Lifestyle Modification-Improving Systemic Athero-Protective Factor, Circulating Pentraxin 3, in High-Risk Patients with Metabolic Syndrome
Taiki Tojo1, Minako Yamaoka-Tojo2 *
1Sagamihara Kyodo Hospital, Sagamihara, Japan
2Kitasato University School of Allied Health Sciences, Sagamihara, Japan
*Corresponding Author: Minako Yamaoka-Tojo, MD, PhD, 1-15-1 Kitasato, Minami-ku, Sagamihara 252-0373, Japan
Received: 24 February 2021; Accepted: 03 March 2021; Published: 10 March 2021
Article Information
Citation: Taiki Tojo, Minako Yamaoka-Tojo. Lifestyle Modification-Improving Systemic Athero-Protective Factor, Circulating Pentraxin 3, in High-Risk Patients with Metabolic Syndrome . Cardiology and Cardiovascular Medicine 5 (2021): 201-212.
View / Download Pdf Share at FacebookAbstract
Background: Metabolic syndrome (MetS) is associated with an increased risk of developing atherosclerotic cardiovascular diseases (CVD). C-reactive protein (CRP) and serum amyloid protein are recognized as classic short pentraxins, whereas pentraxin 3 (PTX3) belongs to the long pentraxins. PTX3 is an acute phase protein, which is strongly expressed by advanced atherosclerosis lesions as a primary inflammatory response in association with macrophage and neutrophil infiltration. We hypothesized that circulating PTX3 could be a useful biomarker to enhance the effects of lifestyle modification on systemic inflammation in patients with MetS.
Methods: To examine the relationship between circulating PTX3 and MetS risk scores, we measured circulating PTX3 in 86 high-risk cardiovascular disease patients with or without MetS before and after lifestyle modification. Circulating levels of PTX3 were measured using ELISA.
Results: All subjects had similar reductions in weight, waist circumference, and blood pressure. Circulating PTX3 was significantly decreased in MetS patients (P < 0.001) and was inversely correlated with the accumulation of MetS risk scores (r = -0.533, P < 0.001), and was correlated with high-density lipoprotein (HDL) cholesterol, the presence of diabetes mellitus, and white cell count, but not with waist circumference, body mass index (BMI), or CRP. An increase in PTX3 levels were significantly correlated with the levels of baseline BMI, waist circumference, circulating PTX3 concentration, and MetS risk scores.
Conclusions: Lifestyle modification increased circulating levels of PTX3 in relation to the accumulation of MetS risk scores in high-risk patients with MetS, who have reduced levels of PTX3, independent of CRP. These data suggest that circulating PTX3 may be an effective novel biomarker that helps to predict the effectiveness o
Keywords
<p>Metabolic Syndrome; PTX3</p>
Article Details
1. Background
Metabolic syndrome (MetS) is a major public health issue and associated with an increased risk of developing atherosclerotic cardiovascular diseases (CVD) [1] . The mechanism of which may be mediated at least in part, by increased secretion of proinflammatory cytokines by adipose tissue and dysfunctional vascular endothelium [2].
Pentraxin 3 (PTX3) belongs to the long pentraxins, whereas C-reactive protein (CRP) and serum amyloid protein (SAP) are recognized as classic short pentraxins. CRP and SAP are released by the liver in response to interleukin-6. On the other hand, PTX3 is produced by a variety of tissues, such as vascular endothelial cells, macrophages, and neutrophils, predominantly in response to proinflammatory signallings. PTX3 is strongly expressed by advanced human atherosclerosis lesions of autopsy specimens by immunohistochemistry, in association with macrophage and neutrophils infiltration [3]. This focal localization of PTX3 is considered to be indicative of primary inflammation stimuli, in contrast to CRP which is induced via secondary inflammatory signals [4-10]. PTX3 has athero-protective effects through the modulation of the immune-inflammatory balance in the cardiovascular system. According these previous data, we hypothesized that circulating PTX3 could be a useful biomarker for systemic inflammation in patients with MetS.
