The Effect of Early Mobilisation on the Sagittal Alignment and Clinical Outcome Following Conservative Treatment of the AO A3 and A4 Thoracolumbar Spine Fracture in Comparison to A1 Fractures. A Retrospective Study
Mahmoud Elshamly1,2,4, Stefan Toegel2,3, Josef Georg Grohs1*
1Department of Orthopedics and Trauma Surgery, Medical University of Vienna, Waehringer Guertel 18-20, A-1090 Vienna, Austria
2Karl Chiari Lab for Orthopaedic Biology, Department of Orthopedics and Trauma Surgery, Medical University of Vienna, Waehringer Guertel 18-20, A-1090 Vienna, Austria
3Ludwig Boltzmann Cluster for Arthritis and Rehabilitation, Vienna, Austria
4Landesklinikum Amstetten, Department of Traumatology, Krankenhausstrasse 21, 3300 Amstetten, Austria
*Corresponding author: Josef Georg Grohs, Department of Orthopedics and Trauma Surgery, Medical University of Vienna, Waehringer Guertel 18-20, A-1090 Vienna, Austria.
Received: 01 August 2022; Accepted: 22 August 2022; Published: 19 September 2022
Article Information
Citation: Mahmoud Elshamly, Stefan Toegel, Josef Georg Grohs. The Effect of Early Mobilisation on the Sagittal Alignment and Clinical Outcome Following Conservative Treatment of the AO A3 and A4 Thoracolumbar Spine Fracture in Comparison to A1 Fractures. A Retrospective Study. Archives of Clinical and Biomedical Research 6 (2022): 749-755.
View / Download Pdf Share at FacebookAbstract
Background: The aim of the study was to correlate the clinical and radiological outcomes following the conservative treatment of neurologically intact patients with AO A4, A3, and A1 thoracolumbar (TL) fractures.
Methods: Retrospective study included 3 cohorts of conservatively treated patients with AO A4, A3, and A1 TL fracture without the use of bracing or casting. At the final follow up Segmental Kyphotic Angle (SKA), Regional Lordotic Angle (RLA), Lordosis Gap (LG), Pelvic Incidence (PI), Pelvic Tilt (PT), Sacral Slope (SS), Sagittal Vertical Axis (SVA), Lumbar Lordosis (LL), Thoracic Kyphosis (TK), and Femoral Obliquity Angle (FOA), and the Oswestry Disability Index (ODI) were assessed. Data were analyzed using descriptive statistics, non-parametric inferential statistics, and Spearman correlation analyses.
Results: Age was significantly higher in A4 group than in A1 group (p=0.04). The median 1ry SKA of the A3 group (15 ± 3) was significantly higher than in A1 group (7 ± 7, p=0.04). The median of total ODI in the A4 group (42 ± 53) and A3 group (31.3 ± 27) was clinically higher than in A1 group (11.1 ± 25), however, this difference was not statistically significant. Age as well as SVA correlated significantly with PT, FOA, and SKA at the follow up, and the total ODI.
Conclusions: Age of the patient is a significant confounder that has an important impact on the type of fracture, sagittal malalignment, its compensatory mechanisms, and the resulting clinical outcome following conservative treatment of AO A4 and A3 TL fracture.
