Adverse Reactions to mRNA COVID-19 Vaccines and Studies of the Mechanisms Involved
María Teresa Audicana*, 1, María Inmaculada Muro2, María Natividad Longo1, Ana Martinez-Arcediano1, Paula Ollo Morales1, Eduardo Fernández Ibañez1
1Allergy and Immunology Department, Hospital Universitario Araba (HUA), BIOARABA Vitoria Basque Country, Spain
2Occupational Health Department, Hospital Universitario Araba (HUA), BIOARABA Vitoria Basque Country, Spain
*Corresponding author: María Teresa Audicana, Allergy and Immunology Department, Hospital Universitario Araba (HUA), BIOARABA Vitoria Basque Country, Spain.
Received: 30 August 2022; Accepted: 06 September 2022; Published: 18 October 2022
Article Information
Citation: María Teresa Audicana, María Inmaculada Muro, María Natividad Longo, Ana Martinez-Arcediano, Paula Ollo Morales, Eduardo Fernández Ibañez. Adverse Reactions to mRNA COVID-19 Vaccines and Studies of the Mechanisms Involved. Archives of Microbiology and Immunology 6 (2022): 221-230.
View / Download Pdf Share at FacebookAbstract
Objective Characterize the immunologic mechanisms underlying allergic reactions to mRNA COVID-19 vaccines.
Material and Methods A total of 85 adverse reactions induced by mRNA COVID-19 vaccines were recorded and graded in severe, moderate and mild/atypical cases. Skin prick tests and intradermal tests were conducted to authorized vaccines, polyethylene glycol (PEG), polysorbate 80 (P80), and trometamol. Total and specific IgE to ethylene oxide (EO) were obtained. Basophil activation test (BAT) to vaccines and PEG were also conducted.
Results Positive results were obtained mainly among moderate/severe patients, and also in 2 atypical cases. Both P80 and Trometamol were negative in all the cases studied. PEG was positive in 3 cases. Among 83out of 85 cases tested cases with vaccines, 11 were positive by intradermal tests and, no case was positive by prick tests. Among the 15 selected patients with positive skin tests and/or severe symptoms, 9 of them presented positive results in BAT.
Conclusions and Relevance Among mild and atypical cases, those with negative skin tests tolerated vaccines with premedication. Women and people with a history of adverse drug reactions appear to be at increased risk of ADRs and allergy to the mRNA vaccine. The most serious cases, however, have been recorded in the only two men in the series. Allergy to PEG has only been confirmed in 3% of the adverse reactions and less than 1 per 100,000 vaccines administered. Immunological tests results suggest different induction mechanisms are involved.
Keywords
<p>mRNA vaccines, PEG, polyethylene glycol, COVID-19, SARS-CoV-2, Basophile Activation Tests, BAT, adverse reactions, allergy, Skin tests</p>
Article Details
Abbreviations:
ADR: adverse reactions to drugs, Astra-Zeneca: DNA & Viral vector vaccine Vaxzevria (before COVID-19 Vaccine AstraZeneca ChAdOx1-S), BAT: basophil activation test, COVID-19: Coronavirus disease 2019, EO: specific IgE to ethylene oxide, IgE: Immunoglobulin E, ID: intradermal test, Janssen: DNA & Viral vector vaccine (JNJ-78436735, Janssen Pharmaceuticals Companies of Johnson & Johnson), LNPs: Lipid nanoparticles, Moderna: Spikevax (formerly COVID-19 Vaccine Moderna m-RNA1273), mRNA: Messenger- ribonucleic acid, OSI ARABA: Organization Sanitaria Integrada ARABA (in spanish) Integrated Health Organization ARABA ( a region of the Basque Country), PEG: Polyethylene glycol or macrogol, Pfizer: Comirnaty (formerly COVID-19 Vaccine Pfizer /BioNTech BNT162B2), P80: polysorbate 80, Tween 80, polyoxyethylene sorbitan monooleate, SARS-CoV-2: Severe Acute Respiratory Syndrome Coronavirus-2, SEAIC: Spanish Society of Allergy and Clinical Immunology , SDRIFE: symmetric intertriginous and flexural drug-related exanthema, SI: stimulation index, SPT: Skin prick test
1. Introduction
Vaccines based on messenger RNA and PEG are the first to be used and the Drug Agencies recommend close surveillance to detect and evaluate possible new adverse reactions not identified during clinical trials of vaccines against COVID-19 [1,2]. Adverse reactions to these vaccines are difficult to classify using the traditional Gell and Coombs classification because differ from most “traditional” vaccines and their metabolism, mode of action and immunogenicity are unlike other drugs and adverse reactions might also differ [3].
