Is the Correct Anatomical Placement of the Electrocardiogram (ECG) Electrodes Essential to Diagnosis in the Clinical Setting: A Systematic Review
Alexandros Hadjiantoni1,2*, Katy Oak3, Siddhartha Mengi4, Judit Konya5, Tamas Ungvari6
1Department of Health and Applied Sciences (HAS), The University of the West of England (UWE), Bristol, United Kingdom
2Department of Cardiology, The Royal Cornwall Hospitals NHS Trust, Cornwall, United Kingdom
3Librarian Specialist, Royal Cornwall Hospitals NHS Trust, Treliske, Truro, Cornwall, United Kingdom
4Interventional Cardiology Registrar, Department of Cardiology, Royal Cornwall Hospitals NHS Trust, Treliske, Truro, Cornwall, United Kingdom
5Health Education England GP Research Fellow, Kernow Health CIC Honary Clinical Research Fellow, University of Exeter, United Kingdom
6Consultant Invasive Cardiologist, Department of Cardiology, Royal Cornwall Hospitals NHS Trust, Treliske, Truro, Cornwall
*Corresponding Author: Alexandros Hadjiantoni, Department of Health and Applied Sciences (HAS), The University of the West of England (UWE), Bristol, United Kingdom
Received: 11 February 2021; Accepted: 19 February 2021; Published: 02 March 2021
Article Information
Citation: Alexandros Hadjiantoni, Katy Oak, Siddhartha Mengi, Judit Konya, Tamas Ungvari. Is the Correct Anatomical Placement of the Electrocardiogram (ECG) Electrodes Essential to Diagnosis in the Clinical Setting: A Systematic Review. Cardiology and Cardiovascular Medicine 5 (2021): 182-200.
View / Download Pdf Share at FacebookAbstract
Background: Anatomical misplacement of the Electrocardiogram (ECG) electrode(s) is common, with significant impact on clinical diagnosis. Reasons are multi-faceted, with this review examining the consequential effects of misplacement to ECG morphology, diagnosis, prognosis, patient outcomes, and potential impact to patient care pathway.
Objectives: This review examined the significance of misplacement, its’ commonality and ensuing effect on patient safety, accurate ECG acquisition and diagnosis, with evaluation of reasons for such misplacement.
Methodology: Review of available literature was conducted using electronic databases. In-line with the Preferred Reporting Items for Systematic reviews and Meta – analysis protocols (PRISMA) 2015 checklist, this review was conducted with search criteria, search terms, eligibility for inclusion/ exclusion criteria, extraction and data analysis predetermined by the authors. Keywords were arranged according to grouping of terms surrounding ECG, anatomical placement, and diagnosis. The search strategy was conducted during September/October 2019. Scoping searches were conducted alongside reference lists of included studies hand searched (Snowballing) for further relevant studies. The Critical Appraisal Skills Programme (CASP) was used to methodically appraise papers (CASP, 2019). Screening of titles and abstracts of identified citations was performed by a single reviewer. Eligible articles then full text screened independently by two reviewers. Disagreements were discussed and resolved by a third reviewer. In instances of unclear reporting, authors were contacted to provide further information and clarity. Assessment of relevant literature and critical appraisal of primary research, pertaining to the clinical diagnosis and effects of anatomical misplacement of ECG electrodes, formulate the thematic discussion drawn by t
Keywords
<p>Electrocardiogram, Electrode, Cardiology, Lead, Anatomy, Systematic Review</p>
Article Details
Abbreviations:
ACS: Acute Coronary Syndrome(s); AHA: American Heart Association; BCS: British Cardiovascular Society; CAD: Coronary Artery Disease; CASP: Critical Appraisal Skills Programme; CWT: Continuous Wavelet Transform; ECG: Electrocardiogram; FT: Fourier Transform; HDAS: Healthcare Databases Advanced Search; IRBBB: Incomplete Right Bundle Branch Block; NICE: National Institute for Health and Clinical Excellence; NMC: Nursing and Midwifery Council; NSTEMI: Non-ST-segment Elevation Myocardial Infarction; PICO: Population Intervention Comparison and Outcome Framework; PRISMA: Preferred Reporting Items for Systematic Reviews and Meta-Analysis Protocols; RCT: Randomised Controlled Trials; SCST: Society for Cardiological Science and Technology; SOB: Shortness of Breath; STEMI: ST-segment Elevation Myocardial Infarction
1. Introduction
Incorrect anatomical placement of ECG electrodes has potential impact on clinical diagnosis. The electrocardiogram (ECG) remains the cornerstone for diagnosing arrhythmia (heart rhythm disorders) and myocardial ischemia (MI). Low cost, ubiquitous and immediate availability, as well as its’ simplicity of application, render the ECG a versatile and indispensable tool especially for cardiologists, emergency physicians and healthcare personnel. Nevertheless, application errors owing to misplacement of electrodes are common place, frequent and with relevant clinical implications. Coronary artery disease (CAD) resides as the leading cause of death in most countries worldwide, yet CAD disease is preventable [1, 2]. The standard 12 lead electrocardiogram (ECG) provides for a non-invasive, cost effective assessment that is convenient to patients [3]. The ECG, being the assessment of the electrophysiological activity of the heart over time, is to date the most frequently requested and conducted diagnostic/prognostic tool within the clinical setting [4-6]. Its’ fundamental morphological features provide useful information in the diagnosis/prognosis of arrhythmia and cardiac disease [7, 8]. Accurate electrode placement and acquisition of ECG is an essential skill required of nursing staff and health professionals alike and duly noted by The Nursing and Midwifery Council (NMC) (2010) standards for preregistration nurses [9].
