High Sensitivity Troponin (at 0 & 2 Hrs) in Emergency Department. Will Reducing the Interval Time, Safely Reduce Admissions and Costs?
Imran Tahir
Worcestershire Acute Hospitals NHS, Charles Hastings Way, Worcester WR5 1DD, UK
*Corresponding Author: Imran Tahir, Worcestershire Acute Hospitals NHS, Charles Hastings Way, Worcester WR5 1DD, UK
Received: 27 March 2017; Accepted: 10 April 2017; Published: 12 April 2017
Article Information
View / Download Pdf Share at FacebookAbstract
Background: Every four minutes someone is admitted to hospital suffering from a heart attack or a chest pain event in the UK, totalling over 150,000 hospitalisations a year. Chest pain is one of the most common presentations in the emergency department and quite a few of them get admitted as low risk ACS patients. With the developments in technology, we have increasingly sensitive troponin assays available. Previous-generation troponin assays have been used as diagnostic and prognostic markers in acute coronary syndrome patients and for risk stratification to guide triage decisions and aid in treatment selection. New, high-sensitivity troponin assays represent an important advance with added sensitivity for cardiac myocyte necrosis. High-sensitivity troponin assays detect concentrations of the same proteins that conventional sensitivity assays are aimed at detecting, just in much lower concentrations.
Objective: Can high sensitivity troponin avoid unnecessary admission and save money.
Methods: We did the retrospective data analysis for 300 patients presenting in the emergency department of University hospitals Birmingham in January to March 2016. All adult patients admitted with the diagnosis of suspected ACS were included in the study.
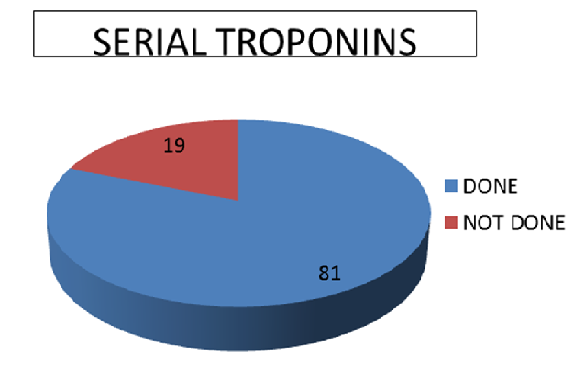
Results: We included 300 patients admitted with the diagnosis of suspected ACS under the medical team. 81% patients had a serial troponin done during the admission. Rest of the 19% had a single troponin done. Only 10.3% patients had a raise in the serial troponin, rest of them were discharged home. The average length of stay was 33 hours.
Conclusion: We have 5-10 patients every day presenting to the emergency department with chest pain. About 50% of them get admitted with the diagnosis of suspected ACS. 81% of our patients could have been potentially disch
Keywords
Acute Coronary Syndrome; High Sensitivity Troponins; Chest Pain
Article Details
Abbreviations
ACS - Acute Coronary Syndrome
AF - Atrial Fibrillation
COPD - Chronic Obstructive Pulmonary Disease
ECG - Electrocardiogram
ED - Emergency Department
EM - Emergency Medicine
GORD - Gastro-Oesophageal Reflux
Hs Tnt - High Sensitivity Troponin T
PE - Pulmonary Embolism
SVT - Supraventricular Tachycardia
1. Background
Acute chest pain can herald serious cardiovascular events such as acute coronary syndrome (ACS). However, the differential diagnosis of acute chest pain is broad and the consequences of a misdiagnosis can be detrimental. Furthermore, the patient load experienced in the emergency department (ED) on a daily basis combined with the 4 hour breech time frame in the NHS adds to this pressure. In such situations, it is quiet important to safely rule in or rule out acute coronary syndrome within this time frame, which ultimately would help to reduce the number of admissions to acute medical beds. A lot of admissions depend on the clinical discretion of the emergency medicine physician who see the patient on presentation to ED [1-4].
The purpose of this article was to observe the proportion of patients whose final diagnosis was ACS after being
admitted from the Emergency department for a suspected ACS diagnosis. As the current guidelines state the use of high sensitivity troponins to be done at 0 and 3 hours, the majority of the patients are being admitted for a 2nd troponin, as this cannot be managed within the 4 hour time limit of the Emergency department.
However, if this interval between serial troponins can be reduced to 2 hours, a majority of the admissions can be avoided by safely ruling out the possibility of ACS in low risk patients.
2. Methods
2.1 Study Design
This was a retrospective observational study done in the Emergency Department of University Hospitals Birmingham NHS Foundation Trust in the months of February - March 2016.
2.2 Participants
All adult patients admitted from ED under the medical team with a suspected diagnosis of acute coronary syndrome were included in this study , irrespective of the presenting symptoms. First 300 patients admitted within the months of February and March were included in the study.
2.3 Procedures
The initial standard clinical workup of these patients included a 12-lead electrocardiogram (ECG) and blood tests including high sensitivity troponin levels and a chest radiograph.
