The Role of Intra-Operative Mobile Gamma Camera and Gamma Probe in Detection of Sentinel Lymph Node in Early Stage Breast Cancer
Maher H Ibraheem1*, Mohamed Gamil2, Ahmed Tantawy3, Omnia Talaat4, Rimoun Boutrrus5, Mohammed Mohammed Mohammed Gomaa6
1Lecturer of Surgical Oncology, National Cancer Institute, Cairo University, Egypt
2Professor of Surgical Oncology, National Cancer Institute, Cairo University, Egypt
3Associate Lecturer of Surgical Oncology, National Cancer Institute, Cairo University, Egypt
4Lecturer of Nuclear Medicine, National Cancer Institute, Cairo University, Egypt
5Lecturer of Radiotherapy, National Cancer Institute, Cairo University, Egypt
6Lecturer of Radiodiagnosis, National Cancer Institute, Cairo University, Egypt
*Corresponding Author: Maher H Ibraheem, Lecturer of Surgical Oncology, National Cancer Institute, Cairo University, Egypt
Received: 22 August 2019 Accepted: 30 September 2019 Published: 07 October 2019
Article Information
Citation: Maher H Ibraheem, Mohamed Gamil, Ahmed Tantawy, Omnia Talaat, Rimoun Boutrrus, Mohammed Mohammed Mohammed Gomaa. The Role of Intra-Operative Mobile Gamma Camera and Gamma Probe in Detection of Sentinel Lymph Node in Early Stage Breast Cancer. Journal of Cancer Science and Clinical Therapeutics 3 (2019): 229-239.
View / Download Pdf Share at FacebookAbstract
Background: The use of intraoperative mobile gamma camera that provide real-time intraoperative images of the sentinel lymph node (SLN), in combination with hand held gamma probe, is assumed to increase the accuracy of yielding the SLN, in early breast cancer patients, with more proper site localization.
Purpose: To assess the added value of intraoperative mobile gamma camera in combination with hand held gamma probe in detection of SLN(s) in early stage breast cancer patients.
Methods: It was a prospective study on 30 patients, with breast cancer scheduled SLN. biopsy in the National Cancer Institute, Cairo University, Egypt. From January 2015 till December 2015. A new device (intraoperative mobile gamma camera) was used in conjunction with a gamma probe in early stage breast cancer patients.
Results: The hand held gamma probe detected SLNs in 28 out of 30 (93.4%) patients, while the intraoperative mobile gamma camera detected SLN(s) in 29 patients out of 30 (96.7%) patients. In total, 59 SLNs were found using the gamma probe, and 62 SLNs were found using the mobile gamma camera. For patients whom underwent a SLNB, the pain in axilla ranged from 1 to 3, while the severity reached 6 and 7 in the two patients who underwent axillary dissection.
Conclusion: The use of intraoperative mobile gamma camera in conjunction with the handheld gamma probe resulted in a higher SLN detection rate, made the SLNB more accurate with proper site localization, either axillary or extra axillary sites and with less complications.
Keywords
<p>SLN; Intraoperative mobile gamma camera; Gamma probe; Breast cancer</p>
Article Details
1. Introduction
Breast cancer is the most common cancer in women. In 2012, it comprised 25.2% of cancers diagnosed in women [1]. Axillary staging is one of the most important prognostic factors in all invasive breast cancer, and imperative for prognosis, regional treatment and local control according to NCCN guidelines [2]. Axillary lymph node dissection was considered the key step for evaluating axillary lymph node status, and it was routine for any patient with invasive breast cancer [3]. After wide implementation early detection protocols for breast cancer, the probability of nodal metastasis has markedly been decreased. Lymphatic mapping with sentinel lymph node biopsy (SLNB) has markedly replaced axillary lymph node dissection in those with clinically and radiologically negative axillae [4]. So, the use of SLNB, added the advantages of limiting the associated morbidities with axillary dissection, including, arm pain, sensory deficit of arm pit and medial side of the arm, limited range of motion at the shoulder level, axillary seroma and the most serious complication is the upper limb lymphedema [5]. The use of intraoperative mobile gamma camera that provide real-time intraoperative images of the SLNs, which can be used in combination with hand held gamma probe, is assumed to increase the accuracy of yielding the SLNs, with proper site localization, either axillary or extra axillary sites like, internal mammary or infra clavicular region [6].