Principally, acquisition of ECG traces should be reproducible and correctly identify various medical conditions such as cardiac arrhythmia, particularly acute coronary syndromes (ACS), and which aid in risk stratification, detection and management of cardiac disease, notably ST elevation myocardial infarction [6, 10]. This graphical representation of the signal potential difference between two points provides for universal standard parameters of the ECG waveform [11]. Typically depicted as the P-wave (Atrial depolarization, with subsequent contraction), the QRS complex (Ventricular depolarization, with subsequent contraction), and the T-wave and U-wave which constitute the repolarisation phase of the cardiac cycle [12]. Any deviation from the perceived normal ECG baseline requires accurate and reliable detection owing to time/frequency varying morphology. It follows that, acquisition, recognition, analysis, diagnosis and subsequent treatment of patients is, in part, reliant on this non-invasive electro-cardiology procedure [13, 14]. Regarded as the ‘gold standard,’ a non-invasive, inexpensive diagnostic tool, integral in medical investigations, the electrocardiogram remains the principal diagnostic method in the recognition of acute myocardial infarction (MI), British Cardiovascular Society (BSC) (2015) and National Institute for Health and Care Excellence (NICE) [15, 16].
Historically, substandard levels have prevailed in the acquisition of ECG, with 50% of nurses and <20% of cardiologists correctly placing precordial electrodes V1 and V2 [17]. This erroneous pervasiveness continues in Today’s practice. These findings were supported by Medani et al., [14], which revealed nurses misplaced precordial electrodes in 64% of cases. Misplacement constitutes for erroneous acquisition, diagnosis, missed diagnosis, interpretation, and treatment/mistreatment of patients [18]. Furthermore, delayed triage to early invasive strategy in the patient care pathway has resulted from erroneous placement, with consequent increased mortality and morbidity [18].
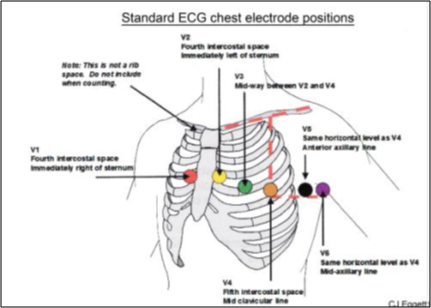
The prevalence of electrode misplacement is a common finding in both acute and clinical settings [13, 14]. Despite the commonality of misplacement, such erroneous practice remains under reported. Of paramount importance in any attempt to acquire an ECG trace that is accurate and of good reproducible quality, is the onus placed on correct anatomical placement of the silver-silver chloride electrodes and their relative leads, Figure 1. The respected ‘gold standard’ should therefore consider the recommendations and guidelines of the Society for Cardiological Science and Technology (SCST) (2017) adherence to which remains widely neglected in clinical practice [19].
The electrocardiogram has changed little since its inception, with the overarching prerequisite for any accurate detection of signal remaining the accurate anatomical placement of electrodes and their contact interface with the skin [20]. With current information regarding electrophysiology and ECG oftentimes disjointed, contradictory and frequently misunderstood, particularly in an era of multi-authored texts, the need for a single authoritative voice is essential [6]. The SCST recommend standardization of the ECG procedure, with training and subsequent accreditation, ensuring operator skill, competency, confidence, and a gold standard of practice and promotion of excellence [19].
1.1 Objectives
This systematic review investigated the significant importance of correct anatomical placement of the electrocardiogram (ECG) electrodes and their relative leads. Objectives were made to establish the commonality of electrode misplacement, its’ subsequent potential effect on patient safety and a review of reasons for such misplacement.
2. Design and Methodology
Consideration has been given to the common denominator governing ECG signal processing modalities. In short, this is reliant upon the interface between the patients’ skin and the silver-silver chloride electrodes with their respective leads, for the acquisition and attainment of the surface 12 - Lead ECG.
