Knowledge and Attitude Regarding HIV/AIDS and Universal Testing and Treatment Strategy in some Selected Communities in Fako Health Districts of Cameroon
Kah Emmanuel Nji1,*, Dickson Shey Nsagha1, Vincent Verla Siysi2, Eno orock GE3, Ngowe Ngowe Marcelin4
1Department of Public Health and Hygiene, University of Buea, Cameroon
2Department of Internal Medicine and Pediatrics, Faculty of Health Sciences, University of Buea, Cameroon
3 Bafoussam Regional Hospital, West Region, Cameroon
4University of Douala BP 2701 -Cameroon
*Corresponding Author: Kah Emmanuel Nji, Department of Public Health and Hygiene, Faculty of Health Sciences, University of Buea, P.O. Box 63 - Buea, Cameroon
Received: 31 July 2020; Accepted: 06 August 2020; Published: 13 August 2020
Article Information
Citation: Kah Emmanuel Nji, Dickson Shey Nsagha, Vincent Verla Siysi, Eno orock GE, Ngowe Ngowe Marcelin. Knowledge and Attitude Regarding HIV/AIDS and Universal Testing and Treatment Strategy in some Selected Communities in Fako Health Districts of Cameroon. Journal of Environmental Science and Public Health 4 (2020): 197-215.
View / Download Pdf Share at FacebookAbstract
Background: HIV/AIDS has emerged as a serious public health threat across the world, especially in developing countries. To attain the 90-90-90 targets and bring the pandemic under control by 2030, Comprehensive knowledge and positive attitudes are cornerstones for the prevention, control, and treatment of HIV/AIDS.
Objective: The objective of this study was to access the knowledge and attitude level of participants towards HIV/AIDS and Universal testing and treatment strategy Fako health districts, Cameroon.
Methods: This was a community based cross sectional study with a sample size of 1501 participants who were randomly selected within 8 communities. Data were collected electronically with android phones/Tablets by researcher through face-face interviews. The questionnaires had 15 items in 2 dimensions, Knowledge and altitude regarding HIV/AIDS and Universal testing and treatment strategy. Data were analyzed using descriptive statistics and logistic regression model.
Results: The mean age of the participants was 29 years, Majority (58.8%) of the participants were males while 797 (53.1%) of the participants had secondary education level. Also, Christians constituted 96.7% of the study population. Only 599 (39.9%) had heard of University test and treatment of HIV/AIDS and among which only 67(12.6%) knew what this means. Overall, 940(62.6%) had correct knowledge on HIV/AIDS and Universal testing and treatment strategy. Those with overall positive attitude towards HIV/AIDS and Universal testing and treatment strategy constituted 1140 (76%) of the study population. Predictors of positive attitudes were: Education level, knowledge level, health districts, Income level and history of having 2 or more sexual partners in the past 12 months. Participants who had tertiary level of education were 6.9 times more likely to have positive attitude towards HIV/AIDS
Keywords
<p>Knowledge; Attitude; HIV/AIDS; Universal testing and treatment approach; Fako health districts</p>
Article Details
Abbreviations
HIV= Human Immunodeficiency Virus
AIDS= Acquired Immunodeficiency Syndrome
UTT= Universal Testing and Treatment
AOR= Adjusted Odd Ratio
COR= Crude Odd Ratio
1. Introduction
Testing for HIV is a gateway to treatment, care and prevention [1]. Awareness to HIV status is usually the primary step that leads to health care seeking behavior in HIV care services [2 ]. This has been advocated in many countries not only as a potential preventive tool but also as a major way to destigmatize and normalize HIV in the entire world [2]. Findings from several studies have revealed that many strategies have been used to increase the uptake of HIV testing and treatment but despite all the strategies in place, testing and treatment of HIV/AIDS remains low [3] . Recent estimates based on survey done in 18 high HIV-prevalence sub-Saharan African countries revealed that only 34% of women and 17% of men had ever been tested for HIV in the general population and have received their results . Another study in south Africa revealed that less than a quarter of 15-49 years old in sub-Saharan Africa know their status [4].
According to the Cameroon Demographic and Health Survey and Multiple Indicators Cluster Surveys (DHS-MICS) conducted by the “National Institute of Statistics” (NIS) in collaboration with the Ministry of Public Health HIV prevalence in Cameroon was 4.3% in 2011[5]. However, following the Cameroon population based HIV impact assessment, the prevalence has dropped from 4.3% in 2011 to 3.7% in 2018. Cameroon still has the highest burden of HIV in West and Central Africa (WCA), with an estimated 620,000 PLHIV, projected to increase to 726,000 by 2020 [6].
In the Fako division of Cameroon, increasing access to HIV testing and treatment has been an essential activity. In recent years, much progress has been made to increase the coverage and uptake of HIV services in many areas through the provision of vertical integrated services; client-initiated testing (voluntary counselling and testing) and provider-initiated HIV counseling and testing (HCT). Despite all the efforts made, the rate of new HIV infections in this division and in Cameroon remain high while the uptake of these services remained generally low [7].
