = 365); Elective Cesarean Section was performed in 36% (n = 230) of the Cesarean Section cases and Emergency Cesarean Section in 22% (n = 135). Women with a previous Cesarean Section and women with in vitro fertilization showed higher percentages for Elective Cesarean Section (46%) compared to women who underwent an Emergency Cesarean Section for the same reasons (42.2%). Besides, a higher percentage of Emergency Cesarean Sections was observed in women living in urban centers (OR = 4.044, p = 0.002) and those diagnosed with stress disorders (OR = 7.048, p = 0.004). Furthermore, Cesarean Section complications were more common among women having undergone Emergency Cesarean Section (OR = 10.357, p < 0.001).
Conclusions: The overall high rates of Cesarean Section in Greece demonstrate the lack of national strategies and prevention mechanisms from iatrogenic interventions and
Keywords
<p>Cesarean Section, Elective Cesarean Section, Emergency Cesarean Section, Risk Factors for Cesarean Sections, Cesarean Section Complications</p>
Article Details
Abbrevations:
CS: Cesarean Section; EMCS: Emergency Cesarean Section; ELCS: Elective Cesarean Section; VBAC: Vaginal Birth after Cesarean; IVF: In Vitro Fertilization; WHO: World Health Organization
1. Background
Cesarean Section (CS) rates have been increasing in recent decades worldwide, and this is a global problem because of the negative effect on maternal and neonatal health [1]. Although CS is a very common surgery, it is associated with an increased risk of hemorrhage, uterine bladder and bowel injury, post-operative sepsis, postoperative ileus [2] and throm-boembolic events [3, 4]. Some studies on neonatal complications have shown that CS is associated with an increased risk for the infant’s obesity, diabetes, respiratory morbidity, and atopic dermatitis in child-hood [5, 6]. Furthermore, women having undergone a CS face an increased risk of placenta previa in a subsequent pregnancy, especially if the second pregnancy occurs within a year after the first CS [7].
Since 1985, the World Health Organization (WHO) has considered that the ideal CS rate ranges from 10–15%. It has also emphasized that a CS rate higher than 10% is not associated with a reduction in maternal-neonatal mortality [8]. In 2009, WHO indicated that both very low and very high CS rates could be dangerous; the ideal CS rate was 5-15% [9]. How-ever, at least 1.4 million cesarean sections were performed in Europe in 2017. In Greece, according to WHO, over half of the deliveries in 2016 were cesarean deliveries, putting Greece among the countries with the highest CS rates [10]. In addition to Greece, CS rates were very high in Cyprus, 54.8%, Romania, 44.1%, Bulgaria, 43.1%, Poland, 39.3%, Hungary, 37.3%, Estonia and Lithuania, (both) 19.4%, France, 19.7% and Finland, 16.5% [11]. Furthermore, there is evidence that there has been an increase in CS rates in middle and high-income countries resulting in the financial burden of health services [12].
The reasons for this phenomenon and the extent of its consequences cannot be explained as a medical necessity. Multiple risk factors are associated with CS deliveries ranging from medical and socio-economic to demographic and institutional factors. Some factors include purported medical as well as non-medical indications, such as maternal characteristics (age and high educational level, high-income level, and social class) maternal request and scientific-technological advances [13, 14]. Another significant factor is a previous CS. It has been observed that a previous CS has become a major driver of increasing total CS rates, due to the increased risk of uterine rupture from the first scar. Attempting a vaginal birth after Cesarean (VBAC) for women having undergone CS is an opportunity to stop this vicious cycle. Of course, this risk increases with the number of previous CS, but after the introduction of the transverse lower incision, this risk decreased [15, 16]. Some other factors are the medical technological advances improving safety in operations [17] and even financial incentives or the physicians’ convenient scheduling, such as CS during weekdays and daylight hours [13, 18]. In addition, an important factor in increasing CS rates is considered to be the high number of gynecologists [19] that results in predominantly medical-orientated health care rather than a friendly and supportive health care based on midwifery practices [20]. In Greece, the estimated CS frequency based on retrospective obstetrical records has been increasing in the past 4 decades, recording a percentage of 13.8% (1977-1983), 17.3% (1984-1988), 22.7% (1989-1993), 29.9% (1994-2000) [21] and the continuing dramatic increase exceeded 50% of all deliveries in 2016 [10]. The aim of this research was to assess the frequency of emergency cesarean section (EMCS) and elective cesarean section (ELCS) deliveries in Greek women, their socio-demographic, medical, obstetrical or psychological factors affecting the type of CS, as well as postoperative complications.
