Evolution of Studies on Orthopaedic Surgery Regarding Cost Management Tools: A Systematic Literature Review
Isabel Cristina Panziera Marques*, Alba Katarine Marques de Carvalho
Management and Economics Department, University Beira Interior (UBI), Pólo IV, Estrada do Sineiro, 6200-209, Covilhã, Portugal
*Corresponding Author: Isabel Cristina Panziera Marques, Management and Economics Department, University Beira Interior (UBI), Pólo IV, Estrada do Sineiro, 6200-209, Covilhã, Portugal
Received: 24 March 2020; Accepted: 31 March 2020; Published: 08 April 2020
Article Information
Citation: Isabel Cristina Panziera Marques, Alba Katarine Marques de Carvalho. Evolution of studies on orthopaedic surgery regarding cost management tools: a systematic literature review. Journal of Orthopaedics and Sports Medicine 2 (2020): 61-88.
View / Download Pdf Share at FacebookAbstract
Objective: The subject of hospital management is relevant given the importance of these institutions in the social and economic sphere, as well as for their managers, considering that in the hospital context, which involves high costs, scarce resources, pressure for quality and good service, information on costs and performance is useful for efficient management. This systematic literature review (SLR) aims to extend knowledge of the evidence linking costing mechanisms to the performance results of health institutions, analysing articles written in the last 10 years dealing with surgery in the specialization of orthopaedics, filling an important gap in the literature.
Methods: Rigorous criteria for selection of articles is followed by use of the PRISMA meta-analysis, which gives an important overview of the types of studies made, as well as classification according to the cost management tools, leading to mapping costing methods and performance analysis.
Results: Studies were classified by measurement methods, costs of decision-making and control and elements of strategic cost management, showing that the greatest number of studies originate in the USA (69, 23%) and use the variable of statistical analysis (53, 85%) in the majority of strategic management methods. As for types of surgical procedures, arthroplasty leads the ranking, accounting for 34, 62% of studies.
Conclusions: Predominance of the use of standard costing as the method of measurement, use of control methods for decision-making and a tendency towards the practice of statistical analysis as a variable of the elements of strategic cost management, with studies of replacement surgery (hip, knee and shoulder) being most prominent. This study provides managers and public policy-makers with challenges and indicators of efficiency and effectiveness for better performance in orthopaedic surgica
Keywords
<p>Costs; Surgery; Hospital; Orthopaedics</p>
Article Details
1. Introduction
Strategic cost management has become an excellent alternative to be used by companies, serving as a guide at the time of decision-making and seen, traditionally, as the process of assessing the financial impact of managerial decisions. Numerous factors encourage researchers to analyse the quality of assistance provided [1-3], seeking to assess the variation in the results and costs of patients in various situations of hospitalization [4-7], compare different surgical methods and determine the reasons for hospital readmission after surgery [8-11], examine alternatives for better rehabilitation following orthopaedic procedures [12-14] and confirm coherence between surgical costs and compensation [15-19, 6, 20-22], among others.
In this context, management tools help decision-makers such as hospital managers and public policy-makers to seek the best practices leading to greater efficiency and effectiveness of processes, examples including the optimization of operating theatres, incentives for alternative models for paying doctors and hospitals, and analysis of the financial risks and risks of post-surgical complications from certain surgery. Controlling the costs involved in health is a challenge [23], due to the complexity of products and the range of human, financial, material and technological resources involved, meaning efficient cost management is necessary. Given this complexity, cost accounting can provide relevant information for hospital management, through its tools for assessing stock (absorption costing), control (standard cost), decision-making (variable costing, activity-based costing) and managerial artefacts in the field of Strategic Management (target costing, cost determinants, analysis of competitors’ costs, cost-effectiveness analysis, ABC/ABM, quality costs). The aim of this systematic review is therefore to contribute by presenting articles published over 10 years and classifying them according to the cost management tools used, the costing formats followed in hospitals using protocols adapted from [24-26]. This will involve appropriate selection of studies, showing in summary form the different types of analysis made.
2. Methodology
The research method is the Systematic Literature Review (SLR). Having defined the objective of the review as analysis of trends in emerging studies, this will include important articles through orientations and strategies that increase the specificity of the search. In selecting studies, assessment of the titles and abstracts identified follows inclusion and exclusion criteria defined as “orthopaedics”. The general description of the review process is presented in (Figure 1).

Figure 1: SLR protocol used.
A search on the Scopus database using the key-words of “costs, surgeries, privatehospita” resulted in 954 articles, and after limitations (“Medicine”, “Economics, Econometrics and Finances”, “Nursing”, “Social Sciences”, English language, document type “Articles “and “Reviews””) 492 articles remained. Data collection took place on 13 February 2020.
Eligibility. The criteria are: i) publications discussing costing of surgical procedures; ii) published between 2010 and 2020; iii) in English; iv) including some performance analysis. The abstracts were reviewed and scored as follows: 3 points for abstracts with definite mention of the research questions and meeting the search criteria described above; 2 points for abstracts that probably deal with the research questions, 1 point for abstracts that may deal with the research questions or 0 points for abstracts that do not deal with the research questions.
According to the proposed objective, to identify articles studying the field of orthopaedics and aiming to analyse health institutions’ performance, the 492 articles retained in the selection phase had their abstract, introduction and conclusions analysed. Of the 492 articles, 52 focused on the orthopaedic specialization and so are categorised according to the country studied, the reasons leading researchers to choose the topic, the type of surgery investigated, the period studied, type of cost management tool used and the variable used to determine results. The articles were read and assessed by peers to determine the quality; the items considered were: the methodological robustness of the study (such as clear sample description, systematization of data collection, validity of measures and degree of confidence, appropriate analyses and interpretations). The methodology for selecting studies is presented in (Figure 2).
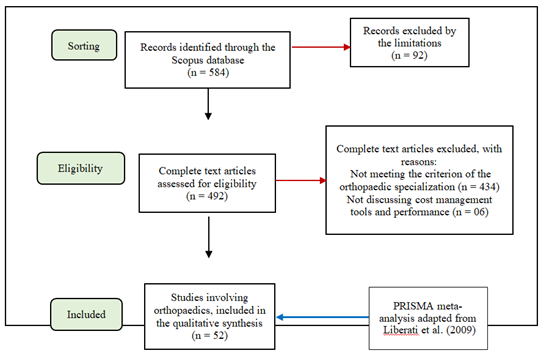
Figure 2: Method of studies at each stage of the bibliographic search.
After the stages of summarising and sorting of the articles, they are classified according to topic groups for analysis. In this phase, no article is eliminated, keeping for analysis all the articles satisfying the criteria of quality and relevance [27].
In this study, an adaptation of the meta-analysis of approximation (PRISMA), by [25] is applied to the 52 studies related to orthopaedic surgery. PRISMA was developed in the field of health sciences, but has already been successfully applied in public administration research [28]. The quality of PRISMA, as an approach to systematic literature reviews, is due to its process of elaboration including repeated improvements based on deliberation among the review specialists, ensuring transparency. Next, the selected studies are classified according to cost management and control tools, showing the costing variables and analyses made in each article.
3. Results and Discussion
Of the 52 articles selected, 36 (69, 23%) originate in the USA, five in Australia, two in the United Kingdom, two in Italy, two in Brazil and the others distributed equally among the Netherlands, France and Austria with one study each (Figure 3). (Figure 4) presents the numbers of articles over the 10 years.
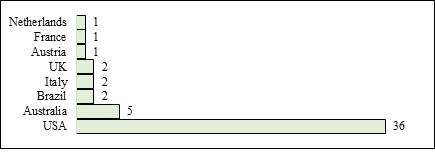
Figure 3: Geographical distribution of the analyzed scientific publications.
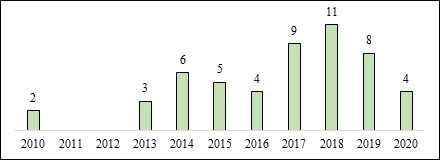
Figure 4: Quantitative studies per year.
3.1 Mapping of the literature on the Orthopaedics speciality
Using an adaptation of the PRISMA meta-analysis by [25] (Figure 5), the articles were classified according to the main components focusing the research methodology (Table 1) with quantitative analysis referring to the: (i) purpose of the study, (ii) information sources, (ii) form of research, (iv) data collection, (v) participants in the study, (vi) type of study, and (vii) period of longitudinal studies.
