Consumption and Intraoperative Controllability of Desflurane-A Randomized Trial Comparing Manually-Assisted (Perseus® A 500- Dräger) and Automated Control (Aisys® Cs2-GE) of End-Tidal Concentrations
Christophe Gutton1, Benjamin Bonnot1, Julien Schroedt2, Emilie Begneu1, Corinne Alberti2, Marc Beaussier3*
1Department of Anaesthesiology and Intensive care, Hôpital Saint-Antoine, Paris, France
2Department of Biostatistic, URC Robert Debré, Hôpital Robert Debré, Paris, France
3Department of Anaesthesiology, Institut Mutualiste Montsouris, Paris, France
*Corresponding author: Marc Beaussier, Department of Anaesthesiology, Institut Mutualiste Montsouris, 42 Boulevard Jourdan, 75014, Paris, France
Received: 11 May 2020; Accepted: 18 May 2020; Published: 05 June 2020
Article Information
Citation:
Christophe Gutton, Benjamin Bonnot, Julien Schroedt, Emilie Begneu, Corinne Alberti, Marc Beaussier. Consumption and Intraoperative Controllability of Desflurane-A Randomized Trial Comparing Manually-Assisted (Perseus® A 500-Dräger) and Automated Control (Aisys® Cs2-GE) of End-Tidal Concentrations. Journal of Pharmacy and Pharmacology Research 4 (2020): 34-43.
View / Download Pdf Share at FacebookAbstract
Purpose : As compared to conventional manually-assisted administration, the automated-control of end-tidal inhalation anaesthetic concentration (EtControl® Aisys® Cs2 - GE) allows for a reduction of halogenated gas consumption and an improvement of the target end-tidal fraction (Fet) controllability. However, recent real time decision support software may help anaesthesiologists to optimize manually-assisted halogenated agent delivery (VaporView®, Perseus A500® - Dräger). The aim of this study was to compare these two delivery methods.
Methods: This was a prospective randomized study comparing the consumption and controllability of Desflurane (Des) between the Vaporview® and Etcontrol® modes of administration in daily clinical practice conditions with a hypothesis of non-inferiority. The Vaporview® mode followed a protocol similar to the Etcontrol® mode for the wash in and wash out periods, and followed the Vaporview® curve to adjust the delivered Fraction (Fd) during the maintenance of the end-tidal fraction (Fe) at 0.5 l.min-1 fresh gas flow. Consumptions were measured by micrometric weighing of the vaporizer.
Results: 58 patients were randomized. The Desflurane consumption in the Perseus Vaporview` group was 13.71 ml.hr-1 (95% CI: 13.02-14.41) versus 13.27 ml.hr-1 (95% CI: 12.30-14.24) in the reference Aisys Etcontrol® group, satisfying statistical criteria for non-inferiority. There were no significant differences either in time to reach MAC 1, or in the number of Fd/Fe adjustments per hour.