2. Methods
2.1 Subjects
The study included 86 Japanese high-risk outpatients of CVD consulted for medical care to lose their weight for improving their CVD risk factors from cardiologists into the Metabolic Syndrome Clinic, Department of Cardioangiology, Kitasato University Hospital. Fifty-two patients with MetS and 34 non-obese patients (waist circumference < 85 cm for men, < 90 cm for women) having more than one coronary risk factors were enrolled. As a reference, 15 control subjects without coronary risk factors were also enrolled. All subjects gave informed consent before participating in this study and anonymity was maintained by tracing the patients through their clinical history number. The project was approved by the Scientific and Ethical Committee of the Kitasato University School of Medicine, Japan. To determine the relationship between circulating PTX3 and MetS risk factors, we measured baseline PTX3 levels in high-risk patients of CVD. Systolic and diastolic blood pressure was measured after a rest for at least 15 minutes with a sphygmomanometer in sitting position.
2.2 Definition for metabolic risk scores
Mtabolic risk scores were calculated using MetS components according to the Japanese MetS criteria [11]. The score consisted of four independent components as abdominal obesity, defined as a waist circumference ≥ 85 cm in men or ≥ 90 cm in women; hypertriglyceridemia and/or low HDL-cholesterolemia; hypertension, and elevated fasting glucose. The diagnosis of hypertension was established based on blood pressure levels measured at the study visit (≥ 130/85 mmHg) or a prior diagnosis of hypertension and current treatment with antihypertensive medications. Diabetes/ impaired fasting glucose was considered present if the subject had history of diabetes or had a fasting glucose level of 110 mg/dL or greater. Patients with abdominal obesity having more than two metabolic scores were defined as MetS. There were 52 patients diagnosed as having MetS and the remaining 34 patients as non-MetS, defined as having more than one component of the MetS criteria without abdominal obesity.
2.3 Blood sample collection and measurement of clinical biomarkers
Blood samples were collected by venipuncture after an overnight fast from 52 MetS patients, 34 high-risk patients of CVD without abdominal obesity, and 15 healthy control subjects. Biochemical markers, such as triglyceride, LDL cholesterol, HDL cholesterol, insulin, plasma glucose, glycated haemoglobin (HbA1c), uric acid, gamma-glutamyl transpeptidase (g-GTP), CRP, and BNP were measured.
2.4 Lifestyle modification
Moreover, to examine whether circulating PTX3 could be a useful biomarker or not to enhance the effects of lifestyle modification in high-risk patients with MetS, we analyzed change levels of PTX3 in those patients before and after the lifestyle modification. We studied 52 patients with MetS (average BMI 32.6) and 34 patients with non-obese patients having high-risk for CVD, termed non-MetS patients (average BMI 26.5). All subjects were instructed a standard mild energy-restricted diet and engaged in walking at least 30 min a day, 5days a week. Serum PTX3 and adiponextin were measeured in those subjects before and after the lifestyle modification for 8 to 46 weeks (average 21.0 weeks).
2.5 Measurement of cytokines
Circulating serum levels of human PTX3 and adiponectin were determined by enzyme-linked immune sorbent assay (ELISA) using the Human Pentraxin 3 / TSG-14 ELISA System (Perseus Protepmics Inc., Tokyo, Japan) and the CircuLexTM human adiponectin ELISA Kit (CycLex Co., Ltd., Nagano, Japan), respectively. Samples were processed according to the manufacturer’s instructions.
2.6 Statistical analysis
Continuous data were summarized as either mean ± SD or median and quartiles, and categorical data were expressed as percentages. Data were compared by unpaired t- test or Mann-Whitney U-test where appropriate. Differences in proportions of variables were determined by chi-squared analysis. To evaluate the correlations between PTX3 and selected variables, we calculated Spearman correlation coefficients between circulating levels of PTX3 and the following variables: 1) conventional risk factors for cardiovascular disease (LDL cholesterol, HDL cholesterol, triglyceride, HbA1c, presence of hypertension, and current smoking), and history of coronary artery disease; 2) measures of adiposity and insulin resistance (BMI, waist circumference, fasting blood glucose, insulin level, and HOMA-IR); and 3) metabolic risk scores (abdominal obesity, hypertension, high triglycerideand/or low HDL cholesterol, and glucose intolerance or diabetes) and MetS-related co-morbidity (hyper uric academia, fatty liver disease, chronic kidney disease, and sleep apnea syndrome). To evaluate the association of PTX3 with MetS, we constructed multivariable logistic regression models to assess whether circulating PTX3 was independently associated with MetS. Two-sided P-values < 0.05 were considered significant.