2. Purpose
The aim of the study is to assess the added value of intraoperative mobile gamma camera in combination with hand held gamma probe in detection of sentinel lymph node SLN(s) in early stage breast cancer patients
3. Patients and Methods
This a prospective study on 30 breast cancer patients whom were operated upon, in the National Cancer Institute (NCI) Cairo University, (Egypt). From January 2015 till December 2015, these patients were operated with the following inclusion criteria: Pathologically proven early stage breast cancer with clinically and radiologically negative axillary nodes (T1, T2, N0, M0). Exclusion criteria were: Patients who underwent previous axillary surgery or radiation, excision of the tumor without axillary staging for more than three months or patients who received neoadjuvant chemotherapy. All patients underwent preoperative patient assessment including full medical history, physical examination, breast imaging, preoperative pathology, routine laboratory investigations, anesthesia assessment. Informed consent was taken from all patients.
4. Methods
Technetium-99m albumin nano colloid (99 mTc-nanocolloid) (500 μCi in a volume of 0.3-0.5 ml) was injected peri-areolar sub-dermal corresponding to site of the lesion 12-24 hours prior to operative time (Figure 1).
Intraoperatively, prior to sterilization, the mobile gamma camera was placed at distance of 15 cm to acquire an overview image of the breast and axilla and to assess radioactive uptake by the SLN(s) either axillary or internal mammary, or infraclavicular region location. (Figure 2). Then this detector was placed nearer to the field to precisely localize the detected SLN uptake using a cross laser pointer on the field that is matched to the hotspot on the camera screen and the location was marked on the patient’s skin. The gamma probe was used to confirm the proper site of the SLN after scanning the axilla, internal mammary region, and infraclavicular region (Figure 3).
During surgery, the arm of the mobile gamma camera was sterile draped allowing the placement and movement above the surgical field by the surgeon. Surgical incision was done guided by the skin marks (Figure 4). In some cases the breast tumor, radiotracer injection site, was located close to the SLN. The gamma probe was in these situations not able to locate the SLNs due to the radioactive noise from the highly radioactive injection site. The ‘masking’ functionality
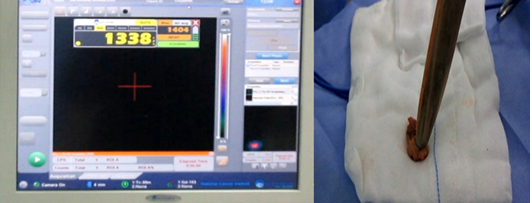
of the mobile gamma camera was used to virtually shield the highly radioactive injection site and improve the SLN localization and visualization close to the injection site (Figure 5). After incision, the hand held gamma probe was used to detect and excise the lymph nodes with high tracer uptake (high count), which were considered the SLNs (Figure 6). After retrieval of a lymph node, the mobile gamma camera was used in conjunction with the gamma probe to confirm ex vivo that the lymph node contained radioactivity (Figure 7). Finally, the surgical field was checked again using the mobile gamma camera and hand held gamma probe to confirm that all radioactive nodes have been removed (Figure 8). The retrieved SLN(s) were sent for frozen section and paraffin section to assess the pathology result. Early postoperative follow up of the patients regarding; axillary and arm pain, sensory changes, seroma, was recorded. Pain assessment was done using a patient questionnaire according to the Numeric Rating Scale of pain (NRS-11), which is an 11-point scale for patient self-reporting of pain (Table 1).
|
Pain level |
|
|
0 |
No pain |
|
1-3 |
Mild pain (nagging, annoying, interfering little with daily life activities). |
|
4-6 |
Moderate pain (interferes significantly with daily life activities). |
|
7-10 |
Severe pain (disabling; unable to perform daily life activities). |
Table 1: Pain assessment scoring according to NRS-11.
