Comparative Study on Intraoperative Localization of Sentinel Lymph Node in Breast Cancer Patients using Tc 99m Sulfur Colloid and Blue Dye
Vindhya Malasani1, Vedant Kabra2, Ishita Barat Sen1*, Parul Thakral1, Pallavi UN1, Kanchan Sharma1, Divya Manda1, Vineet Pant1
1Department of Nuclear Medicine & Molecular Imaging, Fortis Memorial Research Institute, Gurgaon, India
2Department of Surgical Oncology, Manipal Hospitals, Dwarka, New Delhi, India
*Corresponding Author: Ishita Barat Sen, Department of Nuclear Medicine and Molecular Imaging, Fortis Memorial Research Institute, Gurgaon, India
Received: 18 September 2019; Accepted: 30 September 2019; Published: 07 October 2019
Article Information
Citation: Ishita Barat Sen. Comparative Study on Intraoperative Localization of Sentinel Lymph Node in Breast Cancer Patients using Tc 99m Sulfur Colloid and Blue Dye. Journal of Cancer Science and Clinical Therapeutics 3 (2019): 291-296.
View / Download Pdf Share at FacebookAbstract
Background: A sentinel lymph node (SLN) is considered to be the first lymph node which is draining the tumor site. Radioactive Tc-99m labeled sulfur colloid, vital blue dye such as isosulfan blue or methylene blue, or the combination of the both is generally used for sentinel lymph node localization. In this study, we compare the sensitivity of both the methods to establish an effective method for SLN localization among early cases of breast cancer.
Methods: Forty incidental cases, consulting the hospital between Jan 2015- June 2017 and diagnosed with early breast cancer (Stage T1N0M0 and T2N0M0) were subjected to sentinel lymph node detection by both radiocolloid and dye.99mTc-labeled are filtered sulfur colloid was administered intradermally in the periaerolar region in the tumor quadrant, 30 mins-1 h prior to the surgery. 1ml methylene blue dye, was administered, intraparenchymally, by circumareolar region during the surgery. All radioactive lymph nodes were removed until the background activity was less than one-tenth the ex-vivo value of hottest node. All the blue dye positive nodes, whether or not radiocolloid positive were excised and labeled accordingly and sent for histo-pathological examination.
Results: SLN detection & localization was positive in 36 patients with radiocolloid and 34 patients with blue dye and in 2 patients neither of these methods showed any signs of involvement of the lymph node. The ability to identify the SLN for colloid alone, blue dye alone and the combination of both the methods was 90%, 85% and 95%, respectively. The concordance between blue dye and radiocolloid was 80%. Metastatic lymph node involvement was found in 13/38 (34.2 %) of patients.
Conclusion: Both the radiocolloid and dye drains to the same SLN node however, the SLN detection ability was found to be high when both the methods are used in combination.
Keywords
<p>Lymph Node; Breast Cancer; Tumor; Nodal metastases</p>
Article Details
1. Introduction
Incidence of breast cancer in India was estimated to be 25.8 per 100 000 [1]. It is estimated that nodal metastases incidence of tumor <1 cm is approximately 22% [2, 3]. Axillary lymph nodal status has the most prognostic significance which can be assessed by either axillary nodal dissection or by sentinel lymph node biopsy [4]. A sentinel lymph node is the first lymph node which is draining the tumor site. It is believed that if the sentinel lymph node is free of tumor, then the probability of having the spread of the disease remaining lymph nodes of primary and subsequent basin is very low [5, 6] Over past 20 years sentinel lymph node biopsy has been the standard technique for axillary staging [5, 7]. Radiocolloid or blue dye (methylene blue or isosulfan blue) or the combination of both the methods can be used for sentinel lymph node localization [4, 8]. The chief advantage of sentinel lymph node biopsy is to identify the group of patients in whom unwanted axillary dissection can be avoided which is associated with devastating complications like paresthesia’s (78%), lymphedema(15-30%), seroma etc [9]. Several trails and metaanalysis demonstrated that there is no statistical difference in the survival, disease free survival and regional disease control between the patients treated with axillary clearance and who are not in whom sentinel lymph node biopsy was negative [5, 8]. One of the initial studies done by Giuliano et al in 1994 published 93% success rate in detection of sentinel node using blue dye and another initial study done by Krag et al. [6] published a success rate of 82% using radiocolloid [10, 6]. Wide variations in the success rates were seen using either radiocolloid or blue dye in different studies may be because of the difference in the experience among the breast surgeons and nuclear medicine physicians or because of the different techniques [4].