Conclusions: Within clinical daily practice conditions, consumption of Desflurane with manually-assisted delivery (Dräger Perseus Vaporview®) was not statistical
Keywords
<p>Anaesthetic agent; Desflurane; Consumption; Automated low flow; Fresh gas flow; Inhalation economics</p>
Article Details
1. Introduction
Since the early 2000’s, the adoption of low-flow inhaled anaesthesia has proven economic advantages [1,2] and a reduction of environmental concerns by decreasing halogenated agent consumption [3,4]. During that period, the education of anaesthesiologists to manually reduce Fresh Gas Flow (FGF) led to significant results in halogenated agent consumption [5]. Recently, several ventilators proposing Target Controlled Inhaled Anaesthesia (TCIA) have been developed. Using this mode of administration, target end-tidal Fraction (Fet) set by the anaesthesiologist is obtained according to an algorithm which takes into account pharmacokinetic modelisation and patients' functional residual capacity [6] to automatically adjust optimal FGF and delivered fraction (Fd). It has been shown that, as compared to conventional manual adjustment of Fd, TCIA mode allows for a reduction of inhaled agent consumption and an improvement of Fet intraoperative controllability [4,7]. The Aisys® Cs2 ventilator (General Electrics, GE) offers TCIA technology in the EtControl® mode. This ventilator has an initial high FGF period (6 l.min-1) until reaching the desired end-tidal fractions, and automatically « closes the system » thereafter by maintaining a minimal FGF of 0.5 l.min-1 during the time of Desflurane delivery. The major problem of this advanced technology is the acquisition and maintenance cost. It is the reason why new ventilators are proposing less expensive alternatives to TCIA technology with electronic advances that can help anesthesiologists to maintain optimal FGF and Fd manually. The Perseus® A 500 offers the VaporView® mode based on the Bailey model [8, 9], i.e. an algorithm that gives the evolution of inspired (Fi) and end-tidal (Fe) fractions of halogenated agents for the upcoming 20 minutes, based on FGF and Fd. In this mode, FGF is manually adjusted by the practitioner who regulates by himself/herself a short starting period of high FGF to reach the desired Fe. Thereafter, FGF and Fd can be optimized using the VaporView® mode to maintain a stable Fe over the subsequent 20 minutes of anaesthesia. Data curves on Fi and Fe are displayed on the ventilator screen, making the VaporView® technology very easy to use. Until now, the potential benefit of the VaporView® assistance in the manual mode of halogenated agent administration has never been compared to TCIA. The aim of this prospective randomized study was to compare Desflurane consumption and intraoperative concentration controllability between these two administration methods in daily clinical practice conditions.
2. Material and Methods
2.1 Study design
This is a mono-center, randomized, simple-blind trial based on a non-inferiority hypothesis for the consumption of Desflurane between Perseus® (manual mode guided by Vaporview® ventilators) and Aisys® (automated Etcontrol® mode ventilators). Two Aisys® systems and two Perseus® systems were dedicated to the study. The investigator responsible for the protocol included anonymized participants. For the allocation of participants, a randomization was performed manually by an agent of the URC Robert Debré (Research Clinic Unit). The patient and the URC agent were blinded. The e-crf was implemented by the URC agent, copying the data collected by the investigator.
2.2 Patients
This study received an IRB approval (CPP Ile de France 3, n° 2014-A01476-41, November 2014). After information and written consents, 60 adult patients ≥ 18 years, American Society of Anesthesiology (ASA) Physical status I/II, undergoing a general anaesthesia of more than one hour were randomly assigned into two groups: Perseus® and Aisys®. Exclusion criteria were as follows: contraindication for halogenated agents, ASA IV, emergency surgery, sepsis or shock.
2.3 Interventions
Before the procedure, the soda lime tank of the ventilator was systematically changed and the circuit purged. Standard monitoring was placed before the induction of general anaesthesia, associated to a bispectral index BIS® monitor. After pre-oxygenation, the induction of general anaesthesia was achieved using propofol 2 to 3 mg.kg-1, sufentanil Target Control Infusion 0.2 ng.ml-1 and atracurium 0.5 mg.kg-1. After orotracheal intubation, mechanical ventilation was initiated (Vt 7 ml.kg-1, PEEP 6 cm H2O) and set to maintain PetCO2 between 35 and 40 mmHg. An association of TCI sufentanil and the continuous infusion of atracrium were used to maintain anaesthesia and Desflurane in a mixture of O2/air 50/50% was started and set to deliver a constant age-adjusted concentration corresponding to MAC [1 - 1.2] [10]. Patients were randomly allocated to receive Desflurane, delivered either by the Etcontrol® TCIA mode in the Aisys group (reference group) or by the Vapor View® manually assisted mode in the Perseus group. The desired Fe was achieved automatically in the Aisys group with the EtControl® mode and manually in the Perseus group with the VaporView® mode (Figure 1).
- In the Aisys group, FGF was initially set to a maximal of 6 l.min-1 with high Fd until reaching as fast as possible the Fe corresponding to [1 - 1.2] MAC. Thereafter, the circuit was automatically closed to deliver a constant 0.5 l.min-1 FGF and Fd was concomitantly adapted to maintain the Fet.
