Hematometra in a Patient without Previous Surgeries/Anomalies in a Resource Constraint Setting- A Case Report from Bangem District Hospital
Nkengafac N Fobellah*, Constantine Asahngwa, Charlotte Bongfen, Ronald Gobina, Kibu Odette, Wilfred Ngwa, Denis Foretia
Department of General Medicine, Bangem District Hospital, Bangem, Cameroon
*Corresponding author: Nkengafac N Fobellah, Department of General Medicine, Bangem District Hospital, Bangem, Cameroon
Received: 01 May 2021; Accepted: 13 May 2021; Published: 01 June 2021
Article Information
Citation: Nkengafac N Fobellah, Constantine Asahngwa, Charlotte Bongfen, Ronald Gobina, Kibu Odette, Wilfred Ngwa, Denis Foretia. Hematometra in a Patient without Previous Surgeries/Anomalies in a Resource Constraint Setting- A Case Report from Bangem District Hospital. Archives of Clinical and Biomedical Research 5 (2021): 410-414.
View / Download Pdf Share at FacebookAbstract
Background: Hematometra is a disorder where the uterus collects and gets filled with menstrual blood. This is usually due to a blockage at the cervix. It can either be congenital or acquired. Hematometra usually presents after puberty as primary amenorrhea. These patients present with recurrent cramping pelvic pain, urinary frequency or retention and a pelvic mass. On palpation, the uterus feels firm and enlarged. The goal standard is the evacuation of these blood clots by dilation and curettage (D $ C)./p>
Case presentation: This patient was a 39-year-old non-pregnant, G2P1001 female, who presented in October 2020 with complaints of pelvic pain and pelvic pressure for two months with associated amenorrhea. She had no history of previous surgeries or cervical anomalies. Dilatation and curettage did not work out for her and so a low midline incision was done to the uterus and blood from the uterus was evacuated and later dilators were used inwardly to dilate her cervix. Her postoperative recovery was good and menses resumed immediately the month after till date.
Conclusion: Once diagnosed of hematometra, there is immediate is need to evacuate the blood clots. Cervical stenosis is the most common cause of hematometra in patients with no history of previous surgeries or anomalies.
Keywords
<p>Hematometra; Dilatation and curettage; Amenorrhea; Pelvic pain</p>
Article Details
1. Background
Hematometra or hematometra is a disorder in which the uterus filled with menstrual blood [1]. It could be congenital or acquired. Congenitally, it could be due to abnormalities in the cervix or uterus while the acquired type is usually due to processes that cause obstruction of the cervical canal [2]. An example of a congenital defect is cervical atresia while hematometra can be acquired through cervical or uterine procedures like uterine ablation or doing cone biopsy of the cervix [3]. Hematometra usually presents after puberty as primary amenorrhea as there is is usually no passage for menstrual blood. These patients present with recurrent cramping pelvic pain, urinary frequency or retention and a pelvic mass [4]. On palpation, the uterus feels firm and enlarged and management is usually by dilatation and curettage [5].
2. Case Presentation
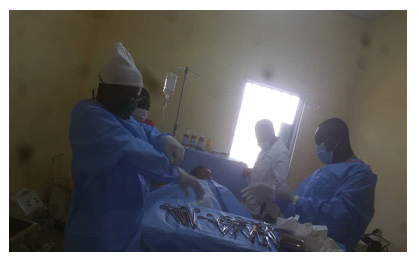
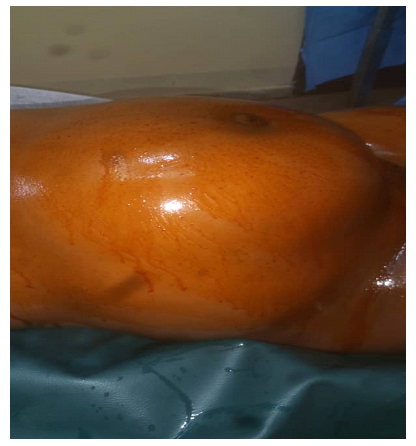
This patient was a 39-year-old non-pregnant, G2P1001 female, who presented in October 2020 with complaints of pelvic pain and pelvic pressure for two months with associated amenorrhea. The pain radiated to her back, no relieving factors, it was excruciating and the patient reported that her last menstrual period (LMP) was in 2019. She has a history of one normal spontaneous vaginal delivery (NSVD), no history of STI’s and no significant medical history. She had no history of previous surgeries. Menarche was at 13 years and her cycles were regular and occurred every 30 days. She had never used any family planning method. On examination, both lower quadrants were very tender to light and deep palpation and there was rebound tenderness. Pelvic exam showed complete occlusion of the cervical canal as well as palpable, boggy uterus. There was a high clinical suspicion for hematometra as the cause of her symptoms and the patient was scheduled for Dilatation and Curettage (D&C) with ultrasound guided placement of a lacrimal probe for management of cervical stenosis, hematometra and hematocolpos and possible laparotomy if dilatation of the cervix fails. Prior to surgery the patient received Misoprostol (Cytotec) 25 microgram vaginally. Perioperative pelvic exam revealed an anteverted uterus (14 weeks size), non-palpable ovaries and adnexa, stenotic closed cervical os, and no active bleeding at the time of examination. Under direct Trans abdominal ultrasound guidance, a dilator was inserted into the stenotic cervical oz and the cervical canal was visualized by sonogram. Serial cervical dilation was tried using cervical dilators to no avail. A low midline incision was done from skin to uterus and blood clots evacuated from the uterus. Cervical dilators were now inserted from inside the uterus and this time the cervix became dilated. Thereafter, the uterus was sutured and other abdominal layers in planes till the skin. The patient had uncomplicated postoperative course and full recovery with resumption of menses in the month following the procedure (Figure 1).
