Report of a Rare Case of Primary Malignant Mesothelioma of the Perineum Presenting as a Scrotal Abscess
Zhiwei Li1+, Qiqi Zhu2+, Kaibing Xiao1+, Zhiyang Xiao1, Pang Yang1*
1Department of Urology, The First Hospital of Nanchang, Nanchang, China
2The First Affiliated Hospital of Nanchang University, Nanchang, China
*Corresponding Author: Pang Yang, Department of Urology, The First Hospital of Nanchang, Nanchang, China.
Received: 12 July 2022; Accepted: 26 August 2022; Published: 09 September 2022
Article Information
Citation: Li Z, Zhu Q, Xiao K, Xiao Z, Yang P. Report of a Rare Case of Primary Malignant Mesothelioma of the Perineum Presenting as a Scrotal Abscess. Journal of Orthopedics and Sports Medicine 4 (2022): 241-245.
View / Download Pdf Share at FacebookAbstract
A 57-year-old man presented with erythema and pain in the scrotum for 1 week, with pus exuding from the ruptured scrotum for 1 day. Physical examination showed an enlarged left scrotum, with a small area of ruptured skin, and yellowish-white discharge from the rupture was visible in the lower posterior part of the testes near the perineum, with slightly high local skin temperature, tenderness, and fluctuating sensation. The initial reproductive system ultrasound and pelvic CT were suggestive of inflammatory infection, which was confirmed by histology following two surgeries. The patient's condition did not show improvement for a long period of time, and repeat pelvic CT suggested multiple enlarged inguinal lymph nodes. Fine needle aspiration cytology suggested metastatic cancer. Histopathological examination and immunohistochemistry of the perineal scrotal area showed malignant mesothelioma, and whole-body PETCT suggested pulmonary metastases and invasion into the surrounding tissues, such as the organs of the reproductive system. The patient received chemotherapy and immunotherapy, but the disease progressed rapidly, and he ultimately died of respiratory failure.
Keywords
<p>Malignant mesothelioma; Scrotal abscess; Perineum; Case report</p>
Article Details
1. Introduction
Malignant mesothelioma is generally considered to be a rare primary malignancy, mostly originating from mesothelial tissue that is highly malignant and extremely aggressive. This tumor is most commonly found in the pleura, peritoneum, and pericardium; it is extremely unlikely to be found in the spermatic sheath, testicular sheath, vaginal sheath, or oral mucosa. Studies have pointed out that asbestos is the main risk factor for this type of tumor and that recurrent inflammation is also associated with the carcinogenic process underlying its development, as well as other factors, such as genetics [1]. The treatment of malignant mesothelioma includes surgery, radiotherapy, chemotherapy and immunotherapy, and the treatment plan is often selected based on the location, progression and complications of the tumor. Due to the rapid progression of this tumor, even with prompt treatment, a good prognosis cannot be achieved, and the overall survival time of patients varies from 4 to 12 months [2]. We report a rare case of malignant mesothelioma of the perineum presenting as a scrotal abscess in a male patient.
2. Case Report
The patient in this case was a 57-year-old male who presented with erythema and pain in the left scrotum for 1 week and pus exuding from the ruptured scrotum for 1 day. He had a previous history of poliomyelitis and, sequelae of left thigh muscle atrophy, but no history of asbestos exposure or cancerous disease. On physical examination, the left scrotal area was found to be significantly enlarged, and a rupture in the scrotum was visible in the lower posterior part of the testes near the perineum, with yellowish-white pus exuding from the rupture, slightly elevated local skin temperature, and a feeling of tenderness and fluctuating sensation. The rest of the physical examination findings were normal. Ultrasound of the male genital system (Figure 1 A-B) displayed an irregular hypoechoic area under the left scrotum with poor demarcation of the epididymis, and inflammation was considered. CT of the pelvis revealed that the scrotum and perineum were swollen, and a few strips of high-density shadow with indistinct borders could be observed. CT of the chest and abdomen showed no other primary tumors or significant disease. Levels of the tumor markers methemoglobin, β-chorionic gonadotropin, Carcinoembryonic Antigen (CEA), CA19-9, total prostate-specific antigen, free prostate-specific antigen, and other routine blood and biochemical tests were all within normal limits, except for leukocytes and neutrophils and C-reactive protein inflammatory markers, which were elevated. The patient underwent local abscess incision and drainage on the same day, and a large amount of yellowish-white foul-smelling pus was found in the abscess, which was managed with anti-inflammatory treatment and drug dressing changes after surgery. The scrotal skin and subcutaneous necrotic tissue were debrided again on the tenth postoperative day because the wound had not healed, and the scrotal incision was explored during the operation. The pathological diagnosis was a perineal cyst with inflammatory granulation tissue, visible necrosis, calcification and foreign body giant cell reaction (Figure 2 A-B). Within 3 weeks after the second surgery, the patient was in good general condition, with only a small amount of white purulent fluid on the wound surface and no signs of healing. During the 4th week, the patient developed recurrent low-grade afternoon fever with distension and pain in the perineal area of the scrotum, and routine blood tests suggested significantly elevated inflammatory indicators, but all tests for tuberculosis infection were negative. The fever resolved after anti-inflammatory and debridement and dressing change treatment, but the patient’s symptoms recurred.
