Predictors of 30-day Readmission among Ovarian Cancer Patients Undergoing Surgery
Rachel L Budker1, Sarah E Rudasill1, Alexandra L Mardock1, Natsai C Nyakudarika3, Peyman Benharash2, Joshua G Cohen3*
1David Geffen School of Medicine, University of California, Los Angeles, CA, USA
2Cardiovascular Outcomes Research Laboratories (CORELAB), Division of Cardiac Surgery, David Geffen School of Medicine, University of California, Los Angeles, CA, USA
3Division of Gynecologic Oncology, Department of Obstetrics and Gynecology, David Geffen School of Medicine, University of California, Los Angeles, CA, USA
*Corresponding author: Joshua Cohen, Division of Gynecologic Oncology, Department of Obstetrics and Gynecology, David Geffen School of Medicine, University of California, 10833 Le Conte Avenue, UCLA Center for Health Sciences, Room 27-139, Los Angeles, CA 90095, USA, Tel: 310-794-9098; Fax: 310-794-9110
Received: 17 April 2021; Accepted: 27 April 2021; Published: 14 May 2021
Article Information
Citation:
Rachel L Budker, Sarah E Rudasill, Alexandra L Mardock, Natsai C Nyakudarika, Peyman Benharash, Joshua G Cohen. Predictors of 30-day Readmission among Ovarian Cancer Patients Undergoing Surgery. Journal of Women’s Health and Development 4 (2021): 064-077.
DOI: 10.26502/fjwhd.2644-28840061
View / Download Pdf Share at FacebookAbstract
Background: Cytoreductive surgery in ovarian cancer remains a complex and invasive procedure with elevated risks of postoperative complications and readmission. We aimed to characterize the rate and predictors of 30-day readmission in patients undergoing ovarian cancer surgery.
Methods: Women undergoing ovarian cancer surgery between 2010 and 2015 were identified in the Nationwide Readmissions Database (NRD). Baseline demographics and clinical features of patients readmitted within 30 days were analyzed. Multivariable logistic regression analysis was used to identify significant perioperative factors associated with readmission.
Results: Of 94,077 patients undergoing surgery for ovarian malignancy, 12,806 (13.6%) were readmitted within 30 days. The proportion of 30-day readmissions has significantly decreased from 15.2% in 2010 to 12.5% in 2015 (p<.001). Readmitted patients were more likely to have large bowel resection during initial surgery (18.9 vs. 11.5%, p<.001), and experience a postoperative complication, including bowel perforation and infection (11.2 vs. 7.7%, p<.001). The primary reasons for 30-day readmission included postoperative infection (10.6%) and gastrointestinal dysfunction or infection (9.0%). In multivariable analysis, Medicaid (OR 1.18 [95% Confidence Interval 1.04-1.35]), age < 50 years old (OR 1.35 [1.17-1.56]), large (OR 1.35 [1.20-1.51]) or small bowel (OR 1.34 [1.14-1.57]) resection, and discharge to a skilled nursing facility (SNF; OR 1.53 [1.34-1.75]) were significantly associated with 30-day readmission. For readmitted patients, index hospitalization cost was higher ($25,021 vs. $19,587, p<.001) and length of stay (LOS) was longer (8.7 vs 6.4 days, p<.001).
Discussion: Rates of 30-day readmission are declining, however, continued optimization of perioperative pathways for patients at highest risk of readm
Keywords
<p>Ovarian Cancer</p>
Article Details
1. Introduction
Cytoreductive surgery in ovarian cancer remains a complex and invasive procedure with elevated risks of postoperative complications and readmission [1]. Ovarian cancer, most often of epithelial origin, is frequently diagnosed at an advanced stage with disease involving the peritoneal cavity and intra-abdominal structures [2]. 35% of ovarian cancer cytoreductive surgeries necessitate extensive procedures such as bowel resection, diaphragm resection and splenectomy [3]. Given the vast array of possible surgical procedures involved in ovarian cancer debulking, post-surgical care is often complex, with a high rate of post-operative complications and readmissions [4]. Following implementation of the Affordable Care Act, 30-day readmissions became an increasingly important metric assessed both institutionally and nationally through the Hospital Readmissions Reduction Program [5]. While initially utilized to reduce unplanned readmissions in specific conditions such as in congestive heart failure, coronary artery disease, and pneumonia, the metric has been more broadly applied to a range of conditions requiring surgical intervention, including gynecological malignancy. However, the use of 30-day readmissions as a quality indicator amongst patients undergoing surgery for ovarian cancer has been criticized particularly for overemphasizing short-term outcomes which may not be consistent with appropriate care and longer-term outcomes that are more relevant in surgical oncological management [6-8]. Regardless of whether 30-day readmission is a true quality indicator of care at index hospitalization, the metric represents increased hospitalizations, medical costs, and subsequent morbidity and mortality among ovarian cancer patients and thus merits further exploration.
