Retroperitoneal Sarcoma Mimicking a Testicular Malignancy
Girish Bakhshi, Aishwarya Dutt*, Sushrut Baligar, Rajalakshmi V, Chettubattina Ravi Teja, Sampada Joshi, Madhu Jha
Department of General Surgery, Grant Government Medical College and Sir J. J. Group of Hospitals, Mumbai, Maharashtra, India
*Corresponding Author: Aishwarya Dutt, Department of General Surgery, Grant Government Medical College and Sir J. J. Group of Hospitals, Mumbai, Maharashtra, India
Received: 18 Febraury 2022; Accepted: 25 Febraury 2022; Published: 11 April 2022
Article Information
Citation: Girish Bakhshi, Aishwarya Dutt, Sushrut Baligar, Rajalakshmi V, Chettubattina Ravi Teja, Sampada Joshi, Madhu Jha. Retroperitoneal Sarcoma Mimicking a Testicular Malignancy. Journal of Surgery and Research 5 (2022): 185-193.
View / Download Pdf Share at FacebookAbstract
Low grade fibromyxoid sarcoma is a rare soft tissue sarcoma with typical histological findings. Growing as a painless mass, it is commonly seen in proximal extremities and trunk. Absence of strict protocols in diagnosis causes difficulty in its approach. Present case is a 52year male who presented with abdominal lump and absent right testis. Clinico-radiological diagnosis suggested a testicular malignancy. Histology showed low grade fibromyxosarcoma. A brief case report with review of literature is presented.
Keywords
<p>Low grade fibromyxoid sarcoma (LGFMS), Retroperitoneum, Soft tissue tumor, Testicular malignancy</p>
Article Details
1. Introduction
Soft tissue malignancies are rare tumors which according to The world Health Organisation(WHO) are further subclassified in approximately 70 subtypes, each characterized by a distinct morphology, low grade fibromyxoid sarcoma(LGFMS) being one of them. The majority of these are initially misdiagnosed as benign entities, such as a fibroma or fibromatosis, and later presented with metastases. One such differential is a testicular neoplasm in a patient who presents with abdominal lump and absent testis in rt scrotum. It is seen that 1% of all cancers found in the global male population are represented by testicular neoplasms which are seen 5-10 times more commonly in cryptorchid testis. Most common type of testicular neoplasm seen in undescended testis are seminomas(74%) [1]. LGFMS occur as a malignant, but often late metastasizing tumor in the proximal extremities and trunk. Sporadically they may be found in unusual locations, such as the retroperitoneum, head or the chest wall [2]. Histologically, they are described as bland spindle cell tumors with angulated nuclei, scant cytoplasm arranged in a whorled pattern with cells that are frequently immunoreactive for mucin. It is mostly treated with surgical excision with proper follow up in view of the possibility of metastasis which is seen most commonly in the lungs, pleura and chest wall [3,4]. We present a case of low grade fibromyxoid sarcoma of retroperitoneum with features clinically suggestive testicular malignancy.
