Severe Acute Hypertension and End-Organ Damage. Do We React Fast Enough?
Guillem Caldentey*#, Teresa Giralt#, Marc Llagostera, Núria Ribas, Lluis Recasens, Xavier Quiroga, Beatriz Vaquerizo
Hospital del Mar, Cardiology Department, Passeig Marítim de la Barceloneta, 25, 29, 08003 Barcelona Barcelona, Spain
*Corresponding author: Guillem Caldentey, Hospital del Mar, Cardiology Department, Passeig Marítim de la Barceloneta, 25, 29, 08003 Barcelona, Barcelona, Spain
# - Authors equally contributed to the paper
Received: 11 October 2019; Accepted: 23 October 2019; Published: 28 October 2019
Article Information
Citation: Guillem Caldentey, Teresa Giralt, Marc Llagostera, Núria Ribas, Lluis Recasens, Quiroga Xavier, Beatriz Vaquerizo. Severe Acute Hypertension and End-Organ Damage. Do We React Fast Enough?. Cardiology and Cardiovascular Medicine 3 (2019): 399-402.
View / Download Pdf Share at FacebookKeywords
<p>Hypertension; Dyspnea; Cardiomegaly</p>
Article Details
Case
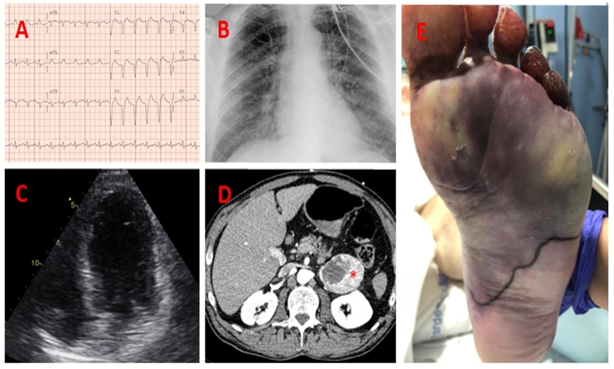
A 55-year-old male with history of tobacco and ethanol consumption consulted to the emergency room complaining of chest pain and dyspnea. Symptoms had begun suddenly at rest, two hours before consultation. At his arrival, blood pressure was 180/120 mmHg, heart rate 120 bpm and arterial oxygen saturation was 95%. The ECG showed sinus rhythm with LBBB (not previously known) (Figure 1A). The chest X radiograph evidenced mild signs of lung congestion and no cardiomegaly (Figure 1B).
With the suspicion of acute coronary syndrome, treatment with ASA (250 mg), ticagrelor (180 mg) and non-fractionated heparin (5000 IU) was administered. An emergent coronarography showed no significant lesions. The echocardiogram showed a hypertrophic and non-dilated left ventricle with severe systolic dysfunction (EF 15%) (Figure 1C). Blood test revealed metabolic acidosis, hyperlactatemia, renal failure (creatinine 2.8 mg/dl) and troponin elevation (TnT-us 3454 ng/l; N < 14).
Blood pressure management required high dose of IV sodium nitroprusside, although with inadequate control. The patient referred mild persistent thoracic oppression and started complaining of a left inferior extremity pain that presented signs of hypoperfusion. Respiratory condition worsened, requiring sedation and orotracheal intubation. As blood pressure remained elevated, despite of maximum nitroprusside doses, IV clevidipine was initiated at increasing doses (2 mg/h, doubling dose every 90 seconds, till 8 mg/h) with good response.
A toracho-abdominal CT scan ruled out aortic alterations. Signs of pulmonary edema were evidenced and the abdominal images showed a heterogeneous left suprarenal mass (Figure 1D).
With the suspicion of pheochromocytoma, IV fluids and alpha blockers (doxazosine at increasing doses) were initiated. Once alpha blockage was completed (doxazosine 16 mg od), treatment with b-blockers (carvedilol 6.25 mg/12h, till 25 mg/12h) was administered. Clevidipine infusion was stopped after 72 hours.
Renal function and signs of congestion normalized, although limb ischemia did not recover, presenting signs of distal necrosis and cellulitis that required IV antibiotic. The ECG showed normalization of the QRS duration with no repolarization abnormalities and a control echocardiogram evidenced normal left ventricular function.
After extubation the patient complained of visual alterations (hemianopsia), therefore a cerebral CT scan was performed that showed an occipital hypodensity compatible with cerebral subacute ischemia.
After medical stabilization, laparoscopic resection of the adrenal mass was performed, also with intraoperative use of Clevidipine, with no complications. The anatomical pathology analysis confirmed the presence of a 61 x 51 x 42 mm pheochromocytoma with central necrotic and hemorrhagic focus, with no evidence of malignancy. After 7 days, an infracondylar left amputation was performed due to distal left limb necrosis (Figure 1E).
The patient was discharged home after 6 weeks of hospitalization. At one month follow up, blood pressure levels were normal with no need of antihypertensive drugs, the EKG showed no abnormalities and left ventricular function was normal.
Conclusions
Even though pheochromocytoma is usually a benign tumor (90% of cases), adrenergic crisis can lead to irreversible damage. In our patient, despite the normalization of cardiac and renal alterations, hemianopsia persisted and limb amputation could not be avoided.
Clevidipine is a short-acting dihydropyrine calcium channel antagonist, with an initial half-life of approximately 1 minute, and duration of effect of 15 minutes. It does not accumulate in the body, and is rapidly metabolized by esterases in the blood and extravascular tissues. Its clearance is independent of body weight. It is administered via continuous perfusion in the form of a lipid emulsion (2-32 mg/h, max. 500 mg per day) and a peripheral venous catheter can be used. Due to its rapid-acting metabolism, clevidipine has been used in pheochromocytoma surgery with good results [1–5].
References
- Brathwaite L & Reif M. Hypertensive Emergencies: A Review of Common Presentations and Treatment Options. Cardiology Clinics 37 (2019): 275-286.
- Grasso M, Boscaro M, Scaroni C & Ceccato F. Secondary Arterial Hypertension: From Routine Clinical Practice to Evidence in Patients with Adrenal Tumor. High Blood Pressure and Cardiovascular Prevention 25 (2018): 345-354.
- Zhang R, Gupta D & Albert SG. Pheochromocytoma as a reversible cause of cardiomyopathy: Analysis and review of the literature. Int J Cardiol 249 (2017): 319-323.
- Ferreira VM, et al. Pheochromocytoma is characterized by catecholamine-mediated myocarditis, focal and diffuse myocardial fibrosis, and myocardial dysfunction. J Am Coll Cardiol 24 (2016): 2364-2374.
- Luis-García C, Arbonés-Aran E, Teixell-Aleu C, Lorente-Poch L & Trillo-Urrutia L. Clevidipine for hypertension treatment in pheochromocytoma surgery. Rev. Española Anestesiol. y Reanim. (English Ed. (2018).


 Impact Factor: * 5.6
Impact Factor: * 5.6 Acceptance Rate: 74.36%
Acceptance Rate: 74.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 