Home-Health-Aides Role in Preventing Pressure Ulcers of the Older Adults: a Scoping Literature Review
Munira Sultana1*, Nazia Ehsan2, Laila Zaman3, Jennifer Pinto4, A. K. M. Shahidur Rahman5, Mohammad Kamrul Ahsan6
1Postdoctoral Fellow, Parkwood Institute and Department of Medicine, Western University, London, Ontario Canada
2Graduate Student, University of Western Ontario, London, Ontario Canada
3Research Assistant, Parkwood Institute, London, Ontario Canada
4Graduate student, University of Toronto, Toronto, Ontario Canada
5Medical Officer, Department of Nephrology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
6Resident Medical Officer, Holy Family Red Crescent Medical College Hospital (HFRCMCH), Dhaka, Bangladesh
*Corresponding author:Dr.Munira Sultana, PhD, MPH, MBBS, Postdoctoral Fellow, Parkwood Institute and Department of Medicine, Western University, London, Ontario, Canada
Received: 08 January 2022; Accepted: 19 January 2022; Published: 26 January 2022
Article Information
Citation: Sultana M, Ehsan N, Zaman L, Pinto J, Rahman AKMS, Ahsan MK. Home-Health-Aides Role in Preventing Pressure Ulcers of the Older Adults: A Scoping Literature Review. Archives of Clinical and Biomedical Research 6 (2022): 74-84.
View / Download Pdf Share at FacebookAbstract
The purpose of this scoping review was to explore the role of home-health-aides in pressure ulcer prevention for the older adults. Controlled vocabulary with a broad range of thesaurus was used to search databases (N=11) to retrieve sources (N=349). We included those sources (n=11) fulfilling all inclusion and exclusion criteria. All sources were charted and analyzed. The sources suggested that home-health-aides play four distinct roles: observing a client’s health condition (s); coaching clients and their informal caregivers; assisting healthcare providers such as physicians, nurses, physical therapists, occupational therapists, and dietitians; and reporting to the healthcare providers, clients and informal caregivers. We report four common themes in this review: Home-health-aides’ training; interdisciplinary care approach; their relationship with older adults; and their own beliefs on their care giving role. We conclude that the home-health-aides play a key role in pressure ulcer prevention and their roles need to be recognized.
Keywords
<p>Home-health-aides; Older adults; Pressure ulcer</p>
Article Details
1. Introduction
A pressure ulcer is a “localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear” [1]. Common risk factors for pressure ulcer include- limited mobility or activity, perfusion (including diabetes), urinary and fecal incontinence, prior skin/pressure injury, dry skin, increasing age, reduced sensory perception, altered mental status, poor nutrition, black race and male gender [2, 3]. The prevalence rates of pressure ulcer across Europe, United States of America (USA), and Canada may range from 8.8% to 53.2% [4]. Since the risk of pressure ulcer in the older adults is higher [5], pressure ulcer prevention is important. Home-health-aide refers to an individual who provides personal care and housekeeping tasks to the older adults, ill or disabled persons living at home [6]. The term, “home-health-aide”, also refers to “home support workers”, “personal support workers”, “community health workers”, “community health care aides”, “home helpers”, “homemakers” [7] and “unregulated health workers” in Canada [8]. They are distinctly different from informal caregivers, carers or attendants (Table 1).