3. Results
3.1 Circulating PTX3 was significantly increased in high-risk patients for cardiovascular disease
To determine whether or not circulating levels of PTX3 could be a specific biomarker to distinguish high-risk patients for CVD, we studied 86 patients having coronary risk factors (average BMI 30.6, average age 53.5) and 15 healthy control subjects (average BMI 23.2, average age 52.1). Serum levels of PTX3 were significantly elevated in patients with atherosclerotic-prone compared with healthy control subjects (3.8 ± 4.1 vs. 1.6 ± 0.6 ng/mL, P < 0.05).
3.2 Circulating PTX3 was decreased in patients with atherosclerotic-prone associated with the accumulation of MetS risk scores
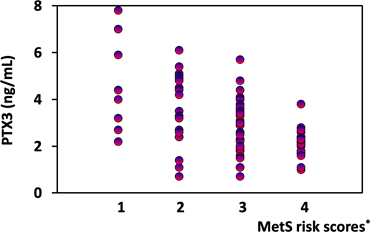
When 86 patients with atherosclerotic-prone were classified with MetS risk scores, consisting of obese, hypertension, diabetes/fasting high glucose, and dyslipidemia (high triglyceride and/or low HDL cholesterol), circulating PTX3 was decreased according to the relation with the accumulation of MetS risk scores (Figure 1).
Circulating PTX3 was reduced in patients having high MetS risk scores.
* MetS risk scores: obese (BMI > 25 or waist circumference > 90 cm), hypertension, diabetes/fasting high glucose, and dyslipidemia (high triglyceride and/or low HDL- cholesterol). According to a previous paper, plasma level of PTX3 in normal Japanese healthy subjects is average 1.87 ng/mL in men and 2.14 ng/mL in women [10].
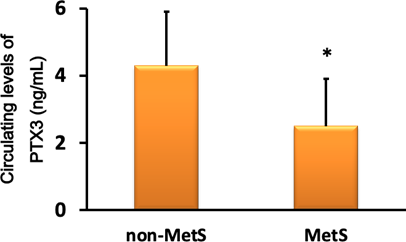
As expected, circulating levels of PTX3 was significantly decreased in MetS patients rather than non-MetS patients (Figure 2). Circulating PTX3 was inversely correlated with the accumulation of MetS risk scores (r = -0.539, P < 0.001), BMI (r = -0.295, P< 0.01), and waist circumference (r = -0.343, P < 0.005). In contrast, PTX3 was positively correlated with serum levels of total bilirubin (r = 0.379, P < 0.001), uric acid (r = 0.247, P < 0.05), male (r = 0.269, P < 0.05), and the presence of diabetes mellitus/fasting high glucose, hypertension, dyslipidemia, coronary artery disease, or current smoking (respectively, P < 0.001). Interestingly, circulating levels of PTX3 was no correlated with CRP or white blood cell counts.
Circulating levels of PTX3 was significantly decreased in MetS patients rather than non-MetS patients. Values are means ± SD. * P < 0.05. MetS, metabolic syndrome; PTX3, pentraxin 3; non-MetS, non-obese patients having risk factors for cardiovascular disease.
3.3 Circulating PTX3 was relatively decreased in patients with MetS compared to non-obese patients having coronary risk factors
There were 52 patients diagnosed as having MetS (average BMI 32.6) and the remaining 34 patients as non-MetS (BMI 26.5), defined non-obese patients for atherosclerotic-prone as having more than one component of the MetS criteria proposed by the Japanese Society of Internal Medicine [11]. The baseline characteristics are shown in Table 1. When patients were divided into two groups with or without obesity, body mass index, body weight, and waist circumferences were increased in MetS patients compared to non-obese patients having risk factors for cardiovascular disease, which defined as “non-MetS patients”.
|
MetS (n=52) |
Non-MetS (n=34) |
|
|
Age (years) |
54.5 ± 13.9 |
50.3 ± 16.1 |
|
Male/Female |
32 / 20 |
20 / 4 |
|
BMI (kg/m2) |
32.6 ± 5.9 |
26.5 ± 6.1 * |
|
Body weight (kg) |
87.5 ± 18.9 |
73.5 ± 12.9 * |
|
Waist (cm) |
105.2 ±12.7 |
92.3 ± 11.9 |
|
Systolic BP (mmHg) |
134.0 ± 17.3 |
130.1 ± 18.2 |
|
Diastolic BP (mmHg) |
77.9 ± 12.5 |
75.7 ± 12.6 |
Values are means ± SD. * P < 0.05. MetS, metabolic syndrome; BMI, body mass index; BP, blood pressure; non-MetS, non-obese patients having risk factors for cardiovascular disease.