2. Methods
The aim of the study was to analyze the factors that lead to EMCS or ELCS, as well as the factors that lead to postoperative complications in a University Hospital of a large Health region state.
2.1 Study population
This cross-sectional study took place from August 2019 to February 2020 at the maternity unit of the University Hospital of Larisa in Greece. This hospital serves a large health district and is considered representative of Greek hospitals. The total sample size was 633 women who gave birth during the research period, out of whom 365 had undergone a CS delivery (EMCS and ELCS).
2.2 Study design
The data were collected from the women’s medical records, (which are paper-based in Greece) and from a researcher’s questionnaire (with the written consent of the women), following an interview onthe 3rd postpartumday. Socio-demographic and financial data of women and information about the health of the mothers before, during, and after the surgery were collected. More specifically, the medical, gyneco-logical, mental history and the pathology of gestation was recorded, as well as the number of previous births, the type of conception, and the causes that led to EMCS or ELCS and any postoperative complications. The combination of questionnaire and medical record was used to detect information better about the women’s socioeconomic status and health level.
2.3 Statistical analysis
Quantitative variables were presentedas mean values (SD) or as median values (interquartile range = IQR). Qualitative variables areexpressed as absolute and relative frequency. For the comparisons of propor-tions, chi-square and Fisher’s exact tests were used. Logistic regression analyses were applied to explore the factors likely to be related to the type of c-section. Unadjusted and adjusted odds ratios with 95% confidence intervals were computed from the results of the logistic regression analyses. All statistic tests were two-tailed, with a significant set at p < 0.05. All statistical analyses were performed with SPSS 22.0 for Windows (SPSS; Chicago, IL, USA).
3. Results
Of the 633 women who gave birth during the study period, 42% (n = 268) had a vaginal delivery and 58% (n = 365) had undergone a CS, 36% (n = 230) had an ELCS and 22% (n = 135) had an EMCS) (Figure 1).
3.1 Demographic characteristics of participants
365 women who had a cesarean section were recruited and evaluated. As shown in Table 1, 81.9% of the respondents live in urban areas while 18.1% live in rural areas. In terms of age, the mean age was 33 years with a standard deviation of 6.12 years (SD = 6.12). Regarding their family status, the majority of women were married (89.9%), while only 0.8% were single. Concerning their educational level, 41.9% of the participants had completed secondary education and 36.7% higher education. The majority of women were employed either in the public/private sector (31%) or in domestic work (26%). The number of women with a medium financial status amounted to 71.2% whereas only 2.7% of the women had a high financial status. 346 (94.8%) were Orthodox Christians and 340 (93.2%) were Greek. In terms of deliveries, 38.6% of the women already had one child, 17% had two or more children and 44.4% no children. Family status, financial status, educational level, occupation, religion and minority groups showed similarity in the results in both study groups. Women with a planned Cesarean Section were more likely to live in rural areas or had a previous delivery and less likely to be of another nationality than Greek.
3.2 Causes of emergency and elective cesarean sections
Figure 2 shows the rates of emergency Cesarean section and elective Cesarean section as per the causes that provoked a Cesarean section. As the graph shows, women with a previous c-section, early water break and a previous c-section, premature contractions and a previous c-section had opted for an elective Cesarean section at a higher rate (66.1%) compared to women who were forced to have an emergency Cesarean section with the same symptoms (8.9%). Additionally, other reasons that women had chosen an elective Cesarean section and were at a higher rate compared to an emergency Cesarean section belonged to the categories: heavy medical history, short-sightedness, previous gynecological history and mother’s desire, bad experience of previous vaginal delivery, fear of vaginal delivery, lack of cooperation with the mother and women with IVF.