Regarding purpose, studies are basically divided into descriptive (48, 07%) and exploratory (46, 15%). The information sources used in 75% of studies were various databases, consisting of state and national databases of several types with records including surgical data, patient data, expenditure, hospitalization and others. As for the form of research, the great majority used the deductive method (80, 77%) and quantitative methods to obtain data (86, 53%). Sample participants in 71, 15% of studies were only patients submitted to surgery. In addition, 88, 46% of studies were longitudinal covering a period of 1 to 5 years (54, 35%) (Table 1).
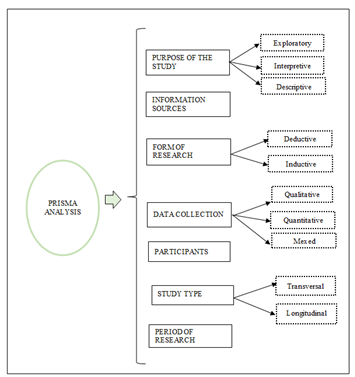
Figure 5: PRISMA analysis for the Orthopedics specialty. Fonte: Adapted from [25].
|
Component |
Classification |
Number of articles |
Relative frequency (%) |
Total frequency |
|
Purpose of the Study |
Interpretative |
3 |
5,77 |
100% |
|
Descriptive |
25 |
48,07 |
||
|
Exploratory |
24 |
46,15 |
||
|
Sources of Information |
Various databanks (state and national of surgery, patients, hospitalization, statistics, expenditure and insurance) |
39 |
75 |
100% |
|
Various databanks and databases (PubMed and Cochrane Library) |
1 |
1,92 |
||
|
Databanks, questionnaires, interviews and records |
2 |
3,84 |
||
|
Various documents |
5 |
9,61 |
||
|
E-mail addresses |
1 |
1,92 |
||
|
Questionnaires |
4 |
7,69 |
||
|
Form of Research |
Inductive |
10 |
19,23 |
100% |
|
Deductive |
42 |
80,77 |
||
|
Data collection |
Qualitative |
1 |
1,92 |
100% |
|
Mixed |
6 |
11,54 |
||
|
Quantitative |
45 |
86,53 |
||
|
Participants |
Health professionals |
4 |
7,69 |
100% |
|
National databanks and insurance |
1 |
1,92 |
||
|
Selected studies |
1 |
1,92 |
||
|
Health organisations (hospitals with doctors and non-doctors, health systems, hospital departments and organisations with quality certification) |
4 |
7,69 |
||
|
Patients |
37 |
71,15 |
||
|
Patients and health professionals |
2 |
3,84 |
||
|
Hospitals |
3 |
5,77 |
||
|
Type of Study |
Transversal |
6 |
11,54 |
100% |
|
Longitudinal |
46 |
88,46 |
||
|
Period of Research |
Under one year |
3 |
6,52 |
100% |
|
1 to 5 years |
25 |
54,35 |
||
|
6 to 10 years |
12 |
26,09 |
||
|
11 years or more |
6 |
13,04 |
Table 1: Classification of studies according to the PRISMA methodology, adapted [25].
(Table 2) classifies and describes the authors and the article’s year of publication, title, research location, the surgery shown, the type of management tool used and the variable used for data treatment.
|
Authors |
Title |
Country of interest |
Surgery / Procedure |
Tool |
Variables |
|
Mealy and Sorensen (2020) [29] [70] |
Effects of an aging population on hospital costs related to elective hip replacements |
Ireland |
Hip replacement |
Elements of strategic cost management |
Homogeneous Diagnostic Group (DRG) - based analyzes |
|
Ackerman et al. (2020) [30] |
Quantifying the likelihood and costs of hip replacement surgery after sports injury: A population-level analysis |
Australia |
Hip replacement |
Elements of strategic cost management |
Statistical analysis |
|
Nassar et al. (2020) [8] |
Rapid recovery following hip and knee arthroplasty using local infiltration analgesia: length of stay, rehabilitation protocol and cost savings |
Australia |
Hip or knee arthroplasty |
Measurement methods |
Standard Cost |
|
Dy et al. (2020) [15] |
Incidence of Surgically Treated Brachial Plexus Injury in Privately Insured Adults Under 65 Years of Age in the USA |
USA |
Nerve grafts |
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
|
Yayac et al. (2019) [31] |
Conversion Total Knee Arthroplasty is Associated with Increased Post-Acute Care Costs |
USA |
Knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Garriga et al. (2019) [5] |
Geographical Variation in Outcomes of Primary Hip and Knee Replacement |
UK |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Slover et al. (2019) [32] |
Factors associated with utilizing the same hospital for subsequent total hip or knee arthroplasty in osteoarthritis patients |
USA |
Total joint arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Boylan et al. (2019) [33] |
Tibial shaft fractures in workers compensation and no-fault insurance: Is there a difference in resource utilization? |
USA |
Fixation of tibial shaft fractures |
Elements of strategic cost management |
Cost effectiveness, competitor analysis, value chain |
|
Bokshan et al. (2019) [16] |
What Are the Primary Cost Drivers of Anterior Cruciate Ligament Reconstruction in the United States? A Cost-Minimization Analysis of 14,713 Patients |
USA |
Ligament reconstruction |
Elements of strategic cost management |
Statistical analysis |
|
Phillips et al. (2019) [10] |
How Much Does a Readmission Cost the Bundle Following Primary Hip and Knee Arthroplasty? |
USA |
Total joint arthroplasty |
Measurement methods |
Standard Cost |
|
Lyons et al. (2019) [17] |
A 5-year review of hospital costs and reimbursement in the surgical management of degenerative spondylolisthesis |
Lebanon |
Single-level fusions of degenerative spondylolisthesis |
Elements of strategic cost management |
Statistical analysis |
|
Padegimas et al. (2019) [18] |
The effect of an orthopedic specialty hospital on operating room efficiency in shoulder arthroplasty |
USA |
Shoulder arthroplasty |
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
|
Cho et al. (2018) [19] |
Finger Replantation Optimization Study (FRONT): Update on National Trends |
USA |
Traumatic digit amputation |
Elements of strategic cost management |
Statistical analysis |
|
Tedesco et al. (2018) [13] |
Impact of rehabilitation on mortality and readmissions after surgery for hip fracture |
Italy |
Hip replacement |
Elements of strategic cost management |
Statistical analysis |
|
Naylor et al. (2018) [12] |
The effectiveness of inpatient rehabilitation after uncomplicated total hip arthroplasty: A propensity score matched cohort |
Australia |
Hip replacement |
Elements of strategic cost management |
Homogeneous Diagnostic Group (DRG) - based analyzes |
|
Bernstein et al. (2018) [1] |
Total Joint Arthroplasty Quality Ratings: How Are They Similar and How Are They Different? |
USA |
Total joint arthroplasty |
Elements of strategic cost management |
Cost effectiveness, competitor analysis, value chain |
|
Thamyongkit et al. (2018) [34] |
Use of reprocessed external fixators in orthopaedic surgery: A survey of 243 orthopaedic trauma surgeons |
USA |
Use of external fixators |
Elements of strategic cost management |
Quality Cost, web-based searches |
|
Courtney et al. (2018) [2] |
Maximizing Physician-Hospital Alignment: Lessons Learned From Effective Models of Joint Arthroplasty Care |
USA |
Hip or knee arthroplasty |
Measurement methods |
Activity-Based Costing (ABC); Time-based ABC costing (TDABC) |
|
Odum et al. (2018) [35] |
Is there value in retrospective 90-day bundle payment models for shoulder arthroplasty procedures? |
USA |
Shoulder arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Boylan et al. (2018) [36] |
Technology-Assisted Hip and Knee Arthroplasties: An Analysis of Utilization Trends |
USA |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Karnon et al. (2018) [6] |
Cost-Utility Analysis of Private Contracting to Reduce Public Waiting Times for Joint Replacement Surgery |
Austria |
Total knee arthroplasty |
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
|
De Paiva Luciano et al. (2018) [37] |
Study of the evolution and variability of nontraumatic orthopedic surgeries in Brazil-9 years of follow-up A database study |
Brazil |
Non-traumatic orthopedic surgeries |
Elements of strategic cost management |
Cost effectiveness, competitor analysis, value chain |
|
Roche et al. (2018) [38] |
Effect of Obesity on Total Knee Arthroplasty Costs and Revision Rate |
USA |
Total knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Rosas et al. (2017) [39] |
National Age and Gender-Specific Costs in Anterior Cruciate Ligament Reconstruction by A Single Nationwide Private Payer |
USA |
Reconstruction of ligament injuries |
Elements of strategic cost management |
Statistical analysis |
|
Curtin et al. (2017) [40] |
