Clinical and Imaging Evaluation of Rotator Cuff in Male Elite Water polo Players - A Cross-Sectional Study
Ruberti A1*, Callegari L2, Ronga M3
1Department of Cardiology, University Hospital of Bern, Bern, Switzerland
2Department of Radiology, Ospedale di Circolo e Fondazione Macchi, Varese, Italy
3Department of Orthopedic Surgery and Traumatology, Ospedale di Circolo e Fondazione Macchi, Varese, Italy
*Corresponding Author: Ruberti A, Department of Cardiology, University Hospital of Bern, Bern, Switzerland.
Received: 21 July 2022; Accepted: 08 August 2022; Published: 11 August 2022
Article Information
Citation: Ruberti A, Callegari L, Ronga M. Clinical and Imaging Evaluation of Rotator Cuff in Male Elite Water polo Players - A Cross-Sectional Study. Journal of Orthopedics and Sports Medicine 4 (2022): 217-223.
View / Download Pdf Share at FacebookKeywords
<p>Water polo; Rotator cuff; Ultrasound; Shoulder</p>
Article Details
Abbreviations:
PD: Power Doppler; MRI: Magnetic Resonance Image; NSAIDs: Non-steroidal anti-inflammatory drugs; L.C: Leonardo Callegari (Author 2); M.R: Mario Ronga (Author 3); CIs: Confidence Intervals; SPSS: Statistical Package for the Social Sciences; SD: Standard Deviation; ESMR: European Society of Musculoskeletal Radiology; LHB: Long Head of Biceps
1. Background
Rotator cuff structural changes are conjoint in the overhead throwing athletes [1]. Sport activities, such as baseball, javelin, tennis, volleyball and swimming require the shoulder to rotate at high speeds with the armabducted, increasing the risk for microtraumatic injury [2-7]. Connor et al. [8] found using Magnetic Resonance Imaging (MRI) that 40% of a group of asymptomatic collegiate baseball players and professional tennis players had partial- or full-thickness tears of the rotator cuff in their dominant arm and 0% in their non-dominant arm. Many studies used ultrasound as diagnostic imaging method for evaluating the rotator cuff [1]. The diagnostic accuracy of ultrasound in the evaluation of rotator cuff tears is comparable with MRI and yields a high correlation to arthroscopy, generating sensitivity and specificity up to 95% in hands of experienced practitioners [7,9]. Power Doppler (PD) has been used to analyze the tendon vascularity. As seen in previous study evaluating Achilles and patellar tendon, the occurrence of new vessels has been found to correlate with pain in chronic tendinosis [10-12]. We suppose that also in rotator cuff structures PD could have a predictive value of future pain and activity limitation. Previous authors in a survey of year 2016 reported that elite swimmers currently suffer rotator cuff (96%, 44/46 shoulders, supraspinatus/infraspinatus) and biceps (72%, 33/46 shoulders) tendinopathy [6,13]. Because of the coexistence of swimming, throwing the ball and contacts among players, it is supposed that shoulder injuries are common in water polo players too [13,14]. In literature there are only two papers carried out in high-level water polo players but Galluccio et al. [14] and Jerosh et al. [15] did not find any difference between dominant and non-dominant shoulder. The aim of this study is to evaluate, clinically and with ultrasound, shoulders of asymptomatic high-level water polo players at the beginning of the season. The hypothesis of this study is that in elite water polo athletes there are some structural alterations of rotator cuff tendons due to overuse of the dominant shoulder compared to the non-dominant, identifiable by ultrasound.
