Pediatric Non-Functional Retroperitoneal Paragangilioma: A Rare Case Report
Abdishakur Mohamed Abdi*, Ismail Haki Gol, Abdullah yusuf Ali
Mogadishu Somali Turkish Training and Research Hospital; Mogadishu, Somalia
*Corresponding Author: Abdishakur Mohamed Abdi, Mogadishu Somali Turkish Training and Research Hospital; Mogadishu, Somalia
Received: 29 December 2021; Accepted: 14 January 2022; Published: 02 June 2022
Article Information
Citation: Abdishakur Mohamed Abdi, Ismail Haki Gol, Abdullah yusuf Ali. Pediatric Non-Functional Retroperitoneal Paragangilioma: A Rare Case Report. Journal of Cancer Science and Clinical Therapeutics 6 (2022): 234-238.
View / Download Pdf Share at FacebookAbstract
Extra-adrenal paragangiliomas are uncommon neuroendocrine neoplasms with frequency 2-8 per million cases. They have an inclination to be malignant more than pheochromocytomas. Here we present a case of nonfunctional extra adrenal retroperitoneal paraganilioma occurring in 16-year-old male patient presented to with complaints of abdominal pain and heavens on the left hypochondria, CT scan revealed a retroperitoneal gross mass lesion measuring 114 × 99mm in the axial plane, extending from the upper quadrant level of the abdomen towards the inferior and containing necrotic areas in the central part. The mass was surgically removed successfully without intraoperative complications. Postoperative period was uneventful and patient discharged on day 7. Careful preoperative preparation and planning is mandatory as nature of tumor is endocrine tumor which secrete certain hormones and sudden rise or fall serum level of those hormones can result life threatening hypertension or hypotension. Full precaution must be taken to avoid these severe complications.
Keywords
<p>Pediatric; Retroperitoneal; Paragangilioma; Neuroendocrine; Neoplasms</p>
Article Details
1. Introduction
Extra-adrenal paragangiliomas are uncommon neuroendocrine neoplasms with frequency 2-8 per million cases [1]. They emerge from neural peak cells and are composed of primarily of chromaffin cells found within the Para aortic sympathetic chain, they synthesize, store and discharge catecholamine’s [1]. Patient may present with headache, diaphoresis and palpitation and high blood pressure. On the other hand they may remain unnoticed, nonfunctional or nonspecific symptoms such as abdominal pain due to periodic release of catecholamine’s. Wen J, et al. Reported that histologically and immunochemically no difference between silent and functional tumors [2]. Essential strategies of preoperative determination include incorporate imaging procedures which guides surgical arranging and preoperative planning. Silent tumors often failed to detect preoperatively and present complications intraoperative. In 95% of the cases of extra-adrenal paragangiliomas are located within the abdominal regions, but they will also occur within the head, neck and thoracic regions. McNicol AM. Reported that extra-adrenal paragangiliomas have an inclination to be malignant more than pheochromocytomas [3]. There are few case reports regarding non-functional extra-adrenal paragangiliomas; the literature is scarce for the early diagnosis and optimal preoperative and intraoperative management. This case report is aimed to highlight the clinical presenatation, diagnosis and treatment outcomes of a case of non-functional extra-adrenal retroperitoneal paraganilioma in 16-years male patient successfully managed with complete surgical resection.
2. Case Report
A 16-year-old male patient presented to pediatric surgery department with complaints of abdominal pain and heavens on the left hypochondria. There was no history of vomiting or altered bowel habits or previous history of similar attacks. The patient was not a known hypertensive and was not on any medication. Per abdominal examination revealed tenderness and a mass in the left hypochondriac region which did not move with respiration. Bowel sounds and rectal examination were normal, contrast ct scan revealed a retroperitoneal gross mass lesion measuring 114 × 99mm in the axial plane, extending from the upper quadrant level of the abdomen towards the inferior and containing necrotic areas in the central part, mass lesion extends to the mid abdomen, there is no calcification in it. There is heterogeneous contrast enhancement in post contrast images. The lesion is hypervascular Figure 1. Laboratory profiles were normal. Transverse left subcostal incision was undertaken for exploration. a retroperitoneal mass was found inferior to the renal vein on the left side of aorta occupying 2nd, 3rd and 4th lumbar vertebral levels. The tumour was adjacent tp the aorta. The ureter was pushed anteriorly while the inferior mesenteric vessels were pushed laterally. There was abundant direct vascular connection from aorta supplying the mass. The mass was found located ventral to the sympathetic and lymphatic chain. During dissection of the mass several veins brusted and ligated. With careful dissection the mass was completely resected (Figure 2).