In 2015 the World Health Organization (WHO) issued updated guidelines recommending immediate ART for all HIV-positive individuals, regardless of CD4 count [7] . However, testing everybody and providing treatment to those who test positive was only implemented in Cameroon in 2016. Universal Testing and Treatment (UTT) involves offering HIV testing to everybody that comes to the hospital for consultation and then putting those who test positive on Antiretroviral treatment (ARTs) irrespective of their clinical stage or CD4 count [8] .The rationale behind this strategy is that it Will help more people find out if they are infected with HIV earlier, and that is when treatment work best ,it will also decrease the number of babies born with HIV, reduce morbidity and mortality due to HIV, stigma associated with HIV testing and Will enable those who are infected to take steps to protect the health of their partners and hence break the chain of transmission [9, 10]. However, Mathematical modeling has also shown that UTT could lead to drastic reduction in HIV incidence and possibly eliminate HIV as a public health problem over a period of 15-20 years as well as reduce HIV- related morbidity and mortality [10]. Therefore, for UTT approach to be a successful and produce the desired effect, it is necessary to assess the Knowledge and attitude level of members of the community on HIV/ADS and Universal testing and treatment strategy (UTT).
2. Materials and Methods
2.1 Study design and setting
This was a community based cross sectional study that was conducted in 8 randomly selected communities within Fako health districts. These communities include, Upper kostain and modeka in Tiko health district, Sandpit, and Mile 16 in Buea Health district, Munyenge in Mayuka health district, Batoke, Watutu, and Idenau in Limbe health district (Figure 1).
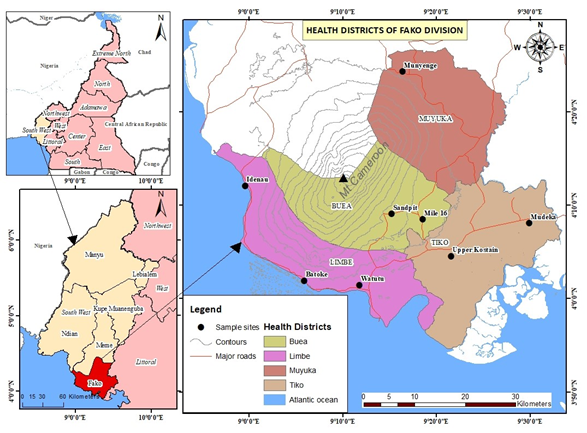
Figure 1: Map showing the study communities.
2.2 Study population
The study population involved members of the selected communities who were of age 18 years and above and who gave their verbal or written consent to participate in the study.
2.2.1 Inclusion and exclusion criteria
Inclusion criteria: Community members who were 18 years and above and accepted to take part in the study verbally or through a written consent were included in the study
Exclusion criteria: Community members who were below the ages of 18 and those who did not give consent including those who were sick were excluded from this study.
2.3 Sampling size calculation and sampling technique
The sample size was calculated using the single population proportion formula by karimollah,2011 [11].To adjust for the design effect of the sample design, the sample size was multiplied by the design effect. Hence, Z-score=1.96; Proportion= 50% marginal error=0.05, Design effect=3.5 and non-response rate=10%.
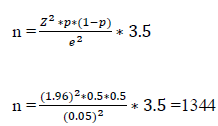
Therefore, the Minimum sample size was 1344 participants but finally a total of 1501 participants were recruited into the study. The number of communities selected in each health districts and number of participants sampled in each health districts were determined based on the probability proportionate to size technique taking into consideration the overall number of communities and the population size respectively (Tables 1 and 2). The sampling technique deployed in this study was simple randomly sampling where all community members had equal opportunities of being selected.
Table 1: Number of communities sampled based on probability proportionate to size, Fako health districts, 2018.
|
Health districts |
Number of communities (clusters) |
Number of community(ies) Sampled |
|
Buea |
95 |
2 |
|
Tiko |
109 |
2 |
|
Muyuka |
45 |
1 |
|
Limbe |
121 |
3 |
|
Total |
367 |
8 |
Table 2: Number of participants sampled per Health district base on probability proportionate to size , 2018.
|
Health district |
Total population |
Targeted population |
Number sampled |
|
Buea |
173526 |
95439 |
409 |
|
Limbe |
198516 |
109184 |
468 |
|
Muyuka |
151400 |
83270 |
357 |
|
Tiko |
113491 |
62420 |
267 |
|
Total |
636933 |
350313 |
1501 |
2.4 Data collection tool and procedures
The data collection tool was a semi structured questionnaire that was designed using Epicollect5 a mobile application that is used to collect data electronically using Android mobile phones or tablets. The questionnaire consisted of three sections: Section A consisted of participants’ sociodemographic and socioeconomic characteristics meanwhile section B consisted of 10 knowledge related questionnaires on HIV/AIDS and universal testing and treatment strategy and section C consisted of 5 attitude questions. The response options of the questions were yes, No and I don’t know. One thousand five hundred and one (1501) structured questionnaires were administered in the selected 8 villages within the 4 Health districts. The data was collected by 11 trained research assistants, all of which were final year master students in Epidemiology. After training a pre-test was done in Tole community, a community different from where the study was to be implemented.