Bundled Payments for Care Improvement: Boom or Bust? |
USA |
Various orthopedic surgeries |
Elements of strategic cost management |
Statistical analysis |
|
Naylor et al. (2017) [14] |
The value of inpatient rehabilitation after uncomplicated knee arthroplasty: A propensity score analysis |
Australia |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Stull et al. (2017) [41] |
Economic Burden of Inpatient Admission of Ankle Fractures |
USA |
Internal fixation of open reduction ankle fracture |
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
|
Sabesan et al. (2017) [42] |
Medicaid payer status is linked to increased rates of complications after treatment of proximal humerus fractures |
USA |
Treatment of proximal humerus fracture |
Elements of strategic cost management |
Statistical analysis |
|
Longo et al. (2017) [43] |
The burden of rotator cuff surgery in Italy: a nationwide registry study |
Italy |
Rotator cuff disease treatment |
Elements of strategic cost management |
Homogeneous Diagnostic Group (DRG) - based analyzes |
|
Maxwell Courtney et al. (2017) [7] |
Reconsidering the affordable care act's restrictions on physician-owned hospitals analysis of CMS data on total hip and knee arthroplasty |
USA |
Hip or knee arthroplasty |
Elements of strategic cost management |
Homogeneous Diagnostic Group (DRG) - based analyzes |
|
Schrock et al. (2017) [11] |
A cost-effectiveness analysis of surgical treatment modalities for chondral lesions of the knee: Microfracture, osteochondral autograft transplantation, and autologous chondrocyte implantation |
USA |
Microfracture, osteochondral autograft transplant |
Elements of strategic cost management |
Statistical analysis |
|
Arshi et al. (2017) [20] |
Outpatient total knee arthroplasty is associated with higher risk of perioperative complications |
USA |
Total knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Narvy et al. (2016) [3] |
Direct Cost Analysis of Outpatient Arthroscopic Rotator Cuff Repair in Medicare and Non-Medicare Populations |
USA |
Rotator cuff disease treatment |
Measurement methods |
Standard Cost |
|
Thorpe et al. (2016) [44] |
Rising trends in surgery for rotator cuff disease in Western Australia |
Australia |
Rotator cuff disease treatment |
Elements of strategic cost management |
Statistical analysis |
|
Kurtz et al. (2016) [45] |
Universal Health Insurance Coverage in Massachusetts Did Not Change the Trajectory of Arthroplasty Use or Costs |
USA |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Zhou et al. (2016) [46] |
In-patient trends and complications after total ankle arthroplasty in the United States |
USA |
Total ankle arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Hernandez et al. (2015) [21] |
Does the Medicare 3-Day Rule Increase Length of Stay? |
USA |
Total knee arthroplasty |
Measurement methods |
Standard Cost |
|
Cortada et al. (2015) [47] |
Comparison of thromboprophylaxis patterns in arthroplasty in public and private hospitals |
Brazil |
Hip or knee arthroplasty |
Measurement methods |
Standard Cost |
|
Maravic and Beaudreuil (2015) [48] |
Impact on costs of switching one-ray aponeurectomy to percutaneous needle aponeurotomy in Dupuytren's disease: A model analysis |
France |
Aponeurectomy |
Elements of strategic cost management |
Homogeneous Diagnostic Group (DRG) - based analyzes |
|
Iorio et al. (2015) [49] |
Economic Impact of Orthopedic Adult Reconstruction Office Practice: The Implications of Hospital Employment Models on Local Economies |
USA |
Hip or knee arthroplasty |
Measurement methods |
Mixed Cost |
|
Vanhegan et al. (2015) [50] |
Effect of an Independent-Sector Treatment Centre on provision of elective orthopaedic surgery in East and North Hertfordshire |
UK |
Various orthopedic surgeries |
Measurement methods |
Mixed Cost |
|
Davis et al. (2014) [22] |
Factors affecting hospital charges after total shoulder arthroplasty: An evaluation of the National Inpatient Sample database |
USA |
Shoulder arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Pugely et al. (2014) [51] |
Database and registry research in orthopedic surgery Part I: Claims-based data |
USA |
Various orthopedic surgeries |
Elements of strategic cost management |
Statistical analysis |
|
Kurtz et al. (2014) [52] |
Impact of the economic downturn on total joint replacement demand in the United States: Updated projections to 2021 |
USA |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Raikin et al. (2014) [53] |
Trends in treatment of advanced ankle arthropathy by total ankle replacement or ankle fusion |
USA |
Total ankle arthroplasty |
Measurement methods |
Standard Cost |
|
Sathiyakumar et al. (2014) [54] |
Patterns of costs and spending among orthopedic surgeons across the United States: a national survey. |
USA |
Various orthopedic surgeries |
Elements of strategic cost management |
Statistical analysis |
|
Saleh et al. (2014) [55] |
Allogenic blood transfusion following total hip arthroplasty: Results from the nationwide inpatient sample, 2000 to 2009 |
USA |
Hip arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Voorn et al. (2013) [56] |
Frequent use of blood-saving measures in elective orthopedic surgery: A 2012 Dutch blood management survey |
Netherlands |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Kamath et al. (2013) [57] |
Unplanned hip arthroplasty imposes clinical and cost burdens on treating institutions |
USA |
Hip arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Mehrotra et al. (2013) [58] |
Evaluation of centers of excellence program for knee and hip replacement |
USA |
Hip or knee arthroplasty |
Measurement methods |
Standard Cost |
|
Baser et al. (2010) [59] |
Impact of postoperative venous thromboembolism on Medicare recipients undergoing total hip replacement or total knee replacement surgery |
USA |
Hip or knee arthroplasty |
Elements of strategic cost management |
Statistical analysis |
|
Althausen et al. (2010) [60] |
Financial impact of a dedicated orthopedic traumatologist on a private group practice |
USA |
Various orthopedic surgeries |
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
Table 2: Classification of studies analyzed in SLR, based on [24, 26].
Of the studies analysed, 55, 77% address the replacement procedure (hip, knee, hip and knee, shoulder), the remaining 44, 23% being divided between procedures such as treatment of fractures, reconstruction of ligaments, amputations and external setting of open reductions. Regarding cost management tools, (Table 3) shows that 53, 85% of the studies used diverse statistical analyses to determine the effects of the variables studied. In general, the cost management tools show the paradigm of the research, according to [61], with the epistemological stance of authors implying positivist or functionalist studies, where relatively solid empirical relations can be recognised, studied and measured through approaches coming from the natural sciences.
|
Tool |
Variables |
Number of Articles |
Relative Frequency (%) |
Total Frequency (%) |
|
Measurement methods |
Activity-Based Costing (ABC); Time-based ABC costing (TDABC) |
1 |
10,00 |
100% |
|
Mixed Cost |
2 |
20,00 |
||
|
Standard Cost |
7 |
70,00 |
||
|
Variable Costing, Departmental Cost, Micro Costing |
0 |
0 |
||
|
Costs for decision making and control |
Breakeven point, contribution margin, models and management methods and tools |
5 |
100,0 |
100% |
|
Elements of strategic cost management |
Cost effectiveness, competitor analysis, value chain |
3 |
8,11 |
100% |
|
Homogeneous Diagnostic Group (DRG) - based analyzes |
5 |
13,51 |
||
|
Statistical analysis |
28 |
75,68 |
||
|
Quality Cost, web-based searches |
1 |
2,7 |
|
Table 3: Classification of studies for cost management tools. |
3.2 Methods of measurement
In the hospital context, studies indicate, although not probabilistically, that the main costing method used is ABC costing [62-67] despite the complexity of allocation of indirect costs, followed by mixed costing [68-71] and standard costing [72-76]. On the other hand, regarding cost measurement, in the area of orthopaedics, most cases focused on standard costing [3, 8, 10, 21, 47, 53, 58], two studies used mixed costing [49, 50] and one ABC costing.