In Spain, from the start of the vaccination campaign until December 2021, 71% of the administered doses corresponded to Pfizer (Comirnaty. Pfizer /BioNTech BNT162B2), 13% to Astra-Zeneca (Vaxzevria, before COVID-19 Vaccine AstraZeneca ChAdOx1-S), 13% to Moderna (Spikevax formerly COVID-19 Vaccine Moderna m-RNA1273) and 3% to Janssen (COVID-19 Vaccine Janssen. Johnson & Johnson JNJ-78436735) Following the decision of the British health authorities to discourage immunization using the Pfizer vaccine against COVID-19 in patients with a history of serious reactions to drugs and / or foods, the Spanish Society of Allergy and Clinical Immunology (SEAIC) issued information in this regard [1,2,4]. Initially, the cause of the allergic reactions was attributed to an excipient of the COVID vaccine named polyethylene glycol, PEG or macrogol. PEG is a substance present in great quantities in some medications, such as laxatives, PEGylated drugs and ultrasound contrasts [5]. However, PEG can also be present in other drugs as excipients such as antibiotics, analgesics, antiacids, corticosteroids and antihypertensive drugs [6]. It is surprising that allergic reactions to this substance are extremely rare, even though it is present in everyday products [7]. Reports of anaphylactic reactions to PEG with cross-reactivity to polysorbate 80 (P80) or Tween 80 are even more anecdotal [8].
As is known, both Pfizer and Moderna vaccines contain PEG, however, live attenuated viruses’ vaccines contain P80 or Tween 80. Polysorbates are increasingly present in drugs including parenteral corticosteroids, monoclonal antibodies, other vaccines (human papillomavirus and influenza), vitamin preparations, erythropoietin and Factor VIII among others [6]. In addition, the Moderna vaccine contains trometamol, which is used in some drugs as an alkalizer. Trometamol is present in other vaccines (meningococcus, hexavalent DTT), some eye drops, anti-inflammatory drugs, fosfomycin and some contrasts of both iodine and gadolinium. So far, allergy to trometamol has only been described in one case in relation to the administration of gadolinium contrast [9]. Trometamol is also currently present in the composition of Pfizer's pediatric vaccines, but it should be noted that the latter did not exist at the time of this study. For the purpose of this review, we will refer to the classification recently proposed by the European Academy of Allergy and Clinical Immunology (EAACI) that includes the new knowledge on phenotypes, endotypes and biomarkers, but also uses classic criteria (Gell and Coombs). This classification divides the hypersensitivity reactions (HSRs) into immediate and delayed reactions. Immediate hypersensitivity reactions (IHSRs) include cytokine release reactions (CRRs), type I reactions, both IgE and non-IgE mediated, infusion-related reactions (IRRs), and mixed reactions [3]. The literature lacks a standardized diagnostic management protocol for patients suspected of hypersensitivity to mRNA vaccines. Since February 2021, the SEAIC has promoted a joint study protocol for the routinely tested patients with adverse reactions using a standardized panel of confirmatory tests [10]. This study protocol has been approved by the Ethics Committee of the Basque Country.
The present study provides clinical data, including skin test, IgE determination and BAT tests for a case series of adverse reactions to m-RNA COVID-19 vaccines within a regional surveillance system that was one of the first to Spain to suffer this pandemic infection. Vitoria, as the capital city of the Integrated Health Organization (OSI) ARABA region, has been considered one of the first gateway for SARS-CoV-2 in Spain [11].
2. Materials and Methods
This case series included 85 vaccinated patients belongings to the region of OSI ARABA with suspected adverse reactions to mRNA COVID-19 vaccines recovered between December 2020 to October 2021. These patients were identified either by their occupational or primary health care physician, and were referred to the Allergy Department for follow-up allergy testing.
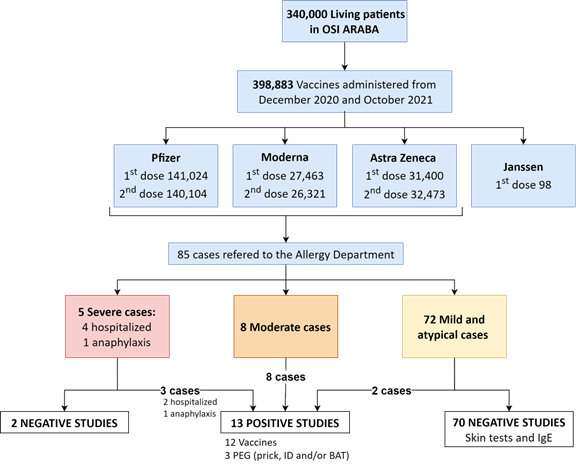
Allergic reactions were graded using standard definitions including the Brighton criteria shown in figure 1. Specifically, the following search criteria were used: any patient who had an adverse reaction within the next 48 hours after receiving at least one dose of a COVID-19 mRNA vaccine.
