Laser Speckle Contrast Imaging, a Feasible Device for Monitoring Postoperative Microcirculation: A Case Report
Muhsin Billah Bin Khashru, Zeng-tao Wang*, Bilkis Akthar
Department of Hand and Foot Surgery, Shandong Provincial Hospital affiliated to Shandong University, Shandong, Jinan, China
*Corresponding Author: Zeng-tao Wang, Department of Hand and Foot Surgery, Shandong Provincial Hospital affiliated to Shandong University, Shandong, Jinan, China
Received: 15 January 2020; Accepted: 21 January 2020; Published: 30 January 2020
Article Information
Citation: Muhsin Billah Bin Khashru, Zeng-tao Wang, Bilkis Akthar. Laser Speckle Contrast Imaging, a feasible device for monitoring postoperative microcirculation: A case report. Journal of Orthopaedics and Sports Medicine 2 (2020): 18-23.
View / Download Pdf Share at FacebookAbstract
Ensuring uninterrupted microcirculation is a fundamental requirement for reconstructive flap surgeries, and tissue viability can be determined by measuring the perfusion to it. There are several laser-based optical imaging procedures have been established to analyze tissue perfusion. Laser speckle contrast imaging (LSCI) is one of them comprising a camera and laser diode that produces a near-infrared laser beam and illuminate the tissue. Over the illuminated area, a scattered speckle pattern is created and measures the perfusion rate. Here we report a case in which post-operative perfusion monitoring of tissue flap was done using the LSCI. Minimal invasive, easy to operate, real-time perfusion measurement, and rapid response to vascular occlusion makes LSCI a prevalent device for measuring pre-, peri- and post-operative microcirculation. However, broaden clinical studies should be necessary to confirm its effectiveness. According to our studies, we found LSCI to be a potential monitoring device.
Keywords
Laser speckle contrast imaging; Microcirculation; Tissue flap; Reconstructive surgery
Hand and Foot articles Hand and Foot Research articles Hand and Foot review articles Hand and Foot PubMed articles Hand and Foot PubMed Central articles Hand and Foot 2023 articles Hand and Foot 2024 articles Hand and Foot Scopus articles Hand and Foot impact factor journals Hand and Foot Scopus journals Hand and Foot PubMed journals Hand and Foot medical journals Hand and Foot free journals Hand and Foot best journals Hand and Foot top journals Hand and Foot free medical journals Hand and Foot famous journals Hand and Foot Google Scholar indexed journals Surgery articles Surgery Research articles Surgery review articles Surgery PubMed articles Surgery PubMed Central articles Surgery 2023 articles Surgery 2024 articles Surgery Scopus articles Surgery impact factor journals Surgery Scopus journals Surgery PubMed journals Surgery medical journals Surgery free journals Surgery best journals Surgery top journals Surgery free medical journals Surgery famous journals Surgery Google Scholar indexed journals Microsurgeons articles Microsurgeons Research articles Microsurgeons review articles Microsurgeons PubMed articles Microsurgeons PubMed Central articles Microsurgeons 2023 articles Microsurgeons 2024 articles Microsurgeons Scopus articles Microsurgeons impact factor journals Microsurgeons Scopus journals Microsurgeons PubMed journals Microsurgeons medical journals Microsurgeons free journals Microsurgeons best journals Microsurgeons top journals Microsurgeons free medical journals Microsurgeons famous journals Microsurgeons Google Scholar indexed journals Flap reconstruction articles Flap reconstruction Research articles Flap reconstruction review articles Flap reconstruction PubMed articles Flap reconstruction PubMed Central articles Flap reconstruction 2023 articles Flap reconstruction 2024 articles Flap reconstruction Scopus articles Flap reconstruction impact factor journals Flap reconstruction Scopus journals Flap reconstruction PubMed journals Flap reconstruction medical journals Flap reconstruction free journals Flap reconstruction best journals Flap reconstruction top journals Flap reconstruction free medical journals Flap reconstruction famous journals Flap reconstruction Google Scholar indexed journals Laser speckle contrast imaging articles Laser speckle contrast imaging Research articles Laser speckle contrast imaging review articles Laser speckle contrast imaging PubMed articles Laser speckle contrast imaging PubMed Central articles Laser speckle contrast imaging 2023 articles Laser speckle contrast imaging 2024 articles Laser speckle contrast imaging Scopus articles Laser speckle contrast imaging impact factor journals Laser speckle contrast imaging Scopus journals Laser speckle contrast imaging PubMed journals Laser speckle contrast imaging medical journals Laser speckle contrast imaging free journals Laser speckle contrast imaging best journals Laser speckle