2.1 Justification
A risk of bias assessment was conducted for each of the included studies using the Critical Appraisal Skills Programme (CASP) (2018). [21] The population, intervention, comparison and outcome (PICO) framework (NICE, 2012) for eligibility criteria are described as follows:
2.1.1 Population: Male or female adults of ≥18 years, regardless of any previous cardiac history were considered.
2.1.2 Intervention: Electrode placement with the sole intention to acquire a 12 - Lead electrocardiogram trace for clinical diagnosis of arrhythmia.
2.1.3 Comparison: Accurate anatomical placement of ECG electrodes in-line with guidelines and recommendations of the (SCST, 2017) compared with those misplaced.
2.1.4 Outcome: The potential effect(s) on patients’ clinical diagnosis, owing to inaccurate ECG electrode placement.
In accordance with the Nursing and Midwifery Code of Conduct (NMC, 2015), [22] and guidelines /recommendations of the SCST [19] justification for this work is demonstration of the ongoing prevalence and relevance of ECG electrode misplacement in the clinical setting. Furthermore, the subsequent ramifications imposed on patient diagnosis and implications of erroneous ECG acquisition.
2.2 Search Strategy
A systematic review was conducted with search criteria, search terms, eligibility for inclusion /exclusion criteria, extraction and analysis of data predetermined by the authors, in-line with the Preferred Reporting Items for Systematic reviews and Meta - analysis protocols (PRISMA) 2015 checklist [23]. Keywords and subject headings were combined according for terms surrounding, ECG, anatomical placement, and diagnosis. Table 1 highlights the systematic review synthesis and data extraction. No time/date restrictions of the literature were implemented. The inclusion criteria for this review included English language articles and international papers. The study is reported and conducted according to the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines. The systematic review protocol was prospectively registered on the PROSPERO database of systematic reviews, Registration Number: CRD42019152461, and in-line with the Preferred Reporting Items for Systematic reviews and Meta-Analyses Protocols (PRISMA-P), (2015) checklist. Critical Appraisal Skills Programme (CASP) was used to methodically appraise papers (CASP, 2019) [21].
The search strategy was developed and conducted during September and October 2019. A total of three (3) scoping searches were conducted along with the reference lists of included studies hand searched (Snowballing) for further relevant studies. A copy of the Healthcare Databases Advanced Search (HDAS) NICE [24] search strategy is included in Table 2. An initial screening of titles and abstracts of identified citations was performed by a single reviewer (AH). Potentially eligible articles were then full text screened independently by two reviewers, (AH and SM) in-line with the inclusion and exclusion criteria. Disagreements regarding eligibility were discussed and resolved by a third reviewer (TU). In instances of unclear reporting, authors were contacted to provide further information and clarity.
Table 1: Systematic Review Synthesis and Data Extraction.
|
# |
Database |
Search term |
Results |
|
1 |
Medline |
(ecg).ti,ab |
60247 |
|
2 |
Medline |
(electrocardiogram).ti,ab |
36766 |
|
3 |
Medline |
ELECTROCARDIOGRAPHY/ |
186536 |
|
22 |
Medline |
(electrocardiograph*).ti,ab |
44904 |
|
23 |
Medline |
(1 OR 2 OR 3 OR 22) |
235131 |
|
5 |
Medline |
(electrode*).ti,ab |
147008 |
|
6 |
Medline |
ELECTRODES/ |
45184 |
|
7 |
Medline |
(5 OR 6) |
163150 |
|
8 |
Medline |
(placement).ti,ab |
121217 |
|
9 |
Medline |
(position*).ti,ab |
567725 |
|
10 |
Medline |
(anatomical).ti,ab |
139469 |
|
12 |
Medline |
(misplacement).ti,ab |
1725 |
|
24 |
Medline |
(Angle of louis).ti,ab |
41 |
|
26 |
Medline |
(malposition).ti,ab |
4122 |
|
29 |
Medline |
(misposition*).ti,ab |
281 |
|
30 |
Medline |
(mis-position*).ti,ab |
30 |
|
31 |
Medline |
(misplaced OR mis-placed).ti,ab |