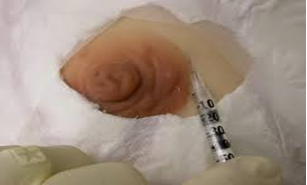
Figure 1: Peri areolar sub-dermal injection of radio-colloid.
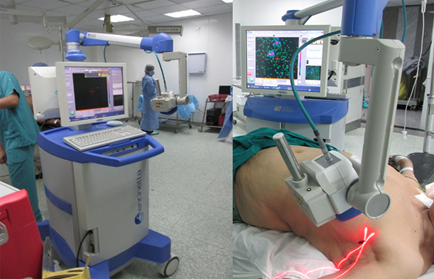
Figure 2: Rapid pre-operative scanning, to properly localize the site of the SlN.
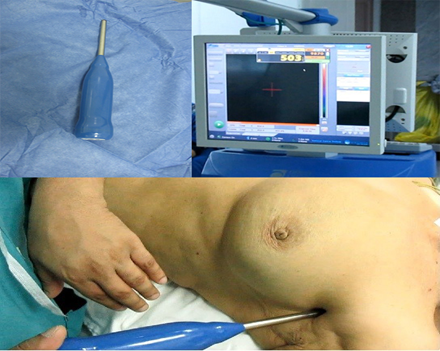
Figure 3: Gamma probe used in SLN detection pre operatively with corresponding high count on the screen.
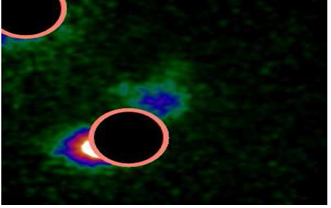
Figure 5: The ‘masking’ functionality of the mobile gamma camera was used to virtually shield the highly radioactive injection site.
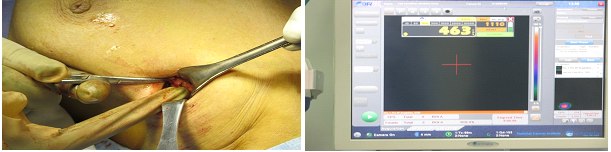
Figure 6: Gamma probe inside surgical field detecting the SLN, with high count on the screen.
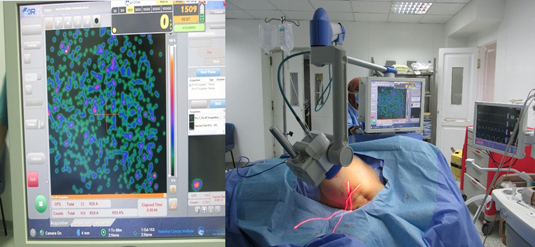
Figure 8: Intra-operative gamma camera scanning the surgical field after SLN excision without any radio activity on the screen.
5. Results
5.1 Patient characteristics
Patients' age ranged from 27-67 years with the mean age at 48.7 (± SD 10.9). Among these patients, 57% were post-menopausal and 43% were premenopausal. 13.3% of the patients had family history of breast cancer. The tumor was located in the upper outer quadrant in 73%, in the upper inner quadrant in 6.7%, in the lower inner quadrant in 10%, in the lower outer quadrant in 6.7%, and central quadrant in 3.3% of the patients. The Pathology of these tumors were; IDC in 24 patients (~ 80%), ILC in 3 patients (~10%), mixed IDC & ILC in 2 patients (~6.6%), DCIS in one patient (~3.4%). Two (~7%) patients had done previous lumpectomy as excisional biopsy not more than 3 months before SLNB operation. CBS have been done for 26 patients (~86.7%) while 4 patients (~13.3) underwent mastectomy.
5.2 Intraoperative findings
The hand held gamma probe detected SLNs in 28 out of 30 patients (93.4%), while the intraoperative mobile gamma camera detected SLN(s) in 29 out of 30 patients (96.7%). The real time gamma camera images helped to retrieve 62 SLNs, while the gamma probe detected only 59 SLNs. 2 out of the three additional SLNs were found in a patient in whom the gamma probe couldn`t detect any SLNs. One of these 3 additional SLNs detected by the mobile gamma camera was found in a patient where already another SLN was found. In total, 61 axillary SLNs and one intramammary SLN was found (Table 2).