Although the rates of 30-day readmissions following ovarian cancer debulking surgery have been reported, few studies have examined both the preoperative and intraoperative factors that are predictive of readmission in patients undergoing ovarian cancer surgery. In addition, with increasing use of neoadjuvant chemotherapy in management of ovarian cancer, it is unclear what impact this change in practice has had on 30-day readmission rates [9]. Using a large national database, this study sought to examine trends and evaluate risk factors for 30-day readmission patients undergoing cytoreduction for ovarian cancer. By understanding the perioperative characteristics associated with readmission, healthcare systems and providers can better target and implement protocols to reduce the morbidity and costs associated with readmissions.
2. Methods
The Nationwide Readmissions Database (NRD) was evaluated and all adult patients (>18 years) with a diagnosis of ovarian, fallopian tube, or primary peritoneal cancer undergoing surgery involving oophorectomy between 2010 and September 2015 were identified. The NRD was developed for the Healthcare Cost and Utilization Project (HCUP) and is maintained by the Agency for Healthcare Research and Quality (AHRQ). It provides nationally representative data on all hospital readmissions for all types of payers. The NRD sources de-identified patient data from the state inpatient databases and contains weighted data describing 36 million discharges each year [10]. Using International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) codes, the study included patients with a diagnosis of ovarian cancer admitted for surgery. The cohort was stratified based on whether or not patients had been readmitted within 30 days of index hospitalization discharge, with reason for readmission documented per Diagnosis Related Group (DRG) codes. Patient and hospital characteristics, as well as patient comorbidities, were characterized using HCUP and ICD-9 codes. The analysis included NRD data regarding patient demographics (including age, income, insurance coverage, discharge location, and elective vs. nonelective presentation), patient comorbidities (HCUP comorbidities including a variety of acute and chronic diseases), and hospital characteristics (including bed size, urban vs. rural location, and teaching status). Thirty common patient comorbidities were used to calculate the Elixhauser index, a widely utilized marker of the relative morbidity of surgical patients [11]. Additionally, ICD-9 codes were utilized to identify key operative characteristics, including surgical approach (open versus laparoscopic), robotic-assisted procedures, the need for a small or large bowel resection, colostomy or ileostomy, and the need for extracolonic resections, including hysterectomy, lymph node resection, splenic, gastric, liver, bladder, and diaphragmatic resections.
The primary outcome was 30-day readmission. Secondary outcomes included predictors of 30-day readmission, as well in-hospital mortality, length of stay (LOS), total charges, and adjusted costs at both index and readmission hospitalizations. Patient characteristics were analyzed by 30-day readmission status. The Kruskal-Wallis test was utilized for continuous variables to identify differences in demographics, comorbidities, and outcomes by 30-day readmission status, while chi-squared analysis was utilized for categorical variables. The reasons for readmission were documented and analyzed using Diagnosis Related Group (DRG) codes for the episode of re-hospitalization. A chi-square statistic for trend was utilized to analyze the rate of 30-day readmissions across the study period. Patient and hospital characteristics that were significantly different in baseline univariate analysis were then included in a multivariable logistic regression model to assess characteristics that independently predict the likelihood of readmission within 30 days. Statistical significance was considered as p-value <0.05. All statistical analyses were performed using STATA 15.1 (StataCorp LP, College Station, Texas). This study was deemed exempt by the Institutional Review Board at the University of California, Los Angeles.
3. Results
Of 94,077 patients undergoing surgery for ovarian malignancy, 12,806 (13.6%) were readmitted within 30 days. Relative to non-readmitted patients, readmitted patients had a higher Elixhauser comorbidity index (3.71 vs 3.24, p<0.001) and were more likely to have congestive heart failure (CHF) (3.3 vs. 2.4%, p<0.001), diabetes mellitus (13.5 vs. 11.7%, p=0.004), coagulopathy (4.2 vs. 3.1%, p<0.001), and metastatic cancer (13.8 vs. 10.1%, p<0.001). Patients readmitted were more likely to be in the lowest income quartile (23.6 vs 21.7%, p<0.001), covered by Medicare insurance (43.8 vs. 40.5%, p<0.001), and discharged to a skilled nursing facility (11.1 vs. 6.3%, p<0.001) rather than home (65.8 vs. 77.3%, p<0.001) when compared to non-readmitted patients (Table 1).
