Raised Serum Homocysteine Level is Associated with Coronary Artery Disease in Young Patients
Rokshana Begum1*, Mohammad Monzurul Alam Bhuiyan2, Sheuly Ferdoushi3, Khandoker Abdur Rahim4, Dipal K. Adhikari5, Shihab Md. Rezoyanur Rahman6, Amit Kumar Pramanik7, AKM Shahidur Rahman8, Farzana Islam Khan9, Mukul Chandra Nath10, Md. Saiful Islam3
1Consultant, Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
2Assistant professor, Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
3Associate professor, Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
4Consultant, Department of Orthopaedic surgery, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
5Associate professor, Department of Cardiology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
6Pathologist, Department of Pathology and Blood Transfusion, Gaibandha General Hospital, Gaibandha, Bangladesh
7Medical officer, Department of Transfusion Medicine, Rajshahi Medical College Hospital, Rajshahi, Bangladesh
8Medical officer, Department of Nephrology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
9Associate professor and Head of the Department, Department of Community Medicine, Ashiyan Medical College, Dhaka, Bangladesh
10Assistant Professor and Head of the Department, Department of Psychiatry, Marine City Medical College, Chattogram, Bangladesh
*Corresponding author: Dr. Rokshana Begum, Consultant, Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh
Received: 13 June 2022; Accepted: 21 June 2022; Published: 27 June 2022
Article Information
Citation: Begum R, Bhuiyan MMA, Ferdoushi S, Rahim KA, Adhikari DK, Rahman SMR, Pramanik AK, Rahman AKMS, Khan FI, Nath MC, Islam MS. Raised Serum Homocysteine Level is Associated with Coronary Artery Disease in Young Patients. Archives of Clinical and Biomedical Research 6 (2022): 575-586.
View / Download Pdf Share at FacebookAbstract
Background: Coronary artery disease (CAD) is increasingly prevalent among young population. High serum homocysteine level has been suggested as a risk factor for atherosclerosis leading to CAD. This study was aimed to evaluate serum homocysteine level in young and adult patients with coronary artery disease.
Methods: This cross-sectional study was conducted at the Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh, from March 2021 to February 2022. A total of 52 patients with coronary artery disease were included. Among them 26 were young patients (age <40 years, group I) and 26 were adults (age ≥40 years, group II). Their relevant history, clinical examination findings and risk factor profiles were noted accordingly. Serum homocysteine level was estimated by automated immunoassay analyzer with the principle of chemiluminescent microparticle immunoassay (CMIA). Data were analyzed and compared by statistical tests.
Results: Male patients were predominant in both groups. Regarding risk factors, smoking habit and diabetes mellitus had significant difference between young and adult individuals having CAD (p<0.05). It was observed that mean(±SD) serum homocysteine level was significantly higher in young patients than adults (21.93±7.56 μmol/L versus 12.04±5.33 μmol/L, p <0.001). Moderate hyperhomocysteinemia and intermediate hyperhomocysteinemia was significantly present in group I than group II (69.2% versus 15.4% and 30.8% versus 0.0%, p <0.001).