- In the Perseus group, Fd was initially set to 12% with a 3 l.min-1 FGF until reaching [1 - 1.2] MAC, then the circuit was manually closed to a 0.5 l.min-1 FGF and Fd was manually adjusted according to VaporView® indications to maintain the Fe plateau curve corresponding to [1 - 1.2] MAC with a 20 minute prediction.
If Fe went out of the range [1 - 1.2] MAC, arterial hypotension (PAS ≤ 80 mmHg) or BIS value out of the range [40 - 60], Fet was reduced in the Aisys group or Fd was changed in the Perseus group, at the discretion of the physician, but without changing FGF whatever the group, unless emergency situations. At the end of the surgery (wound closure), the Desflurane administration was switched off and the circuit purged with a 10 l.min-1 FiO2 100% until the patient's awakening.
2.4 Outcome measurements
The primary outcome was defined as the intraoperative hourly Desflurane consumption. It was measured by micrometric weighing of the vaporizer before and after general anaesthesia (Explorer® EX102202, OHAUS, Greifensee, Switzerland). Secondary outcomes were the kinetics profile of Desflurane to reach the targets: Fe (MAC 1-1.2) at the beginning of the administration; the kinetic profile of elimination (time for Fe to reach MAC ≤ 0,1) at the end of anaesthesia and the number of intraoperative Fd (Perseus group) or Fet (Aisys group) adjustments. Adverse events such as arterial hypotension < 80 mmHg, arterial hypertension > 160 mmHg, bradycardia < 40 bpm and supra-ventricular rhythm disorders were also collected.
2.5 Statistical analysis
The objective of the study was to demonstrate that the Desflurane consumption in the Perseus® (Manual mode guided by Vaporview®) group would be non-inferior to the one obtained in the Aisys® (Automated Etcontrol® mode) group, within a margin of ± 2.5 ml.hr-1. A retrospective pilot assessment during a 3 month period showed that Desflurane consumption on the Aisys® ventilator was at an average of 11.7 ml.hr-1. We calculated that, for the primary outcome, a sample size of 30 patients per group was required to be 90% sure that the lower limit of a one-sided 97.5% confidence interval would be above the non-inferiority limit of 2 ml.h-1 with a standard deviation of 2.5 ml.h-1. The primary analysis was tested on the population constituted of patients who underwent randomization and the scheduled surgery. Patients were excluded from the analysis if they presented a shock during intervention; if the Desflurane vaporizer had to be opened or if the consent was withdrawn. We calculated a 95% confidence interval (CI) of the difference between intraoperative Desflurane consumption per minute. Qualitative variables were described as numbers (percentages) and quantitative variables as median (1st quartile – 3rd quartile) or mean (standard deviation). For secondary outcomes, the Wilcoxon test was used. Statistical analyses were carried out using SAS® 9.4 for PC. All tests were bilateral and the significant level was set to 5%.
3. Results
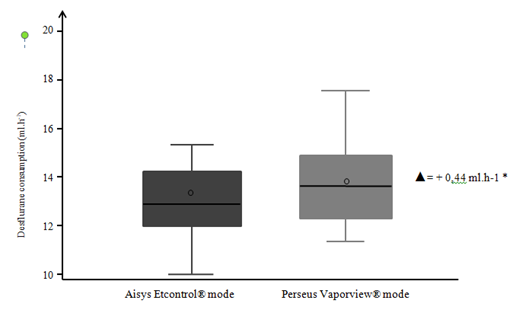
A total of 60 patients were assessed for eligibility. Two of them did not meet inclusion criteria. Fifty eight were randomized (29 in each study group). Demographic patient characteristics are presented in Table 1. There was no difference between the two groups. Desflurane consumption was 13.71 ml.hr-1 (95% CI; 13.02-14.41) versus 13.27 ml.hr-1 (95% CI; 12.30-14.24) in the Perseus® and the Aisys® groups respectively. Mean consumption difference was 0.44 ml.hr-1 satisfying statistical criteria for non-inferiority (Figure 2 and Table 2). Secondary outcomes are presented in Table 3. No significant differences were observed between the groups neither in time to reach MAC 1 nor in time of circuit closure after having reached MAC 1, nor in time to reach MAC ≤ 0,1 at Desflurane discontinuation. There was no significant difference in the number of Fd/Fet adjustments per hour. Concerning adverse events, only arterial hypotension periods were observed, without significant difference between the groups.