3.3 Factors associated with the type of CS
Univariate logistic regression analyses were initially conducted in order to define possible factors which were associated with the type of c-section. In turn, a multivariate regression analysis was applied in order to clarify whether women would choose to undergo an emergency Cesarean section vs an elective Cesarean section by including variables that were statistically significant (p < 0.05) in univariate regression analysis adding factors associated with type for caesarean delivery (kind of conception), independently of their statistical significance in the univariate analysis. According to the univariate logistic regression models, the factors that were associated with the type of c-section were address, age, nationality, parity, psychiatric history, pathology of gestation, gestational week, full-term labor, causes of c- section and complications after c-section. The multivariate logistic regression analysis showed that women residing in cities (OR = 5.532, p-value = 0.005), had normal conception (OR = 20.679, p-value < 0.001), had been diagnosed with stress disorders (OR = 12.940, p-value = 0.002) or depression (OR = 10.259, p-value = 0.039), had late preterm delivery (OR = 6.957, p-value = 0.050) and had developed complications after c-section (OR = 13.430, p-value = 0.001) were more likely to undergo an emergency Cesarean section. On the contrary, women having one previous birth (OR = 0.274, p-value = 0.050) or more than 2 births (OR = 0.252, p-value = 0.041), had been diagnosed with Oligohydramnios/poly-hydramnios (OR = 0.020, p-value = 0.034) or Placenta previa (type 4)/abruption/bleeding during pregnancy (OR = 0.068, p-value = 0.042) and had a previous Caesarean section and possible complicat-ions (premature rupture of membranes in a previous c-section, premature contractions in a previous c-section) (OR = 0.024, p-value = 0.003) or had previous heavy medical/gynecological history or vision problems (short sightedness) (OR = 0.031, p-value = 0.018) were less likely to undergo an emergency Cesarean section.
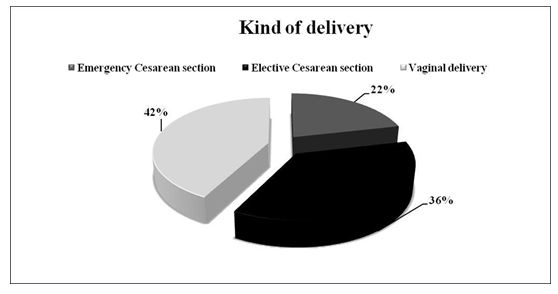
Figure 1: Kind of Delivery.
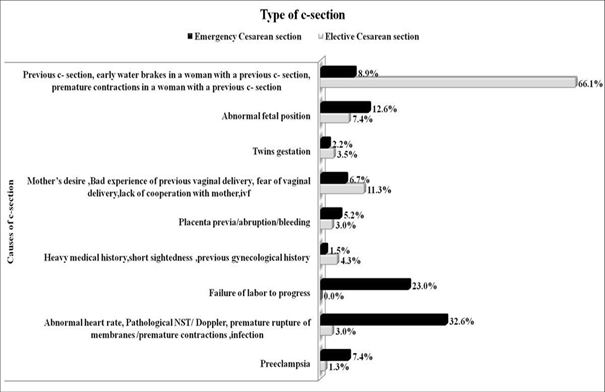
Figure 2: Proportion of causes of Cesarean section according to the type of cesarean section.
|
Total |
Emergency Cesarean section |
Elective Cesarean section |
||||
|
Variables |
N |
% |
N |
% |
N |
% |
|
Address |
||||||
|
City |
299 |
81.9 |
121 |
89.6 |
178 |
77.4 |
|
Village |
66 |
18.1 |
14 |
10.4 |
52 |
22.6 |
|
Age |
||||||
|
Mean (SD) |
33 (6.12) |
32.02 (6.43) |
33.58 (5.85) |
|||
|
Min - Max |
18–48 |
18–48 |
18–45 |
|||
|
Family status |
||||||
|
Single |
3 |
0.8 |
0 |
0 |
3 |
1.4 |
|
In relationship |
28 |
7.7 |
13 |
9.7 |
15 |
6.5 |
|
Married |
328 |
89.9 |
120 |
88.9 |
208 |
90.4 |
|
Divorced |
4 |
1.1 |
1 |
0.7 |
3 |
1.3 |
|
Engaged |
2 |
0.5 |
1 |
0.7 |
1 |
0.4 |
|
Educational level |
||||||
|
Primary school |
28 |
7.7 |
14 |
10.4 |
14 |
6.1 |
|
Junior high school |
23 |
6.3 |
10 |
7.4 |
13 |
5.7 |
|
Senior high school |
153 |
41.9 |
49 |
36.4 |
104 |
45.2 |
|
University |
134 |
36.7 |
50 |
37 |
84 |
36.5 |
|
Msc |
22 |
6 |
11 |
8.1 |
11 |
4.8 |
|
PhD |
5 |
1.4 |
1 |
0.7 |
4 |
1.7 |
|
Occupation |
||||||
|
Public/private sector |
113 |
31 |
43 |
31.9 |
70 |
30.4 |
|
Freelance |
56 |
15.3 |
23 |
17 |
33 |
14.3 |
|
Health care professional |
25 |
6.8 |
8 |
5.9 |
17 |
7.5 |
|
Educators |
32 |
8.8 |
14 |
10.3 |
18 |
7.8 |
|
Household |
95 |
26 |
31 |
23 |
64 |
27.8 |
|
Unemployed |
44 |
12.1 |
16 |
11.9 |
28 |
12.2 |
|
Financial status |
||||||
|
Low |
95 |
26 |
36 |
26.7 |
59 |
25.7 |
|
Middle |
260 |
71.3 |
97 |
71.8 |
163 |
70.8 |
|
High |
10 |
2.7 |
2 |
1.5 |