2.5 Data analysis
All analyses were conducted using SPSS version 25. The analysis examined the knowledge and attitude level of participants on HIV/AIDS and Universal testing and treatment strategy. Descriptive statistics were used to analyze the sociodemographic characteristics of participants and their knowledge and attitude level on HIV/AIDS and UTT. The knowledge assessment was based on 10 point questions with Yes, No and I don’t know responses .However, participants who had the correct respond were scored 1 and those with incorrect response were scored 0 and the sum score of each participant was generated. The mean score for all the participants was calculated and participants who scored below the mean score were considered to have incorrect knowledge on HIV/AIDS and UTT and those whose scores were above the mean score were considered to have correct knowledge on HIV/AIDS and UTT. Similarly, the overall attitude level of the participants was assessed based on 5 point questions with yes and No options. In each question, participants who had correct answer were scored 1 while those with incorrect answer were scored 0. The sum score for each participants was calculated The mean score for all the participants was calculated and participants who scored below the mean were considered to have Negative attitude while those who scored above the mean were classified as having positive attitude.To assess the relative contribution of each predictor variables, a logistic regression analysis was carried out. Univariate logistic regression analysis examined the association between these variables and positive attitude towards HIV/AIDS and Universal testing and treatment. This allowed for the understanding the effect of each independent variable without controlling for confounding variables. Variables that were significant at the bivariate analysis were subjected to multivariate analysis to eliminate confounders. Associations between the outcome and independent variables were assessed using odds ratios at 95% confidence interval limits and all statistical significance were set at P<0.05.
2.6 Ethical and administrative approval
After developing the research protocol, the investigator obtained ethical approval from the University of Buea Institutional Review Board (IRB). Administrative authorisation was received from the Regional Delegation of Public Health for South West and other local administrative and traditional authorities within the study communities. Written/oral consent was obtained from every participant prior to participation.
3. Results
3.1 Socio-demographic and baseline characteristics
A total of 1501 participants were enrolled into this study among which there were 619 (41.2%) males and 882 (58.8%) females. The ages of the participants were categorized into four groups. Majority (41.1%) of them felt within the age group 25-35 years meanwhile 571 (38%) had ages between 15-24 years. However, 197 (13.1%) had ages between 35-44 years meanwhile those who were 45years and above constituted just 108 (7.2%) of the study population.
The mean of age of the participants was 29years. With respect to educational status, More than half (53.1%) had acquired secondary education whereas 400 (26.6% ) reported to have had tertiary education meanwhile those who reported not to have had any formal education and those who had primary education made up 22 (1.5%) and (287) 18.8 % of the study population respectively .A vast majority (96.7%) of the study participants were Christians. As per marital status of participants, 622 (41.4%) were either married or cohabitating meanwhile those who were single constituted 826 (55%) of the study population. Widows/widowers and those who had divorced/separated made up 36 (2.4%) and 17 (1.1%) of the study population, respectively. As concerns occupation, 538 (35.3%) reported Business as their main occupation, however 420 (28%) of the study participants were students meanwhile those who were farmers and civil servants constituted 141 (10.1%) and 64 (4.3%) respectively.
Also 209 (13.9%) reported to have been working in private sector whereas 127 (8.5%) reported that they were jobless. More than half (57.2%) of the participants reported to have monthly earnings less than 50000FCFA. 502 (33.4 %) of the participants reported to have monthly income between 50000-100000FCFAand only 59 (3.9%) have monthly income of more than 200000FCFA (Table 3).
Table 3: Sociodemographic characteristics of study participants, Fako health districts, 2018.
|
Variables |
Frequency(n=1501) |
Percentage (%) |
|
Gender |
||
|
Males |
619 |
58.8 |
|
Females |
882 |
41.2 |
|
Age |
||
|
15-24 |
571 |
38 |
|
25-34 |
625 |
41.6 |
|
35-44 |
197 |
13.1 |
|
45+ |
108 |
7.2 |
|
Educational level |
||
|
No formal education |
22 |
1.5 |
|
Primary education |
282 |
18.8 |
|
Secondary education |
797 |
53.1 |
|
Tertiary education |
400 |
26.6 |
|
Religion |
||
|
Christians |
1451 |
96.7 |
|
Muslims |
32 |
2.1 |
|
Others |
18 |
1.7 |
|
Marital status |
||
|
Married/cohabiting |
622 |
41.4 |
|
Separated/divorce |
17 |
1.1 |
|
Single |
826 |
55 |
|
Widow/widower |
36 |
2.4 |
|
Occupation |
||
|
Business |
530 |
35.3 |
|
civil servant |
64 |
4.3 |
|
Farmer |
141 |
10.1 |
|
Private sector |
209 |
13.9 |
|
student |
420 |
28.0 |
|
unemployed/no job |
127 |
8.5 |
|
Income level/ FCFA |
||
|
< 50000 |
858 |
57.2 |
|
50000-100000 |
502 |
33.4 |
|
101000-200000 |
82 |
5.5 |
|
>200000 |
59 |
3.9 |
3.2 knowledge level of participants on HIV/AIDS and universal testing and treatment strategy
Participants’ knowledge on the cause of AIDS, its transmission, prevention and treatment was assessed based on 10-point questionnaire. As to what causes
AIDS, almost all 1483 (98.8%) of the participants knew that AIDS is cause by a virus whereas a few 18 (1.2%) did not know what causes AIDS. With respect to HIV transmission, 1418 (94.5%) of participants reported that they know how HIV can be transmitted from one person to another. However, as to whether HIV can be transmitted by mosquitoes, 836 (55.7%) participants said mosquitoes cannot transmit HIV while 450 (30%) agreed that HIV can be transmitted by mosquitoes and on the other hand, 215 (14.4%) simply reported that they do not know if mosquitoes can transmit HIV or not (Table 4).
