Effect of Laparoscopic Cholecystectomy in Alleviating Dyspeptic Symptoms in Patients with Cholelithiasis
Mohit S Gupta1,2*, Srivastava KN2, Mohit Jain2, Ajay Chauhan2
1Department of colorectal surgery, Bedford NHS Trust, Bedfordshire, UK
2Department of general and minimal access surgery, BLK Superspeciality hospital, New Delhi, India
*Corresponding Author: Mohit S Gupta, Department of Colorectal Surgery, Bedford NHS Trust, Bedford MK40 3EX, Bedfordshire, UK
Received: 06 May 2020; Accepted: 20 May 2020; Published: 09 June 2020
Article Information
Citation: Mohit S Gupta, Srivastava KN, Mohit Jain, Ajay Chauhan. Effect of Laparoscopic Cholecystectomy in Alleviating Dyspeptic Symptoms in Patients with Cholelithiasis. Journal of Surgery and Research 3 (2020): 119-134.
View / Download Pdf Share at FacebookAbstract
Objective: To compare the change in preoperative and postoperative dyspeptic symptoms.
Introduction: In the era of increasing prevalence of gall stones due to more frequent incidental detection radiologically, it is the need of the hour that we assess the benefit of these increasing cholecystectomies with regard to dyspeptic symptoms. Till now there is not enough evidence on the basis of which we can determine whether laparoscopic cholecystectomy can resolve the dyspeptic symptoms in patients of gall stones. There is a need to establish a guideline to operate in view of alleviating dyspeptic symptoms.
Methodology: A total of 308 (M:F=2:3) patients were evaluated for dyspeptic symptoms using the Glasgow dyspepsia severity score (GDSS). They were followed up after 1 month, 6 months. Disease distribution and change in GDSS scores were analysed.
Results: The mean age was 47.2 ± 15.42 years. Preoperatively mean GDSS was 11.49 ± 2.11. One month post surgery 82% had a GDSS around 2.95. 12% had a significant drop in GDSS at the end of 6 months (p<0.001). 3.89% had a GDSS of more than 10 which indicated persistentdyspepsia. 3 patients 0.97% had subsequent worsening of GDSS.
Conclusion: Most symptomatic patients undergoing laparoscopic cholecystectomy are objectively relieved of dyspeptic symptoms. Very few patients have persistent symptoms even after 6 months. Patients tend to associate relief of dyspepsia with successful outcome of surgery. It is extremely essential that patients be counselled in detail about the possibility of persistence of dyspeptic symptoms which may in-fact be functional/inorganic.
Keywords
<p>Dyspepsia, Laparoscopic Cholecystectomy, Cholelithiasis</p>
Article Details
1. Introduction
Scientific curiosity and the need for innovation has been at the very centre of human nature. The initiation of endoscopic surgery can be traced back to the era of Hippocrates. The brave endeavours of many clinicians of the past have directly and indirectly played a major role in the development of modern day laparoscopy. The great physician, Hippocrates (460-377 BC), made the original reference to a speculum examination of rectum [1]. George Kelling performed the first laparoscopy, using Nitze’s cystoscope, in a living dog and named the procedure “Coelioscopie”. Jacobeus first made the term laparoscopy applicable to humans and is credited with the introduction of laparoscopic technique in humans [2]. In 1985, Prof. Dr. Med Erich Muhe of Boblingen, Germany, performed the first laparoscopic cholecystectomy in man. This was followed by Phillipe Mouret in France. Mouret was a gynaecologist who while doing a laparoscopic gynaecological surgery in women decided to remove the diseased gall bladder laparoscopically [1]. This event has led to the revolution being witnessed by all of us today. The prevalence of gallstone disease in India is 6.12% [5] when compared with the western population which is around 10 to 20% [6]. Laparoscopic cholecystectomy is the gold standard treatment for cholelithiasis [7]. In the yesteryears its role was mainly to alleviate the biliary pain of cholelithiasis, patients at risk for gall bladder cancer, acalculus cholecystitis and complicated cholelithiasis. Over the years the indications for performing the operation have been on the rise, although dyspepsia as a symptom complex has been long associated with cholelithiasis, it has been overshadowed by biliary colic and cholecystitis when it comes to significance. Over the past two decades greater importance has begun to be attributed to dyspepsia lowering the quality of life. As a result, it is the need of the hour that we assess the benefit of these increasing cholecystectomies with regard to dyspeptic symptoms. Till now there is not enough evidence on the basis of which we can determine whether laparoscopic cholecystectomy can resolve the dyspeptic symptoms in patients of gall stones. It is of utmost importance that like the clear indications of operating a cholelithiasis patient with typical abdominal pain, there is a need to establish a guideline to operate in view of alleviating dyspeptic symptoms.
According to the Rome III criteria, diagnostic criteria of dyspeptic symptoms must include one or more of the following:
- Bothersome postprandial fullness
- Early satiation
- Epigastric pain
- Epigastric burning.
