Influence of Cyst Size on Ovarian Reserve after Unilateral Laparoscopic Ovarian Cystectomy for Endometrioma and Ovarian Mature Teratoma
Hee-Suk Chae*
Department of Obstetrics and Gynecology, Research Institute of Clinical Medicine of Jeonbuk National University, Biomedical Research Institute of Jeonbuk National University Hospital, Jeonbuk National University Medical School, Jeonju, Jeonnbuk, South Korea.
*Corresponding Author: Hee-Suk Chae, Department of Obstetrics and Gynecology, Research Institute of Clinical Medicine of Jeonbuk National University, Biomedical Research Institute of Jeonbuk National University Hospital, Jeonbuk National University Medical School, Jeonju, Jeonnbuk, South Korea.
Received: 23 February 2023; Accepted: 01 March 2023; Published: xx March 2023
Article Information
Citation: Hee-Suk Chae. Influence of Cyst Size on Ovarian Reserve after Unilateral Laparoscopic Ovarian Cystectomy for Endometrioma and Ovarian Mature Teratoma. Journal of Surgery and Research. 6 (2023): 130-136.
View / Download Pdf Share at FacebookAbstract
Background: The present study is aimed to investigate the influence of ovarian cyst size on serum anti-Müllerian hormone levels after laparoscopic ovarian cystectomy in women with endometrioma and ovarian mature teratoma.
Methods: From March 2017 to December 2018, we retrospectively studied eighty-one patients who underwent unilateral laparoscopic cystectomy for endometrioma (n = 41, endometrioma group) and ovarian mature cystic teratoma (n = 40, teratoma group). Serum anti-Müllerian hormone (AMH) levels were measured preoperatively and 1 month after surgery.
Results: The rate of decrease in serum AMH levels after laparoscopic cystectomy was significantly higher in the endometrioma group than in the teratoma group (0.35 ± 0.04% vs. 0.19 ± 0.04%, p = 0.013). In patients with mature cystic teratoma, a statistically significant correlation between the rate of decrease in serum AMH levels and cyst size was observed (r = 0.391, p = 0.013); the rate of decrease in serum AMH levels after surgery was significantly higher in the > 5.13 cm subgroup than in the ≤ 5.13 cm subgroup (p = 0.006).
Conclusions: Laparoscopic cystectomy for endometriomas may result in a more significant damage to the ovarian reserve compared with that for ovarian mature cystic teratomas. Cyst diameter and reduced ovarian reserve after surgery were not correlated in patients with endometriomas, whereas a significant correlation was observed in patients with ovarian mature teratomas. The decrease in AMH levels was more evident in patients with a mature teratoma > 5.13 cm.
Keywords
<p>Anti-Müllerian hormone, Endometrioma, Ovarian mature teratoma, Unilateral laparoscopic cystectomy</p>
Article Details
Background
Endometriosis is the presence of endometrial glands and stroma outside the uterine cavity, which affects 10% of women of reproductive age. The most common form of endometriosis is ovarian endometrioma, which accounts for up to 40% of the cases [1,2]. Moreover, endometriosis is a chronic inflammatory disease associated with chronic pelvic pain, dysmenorrhea, and/or reduced fertility [3]. Mature cystic teratomas, which are also called dermoid cysts, are the most common germ cell tumor, accounting for up to 70% of benign ovarian masses in the reproductive years [4].
Laparoscopic cystectomy or the so-called “stripping technique” is an accepted technique for the treatment of benign ovarian cysts and is considered a fertility-preserving procedure [5,6]. However, this surgical technique has concerns related to optimizing the preservation of fertility [5]. Because benign ovarian cysts, such as endometrioma or ovarian mature cystic teratoma, occur most frequently in reproductive women, the aim of the procedure is to have the least possible damage to the ovaries. Ovarian reserve, which is defined as the functional potential of the ovary, reflects the number of follicles left in the ovary at any given time [7]. Several markers and tests of ovarian reserve have been developed, however, no accurate method to measure ovarian reserve exists. Recently, anti-Müllerian hormone (AMH) level has been suggested as the most reliable and reproducible marker because it is menstrual cycle independent and is also unaffected by hormonal drug use [1,8].
