Intravenous Lipoleiomyomatosis Mimicking Malignant Degeneration of Leiomyoma
Jason Ricciuti1*, Devi Jaychandran2, Peter Frederick1
1Department of Gynecologic Oncology, Roswell Park Comprehensive Cancer Center, Buffalo, NY, USA
2Department of Pathology, Roswell Park Comprehensive Cancer Center, Buffalo, NY, USA
*Corresponding Author: Dr. Jason Ricciuti, Department of Gynecologic Oncology, Roswell Park Comprehensive Cancer Center, Buffalo, NY, USA
Received: 06 July 2020; Accepted: 31 July 2020; Published: 24 August 2020
Article Information
Citation: Jason Ricciuti, Devi Jaychandran, Peter Frederick. Intravenous Lipoleiomyomatosis Mimicking Malignant Degeneration of Leiomyoma. Journal of Cancer Science and Clinical Therapeutics 4 (2020): 304-313.
View / Download Pdf Share at FacebookKeywords
Intravenous leiomyomatosis; Neoplasm; Lipoleiomyoma; Lipoleiomyomatosis
Intravenous leiomyomatosis articles, Neoplasm articles, Lipoleiomyoma articles, Lipoleiomyomatosis articles
Intravenous leiomyomatosis articles Intravenous leiomyomatosis Research articles Intravenous leiomyomatosis review articles Intravenous leiomyomatosis PubMed articles Intravenous leiomyomatosis PubMed Central articles Intravenous leiomyomatosis 2023 articles Intravenous leiomyomatosis 2024 articles Intravenous leiomyomatosis Scopus articles Intravenous leiomyomatosis impact factor journals Intravenous leiomyomatosis Scopus journals Intravenous leiomyomatosis PubMed journals Intravenous leiomyomatosis medical journals Intravenous leiomyomatosis free journals Intravenous leiomyomatosis best journals Intravenous leiomyomatosis top journals Intravenous leiomyomatosis free medical journals Intravenous leiomyomatosis famous journals Intravenous leiomyomatosis Google Scholar indexed journals Neoplasm articles Neoplasm Research articles Neoplasm review articles Neoplasm PubMed articles Neoplasm PubMed Central articles Neoplasm 2023 articles Neoplasm 2024 articles Neoplasm Scopus articles Neoplasm impact factor journals Neoplasm Scopus journals Neoplasm PubMed journals Neoplasm medical journals Neoplasm free journals Neoplasm best journals Neoplasm top journals Neoplasm free medical journals Neoplasm famous journals Neoplasm Google Scholar indexed journals Lipoleiomyoma articles Lipoleiomyoma Research articles Lipoleiomyoma review articles Lipoleiomyoma PubMed articles Lipoleiomyoma PubMed Central articles Lipoleiomyoma 2023 articles Lipoleiomyoma 2024 articles Lipoleiomyoma Scopus articles Lipoleiomyoma impact factor journals Lipoleiomyoma Scopus journals Lipoleiomyoma PubMed journals Lipoleiomyoma medical journals Lipoleiomyoma free journals Lipoleiomyoma best journals Lipoleiomyoma top journals Lipoleiomyoma free medical journals Lipoleiomyoma famous journals Lipoleiomyoma Google Scholar indexed journals Lipoleiomyomatosis articles Lipoleiomyomatosis Research articles Lipoleiomyomatosis review articles Lipoleiomyomatosis PubMed articles Lipoleiomyomatosis PubMed Central articles Lipoleiomyomatosis 2023 articles Lipoleiomyomatosis 2024 articles Lipoleiomyomatosis Scopus articles Lipoleiomyomatosis impact factor journals Lipoleiomyomatosis Scopus journals Lipoleiomyomatosis PubMed journals Lipoleiomyomatosis medical journals Lipoleiomyomatosis free journals Lipoleiomyomatosis best journals Lipoleiomyomatosis top journals Lipoleiomyomatosis free medical journals Lipoleiomyomatosis famous journals Lipoleiomyomatosis Google Scholar indexed journals pelvic vessels articles pelvic vessels Research articles pelvic vessels review articles pelvic vessels PubMed articles pelvic vessels PubMed Central articles pelvic vessels 2023 articles pelvic vessels 2024 articles pelvic vessels Scopus articles pelvic vessels impact factor journals pelvic vessels Scopus journals pelvic vessels PubMed journals pelvic vessels medical journals pelvic vessels free journals pelvic vessels best journals pelvic vessels top journals pelvic vessels free medical journals pelvic vessels famous journals pelvic vessels Google Scholar indexed journals uterine tumor articles uterine tumor Research articles uterine tumor review articles uterine tumor