- Severe: A systemic reaction with an anaphylactic profile or that required hospital admission.
- Moderate: Urticaria, angioedema, isolated dyspnea in the first 3 hours after vaccination.
- Mild and atypical cases: other events that happened in the following 48 hours after vaccination.
Allergic reactions were defined as the appearance of symptoms starting within the next 3 hours after vaccination including hives; perioral, periocular, or throat swelling; shortness of breath, wheezing, or chest tightness; changes of blood pressure or loss of consciousness.
Other adverse reactions registered in the next 48 hours after vaccination were: pruritus, urticaria or isolated angioedema, exanthema, intense tremor and perioral paresthesia. Intense local reaction affecting more than one joint, painful lymphadenopathy and other events at the discretion of their responsible physicians were also considered. All participants were invited to perform skin tests, specific IgE and basophil activation test (BAT) after signing a consent for this allergy study. The time interval between the vaccine reaction and the evaluation by the allergy department was between 2 and 6 weeks after the hypersensitivity reaction for both in vivo and in vitro tests. Skin prick tests (SPT) and intradermal tests were conducted to vaccines authorized in Spain during the recruitment period, more specifically: Pfizer, Moderna, Astra-Zeneca and Janssen.
2.1 Skin prick test (SPT)
Single-lancet technique was performed with sterile ALK-Abello lancets, Denmark. Histamine (1 mg/ml) and filtered saline (negative control) were used for internal validation. A wheal size of 3 mm or greater was considered positive. Vaccines’ remnants, kindly supplied by our Occupational Health Department, were used according to the manufacturer’s concentration instructions. In addition, PEG, P80 and trometamol were included as excipients contained in the vaccines, according to a standardized panel designed by SEAIC [8]. Given the impossibility of obtaining pharmaceutical grade PEG 2000 for the study, PEG 1500 at 0.1 mg/ml, 1 mg/ml and 10 mg/ml (Roxall Medicina España SA) and PEG 3350 (Movicol®) and 4000 (Casenlax®) were used diluting the commercial preparations to concentrations at 55 and 50 mg/ml respectively. P80 was tested at concentration of 0.04 mg/ml and Trometamol at 1 mg/ml [9].
2.2 Intradermal test (ID)
Once the negative result of the SPTs was confirmed, intradermal tests were performed, previously ensuring, as a precaution against severe reactions, a venous access. The intradermal tests were carried out at 1:100 dilution of remnant vaccines considering a non-irritating concentration [12]. Due to the risk of systemic reactions described with PEG intradermal tests, only in some cases of young patients without comorbidities, an intradermal skin test was performed with PEG 1500 at 0.01 mg/ml (Roxall Medicina España SA). It is described in table 1. P80 and trometamol were tested at 0.04 mg/ml and 0.1 mg/ml respectively by intradermal tests in all cases [8].
2.3 In vitro test: IgE and BAT
Total immunoglobulin E (IgE) and ethylene oxide (EO)-specific IgE concentrations were performed according to ImmunoCAP Total and specific IgE (Thermo Fisher Scientific) instructions. Basophil activation test (BAT) to vaccines, PEG 1500, PEG 2000 and P80 were also conducted. Whole blood preserved in heparin was collected from participants. Briefly, one hundred microliters of heparinized whole blood were aliquoted per test. Basophil activation was assessed after stimulation with either PEG 1500 (0.2, 0.04 and 0.001 mg/ml), PEG 2000 (0.2, 0.04 and 0.001 mg/ml), both kindly donated by Roxall; or P80 (1/10,000 and 1/50,000) (Millipore Sigma–Sigma Aldrich). Buffer with fMLP or anti-IgE antibody (Sigma-Aldrich, St. Louis, Missouri, USA) was used as a positive control.
Vaccine-discarded remnant materials were used and the final stimulation concentration were: Pfizer at 2.5 and 0.5 μg/ml; Moderna at 2.5 and 0.5 μg/ml; AstraZeneca at 1/40 and 1/200; Janssen at 1/40 and 1/200. Twenty microliters of stimulation buffer were added as a negative control and 20 µL of stimulation buffer with fMLP or anti-IgE antibody (Sigma-Aldrich, St. Louis, Missouri, USA) was used as a positive control. The samples were incubated at 37ºC for 15 minutes in a water bath. After cooling on ice for 5 minutes, basophils were triple-labelled by adding 20 µL of conjugated PE-anti-CD123, PerCP-anti-HLA-DR, and FITC-anti-CD-63 (FastImmune, BD Biosciences, San Jose, California, USA) to each tube. After 20 minutes of incubation at 4ºC, red blood cells were lysed (FACS lysing solution, BD Biosciences) for 10 minutes at room temperature. After centrifugation, 2 ml of washing solution was added and a new centrifugation was performed. After centrifugation, 200 µl of washing solution was added to the cell pellets. Lastly, cytofluorometric analysis of CD63+ cells on at least 200 CD123+DR– cells were performed (FACsCalibur, Becton-Dickinson).