3.2.1 Standard costing: [58] compare results and costs associated with replacing knees and hips in designated hospitals and other hospitals, due to Medicare and private plans encouraging individuals to seek treatment in hospitals designated as centres of excellence. Through a retrospective analysis, they concluded that hospitals designated as centres of excellence for joint replacement presented lower rates of complications for hip replacement, but there was no statistically significant difference for knee replacement or significant difference in the 90-day costs for any procedure. The study by [53] compared epidemiological profiles of complete replacement of the ankle and ankle fusion, through a national databank, where demographic data and patients’ comorbities, geographical distribution and the cost of procedures were compared, finding that the total cost of the procedure and hospitalization was higher for complete ankle replacement (average = US $ 51.656) than for ankle fusion (average = US $ 34.795) during the whole period of study and the total cost for both types of surgery increased year by year.
A retrospective study of patients submitted to arthroplasty in 2010 in one public and two private hospitals in the state of São Paulo [47] , carried out by examining patient records, aimed to compare the therapy for prophylaxis of venous thromboembolism and the costs related to the hospitalization of patients submitted to total knee and hip replacement. Costs were estimated based on the use of health resources during hospitalization and descriptive analysis was performed using frequency and average (standard deviation) according to the type of service (public or private organisation). Prophylaxis of VTE in patients submitted to arthroplasty was found to be more used in private (98%) than in public services (88%), with enoxaparin being the drug most used in both systems. The authors concluded that prevention has a better cost-benefit relation.
Medicare only covers a stay in a specialized nursing centre after total knee replacement if the patient remains at least three days in hospital. Retrospective analysis of 800 procedures showed that the time in hospital was generally longer than three days, which implies increased costs. For patients with private insurance, this period was 2, 3 days, whereas for Medicare beneficiaries it was 3, 02 [3, 21] aimed to determine whether, due to an older population, rotator cuff surgery was more expensive in patients with Medicare insurance than in those covered by other insurers, with operation time, number and cost of implants, hospital refunding, surgeon refunding and the type of insurance being determined from charging records and operational reports. Comparing Medicare vs non-Medicare, no significant difference was found in the number of suture anchors used, in the cost of the implant, in the length of the surgery or in the total cost of the arthroscopic repair of the rotator cuff. In relation to refunding, this was significantly less for Medicare, resulting in an average deficit per case of US $ 263, 54 between charge and reimbursement. In 2019, [10] attempted to quantify the additional costs associated with each cause of readmission after total replacement of the primary joint, where the average costs of readmission to the hospital, post-acute care general costs and general costs of episodes of 90 days between the reasons for readmission were compared, observing a significant increase in costs due to readmissions for surgical reappraisal. [8] aimed to demonstrate the impacts of local infiltration analgesia on the length of stay and cost economics for knee and hip replacement. In a prospective study, the variables included in the comparison were the length of hospitalization, the percentage of patients transferred to rehabilitation or intensive therapy unit (ITU), readmitted within 30 days and the average cost of separation. The wide-ranging approach of the LIA and rapid recuperation mean patients spend less time in hospital, with less incidence of rehabilitation and a consequent reduction in health expenditure.
3.2.2 Mixed Costing: The American Medical Association (AMA) identified a growing tendency for surgical sub-specialists to work in hospitals rather than working independently as private doctors, with significant implications for local economies. [49] State that co-management joint-ventures are considered a better model to align surgeons and hospitals and attain cost-effective targets and improved quality. [50] investigated the effect on the productivity of operating theatres in Independent Centres of Sector Treatment compared to those of Acute Hospital Trusts in the United Kingdom, finding that implementation of Independent Centres of Sector Treatment had a negative effect on departmental efficiency, as there was a 50% reduction in the number of patients treated, as well as triggering a sharp fall in financial productivity, a combined reduction in the potential productivity of £ 128.677 in 3 months or £ 514.708 in 1 year.
3.2.3 Activity-Based Costing (ABC): Recent efforts to reform the area of health, focused on the reward value, rather than volume, has made it important for orthopaedic surgeons to form partnerships and align with their hospitals. [2] Courtney et al. (2018) report experiences in aligning clinical and financial incentives in 6 health systems in the same geographical area of the USA, concluding that large groups of private consultants can successfully align clinical and financial incentives with health systems to provide quality joint replacement treatment at a lower cost.
3.3 Costs for decision-making and controls
Regarding the set of organisations’ costs for controls and decision-making, various studies refer to managerial methods or tools [77-80], which are extremely important for better business management in problem-solving, increased income, reduced expenditure and innovation. In orthopaedics, studies focusing on controls and decision-making examine procedures such as nerve grafting [15], shoulder replacement [18], complete knee replacement [6], internal setting of open reduction ankle fracture [41] and various other operations [60]. [15] aimed to give an estimate of the national incidence of brachial plexus injury treated surgically in the USA and also determine whether changes occurred over time using data from the National Health Interview Survey. A total of 966 patients treated surgically showed the average annual incidence of treated injury in patients with private insurance was 0,64 per 100.000, and when extrapolated to all tax-payers, the average annual incidence was 0,89 per 100.000 people (variation from 0,53 to 1,47), showing increased incidence over time. Time in the operating theatre is an important cost for the health system. The study by [18] analysed operating theatre efficiency in a hospital specializing in orthopaedics and a tertiary centre of reference, finding that despite similar patient populations and complexity of cases, the efficiency of the hospital operating theatre was greater than that in the tertiary centre of reference.
[6] Reported the cost-benefit relation of implementing a private contract model to address alternative goals of maximum waiting time for publicly-financed patients submitted to surgery. A linked decision tree and a Markov cohort model were developed completed and validated using secondary sources of information to represent the paths, costs and years of life adjusted to quality obtained by non-urgent patients with alternative waiting times for total knee replacement. They concluded that new models of assistance can inform new models of financing to support that investment and reduce the price of new technology, leading to more efficient and sustainable, publicly-financed health systems. [41] Sought to characterise the economic impact of routine hospitalization for ankle fractures, due to them being prevalent traumatic orthopaedic injuries, and compared treatment in hospitals and out-patient surgery. They concluded that nationally, annual hospitalization of patients represented US $ 796.033.050 in reimbursements, whereas out-patient surgery would be associated with US $ 419.327.612 for treatment of the same ankle fractures. In the USA, there was resistance to covering under-compensated night-time and high-risk calls by orthopaedic specialists interested in developing non-trauma practices. [60] Aimed to demonstrate the financial impact of adding an orthopaedic trauma surgeon dedicated to a private group practice to a community trauma system. Results were analysed, such as the mix of payers, charge rates, balance time, days off, days on-call, nights worked, long-lasting medical equipment and X-ray reimbursement, finding that the cost of hiring the trauma surgeon, although significant, was recuperated after 6 months.
3.4 Elements of strategic cost management
In the area of management, analysis of the effectiveness of operations generally accounts for the greatest number of studies [81-84], reflecting the benefits of organising the right actions carried out correctly, resulting in gains in competitiveness in relation to competitors. Investigations analysing the compensation obtained by management through Diagnosis-Related Groups (DRG) have increased and demonstrate that the classification system relating the types of patients treated by the hospital, with the resources consumed during their hospitalization, creating patient categories that are similar in their clinical characteristics and consumption of resources, is increasingly implemented by national health systems [85-88]. In this study, the most common strategic cost management tool was statistical analysis, in 28 articles, followed by analyses based on Diagnosis-Related Groups (DRG), indices and scores (5 studies), determination of cost-effectiveness, analysis of competitors, value chain and descriptive studies (3 articles) and one study about the cost of quality and web-based searches.