No evidence of structural disease (including at upper GI endoscopy) that is likely to explain the symptoms. Dyspepsia has been defined as a set of symptoms, related or unrelated to food ingestion, localised to the upper half of the abdomen. Dyspepsia has been divided into,
- a) Organic dyspepsia, in which improvement of the underlying condition would result in elimination of dyspepsia, e.g. peptic ulcer, biliopancreatic aetiologies
- b) Functional dyspepsia, also known as nonorganic, idiopathic or essential dyspepsia, where no identifiable explanation for the symptoms could be said.
- c) Non-investigated dyspepsia, which needs further investigations to deduce the cause.
There has been conflicting evidence about the role of laparoscopic cholecystectomy in curing dyspepsia [8].
2. Material and Methods
2.1 Study Site
Department of General Surgery
Dr. B.L. Kapur Memorial Hospital, New Delhi.
2.2 Time Frame
February 2016 to June 2017.
2.3 Study Design
A prospective observational study.
The study protocol was approved by the Ethics committee. An ethics application was submitted to the ethics committee. In addition, a study proposal, consent form, and the questionnaire were submitted concurrently. All patients were informed about the nature and objectives of the study and informed consent was obtained.
2.4 Sample size
A total of 308 patients were enrolled for the study. All such candidates were considered for the study with the following criteria,
2.5 Inclusion Criteria
All patients above 18 years of age, undergoing elective laparoscopic cholecystectomy for uncomplicated gallstone disease.
2.6 Exclusion criteria
The exclusion criteria involved patients with complicated gallstone disease. Any one of the following were considered as complicated gallstone disease and were excluded:
1) Acute attack of cholecystitis at the time of surgery
2) Complicated gall stone disease like
- Common bile duct stones (choledocholithiasis)
- Obstructive jaundice, cholangitis, gallstone pancreatitis
- Cholecystoenteric fistula
- Previous biliary/pancreatic surgery,
3) Laparoscopic cholecystectomy combined with other operative procedures
4) Patients who are completely asymptomatic ( have neither dyspepsia nor biliary pain).
2.7 Methodology
Patients satisfying the inclusion criteria were taken up for the study. Patient’s demographic and clinical data were be recorded in a standard proforma. An informed consent was taken stating patient is consenting both for volunteering to be a part of the study and willing for follow-up. The patients were educated about the study and an information sheet was provided to the patient to answer their doubts and queries. All these patients were explained about communication media including telephone, email and to come for follow-up on an outpatient basis. They were followed up after 1 month, 6 months and whenever they wanted in case of any adverse event. Outcomes were recorded in proformas provided to the patient at the time of follow-up to be filled up on an outpatient basis. Assessment of outcomes were done by patient feedback via questionnaire done pre operatively and at 1 month and at 6 months postoperatively. We used a recently validated multidimensional disease specific scale for dyspepsia-the Glasgow dyspepsia severity score (GDSS) developed by El-Omar and colleagues [9, 10] as described in Table 1.
For the purpose of this study dyspeptic symptoms included the following:
1) Postprandial fullness
2) Early satiety
3) Epigastric pain or burning
4) Heartburn and reflux
5) Nausea and vomiting.
2.8 Statistical analysis
The data is presented in terms of mean ± sd for numeric variables and frequency distribution for the qualitative variables. Quantitative variables are compared across various follow-ups using paired t-test. A p-value <0.05 is considered statistically significant. The data is entered and stored in the MS Excel package while Statistical Package for Social Sciences (SPSS) version 16.0 software is used for statistical analysis.