PubMed articles uterine tumor PubMed Central articles uterine tumor 2023 articles uterine tumor 2024 articles uterine tumor Scopus articles uterine tumor impact factor journals uterine tumor Scopus journals uterine tumor PubMed journals uterine tumor medical journals uterine tumor free journals uterine tumor best journals uterine tumor top journals uterine tumor free medical journals uterine tumor famous journals uterine tumor Google Scholar indexed journals adipose tissue articles adipose tissue Research articles adipose tissue review articles adipose tissue PubMed articles adipose tissue PubMed Central articles adipose tissue 2023 articles adipose tissue 2024 articles adipose tissue Scopus articles adipose tissue impact factor journals adipose tissue Scopus journals adipose tissue PubMed journals adipose tissue medical journals adipose tissue free journals adipose tissue best journals adipose tissue top journals adipose tissue free medical journals adipose tissue famous journals adipose tissue Google Scholar indexed journals mytotic atypia articles mytotic atypia Research articles mytotic atypia review articles mytotic atypia PubMed articles mytotic atypia PubMed Central articles mytotic atypia 2023 articles mytotic atypia 2024 articles mytotic atypia Scopus articles mytotic atypia impact factor journals mytotic atypia Scopus journals mytotic atypia PubMed journals mytotic atypia medical journals mytotic atypia free journals mytotic atypia best journals mytotic atypia top journals mytotic atypia free medical journals mytotic atypia famous journals mytotic atypia Google Scholar indexed journals levonorgestrel intrauterine articles levonorgestrel intrauterine Research articles levonorgestrel intrauterine review articles levonorgestrel intrauterine PubMed articles levonorgestrel intrauterine PubMed Central articles levonorgestrel intrauterine 2023 articles levonorgestrel intrauterine 2024 articles levonorgestrel intrauterine Scopus articles levonorgestrel intrauterine impact factor journals levonorgestrel intrauterine Scopus journals levonorgestrel intrauterine PubMed journals levonorgestrel intrauterine medical journals levonorgestrel intrauterine free journals levonorgestrel intrauterine best journals levonorgestrel intrauterine top journals levonorgestrel intrauterine free medical journals levonorgestrel intrauterine famous journals levonorgestrel intrauterine Google Scholar indexed journals nephrolithiasis articles nephrolithiasis Research articles nephrolithiasis review articles nephrolithiasis PubMed articles nephrolithiasis PubMed Central articles nephrolithiasis 2023 articles nephrolithiasis 2024 articles nephrolithiasis Scopus articles nephrolithiasis impact factor journals nephrolithiasis Scopus journals nephrolithiasis PubMed journals nephrolithiasis medical journals nephrolithiasis free journals nephrolithiasis best journals nephrolithiasis top journals nephrolithiasis free medical journals nephrolithiasis famous journals nephrolithiasis Google Scholar indexed journals
Article Details
1. Introduction
Intravenous leiomyomatosis (IVL) is a rare condition in which a benign smooth muscle neoplasm is found extending into pelvic vessels. The frequency of IVL is difficult to ascertain due to its potential to be overlooked on routine pathologic assessment of leiomyoma, but it has been reported to be as few as 0.097% of all smooth muscle tumors [1]. While IVL is a benign neoplasm, extension from the pelvic vessels to the inferior vena cava (IVC) and even into the right heart or pulmonary vasculature have been observed [2-5]. Lipoleiomyoma (LPL) is an uncommon, benign uterine tumor distinguished by a mixture of smooth muscle and adipose tissue with little to no mytotic atypia. Both LPL and IVL are rare diagnoses and the combination of the two is exceedingly uncommon with only 8 being reported in the English literature [6-11]. Our case describes a patient with intravenous lipoleiomyomatosis who presented with concern for malignant degeneration of leiomyoma after an incidental finding of a large pelvic mass located at the sight of a previously imaged leiomyoma.