Numerous studies have shown reduction in ovarian reserve based on serum AMH levels after cystectomy [9,10]. Some studies reported a significant postoperative reduction in AMH levels in endometrioma compared with nonendometrioma [11]. whereas other studies showed that the rate of decrease in AMH levels after surgery is similar between women with endometrioma and those with other benign ovarian cysts [12,13]. Hence, the influence of cyst size or histologic type on the ovarian reserve after surgery remains unclear.
Thus, this study aimed to investigate influence of cyst size on the ovarian reserve after laparoscopic ovarian cystectomy based on the changes in the serum AMH levels to identify the cyst size that is associated with more damage to the ovaries, and to determine whether the results between endometrioma and ovarian mature teratoma differ.
Methods
Participants
We reviewed the medical records of patients who underwent laparoscopic unilateral ovarian cystectomy for endometrioma (endometrioma group) or mature cystic teratoma (teratoma group) at the Department of Obstetrics and Gynecology of the Jeonbuk National University Hospital between March 2017 and December 2018. This study was approved by the Institutional Review Board of Chonbuk National University Hospital.
The inclusion criteria were as follows: (1) endometrioma and ovarian mature cystic teratoma confirmed histologically. The exclusion criteria were as follows: age > 42 years; (2) patients with a history of previous adnexal surgery, and any hormonal treatment, such as oral contraceptives, within 6 months.
Data regarding patient’s age, body mass index (BMI), cyst size, locularity of cyst, and serum AMH level, and pathologic reports were retrieved from medical records and operative reports. Cyst size was defined as the largest diameter measured by preoperative imaging studies including computed tomography (CT), or magnetic resonance imaging (MRI). Serum AMH concentrations were measured preoperatively and 1 month after surgery. The serum AMH level was determined using a commercial kit (AMH Gen II assay; Beckman Coulter Inc., USA).
Operation technique
All laparoscopic cystectomies were performed by the same gynecologic surgeon (H.C.). After establishment of the pneumoperitoneum with a Veress needle through a 10-mm subumbilical incision, a laparoscope was introduced. Subsequently, two additional 5-mm trocars were placed suprapubically for the introduction of ancillary instruments. In patients with ovarian endometrioma, the contents of the cyst were aspirated and the outer wall of the cyst was incised from the punctured site thereafter. After identifying the cleavage plane between the normal ovarian tissue and cyst, the cyst capsule was stripped from the ovarian parenchyma by applying atraumatic forceps and counter traction. Hemostasis was achieved by direct suturing with a 2-0 Vicryl suture at the bleeding site. The cleavage plane was not clearly visible when approaching the hilus on the utero-ovarian ligament side; thus, fulguration by bipolar coagulation and cutting by scissors were performed. The cyst was completely removed. After hemostasis, the ovarian edges were not approximated. In patients with mature cystic teratoma, an endobag was used to prevent iatrogenic spillage from a ruptured cyst. The cyst was placed into the endobag and the wall of the cyst was incised. After identifying the cleavage plane between the cyst and normal ovarian tissue, the cyst was enucleated from the normal ovarian tissue by applying counter traction with atraumatic forceps and hydrodissection. The cyst was completely removed. Hemostasis was achieved by direct suturing with a 2-0 Vicryl suture at the bleeding site. After hemostasis, the ovarian edges were not approximated.
Statistical analyses
R language version 3.3.3 (R Foundation for Statistical Computing, Vienna, Austria) and T&F program version 3.0 (YooJin BioSoft, Korea) were used for all statistical analyses. Continuous variables are expressed as mean ± standard deviation and categorical variables as sample number and percentage. For mean comparison, Mann-Whitney U test or Kruskal-Wallis H test was performed according to the compared number of subgroups such as the teratoma vs. the endometrioma group. For categorical variables, the chi-squared test was employed to compare proportions of sample number. A correlation analysis between several factors and the decreasing amount or decreasing ratio of AMH level after operation was performed using the Spearman correlation method. Receiver operating characteristic (ROC) curve analysis was conducted to estimate the prediction accuracy of continuous values on the binary response defined by decreased ratio. A cutoff value was selected to maximize the product of sensitivity and specificity, with sensitivity being greater than specificity. A p value < 0.05 was considered statistically significant.