Basophils activation was expressed as stimulation index (SI) that was calculated as the ratio between the percentage of activated basophils in samples stimulated with either PEG or the vaccines and in the unstimulated samples. BAT was performed in all patients with severe and moderate symptoms. Among the mild and atypical cases, forty participants also consented to perform the same full protocol and BAT trials were performed. More than 10 controls were performed among patients not affected by COVID infection and without adverse reactions to COVID vaccines.
3. Results
During the aforementioned period, almost 400,000 doses of COVID-19 vaccines were administered. Among the vaccines used in our region, the Pfizer vaccine has been the most administered. Far behind are the other three marketed vaccines [Figure 1].
Table 1: Characteristics, grade of severity and demographics of patients who developed ADR induced by COVID-19 mRNA vaccines.
* Hospitalized after skin tests (tremor+anaphylaxis)
** D-dimer elevation confirmed
*** Intradermal positive at 6 hours
Out of the 85 patients studied, 13 (15%), 11 women and 2 men, who ranged in age from 26 to 89 years with a mean (SD) age of 52 years, presented moderate/severe adverse reactions. A total of 72 (85%) mild and atypical reactions were also collected. Positive results were obtained in thirteen patients, 3 from severe cases, 8 from moderate ones and 2 from mild/atypical ones. Adverse reactions to drugs (ADR) were present in the previous history of 7 of the 13 positive cases (53%). Among the negative cases, only 19 out of 70 (27%) had a history of allergy to drugs [Figure 1]. Among the positive cases, a medical history of ADR was documented, specifically opioids and non-steroidal anti-inflammatory drugs. Of the 5 patients with mRNA vaccine-allergic reactions coded as severe cases, 3 were anaphylaxis, all of them received epinephrine and one of them (an 89 years old man) was admitted in the hospital [Table 1]. The fourth and fifth severe cases were two women over 65 years of age in whom D-dimer elevations were detected in the setting of extensive skin disease (4,000 ng/ml and 17,700 ng/ml respectively) without detecting other organic pathology. Case number 12 corresponds to a symmetric intertriginous and flexural drug-related exanthema (SDRIFE). Finally, number 15 was admitted for a multisystem condition consisting of angioedema associated with headache and chest tightness. All reactions fully resolved but patient number 1 required two new admissions for recurrent angioedema and patient number 12 required a subsequent admission for pulmonary embolism (PE).
The moderate cases were characterized by urticaria and/or angioedema (4 cases), severe itching, and tachycardia. Tremor and paresthesia are unusual symptoms of adverse reactions to vaccines, but nevertheless, both were registered on some occasions (case 6 and 14, see Table 1). After performing skin tests with the vaccines, some cases developed tremor (case 5). This patient required hospital admission due to tremor and a systemic reaction during intradermal testing with vaccines and PEG. Seventy-two mild and atypical cases were registered, among which the majority (44%) consulted due to late-onset urticaria/angioedema and pruritus (16 respectively). In addition, other adverse reactions were described: 13 rashes, 10 intense local reactions, and remaining presented dysphagia, dyspnea, paresthesia, vertigo, vomiting, mastitis and a psoriasiform reaction. Among the 72 mild and atypical cases, 24 (33%) had a physician-documented history of previous allergic reactions. Nineteen patients (26%) had a history of ADR especially in relation to beta-lactams and nonsteroidal anti-inflammatory drugs followed by opioids, corticosteroids and contrast media. Five patients (7%) had a history of food allergy (LTP-syndrome, kiwi and nuts).
Positive results were obtained in thirteen patients, three from severe cases (3/5), 8 from moderate ones (8/8) and 2 from mild/atypical ones (2/72). Table 1 shows the moderate/severe cases grouped together with the positive ones.
Regarding the prick tests results, P80, Trometamol, PEG-1500 and vaccines were negative in all the cases studied. Only 2 cases of positive skin prick tests were obtained, both to 3350 PEG (Movicol®). Table 1 shows these cases (7 and 14), with moderate reactions induced by Moderna and Pfizer and both associated to a positive result to vaccines by BAT. Only three positive test were obtained to PEG (2 prick test and 1 intradermal test). Another one showed positive result for EO -IgE. Among 83 out of 85 cases tested with vaccines, 11 were positive by intradermal tests and, no case was positive by prick tests. Differences were observed regarding positive intradermal tests obtained to the vaccines used according to the severity classification, taking into account that both 1 severe and 1 moderate case were not tested by intradermal test. Positive ID tests were obtained in most moderate cases tested (7/7), while the same did not occur in severe (3/4) and mild/atypical cases (2/72). Intradermal PEG 1500 was positive in one case induced by Moderna vaccine (case 8) and positive tests were confirmed in ID and BAT with the vaccine itself as well. All reactions fully resolved, but 4 of them required hospital admission: 3 during their reaction after the vaccine and the fourth (the case number 5) required admission after intradermal tests.
