Contained Rupture of the Aorta: IgG4 Related Aortitis
Arif A Khan1,2*, Isabelle Roussin2, Arthur Wayne2, George Leventogiannis1,3,
Matthew Banks1,3, Joe Martins1,3, Nikolaos Tsanaxidis1,3*
1Royal Wolverhampton NHS Trust, UK
2Royal Shrewsbury nhs trust, UK
3The Dudley Group NHS Trust, UK
*Corresponding author: Arif A Khan, Royal Wolverhampton NHS Trust, UK.
Nikolaos Tsanaxidis, Royal Wolverhampton NHS Trust, UK
Received: 22 November 2020; Accepted: 04 December 2020; Published: 26 September 2022
Article Information
Citation: Arif A Khan, Isabelle Roussin, Arthur Wayne, George Leventogiannis, Craig Barr, Matthew Banks, Joe Martins, Nikolaos Tsanaxidis. Contained Rupture of the Aorta: IgG4 Related Aortitis. Cardiology and Cardiovascular Medicine 6 (2022): 497-498.
View / Download Pdf Share at FacebookKeywords
<p>Aorta; IgG4; Aortitis</p>
Article Details
1. Introduction
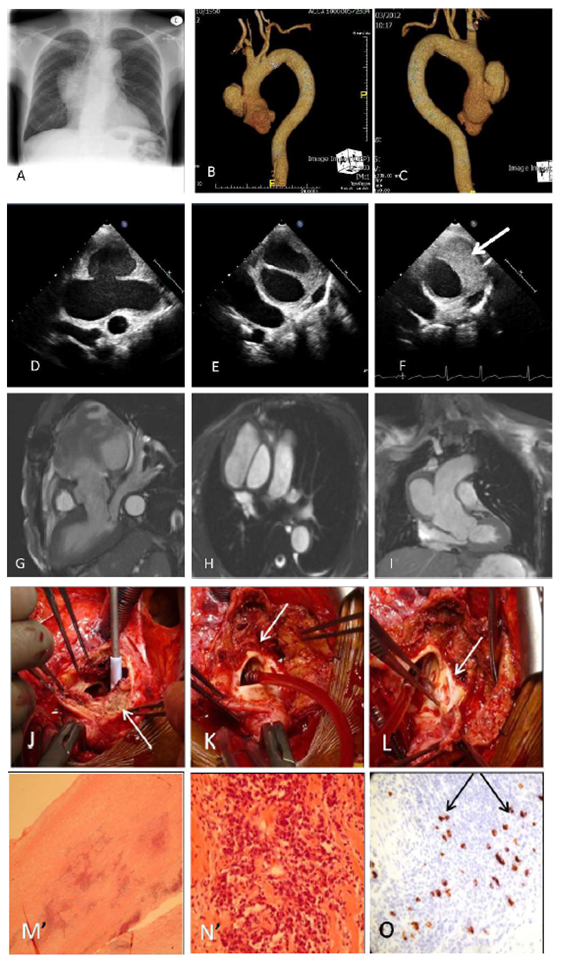
We report the case of a 52 year old Jamaican lady who presented with contained rupture of the aorta. The patient initially presented one year prior to admission with fatigue and weight loss. At the time, her inflammatory markers were non-specifically raised: IgG: 16.6 g/L (normal 5.3- 16.5) and IgA: 4.21 g/L (normal 0.8-4.00), CRP 45 mg/l (normal 0-10), ESR 24mm/hr (normal (1-12), globulins 41 (19-35) but her full blood count and liver function test were normal. Both rheumatoid factor and ANA were negative. A CT scan was performed to investigate the weight loss and revealed a lung nodule but no other abnormalities. On review one year later, her ESR was raised to >100mm/hr and globulins to 48g/L. A follow up chest radiograph (Figure 1A) and CT scan to look for interval change in the lung nodule revealed a 6 cm aneurysm of the ascending aorta together with a large type A aortic dissection (Figure 1B-C). The patient was transferred to our hospital for urgent surgery. On admission, the patient described experiencing an acute back pain 3 weeks earlier which was initially treated as musculoskeletal. Pre-operative transthoracic echo (Figure 1D-F) showed contained rupture of the ascending aorta from the sinus of Valsalva to the proximal arch: 9.0 x 4.3 cm, neck 2.1 cm, no flap and no aortic regurgitation. The ruptured aorta was contained by a 2.6 cm thick mural haematoma (Figure 1F). MRI confirmed these initial findings (Figure 1G-I). Intra-operative findings (Figure 1J-L) confirmed the ruptured aorta with aortic aneurysm originating from the sinotubular junction to the proximal arch, with the unusual finding of a transverse rupture of the aortic wall adjacent to an aortic ulcer. The contained rupture was filled with layers of haematoma. A 36mm Dacron graft was fitted with an uneventful post-operative course. Histology of aorta revealed a lymphoplasmocytic aortitis with destruction of the media (Figure 1M-N). Immunostaining showed 15%.of the lymphocytes positive for IgG4 (Figure 1N). No giant cells were seen and the presence of intimal thrombus was confirmed. Follow-up revealed a persistent increase in inflammatory markers: CRP 40.7 mg/ml, globulin 48 g/L, ESR >100 mm/hr. The patient was referred to her rheumatologist for initiation of glucocorticoid treatment to control the inflammatory syndrome associated with her IgG4- positive lymphoplasmocytic aortitis in order to prevent recurrent vascular disease.