Results
The clinical characteristics and serum AMH changes in the endometrioma and teratoma groups are summarized in table 1. Differences in BMI, cyst size, and locularity of cysts were not statistically significant between the two groups, whereas the differences in age were statistically significant (p = 0.02). Preoperative serum AMH levels between the two groups did not differ (p = 0.561). However, postoperative serum AMH levels were lower in the endometrioma group than in the teratoma group, with a marginal statistical significance (p = 0.051). Differences in the decrease and the rate of decrease of serum AMH levels between the two groups were statistically significant (p = 0.031 and p = 0.013, respectively), indicating that the rate of decrease in serum AMH level after surgery was higher in the endometrioma group than in the teratoma group.
|
Variable |
Subgroup |
Endometrioma group |
Teratoma group |
p value |
|
Sample no (%) |
41 (50.62) |
40 (49.38) |
||
|
Age (year) |
29.56 ± 6.14 |
26.3 ± 6.86 |
0.02* |
|
|
BMI (kg/m2) |
22.13 ± 3.06 |
23.66 ± 5.7 |
0.395 |
|
|
Cyst size (cm) |
5.21 ± 1.94 |
5.76 ± 2.73 |
0.542 |
|
|
Locularity (n) |
0.098 |
|||
|
Unilocular |
26 |
32 |
||
|
Multilocular |
15 |
8 |
||
|
Preoperative AMH level (ng/mL) |
4.18 ± 2.62 |
4.79 ± 3.37 |
0.561 |
|
|
Postoperative AMH level (ng/mL) |
2.62 ± 1.65 |
3.81 ± 2.71 |
0.051 |
Continuous variables are expressed as mean ± SD.
Categorical variables are expressed as sample number and %.
p -values for continuous and categorical variables are computed using Mann-Whitney U test and chi-squared test, respectively.
BMI: body mass index
AMH: anti-Müllerian hormone
* p < 0.05
Table 1: Clinical characteristics and pre- and postoperative serum AMH levels in the endometrioma and teratoma group.
Univariate analyses were performed to identify the correlation between the rate of decrease in AMH level after surgery and other parameters including age, BMI, cyst size, locularity of cyst, and preoperative AMH level (Table 2). A statistically significant positive correlation between cyst size and the rate of decrease in AMH level was noted in the teratoma group (p = 0.013, r = 0.391) (Figure 1A). In the endometrioma group, no statistically significant correlation between cyst diameter and the rate of decrease in serum AMH levels was found (p = 0.405, r = –0.134) (Figure 1B). The rate of decrease in serum AMH levels showed no correlations with age, BMI, locularity of cyst, and preoperative AMH level in both groups. The median rate of decrease in AMH level was 24.7%. Because the rate of decrease in AMH level correlated with cyst size in the teratoma group, the ROC curve was determined using the rate of ≤ 24.7% as a cut-off point. The area under the ROC curve was 0.706 (p = 0.026), indicating that the sensitivity of the rate of decrease in AMH level of ≤ 24.7% after surgery was 65% for patients with ovarian mature teratoma ≤ 5.13 cm, and the corresponding specificity was 75% (Figure 2). Therefore, the rate of decrease in AMH level in the subgroup with cysts > 5.13 cm was significantly higher than that in the subgroup with cysts ≤ 5.13 cm (p = 0.006).
|
Endometrioma group |
Teratoma group |
|||
|
r |
p |
r |
p |
|
|
Age (year) |
0.09 |
0.576 |
-0.015 |
0.925 |
|
BMI (kg/m2) |
0.288 |
0.068 |
-0.179 |
0.269 |
|
Cyst size (cm) |
-0.134 |
0.405 |
0.391 |
0.013* |
|
Locularity (n) |
-0.08 |
0.96 |
0.645 |
0.289 |
|
Preoperative AMH level (ng/mL) |
-0.009 |
0.954 |
0.061 |
0.709 |
Spearman coefficient is shown with p values.