As shown in Table 1, intraoperative characteristics differed between readmitted and non-readmitted patients. Readmitted patients had higher rates of small bowel resection (6.4 vs. 3.6%, p<0001) and colonic resection (18.9 vs. 11.5%, p<0.001) at index hospitalization. Readmitted patients were also at increased risk of subsequent ileostomy (3.4 vs. 1.2%, p<0.001) or colostomy (3.6 vs. 1.9%, p<0.001). Readmitted patients were more likely to have undergone open procedures (94.0 vs. 92.0%, p<0.001), and less likely to have undergone laparoscopic procedures (6.0 vs. 8.0%, p<0.001) or robotic-assisted procedures (2.6 vs. 4.2%, p<0.001) at index hospitalization. Significant factors associated with 30-day readmission in multivariable analysis are shown in Table 2. Significant demographic factors associated with increased risk of readmission included age less than 50 (OR 1.35 [95% Confidence Interval 1.17-1.56]) and ages 50-69 (OR 1.12 [1.01-1.25] relative to age >70, Medicaid relative to private insurance (OR 1.18 [1.04-1.35]), discharge to a skilled nursing facility (SNF) (OR 1.53 [1.34-1.75]) relative to home, and non-elective surgery relative to elective (OR 1.21 [1.12-1.32]). For every one-point increase in the Elixhauser comorbidity index, patients were 14% more likely to be readmitted (OR 1.14 [1.10-1.17]). Documented metastasis was associated with increased risk of readmission (OR=1.14 [1.02-1.28]), while controlled hypertension was associated with a
decreased risk of readmission (OR=0.87 [0.80-0.95]).
Intraoperative characteristics associated with increased risk of 30-day readmission included both small bowel (OR=1.34 [1.14-1.57]) and colonic (OR 1.35 [1.20-1.51]) resections. Furthermore, diaphragmatic resection (OR=1.32 [1.11-1.55]), splenectomy (OR=1.30 [1.05-1.60]), and ileostomy (OR=1.54 [1.23-1.93]) were also associated with increased 30-day readmission. Patients undergoing lymph node resection (OR=0.91 [0.85-0.97]) were less likely to be readmitted within 30 days. Of note, laparoscopic procedures were not associated with reduced risk of readmission relative to open surgery (OR=0.99 [0.84-1.17]) but robotic-assisted surgery was associated with a reduced risk of readmission (OR=0.77 [0.62-0.96]). As shown in Figure 1, trend analysis of the study period revealed a significant decrease in the rate of 30-day readmission from 2010 to 2015. Patients were readmitted at a rate of 15.2% in 2010, which gradually down-trended to the 30-day readmission rate of 12.5% in 2015 (Figure 1, p<0.001). Among all patients readmitted within 30 days, the primary reason for readmission, as designated by the diagnosis related group (DRG), is displayed in Figure 2. The primary reasons for 30-day readmission included postoperative infection (10.6%), gastrointestinal dysfunction or infection (9.0%), complication of treatment (7.2%), chemotherapy (6.3%), esophagitis/gastritis (5.5%), and gastrointestinal obstruction (5.3%).
All diagnoses with greater than 2.5% of readmitted patients are displayed in Figure 2. The most common reasons for readmission included postoperative infection (10.6%) and gastrointestinal dysfunction or infection (9.0%). The outcomes at the index hospitalization are shown in Table 3. Notably, readmitted patients had higher adjusted costs of index hospitalization ($25,021 vs $19,587, p<0.001) and longer length of stay (8.7 vs. 6.4 days, p<0.001) relative to patients not readmitted. Among non-readmitted patients, the in-hospital mortality rate was 1.1% at index hospitalization. For patients readmitted within 30 days, 3.3% died at the readmission hospitalization. The average adjusted cost of the readmission hospitalization for readmitted patients was $12,963, with an average length of stay of 6.2 days.