2. Case Report
A 37-year-old nulliparous woman initially presented to her primary gynecologist for routine exchange of her levonorgestrel intrauterine (IUD). The device’s strings were not visualized on exam so an ultrasound was ordered to assess its positioning. Patient’s medical history was notable for nephrolithiasis and a left lower-extremity deep vein thrombosis that occurred during a period of immobilization while taking combined oral contraceptives (COC). Her surgical history included a laparoscopic left ovarian cystectomy performed 15 years prior to presentation. She had no family history of breast, ovarian, or colon cancer. Transvaginal ultrasound demonstrated a 25.7 × 11.5cm mass with solid components in the right adnexal region and complex cystic components in the left adnexal region. Solid components demonstrated flow on color and spectral Doppler interrogation. Neither ovary was visualized and the uterus was noted to be 9.6 × 3.9 × 8.0cm with IUD in proper position.
A CT scan of the abdomen and pelvis with contrast was obtained to further assess the mass (Figure 1). This confirmed a 18 × 22 × 29cm heterogeneous mass with primarily solid components located in the right side of the pelvis. An additional multi-loculated complex cystic mass was noted arising from the left ovary and measured 18 × 24 × 23 cm. The right ovary was not identified. A few mildly enlarged retroperitoneal para-aortic lymph nodes were noted (largest 22 mm). There was no evidence of omental or mesenteric tumor infiltration and no ascites. When compared to an ultrasound and MRI performed approximately 5 years prior (images not available), the large solid mass was found to originate in the same location as a 5.4cm intramural or subserosal fibroid.
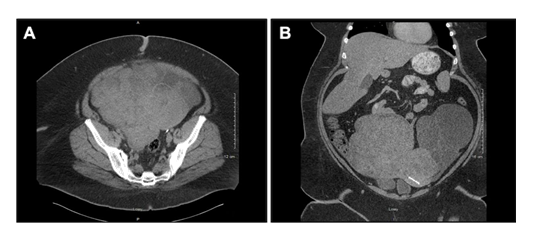
Figure 1: Preoperative CT abdomen and pelvis with IV contrast performed in 2016. (A) Transverse and coronal images demonstrating right-sided pelvic mass contiguous with uterus and left-sided cystic mass. (B) Intrauterine device visible on image B.
Patient had additional abdominal imaging 3 years prior to presentation in the setting of nephrolithiasis and sepsis (Figure 2). The non-contrast CT of the abdomen and pelvis at that time noted “slightly bulbous contour of the uterus…bilateral enlargement of the adnexal regions” with left adnexa measuring 9.8 × 8.7 × 7.7cm and right adnexa measuring 10.2 × 9.2 × 8.2 cm. Tumor markers revealed an elevated CA 125 (106 U/mL) and normal alpha-fetoprotein and CEA (1.1 ng/mL and <0.5 ng/mL, respectively). Given concern for a malignant transformation of the leiomyoma noted on prior imaging, the patient was referred to gynecologic oncology for further treatment. Surgical exploration and removal of the mass was recommended.
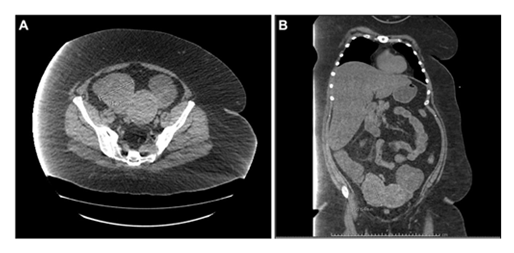
Figure 2: Non-contrast CT performed in 2013, 3 years prior to presentation for non-gynecologic indications. Imaging demonstrates similar orientation and distribution of pelvic masses at an earlier stage.