Table 1. Baseline characteristics.
Predictably, patients with MetS had higher BMI, body weight, and waist circumference at baseline. As shown in Table 2, serum triglyceride and fasting glucose were significantly higher in MetS patients than in non-MetS patients. As expected, HDL cholesterol levels were significantly reduced in MetS patients. Naturally enough, a large proportion of MetS patients have hypertension, diabetes/fasting high glucose, and dyslipidemia.
|
MetS (n=52) |
Non-MetS (n=34) |
|
|
Triglyceride (mg/dL) |
212 ± 182 |
156 ± 134 * |
|
HDL-C (mg/dL) |
49.6 ± 11.9 |
57.2 ± 13.9 |
|
Glucose (mg/dL) |
125 ± 34 |
104 ± 15 * |
|
MetS risk scores |
3.3 ± 0.6 |
1.7 ± 0.9 * |
|
High BP (%) |
48 (92.3%) |
20 (58.8%) |
|
High TG/low HDL-C (%) |
41 (78.8%) |
18 (52.9%) |
|
DM/High glucose (%) |
32 (61.5%) |
5 (14.7%) * |
Values are means ± SD. * P < 0.05. MetS, metabolic syndrome; HDL-C, high density lipoprotein-cholesterol; BP, blood pressure; TG, triglyceride; DM, diabetes mellitus; non-MetS, non-obese patients having risk factors for cardiovascular disease.
Table 2: Baseline characteristics and MetS risk scores.
As shown in Figure 2, circulating PTX3 was significantly decreased in patients with MetS rather than non-MetS (P < 0.05). In MetS patients, the presence of dyslipidemia (high LDL cholesterol, high triglyceride, and/or low HDL cholesterol) was negatively correlated to serum PTX3 (r = -0.302, P < 0.05), but not the statin usage. As concerns sex, circulating levels of PTX3 was positively correlated with male in MetS patients (61.5% male, r = 0.336, P < 0.05) and in all subjects (60.5% male, r = 0.269, P < 0.05).
3.4 Lifestyle modification increased reduced PTX3 in patients with MetS
An increase in PTX3 levels were significantly correlated with the levels of baseline BMI, waist circumference, circulating PTX3 concentration, and MetS risk scores. As shown in Table 3, waist circumferences and systolic/diastolic blood pressure were significantly lowered by lifestyle modification for average 21 weeks in these patients.
|
Before |
After |
|
|
BMI (kg/m2) |
30.6 ± 6.0 |
29.8 ± 5.8 |
|
Body weight (kg) |
82.5 ± 20.2 |
81.0 ± 18.6 |
|
Waist (cm) |
100.9 ± 14.5 |
96.0 ± 13.4 * |
|
Systolic BP (mmHg) |
131.8 ± 17.7 |
123.6 ± 13.2 * |
|
Diastolic BP (mmHg) |
76.3 ± 13.0 |
71.0 ± 11.3 * |
|
Duration (weeks) |
21.0 ± 9.9 (8-46) |
|
Values are means ± SD. * P < 0.05 vs. before lifestyle modification (n = 86). MetS, metabolic syndrome; BMI, body mass index; BP, blood pressure.
Table 3: Change in anthropometric variables.
There was no difference in circulating levels of PTX3 in all subjects before and after lifestyle modification. Only serum adiponectin levels were increased after lifestyle modification (Table 4).
|
Before |
After |
|
|
Triglyceride (mg/dL) |
189 ± 164 |
175 ± 02 |
|
HDL-C (mg/dL) |
52 ± 13 |
54 ± 13 |
|
Glucose (mg/dL) |
119 ± 33 |
113 ± 37 |
|
Uric acid (mg/dL) |
6.1 ± 1.8 |
6.0 ± 1.5 |
|
Adiponectin (µg/mL) |
5.6 ± 3.1 |
6.7 ± 3.2 * |
|
CRP (mg/dL) |
0.31 ± 0.50 |
0.28 ± 0.27 |
|
PTX3 (ng/mL) |
3.5 ± 4.1 |
3.0 ± 1.5 |
Values are means ± SD. * P < 0.05 vs. before. MetS, metabolic syndrome; BMI, body mass index; BP, blood pressure; non-MetS, non-obese patients having risk factors for cardiovascular disease.