3. Observations and Results
The flow of the study is as depicted in figure 1. The mean age of our patients was 47.2 ± 15.42. The youngest patient was 18 years old and the oldest was 88 years of age. Maximum number of patients belonged to 30-40 year age group followed by 40-50 year age group. The age distribution is as shown in figure 2. Our population consisted of 62% females and 38% males. Laparoscopic cholecystectomy was seen to improve dyspepsia scores in 252 (81.82%) patients at the end of 1 month and 293 (95.13%) patients at the end of 6 months. Out of 308, 44 (14.29%) and 12 (3.90%) patients had no relief in dyspepsia at the end of 1 month, 12 (3.90%) patients had worsening symptoms. The number reduced to 3 (0.97%) after 6 months (figure 3). The mean GDSS scores significantly improved at one and six months after surgery. At one month follow up the mean GDSS dropped from11.9 ± 2 to 2.5 ± 1.2. This further decreased to 1.40 ± 1.1 at the 6 month follow up. (GDSS: p<0.001, Table 2). As seen in figure 4 and Table 3, the frequency of symptoms mean score shows a decline from 2.95 ± 1.03 preoperatively to 2.26 ± 0.9 at 1 month and a further decrease to 0.49 ± 0.62 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on normal activities mean score shows a decline from 1.45 ± 0.68 preoperatively to 0.98 ± 0.82 at 1 month and a further decrease to 0.15 ± 0.38 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on time off work mean score shows a decline from 1.41 ± 0.5 preoperatively to 0.72 ± 0.7 at 1 month and a further decrease to 0.14 ± 0.37 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on consultations with medical professionals mean score shows a decline from 1.69 ± 0.47 preoperatively to 1.29 ± 0.62 at 1 month and a further decrease to 0.39 ± 0.5 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on GP visits mean score shows a decline from 0.27 ± 0.44 preoperatively to 0.13 ± 0.34 at 1 month and a further decrease to 0.03 ± 0.46 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on tests for dyspepsia mean score shows a decline from 0.29 ± 0.5 preoperatively to 0.10 ± 0.3 at 1 month and a further decrease to 0.06 ± 0.23 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on self medication mean score shows a decline from 1.65 ± 0.48 preoperatively to 1.29 ± 0.62 at 1 month and a further decrease to 0.86 ± 0.57 at the 6 month follow up. The decrease was statistically significant (p<0.001). The effect on medications prescribed by doctors mean score shows a decline from 1.55 ± 0.51 preoperatively to 1.04 ± 0.56 at 1 month and a further decrease to 0.46 ± 0.51 at the 6 month follow up. The decrease was statistically
significant (p<0.001).
As seen in figure 5, 7.14% had complaints of dyspepsia on most days pre operatively whereas none of the 308 patients had to similar frequency at the end of 6 months. 56.16% were completely relieved at the 6th monthly follow up whereas 39.93% patients had symptoms on only 1 or 2 days. 55.84% patients complained that dyspepsia interfered with their normal activities (eating, sleeping or socialising) regularly preoperatively however 85.71% patients claimed that dyspepsia no longer affected their day to day life 6 months after laparoscopic cholecystectomy.
41.23% patients complained that they have lost more than 7 days of work due to dyspepsia in the past 6 months pre operatively. 58.44% patients complained that they have lost 1-7 days of work due to dyspepsia in the past 6 months pre operatively. 87.01% patients reported that dyspepsia was no longer causing loss of days at work at the 6th month of post operative follow up. 68.83% patients complained that they had attended a doctor due to dyspepsia twice in the last 6 months pre operatively 61.68% patients said that they no longer had to visit a doctor 6 months after laparoscopic cholecystectomy for dyspepsia. 24.35% patients had done 1 test for their dyspepsia in the last 6 months preoperatively. The number reduced to 10.06% patients at 1st month follow up and 5.51% at 6th month of follow up.
73.37% patients had not done any test for their dyspepsia in the last 6 months preoperatively. The number increased to 89.93% patients at 1st month follow up and 94.4% at 6th month of follow up. 65.25% patients had self medicated twice in the last 6 months preoperatively. Only 1 patient had not self medicated in the last 6 months preoperatively. 80.51% patients did not feel the need for self medication after 6 months post surgery. No patient used the drugs prescribed by a doctor for more than 3 months. 54.87% patients had used drugs prescribed by doctor for 1-3 months in the last 6 months preoperatively. 77.27% patients had used drugs prescribed by doctor for less than 1 month in the last 6 months preoperatively. 68.83% patients continued using drugs for less then a month at 1st month of post operative follow up and 45.12% patients at 6th month of post operative follow up. 54.22% patients did not require any drugs 6th month post surgery. Further details can be visualised in supplemental digital content 3. When asked about overall surgery satisfaction 94% i.e 290 patients were satisfied and 6% i.e 18 patients were unsatisfied with the outcome of surgery.
|
(A) Frequency of dyspeptic symptoms |
SCORE |
(C) Time off work
|
SCORE |
(F) Tests for dyspepsia
|
Score |
|
Never |
0 |
None |
0 |
None |
0 |
|
On only 1 or 2 days |
1 |
1-7 days |
1 |
One |
1 |
|
On approximately 1 day per month |
2 |
More than 7 days |
2 |
Two |
2 |
|
On approximately 1 day per week |
3 |
(D) Consultation with medical professional |
Score |
(G) Treatment for dyspepsia (1) Self medication |
Score |
|
On approximately 50% of days |
4 |
None |
0 |
None |
0 |
|
On most days |
5 |
Once |
1 |
Once |
1 |
|
Twice |
2 |
Twice |
2 |
||
|
(B) Effect on normal activities |
Score |
(E) GP visits to patients home |
Score |
(2) Drugs prescribed by a doctor |
Score |
|
Never |
0 |
None |
0 |
Never |
0 |
|
Sometimes |
1 |
Once |
1 |
Less than 1 month |
1 |
|
Regularly |
2 |
Twice |
2 |
1-3 months |
2 |
|
More than 3 months |
3 |
Table 1: Details of GDSS.