|
Variable |
Perseus group (n = 27) |
Aisys group (n = 28) |
|
|
Sex (male / female) |
12 / 15 |
13 / 15 |
|
|
Age (y) |
52.5 (42 to 62) |
55.3 (39 to 66) |
|
|
Weight (kg) |
68 (60 to 74) |
65 (60 to 73) |
|
|
BMI (kg.m-2) |
24.2 (22 to 27) |
22 (20 to 24) |
|
|
ASA |
|||
|
1 |
10 |
6 |
|
|
2 |
17 |
21 |
|
|
3 |
0 |
2 |
|
|
Type of surgery |
|||
|
Laparotomy |
16 |
18 |
|
|
Coelioscopy |
9 |
10 |
|
Table 1: Patients Characteristics. Data expressed as number or median (Interquartile range).
*▲ = Mean consumption differences, ranging from [0 - 2] ml.hr-1, satisfying statistical criteria for non-inferiority
|
Perseus group (n = 27) |
Aisys group (n = 28) |
|
|
Time of Halogenated Anaesthesia (min) |
333 (239 to 396) |
368 (240 to 435) |
|
Desflurane (ml.h-1) |
13.7 (13 to 14.4) |
13.3 (12.3 to 14.2) |
|
Desflurane (ml.min-1) |
0.23 (0.21 to 0.25) |
0.21 (0.2 to 0.24) |
Table 2: Desflurane Consumption. Data expressed in median (Interquartile range).
|
Perseus group (n = 27) |
Aisys group (n = 28) |
P
|
|
|
Time (min) to reach FeDes for MAC [1 - 1,2] |
2 (1.8 to 2.4) |
1.9 (1.6 to 2.6) |
0.88 |
|
Time (min) of circuit closure |
2.3 (1.8 to 2.8) |
2.2 (1.9 to 3.3) |
0.46 |
|
Time (min) to reach MAC ≤ 0.1 at the end of anesthesia |
8 (3.11) |
7.4 (2.73) |
0.4 |
|
Number of FeDes adjustments per hour all elements together |
0.4 (0 to 0.7) |
0.3 (0 to 0.4) |
0.33 |
|
Number of FeDes adjustments per hour due to a MAC out of [1 - 1.2] |
0.06 (0 to 0.3) |
0 (0 to 0.3) |
0.52 |
|
Number of FeDes adjustments per hour due to a BIS out of [40 - 60] |
0 (0 to 0.2) |
0 (0 to 0.2) |
0.84 |
Table 3: Secondary Outcomes: Kinetics and controllability. Data expressed in median (Interquartile range) or mean (Standard deviation).
4. Discussion
In this prospective randomized study, based on daily clinical practice conditions, Desflurane consumption does not statistically differ if administered by either the Perseus® A500 in VaporView® mode or the automated EtControl® mode of the Aisys® Cs2. Moreover the kinetic profiles to reach the targeted Fe (MAC 1-1.2) at the beginning of the administration; the elimination rates at the end of anaesthesia and the number of intraoperative Fd (Perseus group) or Fet (Aisys group) adjustments showed no significant differences between the two groups. The choice of Desflurane was made because this agent is particularly suitable for low-flow anaesthesia [11]. Furthermore, it is the least degradable of the currently available inhaled anesthetics [12]. It is also the most expensive halogenated anesthetic [11] and could be accountable for 20 to 25% of overall anesthetic drug costs [13] and has a potential environmental impact [14]. This makes all endeavors to reduce its consumption highly justified. Vaporview® is software associated with the Perseus® machine. It may be used to help anesthesiologists manually maintain optimal FGF and Fd to predict upcoming Fe according to an algorithm that gives the evolution of inspired (Fi) and end-tidal (Fe) fractions of halogenated agents according to FGF and Fd. The current study is the first one to measure the exact halogenated agent consumption using Vaporview® mode in a controlled clinical situation. It is also the first to compare Desflurane kinetic profiles between Vaporview® and a TCIA mode. Additionally, this study could be helpful for practitioners in providing a clinical protocol to be followed using Vaporview®.