|
Variable |
Not Readmitted (N=81,271) |
Readmitted (N=12,806) |
p-value |
|
Age Category (Years) |
|||
|
<50 |
15,233 (18.7%) |
2,416 (18.9%) |
0.85 |
|
50-69 |
43,842 (53.9%) |
6,690 (52.2%) |
0.06 |
|
>70 |
22,196 (27.3%) |
3,700 (28.9%) |
0.047 |
|
Resident of Same State as Hospital |
73,354 (90.3%) |
11,926 (93.1%) |
<0.001 |
|
Income for Patient Zip code |
|||
|
Q1 |
17,597 (21.7%) |
3,025 (23.6%) |
0.009 |
|
Q2 |
20,288 (25.%) |
2,978 (23.3%) |
0.039 |
|
Q3 |
21,208 (26.1%) |
3,220 (25.1%) |
0.20 |
|
Q4 |
22,178 (27.3%) |
3,583 (28.%) |
0.34 |
|
Emergent |
66,534 (81.9%) |
9,791 (76.5%) |
<0.001 |
|
Insurance |
|||
|
Medicare |
32,875 (40.5%) |
5,592 (43.8%) |
<0.001 |
|
Medicaid |
6,165 (7.6%) |
1,195 (9.3%) |
<0.001 |
|
Private |
37,161 (45.7%) |
5,372 (42.0%) |
<0.001 |
|
Other |
5,071 (6.2%) |
646 (5.0%) |
0.022 |
|
Elixhauser Comorbidity Index |
3.24 ± 0.017 |
3.71 ± 0.036 |
<0.001 |
|
Comorbidities |
|||
|
Anemia |
13,714 (17.4%) |
2,580 (20.8%) |
<0.001 |
|
Congestive Heart Failure |
1,862 (2.4%) |
412 (3.3%) |
<0.001 |
|
Chronic Pulmonary Disease |
8,854 (11.2%) |
1,682 (13.6%) |
<0.001 |
|
Coagulopathy |
2,458 (3.1%) |
522 (4.2%) |
<0.001 |
|
Depression |
7,380 (9.4%) |
1,391 (11.2%) |
0.001 |
|
Diabetes |
9,230 (11.7%) |
1,667 (13.5%) |
0.004 |
|
Hypertension |
32,965 (41.8%) |
5,438 (43.9%) |
0.029 |
|
Liver Disease |
1,078 (1.4%) |
250 (2.0%) |
0.002 |
|
Metastatic Cancer |
7,990 (10.1%) |
1,704 (13.8%) |
<0.001 |
|
Obesity |
10,221 (13.0%) |
1,744 (14.1%) |
0.09 |
|
Renal Failure |
2,458 (3.1%) |
488 (3.9%) |
0.006 |
|
Solid Tumor with Metastasis |
2,639 (3.4%) |
391 (3.2%) |
0.51 |
|
Weight Loss |
4,865 (6.2%) |
1,283 (10.4%) |
<0.001 |
|
Surgery* |
|||
|
Open |
73,333 (92.0%) |
11,824 (94.0%) |
<0.001 |
|
Laparoscopic |
6,402 (8.0%) |
750 (6.0%) |
<0.001 |
|
Robotic-Assisted |
3,382 (4.2%) |
323 (2.6%) |
<0.001 |
|
Intraoperative Procedures |
|||
|
Hysterectomy |
61,170 (75.3%) |
9,439 (73.7%) |
0.036 |
|
Small Bowel Resection |
2,893 (3.6%) |
815 (6.4%) |
<0.001 |
|
Colon Resection |
9,355 (11.5%) |
2,420 (18.9%) |
<0.001 |
|
Rectosigmoid Resection |
8,656 (10.7%) |
2,025 (15.8%) |
<0.001 |
|
Liver Resection |
704 (0.9%) |
157 (1.2%) |
0.010 |
|
Bladder Resection |
489 (0.6%) |
129 (1.0%) |
0.001 |
|
Diaphragm Resection |
2,985 (3.7%) |
744 (5.8%) |
<0.001 |
|
Splenectomy |
2,084 (2.6%) |
570 (4.5%) |
<0.001 |
|
Gastric Resection |
574 (0.7%) |
170 (1.3%) |
<0.001 |
|
Lymphadenectomy |
38,716 (47.6%) |
5,389 (42.1%) |
<0.001 |
|
Ileostomy |
1,003 (1.2%) |
430 (3.4%) |
<0.001 |
|
Colostomy |
1,559 (1.9%) |
456 (3.6%) |
<0.001 |
|
Operative Complication |
6,233 (7.7%) |
1,438 (11.2%) |
<0.001 |
|
Hospital Bed Size |
|||
|
Small |
5,098 (6.3%) |
839 (6.5%) |
0.65 |
|
Medium |
15,337 (18.9%) |
2,412 (18.8%) |
0.96 |
|
Large |
60,837 (74.9%) |
9,555 (74.6%) |
0.78 |
|
Hospital Care Setting |
|||
|
Urban Teaching |
65,735 (80.9%) |
10,472 (81.8%) |
0.19 |
|
Urban Non-Teaching |
13,854 (17.0%) |
2,136 (16.7%) |
0.56 |
|
Rural |
1,682 (2.1%) |
198 (1.5%) |
0.027 |
|
Discharge Location |
|||
|
Home |
62,821 (77.3%) |
8,420 (65.8%) |
<0.001 |
|
Short-Term Hospital |
172 (0.2%) |
26 (0.2%) |
0.91 |
|
Skilled Nursing Facility |
5,119 (6.3%) |
1,423 (11.1%) |
<0.001 |
|
Home Health |
12,169 (15.0%) |
2,914 (22.8%) |
<0.001 |
|
Died |
948 (0.1%) |
0 (0%) |
<0.001 |
|
Other |
43 (0.1%) |
24 (0.2%) |
<0.001 |
*A given patient may be included in more than one operative technique category, such as in the setting of conversion from open to laparoscopic surgery
Table 1: Baseline Demographic and Clinical Characteristics of Ovarian Cancer Surgery Patients by 30-Day Readmission Status.