Keywords
Burst Fracture; Early mobilization; Physiotherapy; Vertebral Compression Fracture
Burst Fracture articles; Early mobilization articles; Physiotherapy articles; Vertebral Compression Fracture articles
Article Details
Abbreviations:
FOA- Femoral Obliquity Angle; IQ- Interquartile Range; LG- Lordosis Gap; LL- Lumbar Lordosis; ODI- Oswestry Disability Index; PI- Pelvic Incidence; PT- Pelvic Tilt; RLA- Regional Lordotic Angle; SS- Sacral Slope; SVA- Sagittal Vertical Axis; SKA- Segmental Kyphotic Angle; STIR- Short Tau Inversion Recovery; TK- Thoracic Kyphosis; TLSO- Thoracolumbar Orthosis
1. Introduction
Burst thoracolumbar spine fractures account for approximately 45 % of all major thoracolumbar trauma, and this devastating injury often results in an abrupt change in the quality of life of the patient. Apart from the conspicuous loss of function, those patients usually develop over time a post-traumatic deformity. Despite the high incidence of thoracolumbar burst fractures, the neurological status in at least 50% of patients remains intact [1–3]. Various studies discussed different techniques of the operative management of thoracolumbar burst fracture that included posterior short segment fusion, anterior decompression and fusion, and many other techniques. Other studies reported the results of conservative treatments that included bed rest, body cast or bracing, rehabilitation and physiotherapy or combination of all. However, there is no consensus about the ideal treatment of thoracolumbar burst fractures without neurological deficits [1–3]. Nevertheless, the literature addressing the effect of sagittal malalignment on the clinical outcome of the conservative treatment of AO A4 and A3 TL fractures with functional treatment without the use of casting or bracing is limited. Therefore, the aim of the current study was to assess the relation of patients’ disability to the fracture type as well as the regional and the global sagittal spinal malalignment following the conservative treatment of thoracolumbar AO A3 and A4 fractures in comparison to AO A1 fractures.
2. Materials and Methods
This is a retrospective study of 3 cohorts of neurologically intact patients with AO A1, AO A3 and A4 TL spine fractures who were treated conservatively in a level 2 trauma center. A positive vote of the local ethics committee was obtained. The medical records of the hospital were reviewed to gather all patients who suffered from radiological proven thoracolumbar AO A1, A3, and A4 fractures between 01.01.2010 to 31.12.2015. The inclusion criteria for the involvement in the final analysis comprised conservative treatment of a TL fracture without bracing or casting, absence of neurological deficits, lateral and anteroposterior (a-p) radiographs and CT scans at time of injury, and age older than 18 years. Exclusion criteria included AO B or C thoracolumbar fracture, previous spinal surgeries, history of spinal disorders that required medical intervention, including spinal canal stenosis, spondylolisthesis or preexisting spinal deformity, serious mental or medical diseases demanding medical treatment, and pregnancy. All relevant clinical data of the selected patients were obtained, including age and gender of the patients, clinical findings, fracture type, parameters of sagittal balance and the follow up findings. The type of fracture was determined using AO classification of the TL spine fracture using the CT and MRT (with Short tau inversion recovery (STIR)) [4]. The patients involved in the study were subjected to conservative treatment. The decision not to treat surgically was based on assumed fracture stability, response to pain management procedures, specialist decision and patients’ preferences. Patients were hospitalized, received pain therapy and were mobilized under supervision of the physiotherapists. The neurological status of the patients was evaluated regularly, and the fracture stability was controlled radiographically during the hospital stay, at time of discharge, and during the follow up. The degree of disability was assessed using the Oswestry Disability Index (ODI) [5] at the final follow up. Long standing anteroposterior and lateral radiographies of the whole spine that had been taken at the final follow up using a standard technique, were analyzed for each patient included in the study. On the lateral radiographs, the following radiologic parameters were determined for each patient: segmental kyphotic angle (SKA), which was determined as the angle between the upper and lower endplates of the broken vertebral body, regional kyphotic angle (RKA), which was defined as the angle between the upper endplate of the vertebral body rostral to the broken vertebral body and the lower endplate of the vertebral body caudal to the broken one, Lordosis Gap (LG), Pelvic Incidence (PI), Pelvic Tilt (PT), Sacral Slope (SS), Sagittal Vertical Axis (SVA), Lumbar Lordosis (LL), Thoracic Kyphosis (TK), and Femoral Obliquity Angle (FOA) [6–10]. Statistical analyses were performed using IBM SPSS v25. Descriptive statistics, non-parametric inferential statistics, as well as Spearman correlation analyses, where r values were interpreted as follows: 0–0.2: weak correlation, > 0.2–0.4: mild correlation, > 0.4–0.6: moderate correlation, > 0.6–0.8: moderately strong correlation, and > 0.8–1: strong correlation. Kruskal–Wallis test (with pairwise comparison) was used for comparing the differences in median values of certain parameters between the 3 groups. Values are given as median with / interquartile range.