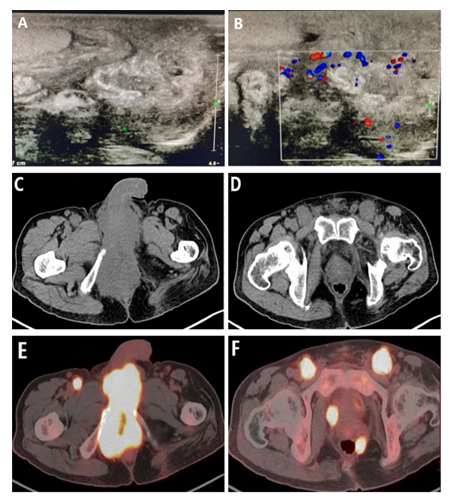
Figure 1: (A-B) - Ultrasound suggests an irregular hypoechoic area under the left scrotum, poorly demarcated from the epididymis, with normal testicular morphology. (C-D) - Pelvic CT suggested multiple enlarged inguinal lymph nodes bilaterally and uneven density of swollen urethral spongiosomes in the scrotum and perineum. (E-F) - PET-CT images suggest high tracer uptake in the perineum, scrotum, testes and lymph nodes, indicating that extensive tumor invasion and metastasis have occurred.
After the 8th week, pelvic CT (Figure 1 C-D) showed abnormal changes in the scrotum and perineal urethral spongiosa, which was considered to be an infection; scrotal effusion; a nodule-like density shadow in the left side of rectum in the fatty space, which was considered to be an infection; and multiple enlarged lymph nodes in the groin bilaterally. Severe edema-like changes in the anterior rectum, and a hard palpable mass in the right side of the rectum, which could not be manipulated without causing the patient pain, were noted during rectal examination.
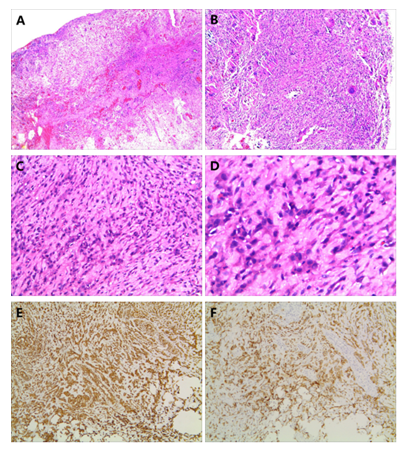
Figure 2: (A-B) - Inflammatory granulation tissue from a perineal cyst can be observed, with necrosis, calcification, and foreign body giant cell reaction (H & E, magnification ×50). (C-D) - Histological features of malignant mesothelioma of the perineum, with tumor cells showing bidirectional epithelial and mesenchymal differentiation, indicative of epithelioid mesothelioma, with markedly enlarged and darkly stained nuclei, pathological mitotic images and necrotic tissue (H & E; magnification ×200 and ×400, respectively). (E-F) - Immunohistochemical examination of tumor cells showed strong expression of vimentin(+) and keratin(+), (Vimentin(+) on the left, CK(+) on the right, magnification ×50).