2. Methods
The study included asymptomatic elite male water polo athletes from three teams in Lombardy participating at the Italian Premier League and attending without any restriction all trainings, practices, matches. After providing informed consent, each player completed a questionnaire with age, sex, hand dominance, numbers of years of training, training volume, his history of throwing shoulder injury, and demographic data. Exclusion criteria included shoulder injury or pain requiring treatment, systemic musculoskeletal diseases, current use of Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) or steroids and metabolic, rheumatic, osteoarticular or neoplastic diseases. Injury data were then confirmed from the medical record of the team. Our examination was performed before the beginning of the regular season and the study protocol was approved by the institutional review board of our Hospital. Each player received an independent physical examination of both shoulders performed by an orthopaedic shoulder surgeon (M.R.) and completed the Oxford Shoulder Score and Constant Shoulder Score [16]. Players with Oxford Shoulder Score value ≥40 and Constant Shoulder Score value <11 were enrolled. The dominant and non-dominant shoulders were examined by a single musculoskeletal radiologist (L.C.), with 30 years of experience in performing shoulder ultrasound, according to the protocol described by the European Society of Musculoskeletal Radiology [17] using a PHILIPS IU 22 HEALTHCARE Ultrasound System, as described in Figure 1 (A and B). A grayscale ultrasound with 7.5- MHz high resolution linear probe (frequency 350 MHZ) with longitudinal and transverse scans, was performed. The arm of the athlete brought posteriorly, placing the palmar side of the hand on the superior aspect of the iliac wing with the elbow flexed and directed posteriorly. The supraspinatus tendon was evaluated along its long and short-axis. Rotate the arm externally fixing the elbow on the iliac crest to show the subscapularis tendon and its insertion on the lesser tuberosity. The biceps tendon was examined placing the arm in slight external rotation (directed towards the contralateral knee) with the elbow flexed 90°, palm up. Shift the probe up to examine the biceps in its intra-articular course with the bicipital groove and down to reach the myotendinous junction. Moving the probe toward medial on transverse planes, look at the coracoid process, the coraco-acromial ligament, the conjoined tendon and the anterior aspect of the subacromial bursa [17].
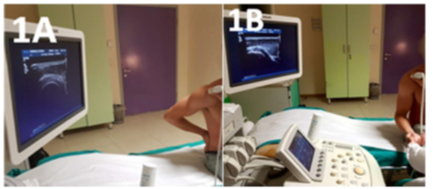
Figure 1: Ultrasonographic technique.
Physicians and the radiologist were blinded to the hand dominance throughout data collection. Supraspinatus, subscapularis and biceps tendons, subacromial bursa were evaluated. The tendons were evaluated for thickness (longitudinal and transversal scans), echotexture (tendinosis graded as 0, 1, 2, 3) and tears (non, partial, full thickness tear), according with the classification used by Rodeo et al. [6] in swimmers. Tendinosis was based on the following criteria: non-homogeneous appearance of the tendon, indistinct tendon margins (fraying), intrasubstance clefts, and cystic degeneration.
Tendon vascularity was graded according to the classification proposed by Chiou et al. [18-20] (Table 1).
|
Grade |
Vascularization Index |
|
0 |
no vessels |
|
1 |
<3 color spots or color lines; MILD intratendon vascularization |
|
2 |
3–6 color spots or color lines; MODERATE intratendon vascularization |
|
3 |
>6 color spots or color lines; MASSIVE intratendon vascularization |
Table 1: Tendon vascularization Power Doppler classification [18-21].
3. Statistical Analysis
Descriptive analysis (means and standard deviation, numbers and percentages) were used to describe the outcome variables of the dominant and no-dominant shoulder. Distribution consistently passed the Shapiro-Wilk normality test (P>.05), so we used parametric statistics. Comparisons between sides were analyzed with a multivariate analysis of variance (MANOVA), in which the within-subjects factor was sides (DO versus NDO). Where appropriate, the differences in frequencies were verified by Chi Square (χ2) test. A Linear Regression model was performed to assess the relationship between structural changes of supraspinatus tendon, subacromialbursa, subscapularis tendon, biceps of the dominant shoulder versus age, career years and playing position. The P<.05 was indicated statistical significance. 95% Confidence Intervals (CIs) were also calculated. All statistical analysis was conducted using SPSS (Statistical Package for the Social Sciences, version 24.0 for Mac; SSPS Inc).
4. Results
Forty athletes completed the questionnaire and were clinically examined. Twenty-three male asymptomatic players followed the inclusion criteria, were included in the study and received the ultrasonographic examination. The mean age was 24.2 ± 3.3 years (range, 19-31): twenty-one outfield players and two goalkeepers, twenty-two right-handed, one left-handed. The athletes reported an average playing background of 13.0 ± 4.4 years (range, 7-22) in competitive water polo (Table 2).