3. Results
The demographic characteristics of the patients are shown in Table 1.
|
A4 Group |
A3 Group |
A1 Group |
Kruskal-Wallis Test |
|
|
AO classification |
A4 |
A3 |
A1 |
|
|
Number F/M |
n = 5 F= 4 M=1 |
n = 12 F= 5 M= 7 |
n =17 F= 11 M= 6 |
|
|
Age (years) Median / IQ range |
70 / 24 |
57.5 / 24 |
49 / 25 |
* 0.04 |
|
BMI Median / IQ range |
25 / 3 |
24 / 7 |
28 / 5 |
0.2 |
|
Follow up Median / IQ range |
3 / 3 |
4 / 3 |
4 / 2 |
0.5 |
Table 1: Demographics and Patients’ Characteristics.
*A4 group vs A1 group.
The results of Kruskal-Wallis Test of age, BMI, and the follow up time between the 3 groups are shown in the table.
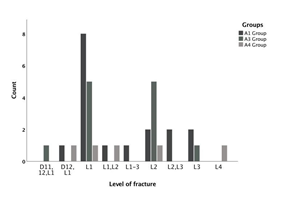
Figure 1 presents an overview of the fracture patterns in the 3 groups. No patient had a fracture of L5. Therefore, the geometric analysis of burst fractures echoed the physiological spatial interplay between the spinal and pelvic parameters as seen in normal subjects [11].
The median values of the SKA measured on the X-ray done at the first time of presentation (SKA 1ry) was significantly higher in the A3 Group (15 / 3°) in comparison to the A1 Group (7 / 7°) (p = 0.04). Contrarily, there was no significant differences between the 3 groups in the other radiological parameters as shown in Table 2.
|
A4 Median / IQ Range |
A3 Median / IQ Range |
A1 group median / IQ range |
Kruskal-Wallis Test |
|
|
SVA (mm) |
33.5 / 93 |
14 / 49 |
25 / 38 |
0.6 |
|
TK (°) |
20.5 / 33 |
30 / 17 |
34 / 19 |
0.21 |
|
LL (°) |
48.5 / 23 |
46 / 19 |
54 / 17 |
0.4 |
|
SS (°) |
42.5 / 17 |
30 / 18 |
35 / 9 |
0.2 |
|
PT (°) |
28.5 / 16 |
18 / 14 |
23 / 18 |
0.2 |
|
PI (°) |
67.5 / 29 |
53 / 11 |
56 / 24 |
0.2 |
|
LG (°) |
20 / 41 |
4 / 23 |
4 / 32 |
0.1 |
|
FOA (°) |
10.5 / 18 |
9 / 6 |
7.5 / 8 |
0.8 |
|
SKA (°) 1ry |
15.5 / 11 |
15 / 3 |
7 / 7 |
** 0.04 |
|
SKA (°) FU |
17 / 11 |
19 / 9 |
9 / 11 |
0.06 |
|
SKA (^) Delta |
-1 / 18 |
5 / 13 |
1 / 11 |
0.7 |
|
RLA (°) 1ry |
5.7 / 6.2 |
1.7 / 16.2 |
3.3 / 11 |
0.3 |
|
RLA (°) FU |
0.5 / 16.3 |
-7.3 / 15.8 |
0.5 / 28.6 |
0.7 |
|
RLA (°) Delta |
-5.5 / 11 |
-7 / 11 |
-5 / 14 |
0.9 |
|
Total ODI |
42 / 53 |
31.3 / 27 |
11.1 / 25 |
0.09 |
Table 2: Radiographic Parameters and Clinical Outcome of the 3 Groups.
** A3 group vs A1 group
The results of Kruskal-Wallis Test of different radiological parameters between the 3 groups are shown in the table.