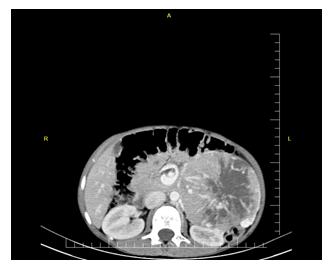
Figure 1: Gross mass lesion measuring 114 × 99mm in the axial plane, with central necrosis.
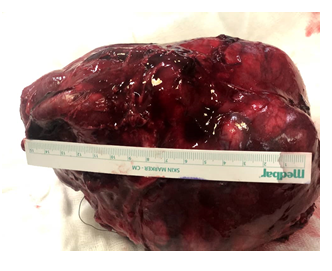
Figure 2: Completely resected paragangilioma.
Histopathological Findings
Gross examination
Consistent cut surface prefer grey white centrally pinkish soft with focal myxoid hemorrhagic changes.
Microscopy
Procedure: Borderline resection
Tumor Site: Retro peritoneum
Tumor Size: 13x10x7 cm
Histologic Type: Paraganglioma
Mitotic Rate: 3/10 HPF
Necrosis: Present (<5%)
Histologic Grade: Intermediate Behavior
Margins: All margins negative for tumor but borderline appearance.
Lymphovascular Invasion: Not identified
Histopathologic diagnosis: retroperitoneal paragangilioma, intermittent behavior.
3. Discussion
Paragangiliomas can develop anywhere along the midline of the retro peritoneum. The precise incidence of retroperitoneal paragangiliomas is unknown, although male are typically affected more than females. Additionally most patients are diagnosed between 30 and 45 years old Masahiro Shibata. Reported A 24-year-old female presented to the regional hospital with complaints of hyperhidrosis and hypertension [4]. In the current case we report a case of non-functional extra-adrenal retroperitoneal paraganilioma in a 16-years male patient successfully managed with complete surgical resection. Clinically, patients with retroperitoneal paragangilioms often present with back pain or palpable mass. Conventional treatment for paragangiliomas typically involves complete surgical excision, while surgical debunking is taken into account as mainstay of palliative therapy for malignant paragangiliomas [2]. In some cases complete excision is sometimes not feasible due to highly vascular characteristics of the paragangiliomas and their closeness to the major blood vessels. Abdominal paragangiliomas are mostly located in the retro peritoneum, overall 85% of the extra-adrenal paragangiliomas. The foremost common site of retroperitoneal paragangiliomas occurs between origin of inferior mesenteric c artery and aortic bifurcation and it is known as organ of zuckerkandl. paragangilioma originating from the jugulotympanic body are called chemodectomas While paragangilioma arising from chemoreceptor are referred to as chemoreceptor tumors. Paragangiliomas residing in the second part of the duodenum are called gangiliocytic paragangilioma [5]. functional paragangiliomas are diagnosed by its clinical presentation and laboratory results showing raised level of catecholamine’s and their byproduct within the urine and blood whereas nonfunctional paragangiliomas are commonly found incidentally or present as mass with compression symptoms of the organ it compresses [6].
4. Conclusion
Extra adrenal retroperitoneal paragangiliomas are uncommon neoplasms which pause difficult in diagnosis and treatment. However careful preoperative preparation and planning is mandatory as nature of tumor is endocrine tumor which secretes certain hormones and sudden rise or fall serum level of those hormones can result life threatening hypertension or hypotension. Full precaution must be taken to avoid these severe complications.
References
- Nancy Perrier, Alexandria Phan, Steven Waguespack, et al. Clinical Benefits of Systemic Chemotherapy for Patients with Metastatic Pheochromocytomas or Sympathetic Extra-Adrenal Paragangliomas. Cancer 1 (2012): 2805.
- Wen J, Li HZ, Ji ZG, et al. A decade of clinical experience with extra-adrenal paragangliomas of retroperitoneum: Report of 67 cases and a literature review. Urology annals 2 (2010): 12.
- McNicol AM. Update on tumours of the adrenal cortex, phaeochromocytoma and extra?adrenal paraganglioma. Histopathology 58 (2011): 155-168.
- Shibata M, Inaishi T, Miyajima N, et al. Synchronous bilateral pheochromocytomas and paraganglioma with novel germline mutation in MAX: a case report. Surgical case reports 3 (2017): 1-5.
- Mete O, Tischler AS, De Krijger R, et al. Protocol for the examination of specimens from patients with pheochromocytomas and extra-adrenal paragangliomas. Archives of Pathology and Laboratory Medicine 138 (2014): 182-188.
- Tischler AS, Pacak K, Eisenhofer G. The adrenal medulla and extra-adrenal paraganglia: then and now. Endocrine pathology 25 (2014): 49-58.


 Impact Factor: * 4.1
Impact Factor: * 4.1 Acceptance Rate: 74.74%
Acceptance Rate: 74.74%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 