Figure 1: Imaging- A: Chest radiograph; B-C: Volume-rendered CT reconstructions; D-F: Transthoracic Echo; G-I: MRI
Surgical views- J: Arrow for intramural hematoma; K: Arrow on the transverse aortic rupture; L: Arrow on transverse ulcer on the aortic wall
Histopathology- M: Perivascular inflammation; N: Lymphocytes and plasma cells; O: IgG4-immunostaining
2. Conclusion
These findings have important implications for potential treatment and longterm management of non-infectious aortitis. IgG4-related systemic disease often responds well to a prolonged course of glucocorticoids. Therefore, treatment of the aortitis might prevent progression of the IgG4-related systemic disease to the remaining aorta and/or involvement of other organs. To our knowledge, this is the first reported case of contained ruptured of the thoracic aorta with aortitis secondary to IgG4 related systemic disease. The concept of IgG4-related systemic disease (RSD) has been recognized recently and can be complicated by autoimmune pancreatitis and retroperitoneal fibrosis. Significant common features in IgG4 related systemic disease are as follow:
- Abundant infiltration of affected organs by IgG4-positive plasma cells (sine qua non)
- Elevated serum IgG4 level in the majority but not all of the patients
- Marked improvement with corticosteroid therapy
Only a few reports of extra-pancreatic lesions in IgG4 RSD have been described. Ascending aorta aneurysm with isolated IgG4 periaortitis have been previously reported in Japan [1-3]. Stone et al reported from a retrospective study in their institution that IgG4-related systemic disease accounts for the majority of thoracic lymphoplasmocytic aortitis cases and ∼9% of all cases of non-infectious thoracic aortitis. Therefore in patients with aortitis, IgG4-related disease should be specifically sought by immunostaining for IgG4.
References
- Stone JH, Khosroshahi A, Deshpande V, et al. IgG4-Related Systemic Disease Accounts for a Significant Proportion of Thoracic Lymphoplasmacytic Aortitis Cases. Arthritis Care Res (Hoboken) 62 (2010): 316-322.
- Kasashima S, Zen Y, Kawashima A, et al. A new clinicopathological entity of IgG4-related inflammatory abdominal aortic aneurysm. J Vasc Surg 49 (2009): 1264-1271.
- Kamisawa T, Okamoto A. IgG4-related sclerosing disease. World J Gastroenterol 14 (2008): 3948-3955.


 Impact Factor: * 5.6
Impact Factor: * 5.6 Acceptance Rate: 74.36%
Acceptance Rate: 74.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 