BMI: body mass index; AMH: anti-Müllerian hormone
Table 2: Correlations coefficients between the rate of decrease in AMH levels and other parameters in the two groups.
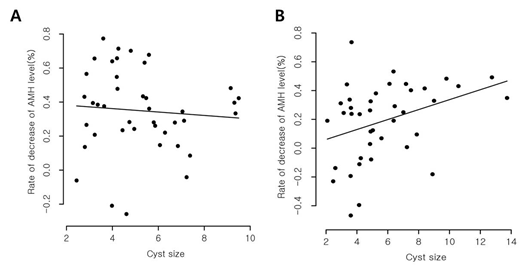
Figure 1: Scatter plot of the correlation between the rate of decrease in AMH level and cyst size after surgery in the two groups. No significant statistical correlation between cyst size and the rate of decrease in AMH level in the endometrioma group (A) was found, whereas cyst size correlated with the rate of decrease in AMH level in the teratoma group (B).
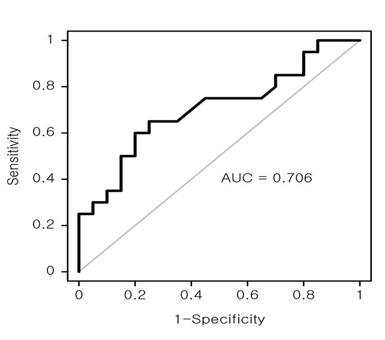
Figure 2: ROC curve analysis representing the rate of decrease in serum AMH level according to cyst size in ovarian mature teratoma. The AUC value was 0.706, corresponding with sensitivity of 65% and specificity of 75%. ROC, receiver operating characteristic; AUC, area under the ROC curve.
Discussion
The present study showed that laparoscopic cystectomy for endometrioma caused a more significant damage to the ovarian reserve compared with that for ovarian mature teratoma. These findings are consistent with recent studies [14]. In addition, this study showed that the damage to the ovarian reserve after cystectomy in patients with mature teratoma is positively correlated with cyst size (especially for cysts > 5.13 cm), whereas cyst size in patients with endometrioma showed no correlation with damage to the ovarian reserve after surgery.
Although laparoscopy is the first–line management for benign ovarian cysts, controversy exists regarding the most appropriate time for surgical intervention that could minimize ovarian damage. These cysts are common in younger women; thus, identifying the appropriate time of surgery is crucial for sparing residual functioning ovarian tissue after surgery.
The European Society of Human Reproduction and Embryology guidelines recommend that surgery should be performed in women complaining of endometriosis-associated pain or in women with endometrioma (≥ 3 cm) [15]. However, a number of studies reported that cystectomy for endometrioma may be harmful for the ovarian tissue [16,17], and some recent studies showed reduction in ovarian reserve after surgery based on serum AMH levels [1]. Moreover, removal of endometriomas before in vitro fertilization did not improve fertility outcomes [18], and post-cystectomy ovaries showed reduced follicular response in natural and clomiphene citrate cycles [19]. However, substantial evidence on expectant versus surgical management of endometrioma is lacking. Few recent studies on the influence of cyst size on ovarian reserve after cystectomy have been conducted. Chen et al. reported that operation-related damage to the ovarian reserve is positively related to bilateral endometriomas and endometrioma > 7 cm [20]. Mehdizadeh Kashi et al. demonstrated that laparoscopic cystectomy, particularly endometriomas with bilateral involvement and those at least 5 cm in diameter, is associated with post-operative decrease in serum AMH level [7]. Exacoustos et al. showed that ovarian stripping of endometriomas, but not of ovarian mature teratomas, is associated with a significant decrease in residual ovarian volume, which could result in diminished ovarian reserve and function [21].