Also, almost all 1374 (91.8%) participants knew that somebody could look physically healthy but infected with HIV as they reported that healthy carriers do exist. However, some people still believe that somebody can be infected with HIV if he shares a meal with HIV infected persons as 11.2% of the participants in this study reported that HIV can be transmitted by sharing a meal with HIV infected person. As to whether condoms can reduce the chances of HIV transmission, 1050 (70%) agreed that condom can minimize the chances of HIV transmission when correctly used but 371 (24.7%) of the participants hold that Condoms do not minimize the chances of HIV transmission. 1152 (76.7%) reported that the risk of HIV infection can be reduced by having sex with only one uninfected partner. As to whether there is treatment for HIV/AIDS, 1124 (74.9%) reported that there is a treatment for HIV while 371 (17.9%) reported that the treatment for HIV does not exist and 109(7.1%) did not know whether treatment exist or not .Majority (60.1%) of the participants had never heard of the universal testing and treatment of HIV/AIDS. Among those who had heard of universal testing and treatment, only 67 (12.6%) knew what its meaning (Table 4).
Table 4: knowledge level of participants on HIV/AIDS and universal testing and treatment strategy, Fako health distracts, 2018.
|
Statement |
Frequency(N=1501) |
Percentage (%) |
|
Have heard of AIDS (n=1501) |
||
|
Yes |
1483 |
98.8 |
|
No |
18 |
1.2 |
|
knows how HIV is transmitted (n=1501) |
||
|
Yes |
1418 |
94.5 |
|
No |
83 |
5.5 |
|
HIV can be transmitted by mosquitoes (n=1501) |
||
|
Yes |
450 |
30.0 |
|
No |
836 |
55.7 |
|
I don’t know |
215 |
14.4 |
|
Can healthy looking person be infected with HIV (n=1501) |
||
|
Yes |
1374 |
91.8 |
|
No |
93 |
6.2 |
|
I don’t know |
20 |
2.0 |
|
Somebody can get HIV by sharing meal with HIV patient (n=1501) |
||
|
Yes |
168 |
11.2 |
|
No |
1243 |
82.8 |
|
I don’t know |
90 |
6.0 |
|
Use of condom reduce the chance of HIV transmission (n=1501) |
||
|
Yes |
1050 |
70.0 |
|
No |
371 |
24.7 |
|
I don’t know |
80 |
5.3 |
|
Risk of HIV infection can be reduced by having sex with only one uninfected partner (n=1501) |
||
|
Yes |
1152 |
76.7 |
|
No |
308 |
20.0 |
|
I don’t know |
41 |
2.7 |
|
There is a treatment for HIV (n=1501) |
||
|
Yes |
1124 |
74.9 |
|
No |
268 |
17.9 |
|
I don’t know |
109 |
7.1 |
|
heard of universal test and treat of HIV (n=n=1501) |
||
|
Yes |
599 |
39.9 |
|
No |
902 |
60.1 |
|
Know what Universal test and treat means (n=597) |
||
|
Yes |
67 |
12.6 |
|
No |
532 |
77.4 |
3.3 Attitude of participants on HIV/AIDS and the universal testing and treatment strategy
The attitude of participants towards HIV/AIDS and the universal testing and treatment approach was accessed based on five questions with Yes or No responses. With regards to accepting an HIV test when ask to do so, almost all 1392 (93.2%) of the participants agreed that they will undertake an HIV when they are offered. On the contrary 102 (6.8%) said they will not accept to do an HIV test when asked to, indicating that they are not interested in knowing their status as they have not been exposed.
With regards to encouraging people to do HIV test, a vast majority 1182 (87.5%) accepted that they will encourage people to do their HIV test as testing for HIV is one of the major steps to HIV prevention While 169 (12.5%) said it’s not their responsibility to encourage people to do HIV test as testing for HIV is a personal decision. Considering the sites for an HIV test and the person who does it, 845 (62.5%) of the participants reported that the sites and the person who does the test do not affect their decision to take the test as they can do the test anywhere and by any medical personnel and not specific people at specific places. However, as much as 506 (37.4%) of the participants reported that they cannot just do HIV test anywhere by anybody and they prefer to do it in the hospital. As concerns disclosing positive results to partner, 1145 (82%) agreed that they will disclose positive results to partner so they can also do their own test and know their status. 252 (18%) said they will not disclose their results to partner because HIV test is something confidential and one should keep it to him or herself. As to whether participants will accept to take drugs following positive results, almost all 11349 (97%) reported that if they are tested HIV positive, they will take drugs as this will make them healthy and live longer (Table 5).