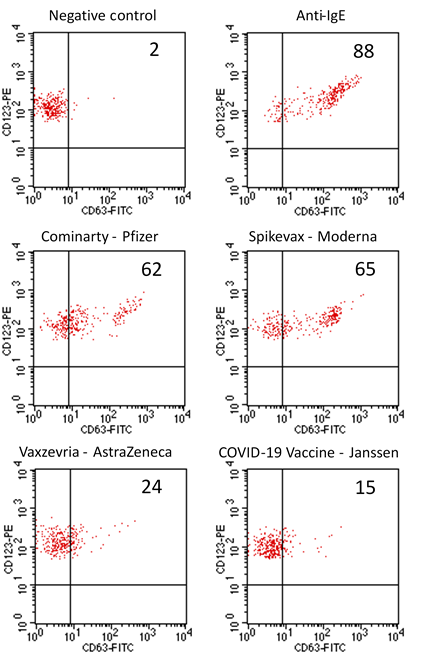
Among the studied patients, 9 out of 15 had a positive BAT test result to the administered vaccines, all of them with positive results by ID tests. In 2 of the 9 positive BAT cases to vaccines, PEG positivity was also obtained. In Figure 2, an example BAT assay is shown. Skin tests were negative at the same concentrations in more than 100 patients with suspected adverse reactions to vaccines or other drugs containing PEG. All negative patients were encouraged to receive the second dose and did not have a recurrent reaction. More than 50 BAT were also performed in some mild cases and controls with negative results to PEG and vaccines. Nine non-responder patients (9/50) and 4 patients with discordant results were observed. Among the latter, two of them had previous COVID infection and 2 finally tolerated a new dose of the vaccine. Among the 15 cases studied in detail (see table 1), eight positive BAT results were obtained with vaccines (53 %) and the values of the stimulation index (SI) were between 2 and 15. Among the BAT positive with vaccines, two cases with additional positivity to PEG were observed.
4. Discussion
To date, severe allergic reactions have been reported with the two mRNA vaccines, produced by Pfizer and Moderna, and much less frequently after the viral vector vaccines [13-15]. For patients who have had such reactions to a COVID-19 vaccine, the Drug Agencies and Allergy Committees recommend an evaluation by an allergist prior to the administration of additional doses [1, 2, 10, 16]. According our data, 3 moderate to severe reactions occur per 100,000 vaccines administered. Women and people with a history of adverse drug reactions appear to be at higher risk of moderate/severe ADRs to the mRNA vaccines. The most serious cases, however, have been registered in two men, one of them with a positive study and the other one with a negative study. Other anaphylaxis series revealed an increased severity in male versus female patients [17]. Most severe reactions have been reported with Moderna vaccines (3/5), however, the most widely used vaccine has been Pfizer (5 times more than Moderna and Astra Zeneca) in our area.
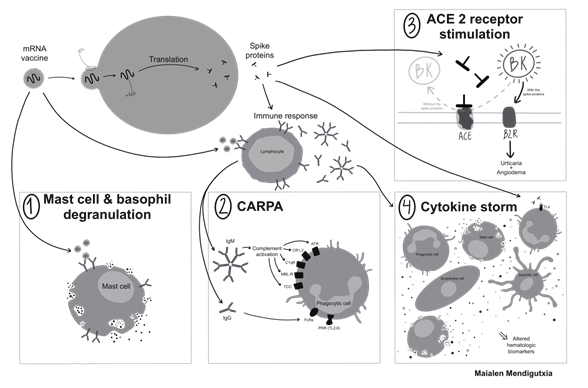
Tremor and paresthesias are unusual symptoms of adverse vaccine reactions, and may be explained by confirmation that purified SARS-CoV-2 spike proteins can cross the blood brain barrier (BBB) [18]. The mechanism of the adverse and allergic/anaphylactic reactions to COVID-19 vaccines has yet to be confirmed, and are attributed to certain excipients such as PEG, PEG conjugated substances, P80 and trometamol [19]. Although tests were carried out with all the substances described above, only three of the 85 cases (about 3% or adverse reactions and less than 1 per 100,000 vaccines administered) have been directly related to PEG. Positive results were mostly obtained with vaccines but not with PEG or other excipients. These results are consistent with recent works that suggest that most of the adverse reactions that occur with mRNA vaccines are produced by mechanisms other than those mediated by IgE to PEG [20]. There are at least 4 possible mechanisms involved in the observed reactions [Figure 3].