Table 4: Changes in metabolic and inflammatory biomarkers.
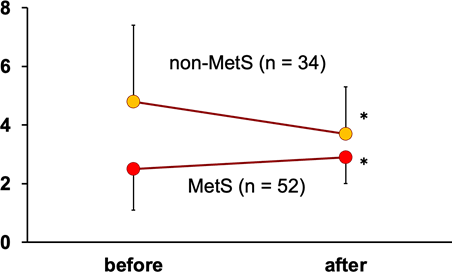
When patients were divided into two groups, MetS group or non-MetS group, circulating PTX3 was significantly reduced in non-MetS group after 21-weeks lifestyle modification (Figure 3). On the other hand, PTX3 was significantly increased in patients with MetS after lifestyle modification.
Circulating levels of pentraxin 3 (PTX3) were significantly lowered by lifestyle modification for average 21 weeks in non-MetS patients, but not in MetS patients. Values are means ±SD. * P < 0.05 vs. before in each group. MetS, metabolic syndrome; non-MetS, non-obese patients having risk factors for cardiovascular disease.
4. Discussion
The present study demonstrates that for the first time, to the best of our knowledge, circulating PTX3 could be a useful biomarker to distinguish high-risk MetS patients for CVD from non-MetS patients. Furthermore, lifestyle modification increased circulating PTX3 in patients with MetS having relatively low levels of PTX3.
4.1 PTX3 and vascular inflammation
In the last decade, accumulating evidence suggested the striking relevance of a low but chronic inflammatory state in obesity and MetS. Research of recent years revealed a role of adipose tissue beyond energy storage harboring inflammatory cells which are believed sustain inflammation and impair adipocyte function [12, 13]. PTX3 was originally found as an essential component of innate immunity, and is correlated with various atherosclerosis- and vascular function-related surrogate markers [14]. PTX3 is produced by immune cells and vascular cells in response to proinflammatory signals, such as inflammatory cytokines, HDL-cholesterol. And oxidized LDL-cholesterol [15, 16]. Excessive ROS production may affect PTX3 production by adipocytes in obese individuals and in MetS patients [17]. PTX3 concentrations are increased in patients with type 2 diabetes, obesity, or polycystic ovary syndrome [18-20].
4.2 PTX3 and metabolic syndrome
Metabolic syndrome is a cluster of risk dfactors including glucose intolerance, dyslipidemia, hypertension, and abdominal obesity. In addition, circulating PTX3 was correlated with the severity of MetS, with other inflammatory parameters and cardiovascular tests [21]. In addition, elevated circulating levels of PTX3 has been reported to be closely associated with moderate to severe obstructive sleep apnea syndrome [22]. According the previous study, the receive operating characteristic (ROC) curve analysis for plasma PTX3 identified a cut-off value of 10.7 ng/dL that differentiates between mild and severe MetS [21].
Paradoxically, the circulating levels PTX3 levels was inversely associated with MetS, overweight/obesity, and parameters of dyslipidemia, suggesting a cardioprotective role of PTX3 in atherosclerosis [23]. Our result also suggests that circulating levels of PTX3 were inversely correlated with the accumulation of MetS components. Moreover, it was reported that PTX3 was negatively associated with the cardiovascular risk factors of atherosclerosis, contrary to CRP [23]. In our present study, circulating levels of PTX3 were significantly reduced after lifestyle modification with synergistically reduction in serum CRP, plasma glucose, and triglyceride in patients with pre-MetS.
4.3 PTX3 as a therapeutic biomarker to enhance coronary risk factor management in MetS
Growing body of evidence supports an important role of PTX3 in the pathogenesis of MetS and atherosclerosis. Increasing levels of PTX3 is strongly associated with vascular endothelial dysfunction in patient with non-alcoholic fatty liver disease (NAFLD) [24]. NAFLD is also strongly associated with atherosclerosis and cardiovascular diseases.