|
Variable |
Odds Ratio |
Standard Error |
P-value |
95% Confidence Interval |
|
Age Category, years |
||||
|
<50 |
1.35 |
0.1 |
<0.001 |
1.17-1.56 |
|
50-69 |
1.12 |
0.06 |
0.04 |
1.01-1.25 |
|
>70 |
reference |
|||
|
Income Quartiles |
||||
|
1st |
1.02 |
0.05 |
0.7 |
0.92-1.12 |
|
2nd |
0.88 |
0.05 |
0.014 |
0.80-0.97 |
|
3rd |
0.92 |
0.04 |
0.1 |
0.84-1.02 |
|
4th |
reference |
|||
|
Insurance Status |
||||
|
Medicare |
1.04 |
0.06 |
0.43 |
0.94-1.16 |
|
Medicaid |
1.18 |
0.08 |
0.01 |
1.04-1.35 |
|
Other |
0.83 |
0.07 |
0.022 |
0.71-0.97 |
|
Private |
reference |
|||
|
Non-Elective Surgery |
1.21 |
0.05 |
<0.001 |
1.12-1.32 |
|
Elixhauser Comorbidity Index |
1.14 |
0.02 |
<0.001 |
1.10-1.17 |
|
Comorbidities |
||||
|
Anemia |
1.05 |
0.05 |
0.29 |
0.96-1.14 |
|
Congestive Heart Failure |
0.93 |
0.1 |
0.52 |
0.75-1.16 |
|
Chronic Lung Disease |
0.99 |
0.06 |
0.9 |
0.89-1.11 |
|
Coagulopathy |
0.94 |
0.08 |
0.47 |
0.80-1.11 |
|
Depression |
0.98 |
0.07 |
0.77 |
0.86-1.12 |
|
Diabetes |
0.96 |
0.06 |
0.51 |
0.85-1.08 |
|
Hypertension |
0.87 |
0.04 |
0.002 |
0.80-0.95 |
|
Metastasis |
1.14 |
0.06 |
0.018 |
1.02-1.28 |
|
Liver Disease |
1.12 |
0.14 |
0.34 |
0.88-1.43 |
|
Renal Failure |
0.91 |
0.08 |
0.31 |
0.76-1.09 |
|
Weight Loss |
1.09 |
0.08 |
0.28 |
0.93-1.26 |
|
Surgery Type |
||||
|
Laparoscopic |
0.99 |
0.08 |
0.92 |
0.84-1.17 |
|
Robotic-Assisted |
0.77 |
0.09 |
0.018 |
0.62-0.96 |
|
Open |
reference |
|||
|
Intraoperative Procedures |
||||
|
Hysterectomy |
0.97 |
0.04 |
0.42 |
0.89-1.05 |
|
Small Bowel Resection |
1.34 |
0.11 |
<0.001 |
1.14-1.57 |
|
Colon Resection |
1.35 |
0.08 |
<0.001 |
1.20-1.51 |
|
Rectosigmoid Resection |
1.02 |
0.06 |
0.77 |
0.91-1.13 |
|
Liver Resection |
0.83 |
0.12 |
0.2 |
0.63-1.10 |
|
Bladder Resection |
1.29 |
0.22 |
0.13 |
0.93-1.80 |
|
Diaphragm Resection |
1.32 |
0.11 |
0.001 |
1.11-1.55 |
|
Splenectomy |
1.3 |
0.14 |
0.015 |
1.05-1.60 |
|
Gastrectomy |
1.28 |
0.26 |
0.22 |
0.86-1.89 |
|
Lymphadenectomy |
0.91 |
0.03 |
0.007 |
0.85-0.97 |
|
Colostomy |
1.05 |
0.11 |
0.62 |
0.86-1.29 |
|
Ileostomy |
1.54 |
0.18 |
<0.001 |
1.23-1.93 |
|
Disposition |
||||
|
Skilled Nursing Facility |
1.53 |
0.11 |
<0.001 |
1.34-1.75 |
|
Home Health |
1.41 |
0.07 |
<0.001 |
1.29-1.55 |
|
Short Term Hospital |
0.8 |
0.26 |
0.5 |
0.43-1.51 |
|
Other |
0.11 |
0.03 |
0 |
0.06-0.20 |
|
Home |
reference |
|||
Table 2: Multivariable Logistic Regression of Perioperative Predictors of 30-Day Readmission.
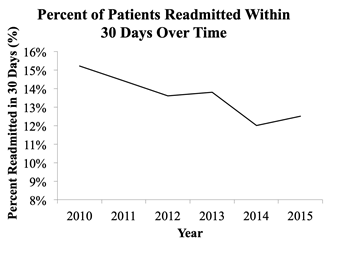
Figure 1: National Trends in 30-Day Readmissions The percent of patients readmitted within 30 days has decreased significantly from 15.2% in 2010 to 12.5% in 2015 (P<0.001).

Figure 2: Readmission Diagnoses.
|
Variable |
Not Readmitted (N=81,271) |
Readmitted (N=12,806) |
P-value |
|
Index Hospitalization |
|||
|
In-Hospital Mortality |
948 (1.1%) |
0 (0%) |
<0.001 |
|
Adjusted Cost (US Dollars) |
$19,587 ± 226 |
$25,021 ± 437 |
<0.001 |
|
Total Charge (US Dollars) |
$69,976 ± 1011 |
$90,001 ± 1787 |
<0.001 |
|
Length of Stay (Days) |
6.4 ± 0.1 |
8.7 ± 0.1 |
<0.001 |
|
Readmission Hospitalization |
|||
|
In-Hospital Mortality |
- |
425 (3.3%) |
- |
|
Adjusted Cost (US Dollars) |
- |
$12,963 ± 329 |
- |
|
Total Charge (US Dollars) |
- |
$46,394 ± 1,234 |
- |
|
Length of Stay (Days) |
- |
6.2 ± 0.1 |
- |
Table 3: Outcomes at Index Hospitalization by 30-Day Readmission Status.