3.4.1 Statistical analyses: Eighteen studies of arthroplasty (hip, knee, shoulder and ankle) use statistical analyses as elements of cost management. (Table 4) presents the aims of those studies and a brief summary of the conclusions.
|
Author (year) |
Aim of the research |
Results/ Conclusions |
|
Ackerman et al. (2020) [30] |
Quantify the probability of hip replacement surgery in the population up to 15 years after sporting injuries. |
During the five-year period of study, 368 cases resulted in hip surgery. Among the main types of hip or thigh injuries, femur fractures and hip dislocations were significantly associated with hip replacement. |
|
Garriga et al. (2019)[5] |
Assess the variation in patients’ results and costs for primary replacement of the hip and knee in English health regions and identify whether patient, surgery or hospital factors are associated with that variation. |
The models indicate that a greater volume of surgery per surgeon and hospital in private hospitals was associated with better results for patients, which can be explained by the change in the combination of cases of public hospitals that deal with a growing number of patients. A larger proportion of less experienced doctors was associated with worse results. This variation was observed geographically. |
|
Slover et al. (2019) [32] |
Verify the factors that determine patients’ hospital change behaviour when they seek a second complete joint replacement. |
Fifteen percent of patients changed hospital for the second complete joint replacement in the 6-year period of study. Those with Medicare or who had surgery in the alternative joint on the second occasion were more likely to change hospital, as well as those waiting more time between operations and those living in a rural area. |
|
Yayac et al. (2019) [31] |
Determine whether patients submitted to conversion of a previous surgery in total knee arthroplasty (TKA) have increased costs compared to primary patients. |
Of the 3.999 primary procedures of total knee arthroplasty, 948 patients (23%) were submitted to conversion. Conversion was associated with a higher cost of post-acute care in patients with commercial insurance (US $ 4714 vs US $ 3759, P = 0,034). Among Medicare beneficiaries, previous reconstruction of the ligament was associated with increased costs of post-acute care (increase of US $ 1917, P = 0,036), whereas previous setting of the fracture came close to statistical significance (increase of US $ 2402, P = 0,055). Conversion of a previous knee operation in TKA is associated with increased costs of post-acute care in 90 days and in the use of resources, particularly previous open procedures. |
|
Boylan et al. (2018) [36] |
Determine the adhesion to robotic technology and computer assistance among orthopaedic surgeons. |
Technological assistance was more common in knee (7,3%) than in hip (1,9%) (P <0,001) replacement. Technology was more likely to be used in patients with private insurance (5,9%) compared to Medicare (4,7%, P <0,001) or Medicaid (2,2%, P <0,001). Technological assistance has been used increasingly by orthopaedic surgeons for hip and knee replacement, but adoption has not been uniform. |
|
Odum et al. (2018) [35] |
Assess the implementation of retrospective payment model for an episode of complete shoulder replacement to determine the value of the episode of this type of arthroplasty in a private consultancy. |
Use of the hospitalized patient in rehabilitation and installation of specialized nursing, and the rate of readmission after 90 days diminished significantly. As a result, it was possible to control post-acute expenditure, which resulted in lowering the costs of carrying out total shoulder replacement. |
|
Roche et al. (2018) [38] |
Assess the impact of different levels of obesity on complete primary knee replacement and review, specifically: incidence and tendencies over time; annual growth rate; and admission costs. |
The number of obese patients receiving complete knee replacement is increasing all the time. The cost of treating obese patients increases as the body mass index deviates from normal, as well as the incidence of review surgery. Therefore, surgeons must be active in advising patients about weight optimization as part of the standard pre-operation service. |
|
Tedesco et al. (2018) [13] |
Analyse the impact of forms of post-acute rehabilitation on mortality and readmission in elderly patients submitted to hip fracture surgery |
Intensive rehabilitation in hospital was significantly associated with a lower risk of mortality compared to rehabilitation by private rehabilitation facilities for hospitalized patients and those without rehabilitation. |
|
Arshi et al. (2017) [20] |
Determine tendencies and rates of complications associated with out-patient total knee replacement compared to surgery in hospital. |
With the potential to minimize the cost of arthroplasty in healthy patients, out-patient TKR is an increasingly popular option. National data from a private insurance databank demonstrated a higher risk of peri-operative surgical and medical complications, including the lack of components, infection in the place of surgery, rigidity of the knee and deep vein thrombosis. |
|
Naylor et al. (2017) [14] |
Compare the effectiveness of rehabilitation after surgery in models with or without a component of hospital rehabilitation. |
Forms of rehabilitation that incorporated hospital rehabilitation did not achieve better specific results of the joint or health scores than alternatives not including hospital rehabilitation. |
|
Kurtz et al. (2016) [45] |
Verify how the number of cases, the mix of payers and the costs of arthroplasty hospitalization changed after introduction of the health insurance reform. |
There was a 59% increase in total hip replacement and 80% in total knee replacement in the period from 2002 to 2011 in Massachusetts. There was a similar trend the United States as a whole. During the period of health insurance reform in Massachusetts there was a greater proportion of patients dealt with by Medicaid, Commonwealth Care or Health Safety Net in both procedures. Until 2011, universal health insurance in Massachusetts covered 2,45% of primary total hip replacement and 2,77% of primary total knee replacement. Medicaid’s coverage in Massachusetts increased from 3,23% and 3,04% of total hip replacement and total knee replacement in 2002 to 4,06% and 4,34% respectively in 2011. |
|
Zhou et al. (2016) [46] |
Assess hospital demographics, complications and readmission rates of patients after total ankle replacement in academic medical centres in the United States. |
The average length of hospitalization for patients submitted to total ankle replacement was 2,2 ± 1,26 days. The hospital’s average total direct cost was 16.212 ± 7.000 per case, with 49,7% of patients having private insurance. Hospital mortality was under 1% and general complications were 1,4%. Complications after discharge included deep vein thrombosis (2,3%), reoperation (0,7%) and infection (3,2%). There was a readmission rate of 2,7% in the first 30 days after discharge. This shows that total ankle replacement is a relatively safe procedure, with generally low rates of complications. |
|
Saleh et al. (2014) [55] |
Determine trends in the use and results of allogeneic blood transfusion in patients submitted to primary totaç hip replacement in the United States from 2000 to 2009. |
An increased rate of allogeneic blood transfusion in patients submitted to total hip replacement was observed (from 11,8% in 2000 to 19,0. % in 2009). However, this use was associated with an increase in surgical complications and adverse occurrences such as: a longer stay in hospital (0,58 ± 0,02 day; p 0,001), increased costs (US $ 1.731 ± US $ 49 [in US dollars in 2009]; p 0,001), increased discharge rate for one hospital (odds ratio, 1,28; confidence interval of 95%, 1,26 to 1,31) and worse surgical and medical results. Nevertheless, intra-hospital mortality was not affected by allogeneic blood transfusion. |
|
Kurtz et al. (2014) [52] |
Assess the hypothetical role of macroeconomic factors on the past and projected use of primary and reviewed total joint replacement in the United States. |
The rate of growth in joint replacement was not sensitive to the economic crises of the 2000s. Between 2009 and 2010, the total number of procedures increased for primary total hip replacement (6,0%), for primary total knee replacement (6,1%), for reviewed total hip replacement (10,8%) and for reviewed total knee replacement (13,5%). Private health insurance increased as the second most frequent payer of hip and knee replacement in the United States, reimbursing 41,6% of primary total hip replacements, 39,9% of primary total knee replacements, 29,2% of reviewed total hip replacements and 34,0% of reviewed total knee replacements in 2010. Projections of the National Health Expenditure model for primary hip replacement in 2020 were higher than the previously projected model, whereas estimates of the current model for total knee replacement were lower. |
|
Davis et al. (2014) [22] |
Identify specific variables affecting the cost of shoulder replacement. |
Hospital expenditure on shoulder replacement was found to increase from 1993 to 2010, with no differences in hospital rates associated with gender, race and obesity. Post-traumatic and rheumatoid arthritis resulted in increased hospital rates, but osteoarthritis resulted in reduced loads from the baseline. In addition, multiple comorbities resulted in increased hospital rates after shoulder replacement. The west and south of the United States had the highest total rates above the baseline, as well as larger hospitals and private urban hospitals. |
|
Kamath et al. (2013) [57] |
Determine the institutional costs associated with unplanned hip replacement; if the moment of operation (urgent/unplanned versus chosen) influences peri-operative results such as mortality, length of stay or the need for advanced care; what diagnoses are associated with unplanned surgery and which are treated urgently more frequently; if demographics and insurance status differ between types of admission (unplanned versus chosen hip replacement). |
Greater total average costs were observed (24% more) for unplanned hip replacement when compared with planned arthroplasty. The same was found when comparing unplanned with planned hospitalization, since the former led to 67% longer hospitalization and had higher rates of femur fracture, peri-prosthetic fracture, prosthetic infection and prosthetic dislocation. Those results should be taken into consideration in elaborating grouped measures of quality and reimbursement for those procedures. |
|
Voorn et al. (2013) [56] |
Assess the frequency of using measures to economize on blood, stratified by hospital type and environment of orthopaedic departments in the Netherlands. |
The research was concluded in 81 (82%) departments, where an increase in the use of blood economy measures was found, with the techniques of erithropoietin and draining and post-surgery infusion being most used by the departments (68% and 69%, respectively). However, these measuring techniques to economize on blood are not effective in terms of cost. So to reduce costs, it is necessary to stop using those uneconomic blood economy measures. |
|
Baser et al. (2010) [59] |
Assess the impact of post-surgery venous thromboembolism during initial hospitalization for total replacement surgery of the hip or total replacement of the knee. |
It was found that episodes of post-surgery venous thromboembolism occurred in 1,77% of the patients studied, during initial hospitalization. These patients presented higher mortality, bleeding and re-hospitalization; they remained longer in hospital; and incurred higher costs than patients without post-surgery venous thromboembolism. |
Table 4: Studies addressing arthroplasty using statistical analysis as a strategic cost management tool.