4.1 Ultrasonographic result
Nine (39%) athletes had bilateral degeneration level ≥1 at supraspinatus tendon: six (26%) had only dominant, two (9%) only non-dominant. Fifteen athletes had a degeneration level ≥1 (65%) at the dominant supraspinatus and eleven at the non-dominant (48%). Six athletes had no echo-structural alteration. Fourteen athletes (61%) presented a higher degeneration grade at the dominant tendon compared to the contralateral, four (17%) had a higher degeneration grade at the non-dominant. The other five patients (22%) had no difference between dominant and non-dominant supraspinatus (P<.05). In fifteen players (65%) was observed a higher longitudinal supraspinatus diameters in the dominant compared to the contralateral (P≥.05). Eight (35%) water polo players had supraspinatus partial tear at dominant shoulder, seven (30%) at non dominant. Mean dominant thinning: 1.5 ± 0.6 mm (0.4-2.2 mm); mean non dominant thinning: 1.3 ± 0.7 mm (0.4-2.2 mm) (Figure 2A).
The area of the tendon degeneration was the same in twenty athletes (87%): anterior, lateral, pre insertional. Only in the two goal-keepers and in one outfield player it was different: posterior and medial (P<.05). Power Doppler evidenced neovascularization in five (22%) players at supraspinatus: four bilaterally, one only at the non-dominant (Figure 2B). No neovascularization in all the players at subacromial bursa and subscapularis tendon. One athlete had PD positivity at biceps (Table 2). In six (21%) athletes was found degeneration at the subacromial bursa at the dominant limb, four (17%) at the non-dominant limb, two (9%) bilaterally. Thirteen players (56%) had no structural alteration bilaterally (P≥.05). In seven patients (30%), ultrasound evidenced associated supraspinatus and subacromial bursa damage: four at only the dominant shoulder, three at only the non-dominant (P≥.05).
In seven players (30%) was observed a grade ≥1 subscapularis tendon degeneration at the only dominant limb, two (9%) at the only non-dominant, one (4%) bilateral degeneration (P≥.05) (Table 2). The damage zone was observed near the insertion on the lesser humeral tuberosity (P<.05). In twenty-two athletes (96%) the long head of biceps tendon was damaged: twenty athletes (87%) bilaterally, two (9%) at only the dominant limb (P<.05). Only one patient had no alteration in this structure (Table 2). In all the athletes analyzed the site of alteration was the same: at the bicipital groove in its insertion on the humerus (P< .05). No statistical correlation was found between tendon degeneration and age, career years.
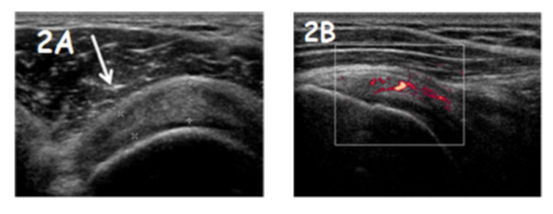
Figure 2: A) Example of supraspinatus partial tear (white arrow). B) Power Doppler at supraspinatus evidenced neovascularization (red spots).
Table 2: Ultrasound examination data results are reported as mean ± SD (range) and numbers/total (percentages). a) Chi-Square (χ2) test (P<.05). b) Multivariate analysis of variance (MANOVA) or Paired T-test. Bolded P values indicate statistically significant difference between dominant and no dominant shoulder (P<.05). c) Linear regression model (P<.05).
5. Discussion
Water polo is a contact sport which also provides a shooting and a swimming phase and this aspect implies a major stress on the shoulder [21]. It is assumed that in elite athletes repeating technical movements induces structural alterations of the stabilizing components of the shoulder, as already observed in studies performed on other overhead athletes [1,6]. Studies have been performed related to the shooting mechanics of the baseball pitchers and the relative injury risk from shoulder overuse [3,6]. The throwing biomechanics in water polo is similar to baseball but there are important differences: the dimensions and weight of the ball, the lack of a solid base during throwing phase. These characteristics influence the angular acceleration of the elbow and cause a decrease of the throwing speed [22].
In literature, there are few data regarding changes of the rotator cuff in water polo [23]. Previous authors have demonstrated that ultrasound and MRI have comparable and high accuracy for detecting full- and partial thickness tears in rotator cuff [24-26]. MRI gives more information about muscle degeneration, the under acromion area and other coexisting pathologic process. We chose ultrasound because it is dynamic, less invasive and more sensitive than MRI in assessment of rotator cuff pre-insetional tendinopathy. Other studies carried out in volleyball, basketball, baseball and swimmers used ultrasound to evaluate the rotator cuff tendinopathy [1,24-27]. The international protocol proposed by European Society of Musculoskeletal Radiology (ESMR) was adopted because considered as the most detailed and effective protocol for analysis and the comparison with other overhead-throwing studies [17].