2.4 Outcome Measures
The pre-defined outcome measures for the study were to record the proportion of patients that had a 2nd troponin done and had a final diagnosis of ACS on discharge after admission for a suspected ACS diagnosis. The second important factor was to observe what proportion of the admitted patients had a non-life threatening chest pain as discharge on diagnosis.
This outcome measure was chosen on the basis of the hypothesis that if the patients with a low risk for ACS, have the serial troponins done at interval of 2 hours instead of 3 , they can be discharged from ED by safely ruling out ACS.
3. Results
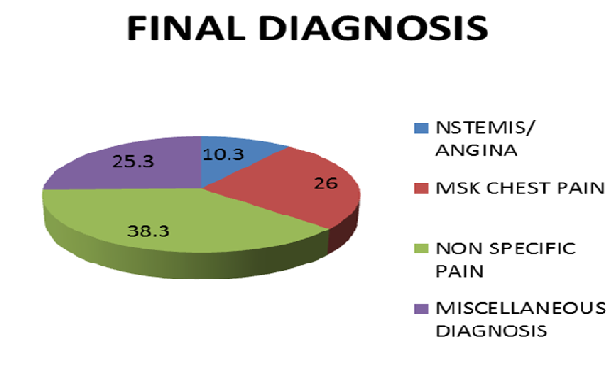
We included 300 patients admitted with the diagnosis of suspected ACS under the medical team. This included 156 males and 144 females. The mean age of this patient population was 62 years. Final results showed that 241(81%) patients had a serial troponin done during the admission. Rest of the 59(19%) patients had a single troponin done because there was an alternative final diagnosis to ACS. Only 10.3% patients had a rise in the serial troponin and a diagnosis of ACS on discharge (Figure 1). 26 % were diagnosed with musculoskeletal chest pain, 25.3 were included in the category of miscellaneous diagnosis which included GORD,
PE , SVT, pericarditis, gastritis, AF, pneumothorax and COPD. In 38.3% of the patients there was no specific cause detected for the chest pain and were labelled ‘’Non-specific chest pain’’ as a diagnosis on discharge (Figure 2). The other important factor determined in this study was that the average length of stay in hospital was 33 hours.
4. Discussion
The main findings of the study can be summarized as follows. 1) amongst the patients admitted for suspected ACS, only 10.3% had a final diagnosis of ACS while the majority patients were discharged home or had an alternative diagnosis. 2) average duration of stay in hospital was 33 hours 3) majority of the patients admitted under the medical team, were admitted for a 2nd troponin 4) more than 60% of patients had non-life threatening chest pain as diagnosis on discharge which did not warrant any further investigations.
The purpose of this study was to observe the impact of the large number of admissions for suspected ACS diagnosis, which could be potentially avoided if the interval between serial troponins could be reduced to 2 hours. With the increasing numbers of patients presenting to the emergency department and the need for acute medical beds in hospitals, the idea to be able to safely discharge low risk patients from ED would have a great impact in reducing admissions and in turn saving money.
As highlighted in the results section of this article, more than 60% patients were discharged after 2 serial Hs- TnT were negative and were diagnosed with non-life threatening chest pain ie musculoskeletal and non-specific chest pain respectively.
It is also worth considering here that combining an effective risk stratification score such as TIMI or GRACE score along with two serial high sensitivity troponins done 2 hours apart in ED would help emergency physicians safely discharge these patients.
5. Conclusion
We have 5-10 patients every day presenting to the emergency department with chest pain. About 50% of them get admitted with the diagnosis of ACS. 86% of our patients could have been potentially discharged home by using high sensitivity troponin at 0 and 2 hours and hence could have avoided 86% admissions. This in turn could have saved quite some money. With the growing pressure in the emergency departments due to ever increasing number of patients all these high sensitivity tests could potentially make some difference.
References
- Bradley, Steven M and Catherine M Otto. Heartbeat: Ruleout of acute myocardial infarction - risky business. Heart 102 (2016): 1249-1250.
- Body R, Collinson P, Goodacre S, Mills NL, Timmis A. High sensitivity cardiac troponin at 3 hours: is the cat among the pigeons? Heart 2016-309461.
- NICE Diagnostics Guidance DG15. Myocardial infarction (acute): early ruleout using high sensitivity troponin tests
- Pickering JW, Greenslade JH, Cullen L, Flaws D, Parsonage W, et al. Validation of presentation and 3 h high-sensitivity troponin to rule-in and rule-out acute myocardial infarction. Heart 102 (2016): 1270-1278.
Related PubMed Articles
- Diagnostic Utility of High Sensitivity Troponins for Echocardiographic Markers of Structural Heart Disease.
- Clinical features and prognosis of patients with acute non-specific chest pain in emergency and cardiology departments after the introduction of high-sensitivity troponins: a prospective cohort study.


 Impact Factor: * 5.6
Impact Factor: * 5.6 Acceptance Rate: 74.36%
Acceptance Rate: 74.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 