4. 1 IgE-mediated allergy to excipients
Positive tests have mostly been demonstrated with the ID test with vaccines and not with PEG. It is possible that the three-dimensional structure or the Lipid nanoparticles (LNPs), the terminal fractions and/or the chemical nature of PEG-acceptor core structure influences the allergenicity of PEG. This hypothesis would explain the findings of recent studies that show that patients previously diagnosed with allergy to PEG-asparaginase, tolerated Pfizer vaccination without adverse event [21,22]. Regarding the BAT, it is striking to obtain a positivity greater than 50% among the 15 cases studied in detail in contrast to negative patients and control group [Figure 1]. Furthermore, the SI correlates in higher values with the vaccine involved in the reaction in most positive cases.
4.2 Complement activation-related pseudo allergy (CARPA)
Another mechanism proposed as a possible cause of apparent mast cell-mediated reactions to PEG in mRNA COVID-19 vaccines is CARPA, where pre-existing IgG or IgM antibody to PEG would activate complement, generating anaphylatoxins (C3a, C4a and C5a), causing mast cell degranulation [23]. In a report of 22 patients with suspected allergic reactions to mRNA COVID-19 vaccines, evaluations for possible IgE-mediated anaphylaxis and for CARPA were performed. The authors concluded that the reactions are likely due to IgG anti-PEG-induced CARPA but acknowledge that additional studies are needed [20]. Testing the reactogenicity of the liposomes (without the drug) during the period of seroconversion in the case of pigs treated with liposome-encapsulated doxorubicin, led to fatal anaphylaxis within 2–3 min only in immunized animals [24]. In the case of mass vaccination used during the pandemic period in OSI-ARABA, the scenario is similar and case number 1 could be explained because he received 2 doses of vaccine a few weeks after coronavirus infection.
4.3 Phenomena associated with ACE 2 receptor stimulation
After administrating the vaccine in the deltoid muscle, it was observed that the spike protein S1 subunit was detectable in the systemic circulation up to approximately two weeks post-immunization in eleven out of thirteen healthcare workers [25]. This interaction may trigger thrombosis, and other adverse inflammatory reactions including activating the kallykrein-bradikinin system [26]. This mechanism could explain most of mild and non-immediate cases of urticaria and angioedema in a similar way to the mechanism involved in angiotensin-converting enzyme inhibitor-induced cases.
4.4 Antibody-dependent enhancement (ADE) and /or Cytokine storm
While no single definition of cytokine storm is widely accepted, three features of cytokine storms are commonly shared: elevated levels of cytokines, acute systemic inflammatory symptoms, and either secondary organ dysfunction or any cytokine-driven organ dysfunction. In very rare cases, antibody-dependent enhancement (ADE) has been related to vaccines, such as the Respiratory syncytial virus (RSV) vaccine in the 1960s and the Dengue vaccine in 2016, due to Dengue's four strains. Marked elevations in hematologic biomarkers such as D-dimer, ferritin, and C-reactive protein are associated with poor outcomes of COVID infection, and spike protein S1 subunit is able to induce pro-inflammatory responses via toll-like receptor 4 signaling in human macrophages [27]. We confirmed that the COVID vaccine may induce D-dimer elevation in two of our severe patients. This syndrome has been acknowledged vaccine-induced immune thrombotic thrombocytopenia (VITT) and confirmed with Astra Zeneca vaccine [28]. Many of the individuals who experienced possible adverse reactions to the mRNA vaccines had a history of allergy to a variety of other allergens, especially adverse drug reactions. These findings warn about the management of patients with suspected allergy with the first administration of the vaccine. The possibility that some adverse reactions are induced by different mechanisms should be taken into account. The present study provides clinical data, including skin prick and identification tests, IgE determination, and BAT tests for a case series of adverse reactions to COVID-19 mRNA vaccines within a regional surveillance system that comprehensively recorded ADRs.
5. Conclusions and Relevance
One of the most interesting benefits of this study is the large number of negative studies obtained that allowed the use of a subsequent dose of vaccine in most of the patients studied. A drug provocation test (DPT) consists in re-administering, in a controlled setting under strict medical supervision, the vaccine suspected to have induced an HSR. The purpose of carrying them out is to de-label individuals with false allergy diagnosis, avoid unnecessary desensitization procedures, and identify the culprit drug in reactions with more than one drug involved. Recent publications proposed a decision algorithm for DPT based on reaction severity. However, other parameters should be considered to perform an accurate risk-assessment. A life threatening reaction, a tryptase increase during the acute phase, and positive ST and BAT would suggest a high risk of reaction during a DPT. Indeed, women are high risk individual. Finally, an adequate setting, with all the technical resources and enough human power, is mandatory to perform a DPT, that is always a high-risk procedure. The underlying mechanisms of reactions are not fully understood and the severity of these reactions is heterogeneous, from local reactions in the injection site to severe systemic. Some of these reactions are potentially dangerous and generally the avoidance of the vaccines is recommended. Local reactions should be followed up to prevent the development of more severe episodes, because currently there are no progression biomarkers.