|
Characteristics |
Home Health Aides |
Carers or Attendants |
Informal Caregivers |
|
Role description |
Home Health Aides (HHA) provide assistive health services and personal care and are not licensed or regulated by a professional or a regulatory body [9]. |
Carers or attendants are usually privately hired non-professionals who are paid either by the patient or private insurance or social service programs [10, 11]. They can be patients’ family members (not spouses) or friends or neighbors [10, 11]. Their title in the America and Canada is attendants [12, 13] and in Europe is carers [10, 11]. |
Informal caregivers are usually spouses, family members, friends or volunteers who are unpaid [12-14]. |
|
Labour force |
Formal labour force [12] |
Formal labour force [12] |
Not a formal labour force [12-14] |
|
Education and training |
A formal education and training certificate are usually required to work as an HHA [12]. The Canadian HHA education ranges from [19] weeks (531 contact hours) in Alberta to over 34 weeks (795 contact hours) in the Yukon [14]. |
No formal education and training certificate are required to work as a carer or attendant [15,16]. However, they require cardiopulmonary resuscitation, first aid certification and a criminal history record check [15, 16]. |
No formal education and training are required [12-14]. |
|
Employment |
Predominantly employed by home health agencies [9, 12]. |
Predominantly employed by patients [15] |
Not employed [12-14] |
|
Supervision |
Usually supervised by a registered nurse (RN) or registered practical nurse (RPN) or licensed practical nurse (LPN) [12, 13]. |
Usually supervised by patient or patient’s family members or friends [15,16] |
Unsupervised [10,12-14] |
|
Accountability |
Accountable to the employing agency [12, 13]. There is a national registry of HHA in America [17] and most European countries [10,11,18]. British Columbia, Nova Scotia, Alberta, and Ontario have Canadian registries [14]. |
Accountable to the patient [15,16] |
No formal accountability [10,12-14] |
Table 1:Comparative description of roles and characteristics of Home Health Aides, Carers/Attendants and Informal Caregivers.
Since home-health-aides arein frequent and direct contact with their clients, and since they are institutionally trained and represent the largest home care workforce, it is of value to examine their potential role in pressure ulcer prevention.
2. Method
Scoping review method is used to capture a wider range of available sources (both qualitative and quantitative studies) [19]. Scoping review is defined as an “exploratory project that systematically map the literature available on a topic, identifying key concepts, theories, sources of evidence and gaps in the research” [20]. This method is useful when a full systematic review is not feasible for reasons such as lack of randomized control trials and few published peer-reviewed journal articles [21]. This review adhered to Levac and colleagues’ [19] scoping review framework to ensure methodological rigor.
2.1.Stage 1: Identifying the research question
We identified the target population, intervention, outcome of interest and time limit to articulate the scope of enquiry after several discussions and consultations among ourselves and the stakeholders. Stakeholders were identified as individuals delivering and planning home care to the older adults suffering from pressure ulcer, providing institutional training to the home-health-aides, and researching pressure ulcer care for the older adult home care clients in Canada (Table 2). The research question for this review was, “What is the role of home-health-aides in preventing pressure ulcer of the older adults?”
|
Role of the stakeholders |
Number of stakeholders |
|
Academics (Western University, McMaster University) |
5 |
|
Home Health work force trainer (Conestoga College, Fanshawe College) |
2 |
|
Home health policymaker (Southwest Local Health Integration Network) |
2 |
|
Wound care specialists (Saint Elizabeth Research Centre, Parkwood Institute) |
3 |
|
Community nurses (Victorian Order of Nurses, Saint Elizabeth Home Health Care) |
2 |
Table 2:Stakeholders for this scoping review.
2.2. Stage 2: Identifying relevant studies
Our search strategy included electronic search of both peer reviewed and non-peer reviewed databases and manual search. Our inclusion criteria were 1) home-health-aides caring for 2) older adults aged ≥65 years 3) diagnosed with pressure ulcer 4) living at home and 5) prevention of pressure ulcer. The age limit was set to ≥65 years following the World Health Organization’s definition of the aged population [22] to capture the target population world-wide. We did not limit our search for a specific time period. However, a limiting criterion, ‘English language’ in the title and abstract was applied to avoid errors in translation of important technical information.
2.3. Stage 3: Study selection
Two reviewers independently reviewed the sources using a set of inclusion and exclusion criteria. A third reviewer was available to consult in case of disagreement between the two reviewers. The reviewers met at the beginning, mid-point and final stage of the full-text review process and discussed discrepancies of their judgment.