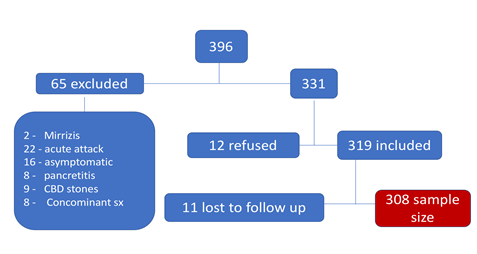
figure 1: Flow of study depicting number of patients from the initial phase to the final study group.
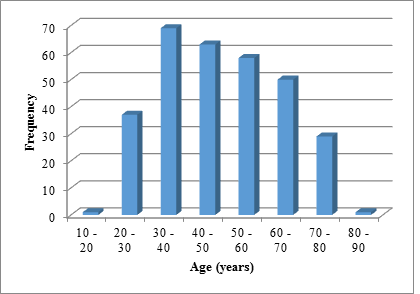
figure 2: figure showing age distribution.
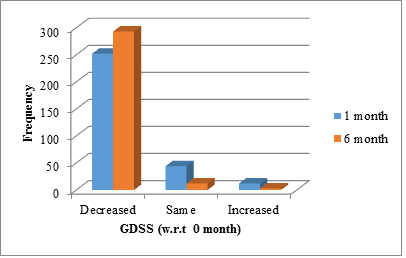
figure 3: Graph depicting comparative change in GDSS at 1 month and 6 month with respect to 0 months.
|
GDSS |
0 month |
1 month |
6 month |
|
Mean ± SD |
11.90 ± 2 |
2.50 ± 1.2 |
1.40 ± 1.1 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
Table 2: Table depicting Mean ± SD GDSS.
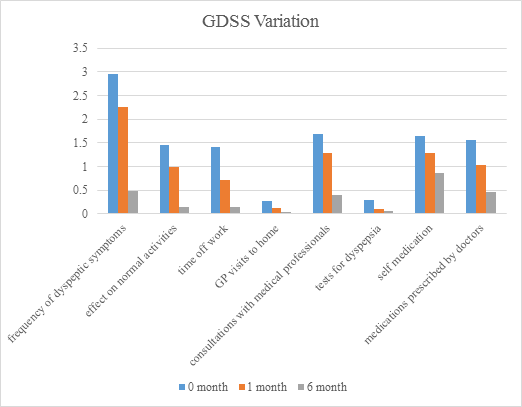
figure 4: Graph depicting overall change in individual components of GDSS.
|
Frequency of dyspeptic symptoms |
|||
|
Mean ± SD |
2.95 ± 1.03 |
2.26 ± 0.9 |
0.49 ± 0.62 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
|
Effect on normal activities |
|||
|
Mean ± SD |
1.45 ± 0.68 |
0.98 ± 0.82 |
0.15 ± 0.38 |
|
p-value (vs 0 month) |
- |
<0.001 |
<0.001 |
|
Consultations with medical professionals |
|||
|
Mean ± SD |
1.69 ± 0.47 |
1.29 ± 0.62 |
0.39 ± 0.5 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
|
GP visits to home |
|||
|
Mean ± SD |
0.27 ± 0.44 |
0.13 ± 0.34 |
0.03 ± 0.46 |
|
p-value (vs 0min) |
- |
<0.001 |
0.091 |
|
Tests for dyspepsia |
|||
|
Mean ± SD |
0.29 ± 0.5 |
0.1 ± 0.3 |
0.06 ± 0.23 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
|
Self medication |
|||
|
Mean ± SD |
1.65 ± 0.48 |
1.29 ± 0.62 |
0.86 ± 0.57 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
|
Medications prescribed by doctors |
|||
|
Mean ± SD |
1.55 ± 0.51 |
1.04 ± 0.56 |
0.46 ± 0.51 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
|
Time off work |
|||
|
Mean ± SD |
1.41 ± 0.5 |
0.72 ± 0.7 |
0.14 ± 0.37 |
|
p-value (vs 0min) |
- |
<0.001 |
<0.001 |
Table 3: Table depicting Mean ± SD of individual components of GDSS.
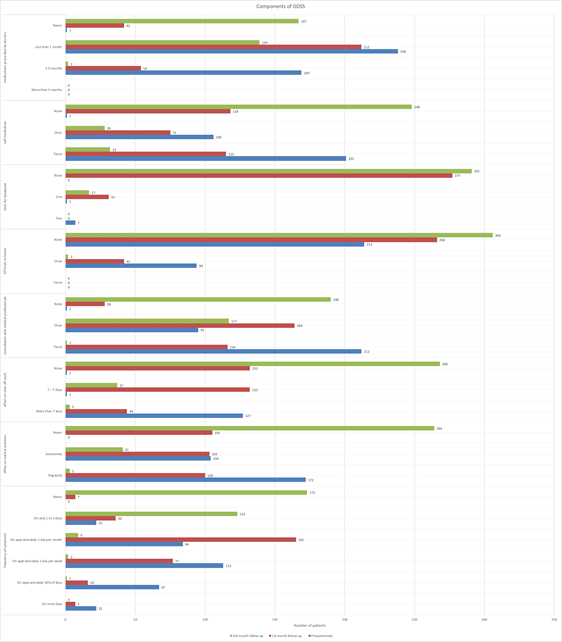
figure 5: Depicting distribution of patients with regards to individual components of GDSS.