The clinical outcome assessed using the ODI score at the final follow up revealed a clinically relevant higher median of total ODI in the A4 Group (42 / 53) and the A3 Group (31.3 / 27) in comparison to the A1 Group (11.1 / 25), however, these differences were not statistically significant (p = 0.09). Age of the patients analyzed together irrespective of the assigned study group correlated mildly with SKA at the follow up (SKA FU) (r = 0.37, p = 0.04), moderately with the SVA (r = 0.409, p = 0.01) and the total ODI (r = 0.45, p = 0.006), and moderately strong with PT (r = 0.66, p < 0.0001) and FOA (r = 0.61, p < 0.0001). The SVA correlated mildly with the change in SKA (SKA Delta) (r = 0.35, p = 0.04), moderately with PT (r = 0.51, p = 0.002), PI (r = 0.45, p = 0.007), and LG (r = 0.53, p = 0.001), and moderately strong with FOA (r = 0.66, p < 0.0001). The LL had a negative moderate correlation with the SKA FU (r=-0.47, p = 0.006), mild negative correlation with the SKA changes (SKA Delta) (r=-0.35, p = 0.04) and the follow up time (r=-0.39, p = 0.02), and mild correlation with RLA FU (r = 0.036, p = 0.004) and RLA Delta (r = 0.35, p = 0.04). The SKA FU had a moderate negative correlation with RLA FU (r=-0.49, p = 0.005). The total ODI score correlated mildly with SVA (r = 0.39, p = 0.02) and the SKA FU (r = 0.36, p = 0.04) and age.
4. Discussion
In this retrospective study we assessed the radiological and clinical outcome of the conservatively treated patients with AO A4, A3, and A1 TL fracture in relation to sagittal profile neurologically intact patients. To the authors’ knowledge, the current study is the first to investigate the sagittal balance and its effect on the clinical outcome in neurologically intact patients with AO A3 and A4 TL fracture, who were treated with early mobilization without bracing or casting. Choosing the ideal management of TL burst fracture without neurological deficits is still challenging, and several studies have compared the operative and non-operative treatment of this fracture [11–17], there is no consensus between countries regarding the management of this type of fracture [18]. Different authors reported some benefits of the operative treatment, for instance, early mobilization, early hospital discharge, correction of the local kyphosis, and faster return to work but the patients were more susceptible to different complications, an increased risk of revision of the surgery, and subsequent greater overall healthcare costs. In this context, a high level of evidence demonstrated similar functional outcomes, lower complication rates, and less costs of the conservative treatment of neurologically intact patients with TL burst fracture [19–25]. After the management of acute painful vertebral fractures using balloon kyphoplasty Wardlaw D. et al [26] reported short term improvements in clinical outcomes compared to non-surgical treatment. Regarding the conservative treatment, there is no consensus on the optimal course of conservative treatment modalities [27, 28]. Including analgesics, physiotherapy, bracing and/or casting, and mobilization. Giele B. et al [29] reported the lack of evidence of effectiveness of bracing in patients with traumatic thoracolumbar fracture in the current literature. Accordingly, Shamji MF. et al [30] reported a nonsignificant difference in the loss of the anterior vertebral body height between the group of patients with a customized thoracolumbar orthosis (TLSO) and the other group without bracing (TLSO: 12.5% ± 10.2% vs. no bracing: 11.9% ± 8.1%; p = 0.88) kyphotic progression (TLSO: 5.3 ± 4.4 degrees vs. no-brace 5.2 ± 3.6 degrees; p = 0.93), or clinical outcome differences at 6 months follow-up of neurologically intact patients with stable thoracolumbar burst fractures. Furthermore, they concluded that conservative therapy involving early mobilization without brace immobilization may be warranted. In this context, Jin Y. et al [31] reported a low-quality evidence of using Spinomed brace® in patients with sub-acute osteoporotic vertebral fractures. In our collective, all patients were treated without bracing or casting. The bed rest was minimized and early mobilization with physiotherapeutic aid was favored for all patients, as prolonged lying can lead to vascular complications, including orthostatic dysregulation, thromboembolic events, decubitus and pneumonia, all of which can lead to death [32]. In all patients in both groups, the use of analgesic drugs was tailored on an individual basis. The correction of dose and class of drugs was performed on a day-to-day basis. The mean period of hospital stay of the patients in both groups was 5 days. In previous reports, the results indicated that increasing residual deformity and alteration of the global sagittal balance can impact the clinical outcomes over the long term [33, 34]. Koller et al [34] observed a strong correlation between the increase in the local deformity and the