Several reasons for the decrease in ovarian reserve after cystectomy have been proposed. First, cystectomy using the stripping technique could result in inadvertent removal of a healthy ovarian tissue and decreased ovarian reserve [13,22]. The second possible reason is the ovarian vascular injury associated with bipolar electrocoagulation [5]. Nevertheless, the mechanisms underlying the decrease in ovarian reserve after cystectomy remain unknown. In addition, the aforementioned reasons were mainly from studies of patients with endometrioma. Thus, whether laparoscopic cystectomy for nonendometriotic ovarian cyst could decrease ovarian reserve remains to be established.
In this study, the postoperative decrease in AMH level in patients with endometrioma showed no correlation with cyst size, age, BMI, locularity of cyst, and preoperative AMH level. Although the size of mature teratoma was positively related to the rate of decrease in the AMH level, it was not correlated with age, BMI, locularity of cyst, and preoperative AMH level. These results indicate that laparoscopic cystectomy for a relatively large mature teratoma could result in significant damage to the ovarian reserve.
In our opinion, the finding that ovarian reserve after cystectomy decreases supports the second reason mentioned previously; i.e., vascular injury during surgery plays a role. The amount of ovarian normal tissue removed during stripping of mature teratoma could be less than that during stripping of endometrioma because mature teratomas, unlike endometriomas, can be enucleated more easily. In this study, further analysis was performed to explore the association between the cyst diameter and the rate of decrease in AMH level after cystectomy. The ROC curve analysis revealed that a larger cyst diameter was associated with increased damage to the ovarian reserve. In the subgroup with a cyst diameter > 5.13 cm, a statistically significant decrease in the ovarian reserve was found. This result could be because the hilum of the ovary opens up and more vessels of the mesovarium are exposed as the diameter of the cyst increases. Thus, hemostasis should be implemented more extensively following stripping of cysts with larger diameters. Moreover, some studies about the effects of different hemostatic methods on ovarian reserve showed that bipolar electrocoagulation hemostasis applied to laparoscopic cystectomy is associated with a significant reduction in ovarian reserve compared with the suture hemostasis technique [23,24] Zhang et al. also showed that recovery of ovarian reserve was greater in patients with suture hemostasis than in those with bipolar electrocoagulation and ultrasonic scalpel [24], and they emphasized the importance of protecting the ovarian blood supply system to maintain ovarian function. In our study, damage to the ovarian reserve after surgery was more severe in patient with mature teratomas with cysts > 5.13 cm, suggesting that sugery on cysts with larger diameters could result in exposure of extensive vessels. Furthermore, controversies regarding the best surgical intervention to manage mature teratomas exist given that these cysts are extremely common among reproductive-aged women and they also grow very slowly, i.e., by 1.7-1.8 mm each year [25]. Kim et al. reported no difference in preoperative serum AMH level between women with mature teratoma and age- and BMI-matched controls [26]. Legendre et al. recommended that a wait-and-see attitude appears reasonable for asymptomatic women, especially for moderate-sized mature teratomas (4-6 cm), where the risk of secondary interventions is low [25]. However, our results showed that laparoscopic cystectomy is associated with severe damage to the ovarian reserve, particularly with cysts > 5.13 cm. Therefore, a surgical approach instead of expectant management should be considered in young patients with a relatively large mature teratoma to minimize the risk of damage to ovarian reserve due to cystectomy.
In endometrioma cases, several other possible reasons for a decrease in ovarian reserve, such as the inadvertent removal of healthy ovarian tissue during cystectomy or vascular compromise, have been proposed, including excessive adhesiolysis [27] and postsurgical inflammation [28,29]. Muzii et al. reported that the ovarian tissue adjacent to the endometrioma wall differs morphologically from the normal ovarian tissue and is possibly nonfunctional, thereby suggesting that ovarian function disruption may have already been present before laparoscopic excision [5]. Hence, factors other than cyst size seems to contribute to the decreased ovarian function after cystectomy in patients with endometrioma.