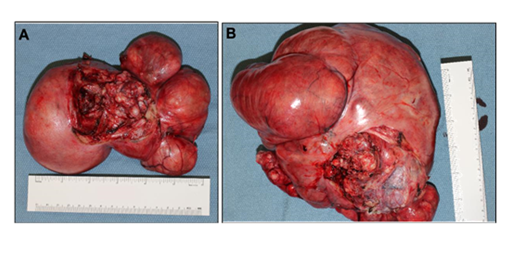
Figure 3: Gross surgical specimen. (A) showing cut edge of right lateral surface of uterus (anterior surface oriented toward top of page) and (B) showing cut edge of right-sided mass.
Laparotomy was performed via a midline vertical incision. Intraoperative findings demonstrated massive enlargement of both ovaries (>25 cm). The right ovary was visibly abnormal and neoplasm was noted to involve the right broad ligament and uterus (Figure 3). The left ovary was independent from this mass and appeared multi-cystic. All other peritoneal and visceral surfaces appeared grossly normal. A right salpingo-oophorectomy was performed and the specimen sent for intraoperative frozen section, which demonstrated a low-grade spindle cell neoplasm. Due to the gross involvement of the uterus with the right-sided neoplasm and the markedly abnormal left ovary, decision was made to proceed with hysterectomy and left salpingo-oophorectomy. Omental biopsy was also obtained. Her surgery was otherwise uncomplicated and had an estimated blood loss of 800 mL.
Histologic assessment of the right adnexal mass and uterus demonstrated intravenous lipoleiomyomatosis (Figures 4). Immunohistochemical staining of the right-sided solid mass was positive for smooth muscle actin (SMA), desmin, and CALD and negative for CD10. Cytogenetics showed 46 XX, t(9;12)(p22;q14) with reciprocal translocation identified in all cells from culture. Left ovary was found to be a benign serous cystadenoma.
Patient’s postoperative course was unremarkable and she was discharged on postoperative day three. Given her history of DVT while using COC, estrogen replacement was deemed to be contraindicated so she was started on Effexor to treat menopausal symptoms. She was seen at routine postoperative visits and was found to be recovering appropriately. At her final clinic visit two months after her initial surgery, the patient was recommended to follow up with her regular OB/GYN for routine care.
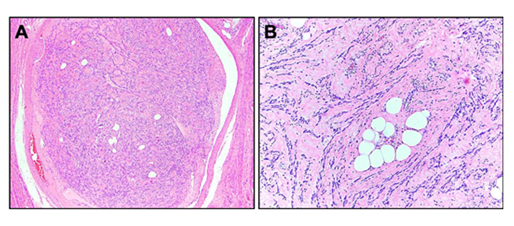
Figure 4: Histologic section (A) demonstrating intravascular component of smooth muscle within vessel on H&E staining. Higher-power representation (B) of lipomatous component within smooth muscle on H&E staining.
3. Discussion
Intravenous lipoleiomyoma is a very rare diagnosis and our case is the first in the literature to provide serial imaging of this condition. Intravenous leiomyomatosis has been reported to account for 0.097% of all smooth muscle tumors [1]. The exact rate of IVL is less clear given its apparent rarity and the potential for very early cases to be missed or misdiagnosed. Many case reports of IVL in the literature highlight cases of cardiac extension given the novelty of benign pelvic disease causing cardiopulmonary pathology. While the neoplasm itself is benign by definition, it has the potential for serious complications as it extends proximally through the vasculature and has even been attributed as the cause of death in several patients [12-14]. The pathogenesis of IVL is unclear and several hypotheses have been advanced. Based on early observations by Knauer, it has been suggested that IVL arises directly from smooth muscle in the vessel wall [15]. Alternatively, Sitzenfry, a contemporary of Knauer, supported IVL deriving from direct extension of primary leiomyoma into the vasculature [16]. Later case reports and evidence of immunohistochemical staining with desmin or ER/PR on tumor, but not vessels walls support the process of direct extension [17, 18]. Our case provides additional evidence for direct extension of the tumor into the vasculature based on the progressive growth and expansion of a uterine mass on imaging, which ultimately demonstrated intravenous components on pathology.