2. Case Description
A 52-year-old male came with complaints of abdominal mass for 6 months which rapidly progressed to accommodate the entire abdomen. He also had associated bilateral lower limb swelling. He has a history of absent right testis and also a history of right hernioplasty done 8 years prior. Radiological examination showed a well defined solid heterogeneously enhancing lesion with fatty areas. It extended anteriorly up to anterior abdominal wall with loss of fat planes. This showed its attachment to the previous operated suture line. Posteriorly, it compressed on the distal abdominal aorta and its branches. The mid segment of right external artery was encased by the lesion. There was associated compression of the sigmoid colon to the left and displacement of intestinal loops supero-laterally. Inferiorly, the mass extended to the right inguinal region. There was displacement of the prostate and bladder inferolaterally with loss of fat planes with the bladder. The right ureter was also displaced to the left side with associated compression of both ureters causing bilateral hydroureter with hydronephrosis (Figure 1(a) and (b)). The clinical presentation along with the radiological imaging was suggestive of a right testicular malignancy which created a dilemma for the further management and diagnosis. Testicular tumor markers were evaluated which only showed an LDH level of 536 IU/L. This suggested the possibility of a testicular seminoma. This was an additional factor that caused a disparity in the possible diagnosis as the radiological imaging directed towards a non seminomatous germ cell tumor (NSGCT) instead of a seminoma. At the same time, this could not completely rule out the possibility of a soft tissue sarcoma. The radiological imaging was taken into consideration not only for diagnostic purposes, but also to plan for the approach of excision of the tumor intraoperatively. The involvement of the surrounding structures and the vascular pedicles supplying the tumor from the external iliac artery was carefully reviewed to prepare for intraoperative findings as well. The patient underwent a bilateral DJ stenting in view of the hydronephrosis and hydroureter prior to the planned operation. Preoperatively, a debulking surgery was planned. Intraoperatively, there was a complete resection possible. The prior sutures in the right inguinal region were appreciated of the previous right inguinal hernioplasty, where the tumor was attached as well. The only difficulty found during the operation was at the point of approximation with the right external artery, which was where the feeding vessels were also identified. Prior to ligation of the vascular pedicle the distal pulsations were felt which was confirmed again after ligation and dissection of the tumor around the external iliac vessels. Once the entire tumor was resected it was identified to be originating from the posterior retroperitoneal surface of the bladder. The specimen was sent for histopathological examination. Post operative period was unremarkable. On gross examination, the specimen had a well-defined nodular surface, greyish white in colour. It was firm in consistency and the cut section showed fibrofatty tissue with areas of vascularity (Figure 2(a) and (b)). On histological examination, there were fusiform cells arranged loosely in a myxoid matrix. The cells had scanty cytoplasm with uniform elongated densely staining nuclei. Infrequent mitosis was seen with curvilinear vessels scattered within the tumor (Figure 3(a)). Immunohistochemical markers were tested which showed positivity to SMA (Figure 3(b)), CD34, MDM2, CDK4 and negativity to S-100 protein, MSA, DOG-1, caldeson, STAT-6, desmin and MUC-4. These features all directed towards a diagnosis of low grade myxofibrosarcoma. Post operatively, the DJ stents were removed and once patient was discharged. Follow up after 3 months has shown to be disease and symptom free. Further regular follow up after 6 months was advised for clinical and radiological follow up to rule out any recurrence or metastasis. Although the diagnosis pointed in favour of a testicular malignancy on clinical and radiological investigations, the final excision along with histopathological correlation helped in resolving this dilemma and provided the diagnosis of a low grade myxofibrosarcoma.
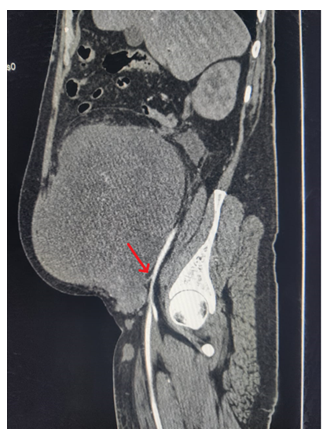
Figure 1a: Sagittal view of contrast enhanced computed tomography (arterial phase) showing the heterogeneously enhaced lension. Arrow points to the vascular pedicle from the external iliac artery.
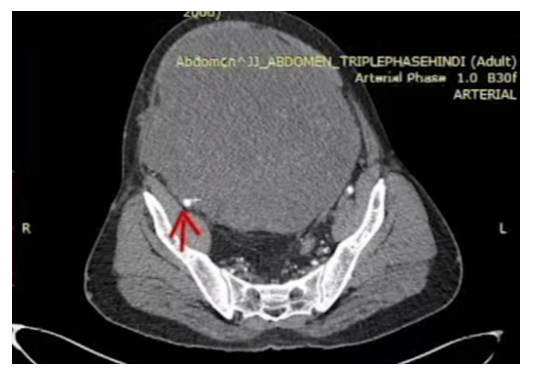
Figure 1b: Transverse section of contrast enhanced computed tomography (arterial phase) showing the tumour. Arrow points to the vascular oedicle from the external iliac artery.