2.4. Stage 4: Charting the data
The reviewers randomly selected two sources and independently extracted data from them to determine consistency of their approaches and to ensure maximum data extraction.
2.5. Stage 5: Collating, summarizing, and reporting the results
Data from the selected sources were summarized in four steps: General description of the sources, home-health-aide’s roles in pressure ulcer prevention, any identified gaps in fulfilling that role, and relevant recommendations. We used Giosa and colleagues [23] framework to report home-health-aides’ roles in pressure ulcer prevention. A summative content analysis [24] was conducted to analyze the original texts and to understand what influenced their roles. This analysis elicited contextual meaning allowing themes to emerge [24]. We used NVivo© software [25] to help us organize the data.
2.6. Stage 6: Consultation
Summary of the data from the selected sources were shared with the stakeholders to help clarify the potential roles of home-health-aides in the emerged themes. They provided insights beyond the literature and helped us to cluster the codes with deeper understanding of their similarities.
3. Results
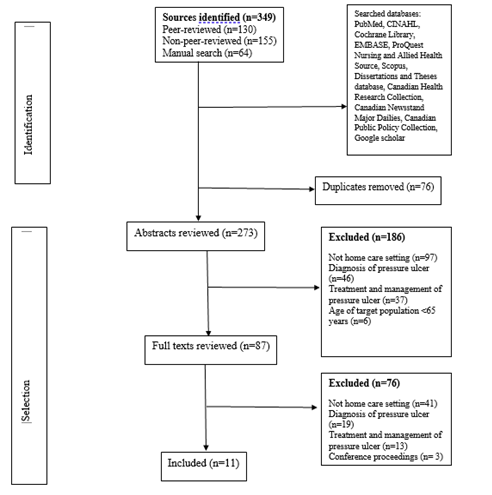
A total 349 sources were identified (Figure 1), and 11sources (Table 3) satisfied all inclusion and exclusion criteria. The identified roles of home-health-aides in pressure ulcer prevention are reporting, assisting, observing, and coaching (Table 4).
|
Sources |
Country of origin |
Study design |
Population |
Intervention and control |
Outcome |
|
Ruotsalainen, Jantunen, Sinervo [26] |
Finland |
Mixed method study |
Home-health-aides (HHA) caring for older adults |
None |
Challenges, stressors, teamwork and management factors that are associated with HHA well-being, job satisfaction and experienced care quality related to pressure ulcer prevention |
|
Martinez-Linares et al. [27] |
Spain |
Qualitative (Exploratory-descriptive) |
HHA caring for older adults |
None |
Unmet health needs of people with dependencyrelated to pressure ulcer prevention |
|
Sorrentino et al. [28] |
Canada |
Course instruction |
HHA caring for older adults |
None |
Pressure ulcer diagnosis, prevention, and treatment |
|
Tasi et al. [29] |
Taiwan |
Retrospective cross-sectional observation study |
Dyads of HHA and their older adult clients |
None |
Factors influencing development and preventionof pressure ulcer |
|
Chayamiti&Caliri [30] |
Brazil |
Survey |
HHA caring for older adults |
None |
Factors influencing pressure ulcer prevention |
|
Jaul [31] |
Israel |
Case report (patient-centered-care theory) |
Older adult at risk of pressure ulcer and HHA |
None |
Role of HHA in pressure ulcer prevention |
|
Goldsworthy [32] |
United States of America (USA) |
Qualitative (Reasoned-action theory) |
HHA caring for older adults |
None |
Role of HHA in pressure ulcer prevention |
|
Appleby et al. [33] |
USA |
Case study |
Older adult at risk of pressure ulcer and HHA |
None |
Pressure ulcer prevention |
|
Lewin et al. [34] |
Australia |
Survey |
Older adult at risk of pressure ulcer |
None |
Implementation of pressure ulcer and prevention guidelines |
|
Lewin et al. [35] |
Australia |
Survey |
Older adult at risk of pressure ulcer and HHA |
None |
Factors influencing development and prevention of pressure ulcer |
|
Hanson et al. [36] |
USA |
Survey |
Older adult at risk of pressure ulcer |
None |
Factors influencing development and preventionof pressure ulcer |
Table 3:General description of the included sources.