Table 1: Summary of patient data from nine largest case series.
Previous cytogenetic analysis of IVL has suggested that rearrangement or deletions of 12q14-15 and possibly 14q24 may contribute to the development of IVL [19-21]. Additionally, cytogenetic characterization of lipoleiomyoma has described reciprocal translocation of t(5;12)(q12;q24) [22] and t(12;14)(q15;q22),der(1),der(5) [23]. Our case demonstrated a karyotype with 46 XX, t(9;12)(p22;q14). While the translocation of 12q14 in our patient does coincide with prior anomalies found in IVL, there have only been two other reports of uterine leiomyomas with translocation of chromosomes 9 and 12 in the literature, both with t(9;12)(p22;q15) [24, 25]. Of note, our patient’s cytogenetic abnormality has been previously reported in only three lipomas and one myolipoma, which is interesting considering the coexistence of lipoleiomyoma in this case [26-29]. Long-term surveillance of patients with IVL is important due to the potential for recurrence. Recurrence of IVL has been reported to range from 0.0% to 50.0% (Table 1) [1, 9, 17, 30-35]. The largest retrospective study of 58 cases from a referral center in China found an association with IVC involvement and recurrence (OR 13.33, 2.68-66.26) in patients who had complete resection of tumor, but no association between age >50 years old, adjuvant hormonal therapy, hysterectomy vs tumor resection, or ovarian conservation. [34] Smaller case series have suggested association between patient age <40 years old, [1] myomectomy instead of hysterectomy [1, 31], and complete resection of tumor [31, 36].
Although IVL is a benign neoplasm, the potential for fatal obstruction of the heart or pulmonary vasculature warrants monitoring for recurrence. One study reviewed atypical histologic variants of IVL (including two cases of LPL) and concluded that histologically benign tumors with intravenous involvement should be managed and monitored in the same manner as typical IVL [9]. Different modalities and frequencies of surveillance have been suggested by different authors, but, most are in agreement that serial imaging is indicated [1, 34, 37, 38].
Lipoleiomyoma presenting with intravascular extension is exceedingly rare. A total of 8 were identified in the English literature since 1988 [6-11]. Lipoleiomyomas are uncommon variants of smooth muscle tumors with a mixture of smooth muscle and mature adipose tissue and no significant nuclear atypia. While there have been a few case reports describing malignant transformation into sarcomas [39, 40], LPL are benign by definition and are managed similar to typical leiomyomas. Imaging findings for IVL or LPL have some classic findings. Intravenous leiomyomatosis beyond the pelvis is most often identified as a continuous, heterogeneous mass originating in the pelvis and extending to the IVC [3, 41]. While IVL that has progressed to the main vasculature is often apparent on imaging, early disease may have less obvious findings or even sub-centimeter vascular involvement that is not visible. One series noted that approximately two thirds of the 22 cases they evaluate had either minimal vascular involvement (≤3mm) or vascular involvement limited to the myometrium [32].
Lipoleiomyoma may have a variable appearance on imaging, which makes radiologic diagnosis sometimes difficult. Ultrasound studies may demonstrate a hyperechoic mass surrounded by a thin, hypoechoic ring of normal myometrium [42, 43]. This presentation is more typical of LPL and may facilitate preoperative diagnosis [44]. Lipoleiomyoma can also present as a heterogeneous uterine mass with less clear margins. Using fat suppression techniques with MRI may help demonstrate the presence of both adipose and non-adipose tissue, but a histologic diagnosis would be necessary to evaluate for a possible liposarcoma [45, 46].
This case is the first to provide serial imaging of intravenous lipoleiomyomatosis over years and additionally provides cytogenetic information that corroborates prior studies.
References
- Du J, et al. Intravenous leiomyomatosis of the uterus: a clinicopathologic study of 18 cases with emphasis on early diagnosis and appropriate treatment strategies. Hum Pathol 42 (2011): 1240-1246.
