Double Rib Sign on Computed Tomography of the Chest-Indication for Surgical Stabilization of Rib Fractures
Article Information
Bhavik Patel*, Martin Wullschleger
Department of Trauma, Gold Coast University Hospital, Southport, Australia
*Corresponding Author: Bhavik Patel, Trauma Department/Acute Care Surgical Unit Gold Coast University Hospital, Southport, Australia
Received: 26 August 2019; Accepted: 09 September 2019; Published: 16 September 2019
Citation: Patel B, Wullschleger M. Double Rib Sign on Computed Tomography of the Chest-Indication for Surgical Stabilization of Rib Fractures. Journal of Surgery and Research 2 (2019): 185-187.
View / Download Pdf Share at FacebookKeywords
Computed Tomography, Surgical Stabilization, Rib Fractures
Computed Tomography articles, Surgical Stabilization articles, Rib Fractures
Computed Tomography articles Computed Tomography Research articles Computed Tomography review articles Computed Tomography PubMed articles Computed Tomography PubMed Central articles Computed Tomography 2023 articles Computed Tomography 2024 articles Computed Tomography Scopus articles Computed Tomography impact factor journals Computed Tomography Scopus journals Computed Tomography PubMed journals Computed Tomography medical journals Computed Tomography free journals Computed Tomography best journals Computed Tomography top journals Computed Tomography free medical journals Computed Tomography famous journals Computed Tomography Google Scholar indexed journals Surgical Stabilization articles Surgical Stabilization Research articles Surgical Stabilization review articles Surgical Stabilization PubMed articles Surgical Stabilization PubMed Central articles Surgical Stabilization 2023 articles Surgical Stabilization 2024 articles Surgical Stabilization Scopus articles Surgical Stabilization impact factor journals Surgical Stabilization Scopus journals Surgical Stabilization PubMed journals Surgical Stabilization medical journals Surgical Stabilization free journals Surgical Stabilization best journals Surgical Stabilization top journals Surgical Stabilization free medical journals Surgical Stabilization famous journals Surgical Stabilization Google Scholar indexed journals Rib Fractures articles Rib Fractures Research articles Rib Fractures review articles Rib Fractures PubMed articles Rib Fractures PubMed Central articles Rib Fractures 2023 articles Rib Fractures 2024 articles Rib Fractures Scopus articles Rib Fractures impact factor journals Rib Fractures Scopus journals Rib Fractures PubMed journals Rib Fractures medical journals Rib Fractures free journals Rib Fractures best journals Rib Fractures top journals Rib Fractures free medical journals Rib Fractures famous journals Rib Fractures Google Scholar indexed journals trauma centre articles trauma centre Research articles trauma centre review articles trauma centre PubMed articles trauma centre PubMed Central articles trauma centre 2023 articles trauma centre 2024 articles trauma centre Scopus articles trauma centre impact factor journals trauma centre Scopus journals trauma centre PubMed journals trauma centre medical journals trauma centre free journals trauma centre best journals trauma centre top journals trauma centre free medical journals trauma centre famous journals trauma centre Google Scholar indexed journals Trachea articles Trachea Research articles Trachea review articles Trachea PubMed articles Trachea PubMed Central articles Trachea 2023 articles Trachea 2024 articles Trachea Scopus articles Trachea impact factor journals Trachea Scopus journals Trachea PubMed journals Trachea medical journals Trachea free journals Trachea best journals Trachea top journals Trachea free medical journals Trachea famous journals Trachea Google Scholar indexed journals Rib fractures articles Rib fractures Research articles Rib fractures review articles Rib fractures PubMed articles Rib fractures PubMed Central articles Rib fractures 2023 articles Rib fractures 2024 articles Rib fractures Scopus articles Rib fractures impact factor journals Rib fractures Scopus journals Rib fractures PubMed journals Rib fractures medical journals Rib fractures free journals Rib fractures best journals Rib fractures top journals Rib fractures free medical journals Rib fractures famous journals Rib fractures Google Scholar indexed journals surgical stabilisation articles surgical stabilisation Research articles surgical stabilisation review articles surgical stabilisation PubMed articles surgical stabilisation PubMed Central articles surgical stabilisation 2023 articles surgical stabilisation 2024 articles surgical stabilisation Scopus articles surgical stabilisation impact factor journals surgical stabilisation Scopus journals surgical stabilisation PubMed journals surgical stabilisation medical journals surgical stabilisation free journals surgical stabilisation best journals surgical stabilisation top journals surgical stabilisation free medical journals surgical stabilisation famous journals surgical stabilisation Google Scholar indexed journals chest wall stabilisation articles chest wall stabilisation Research articles chest wall stabilisation review articles chest wall stabilisation PubMed articles chest wall stabilisation PubMed Central articles chest wall stabilisation 2023 articles chest wall stabilisation 2024 articles chest wall stabilisation Scopus articles chest wall stabilisation impact factor journals chest wall stabilisation Scopus journals chest wall stabilisation PubMed journals chest wall stabilisation medical journals chest wall stabilisation free journals chest wall stabilisation best journals chest wall stabilisation top journals chest wall stabilisation free medical journals chest wall