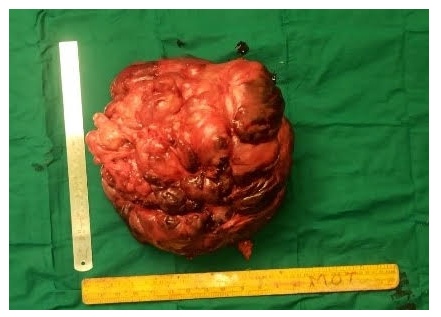
Figure 2a: gross specimen after its exicion from the retroperitoneun. It was seen to be a lobulated mass which was hard in consistency.
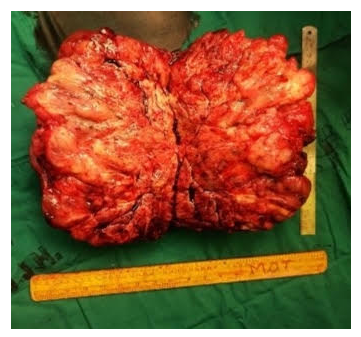
Figure 2b: Cut section of the specimen after its excision from the retroperitoneum. Fibrofatty tissue with high vascularity noted.
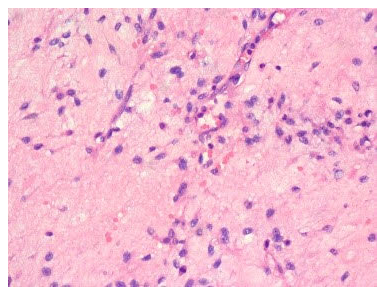
Figure 3a: H & E staining showing the typical oval cells in myxoid stroma suggestive of a fibromxosarcoma.
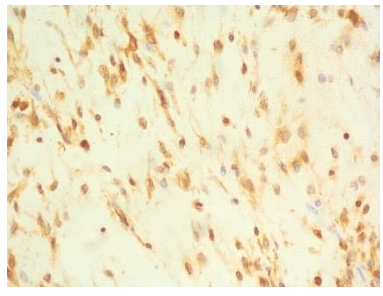
Figure 3b: immunohistochemical staing showing positivity to SMA suggestive of a low grade fibromyxoid sarcoma.
3. Discussion
Low grade fibromyxoid sarcoma are a rare type of fibromyxoma tumors which present as deep soft tissue tumors of the proximal extremities and are rarely seen in the abdominopelvic region and retroperitoneum, including those arising from enteric viscera. The unusual location of these tumors led to the misdiagnosis of other mesenchymal tumors such as desmoid-type fibromatosis, peripheral nerve sheath tumors, gastrointestinal tumors, dedifferentiated liposarcoma and inflammatory myofibroblastic tumor [4]. They usually present as a painless, slow growing mass with compressive complications as seen in this case. LGFMS can present with late metastases, most commonly to the lungs [3]. The incidence of retroperitoneal origin of low grade fibromyxosarcomas have been limited. A case series of 73 patients with Low grade fibromyxoid sarcoma and hyalinising spindle cell tumor with giant rosettes was done by Folpe et al in 2000 which consisted of only one case arising from the retroperitoneum [5]. Another study in 1995 by Goodlal et al. consisted of eleven cases out of which only one was found to retroperitoneal in origin [6]. This was similarly seen in a case series of 33 patients by Evans et al. in 2011 which consisted of only one retroperitoneal low grade fibromyxoid sarcoma [3]. A recent study of 13 cases by Din et al of abdominopelvic and retroperitoneal low grade fibromyxoid sarcomas supported 3 cases of retroperitoneal tumors of this variety [4]. Similarly, testicular malignancies in the abdomen also present as a painless mass. Undescended testis is seen in about 1%-6% of full-term and up to 45% of premature male infants. There can be spontaneous descent of the testis within the first 6 months of life but it is unlikely for spontaneous descent after 1 year of age. Testicular malignancies are seen in 3.5-14.5% of undescended testis [7]. Any patient with an undescended testis and abdominal mass should hence always be evaluated for possible testicular tumors. Preoperative imaging is done with ultrasound, followed by computed tomography and magnetic resonance imaging. For a testicular malignancy, ultrasound, using a high frequency transducer (7-10Mhz), has a sensitivity of 92% to 98% and specificity of 95% to 99.8% [8]. Seminomas can show a homogenous and hypoechoic lesion with few calcifications and cystic areas whereas nonseminomatous germ cell tumors (NSGCT) show heterogenous lesions with few cystic spaces and calcifications [8]. LGFMS also show a picture similar to NSGCT. This can be compared to the heteregenously enhancing lesions visualised in NSGCT along with possible cystic lesions. In the present case, the presence of the heterogenous enhancement in the CT scan was what indicated the possibility of a testicular neoplasm. MRI can be more helpful than CT in the assessment of various muscle disorders due to its subtle multisequence imaging. On MRI, LGFMS is inhomogeneous, owing to its two distinct internal zones: myxoid and fibrous. Magnetic resonance imaging show frequent hypointense or isointense muscle in fluid-sensitive MRI sequences and often shows enhancing