2405 |
|
32 |
Medline |
(error*).ti,ab |
285306 |
|
33 |
Medline |
"MEDICAL ERRORS"/ OR exp "DIAGNOSTIC ERRORS"/ |
129236 |
|
34 |
Medline |
(misdiagnos* OR mis-diagnos*).ti,ab |
31019 |
|
35 |
Medline |
(8 OR 9 OR 10 OR 12 OR 24 OR 26 OR 29 OR 30 OR 31 OR 32 OR 33 OR 34) |
1202184 |
|
36 |
Medline |
(23 AND 7 AND 35) |
1375 |
|
37 |
EMBASE |
(ecg).ti,ab |
103111 |
|
38 |
EMBASE |
(electrocardiogram).ti,ab |
47724 |
|
39 |
EMBASE |
ELECTROCARDIOGRAM/ |
114739 |
|
40 |
EMBASE |
(electrocardiograph*).ti,ab |
51551 |
|
41 |
EMBASE |
(37 OR 38 OR 39 OR 40) |
216323 |
|
42 |
EMBASE |
(electrode*).ti,ab |
165348 |
|
43 |
EMBASE |
ELECTRODE/ |
101835 |
|
44 |
EMBASE |
(42 OR 43) |
185992 |
|
45 |
EMBASE |
(placement).ti,ab |
173569 |
|
46 |
EMBASE |
(position*).ti,ab |
673332 |
|
47 |
EMBASE |
(anatomical).ti,ab |
188133 |
|
48 |
EMBASE |
(misplacement).ti,ab |
2399 |
|
49 |
EMBASE |
(Angle of louis).ti,ab |
31 |
|
50 |
EMBASE |
(malposition).ti,ab |
5477 |
|
51 |
EMBASE |
(misposition*).ti,ab |
381 |
|
52 |
EMBASE |
(mis-position*).ti,ab |
55 |
|
53 |
EMBASE |
(misplaced OR mis-placed).ti,ab |
3209 |
|
54 |
EMBASE |
(error*).ti,ab |
357058 |
|
55 |
EMBASE |
"MEDICAL ERROR"/ OR exp "DIAGNOSTIC ERROR"/ |
110041 |
|
56 |
EMBASE |
(misdiagnos* OR mis-diagnos*).ti,ab |
45090 |
|
57 |
EMBASE |
(45 OR 46 OR 47 OR 48 OR 49 OR 50 OR 51 OR 52 OR 53 OR 54 OR 55 OR 56) |
1443769 |
|
58 |
EMBASE |
(41 AND 44 AND 57) |
1416 |
|
59 |
CINAHL |
(ecg).ti,ab |
12052 |
|
60 |
CINAHL |
(electrocardiogram).ti,ab |
8212 |
|
61 |
CINAHL |
ELECTROCARDIOGRAPHY/ |
35246 |
|
62 |
CINAHL |
(electrocardiograph*).ti,ab |
7423 |
|
63 |
CINAHL |
(59 OR 60 OR 61 OR 62) |
44870 |
|
64 |
CINAHL |
(electrode*).ti,ab |
9324 |
|
65 |
CINAHL |
ELECTRODES/ |
3648 |
|
66 |
CINAHL |
(64 OR 65) |
11348 |
|
67 |
CINAHL |
(placement).ti,ab |
34494 |
|
68 |
CINAHL |
(position*).ti,ab |
79349 |
|
69 |
CINAHL |
(anatomical).ti,ab |
17470 |
|
70 |
CINAHL |
(misplacement).ti,ab |
470 |
|
71 |
CINAHL |
(Angle of louis).ti,ab |
8 |
|
72 |
CINAHL |
(malposition).ti,ab |
948 |
|
73 |
CINAHL |
(misposition*).ti,ab |
8 |
|
74 |
CINAHL |
(mis-position*).ti,ab |
1 |
|
75 |
CINAHL |
(misplaced OR mis-placed).ti,ab |
640 |
|
76 |
CINAHL |
(error*).ti,ab |
52335 |
|
77 |
CINAHL |
"HEALTH CARE ERRORS"/ OR exp "DIAGNOSTIC ERRORS"/ |
21009 |
|
78 |
CINAHL |
(misdiagnos* OR mis-diagnos*).ti,ab |
6531 |
|
79 |
CINAHL |
(67 OR 68 OR 69 OR 70 OR 71 OR 72 OR 73 OR 74 OR 75 OR 76 OR 77 OR 78) |
198453 |
|
80 |
CINAHL |
(63 AND 66 AND 79) |
0 |
Table 2: Healthcare Databases Advanced Search (HDAS) NICE search strategy (Electronic Databases).
Assessment of relevant literature and critical appraisal of primary research, pertaining to the clinical diagnosis and effects of anatomical misplacement of ECG electrodes and leads, formulate the thematic discussion drawn by this review. The primary consideration and rationale for this review is the ongoing potential relevance of electrode misplacement, its frequency in the clinical setting, the subsequent ramifications imposed on patients and reasons leading to such error. In addition, synthesis of the literature correlate the overarching consensus for education, training and a change to practice in order to provide improved safety, and care of patients in line with the Nursing and Midwifery Code of Conduct (NMC, 2015) [22] and guidelines/recommendations of the (SCST, 2017) [19].
2.3 Study Selection
Two independent reviewers (AH and SM) carried out searches of relevant and pertinent studies that met inclusion suitable to this review. Full texts were obtained, with exclusion of obviously irrelevant titles, abstracts, reviews or literature. The independent findings were then cross-examined and assessed against the eligibility criteria. A third reviewer (TU) then made further assessment and agreement, with resolve of any doubt or disagreement prior to the submitted work. English language articles published in indexed journals have been considered along with unpublished works and ‘Grey’ literature considered.