Continuing to address studies using statistical analysis, three different studies used various orthopaedic surgeries to determine the effectiveness of payments for improved care where differences in expenditure and the length of patients’ stay were confirmed [40]. The description of the most commonly used databanks for orthopaedic clinical research and comparison of the strengths are weaknesses of each could be confirmed, with Medicare claims being one of the most robust datasets used to carry out orthopaedic research, with more than 45 million beneficiaries (the US government generally uses these data to promote change in health policies). Data of private claims used in orthopaedic research generally include more heterogeneous demographic samples, but allow longitudinal analyses similar to those provided by Medicare claims and databanks such as the USA National Hospitalization Sample provide a wide national sample of hospitalization among all taxpayers and allow analysis of adverse occurrences associated with the use of resources [51]. The third study, involving various types of orthopaedic surgery was made by [54] to investigate patterns of orthopaedic surgeons’ expenditure in the United States and the financial implications of this behaviour, finding that costs of X-rays were US $ 7.536, costs of computerized tomography were US $ 2.340, those of magnetic resonance were US $ 14.975, those of ultrasound were US $ 686, the cost of laboratory examinations was US $ 969, that of specialist referral was US $ 1.389, that of biopsy was US $ 1.314 and hospitalization costs were US $ 6.808. Annual expenditure on orthopaedic surgery was calculated to be US $ 8, 2 billion, representing a significant part of national health expenditure.
Ligament reconstruction was addressed by [16, 39], with the former analysing the individual costs associated with reconstruction of the anterior cruciate ligament, accounting for patient demography, peri-operative decision-making and the location of the surgical procedure (hospital versus out-patient surgery centre), while [39] made an epidemiological costing on the analysis of reconstruction of the anterior cruciate ligament and described the reimbursement patterns of that procedure. Traumatic amputation of digits to examine the tendency of digit joint implant practice was the subject studied by [19], who found that of the 14.872 adult patients with one digit amputated from 2001 to 2014, only 1.670 (11,2%) had implants, although more amputations of a digit were treated by urban university hospitals more likely to implant. Then again, [42] studied the risks of post-surgery complications for treatment of proximal humerus fracture comparing patients treated by Medicaid and a cohort with private insurance, observing that Medicaid patients have a significantly greater risk of certain hospital complications post-surgery and consume more resources after treatment of proximal humerus fracture. [11] State that comparing the cost-benefit relation of different types of surgeries and places of treatment leads to an increase in financial results, but it is necessary to assess rates, expenses, reimbursement and hospital margins with special medical material [17, 44].
3.4.2 Analyses based on Diagnosis-Related Groups (DRGs): DRGs are sets of patients grouped homogeneously in resource consumption, so as to be clinically coherent and mutually exclusive regarding occurrences. Studies such as those by [29, 48] point out hospitals’ gains in efficiency that can alleviate the future pressure of population growth within the area of planned hip surgery, a common procedure for old people with osteoarthrosis. For [12], attention should focus on considering hospital rehabilitation after total hip replacement, which continues to be a low-cost health service option when compared with the average charges of the provider of rehabilitation, around 10 times more for those who received hospital rehabilitation, while [7] indicate that hospitals belonging to doctors are associated with lower average Medicare costs, fewer complications and greater patient satisfaction after arthroplasty than hospitals not belonging to doctors. Making statistical projections of the volumes and rates of procedures carried out favours better resource management [43].
3.4.3 Cost effectiveness, analysis of competitors, value chain, descriptive studies and costs of quality: Recently, cost effectiveness analyses have appeared more frequently in studies on orthopaedics, to assess the variation in hospitalization for orthopaedic injuries according to the type of insurance [33], to determine the patient’s perception of the quality of the hospital or the provider considering that this can affect reimbursement, the patient’s selection of the surgeon and competition in the area of health [1], to map epidemiological statistics on non-traumatic orthopaedic injuries, their rate of variability, distribution by specialization, mortality rate and the economic impact those injuries and their consequences can cause [37] or even to describe current use, by orthopaedic trauma surgeons, of reprocessed external fixators [34].
- Conclusions and Future Agenda
The aim of this research was to classify the studies selected in this systematic review, in the last decade, according to cost management tools, mapping methods of measurement, costs for decision-making and controls and elements of strategic cost management, aiming for greater competitiveness in hospitals and out-patient institutions, and improved performance. Specifically, it confirmed the types of actions being implemented over time to measure the performance of orthopaedic surgical procedures in hospitals and out-patient departments where comparison between study groups using the standard costing method predominates. Relevant information about control and decision-making mechanisms were stratified, using breakeven strategies, contribution margin, decision tree, models and methods and managerial tools aiming to improve (qualitative and financial) performance in health. Concerning the elements of strategic cost management, an expressive tendency towards statistical analysis was observed, with 75, 68% of relative frequency, and analysis of
replacement surgery (hip, knee and shoulder) predominates. Various reasons stimulate these studies and mean researchers prioritize analysis of this type of surgery, due to the greater risk of complications (including a lack of components, infection in the operating theatre, rigidity and deep vein thrombosis, high costs (use of robotics, prostheses and special material, post-surgery rehabilitation), an ageing population and the association of comorbities (obesity, osteoarthritis).
As far as we can see, the absence of an SLR specifically addressing the costs and performance of orthopaedic surgery, an important gap in the literature, was remedied with this study. As suggestions for future research, different specializations and types of orthopaedic surgery should be considered so that new studies can extend the theoretical framework.
Acknowledgements
The author would like to thank to UBI_Santander Totta Scholarship Program.
Interest Conflicts
The author declares that there are no conflicts of interest in the preparation of this article.
References
- Bernstein DN, Mesfin A, Bozic KJ. Total joint arthroplasty quality ratings: How are they similar and how are they different?American Journal of Orthopedics (Belle Mead, N.J.) 47 (2018).
- Courtney PM, West ME, Hozack WJ. Maximizing physician-hospital alignment: Lessons learned from effective models of joint arthroplasty care.Journal of Arthroplasty 33 (2018): 641-1646.
- Narvy SJ, Didinger TC, Lehoang D, et al. Direct cost analysis of outpatient arthroscopic rotator cuff repair in medicare and non-medicare populations.Orthopaedic Journal of Sports Medicine 4 (2016).
- Jimenez A, Kakazu R, Branam B, et al. No Difference in Failure Rates Between Hybrid Grafts Compared with Hamstring Autografts Following ACL Reconstruction. Journal of Orthopaedics and Sports Medicine 1 (2019): 028-036.
- Garriga C, Leal J, Sánchez-Santos MT, et al. Geographical variation in outcomes of primary hip and knee replacement.JAMA Network Open 2 (2019): 1914325.
- Karnon J, Haghighi BM, Sajjad B, et al. Cost-utility analysis of private contracting to reduce public waiting times for joint replacement surgery.International Journal of Technology Assessment in Health Care 34 (2018): 147-155.
- Maxwell Courtney P, Darrith B, Bohl DD, et al. Reconsidering the affordable care act's restrictions on physician-owned hospitals analysis of CMS data on total hip and knee arthroplasty.Journal of Bone and Joint Surgery - American Volume 99 (2017): 1888-1894.