gyriform patterns [9]. In cases of testicular germ cell tumors T1-weighted images show hypointense or heterogenus lesions, similar to the testis, with variable signal intensity on T2- weighted imaging [10]. MRI was not carried out in this study as the ideal treatment of resection of the tumor and further histopathological assessment was considered to be the final and best diagnostic method. It is important to attempt an excision with negative margins to prevent any further recurrences. Histopathological assessment of the tumor confirmed the diagnosis of a LGFMS in this case which cleared the dilemma which was present due to clinic-radiological investigation. The morphological features as described by Folpe et al. in 2014, shows a circumscribed but subtly infiltrative fashion with hypocellular areas of collagenous zones and myxoid nodules with hypercellular regions of a whirling growth pattern and curvilinear vessels. The cells show low mitotic activity with absence of necrosis. There are a minority of cases that show increased cellularity and nuclear atypia as seen in sclerosing epithelioid fibrosarcoma and giant collagen rosettes. It was first described in 1987 by Evans as bland fibroblastic cells with a swirling growth pattern, and fibrous matrix [11]. A variety of the same was then described by Lane in 1997, the hyalinizing spindle cell tumor with giant rosettes (HSTGR). These tumors have bland spindle cells with fibromyxoid areas resembling LGFMS, histologically. Giant rosettes in HSTGR consists of hyalinized acellular islands surrounded by oval and spindle cells. In this study as well, the typical oval and fusiform cells arranged loosely in a myxoid collagenous matrix with infrequent mitosis helped in the diagnosis of LGFMS. Although there are no treatment policies regarding the usage of radio- or chemotherapy for LGFMS, there are trials that have shown the use of radiotherapy prior to surgery and postoperatively which have had a benefit on tumor clearance in cases of soft tissue tumors [12]. Studies have also been done to review the effectiveness of chemotherapy along with or without surgical resection [13]. Due to the absence of treatment protocols and the dilemma in diagnosis, the decision for surgical excision was taken up in this case. Chemotherapy agents such as ifosfamide, doxorubicin, pazopanib (Tyrosine kinase inhibitor), gemcitabine and more accepted, trabectedin, have been used in the treatment of these tumors [13]. Although there has not been much benefit seen with most of these chemotherapy agents, trabectedin has been the most acceptable chemotherapy agent. Trabectedin has been shown to be effective in translocation-related soft tissue sarcomas. As LGFMS has been seen associated with FUS/GREB3L2 fusion gene, trabectedin has been seen to be effective for its treatment [13]. In the postoperative period of the present study, after histopathological diagnosis, adjuvant chemotherapy or radiotherapy was not given due to lack of evidence of its efficacy. On immunohistochemistry, LGFMS shows immunoreactivity for vimentin, focal immunoreactivity for smooth muscle actin, EMA, CD99, S100, bcl2, and CD68. Cytokeratins and CD34 are negative [14]. Follow up after excision of the tumor is essential in view of the possibility of local recurrences or metastasis. Local recurrence has been seen around 63.3% and 55.5% in the previous case series [3,6]. Metastasis has been seen with a varying incidence of 6% (out of 73 cases) by Folpe et al. [5] to and incidence of 45% (out of 33 cases) by H. Evans et al [3]. Metastasis has been seen to be most commonly to the lungs. In the present study there is a limitation as it is to soon to comment on the extent of resection and hence follow up is required every 6 months.