4. Discussion
4.1 Dyspepsia
Dyspepsia is a common symptom with an extensive differential diagnosis and a heterogeneous pathophysiology [11]. Although it affects 1/4th of the population dyspepsia doesn’t bring most patients to seek out medical care. Also only 1/4th dyspeptic patients suffer from an organic cause. The majority of patients i.e an astonishing 3/4th have functional (idiopathic or nonulcer) dyspepsia which fail to pinpoint a cause on diagnostic evaluation [12-14]. Worldwide dyspepsia affects 5-11 percent population [44]. Dyspepsia is a poorly understood concept when it comes to pathophysiology. A lot of mechanisms have been hypothesized. These mechanisms may differ between subtypes of functional dyspepsia [15].
- Gastric motility and compliance-There have been several associations with motility disorders [16]
- Visceral hypersensitivity-Coexistence of visceral hypersensitivity and functional dyspepsia occurs along with delayed gastric emptying [17]
- Helicobacterpylori infection- pylori causes an inflammatory response which may decrease the discomfort threshold to gastric distension by causing alterations in the enteric or central nervous system [18]
- Altered gut microbiome-Alterated microbiome has been implicated in causing dyspepsia [19]
- Duodenal inflammation-Duodenal eosinophils have found to be raised in patients with early satiety. An association between duodenal inflammations and functional dyspepsia has been implicated [20]
- Psychosocial dysfunction-The interaction between psychosocial factors and functional dyspepsia is complicated [21].
4.2 Assessing Dyspepsia
There are a few scores which have been used to assess dyspepsia. These range from validated scores like Glassgow dyspepsia severity score (GDSS), Leeds score, Napean score, Buckley score to indigenous scores. Whether a qualified personnel should interview a study object or a questionnaire should be used has always been a matter of debate [22-24]. The argument which favours the use of a questionnaire is that a self-assessment questionnaire will make the patient report more complaints than will be revealed by a professional interview as seen in a study by Erim et al. wherein he assessed the quality of life of liver transplant patients [25]. The argument against especially in our study population is that the presence of an appropriately qualified interviewer helps objectify symptoms. The Glassgow dyspepsia score focuses on several aspects of dyspepsia: firstly, the frequency of dyspepsia symptoms and the effect that they have on normal activities and ability to work; secondly, the need for consultations with physicians for dyspepsia and the need for diagnostic investigations for dyspepsia and thirdly, the need for over the counter and prescription medication for dyspepsia. It is worth mentioning that for the GDSS, patients are asked to rate their symptoms over the last six months [9, 10].
Measuring and quantifying dyspepsia is considered problematic due to the vagueness of its presentation Outcome measures can be broadly categorised as:
1) Global scales: A Likert scale ( interval scale) that has graded definitions for the severity of symptoms, ranging from none to very severe. It has to be kept in mind that clinical significance of grades is relevant.Obviously complete disappearance of symptoms clearly is a logical end point and so are symptoms which are absolutely stagnant. But the problem arises in interpreting partial improvement.
2) Generic instruments: Quality of life questionnaires eg. psychological general well being (PGWB) index.
3) Disease specific instruments:
- a) Unidimensional: Assess only gastrointestinal symptoms eg. gastrointestinal symptom rating scale (GSRS)
- b) Multidimensional: Includes domains such as emotional or social functioning and the impact that symptoms have on daily activities. Eg. multidimensional scale is the Glasgow dyspepsia severity score (GDSS).