The most frequently detected number of SLNs in each patient was 2 SLNs in 15 patients (~50%). One SLN was detected 7 patients (~23.3%), 3 SLNs were detected in 4 patients (~13.3%), and 5 SLNs were detected in one patient (~3.3%) (Figure 9).
Frozen section results of detected SLN(s) were negative in 27 out of 29 patients. Micro metastases were found in one patient. In these 28 patients, only the SLNB was performed. In one patient the detected SLNs (3/3) were positive. Axillary lymph node clearance was done in both this patient with positive nodes and in the patient in whom no SLNs could be located (Table 3). The paraffin results of the detected SLN(s) showed similar results as the frozen sections except in one patient in whom a negative SLN appeared to harbor isolated tumor cells. There were no nodal metastases found in the two patient who underwent an axillary lymph node clearance.
5.3 Pain assessment
Post-operative axillary pain assessment for patients who only underwent SLNB ranged from score 1 to 3 (28 patients) and the severity reached score 6 and 7 (2 patients) in patients who underwent axillary clearance (Table 4). One patient out of the 28 who underwent only SLNB reported post-operative numbness at medial side of the arm while both patients who underwent axillary clearance reported numbness at medial side of the arm. Post-operative seroma was reported in one of the 28 patients who underwent only SLNB and for whom no surgical drains were inserted in the axilla. No post-operative seroma was reported in patients who underwent axillary clearance, however in both patients an axillary drain was inserted.
|
SITE of |
Type of axillary surgery |
||||||
|
Sentinel lymph |
Axillary Clearance |
Total |
|||||
|
N |
% |
N |
% |
N |
% |
||
|
Not located |
0 |
0.0 |
1 |
3.3 |
1 |
3.3 |
|
|
Axilla |
27 |
90.0 |
1 |
3.3 |
28 |
93.3 |
|
|
Axilla and intramammary |
1 |
3.3 |
0 |
0.0% |
1 |
3.3 |
|
|
Total |
28 |
93.3 |
2 |
6.7 |
30 |
100.0 |
|
|
Chi-square |
X2 |
14.483 |
|||||
|
P-value |
0.000 |
||||||
Table 2: Site of detected SLN and type of axillary surgery.
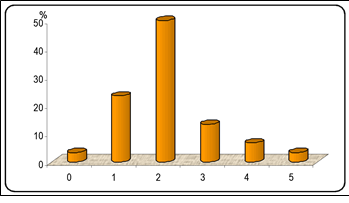
Figure 9: Frequency of detected SLNs in each patient.
|
Frozen |
Type of axillary |
||||||
|
Sentinel lymph |
Axillary |
Total |
|||||
|
N |
% |
N |
% |
N |
% |
||
|
Negative |
27 |
90.0 |
0 |
0.0 |
27 |
90.0 |
|
|
Positive |
0 |
0.0 |
1 |
3.3 |
1 |
3.3 |
|
|
Not done |
0 |
0.0 |
1 |
3.3 |
1 |
3.3 |
|
|
Micrometastases |
1 |
3.3 |
0 |
0.0 |
1 |
3.3 |
|
|
Total |
28 |
93.3 |
2 |
6.7 |
30 |
100.0 |
|
|
Chi-square |
X2 |
30.000 |
|||||
|
P-value |
<0.001* |
||||||
Table 3: Frozen results of SLN and type of axillary surgery.
|
Pain |
Type of axillary |
||||||
|
Sentinel lymph |
Axillary clearance |
Total |
|||||
|
N |
% |
N |
% |
N |
% |
||
|
1 |
9 |
30.0 |
0 |
0.0 |
9 |
30.0 |
|
|
2 |
9 |
30.0 |
0 |
0.0 |
9 |
30.0 |
|
|
3 |
10 |
33.3 |
0 |
0.0 |
10 |
33.3 |
|
|
4 |
0 |
0.0 |
0 |
0.0 |
0 |
0 |
|
|
5 |
0 |
0.0 |
0 |
0.0 |
0 |
0 |
|
|
6 |
0 |
0.0 |
1 |
3.3 |
1 |
3.3 |
|
|
7 |
0 |
0.0 |
1 |
3.3 |
1 |
3.3 |
|
|
Total |
28 |
93.3 |
2 |
6.7 |
30 |
100.0 |
|
|
Chi-square |
X2 |
30.000 |
|||||
|
P-value |
<0.001* |
||||||
Table 4: Pain assessment according to (NRS-11).