2.4 Database Searches
Medline, Embase, CINAHL, were searched, with combinations of subject headings, Boolean terms and Text words agreed from an initial scoping search ensuring a sensitive search. A supplementary search was conducted using NHS evidence and, clinical trials registries, and the international clinical trials registry platform WHO, and the U.K. clinical trials gateway NHIR, with the view to negate publication bias, whereby published papers tend to show the positive effect of an intervention, rather than the negative effect [29, 30]. A hierarchy of evidence framework has been used to aid in the evaluation and reduction of bias of included papers, and in acknowledgement of evidence-based healthcare (i.e. Background information/ expert opinion, case-controlled studies, cohort studies, RCTs etc.). In support of this notion, the included papers provide for a broad range of research methods [31]. No restrictions were placed on type of ECG device (manufacturer or model), algorithm or signal processing.
N.B. The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
3. Results
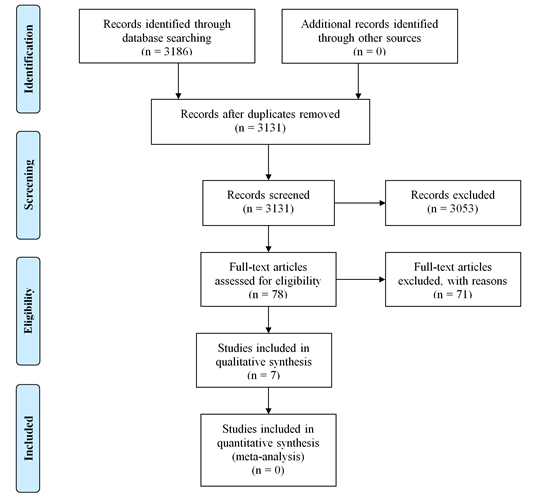
A total of 3186 articles were identified from the initial search strategy, reducing to 3131 after duplicates were removed. Full text screening was performed utilising NICE Healthcare Database Advance Search (HDAS) [24] was conducted on 78 articles, according to the eligibility criteria, which resulted in 7 included studies, Table 1 (Systematic Review Synthesis and Data Extraction) and Figure 4, PRISMA flow diagram, detailing searches strategy of systematic review.
3.1 Data Extraction and Synthesis
Four themes were derived from the Systematic Review Synthesis and Data Extraction Table 1. The chief characteristics of included studies and themes derived are as follows:
3.2 Theme 1 - Misplacement of Electrodes
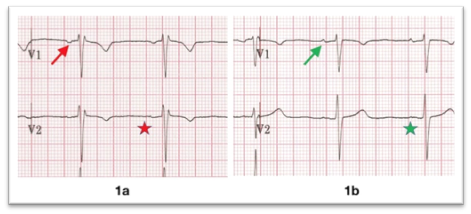
It is well documented within the literature that misplacement of precordial electrodes is long-standing, continues to remain a common occurrence and finding that, so far, has not been effectively addressed [13]. Of concern, are the subsequent clinical and diagnostic/prognostic ramifications for the patient [28]. The findings of this review support this notion, with V1 and V2 being consistently erroneously misplaced superiorly in the 2nd intercostal space rather than in the 4th intercostal space at the right sternal border and left sternal border respectively, Figure 2 [13, 10, 26, 14, 28, 32]. Potentially harmful treatment and/or therapeutic procedures may ensue. Typically, erroneous electrode placement has the potential to affect and alter ECG waveform morphology, clinical interpretation, lead to misclassification of ischemic changes, and a misdiagnosis of arrhythmia [10, 13, 14, 26, 28] Consequently, superior misplacement of V1 and V2 spearheads to spurious ECG abnormalities that may include: poor R-wave progression; ventricular hypertrophy; anteroseptal infarct; QRS complex and T-wave alterations; incomplete right bundle branch block (IRBBB); false positive and false negative ischemic changes and Type 2 Brugada syndrome [14, 27, 28].
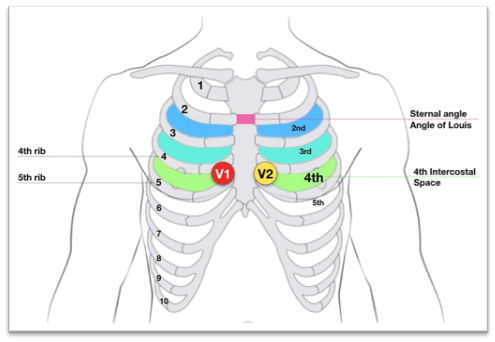
A confounding factor and one worthy of consideration is, almost all of the included papers allude to the frequency of misplaced precordial leads V1-V6 [10, 13, 14, 26, 28]. Reasons for such erroneous placement are multi-factoral and can include poor training, a lack of appreciation of consequences of misplacement, a failure to understand and utilise anatomical landmarks such as the sternal notch (Manubriosternal joint/Angle of Louis), and the Xiphoid process for correct identification of the 4th intercostal space, Figure 3 [27]. Furthermore, levels of undress and the desire to preserve patient modesty, particularly in females, are factors that evidence significant impact. Fewer cardiac investigations are evidenced in women with ACS than in men. Subsequently, such inequities result in less treatment and prove potentially detrimental. It is postulated that particularly amongst paramedics, operator error is compounded by a hesitancy to expose the female breast. The connotation that the female breast is a secondary sexual organ provides ensuing embarrassment [25].