Conclusion: Serum homocysteine level is significantly higher in young patients than adult patients with coronary artery disease. Therefore, high level of serum homocysteine may be used as early detection and disease evaluation
Keywords
<p>Coronary Artery Disease (CAD); Risk Factors; Serum Homocysteine (Hcy); Young Patients</p>
Article Details
1. Introduction
Coronary artery disease (CAD) is a disease in which there is a narrowing or blockage of the coronary arteries that usually caused by atherosclerosis [1]. Coronary artery disease (CAD) is defined as any patient having myocardial infarction (MI) and ischemia evidenced by electrocardiogram (ECG), echocardiogram (Echo) and coronary angiography (CAG) [1]. Coronary artery disease (CAD) is one of the leading causes of death worldwide [2]. Coronary artery disease is more diffuse and aggressive in adult population, although it strikes at a younger age [3, 4]. In South Asians, the prevalence of coronary artery disease is rising, as is the burden of cardiovascular disease [5]. It affects people in South Asia earlier than it does those in Europe and Western countries [5]. Acute myocardial infarction (AMI) is the primary cause of death in persons over the age of 40, and even in those under the age of 40 [6]. It was reported that, the risk of acute myocardial infarction is higher in the younger population than adults [7]. Several risk factors are linked to coronary artery disease [8, 9]. Some are modifiable like-hypertension, dyslipidemia, smoking, diabetes mellitus, obesity, lack of physical activity, an unhealthy diet habit and excessive stress; while others (genetic, racial) are not [8, 9]. Beyond established risk factors, many conditions are gaining attention as emergent risk factors for coronary artery disease [2, 10]. A higher level of homocysteine (Hcy) in the blood is regarded as a new risk factor and a treatable condition of CAD [2, 10. 11]. Homocysteine (Hcy) is a sulfur-containing non-protein forming amino acid, which occurs naturally in the blood plasma [12]. It is an intermediate product in the normal biosynthesis of methionine and cysteine [12]. It is produced via demethylation of dietary methionine, which is abundant in animal protein [12]. Normal homocysteine concentrations in healthy subjects range from 5 µmol/L to 15 µmol/L [13]. Hyperhomocysteinemia (>15 µmol/L) causes endothelial cell damage, smooth muscle cell hyperplasia and vascular occlusion, all of which contribute to atherosclerosis [14]. It was reported that, about half of patients with untreated hyperhomocysteinemia develop different cardiovascular disease before the age of 30 [12, 15]. Moreover, hyperhomocysteinemia is associated with an increased risk of athero-thrombotic disease [12, 14-16]. Atherosclerosis leads to coronary artery disease like- myocardial infarction/ischemia [17]. Recent studies suggested that, nearly one-third of patients with atherosclerosis had elevated plasma homocysteine [15-17]. Elevation by 12% above the upper limit of normal plasma homocysteine (15 µmol/L) is associated with a three-fold increase in the risk of acute myocardial infarction (AMI) [15]. Therefore a high homocysteine level considered as a risk factor for coronary artery disease (CAD) [15-18]. Though age is the most important risk factor for coronary artery disease (CAD), it is becoming more common in young adults [3, 11]. Several studies suggested that hyperhomocysteinemia is associated with coronary artery disease in young patients [2, 10, 11]. Early detection of this risk factor may improve prognosis and helps to prevent coronary artery disease particularly among young patients. In this background this study aimed to evaluate serum homocysteine levels in young and adult patients with coronary artery disease.
2. Methodology
2.1 Study design
This cross-sectional study was conducted in the Department of Laboratory Medicine, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka, Bangladesh from March 2021 to February 2022. The study was approved by the Ethical Review Committee, BSMMU, Dhaka, Bangladesh.
2.2 Study population
Diagnosed cases of young and adult coronary artery disease patients admitted in inpatient department (IPD) of Department of Cardiology, BSMMU were enrolled into the study. Patients with coronary artery disease were confirmed by electrocardiography (ECG), echocardiography (ECHO) and coronary angiography (CAG). A total of 52 patients [26 young patients (Group I) and 26 adult patients (Group II)] were selected purposively according to the selection criteria. Young [age<40 years (18-39 years)] and adult patients (age≥40 years) of both sexes with coronary artery disease (CAD) were included. Patients with renal/hepatic failure, patients having any types of malignancy, patients with myocarditis or infective endocarditis and patients on vitamin B12 or folate supplementation were excluded from the study.