According to this series of cases, 3 moderate to severe reactions occur per 100,000 vaccines administered. Women and people with a history of adverse drug reactions appear to be at higher risk of these moderate/severe ADRs. The most serious cases, however, have been recorded in two men (0.5 per 100,000 vaccinations). Despite the majority use of Pfizer vaccines in our environment, the majority of moderate and severe adverse reactions have been recorded regarding the administration of Moderna vaccines. The most profitable diagnostic method has been the intradermal test with the vaccines along with BAT. It is noteworthy that the initial suspicion of ADR etiology to these vaccines was PEG, and yet positivity has been shown mostly with the vaccines themselves. Allergy to PEG has only been confirmed in 3 of the 85 cases referred. This ratio represents 3% of the adverse reactions and less than 1 per 100,000 vaccines administered.
According to these described findings, different RAM mechanisms are proposed in the discussion of this paper. Currently, there are probably more questions than answers in the field of the HSR related with mAb. How is the kinetics of cytokines in CRRs? Are there different patterns for distinct types of CRRs? Can different types of vaccines induce different cytokine release patterns? What does a positive skin test to a vaccines really reflect? Can BAT aid in the diagnostic of vaccines HSR? Could BAT identify non-IgE type I reactions? What role does IgG ADA play in HSR? Could those really be a predictive marker for HSR? Should they be included as a routine test in subjects in long-term treatments? Could repeated administration of vaccine in the form of DS really desensitize the patient and induce a natural tolerance? Could BAT predict a potential reaction prior to each DS?
Conflict of Interest
All authors declare that they have no conflict of interest in the preparation of this paper.
Funding Source
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Acknowledgements
Amaia Longo in the review of the English language and Maialen Mendiguchia in the design of the images.
References
- Ortega Rodríguez NR, Audicana Berasategui MT, de la Hoz Caballer B, Valero Santiago A. The century of mRNA vaccines: COVID-19 vaccines and allergy. J Investig Allergol Clin Immunol 31 (2021): 89-91.
- Sokolowska M, Eiwegger T, Ollert M, Torres MJ, Barber D, Del Giacco S, et al. EAACI statement on the diagnosis, management and prevention of severe allergic reactions to COVID-19 vaccines Allergy 76 (2021): 1629-39.
- Bavbek S, Pagani M, Alvarez-Cuesta E, Castells M, Dursun AB, Hamadi S, et al. Hypersensitivity reactions to biologicals: An EAACI position paper. Allergy Eur J Allergy Clin Immunol 77 (2021): 39–54.
- Mahase E. Covid-19: People with history of significant allergic reactions should not receive Pfizer vaccine, says regulator. BMJ 10 (2020): m4780.
- Wenande E, Garvey LH. Immediate-type hypersensitivity to polyethylene glycols: a review. Clin Exp Allergy 46 (2016): 907-22.
- Caballero ML, Krantz MS, Quirce S, Phillips EJ, Stone CA. Hidden Dangers: Recognizing Excipients as Potential Causes of Drug and Vaccine Hypersensitivity Reactions. J Allergy Clin Immunol Pract 9 (2021): 2968-82.
- Sellaturay P, Nasser S, Ewan P. Polyethylene glycol-induced systemic allergic reactions (anaphylaxis). J Allergy Clin Immunol Pract 9 (2021): 670-5.
- Palacios Castaño MI, Venturini Díaz M, Lobera Labairu T, González Mahave I, Del Pozo Gil MD, Blasco Sarramián A. Anaphylaxis Due to the Excipient Polysorbate 80. J Investig Allergol Clin Immunol 26 (2016): 394-6.
- Lukawska J, Mandaliya D, Chan AWE, Foggitt A, Bidder T, Harvey J, et al. Anaphylaxis to trometamol excipient in gadolinium-based contrast agents for clinical imaging. J Allergy Clin Immunol Pract 7 (2019): 1086-7.
- Greenhawt M, Abrams EM, Shaker M, Chu DK, Khan D, Akin C, et al. The Risk of Allergic Reaction to SARS-CoV-2 Vaccines and Recommended Evaluation and Management: A Systematic Review, Meta-Analysis, GRADE Assessment, and International Consensus Approach. J Allergy Clin Immunol Pract 9 (2021): 3546-67.