8 |
3.5 |
|
Religion |
||||||
|
Orthodox Christians |
346 |
94.8 |
124 |
91.9 |
222 |
96.5 |
|
Other |
19 |
5.2 |
11 |
8.1 |
8 |
3.5 |
|
Nationality |
||||||
|
Greek |
340 |
93.2 |
121 |
89.6 |
219 |
95.2 |
|
Other |
25 |
6.8 |
14 |
10.4 |
11 |
4.8 |
|
Minority |
||||||
|
No |
342 |
93.7 |
125 |
92.6 |
217 |
94.3 |
|
Yes |
23 |
6.3 |
10 |
7.4 |
13 |
5.7 |
|
Parity |
||||||
|
None |
162 |
44.4 |
99 |
73.3 |
63 |
27.4 |
|
1 birth |
141 |
38.6 |
24 |
17.8 |
117 |
50.9 |
|
2 and more births |
62 |
17 |
12 |
8.9 |
50 |
21.7 |
Table 1: Demographic characteristics of participants in emergency Cesarean section and in elective Cesarean section.
Table 2: Results of logistic regression model for the factors associated with the type of Cesarean section.
4. Discussion
The subject of the present research was the identi-fication of factors that can lead to EMCS or ELCS in Greek women. Despite the worldwide interest in this topic, this is the first research to have used data froma group of postpartum women to identify and explore factors associated with emergency or elective Cesa-rean deliveries and the complication rate that may occur as a result of the surgery. The data from the major university hospital in Greece revealed an increasing rate of CS deliveries driven by increases in both EMCS and ELCS. In EMCS (the majority of which are primary), more subjectively defined indi-cations were the abnormal heart rate during delivery, failure of labor to progress, abnormal fetal position and preeclampsia, while in ELCS the most common subjective causes were previous CS and the mother’s wish, including fear of vaginal delivery, lack of cooperation during delivery and IVF pregnancies.
More specifically, the results show that for the 6-month period, the CS rate was 58% of total births; 36% ELCS and 22% EMCS (Figure 1). The current study revealed that the key factor affecting the mode of birth is the woman’s place of residence. Although in several studies which investigated the CS socio-demographic factors have shown the maternal age, the educational and the financial level as key factors [22], in this research living in rural areas seems to be a determining factor for ELCS. A possible explanation for this phenomenon could be the obstacles in accessing organized obstetrical health care services for women living in rural areas that creates a sense of insecurity in women and physicians and, therefore, leads to a planned CS delivery, compared to women living in urban areas. The findings show that the increased CS rates are mainly due to a change in the risk profile of the mothers and babies. More speci-fically, although a previous CS does not necessarily mean a scheduled CS in next pregnancy [16, 23], the ELCS rates of our findings were 66.1% for women with a previous CS, while in Germany it is just under 24% [14]. This phenomenon may perhaps be explained by the obstetrician’s increasing fear to avoid the risk of uterine rupture. However, in a paper published by Vandenberg in 2016, the estimated prevalence of uterine rupture in women with a previous CS was 3.6 per 10,000 deliveries [24]. The past gynecological history of women seems to have influenced the obstetricians’ decision for a planned caesarean section, probably due to previous abdomi-nal surgeries; therefore, believing that these women should not attempt a vaginal delivery. In addition, the literature shows that women with a heavy medical history [25] are also more likely to have an ELCS and the findings of our study are in agreement. Further-more, there is no sufficient evidence for ELCS in the relevant literature pertaining to short-sightedness, which was a risk factor for ELCS in this research [26].