The results suggested that the inguinal lymph node tissue had heterogeneous epithelial-like tumor cells microscopically, which is typically indicative of metastatic hypofractionated carcinoma; the perineal scrotal fistula tissue displayed epithelial and mesenchymal differentiation in both directions, which is typically indicative of epithelial-like mesothelioma (Figure 2 C-D). Immunohistochemistry revealed the following (Figure 2 E-F): CK(+), EMA(+), Vimentin(+), CK7(-), CK20(-), CD34(vascular+), CD68(-), CDX-2(-), S100(-), PSA(-), SMA(-), Desmin(-), villin(-), P16(-), WT -1(-), P53(+), CR(weak+), D2-40(+), CK5/6(-), CD99(foci+), myoD1(-), myogenin(-), Ki-67(40%,+). Whole-body PET-CT (Figure 1 E-F) was completed at the 9th week, depicting a soft tissue mass shadow in the perineal region with metabolic hyperplasia and poor demarcation of the surrounding tissues; bilateral pubic bone invasion and bone destruction; and multiple enlarged lymph nodes in the presacral, pararectal and bilateral inguinal regions with metabolic hyperplasia. The above findings mostly suggested a malignant tumor in the perineal region with multiple lymph node metastases. A soft tissue nodal shadow was observed in the dorsal segment of the right lower lobe of the lung with metabolic hyperplasia, indicating the possibility of metastatic tumor. The above observations are mostly considered inflammatory or nonspecific changes. After the diagnosis was confirmed by histological examination, the patient received chemotherapy with a pemetrexed (800 mg) + carboplatin (400 mg) regimen for one cycle and sindilizumab (200 mg) immunotherapy for one cycle, but the patient not experience any significant improvement after treatment, so he refused additional chemotherapy and immunotherapy for personal reasons, and ultimately died of complications of respiratory failure due to rapid progression of the disease. From admission to death, the overall survival time of this patient was only 5 months.
3. Discussion
Since malignant mesothelioma was first reported, its incidence has been relatively low and clinically rare. Related cases can be found across all age groups, with an increasing incidence with age and a relatively higher incidence in men than in women [3]. Although some studies have demonstrated a significant relationship between asbestos and the incidence of mesothelioma, they mostly refer to mesothelioma occurring in the pleura, pericardium, and peritoneum. For mesothelioma of the genital system, there are no large samples or high-quality studies to better elucidate the relationship with asbestos [4]. This paper reports a very rare case of primary malignant mesothelioma arising in the perineum presenting as a scrotal abscess, and there are very few similar case reports in the literature. The patient in this case presented clinically with localized inflammation of the perineum of the scrotum, without typical signs or specific symptoms of a tumor, both historically and symptomatically, such as tuberculosis of the epididymis, or epididymal cyst with infection, which can also have the same presentation. Early ultrasound and abdominal or pelvic CT did not suggest obvious evidence of a tumor, but rather inflammation or infection and after two surgeries, inflammation of the perineum and scrotum that responded to anti-inflammatory treatment was confirmed. Histological examination initially indicated an inflammatory reaction without suggesting tumor cells. This posed a great diagnostic interference and increased the difficulty of confirming the tumor diagnosis. Ultimately, tumor cells were first detected by puncture biopsy of enlarged lymph nodes, and then combined with the histopathological examination of perineal scrotal fistula granulation, the tumor was determined to be of perineal rather than metastatic origin. These findings reflected the certain clinical features of malignant mesothelioma of the perineal region combined with scrotal abscess. Due to the deep location of this tumor in the perineal area and the complex anatomy of this area, there may be no obvious symptomatic manifestations during the early stage. In cases of combined acute inflammation around the perineum, even with the assistance of routine adjuvant examination, the initial diagnosis and treatment can be easily misguided by the symptoms and signs of inflammation, affecting clinician’s empirical judgment and causing them to miss the underlying tumor factors. When the inflammation around the tumor is extensive or widespread, even with conventional surgery and drug control, the wound will not heal for a long time and can become repeatedly infected, and the increased level of inflammation can obfuscate obvious clinical judgments regarding the presence of tumors based on images on conventional imaging, resulting in a low probability of obtaining diagnostic tumor tissue specimens and a high probability of misdiagnosis or missed diagnosis. The late PET-CT images significantly suggested tumor infiltration and metastasis, which correlated with the macroscopic manifestations of the tumor during the late stage. Because of the more delicate and sensitive imaging characteristics of PET-CT, perhaps improving PET-CT examination at an early stage may lead to early detection of this type of tumor and thus improve the tumor diagnosis rate. The patient had no history of asbestos exposure; if this highly aggressive mesothelioma could have been correlated with a history of asbestos exposure, it could have been determined to be a low-grade aggressive mesothelioma. However, the tumor developed rapidly, with peripheral organ invasion of the penis, urethra, scrotum, testes, prostate, and pubic bone in a short period of time, and distant metastases to the inguinal lymph nodes and lungs. According to its histological