- Murphy AN, et al. Intravenous leiomyomatosis manifesting as saddle embolism. BMJ Case Rep 12 (2019).
- Gui T, et al. Computerized tomography angiography in preoperative assessment of intravenous leiomyomatosis extending to inferior vena cava and heart. BMC Cancer 16 (2016): 73.
- Zhang H, et al. Giant intravenous leiomyomatosis with intracardiac extension. Ann Thorac Surg 94 (2012): 1013.
- Grella L, et al. Intravenous leiomyomatosis. J Vasc Surg 20 (1994): 987-994.
- Dolgun ZN, et al. Incidental intravascular lipoleiomyomatosis in a hysterectomy specimen: how to manage? J Clin Diagn Res 9 (2015): QD07-8.
- Hashiguchi J, et al. Intravascular Leiomyomatosis with Uterine Lipoleiomyoma. Gynecol Oncol 52 (1994): 94-98.
- Bilyeu S.P, J.D. Bilyeu and R. Parthasarathy Intravenous lipoleiomyomatosis. Clin Imaging 30 (2006): 361-364.
- Clement PB, Young RH, Scully RE. Intravenous leiomyomatosis of the uterus. A clinicopathological analysis of 16 cases with unusual histologic features. Am J Surg Pathol 12 (1988): 932-945.
- Vural C, Ozen O, Demirhan B. Intravenous lipoleiomyomatosis of uterus with cardiac extension: a case report. Pathol Res Pract 207 (2011): 131-134.
- Brescia RJ, et al. Intravascular lipoleiomyomatosis: a report of two cases. Human pathology 20 (1989): 252-256.
- Dürk H, Ueber ein kontinvierlich durch die entere Hohlvene in das Herz vorwachsendes. Fibroma des Uterus. MMW 54 (1907): 1154.
- Hormann K, Ueber einen fall von myomatosem uterustumor. Zentralbl Gynaekol 51 (1907): 1604-1605.
- Roman D, Mirchandani H. Intravenous leiomyoma with intracardiac extension causing sudden death. Archives of pathology & laboratory medicine 111 (1987): 1176-1178.
- Knauer E, Beitrag zur anatomie der uterusmyome. Beitr z Geburtsh u Gynak 1 (1903): 695.
- Sitzenfrey A, Ueber venenmyome des uterus mit intravaskularem wachstum. Z. Geburtshulfe Gynakol 68 (1911): 1-25.
- Tang L, Lu B. Intravenous leiomyomatosis of the uterus: A clinicopathologic analysis of 13 cases with an emphasis on histogenesis. Pathol Res Pract 214 (2018): 871-875.
- Kir G, et al. Estrogen and progesterone expression of vessel walls with intravascular leiomyomatosis; discussion of histogenesis. Eur J Gynaecol Oncol 25 (2004): 362-366.
- Dal Cin P, et al. Intravenous leiomyomatosis is characterized by a der(14)t(12;14)(q15;q24). Genes Chromosomes Cancer 36 (2003): 205-206.
- Ordulu Z, et al. Intravenous leiomyomatosis: an unusual intermediate between benign and malignant uterine smooth muscle tumors. Mod Pathol 29 (2016): 500-510.
- Quade BJ, et al. Intravenous leiomyomatosis: molecular and cytogenetic analysis of a case. Mod Pathol 15 (2002): 351-356.
- Havel G, et al. Cytogenetic relationship between uterine lipoleiomyomas and typical leiomyomas. Virchows Arch B Cell Pathol Incl Mol Pathol 57 (1989): 77-79.
- Hu J, Surti U, Tobon H. Cytogenetic analysis of a uterine lipoleiomyoma. Cancer Genet Cytogenet 62 (1992): 200-202.
- Kiechle-Schwarz M, et al. Nonrandom cytogenetic changes in leiomyomas of the female genitourinary tract: a report of 35 cases. Cancer genetics and cytogenetics 53 (1991): 125-136.