6. Discussion
The SLNB has become the standard of care for early stage breast cancer in clinically and radiologically negative axilla as the main detector of nodal metastases according to NCCN guidelines [2]. Nowadays, a mobile intraoperative gamma camera is developed that gives a rapid intraoperative real time image of the SLN that can replace the preoperative conventional gamma camera images [8].
In our study, the SLN detection and identification rate was 96.7%. The SLN(s) wasn`t localized in only one out of 30 patients with the use of the mobile gamma camera. With the hand held gamma probe alone, the detection rate was 93.4%. The gamma probe did not detect SLNs in two patients. The real time images helped to retrieve 62 SLNs in 29 patients, while the gamma probe detected only 59 SLNs. Although, we cannot assume independence of the two techniques in our study and the difference is minimal, however the better performance of the gamma camera over the gamma probe was demonstrated by Goni et al. who reported in 754 patients, who had undergone a SLNB in the period between January 2003 and December 2011, an improved SLN detection rate using the mobile gamma camera [9].
In October 2009, a mobile gamma camera was introduced in the surgical procedure, Group 1 consisted of 501 patients in which the procedure was performed using only a gamma probe. Group 2 consisted of 253 patients in which the SLN biopsy was performed using both the mobile gamma camera and a gamma probe. The SLN identification rate was improved from 94.6 to 99.2 % in groups 1 and 2, respectively. The authors concluded that this achievement can be explained by the experience and that the introduction of the intraoperative imaging plays an important role as well [9]. Lombardi et al. reported that radio-guided axillary SLNB was successful in 184/186 patients (99 %) with the use of intraoperative mobile gamma camera [10]. Additionally, a study in 16 patients showed that the mobile gamma camera detected more SLNs than conventional gamma camera imaging and gamma probe usage in 5/16 patients [11].
In addition, the mobile gamma camera didn`t miss any residual radioactive nodes thanks to the post-excision images of the surgical field. These images scan the surgical field for any residual radioactivity. This can particularly be important when the SLN is located near the injection site as intramammary SLNs. This is compatible with what was concluded by Lombardi A et al., Motomura K et al. and Vidal-Sicart S et al. and all who used intraoperative gamma camera imaging which helped them to ensure the absence of any residual activity in the surgical field with the help of post-excision images [10, 12, 13].
The frozen section results of all detected SLNs nearly the same as the paraffin results, except for one SLN that contained isolated tumor cells. However, this did not affect the patient management and no patient needed a second operation. This was in contrast with another study performed in 25 patients. In this study, the SLN(s) in 4 patients were metastatic by paraffin section while these were negative during the frozen pathological examination. These 4 patients underwent delayed axillary clearance in a second setting [8]. In a randomized multicenter study (ALMANAC trial), comparing SLNB vs axillary lymph node dissection (ALND) in operable breast cancer patients, was reported that only small number of patients who underwent SLNB needed surgical drain insertion (17%), while most of patient who underwent ALND needed surgical drain insertion (79%) [14].
In our study, the mobile gamma camera helped 28 out of 30 (~93.3%) patients to avoid surgical drain insertion in the axilla which is markedly annoying for the patients and carry the risk of infection. One of the patients developed post-operative seroma in the axilla. The wound size of SLNB ranged from 2-3 cm, while the wound size of axillary dissection was nearly 7cm. This was thanks to the precise localization of the SLN using the intraoperative gamma camera prior to incision and the complementary use of the hand held gamma probe. Thus, resulted in better cosmetic outcome. The same wound size was reported in a study on 163 breast cancer patients who underwent SLNB using radio guided detection with a gamma probe and preoperative lymphoscintigraphy [15].