- Nassar I, Fahey J, Mitchell D. Rapid recovery following hip and knee arthroplasty using local infiltration analgesia: Length of stay, rehabilitation protocol and cost savings.ANZ Journal of Surgery (2020).
- RI T-H, Kim H-S, O C-H, et al. Minimally-Invasive Treatment of Multiple Trauma Concomitant with Idiopathic Portal Hypertension (IPH). Journal of Orthopaedics and Sports Medicine 1 (2019): 114-119.
- Phillips JLH, Rondon AJ, Vannello C, et al. How much does a readmission cost the bundle following primary hip and knee arthroplasty?Journal of Arthroplasty 34 (2019): 819-823.
- Schrock JB, Kraeutler MJ, Houck DA, et al. A cost-effectiveness analysis of surgical treatment modalities for chondral lesions of the knee: Microfracture, osteochondral autograft transplantation, and autologous chondrocyte implantation.Orthopaedic Journal of Sports Medicine 5 (2017).
- Naylor JM, Hart A, Mittal R, et al. The effectiveness of inpatient rehabilitation after uncomplicated total hip arthroplasty: A propensity score matched cohort.BMC Musculoskeletal Disorders 19 (2018).
- Tedesco D, Gibertoni D, Rucci P, et al. Impact of rehabilitation on mortality and readmissions after surgery for hip fracture.BMC Health Services Research 18 (2018): 701.
- Naylor JM, Hart A, Mittal R, et al. The value of inpatient rehabilitation after uncomplicated knee arthroplasty: A propensity score analysis.Medical Journal of Australia 207 (2017): 250-255.
- Dy CJ, Peacock K, Olsen MA, et al. Incidence of surgically treated brachial plexus injury in privately insured adults under 65 years of age in the USA.HSS Journal (2020).
- Bokshan SL, Mehta S, DeFroda SF, et al. What are the primary cost drivers of anterior cruciate ligament reconstruction in the United States? A cost-minimization analysis of 14,713 patients.Arthroscopy - Journal of Arthroscopic and Related Surgery 35 (2019): 1576-1581.
- Lyons KW, Klare CM, Kunkel ST, et al. A 5-year review of hospital costs and reimbursement in the surgical management of degenerative spondylolisthesis.International Journal of Spine Surgery 13 (2019): 378-385.
- Padegimas EM, Hendy BA, Chan WW, et al. The effect of an orthopedic specialty hospital on operating room efficiency in shoulder arthroplasty.Journal of Shoulder and Elbow Surgery 28 (2019):15-21.
- Cho HE, Zhong L, Kotsis SV, et al. Finger replantation optimization study (Front): Update on national trends.Journal of Hand Surgery 43 (2018): 903-912.
- Arshi A, Leong NL, D'Oro A, et al. Outpatient total knee arthroplasty is associated with higher risk of perioperative complications.Journal of Bone and Joint Surgery - American Volume 99 (2017): 1978-1986.
- Hernandez VH, Ong A, Post Z, et al. Does the medicare 3-day rule increase length of stay?Journal of Arthroplasty 30 (2015): 34-35.
- Davis DE, Paxton ES, Maltenfort M, et al. Factors affecting hospital charges after total shoulder arthroplasty: An evaluation of the national inpatient sample database.Journal of Shoulder and Elbow Surgery 23 (2014): 1860-1866.
- Neriz L, Núñez A, Ramis F. A cost management model for hospital food and nutrition in a public hospital. BMC Health Services Research 14 (2014).
- Massaro M, Dumay J, Guthrie J. On the shoulders of giants: undertaking a structured literature review in accounting. Accounting, Auditing and Accountability Journal 29 (2016): 767-801.
- Liberati A, Altman DG, Tetzlaff J, et al. The Prisma Statement for Reporting Systematic Review and Meta-Analuses of Studies that Evaluate Health Care Interventions: Explanation and Elaboration. Polos Medicine 6 (2009):1000 100.
- Transfield D, Denyer D, Palminder S. Towards a methodology for developing evidence informed management knowledge by means of systematic review. Journal British Academy of Management 14 (2003): 207-222.
- Popay J, Roberts H, Sowden A, et al. Developing guidance on the conduct of narrative synthesis in systematic reviews. J Epidemiol Comm Health 59 (2005): 7.
- Moyson S, Raaphorst N, Groeneveld S, et al. Organizational socialization in public administration research: A systematic review and directions for future research. American Review of Public Administration 48 (2018): 610-627.
- Mealy A, Sorensen J. Effects of an aging population on hospital costs related to elective hip replacements.Public Health 180 (2020): 10-16.
- Ackerman IN, Bohensky MA, Kemp JL, et al. Quantifying the likelihood and costs of hip replacement surgery after sports injury: A population-level analysis.Physical Therapy in Sport, 41 (2020): 9-15.
- Yayac MF, Harrer SL, Deirmengian GK, et al. Conversion total knee arthroplasty is associated with increased post-acute care costs.Journal of Arthroplasty 34 (2019): 2855-2860.
- Slover J, Lavery JA, Toombs C, et al. Factors associated with utilizing the same hospital for subsequent total hip or knee arthroplasty in osteoarthritis patients. Bulletin of the Hospital for Joint Diseases 77 (2019): 64-170.
- Boylan MR, Suchman KI, Bosco JA, et al. Tibial shaft fractures in workers compensation and no-fault insurance: Is there a difference in resource utilization? Bulletin of the Hospital for Joint Diseases 77 (2019): 200-205.
- Thamyongkit S, Bachabi M, Thompson JM, et al. Use of reprocessed external fixators in orthopaedic surgery: A survey of 243 orthopaedic trauma surgeons.Patient Safety in Surgery 12 (2018).
- Odum SM, Hamid N, Van Doren BA, et al. Is there value in retrospective 90-day bundle payment models for shoulder arthroplasty procedures?Journal of Shoulder and Elbow Surgery 27 (2018): 149-154.
- Boylan M, Suchman K, Vigdorchik J, et al. Technology-assisted hip and knee arthroplasties: An analysis of utilization trends.Journal of Arthroplasty 33 (2018): 1019-1023.
- De Paiva Luciano A, Do Carmo Almeida TC, Dos Santos Figueiredo FW, et al. Study of the evolution and variability of nontraumatic orthopedic surgeries in brazil-9 years of follow-up A database study.Medicine (United States) 97 (2018).
- Roche M, Law TY, Kurowicki J, et al. Effect of obesity on total knee arthroplasty costs and revision rate.Journal of Knee Surgery 31 (2018): 38-42.
- Rosas S, Kurowicki J, Hughes M, et al. National age and gender-specific costs in anterior cruciate ligament reconstruction by a single nationwide private payer. Surgical Technology International 31 (2017): 285-293.
- Curtin BM, Russell RD, Odum SM. Bundled payments for care improvement: Boom or bust?Journal of Arthroplasty 32 (2017): 2931-2934.
- Stull JD, Bhat SB, Kane JM, et al. Economic burden of inpatient admission of ankle fractures.Foot and Ankle International 38 (2017): 997-1004.
- Sabesan VJ, Petersen-Fitts G, Lombardo D, et al. Medicaid payer status is linked to increased rates of complications after treatment of proximal humerus fractures.Journal of Shoulder and Elbow Surgery 26 (2017): 948-953.
- Longo UG, Salvatore G, Rizzello G, et al. The burden of rotator cuff surgery in Italy: A nationwide registry study.Archives of Orthopaedic and Trauma Surgery 137 (2017): 217-224.
- Thorpe A, Hurworth M, O'Sullivan P, et al. Rising trends in surgery for rotator cuff disease in western australia.ANZ Journal of Surgery 86 (2016): 801-804.
- Kurtz SM, Lau E, Ong KL, et al. Universal health insurance coverage in Massachusetts did not change the trajectory of arthroplasty use or costs.Clinical Orthopaedics and Related Research 474 (2016): 1090-1098.
- Zhou H, Yakavonis M, Shaw JJ, et al. In-patient trends and complications after total ankle arthroplasty in the United States.Orthopedics 39 (2016): 74-79.
- Cortada AP, Silva TG, Silva AC, et al. Comparison of thromboprophylaxis patterns in arthroplasty in public and private hospitals.Einstein (São Paulo, Brazil) 13 (2015): 410-416.