Table 5: Attitude level of participants on HIV/AIDS and universal testing and treatment strategy Fako health districts, 2018.
|
Statement |
Frequency (%) |
Percentage (%) |
|
Accept to do HIV test when ask to (n=1494) |
||
|
Yes |
1392 |
93.2 |
|
No |
102 |
6.8 |
|
Encourage somebody to do HIV test(n=1391) |
||
|
Yes |
1182 |
87.5 |
|
No |
169 |
12.5 |
|
Site affects decision to take HIV test(n=1352) |
||
|
Yes |
506 |
37.4 |
|
No |
845 |
62.6 |
|
Disclose results to partner (n=1397) |
||
|
Yes |
1145 |
82 |
|
No |
252 |
18 |
|
Take drugs when positive (n=1391) |
||
|
Yes |
1349 |
97 |
|
No |
42 |
3 |
3.4 Overall level of knowledge and attitude of participants on HIV/AID and universal testing and treatment strategy
After assessing participants knowledge and attitude based on individual questions, the overall level of participants knowledge and attitude on HIV/AIDS and UTT strategy was determined, With respect to knowledge, there were 10 questions assessing the level of knowledge of participants on HIV/AIDS and UTT, each of these questions had Yes, No and I don’t know response options. However, participants who had the correct respond were scored 1 and those with incorrect rsponse were scored 0 and the sum total score of each participant was generated. The mean score for all the participants was calculated and participants who scored below the mean were considered to have incorrect knowledge on HIV/UTT and those whose scored were above the mean score were considered to have correct knowledge on HIV/AIDS and UTT. As such, 62.6% of the participants had correct knowledeg on HIV/AIDS and UTT whereas those who had incorrect knowledge made up 37.4% of the participants. Similary, the overall attitude of the participants was assessed based on 5 questions with yes and No anwer options In each question, .participants who had correct answer were scored 1 while those with incorrect answer were scored 0. The mean score for all the participants was calculated and participants who scored below the mean were considered to have Negative attitude while those who scored above the mean were classified as having positive attitude. In this regard, 1140 (76%) of the participants had positive attitude to HIV/AIDS and Universal testing and treatment startegy while 940 (62.6%) had cprrect knowledge on HIV/AIDS and UTT (Table 6).
Table 6: Overall level of knowledge and attitude of participants on HIV/AIDS and universal testing and treatment, Fako health districts,2018.
|
Variable |
Level |
Mean Score |
n=1501 |
% |
|
Knowledge |
Correct knowledge |
≥ 4.10 |
940 |
62.6 |
|
Incorrect knowledge |
<4.10 |
561 |
37.4 |
|
|
Attitude |
Positive attitude |
≥2.41 |
1140 |
76.0 |
|
Negative attitude |
<2.41 |
361 |
24.0 |
3.5 Predictors of positive attitude towards HIV/AIDS and universal testing and treatment strategy
In determining predictors of positive attitude towards HIV/AIDS and Universal testing and treatment strategy, a logistic regression model was deployed whereby different variables were subjected into to the model for bivariate logistic regression analysis and Crude Odd Ratios (COR) were determined at 95% Confidence interval and variables that were statistically significant (P<0.05) were further subjected to multivariate logistic analysis and Adjusted Odd ratios (AOR) were also determined. Factors significant at multivariate analysis were: Educational level, self-risk perception, participants knowledge level on HIV/AIDS and UTT Health districts, history of having 2 or more sexual partner in the past 12 months and income level. With respect to educational level, participants who had tertiary level of education were 6.9 times more likely to have a positive attitude towards HIV/AIDS and UTT approach compared to those who had no formal level of education. In the same line, individuals who had high self-risk perception were 3.9 times more likely have a positive attitude towards HIV/AIDS and UTT strategy compared to those who reported low risk perception .As per the level of knowledge on HIV/UTT strategy, participants who have correct knowledge were 4.1 times more likely to have positive attitude as opposed to those with incorrect knowledge. However, participants from Buea health districtwere 0.25 times less likely to have a positive attitude compared to those from Tiko. The study also revealed that participants who reported to earn monthly income of less than 50000 FCFA were 3.4times more likely to have a positive attitude compared to those earn more 200000 FCFA (Table 7).
Table 7: Predictors of positive attitude towards HIV/AIDS and universal testing and treatment strategy, Fako health districts, 2018.