worsening of the clinical outcome in patients treated conservatively with bracing. Mayer et al [35] reported a superior outcome with restoration of the sagittal balance in surgical treatment of thoracolumbar spine fracture. In our study, we observed a worsening of the clinical outcome with the increase of local kyphotic changes and subsequent sagittal malalignment. Moreover, the group of patients with A3 and A4 TL fracture had a worse clinical outcome than the group of patients with A1 fracture at the last follow up. Our findings coincide with the previous reports that showed an increase of RKA of 13° in patients treated conservatively after thoracolumbar burst fracture [21, 23, 36–39]. Other authors reported a mean final SKA of about 10° ± 3° after posterior-only, and 8° ± 1.8° after anterior-only treatment of burst fracture [11]. Koller et al. [11] assessed the clinical and radiological long-term results in patients with thoracolumbar burst who were treated conservatively using a cast, they reported a final RKA of 4.7° ± 10.9 on average, while the SKA was 12.8° ± 5.8. Comparably, in our collective with A4 and A3 TL fracture the mean of SKA at the last follow up was 16.5 ± 5.8 and 19.3 ± 9.6, respectively. A pathological sagittal profile is defined, therefore, by a combination of pathological values of all the spinopelvic parameters than just by a single pathological parameter. Abnormal sagittal balance is associated with many spinopelvic changes in attempt to compensate the imbalance. Reduction in the thoracic kyphosis, intervertebral hyperextension, retrolisthesis, pelvic back tilt, knee flexion and ankle extension were the main mechanisms described in the literature [32]. The correlation analysis in our study revealed a significant correlation between the age and the increase in the anterior shift of C7 plumb line with subsequent increase in pelvic retroversion following the increasing local kyphosis with subsequent worsening of the clinical outcome. This accords the previous finding presented by Vendatam et al. who demonstrated that the mean sagittal vertical axis (SVA) shifts forward in the ageing population, ensuing the loss of lumbar lordosis and the onset of symptoms in these patients [6]. In our study, we observed a significant negative correlation between the LL and the SKA as well as with follow up time. The progressive increase in the local kyphosis following the thoracolumbar fracture led to progressive loss in LL which affected the overall sagittal alignment and resulted in worse outcomes scores and greater self-reported pain and disability. This coincides with the previous results indicating worse disability amongst those with an increased degree of kyphosis in their lumbar spine in comparison to those with normal and lordotic lumbar spines [32]. The progressive kyphotic changes may lead to progressive shift of the C7 plumb line anteriorly, as an attempt to restore the sagittal balance, the PT would increase in a mechanism described by Barrey et al [32] who reported the role of pelvic retroversion as the only mechanism in the pelvic area to compensate for the sagittal imbalance by bringing back the sacral plate and increasing the sacro-femoral distance, another step in the compensation for the sagittal malalignment is through the increase in knee flexion which explains the significant correlation we have noticed between the SVA and the SKA Delta, PT, LG, and FOA. This reflected the impact of the increasing local kyphosis on the local lordotic angle, as we found a negative correlation between the increase in the SKA FU and the RLA FU.
Conclusion
Age of the patient is a significant confounder that has an important impact on the type of fracture, sagittal malalignment (increasing SVA), and the compensatory mechanisms (increasing PT) that are related to the increasing SKA. All these may be associated with worse clinical outcome following conservative treatment of AO A4 and A3 TL fracture.
Declarations
Ethics approval and Consent to Participate
For this study, a positive vote of the local ethics committee was obtained (EK-Number: GS1-EK-4/518-2017). EC of the Federal Stat Lower Austria.
Consent for Publication
Not applicable
Acknowledgments
Not applicable
Competing Interests
The authors declare that they have no competing interests.
Availability of Data and Material
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Authors' Contributions
JGG conceived and designed the study. ME wrote the manuscript with contributions by JGG and ST. ME and JGG did the radiological measures and the assessment of the clinical outcome. ME, JGG, and ST performed the statical analysis. All authors analysed and interpreted the data. All authors discussed, revised and approved the final manuscript.
Funding
Not applicable.
References
- van der Roer N, de Lange ESM, Bakker FC, et al. Management of traumatic thoracolumbar fractures: a systematic review of the literature. Eur Spine J 14 (2005): 527-534.