contrast imaging top journals Laser speckle contrast imaging free medical journals Laser speckle contrast imaging famous journals Laser speckle contrast imaging Google Scholar indexed journals Fingers articles Fingers Research articles Fingers review articles Fingers PubMed articles Fingers PubMed Central articles Fingers 2023 articles Fingers 2024 articles Fingers Scopus articles Fingers impact factor journals Fingers Scopus journals Fingers PubMed journals Fingers medical journals Fingers free journals Fingers best journals Fingers top journals Fingers free medical journals Fingers famous journals Fingers Google Scholar indexed journals Distal phalanx articles Distal phalanx Research articles Distal phalanx review articles Distal phalanx PubMed articles Distal phalanx PubMed Central articles Distal phalanx 2023 articles Distal phalanx 2024 articles Distal phalanx Scopus articles Distal phalanx impact factor journals Distal phalanx Scopus journals Distal phalanx PubMed journals Distal phalanx medical journals Distal phalanx free journals Distal phalanx best journals Distal phalanx top journals Distal phalanx free medical journals Distal phalanx famous journals Distal phalanx Google Scholar indexed journals Tissue flap articles Tissue flap Research articles Tissue flap review articles Tissue flap PubMed articles Tissue flap PubMed Central articles Tissue flap 2023 articles Tissue flap 2024 articles Tissue flap Scopus articles Tissue flap impact factor journals Tissue flap Scopus journals Tissue flap PubMed journals Tissue flap medical journals Tissue flap free journals Tissue flap best journals Tissue flap top journals Tissue flap free medical journals Tissue flap famous journals Tissue flap Google Scholar indexed journals Arteries articles Arteries Research articles Arteries review articles Arteries PubMed articles Arteries PubMed Central articles Arteries 2023 articles Arteries 2024 articles Arteries Scopus articles Arteries impact factor journals Arteries Scopus journals Arteries PubMed journals Arteries medical journals Arteries free journals Arteries best journals Arteries top journals Arteries free medical journals Arteries famous journals Arteries Google Scholar indexed journals Veins articles Veins Research articles Veins review articles Veins PubMed articles Veins PubMed Central articles Veins 2023 articles Veins 2024 articles Veins Scopus articles Veins impact factor journals Veins Scopus journals Veins PubMed journals Veins medical journals Veins free journals Veins best journals Veins top journals Veins free medical journals Veins famous journals Veins Google Scholar indexed journals
Article Details
1. Introduction
Free flap reconstructive surgery is a practical challenge for microsurgeons. For successful free flap reconstruction, it is essential to evaluate the reconstructed area perfusion for the prompt identification and revision of compromised vascular supply. Nevertheless, it has been not very easy to find a feasible way to evaluate the transferred tissue flap with higher sensitivity and specificity. Vascular compromise classically occurs within the post-operative first day, [1] within that time, it is essential for the surgeons to follow up the consequence of the reconstructed flap or replanted fingers [2]. Laser speckle contrast imaging (LSCI) refers to a photography based method that comprises a camera and a laser diode. The laser diode generates a divergent 785-nm laser light, illuminates an area of tissue, and scrutinizes the interference pattern of the scattered light from the tissue. The most recent study showed the sensitive and reproducible measurements of a cranial gluteal artery perforator flap microcirculation in a model of porcine flap observed by LSCI [7]. Here, we report a case in which post-operative monitoring of an Anterolateral thigh flap (ALT) microcirculation which was used to cover a wound of the hand using LSCI that showed a feasible result.
2. Case Report
A 22-year-old male suffered from the amputation of the distal phalanx of his left thumb and middle and distal phalanges of his index finger by a compression injury involving a grinding machine at his workplace. The primary debridement procedure was performed on the same night as an emergency surgery under a brachial plexus block. The wound was primarily covered by Vacuum Sealing Drainage (VSD) and left it for the second time surgery. On the second surgery, the recipient veins were identified preoperatively by a handheld Doppler. One arteries, one vein, and one nerve were anastomosed. (Figure 1) shows the perioperative photos of second surgery. Post-operatively, the microcirculation of the reconstructed area was monitored using LSCI straightaway after the surgery, and post-operative morning was done in the temperature-controlled ward every hour throughout the day after the surgery for seven days.