|
Variables |
Positive attitude(n=1129) |
COR (95%CI |
AOR (95% CI ) |
|
Gender |
|||
|
males |
454 |
1 |
- |
|
Females |
675 |
1.19(0.93-1.05) |
- |
|
Age |
|||
|
45+ |
85 |
1 |
- |
|
35-44 |
136 |
0.60(0.35-1.10) |
- |
|
25-34 |
468 |
0.81(0.49-1.50) |
- |
|
15-24 |
440 |
0.91(0.55-1.45) |
- |
|
Educational level |
|||
|
No school |
19 |
1 |
1 |
|
primary |
249 |
2.91(2.24-3.78)* |
2.81(2.41-4.22) |
|
secondary |
633 |
5.67(3.76-8.61)* |
5.11(2.88-9.34) |
|
Tertiary |
228 |
6.22(4.21-9.82)* |
6.91(3.89-10.21)* |
|
Marital status |
|||
|
Widow(er) |
29 |
1 |
|
|
single |
608 |
0.67(0.29-1.56) |
- |
|
Separated |
11 |
0.44 ( 0.12-1.62) |
- |
|
Married |
581 |
1.21(0.12-12.04) |
- |
|
Occupation |
|||
|
unemployed |
96 |
1 |
- |
|
Students |
313 |
0.94(0.60-1.50) |
- |
|
Private |
176 |
1.72(0.94-2.98) |
- |
|
farmers |
110 |
0.87(0.50-1.41) |
- |
|
Civil servants |
38 |
0.47(0.25-0.90) |
- |
|
Business |
396 |
0.95(0.61-1.50) |
- |
|
Self-Risk perception |
|||
|
Low risk perception |
611 |
1 |
1 |
|
High risk perception |
518 |
4.1(1.52-8.33)* |
3.9(1.45-8.44)* |
|
Knowledge level |
|||
|
incorrect knowledge |
566 |
1 |
1 |
|
Correct knowledge |
563 |
4.6(2.44 -9.32)* |
4.1(2.34-8.99)* |
|
Health district |
|||
|
Tiko |
251 |
1 |
1 |
|
Muyuka |
334 |
0.93(0.48-1.79) |
0.83(0.34-1.74) |
|
limbe |
422 |
0.59(0.34-1.05) |
0.60(0.32-1.22) |
|
Buea |
122 |
0.27(0.02-0.05)* |
2.11(1.11-3.33)* |
|
Have had 2 or more sexual partner past 12 months |
|||
|
Yes |
264 |
1 |
1 |
|
No |
865 |
4.23(5.97-313.7)* |
4.11(5.78-312.4)* |
|
Income level/FCFA |
|||
|
>200000 |
36 |
1 |
1 |
|
101000-200000 |
54 |
1.23(0.62-2.45) |
1.22(0.55-2.84) |
|
50000-100000 |
321 |
1.13(0.65-1.97) |
1.11(0.63-1.75) |
|
<50000 |
718 |
3.27(1.88-5.70)* |
3.44(2.78-6.34)* |
|
Religion |
|||
|
Others |
16 |
1 |
- |
|
Muslims |
20 |
0.21(0.04-1.07) |
- |
|
Christians |
1093 |
0.38(0.09-1.67) |
- |
COR: Crude Odd Ratio, AOR: Adjusted Odd Ratio, *Statistically significant
4. Discussion
4.1 knowledge level of participants on HIV/AID and Universal testing and treatment strategy
This study was aimed at assessing the knowledge and attitude level of participants on HIV/AIDS and Universal testing and treatment strategy. Participants’ knowledge on the causes, transmission, prevention, and treatment of HIV/AID was assessed using structured questionnaires. With respect to causes of HIV/AIDS, A vast majority (98.8%) of the participants reported to have heard of HIV/AIDS. Also, Majority (94.5%) of the respondents also reported that they know how HIV can be transmitted from one person to another. These findings are similar to that of a study carried out in Ghana among University students [12]) .Surprisingly, as much as much 30% of the study participants still believed that mosquitoes transmit HIV/AID. This is very similar to a study conducted in Napel by Dhungel et al where 32% of the participants reported that HIV can be transmitted by mosquitoes [13] meanwhile another studies carried in Rwanda also showed that 10% of the participants believe that HIV can be transmitted by mosquitoes [14]. Also, almost all participants knew that somebody could look physically healthy but infected with HIV/AIDS and could transmit the virus to others. On the contrary, a study carried in Nepal reported that more than half of the participants believed that healthy looking individuals cannot be infected and consequently cannot infect others [13]. As to whether condom can prevent the transmission of HIV ,majority of the participants agreed that condom can prevent the transmission of HIV when correctly used. This findings align with studies carried out by Dzah et al among high school students in Ghana [15]. As concerns HIV treatment , a vast majority of the respondents were knowledgeable that HIV/AIDS can be treated though they did not know how these drugs are called .These findings are in the line with a study conducted by Mihaja et al in Madagascar where majority of the respondents reported that HIV/AIDS can be treated [16]. This study also revealed that majority of the participants did not know what UTT means and have never heard about it as they did not know that testing and treatment now is systematic. In general, the overall participants knowledge on HIV/AIDS and UTT was 62.6%. However, these findings differ from findings reported by shirim and Ahmed where they noted that only 56.1% of their participants had correct knowledge on HIV/AIDS and Universal Testing and treatment [17].
4.2 Attitude of participants towards HIV/AIDS and the universal testing and treatment strategy
The attitude of participants towards HIV/AIDS and the universal test and treat approach was accessed. The findings showed that Almost all (93.2%) of the participants agreed that if they are offered HIV test, they will accept and even go ahead to encourage somebody to go for voluntary testing .This is contrary to a study conducted in Southern Ethiopia [18] where only 68.8% reported they will accept to take an HIV test when offered. This difference could be attributed to the knowledge level of participants in the different studies. In this study the overall correct knowledge level of participants regarding HIV/AIDs and UTT was 78.6% as opposed to 67.4% reported in southern Ethiopia. This study has shown an association between participants’ knowledgeable level and acceptability of HIV testing and treatment. This means that Participants with correct knowledge level had higher odds of accepting HIV testing and treatment when tested positive. This coincides with findings reported by Lucy Chimoyi et al in south Africa [19]. Also, as to whether HIV testing site affects decision to take an HIV test, 37.4% reported that they cannot take an HIV anywhere, they preferred specific places to take their test. More than half (51.2%) of the participants indicated that their testing preference is the hospital. This is in line with studies conducted by Ucheoma Nwaozoru et al in Nigeria where 69% of the participants reported that they prefer to be tested in the hospital [20] As concerns results disclosure to partners, majority (82%) reported that they will disclose their results to partner if tested positive. This is higher than the findings reported in south Africa where only 58.4% agreed to disclose their positive results to partners [21]. The difference could be attributed to the differences in the targeted population, while this study targeted randomly selected individuals within the communities, the study in South Africa was limited to pregnant women who were attending their first ANC. Also almost all participants showed willingness to accept treatment if tested positive for HIV/AIDS and explained that positive HIV patients can only stay longer if they take their medications regularly. In general, 76% of the participants had a positive attitude towards HIV/AIDS and Universal testing and treatment .These findings are in line with studies conducted in Ethiopia among University students [22]. However, as much as 34% of the participants had negative attitudes towards HIV/AID and universal testing and treatment as they reported that they will turn down the test when offered, while others reported that if they carry out the test and it is positive, they will not tell their partners as they claim their result are personal and should not be shared with anybody not even their partners. These findings coincide with findings in Tanzania where among those with poor attitudes, majority reported that they will not take the test while other said even if they do the test and it comes out positive , nobody will be informed about as it their personal information [23] similar findings were reported in Tanzania where participants where some reported that they will not disclose their positive results to anybody not even to their partners.