61% of patients had a higher degeneration of the dominant supraspinatus compared at the non-dominant (P<.05). In the 87% of athletes, the location of the tendon degeneration was anterior, lateral and pre insertional, like in baseball and volley ball players (P<.05). All were outfield players. In the two goal-keepers the degeneration was bilateral, symmetrical and in a different position: posterior and medial.
We suppose that this difference is due to the activities performed by goalkeepers that are not the same of outfield players: the goalkeeper makes rarely high energy shots on goal, but often performs slow passages at variable distance not exceeding 20 meters. During the defensive phases the upper limbs of the goalkeeper are both raised to defend the goal area or move simultaneously underwater, increasing the leg thrust to reach the extreme limits of the goal. In the sessions of swimming, unlike outfield players who practice predominantly freestyle, the goalkeeper performs predominantly butterfly. Like in other studies, no statistically significant difference in tendon diameter was found between dominant and non-dominant supraspinatus [2,28,29]. The more stressed structure in the water polo throwing technique is the supraspinatus tendon, like in other overhead throwing disciplines [1,5,6,8,29]. Nine athletes (39%) had bilateral grade ≥1 supraspinatus degeneration because also non-dominant shoulder is stressed during swimming phases [23]. The statistical analysis evidenced that among the variables studied, structural degeneration is the most influential to define the difference between the tendons of the shoulder. Ocguder et al. [28] evidenced that, in overhead sports, supraspinatus tendon is overloaded, with its bursa. In our study, the supraspinatus alteration is associated with bursa in only 30% of cases and without relevance in dominant or non-dominant arm. Subacromial bursa is low stressed in our study. We suppose that this difference is due to the time when we analyzed the athletes, at the beginning of the season. This difference into overhead disciplines is probably due also to a different shoot dynamic, heavy and measures of the ball, friction with the water, absence of fixed support. This induces a displacement of the vector sum of forces at the level of stabilizing structures of the shoulder, resulting in an increased stress at these levels [22]. The subscapularis tendon is less stressed in overhead sports, like described in other works in this study, therefore we analyzed the tendon echotexture and not the diameter [1,2,4,15,27]. Only eight (35%) of the evaluated athletes had a tendon degeneration ≥1 at the dominant subscaularis. No difference of subscapularis degeneration between the two limbs confirms a predominant involvement of this tendon in swimming and less in the throwing phase [6].
The LHB in the water polo player, unlike what is observed in the other overhead throwing disciplines, is very stressed [4,30]. In the 96% of the cases degeneration has been observed, 91% bilaterally. The area of the degeneration was for every athlete the same, where the tendon goes into the biceps pulley (P<.05). It can be assumed that this tendon is involved especially during the swimming phases, as seen in the study of Rodeo et.al [6] in swimmers, who noted biceps tendinosis in 72% of the analyzed shoulders [6,31]. Previous studies have shown that the severity of the tendon degeneration shoulder would correlate with the number of trainings per week, career years, and the role and of course with any work activity that the athlete engages outside the pool. In this study, as in many others carried out on athletes, ages and years of activity were not influential [32]. Ultrasound examination was completed for each patient with power doppler: previous studies, carried out mainly on Achilles and patellar tendons in marathon runners, footballers and volleyball players, have shown a variation of the local tendon vascularity associated with the increase of activity and have identified a data correlation with risk of injury during the course of the season. PD was defined as a predictive method for future pain and injuries [33-35]. At the beginning of the season PD has shown low percentage of vascularity. Our next goal is to assess new PD evaluation at the end of the season and correlate the vascularity status with symptoms. Our hypothesis is that PD can have a predictive value of shoulder pain also for rotator cuff tendons. Strength points of our study are the careful high level water polo player selection: asymptomatic, no previous surgery or accident, no intra-perirticular infiltration. The ultrasound was performed at the beginning of the season, when tendon stress was low. The radiologist had 30 years of experience in shoulder ultrasound examination. It has been a single-blind evaluation: dominant arm, age, position, career years of the athletes were unknown to the radiologist. The study limits are the low number of chosen athletes: in Lombardy there are three Italian Premier League teams, composed by average 13-15 athletes in each team. The goal-keeper number is very low compared with movement players: a water polo team is composed by fifteen athletes, with only two goal-keepers. Left-handed players number is lower than right-handed: this aspect characterize also daily life. In a water polo team, usually there are one or two left-handed athletes.