In our research, the ELCS rates appear to be affected by the type of conception. Pregnant women after IVF conception show a significant higher rate of ELCS compared to women with the same characteristics who conceive naturally. Precious pregnancies of women with IVF conception, a high risk of placenta accrete [27] and, in some cases, the maternal age [28] constitute factors for ELCS in contrast with women with natural conception. Several studies have shown that women with a history of anxiety disorder or depression, with or without psychiatric treatment, are more likely to be unable to cooperate during delivery or exhibit tokophobia and prefer in some cases ELCS. It has also been shown that in women with tokophobia the first two stages of labour are prolonged by 30% resulting in increased medical interventions and medication, fetal difficulties and EMCS [29], which has been shown to be responsible for a large percentage of postpartum posttraumatic stress disorder [30]. In our study, women with anxiety disorder or depression were more likely to have an EMCS, confirming the above findings and revealing a deficit in perinatal mental health in Greece, due to a deficit in mental health services, lack of health professionals’ appropriate training in addition to the stigma of mental illness which is a deterrent to access appropriate mental health services in Greece [31].
Women with oligohydramnios/hydramnios and placenta previa were more likely to have a scheduled CS, in relation to women who did not face such problems. In a study published in 2013, polyhy-dramnios was associated with increased risk of CS due to suspected fetus macrosomia. Polyhydramnios is also associated with increased rate of maternal diabetes mellitus, fetal genetic syndromes or malfor-mations, premature rupture of membranes, abnormal fetal presentation or cord prolapse and postpartum hemorrhage [32]. For all these reasons, such pregnancies are considered high risk and are usually planned for ELCS in Greece. On the other hand, placenta previa rates have increased and are likely to continue to increase as a result of CS deliveries. The aim of ELCS is to secure the safest route of delivery, to avoid the anticipated risks of bleeding that could occur during vaginal delivery due to the position of the placenta. These complications resulting from the above pregnancy conditions would pose a greater risk compared to a routine ELCS [33].
Another important factor associated with EMCS in this research is low preterm delivery (32–36, 6 weeks). Women who gave birth during these weeks were more likely to undergo an EMCS, especially when there was an underlying pregnancy pathology [34]. In Greece, the meaning of emergency does not really apply because the term EMCS includes cases of relevant medical indications, i.e. a previous CS is a relevant and not an absolute indication such as hemorrhage, preeclampsia, pathological Doppler, leading in most cases again to a Cesarean delivery, while the VBAC is almost not used at all. In general, an individual approach to assessing the urgency for surgery (in 30 min.) must be implemented [35]. In addition to prematurity, EMCS is also associated with a greater likelihood of complications after surgery. CS is a major surgery with high morbidity rates; however, the urgent nature of surgery after obstetric complications (eg, bleeding, preeclampsia, sepsis) seems to be related to postoperative compli-cations. In contrast with our results, a retro-spective study published in 2005 suggests that the risk of postoperative complications in cases of repeated ELCS seems to be higher [36].
5. Conclusion
The present study identified the iatrogenic and non-iatrogenic-based vulnerabilities associated with EMCS or ELCS in Greek women. Furthermore, the existence of postoperative complications and their association with the type of CS have also been identified. The findings show increased EMCS possibility for women living in urban areas, with naturalconception, diagnosed with stress disorders or depression, late preterm delivery and postoperative complications. The identified factors related to ELCS were previous births, previous CS, polyhydramnios/hydramnios dia-gnosis, placenta previa/abruption/bleeding during pregnancy and previous medical/gynecological or visions problem. The high CS rates must be confro-nted with a less interventionist care and a focus on midwifery practice. The goal of reducing primary CS and the possibility of VBAC for women with previous CS are the indicated ways to reduce CS rates in Greece. Both EMCS and ELCS factors are not in all cases related to absolute medical indica-tions. The total CS rates are a combination of increa-sed primary CS rates, as well as a lack of VBAC politics in women with previous CS. Furthermore, health professionals need to understand that a CS decision based on unsupported data by scientific evidence could lead to unnecessary procedures and expose women and infants to unnecessary risks.To understand other factors influencing CS delivery and to design the appropriate interventions, to reduce CS and prevent complications, we recommend further research in this specific area.