The EtControl® TCIA mode was chosen because Aisys® is actually a workstation commonly used for performing TCIA. The EtControl® mode is easy to handle, adjusting automatically the FGF to 0.5l.min-1 during the longest period of inhaled anaesthesia. The Aladin® halogenated tank of the Aisys® is a vaporizer that needs a minimum FGF passing through it to deliver halogenated agent in the system. That is why FGF with the Aisys® is limited to 0.5 l.min-1. A median Desflurane consumption, under 14 ml.hr-1 (i.e. under 0.23 ml.min-1) in both groups was observed. For Aisys® in EtControl® mode, it is less than previously described by Singaravelu and Barclay [15], probably because the period at low FGF was much longer in our study with a 330 min median anaesthesia. Indeed, it has been shown that 50% of the consumption happens during the first 10 minutes of administration [16]. The current study is the first measuring the exact halogenated agent consumption administered using Perseus® in Vaporview® mode. In previous publications, a few studies have compared manual versus automated modalities of halogenated agent delivery. Struys and colleagues [6] compared the Zeus® (Dräger) in auto-control mode (FGF 0.5l.min-1) and the Primus® (Dräger) in manual mode with a stable FGF (1l.min-1). But this study was an in-vitro comparison, with a very short period of anaesthesia (30 minutes) and the lowest FGF in the Primus® group was only 1l.min-1. To our knowledge, De Cooman and colleagues [17] are the first ones finding a consumption difference in favor of a manual mode. In this study, the Zeus® in auto-control mode was compared with the ADU® (GE), but the groups were not comparable (n=26 versus n=10) and not randomized. Moreover, unlike us, Desflurane consumption was calculated and not directly measured.
Another crucial part of our results is that the manually-assisted Vaporview® and automated protocol Aisys® displayed similar Fe kinetic profiles at the initiation of inhaled anaesthesia (Table 3). This is consistent with previous arguments showing that it is more efficient to saturate the breathing system with an overshoot of high Fd than with a high FGF [16,18] Accordingly, a recent study comparing Sevoflurane and Desflurane kinetics between four groups using Aisys® showed that the initiation of inhaled anaesthesia using only very low FGF was clinically possible [19]. In this study, the wash-in was made by an overshoot of Fd (18% Desflurane) keeping the same low FGF (0.5 or 1 l.min-1). But the time to reach MAC 1 at 0.5 l.min-1 FGF was 8.5 +/- 0.7 min, about 6 minutes longer than in our study. In clinical practice this wash-in duration is too long with the risk of the patient awakening during this period. This explains why in auto-control mode of the Aisys® ventilator, a short period of high but not excessive FGF (6l.min-1) is automatically provided to obtain a faster target Fe. This is also why in the current study a short period of high FGF (3l.min-1) was maintained in manual mode to rapidly obtain MAC 1. This reduced 3 l.min-1 FGF regimen in the Perseus® group was chosen because it was noticed in the pilot study that the velocity for reaching high Fe was too high at 6l.min-1 (less than 1 min). An explanation could be that the breathing system, including the absorbent canister is two times larger for the Aisys® than for the Perseus®.
During the maintenance of anaesthesia at 0.5 l.min-1, the necessity to adapt Fd to keep the MAC did not differ between the EtControl® and the VaporView® modes. The median duration of inhaled anaesthesia of more than five hours showed that it was able to remain at 0.5 l.min-1 FGF in both groups, with a stable Fet and MAC objective regardless of the anaesthesia duration. Finally median time to extubation was 11.7 min in the Perseus® group and 12.1 min in the Aisys® group. No tapering technique was used because of the Desflurane properties for which the 90% decrement time is quite similar whatever the duration of administration [9].