- Thomas C, Baily C, et al. Comparison of operative and nonoperative treatment for thoracolumbar burst fractures in patients without neurological deficit: a systematic review 19 (2006): 1-8.
- Vaccaro AR, Silber JS. Post-traumatic Spinal Deformity30 (2001): 1-8.
- Reinhold M, Audigé L, Schnake KJ, et al. AO spine injury classification system: a revision proposal for the thoracic and lumbar spine. Eur Spine J. 1st ed 22 (2013): 2184-2201.
- Fairbank JCT. Oswestry disability index. Journal of Neurosurgery: Spine. American Association of Neurological Surgeons 20 (2014): 239-241.
- Vedantam R, Lenke LG, Keeney JA, et al. Comparison of Standing Sagittal Spinal Alignment in Asymptomatic Adolescents and Adults. SPINE 23 (1998): 211-215.
- Berthonnaud É, Dimnet JS, Roussouly P, et al. Analysis of the Sagittal Balance of the Spine and Pelvis Using Shape and Orientation Parameters. J Spinal Disord Tech. Journal of Spinal Disorders & Techniques 18 (2005): 40-47.
- Boulay C, Tardieu C, Hecquet J, et al. Sagittal alignment of spine and pelvis regulated by pelvic incidence: standard values and prediction of lordosis. Eur Spine J 15 (2005): 415-422.
- Gelb DE, Lenke LG, Bridwell KH, et al. An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine 20 (1995): 1351-1358.
- Vialle RL, Levassor N, Rillardon L, et al. Radiographic Analysis of the Sagittal Alignment and Balance of the Spine in Asymptomatic Subjects. The Journal of Bone & Joint Surgery 87 (2005): 260-267.
- Koller H, Acosta F, Hempfing A, et al. Long-term investigation of nonsurgical treatment for thoracolumbar and lumbar burst fractures: an outcome analysis in sight of spinopelvic balance. Eur Spine J 17 (2008): 1073-1095.
- Rechtine GR, Bono PL, Cahill D, et al. Postoperative Wound Infection after Instrumentation of Thoracic and Lumbar Fractures. Journal of Orthopaedic Trauma 15 (2001): 566-569.
- Korovessis P, Baikousis A, Zacharatos S, et al. Combined Anterior Plus Posterior Stabilization Versus Posterior Short-Segment Instrumentation and Fusion for Mid-Lumbar (L2–L4) Burst Fractures. Spine 31 (2006): 859-868.
- Agus H, Kayal? C, Arslantas M. Nonoperative treatment of burst-type thoracolumbar vertebra fractures: clinical and radiological results of 29 patients. Eur Spine J 14 (2004): 536-540.
- Bence T, Schreiber U, Grupp T, et al. Two column lesions in the thoracolumbar junction: anterior, posterior or combined approach? A comparative biomechanical in vitro investigation. Eur Spine J 16 (2006): 813-820.
- Kandziora F, Schnake KJ, Pingel A, et al. Posttraumatic thoracolumbar kyphosis. Trauma und Berufskrankheit. Springer-Verlag 11 (2009): 80-86.
- Oner FC, van Gils APG, Faber JAJ, et al. Some Complications of Common Treatment Schemes of Thoracolumbar Spine Fractures Can Be Predicted With Magnetic Resonance Imaging. Spine 27 (2002): 629-636.
- Pishnamaz M, Curfs I, Balosu S, et al. Two-Nation Comparison of Classification and Treatment of Thoracolumbar Fractures: An Internet-Based Multicenter Study Among Spine Surgeons. Spine 40 (2015): 1749-1756.
- Scheer JK, Bakhsheshian J, Fakurnejad S, et al. Evidence-Based Medicine of Traumatic Thoracolumbar Burst Fractures: A Systematic Review of Operative Management across 20 Years. Global Spine Journal 5 (2014): 73-82.
- Aleem IS, Nassr A. Cochrane in CORR®: Surgical Versus Non-surgical Treatment for Thoracolumbar Burst Fractures without Neurological Deficit. Clinical Orthopaedics and Related Research®. Springer US 22 (2015): 1-6.
- Gnanenthiran SR, Adie S, Harris IA. Nonoperative versus Operative Treatment for Thoracolumbar Burst Fractures without Neurologic Deficit: A Meta-analysis. Clinical Orthopaedics and Related Research® 470 (2011): 567-77.