4. Discussion
Given the extensive nature of many cytoreductive surgeries for ovarian cancer, post-surgical care remains complex with a high risk for patient readmissions. We aimed to better understand national trends in 30-day readmission among ovarian cancer patients while further characterizing both preoperative and intraoperative factors associated with 30-day readmission. In this retrospective cohort study, we analyzed 94,077 patients undergoing surgery for ovarian malignancy over a 5-year period using the Nationwide Readmissions Database. We found that rates of 30-day readmission appear to be declining, but younger patients undergoing non-elective surgery for intraoperative bowel, splenic, and diaphragm resections were at high risk of 30-day readmission. Several findings may allow for risk stratification and preoperative pathways to improve patient outcomes.
First, we found that 13.6% of patients undergoing
surgery for ovarian malignancy were readmitted within 30 days. This is consistent with previous institutional and national studies, which have reported readmission rates ranging from 10-19.5% [4, 6, 12-16]. While readmission rates have been well-described in the literature, our updated and large dataset reflects more recent changes in clinical practice and describes national trends rather than institution-specific findings. Importantly, we found that the rate of 30-day readmissions has been significantly decreasing over the 5-year study period (Figure 1). One possible explanation is increased institutional attention to 30-day readmission rates as a metric for hospital quality. In fact, institutions have increasingly adopted an Enhanced Recovery After Surgery (ERAS) protocol, which has been shown to be effective in reducing costs, length of stay and improving quality of care [17]. Possibly, ERAS-related improvement in recovery and functioning at index hospitalization may at least partially explain this trend in decreased admission. As ERAS protocols are by no means standardized, further study of specific ERAS interventions and their effects on 30-day readmission rates is warranted. Another possible reason for decreased readmission rates may be related to increasing use of neoadjuvant chemotherapy with the potential for less radical surgery over time [9, 18], however the effects of these trends on quality of care and long-term outcomes is outside the scope of this study.
Our study demonstrated that patients with more extensive surgery at index hospitalization experienced significantly higher rates of readmission. Particularly, patients undergoing large or small bowel resection during initial surgery were more likely to be readmitted at 30 days (OR 1.35 [1.20-1.51] and OR 1.34 [1.14-1.57], respectively). Given that postoperative GI obstruction and infection remain the primary reasons for readmission in our cohort, these patients appear to be at high risk for bowel-related post-operative complications. These findings are consistent with other studies that have shown that GI complications are amongst the biggest predictors of readmission [4, 7, 14]. Possibly, greater intraoperative resection produces surgical complications necessitating readmission, however patients presenting with disease necessitating bowel resection may have increased 30-day readmission regardless of the quality of surgical intervention due to more advanced disease. Patients who undergo bowel resection as a cohort are at high risk of future readmissions and may benefit from targeted care efforts in the postoperative period including remote monitoring, nurse visits at home, or sooner in-office postoperative exams.
In our multivariable analysis, we found that younger age (<50) was associated with increased risk of readmission compared to older age categories (>70 years old) (OR 1.35 [95% Confidence Interval 1.17-1.56]). Previous studies have found that older patients experience greater morbidity and mortality associated with surgical care of ovarian cancer [21, 22]. Additionally, some studies have found that older patients are less likely to undergo aggressive surgical management for ovarian cancer [23, 24] and more likely to receive neoadjuvant therapy [25, 26]. Younger patients have been shown to have better overall survival when controlling for stage and other clinicopathologic factors [27]. More aggressive surgical intervention for tumor cytoreduction and underlying sociodemographic factors may actually result in higher risk of readmission in this age group. For patients less than 50, further study and possibly additional risk stratification at index hospitalization is warranted. Increasing implementation of robotic-assisted and laparoscopic surgical techniques has further complicated optimal surgical management of ovarian cancer patients. Previous studies have found robotic surgery for ovarian cancer to have lower estimated blood loss, shorter hospitalization, decreased postoperative complication, and improved survival compared with laparotomy [28, 29]. In this study, robotic surgery, but not laparoscopic surgery, was associated with less risk of 30-day readmission relative to open surgery (OR 0.77 [0.62-0.96]) even when controlling for more extensive surgery (i.e. bowel or bladder resection) and patient age, insurance status, and the comorbidities listed in Table 2. This may reflect a patient population with less extensive disease at presentation, thus permitting use of this technique. There are concerns regarding additional costs of robotic surgery, but our study highlights the significant cost and length of stay associated with readmission for ovarian cancer patients. Minimally invasive surgery for advanced stage disease is still under investigation to determine efficacy and safety. The lower number of surgical cases with a robotic approach or use of conventional laparoscopy in this study may explain why conventional laparoscopy and robotic surgery have different 30-day readmission rates. There are also concerns regarding overall survival outcomes for suspected early stage ovarian cancer with a minimally invasive approach [30]. Continued study of the differences in surgical technique and subsequent outcomes is warranted.