This study has some limitations. The number of patients was small, and the study had a retrospective design. In addition, only serum AMH levels measured 1 month after surgery were used to assess the risk of postoperative damage to ovarian reserve. Nonetheless, our study has several strengths. The same skilled operator performed each surgery, which removed the influence of surgical skill on surgical outcomes. Additionally, CT or MRI was used to accurately measure the diameter of the ovarian cyst. Only patients with unilateral ovarian cysts were included in the investigation of the relationship between cyst size and postoperative ovarian damage.
Conclusions
Damage to ovarian reserve after laparoscopic cystectomy may be greater in endometrioma than in ovarian mature teratoma. Cyst size is associated with the decrease in ovarian reserve after surgery in mature teratoma, but not in endometrioma. Operation-related damage to the ovarian reserve is associated with the size of mature teratoma. Nevertheless, large-scale prospective studies are needed to confirm our findings.
Abbreviations
AMH: anti-Müllerian hormone
BMI: body mass index
CT: computed tomography
MRI: magnetic resonance imaging
ROC: Receiver operating characteristic
Acknowledgements
None
Funding
This paper was supported by Fund of Biomedical Research Institute, Jeonbuk National University Hospital.
Contributions
H.-S.C. designed the study and analyzed the data. H.-S.C. wrote the main manuscript. All authors read and approved the final manuscript.
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Institutional Review Board of Jeonbuk National University Hospital with ethical code number 2018-05-018-010. Due to the retrospective design of the study an informed consent is not applicable.
Consent for publication
Not applicable
Competing interests
The authors declare that they have no interests.
References
- Celik HG, Dogan E, Okyay E, et al. Effect of laparoscopic excision of endometriomas on ovarian reserve: serial changes in the serum antimüllerian hormone levels. Fertil Steril 97 (2012): 1472-1478.
- DoganE, Ulukus EC, Okyay E, et al. Retrospective analysis of follicle loss after laparoscopic excision of endometrioma compared with benign nonendometriotic ovarian cysts. Int J Gynaecol Obstet 114 (2011): 124-127.
- Coccia ME, Rizzello F, Barone S, et al. Is there a critical endometrioma size associated with reduced ovarian responsiveness in assisted reproduction techniques? Reprod Biomed Online 29 (2014): 259-266.
- Sinha A, Ewies AA. Ovarian mature cystic teratoma: challenges of surgical management. Obstet Gynecol Int (2016).
- Muzil L, Bianchi A, Crocè C, et al. Laparoscopic excision of ovarian cysts: is the stripping technique a tissue-sparing procedure? Fertil Steril 77 (2002): 609-614.
- Legendre G, Catala L, Morinière C, et al. Relationship between ovarian cysts and infertility: what surgery and when? Fertil Steril 101 (2014): 608-614.
- Mohamed ML, Nouh AA, El-Behery MM, Mansour SA. Effect on ovarian reserve of laparoscopic bipolar electrocoagulation versus laparotomic hemostatic sutures during unilateral ovarian cystectomy. Int J Gynaecol Obstet 114 (2011): 69-72.
- Alborzi S, Keramati P, Younesi M, et al. The impact of laparoscopic cystectomy on ovarian reserve in patients with unilateral and bilateral endometriomas. Fertil Steril 10 (2014): 427-434.
- Raffi F, Metwally M, Amer S. The impact of excision of ovarian endometrioma on ovarian reserve: a systematic review and meta-analysis. J Clin Endocrinol Metab 97 (2012): 3146-3154.
- Somigliana E, Berlanda N, Benaglia I, et al. Surgical excision of endometriomas and ovarian reserve: a systematic review on serum antiMüllerian hormone level modifications. Fertil Steril. 98 (2012):1531-1538.
- Lee DY, Young KN, Jae KM, et al. Effects of laparoscopic surgery on serum antiMüllerian hormone levels in reproductive-aged women with endometrioma. Gynecol Endocrinol 27 (2011): 733-736.