Figure 2: (1a) V1 and V2 are placed too high, the P wave in V1 is fully negative (red arrow), and the P wave in V2 is biphasic (red star); (1b) Placed at their proper location, V1 shows a mostly-upright biphasic P (green arrow) and a fully upright P in V2 (green star). Courtesy of Life In The Fast Lane (2020).
3.3 Theme 2 - Anatomical Differences
Anatomical differences between male and female patients provide additional challenges in electrode placement and accurate ECG acquisition. SCST guidelines and recommendations state, by convention electrodes V4, V5 and V6 ought to be placed beneath the breast when breast tissue overlies the correct anatomical positions [19]. A study conducted by Wallen et al., (2013) [25] noted 52% of women preferred electrodes placed on the breast tissue, deeming it less intrusive, 38% were indifferent and 10% preferring under the breast [25]. Review of the wider literature and that of the included studies of this review allude to difficulties, particularly on women with large breast tissue mass and, in obese patients, in accurately identifying bony landmarks as anatomical reference points to aid in the correct placement of electrodes. However, current evidence pertaining to misplacement because of women’s breast tissue and obesity is inconclusive and warrants further investigation [13, 27, 28].
In contrast, a prospective observational study by McCann et al., (2007) [10] evidenced greater lateral chest electrode discordance (V4-V6), irrespective of gender, than those of central chest electrodes (V1-V3), however, identification of anatomical landmarks and accurate location were impeded particularly in older, larger women and the obese [10, 27]. This was further supported by the findings of the PULSE multi-site randomised clinical trial, (2018), where < 50% of both male and female participants were found to have accurate electrode placement [26]. PULSE concluded no significant difference in accuracy for precordial electrode placement between men and women. Inter-operator variability, even among senior clinicians, is a factor widely acknowledged for the occurrence of electrode misplacement [10]. Causes of misplacement extend to both modifiable and non-modifiable patient factors, such as body habitus, body position, lack of anatomical awareness, lack of confidence, competence or even over confidence [10, 13]. However, confidence is no substitute for competence [19]. Cardiologists in particular fall prey to such over confidence. Assuming the position of V1 and V2 electrodes in the 2nd intercostal space rather than that of the 4th, which may arise from a complacency through regularly listening to auscultations of heart sounds at 2nd intercostal level [13].
3.4 Theme 3 - Clinical Impact on Diagnosis, Treatment & Management
Correlation between misplaced precordial electrodes with changes to ECG morphology dominates the theme of the majority of papers included in this review. Such alterations have the potential to significantly impact clinical interpretation and diagnosis, leading to over, under or even a missed diagnosis. Conversely, superior misplacement of V1 and V2 has proven beneficial in the detection of ST-segment elevation myocardial infarction (STEMI), Non-ST-segment elevation myocardial infarction (NSTEMI) and Brugada syndrome, with no noted significant change to specificity [28]. However, studies have purported a shift in placement by as little as 2cm; can affect interpretation and diagnosis in as much as 17-24% of patients [27].
3.5 Theme 4 - Education & Training
Overarching consensus of included papers, place education and training as tantamount, and of paramount importance to accurate ECG acquisition. Thus, optimising sound clinical diagnosis and practice. Implementation and adherence to SCST and the American Heart Association (AHA) guidelines, yields significant improvement [14, 26] Correct identification of anatomical landmarks, notably, the sternal notch (Angle of Louis), Xiphoid process and the 4th intercostal space for the correct placement of electrodes is essential in the undertaking of ECG. This coupled with on-line education and strategies to change current erroneous practice, through raising awareness and knowledge, are fundamental to good clinical practice, quality of care and outcomes for patients, with a reduction in patient morbidity and mortality [10, 26].
4. Discussion
Types of studies included randomised controlled trials (RCT), systematic reviews, literature reviews and observational studies. Studies were identified irrespective of design, complexity, aims and time of follow-up or hypotheses. Of note, the overriding theme and consensus of the included papers allude to the frequency, commonality and potential for erroneous recordings owing to ECG electrode misplacement. As aforementioned, V1 and V2 are most commonly misplaced anatomically superiorly, with V4 - V6 misplaced inferiorly. The majority of reviewed papers acknowledge the frequency of misplaced precordial electrodes and leads. Subsequently, this results in alteration of ECG waveform morphology, misclassification of ischemic changes and erroneous clinical interpretation. Consensus further points to operator error, with inability to correctly identify intercostal spaces and accurate placement of electrodes, as the overriding underpinning factor for such error. Anatomical differences prove challenging and are factors compounded by obesity and breast tissue mass particularly in women.