Although circulating levels of PTX-3 have been found to be elevated in patients with vasculitis[4], acute myocardial infarction [25], systemic inflammation or sepsis [26], psoriasis, unstable angina pectoris, and heart failure [6, 27-29]. Our data suggests that PTX3 expression could reduce ROS production by human visceral adipocytes. Thus, PTX3 may reflect a higher inflammatory status associated with increased number of components comprising pre-MetS conditions [30].
5. Study Limitations
We would like to discuss a weakness of the study: a study limitation is that the study cohort is comparably small. Since circulating levels of PTX3 correlated well with waist circumference in patients with MetS and pre-MetS conditions, it is reasonable to speculate that there might also be a difference between groups if group size would be bigger. However, group sizes for lifestyle modification were powerful enough to reveal significant differences for a change in circulating levels of PTX3 and other inflammatory biomarkers.
6. Conclusions
In summary, relatively low circulating levels of PTX3 were associated with accumulations of MetS risk scores and other MetS-related comorbidity, independent of CRP, LDL cholesterol, or HbA1c. Circulating PTX3 may be a novel biomarker for high-risk patients with metabolic syndrome, and further studies are warranted to assess its utility as a predictor of incident MetS and atherogenic conditions. These findings suggest a novel pathophysiological mechanism underlying insulin resistance, PTX3 dysfunction, and metabolic syndrome. Moreover, lifestyle modification increased circulating levels of PTX3 in relation to the reduction in waist circumference, vascular inflammation, and blood pressure, suggesting that this degree of circulating PTX3-guided weight management may be effective for cardiovascular benefit and prevention of cardiovascular events.
Competing Interests
The authors declare no conflict interest.
Acknowledgements
This work was partly supported by JSPS KAKENHI grant number JP19K11371.
References
- Grundy SM: Metabolic syndrome pandemic. Arterioscler Thromb Vasc Biol 28 (2008): 629-636.
- Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, et al. Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120 (2009): 1640-1645.
- Savchenko A, Imamura M, Ohashi R, Jiang S, Kawasaki T, et al. Expression of pentraxin 3 (PTX3) in human atherosclerotic lesions. J Pathol 215 (2008): 48-55.
- Fazzini F, Peri G, Doni A, Dell'Antonio G, Dal Cin E, et al. PTX3 in small-vessel vasculitides: an independent indicator of disease activity produced at sites of inflammation. Arthritis Rheum 44 (2001): 2841-2850.
- Latini R, Maggioni AP, Peri G, Gonzini L, Lucci D, et al. Prognostic significance of the long pentraxin PTX3 in acute myocardial infarction. Circulation 110 (2004): 2349-2354.
- Inoue K, Sugiyama A, Reid PC, Ito Y, Miyauchi K, et al. Establishment of a high sensitivity plasma assay for human pentraxin3 as a marker for unstable angina pectoris. Arterioscler Thromb Vasc Biol 27 (2007):161-167.
- Kotooka N, Inoue T, Aoki S, Anan M, Komoda H, et al. Prognostic value of pentraxin 3 in patients with chronic heart failure. Int J Cardiol 130 (2008): 19-22.
- Kotooka N, Inoue T, Fujimatsu D, Morooka T, Hashimoto S, et al. Pentraxin3 is a novel marker for stent- induced inflammation and neointimal thickening. Atherosclerosis 197 (2008): 368-374.
- Suliman ME, Yilmaz MI, Carrero JJ, Qureshi AR, Saglam M, et al. Novel links between the long pentraxin 3, endothelial dysfunction, and albuminuria in early and advanced chronic kidney disease. Clin J Am Soc Nephrol 3 (2008): 976-985.
- Yamasaki K, Kurimura M, Kasai T, Sagara M, Kodama T, et al. Determination of physiological plasma pentraxin 3 (PTX3) levels in healthy populations. Clin Chem Lab Med 47 (2009): 471-477.
- Arai H, Yamamoto A, Matsuzawa Y, Saito Y, Yamada N, et al. Prevalence of metabolic syndrome in the general Japanese population in 2000. Journal of atherosclerosis and thrombosis 13 (2006): 202-208.
- Xu H, Barnes GT, Yang Q, Tan G, Yang D, et al. Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112 (2003): 1821-1830.
- Jung C, Gerdes N, Fritzenwanger M, Figulla HR. Circulating levels of interleukin-1 family cytokines in overweight adolescents. Mediators Inflamm (2010): 958403.