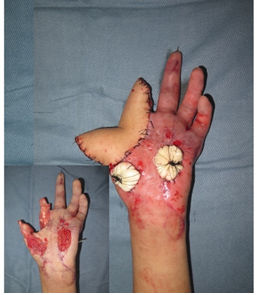
Figure 1: Shows the perioperative pictures of the 2nd surgery. The smaller picture on the left side shows the condition after debridement and the bigger picture on the right shows the condition after the coverage of the wound with an ALT flap. The two round things on the palm are made of sterile gauze covered by paraffin gauze to create pressure on the skin grafted area.
3. Method
A Laser Speckle Contrast imaging device (PeriCam PSI System, Perimed AB, Järfälla, Sweden) LSCI was recruited in this study, which measures perfusion illuminating the tissue with an invisible near infra-red laser (785 nm). It generates a speckle pattern over the region of interest (ROI). The principle of the measurement technique of the PeriCam PSI System is done by an advanced CCD camera that records these changes in the speckle pattern at a speed of up to 113 images per second and up to 1386 x 1036 pixels per image [4]. We placed the laser head approximately 15-20 CM above the reconstructed area (Figure 2), and the image acquisition rate was set to 10 images per second. The principle of LSCI has been explained previously in other literature [5].
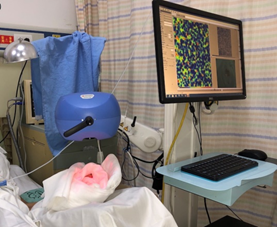
Figure 2: Post-operative evaluation of microcirculation in a temperature-controlled ward.
The camera was kept 15-20 cm over the patient’s hand as literature was reported that the space kept between the laser and the patient does not influence the LSCI value [6]. During every measurement, the data from 600 consecutive images were calculated. LSCI images were processed using their own system analyzing software program named PSIWin; Perimed AB. 2 region of interests (ROIs) were chosen to differentiate the perfusion, and then the perfusion values were collected hourly and later the mean was calculated offline on excel spreadsheets (Excel 2016 V3 ®, Microsoft USA).
4. Discussion
The perfusion in the reconstructed area and the average perfusion of the palm immediately after the operation was 37.6 and 75.2 perfusion units, correspondingly. The change in the skin perfusion post-operatively was measured by LSCI is presented in (Figure 3). The post-operative perfusion values were different, and the perfusion observed by LSCI was stable and uprising day by day during the observation period. In the end, the transferred tissue flap survived successfully without any further complication (Figure 4). In the setting of transferring tissue flap, even though several arteries and veins are being anastomosed, pos-toperative monitoring of the tissue flap is still essential as there are some possibilities of tissue morbidity in the distal portion of the flap. Zötterman et al. did one study on the porcine model to predict flap necrosis and found partial necrosis to happen in the distal portion of the flap with a perfusion value below 20 PU [7].
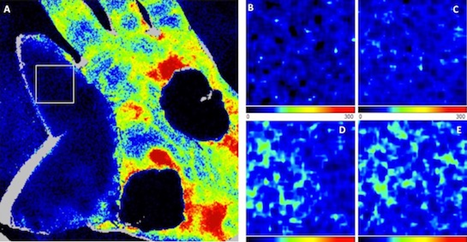
Figure 3: Represents LSCI image of the hand showing the typical perfusion in both tissue flap and the palm on post-operative day 1 (A) The white box on image (A) represents the chosen ROI, as it was the distal portion of the flap which is considered under danger; (B) Shows development in perfusion on the third day followed by; (C) On fifth day; (D) On sixth day and; (E) On seventh day. The two dark round things are made of sterile gauze to create pressure on skin grafted area.
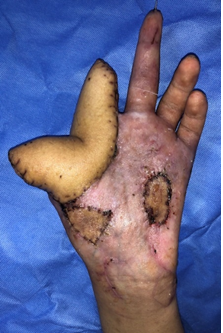
Figure 4: Shows the outcome of post-operative day 30. The flap was successfully viable without any partial necrosis.