|
Source |
Observation |
Coach |
Assist |
Report |
|
Ruotsalainen, Jantunen, Sinervo [26] |
× |
× |
× |
× |
|
Martinez-Linares et al. [27] |
× |
× |
× |
× |
|
Sorrentino et al. [28] |
× |
× |
× |
× |
|
Tsai et al. [29] |
× |
× |
× |
|
|
Chayamiti&Caliri [30] |
× |
× |
||
|
Jaul [31] |
× |
× |
× |
|
|
Goldsworthy [32] |
× |
|||
|
Appleby et al. [33] |
× |
× |
||
|
Lewin et al. [34] |
× |
× |
× |
|
|
Lewin et al. [35] |
× |
× |
||
|
Hanson et al. [36] |
× |
× |
||
|
Stakeholder agreement |
Yes (n=13) |
Yes (n=2) |
Yes (n=7) |
Yes (n=13) |
Table 4:Four roles for home health aides’ involvement in pressure ulcer prevention.
Reporting: Ten out of 11 sources discussed home-health-aides’ role in reporting any change of the older adults to client him/herself, his/her informal caregivers, and his/her healthcare providers. The regular reporting to the healthcare providers is also emphasized.
Assisting:Ten out of 11 sources identified home-health-aides’ role in assisting the older adults, informal caregivers, and healthcare providers in different ways such as positioning and re-positioning; ensuring the bed is wrinkle-free; noticing no bony prominences are compressed; using cushions, pillows or pressure-relieving assistive devices; transferring the older adults with the help of lifting devices and turning sheets; avoiding shear or friction during ambulation; assisting the them to the bathroom; bathing; maintaining personal hygiene; keeping the skin dry after incontinence; and moisturizing skin to prevent pressure ulcers. Their assistive role was extended to dry dressing, negative pressure wound therapy, and ensuring oxygenation of the affected body part.
Observing:Eight sources recognized home-health-aides’ role in observing for redness of the skin, foul smell from the wound, any change in the wound-dressing color, and presence or absence of pain. Their observation could help healthcare providers to discover new wounds and to identify worsening or healing wounds.
Coaching:Three sources suggested that they could play an important role in coaching the older adults and their caregivers on changing position at least every two hours and maintaining appropriate nutrition and hydration.
Summative analysis revealed four themes described in detail in the following sections.
Theme-1:Home-health-aides training. The need for training of home-health-aides on pressure ulcer prevention, particularly in the home care context was discussed in the selected sources (n=5) that may include 1) skills and competences required to: understand the risk of pressure ulcer, 2) recognize a pressure ulcer, 3) identify the early signs of pressure ulcer development, 4) use lifting and turning devices appropriately, and 5) use pressure ulcer preventive equipment safely. The home-health-aides’ training was significantly associated with a lower risk of pressure ulcer development at home (Odds Ratio 0.366; p<0.05) [29]. Nurses were identified as a potential educator and trainer.
Theme-2: Interdisciplinary care approach. Integration of home-health-aides into the interdisciplinary team was emphasized (n=8) as they followed the team developed plan of care. They should be included during developing and re-evaluating a plan of care. A flexible plan of care matching the changing needs of the older adult was identified as a key to successful pressure ulcer prevention.
Theme-3:Relationship between home-health-aides and older adults. The older adults and their informal caregivers often positively influenced a home-health-aide’s performance (n=4). Admiring a home health aide’s empathy positively influenced their relationship with the older adults while fear, refusal, discomfort, and embarrassment negatively influenced their performance.