- Gómez-Carballa A, Bello X, Pardo-Seco J, Pérez Del Molino ML, Martinón-Torres F, Salas A. Phylogeography of SARS-CoV-2 pandemic in Spain: a story of multiple introductions, micro-geographic stratification, founder effects, and super-spreaders Zool Res 41 (2020): 605-20.
- Wood RA, Setse R, Halsey N. Irritant skin test reactions to common vaccines. J Allergy Clin Immunol 120 (2007): 478-81.
- CDC COVID-19 Response Team, Food and Drug Administration. Allergic Reactions Including Anaphylaxis after Receipt of the First Dose of Pfizer-BioNTech COVID-19 Vaccine - United States, December 14-23, 2020 MMWR Morb Mortal Wkly Rep 70 (2021): 46-51
- Shay DK, Gee J, Su JR, Myers TR, Marquez P, Liu R, et al. Safety Monitoring of the Janssen (Johnson & Johnson) COVID-19 Vaccine - United States, March-April 2021. MMWR Morb Mortal Wkly Rep 70 (2021): 680-4.
- CDC COVID-19 Response Team, Food and Drug Administration. Allergic Reactions Including Anaphylaxis After Receipt of the First Dose of Moderna COVID-19 Vaccine - United States, December 21, 2020-January 10, 2021. MMWR Morb Mortal Wkly Rep 70 (2021): 125-9.
- COVID-19: Allergic reactions to SARS-CoV-2 vaccines Up To Date (2022).
- Reber LL, Hernandez JD, Galli SJ. The pathophysiology of anaphylaxis. J Allergy Clin Immunol 140 (2017): 335-48.
- Buzhdygan TP, DeOre BJ, Bawdwin-Leclair A, Bullock TA, McGary HM, Khan JA, et al. The SARS-CoV-2 spike protein alters barrier function in 2D static and 3D microfluidic in-vitro models of the human blood–brain barrier. Neurobiol Dis 146 (2020): 105131.
- Cabanillas B, Novak N, Akdis C. The form of PEG matters: PEG conjugated with lipids and not PEG alone could be the specific form involved in allergic reactions to COVID-9 vaccines Allergy (2021).
- Warren CM, Snow TT, Lee AS, Shah MM, Heider A, Blomkalns A, et al. Assessment of Allergic and Anaphylactic Reactions to mRNA COVID-19 Vaccines With Confirmatory Testing in a US Regional Health System. JAMA Netw Open 4 (2021): e2125524.
- Mark C, Gupta S, Punnett A, Upton J, Orkin J, Atkinson A, et al. Safety of administration of BNT162b2 mRNA (Pfizer-BioNTech) COVID-19 vaccine in youths and young adults with a history of acute lymphoblastic leukemia and allergy to PEG-asparaginase. Pediatr Blood Cancer 68 (2021): e29295.
- Koo G, Anvari S, Friedman DL, Zarnegar-Lumley S, Szafron V, Kahwash BM, et al. mRNA COVID-19 vaccine safety in patients with previous immediate hypersensitivity to pegaspargase. J Allergy Clin Immunol Pract 10 (2022): 322-5.
- Klimek L, Novak N, Cabanillas B, Jutel M, Bousquet J, Akdis CA, et al. Allergenic components of the mRNA-1273 vaccine for COVID-19: Possible involvement of polyethylene glycol and IgG-mediated complement activation Allergy 76 (2021): 3307-13.
- Kozma GT, Shimizu T, Ishida T, Szebeni J. Anti-PEG antibodies: Properties, formation, testing and role in adverse immune reactions to PEGylated nano-biopharmaceuticals. Adv Drug Deliv Rev 154 (2020): 163-175.
- Verdecchia P, Cavallini C, Spanevello A, Angeli F. The pivotal link between ACE2 deficiency and SARS-CoV-2 infection. Eur J Intern Med 76 (2020): 14-20.
- Ogata AF, Cheng C, Desjardins M, Senussi Y, Sherman AC, Powell M, et al. Circulating SARS-CoV-2 Vaccine Antigen Detected in the Plasma of mRNA-1273 Vaccine Recipients. Clin Infect Dis 74 (2022): 715-8.
- Shirato K, Kizaki T. SARS-CoV-2 spike protein S1 subunit induces pro-inflammatory responses via toll-like receptor 4 signaling in murine and human macrophages. Heliyon 7 (2021): e06187.
- Chan B, Odutayo A, Jüni P, Stall NM, Bobos P, Brown AD, et al. Risk of Vaccine-Induced Thrombotic Thrombocytopenia (VITT) following the AstraZeneca/COVISHIELD Adenovirus Vector COVID-19 Vaccines. Science Briefs of the Ontario COVID-19 Science Advisory Table 2 (2021).


 Impact Factor: * 3.5
Impact Factor: * 3.5 Acceptance Rate: 71.36%
Acceptance Rate: 71.36%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