4.3 The Glassgow dyspepsia severity score
Developed by El Omar et al. the GDSS is a multimodality severity symptom score which analyses various aspects of dyspepsia especially the extent to which dyspepsia affects the patients lifestyle, the consultations required, tests taken and need for medications. The score was developed at the Western Infirmary in Glasgow, United Kingdom. The mean score in the general population was 1.16 compared with 10.5 in the non ulcer dyspepsia patients and 11.1 in the duodenal ulcer group. It has been assessed for validity and reproducibility and has been extensively used [26-28]. 308 patients having gallstones suffering from dyspeptic symptoms in a tertiary care hospital were included in this study. Most patients with cholelithiasis were in the age group of 30-40 years. In western population maximum incidence is noted in age group of 50-59 years [29]. In our study patients were between 18-88 years if age. Cholelithiasis is uncommon in first two decades of life. In India Rattan et al. have reported 6 years old with non hemolytic gall stones [30]. Youngest reported infant with gall stones in worldwide is being 41 days old by as reported by Morales et al. [31]. In our study females were affected predominantly with a F:M ratio being 1.63:1. In western literature this ratio varies from 2:1 to 4:1. Raza et al. [32] reported female to male ratio 5:1, while Ghosh et al. reported it to be 6:1 [33]. Table 4 shows follow up period of other studies along with sample size given below,
|
Study |
Follow up period |
Sample size |
|
Mehrvaz et al. [34] |
4 months |
175 |
|
Amir et al. [35] |
6 weeks |
200 |
|
Mertens et al. [36] |
6 months |
129 |
|
Gi Hyun Kim et al. [37] |
6 months |
65 |
|
Aggarwal et al. [38] |
2 months |
27 |
|
Schmidt et al. [39] |
6 months |
128 |
|
Borly et al. [40] |
2 years |
80 |
|
Lorussu et al. [41] |
1 year |
52 |
|
Middlefart [42] |
10 years |
519 |
|
Our study |
6 months |
308 |
Table 4: Table showing Follow up and sample sizes of other studies.
We followed our patients for 6 months and had a sample size of 308 patients. As can be seen our sample size is larger than most studies with the exception of the one by Middlefart et al. which was conducted in the pre laparoscopy era on patients undergoing open cholecystectomy. Amir, Mehrvaz and Mertens et al. studied patients with both dyspeptic as well as biliary symptoms (biliary colic and cholecystitis). Gi Hyun Kim et al. Analysed dyspepsia as well as colonic symptoms. Apart form our study we found only two others-Schmidt et al. and Aggarwal et al. included only patients with purely dyspeptic symptoms. Our study considered dyspeptic symptoms as a symptom complex and did not differentiate between individual complaints. Early satiety, epigastric pain or burning, heartburn and reflux, nausea and vomiting and postprandial fullness were asked for and the presence of any of these were considered significant. The studies by Mehrvarz et al., Amir et al. and Gi Hyun Kim gave a lot of importance to individual symptoms and even tried to establish them as predictors. However we felt that dyspepsia is a very vague symptom and to elicit it in history especially in our sub population where more often than not it is a component of patient complaints was considered as an unnecessary excercise. What was more essential was how much it affected the patients routine activity and the extent to which it would necessitate contact with the healthcare system. In our study 14.29% had persistent symptoms at the end of 1 month and 12 3.90% patients had no relief in dyspepsia at the end of 6 month. Comparison with other studies is shown in Table 5.
In the study by Amir et al. de novo symptoms developed in 5% of the patients. Compared to 3.9% increase in GDSS in our patients at the end of 1 month and 0.97% increase in GDSS at the end of 6 months. Although the number was small in both the studies it does correlate with the observations made by Schmidt et al. that these symptoms may have been due to Functional Gastrointestinal disease and not due to cholelithiasis. All our parameters including frequency of symptoms, time off work, consultations, home visits, tests for dyspepsia and use of medications decreased significantly over 6 months. When asked about overall surgery satisfaction 94% i.e 190 patients were satisfied and 6% patients were unsatisfied with the outcome of surgery. Craig et al. conclusively determined that the major correlate of not achieving a very successful outcome (15.2% of patients) was the persistence of symptoms post surgery. Symptoms categorized as dyspeptic were more likely to persist than were biliary symptoms [43].
|
Study |
Persistent dyspeptic symptoms |
|
Amir et al. [35] |
38% |
|
Mertens et al. [36] |
57.3% |
|
Gi Hyun kyun et al. [37] |
55.4% |
|
Schmidt et al. [39] |
57% |
|
Mehrvaz et al. [34] |
30% |
|
Craig et al. [43] |
40.2% |
|
Our study |
14.29% (1 month) and 3.90% (6 months) |
Table 5: Table showing persisting symptoms in other studies.
Study Strengths
- The study was a prospective one.
- This study used a validated symptom score to assess dyspepsia.
- The results were assessed by a qualified interviewer along with a pre determined questionnaire.
Study limitations
- This was a single centre study.
- Cause for dyspepsia not relieved by laparoscopic cholecystectomy was not found out.
- Memory recall bias may have come into play as patients were followed up for 6 months post surgery.