In this study, we compared the sensitivity of both the methods to establish an effective method for SLN localization. It was hypothesized that the sensitivity of sentinel lymph node localization using a combination of both the methods is better than either of the one alone.
2. Patients Selection and Method
2.1 Patients selection
This is a single institution prospective analysis conducted from 2015- 2017. In this study, we included 40 patients undergoing SLN localization, diagnosed with high-risk or micro-invasive ductal carcinomas in situ or invasive ductal carcinoma (stage T1N00 and T2N0M0) evidenced by fine-needle aspiration or core biopsy without clinically palpable lymph nodes. Our exclusion criteria were patients with regional or distant metastases, clinically palpable large tumor, locally advancing breast cancer, previous extensive surgery, radiotherapy to the tumor site, ipsilateral axilla and pregnant females. As per the institutional ethics committee protocol, informed written consent were obtained prior to sentinel lymph node localization procedure. All the patients underwent sentinel lymph node localization using the combination technique of both methylene blue and radioactive colloid.
2.2 Method
99mTc-labeled are filtered sulfur colloid of 12-15 MBq (300-400µCi) in 0.3–0.4 ml volume was administered intradermally in the periaerolar region in the tumor quadrant using an insulin syringe, 30 mins-1 h prior to the surgery. The radioactive colloid was administered by a group of qualified nuclear medicine physicians for every patient. For blue dye analysis, 1ml of methylene blue dye was administered intraparenchymally in circumareolar region during the surgery 10-15 minutes prior to the skin incision and the breast was massaged for 1-2 minutes. Massaging the breast after the blue dye injection facilitates in identifying the blue lymphatics and lymph nodes. Radioactive lymph nodes were detected by the surgeon using a hand-held surgical gamma probe (Euro probe 3.2) Figure 1. All the radioactive nodes were removed until background activity was less than one-tenth the ex-vivo value of hottest node i.e. the lymph node with highest radioactive counts. The blue lymphatic vessels were traced during the surgery and all blue positive nodes, whether or not radiocolloid positive were excised and labeled accordingly. Additionally, lymph nodes, which appeared suspicious to the surgeon were also removed. Frozen sectioning, hematoxylin & eosin and immunohistologic (cytokeratin) staining were conducted on all lymph nodes.
3. Results
Forty incidental patients attending the hospital between Jan 2015 to June 2017, and fulfilling the inclusion and exclusion criteria were included in the study. The success rate (ability to detect the sentinel lymph node) for combined methods and radiocolloid and the blue dye methods separately were calculated according to the surgeon’s notes. Blue dye was successful in detecting sentinel lymph node in 34 patients with a detection rate of 85%. Similarly, when radioactive colloid was used, out of 40 patients suffering from early stages of breast cancer, 36 sentinel lymph nodes were found to be positive with a detection rate of 90%. Table 1 shows that the concordance between blue dye and radiocolloid was 80% (32/40). The overall detection rate was found to be 95% when both the techniques were simultaneously used. In 4 patients (4/40, 10%), radioactive colloid was successful in detecting sentinel node whereas blue dye failed to detect them. However, blue dye was positive to detect sentinel node in 2 patients (2/40) where radiocolloid missed them. Metastatic lymph node involvement was found in 13/38 (34.2 %) of patients as per histopathological findings. Both the radiocolloid and blue dye failed to localize sentinel lymph node in 2 patients. As a result, prophylactic level I and II lymph nodal dissection were done in these two patients, although no metastatic deposits were found on histopathology. All the suspicious lymph nodes other than the sentinel lymph nodes, which were removed by the surgeon during surgery were found to also negative for tumor on histopathology. This can lead to the interpretation that the false-negative results were less likely with either blue dye or radiocolloid.
|
SLN Detection Method |
No. patients positive (n=40) |
Detection rate % |
|
Radiocolloid positive with blue dye negativity |
4 |
10% |
|
Only Blue dye positive with Radiocolloid negativity |
2 |
5% |
|
Both Blue Dye & Radioactive Colloid positive |
32 |
80% |
|
Positive either by Radioactive colloid and or blue dye |
38 |
95% |
Table 1: The detection rates with blue dye, radiocolloid and combined methods.