Theme-4:Beliefs on care giving role. A home-health aide’s own beliefs on their caregiving role can influence their performance (n=3). Almost 90% of the older adults without pressure ulcers were cared for by home-health-aides who believed that they were responsible to report any change of their client’s condition to the nurse [26,27,29].
4. Discussion
This scoping review revealed how home-health-aides could play an important role in preventing pressure ulcer in older adults. Our notion is equally shared in the Safe Seniors’ Care Strategy [37] where increased funding on the education and training of the home-health-aides were emphasized. We must also mention that restructuring and cutbacks in the health care system resulted in understaffing in home care, which altered home care human resources by shifting the workload of care from healthcare providers to informal caregivers [37]. As a result, almost 30% of older adults are being cared for by their informal caregivers [38]. Therefore, both the informal caregivers and the older adults are at a risk, as shifting the burden of care to the informal caregivers had ignored the skills necessary for home care work [37]. Home-health-aides act as the eye, ear, nose, voice and hand of the health care providers in a home care setting [39]. Therefore, their training, their integration in the interdisciplinary care team, their relationship with the patients and their informal caregivers, and their beliefs could make best utilization of existing resources in a home care setting. Several Canadian best practice guidelines on pressure ulcer prevention [39-48] identified interventions such as re-positioning; avoiding pressure, friction and shear on all surfaces; keeping the skin clean and dry after episodes of incontinence; and using a skin moisturizer to keep the dry skin hydrated to prevent pressure ulcer that aligned with home-health-aides’ role discussed in this review. However, home-health-aides are not allowed to participate in the development and revision of the patient plan of care in Canada [49] indicating a discrepancy in the policy and practice. We noticed that no Canadian research study was available on the role of home-health-aides in pressure ulcer prevention for the older adults living at their own homes at the time of this review despite a number of policy and practice recommendations. Since home-health-aides are the largest home care workforce in Canada [15], we identify this finding as a potential research gap. We also noticed that none of the included sources mentioned how to integrate home-health-aides in pressure ulcer prevention interdisciplinary team. Therefore, future research in this area may aid clinical community in preventing pressure ulcer at home. Our recommendations for the health care stakeholders based on our findings to fulfill a home-health-aide’s role in pressure ulcer prevention are-1) to create a clear guideline on how to integrate home-health-aides in the interdisciplinary pressure ulcer prevention team, especially in a home care setting, 2) to provide regular ongoing education and training of the home-health-aides on pressure ulcer prevention, and 3) to ensure that the home-health-aides were following the pressure ulcer prevention guidelines.
5. Conclusion
Our scoping review reveals four distinct roles of the home-health-aides in pressure ulcer prevention of the older adults. The emerged themes also provided a contextual interpretation of their roles, identified areas needing attention for maximum benefit in pressure ulcer prevention at home. We recognize that the pressure ulcer prevention is one of the quality indicators in the geriatric health care. Therefore, the role home-health-aides in pressure ulcer prevention needs to be better recognized as they are in direct daily contact with the older adults being cared for at their own homes. A better utilization of home-health-aides in the interdisciplinary team may also improve health outcomes of the older adults, ultimately, optimizing our scarce healthcare resources.
Declaration of conflicts of interest
Authors have no conflicts of interest to declare.
References
- European Pressure Ulcer Advisory Panel & National Pressure Ulcer Advisory Panel. Prevention and Treatment of Pressure Ulcers: Quick Reference Guide. (Report). Washington DC: National Pressure Ulcer Advisory Panel; (2009).
- Coleman S, Gorecki C, Nelson EA, et al. Patient risk factors for pressure ulcer development: systematic review. International journal of nursing studies 50 (2013): 974-1003.
- Baumgarten M, Margolis DJ, Localio AR, et al. Pressure ulcers among elderly patients early in the hospital stay. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences 61 (2006): 749-754.
- Haesler E. National pressure ulcer advisory panel, European pressure ulcer advisory panel and pan pacific pressure injury alliance. Prevention and treatment of pressure ulcers: quick reference guide (2014): 14-32.