Declarations
Ethical approval
The research was approved by:
Availability of data and materials
The dataset analyzed for the current study is available from the corresponding author of reasonable request.
Competing interests
The authors declare that they have no competing interests
Funding
No funding: private or public. The study was completely funded by the authors.
Authors’ contributions
All authors have contributed to the creation of this article. Evangelia Antoniou and Eirini Orovou contri-buted to the collection of the sample; Evangelia Antoniou also contributed to the writing of the article; Georgios Iatrakis; Maria Iliadou; Angeliki Sarella; Ermioni Palaska; Antigoni Sarantaki, Georgios Iatra-kis and Maria Daglacontributed to the design and methodology. Evangelia Antoniou and Eirini Orovou also contributed to the software and formal analysis.
Acknowledgement
We wish to thank the Chief of the Obstetric and Gynecological Department of University Hospital of Larisa, Professor Alexandros Daponte. Also, we express our deep gratitude to the participating postpartum women.
References
- Ayres-De-Campos D, Cruz J, Medeiros-Borges C, et al. Lowered National Cesarean Section Rates after a Concerted Action. Acta Obstet Gynecol Scand 94 (2015): 391-398.
- Field A, Haloob R. Complications of Caesarean Section. Obstet Gynaecol 18 (2016): 265-272.
- Blondon M, Casini A, Hoppe KK, et al. Risks of Venous Thromboembolism After Cesarean Sections: A Meta-Analysis. Chest 150 (2016): 572-596.
- Tsikouras P, Deftereou T, Anthoulaki X, et al. Thrombophilia and Pregnancy: Diagnosis and Management. Embolic Dis - Evol Diagn Manag Approaches (2019).
- Cardwell CR, Stene LC, Joner G, et al. Caesarean Section Is Associated with an Increased Risk of Childhood-Onset Type 1 Diabetes Mellitus: A Meta- Analysis of Observational Studies. Diabetologia 51 (2008): 726-735.
- Magnus MC, Håberg SE, Stigum H, et al. Delivery by Cesarean Section and Early Childhood Respiratory Symptoms and Disorders: The Norwegian Mother and Child Cohort Study. Am J Epidemiol 174 (2011): 1275-1285.
- Getahun D, Oyelese Y, Salihu HM, et al. Previous Cesarean Delivery and Risks of Placenta Previa and Placental Abruption. Obstet Gynecol 107 (2006): 771-778.
- Betran A, Torloni M, Zhang J, et al. WHO Statement on Caesarean Section Rates. Bjog 123 (2016): 667-670.
- Monitoring Emergency Obstetric Care: A Handbook; Bailey, P., Lobis, S., Fortney, J., Maine, D., Family Health International (Organization), Joseph L. Mailman School of Public Health, UNICEF, United Nations Population Fund, World Health Organ-ization, Eds.; World Health Organization: Geneva, Switzerland (2009).
- Greece commits to addressing excessive reliance on caesarean sections. World Health Organization (2016).
- Large differences in share of caesarean births (2020).
- Vassilaki M, Chatzi L, Rasidaki M, et al. Caesarean Deliveries in the Mother-Child (Rhea) Cohort in Crete, Greece: Almost as Frequent as Vaginal Births and Even More Common in First-Time Mothers. Hippo-kratia 18 (2014): 298-305.
- Mossialos E, Allin S, Karras K, et al. An Investigation of Caesarean Sections in Three Greek Hospitals: The Impact of Financial Incentives and Convenience. Eur J Public Health 15 (2005): 288-295.
- Mylonas I, Friese K. Indications for and Risks of Elective Cesarean Section. Dtsch Arzteblatt Int 112 (2015): 489-495.
- Cegolon L, Mastrangelo G, Maso G, et al. Understanding Factors Leading to Primary Cesarean Section and Vaginal Birth After Cesarean Delivery in the Friuli-Venezia Giulia Region (North-Eastern Italy), 2005–2015. Sci Rep 10 (2020): 1-18.
- ACOG Practice Bulletin No. 205: Vaginal Birth After Cesarean Delivery. Obstet Gynecol 133 (2019): e110.