However, surgeons till now rely significantly on clinical outcomes, for example, color changes on the flap surface, slow capillary refill, temperature changes, and very commonly, the pinprick test. By pinpricking the test, they determine the condition of the flap observing the color of the blood and the speed of bleeding. There are several advantages of post-operative evaluation using LSCI. First of all, this technique is risk-free to the patients and the flap. A laser-based approach assists to perform microcirculation monitoring being noninvasive to the patient. Additionally, measuring tissue perfusion in real-time allows us to see the rapid reaction to the occlusion of both artery or vein [3]. Finally, we can measure skin perfusion using LSCI in a quantitative way. The quantification of the skin perfusion is easier to calculate offline to determine the consequence of the flap in its different areas. In our current case, although the perfusion of the transferred tissue flap was notably lower than that of the unaffected hand, however, the good thing was the continuous rise in the perfusion value in the ward afterward. (Figure 5) represents the mean perfusion change throughout the day till post-operative day five. Furthermore, LSCI can help us detect flap condition and take necessary steps earlier as it takes a while to detect the changes in skin color visually (Figure 6).
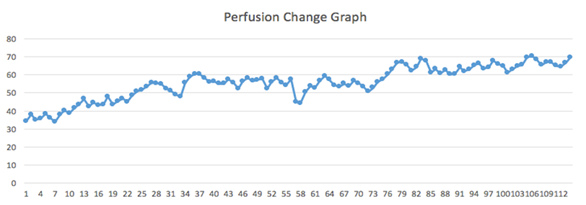
Figure 5: Shows post-operaive evaluation of microcirculation. We measured the perfusion data every hour till day 5.
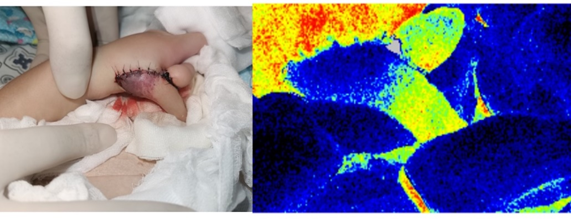
Figure 6: Shows the differences of LSCI image between a healthy and compromised blood flow area on a pedicled groin flap.
5. Conclusion
To our knowledge, this is the freshest report in which successful flap reconstructive surgery was performed and monitored post-operatively using LSCI in the human patient. Nevertheless, more clinical researches are necessary to confirm its potency in different kinds of conditions; to our understanding, LSCI is a potential device to monitor perfusion post-operatively.
Acknowledgments
We would particularly like to thank Chaoxi Wen, Lishan Zhang and Shuyi Liu for their valuable help with providing data.
Funding
None.
Conflict of Interest
None.
Ethical Approval
Not required.
References
- Smit JM, Acosta R, Zeebregts CJ, et al. Early reintervention of compromised free flaps improves success rate. Microsurgery 27 (2007): 612-616.
- Pattani KM, Byrne P, Boahene K, et al. What makes a good flap go bad?: A critical analysis of the literature of intraoperative factors related to free flap failure. The Laryngoscope 120 (2010): 717-723.
- Zötterman J, Bergkvist M, Iredahl F, et al. Monitoring of partial and full venous outflow obstruction in a porcine flap model using laser speckle contrast imaging. Journal of Plastic, Reconstructive & Aesthetic Surgery 69 (2016): 936-943.
- PeriCam PSI System - perimed.fr. https://www.perimed.fr/wp-content/uploads/2018/12/44-00461-01-BR-PeriCam-PSI-Animal.pdf
- Briers D, Duncan DD, Hirst E, et al. Laser speckle contrast imaging: theoretical and practical limitations. Journal of Biomedical Optics 18 (2013): 066018.
- Mahe G, Haj-Yassin F, Rousseau P, et al. Distance between laser head and skin does not influence skin blood flow values recordedby laser speckle imaging. Microvascular research 82 (2011): 439-442.
- Zötterman J, Tesselaar E, Farnebo S. The use of laser speckle contrast imaging to predict flap necrosis: An experimental study in a porcine flap model. Journal of Plastic, Reconstructive & Aesthetic Surgery (2019).


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 73.64%
Acceptance Rate: 73.64%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 