- Maravic M, Beaudreuil J. Impact on costs of switching one-ray aponeurectomy to percutaneous needle aponeurotomy in dupuytren's disease: A model analysis.Joint Bone Spine 82 (2015): 264-266.
- Iorio R, Fehring T, York S, et al. Economic impact of orthopedic adult reconstruction office practice: The implications of hospital employment models on local economies.Journal of Arthroplasty 30 (2015): 923-930.
- Vanhegan I, Hakmi A, De Roeck N, et al. Effect of an independent-sector treatment centre on provision of elective orthopaedic surgery in east and north hertfordshire.Annals of the Royal College of Surgeons of England 97 (2015): 519-525.
- Pugely AJ, Martin CT, Harwood J, et al. Database and registry research in orthopaedic surgery part I: Claims-based data.Journal of Bone and Joint Surgery - American Volume 97 (2014): 1278-1287.
- Kurtz SM, Ong KL, Lau E, et al. Impact of the economic downturn on total joint replacement demand in the United States: Updated projections to 2021.Journal of Bone and Joint Surgery - American Volume 96 (2014): 624-630.
- Raikin SM, Rasouli MR, Espandar R, et al. Trends in treatment of advanced ankle arthropathy by total ankle replacement or ankle fusion.Foot and Ankle International 35 (2014): 216-224.
- Sathiyakumar V, Jahangir AA, Mir HR, et al. Patterns of costs and spending among orthopedic surgeons across the United States: A national survey. American Journal of Orthopedics (Belle Mead, N.J.) 43 (2014): 7-13.
- Saleh A, Small T, Pillai ALPC, et al. Allogenic blood transfusion following total hip arthroplasty: Results from the nationwide inpatient sample, 2000 to 2009.Journal of Bone and Joint Surgery - American Volume 96 (2014): 155.
- Voorn VMA, Marang-Van De Mheen PJ, Wentink MM, et al. Frequent use of blood-saving measures in elective orthopaedic surgery: A 2012 dutch blood management survey.BMC Musculoskeletal Disorders 14 (2013).
- Kamath AF, Austin DC, Derman PB, et al. Unplanned hip arthroplasty imposes clinical and cost burdens on treating institutions.Clinical Orthopaedics and Related Research 471 (2013): 4012-4019.
- Mehrotra A, Sloss EM, Hussey PS, et al. Evaluation of centers of excellence program for knee and hip replacement.Medical Care 51 (2013): 28-36.
- Baser O, Supina D, Sengupta N, et al. Impact of postoperative venous thromboembolism on medicare recipients undergoing total hip replacement or total knee replacement surgery.American Journal of Health-System Pharmacy 67 (2010): 438-1445.
- Althausen PL, Davis L, Boyden E, et al. Financial impact of a dedicated orthopaedic traumatologist on a private group practice.Journal of Orthopaedic Trauma 24 (2010): 350-354.
- Burrel G, Morgan G. Sociological paradigms and organisational analyses. London: Heinemann Educational Books (1979).
- Kempeneers N, Van Aken L, Van Herck G. Toward more economic rationality in hospital cost accounting. [Naar Een Meer Economische Rationaliteit In De Verzorgingssector] Acta Hospitalia 35 (1995): 35-41+115.
- Waters H, Abdallah H, Santillán D. Application of activity-based costing (ABC) for a peruvian NGO healthcare provider.International Journal of Health Planning and Management 16 (2001): 3-18.
- Dugel PU, Tong KB. Development of an activity-based costing model to evaluate physician office practice profitability.Ophthalmology 118 (2011): 203-208.
- Bayati M, Ahari AM, Badakhshan A, et al. Cost analysis of MRI services in iran: An application of activity based costing technique.Iranian Journal of Radiology 12 (2015).
- Afzali A, Ogden K, Friedman ML, et al. Costs of providing infusion therapy for patients with inflammatory bowel disease in a hospital-based infusion center setting. Journal of Medical Economics 20 (2017): 409-422.
- Bauer-Nilsen K, Hill C, Trifiletti DM, et al. Evaluation of delivery costs for external beam radiation therapy and brachytherapy for locally advanced cervical cancer using time-driven activity-based costing. International Journal of Radiation Oncology Biology Physics 100 (2018): 88-94.
- Rinaldo JA, McCubbrey DJ, Shryock JR. The care monitoring, cost forecasting and cost monitoring system. Journal of Clinical Computing 9 (1981): 72-85.
- Orloff TM, Littell CL, Clune C, et al. Hospital cost accounting: Who’s doing what and why.Health Care Management Review 15 (1990): 73-78.
- Levy E, Gabriel S, Dinet J. The Comparative Medical Costs of Atherothrombotic Disease in European Countries. Pharmaco Economics 21 (2003): 651-659.
- Bermudez-Tamayo C, Johri M, Perez-Ramos FJ, et al. Evaluation of quality improvement for cesarean sectionscaesarean section programmes through mixed methods. Implementation Science 9 (2014):182.
- Bennett JP. Standard cost systems lead to efficiency and profitability. PubMed 39 (1985): 46-52.
- Cooper JC, Suver JD. Product line cost estimation: A standard cost approach. Healthcare Financial Management: Journal of the Healthcare Financial Management Association 42 (1988).
- Colin X, Lafuma A, Costagliola D, et al. The Cost of Managing HIV Infection in Highly Treatment-Experienced, HIV-Infected Adults in France. Pharmaco Economics 28 (2010): 59-68.
- Cyganska M. Analysis of High Cost Outliers in a Polish Reference Hospital. E and M Ekonomie a Management 4 (2017): 59-69.
- Tran PTH, Vo TQ, Huynh DTP, et al. Medical services for a provincial hospital in vietnam: Cost analysis for data management.Journal of Clinical and Diagnostic Research 12 (2018): 33- 37.
- Powe NR, Weiner JP, Starfield B, et al. Systemwide Provider Performance in a Medicaid Program: Profiling the Care of Patients with Chronic Illnesses. Medical Care 34 (1996): 798-810.
- Oostenbrink R, Oostenbrink JB, Moons KGM, et al. Application of a Diagnostic Decision Rule in Children with Meningeal Sins: A Cost-minimization Study. International Journal of Technology Assessment in Health Care 19 (2003): 698-704.
- Harper PR, Powell NH, Williams JE. Modelling the size and skill-mix of hospital nursing teams. Journal of the Operational Research Society 61 (2010): 768-779.
- Kim E, Kwon HY, Baek SH, et al. Medical costs in patients with heart failure after acute heart failure events: one-year follow-up study. Journal of Medical Economics 21 (2018): 288-293.
- Bertapelle MP, Vottero M, Popolo GD, et al. Sacral neuromodulation and botulinum toxin A for refractory idiopathic overactive bladder: A cost-utility analysis in the perspective of italian healthcare system.World Journal of Urology 33 (2015): 1109-1117.
- Salas JD, Lima AOD, Balbino JE, et al. An economic evaluation of two interventions for the prevention of post-surgical infections in cardiac surgery. Revista de Calidad Asistencial 31 (2016): 27-33.
- Espinoza AV, Devos S, van Hooff RJ, et al. Time Gain Needed for In-Ambulance Telemedicine: Cost-Utility Model. JMIR Mhealth and Uhealth 5 (2017): 11.
- Mortuaire G, Theis D, Fackeure R, et al. Cost-effectiveness assessment in outpatient sinonasal surgery.European Annals of Otorhinolaryngology, Head and Neck Diseases 135 (2018): 11-15.
- Vogl M. Improving patient-level costing in the english and the german 'DRG' system.Health Policy 109 (2013): 290-300.
- Eti S, O’Mahony S, McHugh M, et al. Outcomes of the Acute Palliative Care Unit in an Academic Medical Center. American Journal of Hospice and Palliative Medicine 31 (2013): 380-384.
- Hidalgo-Vega Á, Askari E, Vidal R, et al. Direct vitamin k antagonist anticoagulant treatment health care costs in patients with non-valvular atrial fibrillation. BMC Health Services Research 14 (2014).
- Russell H, Street A, Ho V. How Well Do All Patient Refined–Diagnosis-Related Groups Explain Costs of Pediatric Cancer Chemotherapy Admissions in the United States? Journal of Oncology Practice 12 (2016): 564-575.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 73.64%
Acceptance Rate: 73.64%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 