- Kwon SK, Kim SH, Yun SC, et al. Decline of serum antiMüllerian hormone levels after laparoscopic ovarian cystectomy in endometrioma and other benign cysts: a prospective cohort study. Fertil Steril 101 (2014): 435-441.
- Chun S, Cho HJ, Ji YI. Comparison of early postoperative decline of serum antiMüllerian hormone levels after unilateral laparoscopic ovarian cystectomy between patients categorized according to histologic diagnosis. Taiwan J Obstet Gynecol. 55 (2016): 641-645.
- Perlman S, Kjer JJ. Ovarian damage due to cyst removal: a comparison of endometriomas and dermoid cysts. Acta Obstet Gynecol Scand 95 (2016): 285-290.
- Dunselman GA, Vermeulen N, Calhaz-JC, et al. ESHRE guideline: management of women with endometriosis. Hum Reprod 29 (2014): 400-412.
- Roman H, Tarta O, Pura I, et al. Direct proportional relationship between endometrioma size and ovarian parenchyma inadvertently removed during cystectomy, and its implication on the management of enlarged endometriomas. Hum Reprod 25 (2010): 1428-1432.
- Muzii L, Bellati F, Bianchi A, et al. Laparoscopic stripping of endometriomas: a randomized trial on different surgical techniques. Part II. Pathological results. Hum Reprod 20 (2005): 1987-1992.
- Garcia-Velasco JA, Mahutte NG, Corona J, et al. Removal of endometriomas before in vitro fertilization does not improve fertility outcomes: a matched, case-control study. Fertil Steril 81 (2004): 1194-1197.
- Loh FH, Tan AT, Kumar J, et al. Ovarian response after laparoscopic ovarian cystectomy for endometriotic cysts in 132 monitored cycles. Fertil Steril 72 (1999): 316-321.
- Chen Y, Pei H, Chang Y, et al. The impact of endometrioma and laparoscopic cystectomy on ovarian reserve and the exploration of related factors assessed by serum antiMüllerian hormone: a prospective cohort study. J Ovarian Res 26 (2014): 7-108.
- Exacoustos C, Zupi E, Amadio A, et al. Laparoscopic removal of endometriomas; sonographic evaluation of residual functioning ovarian tissue. Am J Obstet Gynecol 191 (2004): 68-72.
- Mehdizadeh KA, Chaichian S, Arianan S, et al. The impact of laparoscopic cystectomy on ovarian reserve in patients with unilateral and bilateral endometrioma. Int J Gynecol Obstet. 136 (2017): 200-204.
- Fedele L, Bianehi S, Zanconato G, et al. Bipolar electrocoagulation versus suture of solitary ovary after laparoscopic excision of ovarian endometriomas. J Am Assoc Gynecol Laparosc 11 (2004): 344-347.
- Zhang CH, Wu L, Li PQ. Clinical study of the impact on ovarian reserve by different hemostasis methods in laparoscopic cystectomy for ovarian endometrioma. Taiwan J Obstet Gynecol 55 (2016): 507-511.
- Legendre G, Catala L, Morinière C, et al. Relationship between ovarian cysts and infertility: what surgery and when? Fertil Steril. 101 (2014): 608-614.
- Kim JY, Jee BC, Suh CS, et al. Preoperative serum anti-Müllerian hormone level in women with ovarian endometrioma and mature cystic teratoma. Yonsei Med J 54 (2013): 921-926.
- Saito A, Iwase A, Nakamura T, et al. Involvement of mesosalpinx in endometrioma is a possible risk factor for decrease of ovarian reserve after cystectomy: a retrospective cohort study. Reprod Biol Endocrinol 14 (2016): 72.
- Hachisuga T, Kawar T. Histopathological analysis of laparoscopically treated ovarian endometriotic cysts with special reference to loss of follicles. Hum Reprod 17 (2002): 432-435.
- Li CZ, Liu B, Wen ZQ, et al. The impact of electrocoagulation on ovarian reserve after laparoscopic excision of ovarian cysts: a prospective clinical study of 191 patients. Fertil Steril. 92 (2009): 1428-1435.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 