Finally, insurance status is associated with increased risk of 30-day readmission. Relative to private insurance, Medicaid insurance was associated with increased likelihood of subsequent 30-day readmission (OR 1.18 [1.04-1.35]). It has been well established that Medicaid patients have worse outcomes in cervical cancer [31], endometrial cancer [32], and ovarian cancer, possibly related to delayed presentation for care, reduced healthcare accessibility, decreased treatment adherence, or a lack of social support [33]. Additional disparities intersect with insurance status and cancer outcomes, including geographic location and access to high volume cancer centers, socioeconomic status, and race [34]. For example, in their analysis of survival in patients with advanced ovarian cancer, Bristow and colleagues demonstrated that patients with Medicaid had lower access to high volume hospitals and physicians which in turn was associated with worse survival [35]. Increased readmission rates in patients with Medicaid is yet another metric by which health disparity in cancer care is made apparent and continues to be an urgent public health problem.
Our study has several inherent limitations. Given the nature of retrospective national database analysis, there is a lack of data regarding ovarian cancer histology, grade and stage of the cancer, the administration of neoadjuvant chemotherapy, operative techniques, residual disease, and postoperative course. Additionally, it is possible that admissions within the 30-day window may be related to administration or adverse effects of chemotherapy. Furthermore, the NRD is only able to track patients within the calendar year and thus cannot assess long-term outcomes. It is also important to note that there may be inherent flaws in the use of 30-day readmission for complex cancer patients. Uppall and colleagues demonstrated that hospitals with increased readmission rates for patients with ovarian cancer actually had higher adherence to cancer treatment guidelines and improved 5-year survival, potentially representing earlier detection and treatment of complications [8]. Nevertheless, 30-day readmission remains an important marker for hospital quality at this time. The retrospective cohort study allows us only to identify trends and associations rather than causal relationships between our perioperative factors of interest. Despite these limitations, our study shows that rates of 30-day readmission remain high among patients receiving surgery for ovarian cancer, but is declining, which is an encouraging finding given increasing efforts to improve recovery after surgery, reduce readmission rates, and lower healthcare costs. Further targeting of patients with complex gynecologic surgical operations including bowel resections is warranted. Further research should focus on continuing to better understand the disparities that patient insurance and discharge location have on subsequent patient readmissions and outcomes in ovarian cancer. Future study is warranted of preoperative and postoperative care pathways that are designed to address the risk factors above to improve quality of care and patient outcomes.
References
- Torre LA, Trabert B, DeSantis CE, et al. Ovarian Cancer Statistics, 2018. CA Cancer J Clin 68 (2018): 284-296.
- Yeung T-L, Leung CS, Yip K-P, et al. Cellular and molecular processes in ovarian cancer metastasis. A Review in the Theme: Cell and Molecular Processes in Cancer Metastasis. Am J Physiol - Cell Physiol 309 (2015): C444-C456.
- Jones NL, Chen L, Chatterjee S, et al. National Trends in Extended Procedures for Ovarian Cancer Debulking Surgery. Int J Gynecol Cancer Off J Int Gynecol Cancer Soc 28 (2018): 19-25.
- Clark RM, Growdon WB, Wiechert A, et al. Patient, treatment and discharge factors associated with hospital readmission within 30days after surgical cytoreduction for epithelial ovarian carcinoma. Gynecol Oncol 130 (2013): 407-410.
- Hospital Readmissions Reduction Program (HRRP) | CMS (2020).
- Barber EL, Rossi EC, Gehrig PA. Surgical readmission and survival in women with ovarian cancer: Are short-term quality metrics incentivizing decreased long-term survival?. Gynecol Oncol 147 (2017): 607-611.
- Barber EL, Doll KM, Gehrig PA. Hospital readmission after ovarian cancer surgery: Are we measuring surgical quality? Gynecol Oncol 146 (2017): 368-372.
- Uppal S, Spencer RJ, Rice LW, et al. Hospital Readmission as a Poor Measure of Quality in Ovarian Cancer Surgery. Obstet Gynecol 132 (2018): 126-136.
- Melamed A, Hinchcliff EM, Clemmer JT, et al. Trends in the use of neoadjuvant chemotherapy for advanced ovarian cancer in the United States. Gynecol Oncol 143 (2016): 236-240.
- The Hcup Nationwide Readmissions Database (NRD), 2015. Agency for Healthcare Research and Quality (2017).
- Elixhauser A, Steiner C, Harris DR, et al. Comorbidity Measures for Use with Administrative Data. Med Care 36 (1998): 8-27.
- Henretta MS, Scalici JM, Engelhard CL, et al. The revolving door: Hospital readmissions of gynecologic oncology patients. Gynecol Oncol 122 (2011): 479-483.
- Eskander RN, Chang J, Ziogas A, et al. Evaluation of 30-Day Hospital Readmission After Surgery for Advanced-Stage Ovarian Cancer in a Medicare Population. J Clin Oncol 32 (2014): 4113-4119.