features, malignant mesothelioma can be divided into three subtypes—epithelial, sarcomatous and biphasic. The specific immunohistochemical markers for malignant mesothelioma are calretinin, EMA, Vimentin, CK5/6, D2-40, WT1 and MC, among which calretinin is the most specific and sensitive [5]. In our case study, the patient had the epithelial subtype, and immunohistochemical staining revealed EMA(+), CK(+), Vimentin(+), CR(weak +), and D2-40(+). The above findings are consistent with malignant mesothelioma features both in terms of tumor progression and histologic features. There are no definite standards to guide the clinical management of perineal primary malignant mesothelioma because of the very small number of cases. We believe that for the early detection of malignant mesothelioma in the perineum, early radical tumor resection and lymph node dissection, as well as postoperative combined adjuvant radiotherapy and chemotherapy, may be key to improving the survival time of patients. Malignant mesothelioma in the perineal region is highly aggressive and can rapidly invade the surrounding tissues and organs due to the complex anatomy of this region and its rich vascularity and lymph network, facilitating lymph node and distant organ metastasis. It has been reported in the literature that pemetrexed combined with cisplatin is effective for the treatment of mesothelioma and is most commonly used in cases with poor prognosis; gemcitabine may be used as an alternative treatment if platinum drugs are not effective [6]. In addition, it has been reported in the literature that bevacizumab combined with pemetrexed and cisplatin significantly improves the survival of patients with mesothelioma [7]. In the present case, the patient already had genital invasion and distant metastases at the time of diagnosis, and despite receiving treatment with pemetrexed + carboplatin in combination with sindilizumab, the disease progressed rapidly, leading to death. Therefore, palliative surgery and radiotherapy may be considered to relieve symptoms in patients with perineal malignant mesothelioma who have genital organ invasion, but these approaches have no significant effect on prolonging survival. We also believe that the earliest distant organ metastasis site in patients is the lung, as metastatic lesions were not found in the abdominal viscera, such as the liver, spleen, kidney, or retroperitoneum. The main reason for this metastatic pattern may be due to the initial route of invasion into the genital system tissues and organs, such as the testes and penis, which would be more likely to cause distant pulmonary metastases via the circulation.
4. Conclusion
Primary malignant mesothelioma of the perineum is a rare and under recognized disease, the diagnosis of which is currently confirmed mainly via pathological histological examination. Surgery and adjuvant therapy are the main treatment approaches for patients if early diagnosis can be made. Due to the low number of reported cases in the literature, it has been difficult to develop and analyze clinically relevant treatment options. The rapid progression of this disease, tendency toward metastasis, poor prognosis, and short survival time further hinder effective clinical studies.
5. Declarations
Ethics approval
As it is a case report, ethics approval is not necessary after consulting the Ethics Committee of Nan Chang First Hospital.
Consent to participate
Written informed consent was obtained from the patient's relatives for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Consent for publication
All authors agree to submit this manuscript.
Data availability
The datasets generated and/or analysed during the current study are not publicly available due to individual privacy of the patients included but are available from the corresponding author on reasonable request.
Conflicts of interest
The authors declare no competing financial interests.
Funding
No financial support was received for this submission.
Author contributions
ZL, PY designed, performed the study and carried out literature search; ZL, QZ helped in literature search and wrote the paper; ZL, KX, ZX helped in acquisition of data; PY made critical revision and supervision. All authors have read and approved the manuscript.
Author details
1Department of Urology, The First Hospital of Nanchang, Nanchang, China, 2The First Affiliated Hospital of Nanchang University, Nanchang, China, +Zhiwei Li, Qiqi Zhu, Kaibing Xiao have equally contributed to this work.
Acknowledgements
We would like to thank the patient for his participation and his consent to the publication of the case details and associated images.
References
- Mezei G, Chang ET, Mowat FS, et al. Epidemiology of mesothelioma of the pericardium and tunica vaginalis testis. Ann Epidemiol 27 (2017): 348-359.
- Delgermaa V, Takahashi K, Park EK, et al. Global mesothelioma deaths reported to the World Health Organization between 1994 and 2008. Bull World Health Organ 89 (2011): 716-724.
- Craighead JE. Epidemiology of mesothelioma and historical background. Recent Results Cancer Res 189 (2011): 189: 13-25.
- Huang XY, Ye Q. Asbestos exposure and asbestos-related malignant diseases: an epidemiological review. Zhonghua Lao Dong Wei Sheng Zhi Ye Bing Za Zhi 39 (2021): 233-236.
- Moore AJ, Parker RJ, Wiggins J. Malignant mesothelioma. Orphanet J Rare Dis 3 (2008): 34.
- Recabal P, Rosenzweig B, Bazzi WM, et al. Malignant Mesothelioma of the Tunica Vaginalis Testis: Outcomes Following Surgical Management Beyond Radical Orchiectomy. Urology 107 (2017): 166-170.
- Zauderer MG. A new standard for malignant pleural mesothelioma. Lancet 387 (2016): 1352-1354.


 Impact Factor: * 5.3
Impact Factor: * 5.3 Acceptance Rate: 73.64%
Acceptance Rate: 73.64%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 