3. Discussion
Hematometra is the collection and filling of the uterus with menstrual blood. It could be congenital or acquired [1]. It still stands out as a challenging abdominal pain to diagnose. Hematocolpos is a general term for a medical condition in which the vagina is pooled with menstrual blood. Hematocolpos can be caused by a combination of menstruation with an imperforate hymen, and can be seen in Robinow Syndrome, uterus didelphys, and other vaginal anomalies [6]. The diagnosis for hematometra could be difficult in patients without anomalies or history of previous surgery or gynecological procedures. One case of hematometra was reported with a previous cervical cone biopsy and loop electrosurgical excision procedure [7].
Hematometra most commonly presents with amenorrhea, pelvic pain with or without urinary symptoms. A good pelvic exam and ultrasound is very useful to aid your diagnosis [8]. Management of hematometra involves dilatation of the cervix to drain the blood using lacrimal or Hegars dilators [9]. This is done by ultrasound guidance. This was a limitation in this our rural setting and explains the reasons why despite all attempts, the cervix did not dilate and a low midline incision was done to the uterus before the cervix was dilated from inside. There’s therefore the need for more studies to be done on the predisposing factors leading to hematometra and eventual different methods in the management of hematometra.
4. Conclusion
The diagnosis of hematometra is difficult in patients without previous surgery or any anomalies. Whenever any patient presents with pelvic pain and amenorrhoea, hematometra should be a differential diagnosis especially in women of child bearing age. Management by dilatation and curettage is goal standard though in extreme cases, surgery could be necessary. Cervical stenosis is a common cause of hematometra.
References
- Kloss, Brian T, Nacca, et al. Hematocolpos secondary to imperforate hymen. International Journal of Emergency Medicine 3 (2010): 481-482.
- Motegi E, Hasegawa K, Kawai S, et al. Levonorgestrel-releasing intrauterine system placement for severe uterine cervical stenosis after conization: two case reports. J Med Case Rep 10 (2016): 56-60.
- Hoffman BL, Schorge JO, Schaffer JI, et al. Williams Gynecology (2nd edtn), New York City: Mc Graw- Hill companies, INC, USA (2012).
- Verma SK, Baltarowich OH, Lev-Toaff AS, et al. Hematocolpos secondary to acquired vaginal scarring after radiation therapy for colorectal carcinoma. Journal of ultrasound in medicine 28 (2009): 949-953.
- Wikipedia (2019).
- The treatment of imperforate hymen with Hematocolpos. Journal of the American Medical Association 113 (1939): 913-916.
- Shadi R, Daniel L, Kimberley C, et al. Hematometra and hematocolpos, secondary to cervical canal occlusion, a case report and review of literature (2018).
- Dupuis CS, Kim YH. Ultrasonography of adnexal causes of acute pelvic pain in premenopausal non pregnant women 34 (2015): 258-67.
- Crane JM. How to overcome a resistant cervix for hysteroscopy and endometrial biopsy. OBG Management 19 (2007): 37-44.


 Impact Factor: * 5.8
Impact Factor: * 5.8 Acceptance Rate: 71.20%
Acceptance Rate: 71.20%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 