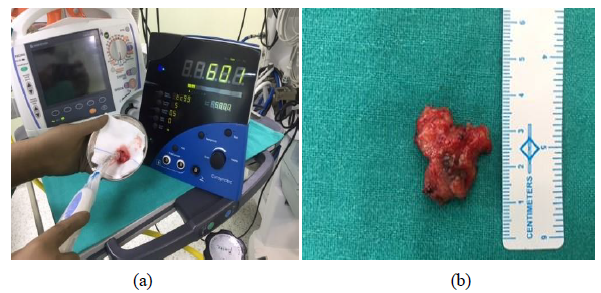
Figure 1: Hand held Gamma Probe to identify SLNB (a): Hand gamma probe for reconfirmation of hot node (b): Exvivo SLNB.
4. Discussion
As we all know that sentinel lymph node is defined as one or a few lymph nodes that receive the first drainage from a tumor site, it is hypothesized that if SLNs are proved to be negative for malignancy, the regional node dissection and its morbidity can be avoided. Sentinel lymph node localization was first proposed by Cabanas for penile cancer [11]. SLN biopsy has now emerged as the new standard of care in melanoma and breast cancer [5, 8, 12]. It is estimated that the probability of isolated axillary relapse after a negative SLN biopsy was less than or equal to 1% when compared with the gold standard axillary lymph node dissection [13]. The long-term morbidities associated with SLN biopsy were much lesser than the axillary lymph node dissection [13].
In our study, the detection rate using radioactive colloid was 90%, with methylene blue dye was 85% and when both were used in combination the detection rate raised significantly to 95%. According to the results of our study, radiocolloid method had a higher success rate than the blue dye method (90% vs. 85%). The results of this validation study are in alliance when compared with other studies on the sentinel node biopsy in early breast carcinoma [4, 8, 3]. A significant difference in success rate was found between the blue dye and combined methods (85% vs. 95%) which is in line with the other study by S. P. Somashekhar et al. [14] who had the difference of 84% and 100%. The concordance rate between the radiocolloid and the blue dye was 80% in the current study. According to the other studies done by Rakesh Kumar et al. [4] and Borrgstein et al. [15] the concordance in SLN detection between blue dye and radiocolloid were 90% and 100%. The difference could be attributable to a learning curve for the surgeons [4]. A large multi-institutional study done by McMasters et al. suggested that an individual surgeon should at least perform 20 SLNB with accompanying complete axillary dissection to reach an acceptable level of identification rate [16].
We found that in 10% (4/40) patients, SLN were localized by radiocolloid only and not by blue dye. However, there were only 2 patients (5%) in which blue dye was successful in detecting the sentinel nodes whereas radio-colloid failed to detect them. Rakesh Kumar et al [4] reported that 6.8% of SLNs localized by radiocolloid were not identified by blue dye and, in the same study, 2% of SLNs were identified by blue dye but were radiocolloid negative. Therefore, we could justify that using both the techniques simultaneously can attain the maximum possible success rate than using either of them alone. In this study, radiocolloid and blue dye both failed to localize the SLN in 5% of patients (2/40). In the literature, it is documented that there is a probability of 3%-8% failure rate even after using both techniques simultaneously [17]. Reasons for failure of sentinel lymph node localization may be prior excision of the breast tumor or prior axillary node surgery or faulty techniques etc. [18]. In our study, we were not able to exactly identify the cause, but one of the reasons could be that not all the patients were administered with radiocolloid by same nuclear medicine physician which can be lead to varying results due to varying techniques. One of the limitations of our study is the small cohort of the patients and the other one is that not all the patients underwent axillary dissection to comment on actual true negatives.