4.3 Predictors of positive attitude towards HIV/AIDS and universal testing and treatment strategy
Our analysis showed that parameters that were significantly associated with good attitudes of participants towards HIV/AIDS and Universal testing and treatment were Educational level, HIV self-risk perception, participants knowledge level on HIV/AIDS and UTT , Health districts, history of having 2 or more sexual partner in the past 12 months and income level. With respect to educational level, participants who had no formal education were 6.9 times more likely to have a positive attitude towards universal test and treat approach compared to those who had tertiary education .This is in contrast with studies conducted in Zambia where participants with formal education had higher odds of having positive attitudes towards. HIV/AIDS and UTT compared to those with no formal education level [24]. Also, As per the level of knowledge on HIV/AIDS and UTT strategy, participants who had correct knowledge were 4.1 times more likely to have positive attitude as opposed to those with incorrect knowledge. multiple studies have demonstrated an association between HIV/AIDS knowledge and attitudes towards [16, 25, 26].This findings are in line with studies conducted in south Africa where participants with correct knowledge level had higher odds of adopting a good attitude towards HIV/AIDS and UTT [25].
However, participants from Buea health district were 2.11 times more likely to have a positive attitude compared to those from Tiko. This could be explained by the fact the communities that were selected for this studies in Tiko were more remote and majority of the participants were farmers with low level of education hence low level of knowledge on HIV/AIDS and UTT meanwhile Buea harbors mostly students and civil servants with high level of education and knowledge of HIV/AIDS and UTT hence this plays positivity on their attitude towards HIV/AIDS and UTT. Also participants who reported to earn monthly income of less than 50000 FRS (<$85) were 3.4times more likely to have positive attitude towards HIV/AIDS compared to those who earn more than 200000 FRS (>$333).This could be explained by the fact that participants monthly income of less than $85 per month are more conscious of the financial consequences of HIV/AIDS as compared to those with more than $333.
5. Conclusion
The level of knowledge regarding HIV/AIDS causes, transmission, prevention and treatment was considered satisfactory though majority of the participants had no information of on the testing and treatment approach Also ,some misconceptions about HIV transmission, risky behaviors and discriminatory attitudes were observed among participants that call for concern and must be addressed promptly. Regular education talks within the communities and in schools, should be reinforced to correct the misconceptions observed in this study and encourage positive attitudes towards PLHIV.
Declaration
Ethics Approval and Consent to Participate
All the principles of a good ethical research were respected. Ethical approval was obtained from the Institutional Review Board of the Faculty of Health Sciences of the University of Buea and during data collection, participants approval was sought prior to data collection.
Consent for Publication
Not applicable.
Availability of Data and Material
Not applicable.
Competing Interests
The authors declare that they have no competing interests.
Funding
No funding for the study was available.
Acknowledgments
This is part of a Ph.D. thesis by Kah Emmanuel Nji under the supervision of Prof. Ngowe Ngowe Marcelin and co-supervised by professor Enow Orock George and Professor Vincent Verla in the Department of Public Health and Hygiene of the University of Buea. We acknowledge all stakeholders including the District Medical Officers of Fako Health Districts, Regional Delegate for Public Health-South West Region, Chief of Health Centres, Heads of HIV treatment centers, Community leaders and colleagues for their contributions in the realization of this study. We equally acknowledge all the participants of this study for their collaboration.
Authors’ Contributions
KEN and NNM developed the study conception and design. KEN, NNM, DSN wrote the manuscript and contributed in the analysis and interpretation of the data. VVS, EOG contributed in the critical revision of the intellectual content of the manuscript. All the authors read and approved the final manuscript.
References
- Mohlabane N, Tutshana B, Peltzer K, et al. Barriers and facilitators associated with HIV testing uptake in South African health facilities offering HIV Counselling and Testing. Health SA Gesondheid 21 (2016): 86-95.
- Tarkang EE, Pietra V. Adolescents and Young Women’s Perceived Reasons for the Continued HIV/AIDS Prevalence in Kumba, Cameroon: A Qualitative Study. Int J HIVAIDS Prev Educ Behav Sci 1 (2015): 8.