- National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel, and Pan Pacific Pressure Injury Alliance. Prevention and Treatment of Pressure Ulcers: Quick Reference Guide. Osborne Park, Western Australia: National Pressure Ulcer Advisory Panel, European Pressure Ulcer Advisory Panel, and Pan Pacific Pressure Injury Alliance 2019.
- National Library of Medicine. Fact Sheet: Medical Subject Headings (MeSH) 2021.
- Sims-Gould J, Byrne K, Craven C, et al. Why I became a home support worker: recruitment in the home health sector. Home health care services quarterly 29 (2010): 171-194.
- Canadian Nurses Association. Unregulated health workers: A Canadian and global perspective. Canadian Nurses Association, Ottawa, ON, Canada (2005).
- Sinclair S, Torres MB, Raffin-Bouchal S, et al. Compassion training in healthcare: what are patients’ perspectives on training healthcare providers? BMC Medical Education 16 (2016): 1-10.
- Kringos DS, Boerma WG, Hutchinson A, et al. Building primary care in a changing Europe: case studies. World Health Organization. Regional Office for Europe (2015).
- Riedel M, Kraus M. Informal care provision in Europe: regulation and profile of providers. ENEPRI Research Report No 96 (2011).
- Health Professions Regulatory Advisory Council. The regulation of personal support workers (2006).
- Emanuel RH, Emanuel GA, Reitschuler EB, et al. Challenges faced by informal caregivers of hospice patients in Uganda. Journal of Palliative Medicine 11(2008): 746-753.
- Estabrooks CA, Squires JE, Carleton HL, et al. Who is looking after Mom and Dad? Unregulated workers in Canadian long-term care homes. Canadian Journal on Aging/La Revue canadienne du vieillissement 34 (2015): 47-59.
- Centre for Independent Living in Toronto. Annual Report 2019-2020.
- Canada Revenue Agency. Attendant care and care in a facility (2021).
- Keefe JM, Knight L, Martin-Matthews A, et al. Key issues in human resource planning for home support workers in Canada. Work 40 (2011): 21-28.
- Organization for Economic Co-operation and Development & European Commission. Long-term care workforce: caring for the ageing population with dignity (2021).
- Levac D, Colquhoun H, O'Brien K. Scoping studies: advancing the methodology implementation science 5 (2010): 69.
- Grimshaw J. A guide to knowledge synthesis: a knowledge synthesis chapter. Ottawa: Canadian Institutes of Health Research 8 (2010): 1-56.
- Arksey H, O'Malley L. Scoping studies: towards a methodological framework. International journal of social research methodology 8 (2005): 19-32.
- World Health Organization. World report on ageing and health. World Health Organization (2015).
- Giosa J, Holyoke P, Bender D, et al. Observe, coach, assist, and report: An emerging framework for integrating unregulated healthcare providers into interdisciplinary healthcare teams. Journal of Research in Interprofessional Practice and Education 5 (2015): 1-20.
- Hsieh HF, Shannon SE. Three approaches to qualitative content analysis. Qualitative health research 15 (2005): 1277-1288.
- QSR International Incorporation. NVivo 12 Plus for Windows (2019).
- Ruotsalainen S, Jantunen S, Sinervo T. Which factors are related to Finnish home care workers’ job satisfaction, stress, psychological distress and perceived quality of care?-a mixed method study. BMC Health Services Research 20 (2020): 1-3.
- Martínez-Linares JM, Andújar-Afán FA, Martínez-Yébenes R, et al. A Qualitative View of Homecare Support Workers on Unmet Health Needs of People with Dependency. International journal of environmental research and public health 17 (2020): 3166.
- Sorrentino SA, Remmert L, Wilk MJ. Mosby's Canadian Textbook for the Support Worker-E-Book. Mosby Canada (2016).