5. Limitations
The inclusion criteria for this review included English language articles, international papers, and unpublished works. However, the authors acknowledge that the reviews findings are limited, despite supplementary searching, and that no guarantee can be assigned that all relevant literature has been included. It is further acknowledged that there are inaccessible papers and/ or ‘Grey’ literature that authors did not have rights over.
6. Conclusion
This review has identified that electrode misplacement is well documented, common, ongoing and prevalent throughout healthcare. Misplacement of precordial electrodes is synonymous with erroneous acquisition and significantly alters ECG waveform morphology, leading to misinterpretation and the potential to alter diagnosis. Therefore, correct anatomical placement of the ECG electrodes is in fact essential to diagnosis in the clinical setting. Reasons for misplacement are as aforementioned multifaceted, however the recommendation is that peer-led educational intervention with mandatory training is essential to improve practice and thereby enhance patient safety and outcome. Whilst the topic of this review may not be wholly novel, and its’ conclusions not entirely surprising, it is however fundamental and imperative to acknowledge that as health care providers and practitioners, we have a responsibility and duty to ensure our practice is of the highest calibre. The seemingly mundane task of correct anatomical electrocardiogram electrode placement is in fact relevant and pertinent to erroneous/artefact free, accurate diagnosis of patients and should not be taken for granted neither overlooked.
Key Points and Recommendations
- Precordial electrodes V1 &V2 are most misplaced
- Operator error, anatomical differences including obesity and breast tissue mass influence electrode misplacement
- Misplacement of electrodes can lead to a misdiagnosis, a missed diagnosis, under or over diagnosis
- Educational intervention through peer-led training is essential.
Declarations
- Ethics approval and consent to participate - ‘Not Applicable’
- Consent for publication - ‘Not Applicable’
- Availability of data and materials - The datasets generated and/or analysed during the current study are available in the National Institute for Health and Clinical Excellence (NICE), Healthcare Databases Advanced Search (HDAS) (2019) [Online]. Available: http://www.nice.org.uk/ (accessed 25 October 2019) repository.
- Competing interests - The authors declare that they have no competing interests.
- Funding - This review has been self-funded.
Authors' contributions - Author Details
AH1, SM2, TU3, KO4
- Chief Cardiac Physiologist, Royal Cornwall Hospitals NHS Trust, Truro, Cornwall.
- Interventional Cardiology Registrar, Royal Cornwall Hospitals NHS Trust, Truro, Cornwall.
- Consultant Cardiologist, Royal Cornwall Hospitals NHS Trust, Truro, Cornwall.
- Librarian Specialist, Royal Cornwall Hospitals NHS Trust, Truro, Cornwall.
All persons who meet authorship criteria are listed as authors and have participated sufficiently in the work to take responsibility for the content, including participation in the concept, design, analysis, writing, or revision of the manuscript. Outlining everyone's contribution, conception or design performed by Alexandros Hadjiantoni. Data collection was performed by Alexandros Hadjiantoni and Siddhartha Mengi. Article drafting was performed by Alexandros Hadjiantoni and Siddhartha Mengi. Critical revision of the article was performed by Siddhartha Mengi and Tamas Ungvari. Furthermore, each author certifies that this material or similar material has not been and will not be submitted to or published in any other publication.
Acknowledgements
This manuscript has been released as a pre-print at source,
https://www.researchsquare.com
Citation, rs-74147/v1
https: //www.researchsquare.com/ rs-74147/v1
The authors extend their gratitude to Dr. Judit Ungvari and librarian specialist, Mrs. Katy Oak for their expertise and insight.
Competing Interests
There are no conflicts of interest to declare. The authors declare that they have no competing interests.
References
- Jones DS, Greene JA. The decline and rise of coronary heart disease: understanding public health catastrophism. Am J Public Health 103 (2013): 1207-1218.
- Fisher EA, Lee J. Coronary Artery Disease. [Internet]. Dallas: American Heart Association (2015).
- Mahmoodzadeh S, Moazenzadeh M, Rashidinejad H, et al. Diagnostic performance of electrocardiography in the assessment of significant coronary artery disease and its anatomical size in comparison with coronary angiography. J Res Med Sci 16 (2011): 750-755.
- Keogh JE, Reed D. Schaum’s outline of ECG interpretation. New York: McGraw-Hill (2011).
- Klabunde RE. Cardiovascular physiology concepts. 2nd Philadelphia: Wolters Kluwer (2012).
- Bayes de Luna A. Clinical electrocardiography: a textbook. 4th Chichester: Wiley-Blackwell (2012).