2.3 Recruitment of study subjects
From inpatient department of Department of Cardiology, BSMMU; diagnosed cases of coronary artery disease (CAD) patients were included in this study. Coronary artery disease (CAD) cases were diagnosed by cardiologist according to electrocardiography (ECG), echocardiography (ECHO) and coronary angiography (CAG). Report of ECG, ECHO and CAG were collected from patient files. Report of serum lipid profile [Total Cholesterol (TC), High Density Lipoprotein- Cholesterol (HDL- C), Low Density Lipoprotein- Cholesterol (LDL- C) and Triglyceride (TG)] was also collected from patient files.
2.4 Study procedure
After ethical clearance from institutional review board (IRB), diagnosed case of young and adult coronary artery disease (CAD) patients who admitted in Department of Cardiology, BSMMU were selected. Informed written consent was taken from each study participant prior to the enrollment. Patients ECG, ECHO and CAG reports were evaluated to diagnose as coronary artery disease. Their demographic data, detailed history and relevant clinical examination findings were recorded. Risk factor profiles including- smoking, hypertension, family history of coronary artery disease, diabetes mellitus, dyslipidaemia and obesity were noted. Then fasting venous blood of the study subjects was collected for estimation of serum homocysteine level.
2.5 Collection, processing and analysis of blood samples
With all aseptic precaution 2 ml venous blood (fasting) from the median cubital vein of each study subject was collected in a red test tube following standard procedure. After collection, tubes were labeled with the patient’s identification number and kept in vertical position for 30 minutes. Then blood was centrifuged at 3000 rpm/minutes for 5 minutes in room temperature (22°C - 24°C). Serum was separated by micro-pipette and collected into appendrope, then preserved at −20°C temperature until further analysis. Collected every test sample was run two successive days per week. Serum homocysteine level was estimated by automated immunoassay analyzer with the principle of chemiluminescent microparticle immunoassay (CMIA) in the Department of Biochemistry and Molecular Biology, BSMMU, Dhaka, Bangladesh.
2.6 The reference value of serum homocysteine
The reference normal range of serum homocysteine (5-15 µmol/L) used in this study was according to the Biochemistry and Molecular Biology Laboratory, Department of Biochemistry and Molecular Biology, Bangabandhu Sheikh Mujib Medical University(BSMMU) Dhaka, Bangladesh [13]. Elevated serum homocysteine is referred to as hyperhomocysteinemia (HHCy). Hyperhomocysteinemia has been classified by Kang et al. as follows [19] -
- Moderate hyperhomocysteinemia (16 to 30 µmol/L)
- Intermediate hyperhomocysteinemia (31 to 100 µmol/L)
- Severe Hyperhomocysteinemia (>100 µmol/L)
2.7. Statistical analysis
Data were processed and analyzed using Statistical Package for Social Sciences (SPSS) version 26. Quantitative variables were measured as mean ± SD (standard deviation). Qualitative variables were measured as the frequency and percentage. Chi-square (x2) test and unpaired t-test was performed to analyze the data. A p value <0.05 was considered as statistically significant.
3. Results
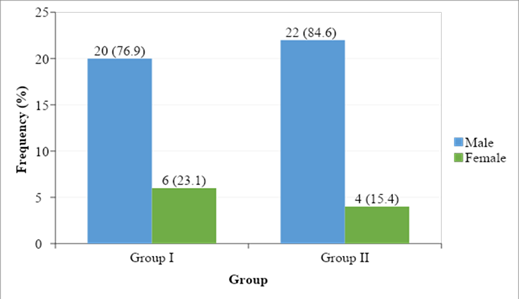
This cross-sectional study was intended to assess serum homocysteine level in young and adult patients with coronary artery disease. A total of fifty two (52) patients with coronary artery disease were included. Of them; 26 young patients (age <40 years) were categorized as group I and 26 adult patients (age ≥40 years) were categorized as group II. Among the young patients (group I); 20 (76.9%) were male and 6 (23.1%) were female. While in the group II (adult patients); 22 (84.6%) were male and rest 4 (15.4%) were female (Figure- 1).