In conclusion, in daily clinical practice conditions, Desflurane consumption is not inferior between the manually-assisted administration in the Dräger Perseus Vaporview® mode and the automated-controlled administration using the General Electrics Aisys EtControl®. Fe kinetic profiles and ventilator adjustment requirements did not differ between these two administration methods.
Funding
An external funding was obtained by the Dräger Company to perform this evaluation.
Conflicts of Interest
The Dräger engineers provided an explanation of the software and functions, but the data collection, analysis and interpretation were performed entirely by independent investigators. The micrometric weighing machine was lent by the Dräger Company. Both the GE Aisys Carestation and the Dräger Perseus Carestation were purchased by the hospital.
References
- Baxter AD. Low and minimal flow inhalational anaesthesia. Can J Anaesth 44 (1997): 643-652.
- Lockwood GG, White DC. Measuring the costs of inhaled anaesthetics. Br J Anaesth 87 (2001): 559-563.
- Feldman JM. Managing fresh gas flow to reduce environmental contamination. Anesth Analg 114 (2012): 1093-1101.
- Tay S, Weinberg L, Peyton P, et al. Financial and environmental costs of manual versus automated control of end-tidal gas concentrations. Anaesth. Intensive Care 41 (2013): 95-101.
- Kennedy RR, French RA. Changing patterns in anesthetic fresh gas flow rates over 5 years in a teaching hospital. Anesth Analg 106 (2008): 1487-1490.
- Struys MMRF, Kalmar AF, De Baerdemaeker LEC, et al. Time course of inhaled anaesthetic drug delivery using a new multifunctional closed-circuit anaesthesia ventilator. In vitro comparison with a classical anaesthesia machine. Br J Anaesth 94 (2005): 306-317.
- Suttner S, Boldt J. Low-flow anaesthesia. Does it have potential pharmacoeconomic consequences? Pharmacoeconomics 17 (2000): 585-590.
- Bailey JM. The pharmacokinetics of volatile anesthetic agent elimination: a theoretical study. J. Pharmacokinet Biopharm 17 (1989): 109-123.
- Bailey JM. Context-sensitive half-times and other decrement times of inhaled anesthetics. Anesth Analg 85 (1997): 681-686.
- Eger EI, Saidman LJ, Brandstater B. Minimum alveolar anesthetic concentration: a standard of anesthetic potency. Anesthesiology 26 (1965): 756-763.
- Jakobsson J. Desflurane: A clinical update of a third-generation inhaled anaesthetic. Acta Anaesthesiol Scand 56 (2012): 420-432.
- Kapoor M, Vakamudi M. Desflurane - Revisited. J. Anaesthesiol Clin Pharmacol 28 (2012): 92.
- Odin I, Feiss P. Low flow and economics of inhalational anaesthesia. Best Pract Res Clin Anaesthesiol 19 (2005): 399-413.
- Sulbaek Andersen MP, Sander SP, Nielsen OJ, et al. Inhalation anaesthetics and climate change. Br J Anaesth 105 (2010): 760-766.
- Singaravelu S, Barclay P. Automated control of end-tidal inhalation anaesthetic concentration using the GE Aisys Carestation. Br J Anaesth 110 (2013): 561-566.
- Quénet E, Weil G, Billard V. Which settings to optimize anaesthetics delivery: fresh gas flow or delivered fraction? Ann Fr Anesth Reanim 27 (2008): 900-908.
- De Cooman S, De Mey N, Dewulf BB, et al. Desflurane Consumption During Automated Closed-circuit Delivery is Higher Than When a Conventional Anesthesia Machine is Used With a Simple Vaporizer-O2-N2O Fresh Gas Flow Sequence. BMC Anesthesiol 8 (2008): 4.
- Coetzee JF, Stewart LJ. Fresh gas flow is not the only determinant of volatile agent consumption: a multi-centre study of low-flow anaesthesia. Br J Anaesth 88 (2002): 46-55.
- Horwitz M, Jakobsson JG. Desflurane and sevoflurane use during low- and minimal-flow anesthesia at fixed vaporizer settings. Minerva Anestesiol 82 (2016): 180-185.
Article Views: 3621
Journal Statistics




Discover More: Recent Articles