6. Conclusion
Our study shows a high prevalence of structural changes in supraspinatus tendon in asymptomatic elite water polo players. Outfield players have peculiar changes in supraspinatus at pre-insertional level, as seen in other overhead throwing athletes. In goal-keepers supraspinatus degeneration is bilateral and located more medially and posteriorly. We found changes also in biceps tendon, bilaterally, like in shoulders of elite swimmers. We suppose that these changes are predictive of shoulder pain. Our perspectives are to follow the athletes, clinically and with ultrasound, to demonstrate our hypothesis and draft more players.
Declarations
Ethics approval and consent to participate
The study design was approved by the Insubria University ethics committee. An informed verbal consent by each athlete to participate to this study was obtained. We took only verbal consent because no invasive intervention was performed and athletes were enrolled with scientific purpose. At the beginning of the enrollment they should complete two clinic selection questionnaires (Oxford Shoulder Score and Constant Shoulder Score) and we considered these as a written consent.
Consent to publish
At the time of enrollment it was clearly specified our scientific objective to publish the manuscript on a sport medical journal. Every athletes enrolled gave his verbal consent. However images in our manuscript are entirely unidentifiable and there are no details of individuals reported.
Availability of data and material
The authors declare that all relevant data are available within the article. All measurements are available in additional file. If necessary, complete collection of ultrasound images is available from the corresponding author upon reasonable request.
Competing interests
The authors declare that there were no competing interests.
Funding
No funding was received in the development of this study, but only passion for a sport associated with passion for our job.
Authors’ contribution:
Author 1: AR (Medical Resident) andrea.ruberti5@gmail.com: enlisted the patients, collected the clinical data, got informed consent, contributed analysis tools, performed the analysis of data with the help of MR and wrote the paper.
Author 2: LC (Musculoskeletal Radiologist): Collected data performing shoulder ultrasound.
Author 3: MR (Orthopedic surgeon): conceived and designed the analysis and helped AR in writing the paper.
All authors have read and approved the manuscript.
Acknowledgements
We thank all the athletes who have agreed to participate in this study.
References
- Malanga G, SK C, Ramirez Del Toro J, et al. Sonographic Evaluation of Supraspinatus Cross-sectional Area in Collegiate Baseball Players. PMR 4 (2012): 488-492.
- Girometti R, De Candia A, Sbuelz M, et al. Supraspinatus tendon US morphology in basketball players: correlation with main pathologic models of secondary impingement syndrome in young overhead athletes. Preliminary report. Radiol Med 111 (2006): 42-52.
- Meister K. Current Concepts Injuries to the Shoulder in the Throwing Athlete Part One: Biomechanics/Pathophysiology/Classification of Injury. Am J Sport Med 28 (2000): 265-275.
- Nadler S, Sherman A, Malanga G. Sport-specific shoulder injuries. Phys Med Rehabil Clin N Am 15 (2004): 607-626.
- Rizio L, Uribe JW. Overuse injuries of the upper extremity in baseball. Clin Sports Med 20 (2001): 453-468.
- Rodeo S, Nguyen J, Cavanaugh J, et al. Clinical and Ultrasonographic Evaluations of the Shoulders of Elite Swimmers. Am J Sports Med 44 (2016): 3214-3221.
- Yablon C, Bedi A, Morag Y, et al. Ultrasonography of the shoulder with arthroscopic correlation. Clin Sports Med 32 (2013): 391-408.
- Connor P, Banks D, Tyson A, et al. Magnetic Resonance Imaging of the Asymptomatic Shoulder of Overhead Athletes A 5-Year Follow-up Study. Am J Sport Med 31 (2003): 724-727.
- Kijowski R, De Smet A. The Role of Ultrasound in the Evaluation of Sports Medicine Injuries of the Upper Extremity. Clin Sports Med 25 (2006): 569-590.
- Boesen M, Boesen A, Koenig M, et al. Ultrasonographic investigation of the Achilles tendon in elite badminton players using color Doppler. Am J Sports Med 34 (2006): 2013-2021.
- Boesen A, Boesen M, Koenig M, et al. Evidence of accumulated stress in Achilles and anterior knee tendons in elite badminton players. Knee Surgery, Sport Traumatol Arthrosc 19 (2011): 30-37.
- Boesen M, Koenig M, Torp-Pedersen S, et al. Tendinopathy and Doppler activity: the vascular response of the achilles tendon to exercise. Scand J Med Sci Sport 16 (2006): 463-469.