On risk factor analysis among the study subjects, it was observed that smoking habit was significantly higher in group I than group II patients (65.4% versus 34.6%, p= 0.027). Diabetes mellitus was significantly higher in group II than group I (61.5% versus 26.9%,p= 0.012). Hypertension and dyslipidemia were comparatively higher in group II than group I (76.9% versus 61.5%, p= 0.229 and 53.8% versus 46.2%, p = 0.579 respectively). Family history of CAD and obesity were relatively more in group I than group II (53.8% versus 46.2%,p = 0.579 and 53.8% versus 42.3%, p = 0.405) (Table- I).
Table I: Distribution of risk factors in two groups among the study subjects (N=52)
|
Risk factors* |
Group I (Young) No. (%) |
Group II (Adult) No. (%) |
p-value |
|
Smoking |
17 (65.4%) |
9 (34.6%) |
0.027s |
|
Diabetes mellitus |
7 (26.9%) |
16 (61.5%) |
0.012s |
|
Hypertension |
16 (61.5%) |
20 (76.9%) |
0.229 ns |
|
Family of CAD |
14 (53.8%) |
12 (46.2%) |
0.579ns |
|
Dyslipidemia |
12 (46.2%) |
14 (53.8%) |
0.579 ns |
|
Obesity |
14 (53.8%) |
11 (42.3%) |
0.405ns |
*Multiple response, Chi-square test was performed to compare the differences between two groups, s=significant, ns= not significant
Table II shows the comparison of serum lipid profile [Total Cholesterol (TC), High Density Lipoprotein- Cholesterol (HDL- C), Low Density Lipoprotein- Cholesterol (LDL- C) and Triglyceride (TG)] findings among the study subjects. The mean (±SD) serum total cholesterol (219.65±40.50 mg/dl versus 182.85±42.17 mg/dl, p = 0.002), HDL- C (52.81±11.03 mg/dl versus 46.31±7.07mg/dl, p = 0.015) and triglyceride (283.69±69.99 mg/dl versus 223.42±52.08 mg/dl, p =0.001) levels were significantly higher in group II patients than group I patients. While no significant difference was observed in mean (±SD) LDL- C level among the groups (128.04±41.99mg/dl versus 128.5 ± 33.12mg/dl, p= 0.965) (Table- II).
Table II: Comparison of lipid profile between the groups (N=52)
|
Lipid profile |
Group I (n=26) Mean (±SD) |
Group II (n=26) Mean (±SD) |
p-value |
|
Total Cholesterol (mg/dl) |
182.85±42.17 |
219.65±40.50 |
0.002s |
|
HDL- C (mg/dl) |
46.31±7.07 |
52.81±11.03 |
0.015s |
|
LDL- C (mg/dl) |
128.04±41.99 |
128.5 ± 33.12 |
0.965ns |
|
Triglyceride (mg/dl) |
223.42±52.08 |
283.69±69.99 |
0.001s |
Unpaired t-test was performed to compare differences between two groups, s= significant, ns= not significant
Table III shows the electrocardiographic (ECG) findings in two groups. We found that myocardial infarction (MI) was significantly prevalent in group I patients than group II patients (65.4% versus 34.6%, p = 0.027). On the other hand ischemia was significantly high in group II patients than group I patients (65.4% versus 34.6%, p = 0.027) (Table- III).
Table III: Electrocardiographic (ECG) findings of the study subjects (N=52)
|
Electrocardiography (ECG) |
Group I (n=26) No. (%) |
Group II (n=26) No. (%) |
p-value |
|
Presence of MI |
17 (65.4%) |
9 (34.6%) |
0.027s |
|
Presence of Ischemia |
9 (34.6%) |
17 (65.4%) |
|
|
Total |
26 (100.0%) |
26 (100.0%) |
Chi-square test was performed to compare the differences between two groups, s= significant
Table- IV shows the echocardiographic findings among the study patients in two groups. Presence of echocardiographic regional wall motion abnormalities (RWMA) was more frequent in group I patients than group II patients (57.7% versus 38.5%, p=0.165) (Table- IV).