- Wilbur MB, Mannschreck DB, Angarita AM, et al. Unplanned 30-day hospital readmission as a quality measure in gynecologic oncology. Gynecol Oncol 143 (2016): 604-610.
- AlHilli M, Langstraat C, Tran C, et al. Risk Factors and Indications for 30-Day Readmission After Primary Surgery for Epithelial Ovarian Cancer. Int J Gynecol Cancer Off J Int Gynecol Cancer Soc 25 (2015): 193-202.
- Cham S, Wen T, Friedman A, et al. Fragmentation of postoperative care after surgical management of ovarian cancer at 30 days and 90 days. Am J Obstet Gynecol (2019).
- Ljungqvist O, Scott M, Fearon KC. Enhanced Recovery After Surgery: A Review. JAMA Surg 152 (2017): 292-298.
- Vergote I, Tropé CG, Amant F, et al. Neoadjuvant Chemotherapy or Primary Surgery in Stage IIIC or IV Ovarian Cancer. N Engl J Med 363 (2010): 943-953.
- Andiman SE, Xu X, Boyce JM, et al. Decreased Surgical Site Infection Rate in Hysterectomy: Effect of a Gynecology-Specific Bundle. Obstet Gynecol 131 (2018): 991-999.
- Lippitt MH, Fairbairn MG, Matsuno R, et al. Outcomes Associated With a Five-Point Surgical Site Infection Prevention Bundle in Women Undergoing Surgery for Ovarian Cancer. Obstet Gynecol 130 (2017): 756-764.
- Díaz-Montes TP, Zahurak ML, Giuntoli RL, et al. Surgical care of elderly women with ovarian cancer: A population-based perspective. Gynecol Oncol 99 (2005): 352-357.
- Thrall MM, Goff BA, Symons RG, et al. Thirty-Day Mortality After Primary Cytoreductive Surgery for Advanced Ovarian Cancer in the Elderly. Obstet Gynecol 118 (2011): 537-547.
- Bruchim I, Altaras M, Fishman A. Age Contrasts in Clinical Characteristics and Pattern of Care in Patients with Epithelial Ovarian Cancer. Gynecol Oncol 86 (2002): 274-278.
- Vitale SG, Capriglione S, Zito G, et al. Management of endometrial, ovarian and cervical cancer in the elderly: current approach to a challenging condition. Arch Gynecol Obstet 299 (2019): 299-315.
- Hinchcliff E, Melamed A, Bregar A, et al. Factors associated with delivery of neoadjuvant chemotherapy in women with advanced stage ovarian cancer. Gynecol Oncol 148 (2018): 168-173.
- Rauh-Hain JA, Melamed A, Wright A, et al. Overall Survival Following Neoadjuvant Chemotherapy vs Primary Cytoreductive Surgery in Women With Epithelial Ovarian Cancer: Analysis of the National Cancer Database. JAMA Oncol 3 (2017): 76-82.
- Chan JK, Urban R, Cheung MK, et al. Ovarian cancer in younger vs older women: a population-based analysis. Br J Cancer 95 (2006): 1314-1320.
- Kristensen SE, Mosgaard BJ, Rosendahl M, et al. Robot-assisted surgery in gynecological oncology: current status and controversies on patient benefits, cost and surgeon conditions – a systematic review. Acta Obstet Gynecol Scand 96 (2017): 274-285.
- Shi C, Gao Y, Yang Y, et al. Comparison of efficacy of robotic surgery, laparoscopy, and laparotomy in the treatment of ovarian cancer: a meta-analysis. World J Surg Oncol 17 (2019): 162.
- Matsuo K, Huang Y, Matsuzaki S, et al. Minimally Invasive Surgery and Risk of Capsule Rupture for Women With Early-Stage Ovarian Cancer. JAMA Oncol 6 (2020): 1110-1113.
- Churilla T, Egleston B, Dong Y, et al. Disparities in the management and outcome of cervical cancer in the United States according to health insurance status. Gynecol Oncol 141 (2016): 516-523.
- Fader AN, Habermann EB, Hanson KT, et al. Disparities in treatment and survival for women with endometrial cancer: A contemporary national cancer database registry analysis. Gynecol Oncol 143 (2016): 98-104.
- Goff BA, Matthews BJ, Larson EH, et al. Predictors of comprehensive surgical treatment in patients with ovarian cancer. Cancer 109 (2007): 2031-2042.
- Bristow RE, Powell MA, Al-Hammadi N, et al. Disparities in Ovarian Cancer Care Quality and Survival According to Race and Socioeconomic Status. JNCI J Natl Cancer Inst 105 (2013): 823-832.
- Bristow RE, Chang J, Ziogas A, et al. High-volume ovarian cancer care: Survival impact and disparities in access for advanced-stage disease. Gynecol Oncol 132 (2014): 403-410.


 Impact Factor: * 3.4
Impact Factor: * 3.4 Acceptance Rate: 78.89%
Acceptance Rate: 78.89%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 