5. Summary
There is a global increase in incidentally detected gallstones. Dyspepsia has been know to be caused by gallstones. There is no clear cut guideline for performing laparoscopic cholecystectomy to alleviate dyspepsia. This study was carried out on 308 participants to determine objectively if laparoscopic cholecystectomy has any role in relieving dyspepsia. The participants were evaluated using a validated multimodality global symptom score-“Glassgow dyspepsia severity score” preoperatively, at 1 months and at 6 months. Laparoscopic cholecystectomy was seen to improve dyspepsia scores in 252 (81.82%) patients at the end of 1 month and 293 (95.13%) patients at the end of 6 months Out of 308, 44 (14.29%) at the end of 1 month and 12 (3.90%) at the end of 6 months patients had no relief in dyspepsia. At the end of 1 month 12 patients (3.90%) had worsening symptoms.The number reduced to 3 (0.97%) after 6 months. The mean GDSS scores significantly improved at one and six months after surgery (p<0.001). Patient satisfaction was co-related with relief of symptoms. The study concludes that in cholelithiasis patients presenting with dyspeptic symptoms do find relief after laparoscopic cholecystectomy, however the symptoms may persist due to a functional component and patients should be counselled adequately in the preoperative period.
6. Conclusion
Our study concludes the following
- Most symptomatic patients undergoing laparoscopic cholecystectomy are objectively relieved of dyspeptic symptoms.
- Very few patients have persistent symptoms even after 6 months.
- Patients tend to associate relief of dyspepsia with successful outcome of surgery.
Effect on clinical practise
- It is extremely essential that patients be counselled in detail about the possibility of persistence of dyspeptic symptoms which may in-fact be functional/inorganic.
- Significant stress should be given to rationale for gallbladder removal and clarification of patient symptom relief.
The fact that laparoscopic cholecystectomy may or may not cure dyspepsia should be brought across very strongly especially to patients who primarily present with dyspeptic symptoms.
References
- Branka Radojcic, Radoica Jokic, Slobodan Grebeldinger, et al. History of minimally invasive surgery. Med Pregl 62 (2009): 597-602.
- Vecchio R, MacFayden BV, Palazzo F. History of laparoscopic surgery. Panminerva Med 42 (2000): 87-90.
- Litynski GS. Erich Mühe and the rejection of laparoscopic cholecystectomy (1985): a surgeon ahead of his time. JSLS 2 (1998): 341-346.
- Reddick EJ, Olsen DO. Laparoscopic laser cholecystectomy. A comparison with mini-lap cholecystectomy. Surg Endosc 3 (1989): 131-133.
- Unisa S, Jagannath P, Dhir V, et al. Population-based study to estimate prevalence and determine risk factors of gallbladder diseases in the rural Gangetic basin of North India. HPB (Oxford) 13 (2011): 117-125.
- Jackson PG, Evans SRT. Biliary system. In Eds.: Beauchamp RD, Evers BM, Mattox KL. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice, (19th) Philadelphia, PA: Saunders Elsevier (2008): 1485-1501.
- Turan Acar, Erdinç Kamer, Nihan Acar, et al. Laparoscopic Cholecystectomy in the Treatment of Acute Cholecystitis: Comparison of Results between Early and Late Cholecystectomy. The Pan African Medical Journal 26 (2017): 49.
- Egbert AM. Gallstone symptoms. Myth and reality. Postgrad Med 90 (1991): 119-126.
- El-Omar EM, Banerjee S, Wirz A, et al. The Glasgow dyspepsia severity score-a tool for the global measurement of dyspepsia. Eur J Gastroenterol Hepatol 8 (1996): 967-971.
- Tytgat UA. Grading and staging in Gastroentrology. (1st) (2008): 120.
- Talley NJ, Ford AC. Functional Dyspepsia. N Engl J Med 373 (2015): 1853.
- Bytzer P, Talley NJ. Dyspepsia. Ann Intern Med 134 (2001): 815.
- Koch KL, Stern RM. Functional disorders of the stomach. Semin Gastrointest Dis 7 (1996): 185.
- Malagelada JR. Functional dyspepsia. Insights on mechanisms and management strategies. Gastroenterol Clin North Am 25 (1996): 103-112.
- Vanheel H, Carbone F, Valvekens L, et al. Pathophysiological Abnormalities in Functional Dyspepsia Subgroups According to the Rome III Criteria. Am J Gastroenterol 112 (2017): 132.
- Tack J, Piessevaux H, Coulie B, et al. Role of impaired gastric accommodation to a meal infunctional dyspepsia. Gastroenterology 115 (1998): 1346.
- Mertz H, Fullerton S, Naliboff B, et al. Symptoms and visceral perception in severe functional and organic dyspepsia. Gut 42 (1998): 814.
- Bercík P, De Giorgio R, Blennerhassett P, et al. Immune-mediated neural dysfunction in a murine model of chronic Helicobacter pylori infection. Gastroenterology 123 (2002): 1205.
- Zhong L, Shanahan ER, Raj A, et al. Dyspepsia and the microbiome: time to focus on the small intestine. Gut 66 (2017): 1168.
- Talley NJ, Walker MM, Aro P, et al. Non-ulcer dyspepsia and duodenal eosinophilia: an adult endoscopic population-based case-control study. Clin Gastroenterol Hepatol 5 (2007): 1175.