stabilisation famous journals chest wall stabilisation Google Scholar indexed journals radiological features articles radiological features Research articles radiological features review articles radiological features PubMed articles radiological features PubMed Central articles radiological features 2023 articles radiological features 2024 articles radiological features Scopus articles radiological features impact factor journals radiological features Scopus journals radiological features PubMed journals radiological features medical journals radiological features free journals radiological features best journals radiological features top journals radiological features free medical journals radiological features famous journals radiological features Google Scholar indexed journals Trauma Series Computed Tomography scan articles Trauma Series Computed Tomography scan Research articles Trauma Series Computed Tomography scan review articles Trauma Series Computed Tomography scan PubMed articles Trauma Series Computed Tomography scan PubMed Central articles Trauma Series Computed Tomography scan 2023 articles Trauma Series Computed Tomography scan 2024 articles Trauma Series Computed Tomography scan Scopus articles Trauma Series Computed Tomography scan impact factor journals Trauma Series Computed Tomography scan Scopus journals Trauma Series Computed Tomography scan PubMed journals Trauma Series Computed Tomography scan medical journals Trauma Series Computed Tomography scan free journals Trauma Series Computed Tomography scan best journals Trauma Series Computed Tomography scan top journals Trauma Series Computed Tomography scan free medical journals Trauma Series Computed Tomography scan famous journals Trauma Series Computed Tomography scan Google Scholar indexed journals
Article Details
1. Case Report
A 30-year-old man presented to our Level I trauma centre being rolled over in a car crash at 90km/hr. The patient was alert and oriented but complained of significant pain on the right lower chest wall and upper abdomen. On clinical examination of the chest, Trachea was central, but he had right sided tenderness and reduced air entry. X Ray chest (Figure 1) was suggestive of hemopneumothorax and fracture ribs on the Right side which was managed with an intercostal catheter. He underwent Trauma Series Computed Tomography scan(CT). The Chest CT (Figure 2, 3) was suggestive of Right-sided rib anterior and posterior 6th, 7th, 8th, 9th (constituting flail segment), and posterior 10th, 11th fractures. There is up to 13 mm of trans axial displacement of fragments at the 7th, 8th rib fractures and up to 5 mm displacement at the 10th, 11th rib fractures. The CT abdomen was suggestive of American Association for Severity of Trauma (AAST) Grade IV liver injury and AAST Grade IV right kidney injury notably without clear evidence of ongoing haemorrhage. As the patient was hemodynamically robust, he was transferred to High Dependency Unit for close observation. Over a period of 24 hours, despite various modalities of pain control utilised by our specialist service he was only able to achieve 500cc on the incentive spirometer. We then proceeded to surgical stabilisation of Rib fractures on day 2 of his admission (Figure 4). He tolerated the procedure well and was discharged home on day 5.
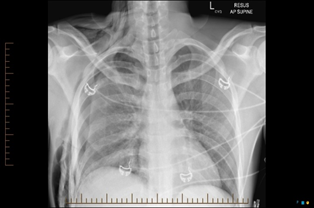
Figure 1: Chest X ray suggestive of Hemopnuemothorax and Fracture ribs.
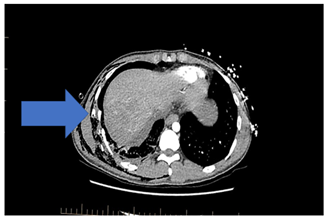
Figure 2: CT scan suggestive of Double rib sign.
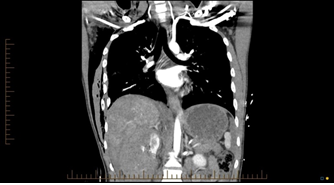
Figure 3: Sagittal CT view suggestive of Double Rib Sign.
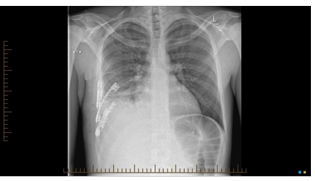
Figure 4: Post -Operative X- Ray Chest.
2. Discussion
Surgical stabilisation of Rib fractures is the modality of management in the acutely unstable chest wall1,2. However there has been no clear definition of the flail or unstable chest wall [3]. Similarly, there has been no literature documentation of radiological features which may guide chest wall stabilisation surgeons with regards to early intervention for fixation. Our Institution has initiated a surgical stabilisation of rib fracture program since 2014. We have to date stabilised 60 rib fractures both anterior and posterior following early intervention when the CT scan suggests a double rib sign. This is defined as two fragments of single rib being seen on the same slice in both Transverse and Sagittal views of the Chest in the Bone window (Figure 2, 3). We regularly look out for the double rib sign as an indicator of early surgery. The volume of our work has gradually increased over the last 5 years with not only having reduced the ventilator days but also reduction in hospital days when compared to those patients not being offered an operative intervention. The procedure has been carried out with minimum morbidity and no mortality. We think this sign could provide future chest wall stabilisation surgeons as a good indicator for early intervention.
References
- Fredric M Pieracci, Julia Coleman, Francis Ali-Osman, et al. A multicenter evaluation of the optimal timing of surgical stabilization of rib fracture. J Trauma Acute Care Surg 84 (2018): 1-10
- Fredric M Pieracci, Yihan Lin, Maria Rodil, et al. A prospective, controlled clinical evaluation of surgical stabilization of severe rib fractures. J Trauma Acute Care Surg 80 (2016): 187-194.
- Johnson MC, Miller CP, Stolarski AE, et al. Perceptions in Rib Injuries: A multidisciplinary single centre survey of clinician differences in risk stratification and management of patients with rib fractures. The American Journal of Surgery 218 (2019): 32-36.


 Impact Factor: * 4.2
Impact Factor: * 4.2 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 