- Kataoka S, et al. Cytogenetic analysis of uterine leiomyoma: the size histopathology and GnRHa-response in relation to chromosome karyotype. European Journal of Obstetrics & Gynecology and Reproductive Biology 110 (2003): 58-62.
- Italiano A, et al. NFIB rearrangement in superficial retroperitoneal and colonic lipomas with aberrations involving chromosome band 9p22. Genes Chromosomes Cancer 47 (2008): 971-977.
- Lacaria M, El Demellawy D, McGowan-Jordan J. A rare case of pediatric lipoma with t(9;12)(p22;q14) and evidence of HMGA2-NFIB gene fusion. Cancer Genet 216-217 (2017): 100-104.
- Panagopoulos I, et al. Fusion of the HMGA2 and C9orf92 genes in myolipoma with t(9;12)(p22;q14). Diagn Pathol 11 (2016): 22.
- Pierron A, et al. HMGA2-NFIB fusion in a pediatric intramuscular lipoma: a novel case of NFIB alteration in a large deep-seated adipocytic tumor. Cancer Genet Cytogenet 195 (2009): 66-70.
- Carr R.J, Hui and N. Buza Intravenous leiomyomatosis revisited: an experience of 14 cases at a single medical center. Int J Gynecol Pathol 2015. 34(2): 169-76.
- Low HY, et al. Intravenous leiomyomatosis of the uterus: A clinicopathological analysis of nine cases and literature review. Taiwan J Obstet Gynecol 56 (2017): 362-365.
- Mulvany NJ, et al. Intravenous leiomyomatosis of the uterus: a clinicopathologic study of 22 cases. Int J Gynecol Pathol 13 (1994): 1-9.
- Norris HJ, Parmley T. Mesenchymal tumors of the uterus. V. Intravenous leiomyomatosis. A clinical and pathologic study of 14 cases. Cancer 36 (1975): 2164-2178.
- Yu X, et al. Factors Associated With Recurrence After Surgical Resection in Women With Intravenous Leiomyomatosis. Obstet Gynecol 128 (2016): 1018-1024.
- Nogales FF, et al. Uterine intravascular leiomyomatosis: an update and report of seven cases. Int J Gynecol Pathol 6 (1987): 331-339.
- Wang J, et al. Management of intravenous leiomyomatosis with intracaval and intracardiac extension. Obstet Gynecol 120 (2012): 1400-1406.
- Valdes Devesa V, et al. Update on intravenous leiomyomatosis: report of five patients and literature review. Eur J Obstet Gynecol Reprod Biol 171 (2013): 209-213.
- Castagneto Gissey L, et al. Massive pelvic recurrence of uterine leiomyomatosis with intracaval-intracardiac extension: video case report and literature review. BMC Surg 17 (2017): 118.
- McDonald AG, et al. Liposarcoma arising in uterine lipoleiomyoma: a report of 3 cases and review of the literature. Am J Surg Pathol 35 (2011): 221-227.
- Scurry J, Hack M. Leiomyosarcoma arising in a lipoleiomyoma. Gynecol Oncol 39 (1990): 381-383.
- Wang H, et al. Contrast-enhanced CT findings of intravenous leiomyomatosis. Clin Radiol 73 (2018): 503 e1-503 e6.
- Villanueva AJ, et al. Uterine myolipoma: CT and US. Abdom Imaging 18 (1993): 402-403.
- Johari B, et al. Lipoleiomyoma: a rare benign tumour of the uterus. BMJ Case Rep (2014).
- Tyagi N, Tyagi R, Griffin Y. Uterine lipoleiomyoma. BMJ Case Rep (2014).
- Fujiwaki R, et al. Uterine lipoleiomyoma in an elderly patient: a case report. Arch Gynecol Obstet 277 (2008): 471-474.
- Prieto A, et al. Uterine lipoleiomyomas: US and CT findings. Abdominal Imaging 25 (2014): 655-657.


 Impact Factor: * 4.1
Impact Factor: * 4.1 Acceptance Rate: 74.74%
Acceptance Rate: 74.74%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 