- Webster M, Morris M, Galna B. Shoulder pain in water polo: A systematic review of the literature. J Sci Med Sport 12 (2009): 3-11.
- Galluccio F, Bellucci E, Porta F, et al. The water polo shoulder paradigm: Results of ultrasound surveillance at poolside. BMJ Open Sport Exerc Med 3 (2017): 1-4.
- Jerosch J, Castro WH, Drescher H AJ. Kernspinmorphologische Veränderungen an Schultergelenken von Weltklasse-Wasserballspielern. Sportverletzung Sportschaden 7 (1993): 109-114.
- Constant C, Murley A. A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 214 (1987):160-164.
- Beggs I. Shoulder Ultrasound. Semin Ultrasound, CT MRI 32 (2011): 101-113.
- Chiou H, Chou Y, Wu J, et al. Evaluation of calcific tendonitis of the rotator cuff: role of color Doppler ultrasonography. J Ultrasound Med 21 (2002): 289-295.
- Chiou H, Chou Y, Wu J, et al. The role of high-resolution ultrasonography in management of calcific tendonitis of the rotator cuff. Ultrasound in Medicine and Biology 27 (2001): 735-743.
- Chang CY, Wang SF, Chiou HJ, et al. Comparison of shoulder ultrasound and MR imaging in diagnosing full-thickness rotator cuff tears. Clin Imaging 26 (2002): 50-54.
- Brooks J. Injuries in water polo. Clin Sports Med 18 (1999): 313-319.
- McMaster WC, Long SC, Caiozzo VJ. Isokinetic torque imbalances in the rotator cuff of the elite water polo player. Am J Sport Med 19 (1991): 72-75.
- Alexander M, Hayward JAH. Water polo: A Biomechanical Analysis of the Shot (2010).
- Bryant L, Shnier R, Bryant C, et al. A comparison of clinical estimation, ultrasonography, magnetic resonance imaging, and arthroscopy in determining the size of rotator cuff tears. J Shoulder Elb Surg 11 (2002): 219-224.
- Co S, Bhalla S, Rowan K, et al. Comparison of 2- and 3-dimensional shoulder ultrasound to magnetic resonance imaging in a community hospital for the detection of supraspinatus rotator cuff tears with improved worktime room efficiency. Can Assoc Radiol J 63 (2012): 170-176.
- Nazarian L. The top 10 reasons musculoskeletal sonography is an important complementary or alternative technique to MRI. Am J Roentgenol 190 (2008): 1621-1626.
- Rutten M, Maresch B, Jager G, et al. Ultrasound of the rotator cuff with MRI and anatomic correlation. Eur J Radiol 62 (2007): 427-436.
- Ocguder DA, Tosun O, Bektaser B, et al. Ultrasonographic evaluation of the shoulder in asymptomatic overhead athletes. Acta Orthop Belg 76 (2010): 456-4-461.
- Wang H, Lin J, Pan S, et al. Sonographic evaluations in elite college baseball athletes. Scand J Med Sci Sport. 15 (2005): 29-35.
- Malanga GA, Jenp YN, Growney ES, et al. EMG analysis of shoulder positioning in testing and strengthening the supraspinatus. Med Sci Sports Exerc 28 (1996): 661-664.
- Wolf B, Ebinger A, Lawler M, et al. Injury patterns in Division I collegiate swimming. Am J Sports Med 37 (2009): 2037-2042.
- Yen C, Chiou H, Chou Y, et al. Six surgery-correlated sonographic signs for rotator cuff tears: Emphasis on partial-thickness tear. Clin Imaging 28 (2004): 69-76.
- Gisslen K, Gyulai C, Soderman K, et al. High prevalence of jumper’s knee and sonographic changes in Swedish elite junior volleyball players compared to matched controls. Br J Sports Med 39 (2005): 298-301.
- Hirschmüller A, Frey V, Konstantinidis L, et al. Prognostic value of Achilles tendon Doppler sonography in asymptomatic runners. Med Sci Sports Exerc 44 (2012): 199-205.
- Richards PJ, McCall IW, Day C, et al. Longitudinal microvascularity in Achilles tendinopathy (power Doppler ultrasound, magnetic resonance imaging time-intensity curves and the Victorian Institute of Sport Assessment-Achilles questionnaire): A pilot study. Skeletal Radiol 39 (2010): 509-521.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 73.64%
Acceptance Rate: 73.64%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 