Table- IV: Echocardiographic (ECHO) findings of the study subjects (N=52)
|
Echocardiogram |
Group I (n=26) No. (%) |
Group II (n=26) No. (%) |
p-value |
|
Presence of RWMA |
15 (57.7%) |
10 (38.5%) |
0.165ns |
|
Absence of RWMA |
11 (42.3%) |
16 (61.5%) |
|
|
Total |
26 (100.0%) |
26 (100.0%) |
Chi-square test was performed to compare the differences between two groups, ns= not significant
Table- V shows the angiographic findings in two groups. Single vessel disease was significantly more prevalent in group I patients than group II patients (61.5% versus 23.1%, p= 0.005). While, double vessel disease (50.0% versus 26.9%, p = 0.087) and triple vessel disease (26.9% versus 11.5%, p= 0.159) were comparatively more frequent in group II patients than group I patients (Table- V).
Table- V: Angiographic findings of the study subjects (N=52)
|
Angiographic findings |
Group I (n=26) No. (%) |
Group II (n=26) No. (%) |
p-value |
|
Single vessel disease |
16 (61.5%) |
6 (23.1%) |
0.005s |
|
Double vessel disease |
7 (26.9%) |
13 (50.0%) |
0.087ns |
|
Triple vessel disease |
3 (11.5%) |
7 (26.9%) |
0.159ns |
|
Total |
26 (100.0%) |
26 (100.0%) |
Chi-square test was performed to compare the differences between two groups, s= significant, ns= not significant
Among the study population the mean (±SD) serum homocysteine level was significantly high in group I patients than that in group II patients (21.93±7.56 µmol/L and 12.04±5.33 µmol/L, p=0.001) (Table- VI).
Table- VI: Comparison of serum homocysteine level between two groups (N=52)
|
Serum homocysteine (µmol/L) |
Group I (n=26) |
Group II (n=26) |
p-value |
|
Mean (±SD) |
21.93±7.56 |
12.04±5.33 |
0.001s |
|
Range (minimum- maximum) |
15.33 – 48.42 |
5.90 – 18.45 |
Unpaired t-test was performed to compare the difference between two groups, s= significant
Data analysis revealed that, serum homocysteine level was within normal limit among 22 (84.6%) patients in group II. Patients with moderate hyperhomocysteinemia and intermediate hyperhomocysteinemia was significantly present in group I than group II [18 (69.2%) patients versus 4 (15.4%) patients and 8 (30.8%) patients versus 0 (0.0%) patients, p <0.001]. Patient with severe hyperhomocysteinemia was not observed in this study (Table- VII).
Table- VII: Severity of serum homocysteine levels in two groups (N=52)
|
Serum homocysteine (µmol/L) |
Group I (n=26) No. (%) |
Group II (n=26) No. (%) |
p-value |
|
Normal limit (5-15) |
0 (0.0%) |
22 (84.6%) |
<0.001s |
|
Moderate hyperhomocysteinemia (16-30) |
18 (69.2%) |
4 (15.4%) |
|
|
Intermediate hyperhomocysteinemia (31-100) |
8 (30.8%) |
0 (0.0%) |
|
|
Severe hyperhomocysteinemia(>100) |
0 (0.0%) |
0 (0.0%) |
|
|
Total |
26 (100.0%) |
26 (100.0%) |
Chi-square test was performed to compare the differences between two groups, s= significant
4. Discussion
Coronary artery disease (CAD) is one of the major public health problems. It is the leading cause of morbidity and mortality in both developed and developing countries [20]. The incidence is doubled in South Asia than in any other regions of the world [5, 21]. CAD is the leading cause of death in people aged more than 40 years and even in the younger individuals [20]. Coronary artery disease is a serious condition and early diagnosis is necessary to halt the disease progress. High level of homocysteine causes- proliferation/thickening of vascular smooth muscle cells, oxidative stress and endothelial dysfunction which can lead to coronary artery disease [22]. During recent years it has been suggested that raised serum homocysteine level is significantly associated with the coronary artery disease [20-21]. Therefore the aim of this study was to evaluate the serum homocysteine level in young and adult patients with coronary artery disease. Total 52 patients with coronary artery disease were included. Of them 26 were young patients [(age <40), group I] and 26 were adult patients [age (≥40 years), group II]. Among the young patients; 20 were male and 6 were female. While among the adult patients; 22 were male and 4 were female. Male patients were comparatively predominant in both groups. This finding was consistent with similar previous studies [10, 21, 23].