- Wood KB, Buttermann GR, Phukan R, Deficit. The Journal of Bone & Joint Surgery 97 (2014): 3-9.
- Verlaan JJ, Diekerhof CH, Buskens E, et al. Surgical Treatment of Traumatic Fractures of the Thoracic and Lumbar Spine 16 (2004):1-12.
- Giele BM, Wiertsema SH, Beelen A, et al. No evidence for the effectiveness of bracing in patients with thoracolumbar fractures 24 (2009):1-7.
- Wood KB, Buttermann GR, Phukan R, et al. Operative Compared with Nonoperative Treatment of a Thoracolumbar Burst Fracture without Neurological Deficit. The Journal of Bone & Joint Surgery 97 (2014): 3-9.
- Wardlaw D, Cummings SR, Van Meirhaeghe J, et al. Efficacy and safety of balloon kyphoplasty compared with non-surgical care for vertebral compression fracture (FREE): a randomised controlled trial. The Lancet. Elsevier Ltd 373 (2009): 1016-1024.
- Rzewuska M, Ferreira M, McLachlan AJ, et al. The efficacy of conservative treatment of osteoporotic compression fractures on acute pain relief: a systematic review with metaanalysis. Eur Spine J 24 (2015): 702-714.
- Slavici A, Rauschmann M, Fleege C. Conservative management of osteoporotic vertebral fractures: an update. Eur J Trauma Emerg Surg 43 (2017): 19-26.
- Giele BM, Wiertsema SH, Beelen A, et al. No evidence for the effectiveness of bracing in patients with thoracolumbar fractures. Acta Orthopaedica 80 (2009): 226-232.
- Shamji MF, Roffey DM, Young DK, et al. A pilot evaluation of the role of bracing in stable thoracolumbar burst fractures without neurological deficit. J Spinal Disord Tech 27 (2014): 370-375.
- Jin YZ, Lee JH. Effect of Brace to Osteoporotic Vertebral Fracture: a Meta-Analysis. J Korean Med Sci 31 (2016): 1641-1649.
- Barrey CD, Roussouly P, Perrin G, et al. Sagittal balance disorders in severe degenerative spine. Can we identify the compensatory mechanisms? Eur Spine J 20 (2011): 626-633.
- Diebo BG, Varghese JJ, Lafage R, et al. Sagittal alignment of the spine: What do you need to know? Clinical Neurology and Neurosurgery. Elsevier B.V 139 (2015): 295-301.
- Koller H, Acosta F, Hempfing A, et al. Long-term investigation of nonsurgical treatment for thoracolumbar and lumbar burst fractures: an outcome analysis in sight of spinopelvic balance. Eur Spine J 17 (2008): 1073-1095.
- Mayer M, Ortmaier R, Koller H, et al. Impact of Sagittal Balance on Clinical Outcomes in Surgically Treated T12 and L1 Burst Fractures: Analysis of Long-Term Outcomes after Posterior-Only and Combined Posteroanterior Treatment. BioMed Research International 2017 (2017): 1-10.
- Agus H, Kayal? C, Arslantas M. Nonoperative treatment of burst-type thoracolumbar vertebra fractures: clinical and radiological results of 29 patients. Eur Spine J 14 (2004): 536-540.
- Siebenga J, Leferink JMV, Segers JMM, et al. Treatment of Traumatic Thoracolumbar Spine Fractures: A Multicenter Prospective Randomized Study of Operative versus Nonsurgical Treatment. Randomized Controlled Trial 17 (2006):1-10.
- Tezer M, Erturer RE, Ozturk C, et al. Conservative treatment of fractures of the thoracolumbar spine. International Orthopaedics (SICOT) 29 (2005): 78-82.
- Wood K, Buttermann G, Mehbod A, et al. Operative Compared with Nonoperative Treatment of a Thoracolumbar Burst Fracture without Neurological Deficit 22 (2003): 1-9.


 Impact Factor: * 5.8
Impact Factor: * 5.8 Acceptance Rate: 71.20%
Acceptance Rate: 71.20%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 