5. Conclusion
Both the radioactive colloid and blue dye drain to the same node in most of the patients. The sensitivity is found to be highest with the combination of the two methods.
References
- Gupta A, Sridhar K, Dhillon PK. A review of breast cancer awareness among women in India: cancer literate or awareness deficit? Eur J Cancer 51 (2015): 2058-2066.
- Fisher B, Slack NH. Number of lymph nodes examined and their prognosis of breast carcinoma. Surg Gynecol Obstet 131 (1970): 79–88.
- Rivadeneira DE, Simmons RM, Christos PJ, et al. Predictive factors associated with axillary lymph node metastases in T1a and T1b breast carcinomas: analysis in more than 900 patients. J Am Coll Surg 191 (2000): 1-6.
- Kumar R, Jana S, Heiba SI, et al. Retrospective analysis of sentinel node localization in multifocal, multicentric, palpable, or nonpalpable breast cancer. J Nucl Med 44 (2003): 7-10.
- Moncayo VM, Aarsvold JN, Alazraki NP. Lymphoscintigraphy and sentinel nodes. J Nucl Med 56 (2015): 901-907.
- Krag DN, Weaver DL, Alex JC, et al. Surgical resection and radiolocalization of the sentinel lymph node in breast cancer using a gamma probe. Surg Oncol 2 (1993): 335-340.
- Cody HS, Fey J, Akhurst T, et al. Complementarity of blue dye and isotope in sentinel node localization for breast cancer: univariate and multivariate analysis of 966 procedures. Ann. Surg. Oncol 8 (2001): 13-19.
- Tafra L, Lannin DR, Swanson MS, et al. Multicenter trial of sentinel node biopsy for breast cancer using both technetium sulfur colloid and isosulfan blue dye. Ann Surg 233 (2001): 51.
- Varghese P, Mostafa A, Abdel-Rahman AT, et al. Methylene blue dye versus combined dye-radioactive tracer technique for sentinel lymph node localisation in early breast cancer. Eur J Surg Oncol 33 (2007): 147-152.
- Giuliano AE, Kirgan DM, Guenther JM, et al. Lymphatic mapping and sentinel lymphadenectomy for breast cancer. Ann Surg 220 (1994): 391-401.
- Cabanas R. An approach for the treatment of penile carcinoma. Cancer 39 (1977): 456–466.
- Morton DL, Wen DR, Wong JH, et al. Technical details of intraoperative lymphatic mapping for early stage melanoma. Arch Surg 127 (1992): 392–399.
- Cody HS. Clinical aspects of sentinel node biopsy. Breast Cancer Research 3 (2001): 104.
- Somashekhar SP, Zaveri Shabber S, Udupa Venkatesh K, et al. Sentinel lymphnode biopsy in early breast cancer using methylene blue dye and radioactive sulphur colloid-a single institution Indian experience. Indian J Surg 70 (2008): 111-119.
- Borgstein PJ, Meijer S, Pijper R. Intradermal blue dye to identify sentinel lymph node in breast cancer. Lancet 349 (1997): 1668-1669.
- McMasters KM, Wong SL, Chao C, et al. Defining the optimal surgeon experience for breast cancer sentinel lymph node biopsy: a model for implementation of new surgical techniques. Ann Surg 234 (2001): 292-299.
- Wu CT, Morita ET, Treseler PA, et al. Failure to harvest sentinel lymph nodes identified by preoperative lymphoscintigraphy in breast cancer patients. Breast J 9 (2003): 86-90.
- Ratchaworaponga K, Thanawuta S, Yodavudhb S, et al. Rate of sentinel lymph node identification using isosulfan blue dye in breast cancer patients at Charoenkrung Pracharak Hospital, Thailand. Asian Biomedicine 8 (2014): 517-552.


 Impact Factor: * 4.1
Impact Factor: * 4.1 Acceptance Rate: 74.74%
Acceptance Rate: 74.74%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 