The current study demonstrates that baseline risk factors had an important role in identifying young and adult patients at risk for CAD. Traditional risk factors such as smoking, hypertension, diabetes mellitus, dyslipidemia, family history of CAD and obesity were more prevalent in CAD [10, 23]. Among the study patients, smoking habit was found significantly higher in young than adults (64.4% versus 34.6%, p= 0.027). In accordance Islam et al. found a significant high prevalence of smoking in young than adults [23]. In this present study, diabetes mellitus was found significantly higher in adults than young patients (61.5% versus 26.9%, p= 0.012). Similar finding was observed in a couple of previous studies [10, 23]. In this study, other risk factors like hypertension, dyslipidemia were relatively higher in adults than young patients (76.9% versus 61.5% and 53.8% versus 46.2% respectively). While family history of CAD and obesity were more frequent in young patients than adults (53.8% versus 46.2% and 53.8% versus 42.3% respectively).These findings were closely resembled with related previous studies [14, 23, 24].
In this present study, serum fasting lipid profile of both young and adult groups was evaluated. The mean (±SD) serum total cholesterol (219.65±40.50 mg/dl versus 182.85±42.17 mg/dl, p = 0.002), HDL- C (52.81±11.03 mg/dl versus 46.31±7.07 mg/dl, p = 0.015) and triglyceride (283.69±69.99 mg/dl versus 223.42±52.08 mg/dl, p =0.001) levels were significantly higher in group II patients than group I patients. But no significant difference was observed in mean (±SD) LDL- C level among the groups (128.04±41.99 mg/dl versus 128.5 ± 33.12 mg/dl, p= 0.965).In this context Ibrahim et al. also found that mean cholesterol was significantly higher in young than adult group (231.0 versus. 217.8, p= 0.05) [25]. While opposite result was observed in another previous study [26].They found no significant differences in serum LDL, HDL and serum triglyceride levels among the groups [26]. This variability of lipid profile may be due to difference in genetic makeup, lifestyle and dietary/nutritional habits among different population.
In this study, it was observed that myocardial infarction (MI) was more significantly associated with young patients than adults (65.4% versus 34.6%, p=0.027). This finding was in a line of similar previous studies [27, 28]. The present study demonstrated that regional wall motion abnormality (RWMA) was found more frequent in young than adults (57.7% versus 38.5%, p= 0.165). In a previous study it also found that RWMA was relatively higher among young patients than adults [44.4% versus 33.3%,p=0.4858] [28]. In this present study, single vessel disease was found significantly higher in young than adults (61.5% versus 23.1%, p= 0.005). In accordance Bush et al. reported that single vessel disease was significantly higher in young than adults (39.6% versus 27.1%, p=0.001) [5]. This current study also showed that the prevalence of double vessel disease (50.0% versus 26.9%, p=0.087) and triple vessel disease (26.9% versus 11.5%, p=0.159) were comparatively high in adults than young patients. This finding was consistent with a related previous study [5].