- Vilahur G, Badimon L. Biological actions of pentraxins. Vascul Pharmacol 73 (2015): 38-44.
- Norata GD, Marchesi P, Pirillo A, Uboldi P, Chiesa G, et al. Long pentraxin 3, a key component of innate immunity, is modulated by high-density lipoproteins in endothelial cells. Arterioscler Thromb Vasc Biol 28 (2008): 925-931.
- Magrini E, Mantovani A, Garlanda C. The Dual Complexity of PTX3 in Health and Disease: A Balancing Act? Trends Mol Med 22 (2016): 497- 510.
- Tomandlova M, Jarkovsky J, Tomandl J, Kubkova L, Kala P, et al. Prognostic value of pentraxin-3 level in patients with STEMI and its relationship with heart failure and markers of oxidative stress. Dis Markers 2015 (2015): 159051.
- Netea MG, Joosten LA, Lewis E, Jensen DR, Voshol PJ, et al. Deficiency of interleukin- 18 in mice leads to hyperphagia, obesity and insulin resistance. Nature medicine 12 (2006): 650-656.
- Fischer CP, Perstrup LB, Berntsen A, Eskildsen P, Pedersen BK. Elevated plasma interleukin-18 is a marker of insulin-resistance in type 2 diabetic and non-diabetic humans. Clinical immunology (Orlando, Fla 117 (2005): 152-160.
- Aso Y, Okumura K, Takebayashi K, Wakabayashi S, Inukai T. Relationships of plasma interleukin-18 concentrations to hyperhomocysteinemia and carotid intimal-media wall thickness in patients with type 2 diabetes. Diabetes care 26 (2003): 2622-2627.
- Zlibut A, Bocsan IC, Pop RM, Vesa SC, Bheecarry K, et al. Role of pentraxin-3 in risk assessment of patients with metabolic syndrome. Physiol Int 106 (2019): 283-293.
- Slouka D, Kucera R, Gal B, Betka J, Skalova A. Biomarkers - a possibility for monitoring of obstructive sleep apnea syndrome. Neuro Endocrinol Lett 40 (2019): 85-92.
- Lee R, Ahn HR, Shin MH, Kim HN, Lee YH, et al. Association of Plasma Pentraxin-3 Level with Lipid Levels and Cardiovascular Risk Factors in People with No History of Lipid- Lowering Medication: the Dong-gu Study. Journal of atherosclerosis and thrombosis 26 (2019): 738-745.
- Gurel H, Genc H, Celebi G, Sertoglu E, Cicek AF, et al. Plasma pentraxin-3 is associated with endothelial dysfunction in non-alcoholic fatty liver disease. Eur Rev Med Pharmacol Sci 20 (2016): 4305-4312.
- Latini R, Maggioni AP, Peri G, Gonzini L, Lucci D, et al. Prognostic significance of the long pentraxin PTX3 in acute myocardial infarction. Circulation 110 (2004): 2349-2354.
- Muller B, Peri G, Doni A, Torri V, Landmann R, et al. Circulating levels of the long pentraxin PTX3 correlate with severity of infection in critically ill patients. Critical care medicine 29 (2001): 1404- 1407.
- Bevelacqua V, Libra M, Mazzarino MC, Gangemi P, Nicotra G, et al. Long pentraxin 3: a marker of inflammation in untreated psoriatic patients. Int J Mol Med 18 (2006): 415-423.
- Suzuki S, Takeishi Y, Niizeki T, Koyama Y, Kitahara T, et al. Pentraxin 3, a new marker for vascular inflammation, predicts adverse clinical outcomes in patients with heart failure. American heart journal 155 (2008): 75-81.
- Matsubara J, Sugiyama S, Nozaki T, Sugamura K, Konishi M, et al. Pentraxin 3 is a new inflammatory marker correlated with left ventricular diastolic dysfunction and heart failure with normal ejection fraction. Journal of the American College of Cardiology 57 (2011): 861-869.
- Karakas MF, Buyukkaya E, Kurt M, Motor S, Akcay AB, et al. pentraxin-3 levels are associated with the severity of metabolic syndrome. Med Princ Pract 22 (2013): 274-279.


 Impact Factor: * 5.6
Impact Factor: * 5.6 Acceptance Rate: 74.36%
Acceptance Rate: 74.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 