- Tsai YC, Lin SY, Liu Y, et al. Factors related to the development of pressure ulcers among new recipients of home care services in Taiwan: A questionnaire study. International journal of nursing studies 49(2012):1383-1390.
- Chayamiti EM, Caliri MH. Pressure ulcer in patients under home care. ActaPaulista de Enfermagem23 (2010):29-34.
- Jaul, Efraim. Assessment and Management of Pressure Ulcers in the Elderly. Drugs & Aging 27 (2010): 311-325.
- Goldsworthy RC. Pressure Ulcer PREVENTIVE CARE. Home Healthcare Now26(2008):113-120.
- Appleby SL, Eberhard MH, Spears MA. A Home Care Wound Care Challenge: Its Rewards, Inspiration, and Positive Outcomes. Home Healthcare Now25(2007):362-368.
- Lewin G, Carville K, Newall N, et al. Skin safe: implementing clinical guidelines to prevent pressure ulcers in home care clients. Primary Intention: The Australian Journal of Wound Management 15 (2007).
- Lewin G, Carville K, Newall N, et al. Determining the effectiveness of implementing the AWMA'Guidelines for the prediction and prevention of pressure ulcers' in silver chain, a large home care agency stage 1: baseline measurement. Primary Intention: The Australian Journal of Wound Management 11 (2003).
- Hanson DS, Langemo D, Olson B, et al. Decreasing the prevalence of pressure ulcers using agency standards. Home healthcare nurse 14 (1996): 525-531.
- Armstrong P, Armstrong H, Choiniere J. Before It's Too Late: A National Plan for Safe Seniors' Care (report). Ottawa, ON: Canadian Federation of Nurses Unions (2015).
- Turner A, Findlay L. Informal care giving for seniors. Health Rep 23 (2012): 33-36.
- Registered Nurses’ Association of Ontario. Clinical Best Practice Guidelines: Assessment and management of pressure injuries for the interprofessional team (3rd ed). Toronto, ON: Registered Nurses' Association of Ontario (2016).
- British Columbia Provincial Nursing Skin and Wound Committee. Guideline: Assessment and Treatment of Pressure Ulcers in Adults & Children. Vancouver, BC (2014).
- Community Care Access Centre. Delivering Quality Care in the Home and Community (2013).
- Health Quality Council & Saskatchewan Association of Health Organizations. Saskatchewan skin and wound care guidelines. Journal of Chemical Information and Modeling. Saskatoon, SK (2006).
- Houghton PE, Campbell K. Canadian best practice guidelines for the prevention and management of pressure ulcers in people with Spinal Cord Injury: a resource handbook for clinicians. Ontario Neurotrauma Foundation (2013).
- Labrador-Grenfell Health, Western Health, Eastern Health, & Central Health. Newfoundland Labrador: Skin and Wound Care Manual. Labrador City, NL (2008).
- North East Community Care Access Centre. Helping You Heal: Your Guide to Wound Care: Wound Self-management Program (2016).
- Occupational Therapists in Vancouver Coastal Health and Providence Health Care. Occupational Therapy Skin Care Guideline: Best Practice for the Prevention and Treatment of Pressure Ulcers. Vancouver, BC: Vancouver Coastal Health and Providence Health Care (2008).
- Registered Nurses’ Association of Ontario. Nursing Best Practice Guideline: Shaping the Future of Nursing. Toronto, ON: Registered Nurses’ Association of Ontario (2007).
- Registered Nurses’ Association of Ontario. Nursing Best Practice Guideline: Shaping the Future of Nursing: Risk Assessment &Prevention of Pressure Ulcers. ON, CA: Registered Nurses’ Association of Ontario (2011).
- Regulated Health Professions Act of 1991, S.O. c.18, ss. 2, 3 ( 2015).


 Impact Factor: * 5.8
Impact Factor: * 5.8 Acceptance Rate: 71.20%
Acceptance Rate: 71.20%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 