In this current study, we found that mean serum homocysteine level was significantly higher in young group than adult group (21.93±7.56 µmol/L versus 12.04±5.33 µmol/L, p=0.001). This finding was supported by a couple of previous studies [15-17]. In this present study, it was observed that severity of serum homocysteine level was significantly associated with young patients than adults. Serum homocysteine level was found within normal limit among 84.6% patients in adult group. On the other hand, patients with moderate hyperhomocysteinemia and intermediate hyperhomocysteinemia were significantly frequent in young patients group [69.2% versus 15.4% and 30.8% versus 0.0%, p <0.001]. Patient with severe hyperhomocysteinemia was not observed in this study. These results were consistent with a similar previous study [15]. This study observed that young patients with coronary artery disease had a raised serum homocysteine level than adults. Therefore, present study finding may help in disease evaluation of early coronary artery disease in young individuals.
5. Conclusion
This study concluded that, serum homocysteine level was significantly higher in young patients with coronary artery disease than adult patients with coronary artery disease. Therefore, high level of serum homocysteine may be used for detection and disease evaluation for coronary artery disease in young patients. Further studies warranted to elucidate the fact.
Limitations of the study
It was a single center study with a relatively small size.
Recommendations
Multicenter broad based prospective cohort study is required to confirm the findings of this present study.
Conflict of interest
The authors declare no conflicts of interest regarding the publication of this paper.
References
- Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD, Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. Fourth universal definition of myocardial infarction (2018). Journal of the American College of Cardiology 72 (2018): 2231-64.
- Chakrabarty U, Datta S, Mukherjee P. Correlation of Novel Risk Factors with Syntax Score in Young and Elderly Males with Coronary Artery Disease. Journal of Medical Science And clinical Research 8 (2020): 388-393.
- Klein LW, Agarwal JB, Herlich MB, Leary TM, Helfant RH. Prognosis of symptomatic coronary artery disease in young adults aged 40 years or less. The American journal of cardiology 60 (1987): 1269-72.
- Vardan S, Mookherjee S, Sinha AK. Special features of coronary heart disease in people of the Indian sub-continent. Indian heart journal 47 (1995): 399-407.
- Bush N, Sharma YP, Prasad K, Kumar P, Mehrotra S. Comparison of demographic profile, risk factors, and in-hospital outcome in young and old patients with acute coronary syndrome: A single-center experience. Journal of Family Medicine and Primary Care 10 (2021): 871.
- Fournier JA, Sanchez A, Quero J, Fernandez-Cortacero JA, González-Barrero A. Myocardial infarction in men aged 40 years or less: A prospective clinical-angiographic study. Clinical cardiology 19 (1996): 631-6.
- Joshi P, Islam S, Pais P, Reddy S, Dorairaj P, Kazmi K, Pandey MR, Haque S, Mendis S, Rangarajan S, Yusuf S. Risk factors for early myocardial infarction in South Asians compared with individuals in other countries. Jama 297 (2007): 286-94.
- Puri A, Gupta OK, Dwivedi RN, Bharadwaj RP, Narain VS, Singh S. Homocysteine and lipid levels in young patients with coronary artery disease. J Assoc Physicians India 51 (2003): 681-5.
- Roy S. Atherosclerotic cardiovascular disease risk and evidence-based management of cholesterol. North American Journal of Medical Sciences 6 (2014): 191.
- Shah H, Jan MU, Altaf A, Salahudin M. Correlation of hyper-homocysteinemia with coronary artery disease in absence of conventional risk factors among young adults. Journal of the Saudi Heart Association 30 (2018): 305-10.
- Kumar V, Kumar T, Sharma AK, Nath RK, Sharma LK, Pandit N, Raj A, Pandit BN. Risk factors, clinical presentation, angiographic profile and 30-day outcomes of young patients (aged≤ 35 Years) with ST-elevation myocardial infarction. Advances in Human Biology 11 (2021): 188.
- Faeh D, Chiolero A, Paccaud F. Homocysteine as a risk factor for cardiovascular disease: should we (still) worry about it?. Swiss medical weekly 136 (2006): 745-56.