- Abdurahman S, Seyoum B, Oljira L, et al. Factors affecting acceptance of provider-initiated HIV testing and counseling services among outpatient clients in selected health facilities in Harar Town, Eastern Ethiopia. HIVAIDS Auckl NZ 7 (2015): 157.
- Organization WH. Towards universal access: scaling up priority HIV (2009).
- Demographic C. Health Survey and Multiple Indicators Cluster Survey (DHS-MICS). Cameroon (2011).
- Kwenti TE, Nsagha DS, Kwenti BDT, et al. Sexual risk behaviours among people living with HIV and implications for control in the north west region of Cameroon. World J AIDS (2014): 2014.
- Haddison EC, Nguefack-Tsagué G, Noubom M, et al. Voluntary counseling and testing for HIV among high school students in the Tiko health district, Cameroon. Pan Afr Med J 13 (2012).
- Organization WH. Progress report 2016: prevent HIV, test and treat all: WHO support for country impact. World Health Organization (2016).
- Dieffenbach CW, Fauci AS. Universal voluntary testing and treatment for prevention of HIV transmission. Jama 301 (2009): 2380-2382.
- Granich RM, Gilks CF, Dye C, et al. Universal voluntary HIV testing with immediate antiretroviral therapy as a strategy for elimination of HIV transmission: a mathematical model. The Lancet 373 (2009): 48-57.
- Hajian-Tilaki K. Sample size estimation in epidemiologic studies. Casp J Intern Med 2 (2011): 289.
- Oppong AK, Oti-Boadi M. HIV/AIDS knowledge among undergraduate university students: implications for health education programs in Ghana. Afr Health Sci 13 (2013): 270-277.
- Dhungel BA, Shrestha N, U-Dhungel K. Perception and knowledge about HIV/AIDS among Nepalese adolescent. Janaki Med Coll J Med Sci 1 (2013): 32-39.
- Kambutse I, Igiraneza G, Ogbuagu O. Perceptions of HIV transmission and pre-exposure prophylaxis among health care workers and community members in Rwanda. PloS One 13 (2018): e0207650.
- Dzah SM, Tarkang EE, Lutala PM. Knowledge, attitudes and practices regarding HIV/AIDS among senior high school students in Sekondi-Takoradi metropolis, Ghana. Afr J Prim Health Care Fam Med [Internet] 11 (2019): e1-e11.
- Raberahona M, Lidamahasolo Z, Andriamamonjisoa J, et al. Knowledge, attitudes, perception and practices regarding antiretroviral therapy among HIV-infected adults in Antananarivo, Madagascar: a cross-sectional survey. BMC Health Serv Res [Internet] 19 (2019): 341.
- Shirin S, Ahmed S. Knowledge of AIDS among the adolescent students of two selected colleges of Dhaka City. Ibrahim Med Coll J 1 (2007): 5-8.
- Atnafu GN, Yeshambel WA, Abebe GK. Acceptance Of HIV Testing And Associated Factors Among Pregnant Women Attending Antenatal Care In Gunino Health Center, Southern Ethiopia 2019: An Institutional Based Cross-Sectional Study. HIVAIDS Auckl NZ 11 (2019): 333.
- Chimoyi L, Tshuma N, Muloongo K, et al. HIV-related knowledge, perceptions, attitudes, and utilisation of HIV counselling and testing: a venue-based intercept commuter population survey in the inner city of Johannesburg, South Africa. Glob Health Action [Internet] 8 (2015): 26950.
- Nwaozuru U, Iwelunmor J, Ong JJ, et al. Preferences for HIV testing services among young people in Nigeria. BMC Health Serv Res 19 (2019): 1-9.
- Ramlagan S, Matseke G, Rodriguez VJ, et al. Determinants of disclosure and non-disclosure of HIV-positive status, by pregnant women in rural South Africa. SAHARA-J J Soc Asp HIVAIDS [Internet] 15 9 2018): 155-163.
- Shiferaw Y, Alemu A, Girma A, et al. Assessment of knowledge, attitude and risk behaviors towards HIV/AIDS and other sexual transmitted infection among preparatory students of Gondar town, north west Ethiopia. BMC Res Notes 4 (2011): 505.
- Kikwasi GJ, Lukwale SR, Mwageni EA. A Study of First Year Students Attitude towards HIV and AIDS. Glob J Health Sci [Internet] 9 (2017): 117.
- Muyunda B, Musonda P, Mee P, et al. Educational attainment as a predictor of HIV testing uptake among women of child-bearing age: analysis of 2014 demographic and health survey in Zambia. Front Public Health 6 (2018): 192.
- Ryan S, Hahn E, Rao A, et al. The impact of HIV knowledge and attitudes on HIV testing acceptance among patients in an emergency department in the Eastern Cape, South Africa. BMC Public Health 20 (2020): 1-10.
- Cherutich P, Kaiser R, Galbraith J, et al. Lack of knowledge of HIV status a major barrier to HIV prevention, care and treatment efforts in Kenya: results from a nationally representative study. PloS One 7 (2012): e36797.


 Impact Factor: * 3.6
Impact Factor: * 3.6 Acceptance Rate: 76.49%
Acceptance Rate: 76.49%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 