- Kligfield P, Gettes LS, Bailey JJ, et al. Recommendations for the standardization and interpretation of the electrocardiogram: part I: The electrocardiogram and its technology: a scientific statement from the American Heart Association Electrocardiography and Arrhythmias Committee, Council on Clinical Cardiology; the American College of Cardiology Foundation; and the Heart Rhythm Society: endorsed by the International Society for Computerized Electrocardiology. Circulation 115 (2007): 1306-1324.
- Lynch R. ECG lead misplacement: a brief review of limb lead misplacement. Afr J Emerg Med 4 (2014): 130-139.
- Pearce A. Examining the causes and effects of electrode misplacement during electrocardiography: a literature review. Br J Card Nurs 14 (2019): 1-15.
- McCann K, Holdgate A, Mahammad R, et al. Accuracy of ECG electrode placement by emergency department clinicians. Emerg Med Australas 19 (2007): 442-448.
- Kaur I, Rajni R, Marwaha AJ. ECG signal analysis and arrhythmia detection using wavelet transform. Inst. Eng. India Ser. B 97 (2016): 499-507.
- Goldberger AL, Goldberger ZD, Shvilkin A. Goldberger’s clinical electrocardiography: a simplified approach. Philadelphia: Elsevier (2018): 6.
- Rajaganeshan R, Ludlam CL, Francis DP, et al. Accuracy in ECG lead placement among technicians, nurses, general physicians and cardiologists. Int J Clin Pract 62 (2008): 65-70.
- Medani SA, Hensey M, Caples N, et al. Accuracy in precordial ECG lead placement: improving through a peer-led educational intervention. J Electrocardiol 51 (2018): 50-54.
- British Cardiovascular Society. Strategic review of cardiac physiology services In England: final report (2015).
- National Institute for Health and Clinical Excellence. Developing review questions and planning the evidence review [Internet]. London: National Institute for Health and Clinical Excellence (2014).
- Khunti K. Accurate interpretation of the 12-lead ECG electrode placement: A systematic review. Health Educ J 73 (2014): 610-623.
- Bond RR, Finlay DD, Nugent CD, et al. The effects of electrode misplacement on clinicians’ interpretation of the standard 12-lead electrocardiogram. European Journal of Internal Medicine 23 (2012): 610-615.
- Campbell B, Richley D, Ross C, et al. Clinical Guidelines by Consensus: Recording a standard 12-lead electrocardiogram: an approved method by the Society for Cardiological Science and Technology (SCST) (2014).
- Apoorv G, Kaur M. ECG analysis using Continuous Wavelet Transform (CWT): IOSR J Eng 2 (2012): 632-635.
- Critical Appraisal Skills Programme. CASP 12 questions to help you make sense of a cohort study checklist. [Internet]. Oxford: CASP (2020).
- Nursing and Midwifery Council. ‘The code’: professional standards of practice and behaviour for nurses and midwives. London: Nursing and Midwifery Council (2015).
- Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) [Internet]. Ottawa, Ca:PRISMA (2015).
- National Institute for Health and Clinical Excellence (NICE). Healthcare Databases Advanced Search (HDAS) [Internet]. London: NICE (2020).
- Wallen R, Tunnage B, Wells S. The 12-Lead ECG in the emergency medical service setting: how electrode placement and paramedic gender are experienced by women. EMJ 31 (2014): 851-852.
- Davis LL, Funk M, Fennie KP, et al. Does accuracy of V lead electrode placement differ based on gender of patient: results of the practical use of the latest standards of electrocardiography (PULSE) trial. Circulation 134 (2016): A16195.
- Day K, Oliva I, Krupinski E, Marcus F. Identification of 4th intercostal space using sternal notch to xiphoid length for accurate electrocardiogram lead placement. J Electrocardiol 48 (2015): 1058-1061.
- Walsh B. Misplacing V1 and V2 can have clinical consequences. The Am J Emerg Med 36 (2018): 865-870.
- Aveyard H. Doing a literature review in health and social care: a practical guide. 3rd Berkshire: Open University Press (2014).
- Walker Sharon. Literature Reviews: Generative and Transformative Textual Conversations [21 paragraphs]. Forum Qualitative Sozialforschung / Forum: Qualitative Social Research 16 (2015).
- Evans D. Hierarchy of evidence: a framework for ranking evidence evaluating healthcare interventions. J Clin Nurs 12 (2003): 77-84.
- Bond RR, Finlay DD, Nugent CD, et al. A simulation tool for visualizing and studying the effects of electrode misplacement on the 12-lead electrocardiogram. Journal of Electrocardiology [online] 44 (2011): 439-444.


 Impact Factor:
* 5.6
Impact Factor:
* 5.6
 Acceptance Rate:
74.36%
Acceptance Rate:
74.36%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