Patients who underwent SLNB alone experienced mild pain with score ranged from 1-3 out of 10, while patients who underwent axillary clearance experienced moderate to severe pain in the axilla with a score ranged from 6-7 according to the numeric pain scoring system (NRSS) [7].
7. Conclusion
The real time imaging of the SLNs using an intraoperative mobile gamma camera in combination with the hand held gamma probe results in a high SLN detection rate, made the SLNB more accurate with proper site localization, either axillary or extra axillary sites and less time consuming with less complications in breast cancer patients. Basically, the mobile gamma camera brings the nuclear medicine department to the operating room. This simplifies the surgical planning, because the surgical schedule does not need to depend on the preoperative lymphoscintigraphy planning, using a conventional gamma camera, at the Nuclear Medicine department.
References
- World Cancer Report. International Agency for Research on Cancer, World Health Organization (2014).
- National Comprehensive Cancer Network (NCCN). NCCN Clinical practice guidelines in oncology (2016).
- Gatti A, Ballardini G, et al. Development of axillary surgery in breast cancer Ann Oncol 2 (2005): 259-262.
- Veronesi U, Paganelli G, Viale G, et al. A randomized comparison of sentinel-node biopsy with routine axillary dissection in breast cancer. N Engl J Med 6 (2003): 546-553.
- Krag D, Anderson S, Julian T, et al. Sentinel-lymph-node resection compared with conventional axillary-lymph-node dissection in clinically node-negative patients with breast cancer: overall survival findings from the NSABP B-32 randomised phase 3 trial. Lancet Oncol 11 (2010): 927-933.
- Bricou A, Charon Y, Barrangerc E, et al. Mobile gamma cameras in breast cancer care EJSO 39 (2013): 409-416.
- Hartrick C, Kovan J, Shapiro S. The numeric rating scale for clinical pain measurement: a ratio measure. Pain Practice 4 (2003): 310-316.
- Mathelin C, Salvador S, Huss D, et al. Precise localization of sentinel lymph nodes and estimation of their depth using a prototype intraoperative mini gamma-camera in patients with breast cancer. J Nucl Med 48 (2007): 623-629.
- Goni E, Vicente G, Serra A, et al. Evaluation of the efficacy of sentinel node detection in breast cancer: chronological course and influence of the incorporation of an intra-operative portable gamma camera. Rev Esp Med Nucl Imagen Mol 32 (2013): 343-349.
- Lombardi A, Nigri G, Scopinaro F, et al. High-resolution, handheld camera use for occult breast lesion localization plus sentinel node biopsy (SNOLL): a single-institution experience with 186 patients. Surgeon 13 (2015): 69-72.
- Chondrogiannis S, Ferretti A, Facci E, et al. Intraoperative hand-held imaging γ-camera for sentinel node detection in patients with breast cancer: feasibility evaluation and preliminary experience on 16 patients. Clin Nucl Med 38 (2013): 132-136.
- Motomura K, Noguchi A, Hashizume T, et al. Usefulness of a solid-state gamma camera for sentinel node identification in patients with breast cancer. J Surg Oncol 89 (2005): 12-17.
- Vidal-Sicart S, Paredes P, Zano G, et al. Added Value of Intraoperative Real-Time Imaging in Searches for Difficult-to-Locate Sentinel Nodes, Eur J Nucl Med 51 (2010): 1219-1225.
- Mansel R, Fallowfield L, Kissin M, et al. Randomized multicenter trial of sentinel node biopsy versus standard axillary treatment in operable breast cancer: the ALMANAC Trial. J Natl Cancer Inst 98 (2006): 599.
- Veronesi U, Paganelli G, Viale G, et al. A randomized comparison of sentinel-node biopsy with routine axillary dissection in breast cancer. N Engl J Med 6 (2003): 546-553.


 Impact Factor: * 4.1
Impact Factor: * 4.1 Acceptance Rate: 74.74%
Acceptance Rate: 74.74%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 