- Bragg F, Cromwell DA, Edozien LC, et al. Variation in Rates of Caesarean Section among English NHS Trusts after Accounting for Maternal and Clinical Risk: Cross Sectional Study. The BMJ (2010).
- Goyert GL, Bottoms SF, Treadwell MC, et al. The Physician Factor in Cesarean Birth Rates. N Engl J Med 320 (1989): 706-709.
- Alran S, Sibony O, Oury J-F, et al. Differences in Management and Results in Term-Delivery in Nine European Referral Hospitals: Descriptive Study. Eur J Obstet Gynecol Reprod Biol 103 (2002): 4-13.
- Wang Z, Sun W, Zhou H. Midwife-Led Care Model for Reducing Caesarean Rate: A Novel Concept for Worldwide Birth Units Where Standard Obstetric Care Still Dominates. J Med Hypotheses Ideas 6 (2012): 28-31.
- Tampakoudis P, Assimakopoulos E, Grim-bizis G, et al. Cesarean Section Rates and Indications in Greece: Data from a 24-Year Period in a Teaching Hospital. Clin Exp Obstet Gynecol 31 (2004): 289-292.
- Alfred Kwesi Manyeh, Alberta Amu, David Etsey Akpakli, et al. Socioeconomic and demographic factors associated with caesa-rean section delivery in Southern Ghana: evidence from INDEPTH Network member site. BMC Pregnancy and Childbirth (2018).
- Bangal VB, Giri PA, Shinde KK, et al. Vaginal Birth after Cesarean Section. North Am J Med Sci 5 (2013): 140-144.
- Vandenberghe G, Blaere MD, Leeuw VV, et al. Nationwide Population- Based Cohort Study of Uterine Rupture in Belgium: Results from the Belgian Obstetric Survei-llance System. BMJ Open 6 (2016): e010415.
- Amjad A, Amjad U, Zakar R, et al. Factors Associated with Caesarean Deliveries among Child-Bearing Women in Pakistan: Secondary Analysis of Data from the Demographic and Health Survey, 2012–13. BMC Pregnancy Childbirth 18 (2018): 113.
- Petrovic O, Prodan M, Loncarek K, et al. Myopia and Delivery: Should Mode of Delivery Be Influenced by Moderate and High Myopia? Gynaecol Perinatol 18 (2009): 13-16.
- Esh-Broder E, Ariel I, Abas-Bashir N, et al. Placenta Accreta Is Associated with IVF Pregnancies: A Retrospective Chart Review. BJOG Int J Obstet Gynaecol 118 (9): 1084-1089.
- Egbe TO, Sandjon G, Ourtchingh C, et al. In-Vitro Fertilization and Spontaneous Pregnancies: Matching Outcomes in Douala, Cameroon. Fertil Res Pract 2 (2016): 1.
- Holka-Pokorska J, Jarema M, Stefanowicz A, et al. Elective Cesarean Section on Psychiatric Indications – the Phenomenon Analysis, Report of Two Cases and Psychiatric Clinical Recommendations. Psychiatr Pol 50 (2016): 357-373.
- Orovou E, Dagla M, Iatrakis G, et al. Correlation between Kind of Cesarean Section and Posttraumatic Stress Disorder in Greek Women. Int J Environ Res Public Health 17 (2020): 1592.
- Tzouvara V, Papadopoulos C. Public Stigma towards Mental Illness in the Greek Culture. J Psychiatr Ment Health Nurs 21 (2014): 931-938.
- Hamza A, Herr D, Solomayer EF, et al. Causes, Diagnosis and Therapy. Geburt-shilfe Frauenheilkd 73 (2013): 1241-1246.
- Early diagnosis key to reducing harm from placental complications (2020).
- Suman V, Luther EE. Preterm Labor. In StatPearls; StatPearls Publishing: Treasure Island (FL) (2020).
- Schauberger CW, Chauhan SP. Emergency Cesarean Section and the 30-Minute Rule: Definitions. Am J Perinatol 26 (2009): 221-226.
- Dimitrova V, Pandeva I, Tsankova M, et al. Post-operative complications following elec-tive and emergency caesarean delivery. Akush Ginekol (Sofiia) 44 (2005): 15-21.


 Impact Factor: * 3.4
Impact Factor: * 3.4 Acceptance Rate: 78.89%
Acceptance Rate: 78.89%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 