4. Conclusion
As seen in the present study, patients with LGFMS, present with abdominal lump. Similarities in its presentation with other intraabdominal tumors, such as intraabdominal testicular neoplasm in a case of undescended or absent testis, causes a clinical dilemma. Radiological imaging cannot help in finalising the diagnosis; however, it can help to map the vascularity of tumors, their infiltration or involvement of surrounding structures. This helps to plan the intraoperative procedure and management. Primary excision followed by histopathological examination confirms the diagnosis and governs the post operative treatment. Follow up every 6 months with clinical and radiological examination is advised to avoid any recurrences. Being a rare disease, further studies and understanding is required to plan a defined management and follow up protocol.
Conflicts of interest
None.
Author contributions
- Dr. Girish D. Bakhshi: Conceptualization, Methodology, Validation, Supervision
- Dr. Aishwarya Sunil Dutt: Investigation, Resources, Data curation, Writing, Visualisation
- Dr. Sushrut Baligar: Investigation, Resources, Data curation, Writing
- Dr. Rajalakshmi V: Investigation, Resources, Data curation, Writing
- Dr. Sampada Joshi: Investigation, Data curation
- Dr. Madhu Jha: Investigation, Data curation
- Dr. Chettubattina Ravi Teja: Investigation, Data curation
References
- Suciu MD, Marica NA, Oniu T, et al. Embryonal carcinoma of an intraabdominal testicular tumor on an undescended testicle: a case report. Med Pharm Reports 93 (2020): 213-218.
- Arnaoutoglou C, Lykissas MG, Gelalis ID, et al. Low grade fibromyxoid sarcoma: A case report and review of the literature. J Orthop Surg Res 5 (2010): 1-7.
- Evans HL. Low-grade fibromyxoid sarcoma: A clinicopathologic study of 33 cases with long-term follow-up. Am J Surg Pathol 35 (2011): 1450-1462.
- Din NU, Ahmad Z, Zreik R, et al. Abdominopelvic and retroperitoneal low-grade fibromyxoid sarcoma: A clinicopathologic study of 13 cases. Am J Clin Pathol 149 (2018): 128-134.
- Folpe AL, Lane KL, Paull G, et al. Low-grade fibromyxoid sarcoma and hyalinizing spindle cell tumor with giant rosettes: A clinicopathologic study of 73 cases supporting their identity and assessing the impact of high-grade areas. Am J Surg Pathol 24 (2000): 1353-1360.
- Goodlad JR, Mentzel T, Fletcher CDM. Low grade fibromyxoid sarcoma: clinicopathological analysis of eleven new cases in support of a distinct entity. Histopathology 26 (1995): 229-237.
- Woodward PJ. Case 70: Seminoma in an Undescended Testis. Radiology 231 (2004): 388-392.
- Moreno CC, Small WC, Camacho JC, et al. Testicular tumors: What radiologists need to know- differential diagnosis, staging, and management. Radiographics 35 (2015): 400-415.
- Hwang S, Kelliher E, Hameed M. Imaging features of low-grade fibromyxoid sarcoma (Evans tumor). Skeletal Radiol 41 (2012): 1263-72.
- Tsili AC, Sofikitis N, Stiliara E, Argyropoulou MI. MRI of testicular malignancies. Abdom Radiol 44 (2019): 1070-1082.
- Evans HL. Low-grade fibromyxoid sarcoma. A report of two metastasizing neoplasms having a deceptively benign appearance. Am J Clin Pathol 12 (1987): 657-659.
- Gerrand CH, Rankin K. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: A randomised trial. Class Pap Orthop 359 (2014): 485-486.
- Maretty-Nielsen K, Baerentzen S, Keller J, et al. Low-grade fibromyxoid sarcoma: Incidence, treatment strategy of metastases, and clinical significance of the FUS gene. Sarcoma (2013).
- Folpe AL. Fibrosarcoma: A review and update. Histopathology 64 (2014): 12-25.


 Impact Factor: * 4.2
Impact Factor: * 4.2 Acceptance Rate: 72.62%
Acceptance Rate: 72.62%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 