- Ueland PM, Refsum H, Stabler SP, Malinow MR, Andersson A, Allen RH. Total homocysteine in plasma or serum: methods and clinical applications. Clinical chemistry 39 (1993): 1764-79.
- Zhang S, Bai YY, Luo LM, Xiao WK, Wu HM, Ye P. Association between serum homocysteine and arterial stiffness in elderly: a community-based study. Journal of geriatric cardiology: JGC 11 (2014): 32.
- Shenoy V, Mehendale V, Prabhu K, Shetty R, Rao P. Correlation of serum homocysteine levels with the severity of coronary artery disease. Indian Journal of Clinical Biochemistry 29 (2014): 339-44.
- Veeranna V, Zalawadiya SK, Niraj A, Pradhan J, Ference B, Burack RC, Jacob S, Afonso L. Homocysteine and reclassification of cardiovascular disease risk. Journal of the American College of Cardiology 30 (2011): 1025-33.
- Ganguly P, Alam SF. Role of homocysteine in the development of cardiovascular disease. Nutrition journal 14 (2015): 1-0.
- Pang X, Liu J, Zhao J, Mao J, Zhang X, Feng L, Han C, Li M, Wang S, Wu D. Homocysteine induces the expression of C-reactive protein via NMDAr-ROS-MAPK-NF-κB signal pathway in rat vascular smooth muscle cells. Atherosclerosis 236 (2014): 73-81.
- Kang SS, Wong PW, Malinow MR. Hyperhomocyst (e) inemia as a risk factor for occlusive vascular disease. Annual review of nutrition 12 (1992): 279-98.
- Sun J, Han W, Wu S, Jia S, Yan Z, Guo Y, Zhao Y, Zhou Y, Liu W. Associations between hyperhomocysteinemia and the presence and severity of acute coronary syndrome in young adults≤ 35 years of age. BMC Cardiovascular Disorders 21 (2021): 1-0.
- Ranjith R, Devika P. Clinical correlation between plasma homocysteine level and coronary artery disease in Indian patients. World Journal of Cardiovascular Diseases 26 (2017): 477.
- Bozkurt E, Keles S, Acikel M, Islek M, Atesal S. Plasma homocysteine level and the angiographic extent of coronary artery disease. Angiology 55 (2004): 265-70.
- Islam KN, Chowdhury AW, Khandaker AH, Sabah KM, Amin MG, Kabir SR, Saleh MA. Comparison of Different Risk Factors and Coronary Angiographic Profile in Younger and Older Patients with Ischeamic Heart Disease. Cardiovascular Journal 8 (2015): 23-9.
- Liu Y, Tian T, Zhang H, Gao L, Zhou X. The effect of homocysteine-lowering therapy with folic acid on flow-mediated vasodilation in patients with coronary artery disease: a meta-analysis of randomized controlled trials. Atherosclerosis 235 (2014): 31-5.
- Ibrahim MM, Ibrahim A, Shaheen K, Nour MA. Lipid profile in Egyptian patients with coronary artery disease. The Egyptian Heart Journal 65 (2013): 79-85.
- Khan AR, Majumder AA. Study of lipid profile and coronary angiographic pattern in young Bangladeshi patients with acute coronary syndrome. Cardiovascular Journal 1 (2009): 183-8.
- Obaya M, Yehia M, Hamed L, Fattah AA. Comparative study between elderly and younger patients with acute coronary syndrome. The Egyptian Journal of Critical Care Medicine 3 (2015): 69-75.
- Van Minh H, Binh HA, Bao TQ, Hai NT, Nam LX, Anh TD. Age related differences in acute coronary syndrome: An observation at a central hospital in Vietnam. Journal of Translational Internal Medicine 9 (2021): 32-7.


 Impact Factor: * 5.8
Impact Factor: * 5.8 Acceptance Rate: 71.20%
Acceptance Rate: 71.20%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 