- Mak AD, Wu JC, Chan Y, et al. Dyspepsia is strongly associated with major depression and generalised anxiety disorder-a community study. Aliment Pharmacol Ther 36 (2012): 800.
- Mertens MC, Roukema JA, Scholtes VP, et al. Risk assessment in cholelithiasis: is cholecystectomy always to be preferred? J Gastrointest Surg 14 (2010): 1271-1279.
- Sondenaa K, Nesvik I, Solhaug JH, et al. Randomization to surgery or observation in patients with symptomatic gallbladder stone disease. The problem of evidence-based medicine in clinical practice. Scand J Gastroenterol 32 (1997): 611-616.
- Weinert CR, Arnett D, Jacobs D, et al. Relationship between persistence of abdominal symptoms and successful outcome after cholecystectomy. Arch Intern Med 160 (2000): 989-995.
- Erim Y, Beckmann M, Valentin-Gamazo C, et al. Quality of life and psychiatric complications after adult living donor liver transplantation. Liver Transpl 12 (2006): 1782-1790.
- Yamawaki H, Futagami S, Shimpuku M, et al. Impact of Sleep Disorders, Quality of Life and Gastric Emptying in Distinct Subtypes of Functional Dyspepsia in Japan. Journal of Neurogastroenterology and Motility 20 (2014): 104-112.
- McColl KEL, El-Nujumi A, Murray LS, et al. Assessment of symptomatic response as predictor ofHelicobacter pylori status following eradication therapy in patients with ulcer Gut 42 (1998): 618-622.
- Heaney A, Collins JS, Watson RG, et al. A prospective randomised trial of a “test and treat” policy versus endoscopy based management in young Helicobacter pylori positive patients with ulcer-like dyspepsia, referred to a hospital clinic. Gut 45 (1999): 186-190.
- Chuttani PN. Cholelithiasis in India. Proceedings of the third world congress of gastroenterology, vol 4, Tokyo Bassel Karger (1996): 163.
- Ratan KN, Sodhi D, Geeta G, et al. Gall stones in children (non hemolytic). Indian J Med Science 49 (1995): 32-34.
- Morales D. Acute cholecystitis and cholelithiasis in a 41 day old newborn. British journal of surgery 82 (1995): 13.
- Raza MH, Khan MA. Gall stone disease. Indian journal of Surgery 52 (1990): 415-420.
- Ghosh SK, Das KN, Dose D, et al.: Aetiopathogenesis of chronic cholecystitis in Gangetic West Bengal. A study of 300 cases: Indian Journal of Surgery 57 (1995): 313-315.
- Mehrvarz SH, Fanaei SA. The role of laparoscopic cholecystectomy in alleviating gastrointestinal symptoms.International Journal of Medicine and Medical Sciences 2 (2010): 153-157.
- Amir M, Zubair M. Influence of cholecystectomy on symptomatic cholelithiasis: can all symptoms be improved?. RMJ 34 (2009): 141-144.
- Mertens C, De Vries J, Scholtes VPW, et al. Prospective 6 Weeks Follow-up Post-cholecystectomy: The Predictive Value of Pre-Operative Symptoms J Gastrointest Surg 13 (2009): 304-311.
- Gi Hyun Kim, Hyo Deok Lee. Fate of Dyspeptic or Colonic Symptoms After Laparoscopic Cholecystectomy, J Neurogastroenterol Motil 20 (2014): 253-260.
- Manas Aggarwal, Nitin Agarwal, Tushar S Mishra, et al. Is laparoscopic cholecystectomy effective in relieving dyspepsia in patients of cholelithiasis? A prospective study. Tropical Gastroenterology 37 (2016): 86-92.
- Malte Schmidt, Karl Sondenaa. Post-cholecystectomy symptoms were caused by persistence of a functional gastrointestinal disorder, World J Gastroenterol 2818 (2012): 1365-1372.
- Borly L, Anderson IB, Bardram L, et al. Preoperative prediction model of outcome after Cholecystectomy for symptomatic gallstones. Scand J Gastoenterol 11 (1999): 1144-1152.
- Lorusso D, Porcelli P, Pezzolla F, et al. Persistent dyspepsia after laparoscopic cholecystectomy. The influence of psychological factors.Scand J Gastroenterol 38 (2003): 653-658.
- Middlefart HV, Kristensen JU, Laursen CN, et al. Pain and dyspepsia after elective and acute cholecystectomy. Scand J Gastroenterology 33 (1998): 10-14.
- Craig R Weinert, Donna Arnett, David Jacobs, et al. Relationship Between Persistence of Abdominal Symptoms and Successful Outcome After Cholecystectomy. Arch Intern Med 160 (2000): 989-995.
- Ford AC, Marwaha A, Sood R, et al. Global prevalence of, and risk factors for, uninvestigateddyspepsia: a meta-analysis. Gut 64 (2015): 1049.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 