Use of Indocyanine Green Imaging in Gastroyeyunal Reconstruction For Recalcitrant Gastroparesis - Case Report
Article Information
Adolfo Leyva Alvizo*, Cristina Villar-Canton, Giovanna Yazmin Arteaga-Müller, Meri Yeghiazaryan
School of Medicine, Tecnologico de Monterrey, Monterrey, Mexico
*Corresponding Author: Adolfo Leyva Alvizo, School of Medicine, Tecnologico de Monterrey, Monterrey, Mexico
Received: 21 February 2023; Accepted: 20 March 2023; Published: 10 May 2023
Citation: Adolfo Leyva Alvizo, Cristina Villar- Canton, Giovanna Yazmin Arteaga-Müller, Meri Yeghiazaryan. Use of Indocyanine Green Imaging in Gastroyeyunal Reconstruction For Recalcitrant Gastroparesis - Case Report. Journal of Surgery and Research. 6 (2023): 174-177.
View / Download Pdf Share at FacebookAbstract
Diagnosis of diabetic gastroparesis relies on identifying delayed gastric emptying in ulcers or obstruction absence, with associated gastrointestinal symptoms. Regarding a clinical case presentation, the article provides an overview of diabetic gastroparesis and its implications. Discussion includes surgical management as the treatment of choice from the clinical perspective
Keywords
Gastroparesis, Indocyanine green, Gastrojejunal anastomosis, Antrectomy
Gastroparesis articles; Indocyanine green articles; Gastrojejunal anastomosis articles; Antrectomy articles
Gastroparesis articles Gastroparesis Research articles Gastroparesis review articles Gastroparesis PubMed articles Gastroparesis PubMed Central articles Gastroparesis 2023 articles Gastroparesis 2024 articles Gastroparesis Scopus articles Gastroparesis impact factor journals Gastroparesis Scopus journals Gastroparesis PubMed journals Gastroparesis medical journals Gastroparesis free journals Gastroparesis best journals Gastroparesis top journals Gastroparesis free medical journals Gastroparesis famous journals Gastroparesis Google Scholar indexed journals Indocyanine green articles Indocyanine green Research articles Indocyanine green review articles Indocyanine green PubMed articles Indocyanine green PubMed Central articles Indocyanine green 2023 articles Indocyanine green 2024 articles Indocyanine green Scopus articles Indocyanine green impact factor journals Indocyanine green Scopus journals Indocyanine green PubMed journals Indocyanine green medical journals Indocyanine green free journals Indocyanine green best journals Indocyanine green top journals Indocyanine green free medical journals Indocyanine green famous journals Indocyanine green Google Scholar indexed journals Gastrojejunal anastomosis articles Gastrojejunal anastomosis Research articles Gastrojejunal anastomosis review articles Gastrojejunal anastomosis PubMed articles Gastrojejunal anastomosis PubMed Central articles Gastrojejunal anastomosis 2023 articles Gastrojejunal anastomosis 2024 articles Gastrojejunal anastomosis Scopus articles Gastrojejunal anastomosis impact factor journals Gastrojejunal anastomosis Scopus journals Gastrojejunal anastomosis PubMed journals Gastrojejunal anastomosis medical journals Gastrojejunal anastomosis free journals Gastrojejunal anastomosis best journals Gastrojejunal anastomosis top journals Gastrojejunal anastomosis free medical journals Gastrojejunal anastomosis famous journals Gastrojejunal anastomosis Google Scholar indexed journals Antrectomy articles Antrectomy Research articles Antrectomy review articles Antrectomy PubMed articles Antrectomy PubMed Central articles Antrectomy 2023 articles Antrectomy 2024 articles Antrectomy Scopus articles Antrectomy impact factor journals Antrectomy Scopus journals Antrectomy PubMed journals Antrectomy medical journals Antrectomy free journals Antrectomy best journals Antrectomy top journals Antrectomy free medical journals Antrectomy famous journals Antrectomy Google Scholar indexed journals gastroparesis articles gastroparesis Research articles gastroparesis review articles gastroparesis PubMed articles gastroparesis PubMed Central articles gastroparesis 2023 articles gastroparesis 2024 articles gastroparesis Scopus articles gastroparesis impact factor journals gastroparesis Scopus journals gastroparesis PubMed journals gastroparesis medical journals gastroparesis free journals gastroparesis best journals gastroparesis top journals gastroparesis free medical journals gastroparesis famous journals gastroparesis Google Scholar indexed journals pacemakers articles pacemakers Research articles pacemakers review articles pacemakers PubMed articles pacemakers PubMed Central articles pacemakers 2023 articles pacemakers 2024 articles pacemakers Scopus articles pacemakers impact factor journals pacemakers Scopus journals pacemakers PubMed journals pacemakers medical journals pacemakers free journals pacemakers best journals pacemakers top journals pacemakers free medical journals pacemakers famous journals pacemakers Google Scholar indexed journals blood dilation articles blood dilation Research articles blood dilation review articles blood dilation PubMed articles blood dilation PubMed Central articles blood dilation 2023 articles blood dilation 2024 articles blood dilation Scopus articles blood dilation impact factor journals blood dilation Scopus journals blood dilation PubMed journals blood dilation medical journals blood dilation free journals blood dilation best journals blood dilation top journals blood dilation free medical journals blood dilation famous journals blood dilation Google Scholar indexed journals antrectomy articles antrectomy Research articles antrectomy review articles antrectomy PubMed articles antrectomy PubMed Central articles antrectomy 2023 articles antrectomy 2024 articles antrectomy Scopus articles antrectomy impact factor journals antrectomy Scopus journals antrectomy PubMed journals antrectomy medical journals antrectomy free journals antrectomy best journals antrectomy top journals antrectomy free medical journals antrectomy famous journals antrectomy Google Scholar indexed journals Clostridium difficile articles Clostridium difficile Research articles Clostridium difficile review articles Clostridium difficile PubMed articles Clostridium difficile PubMed Central articles Clostridium difficile 2023 articles Clostridium difficile 2024 articles Clostridium difficile Scopus articles Clostridium difficile impact factor journals Clostridium difficile Scopus journals Clostridium difficile PubMed journals Clostridium difficile medical journals Clostridium difficile free journals Clostridium difficile best journals Clostridium difficile top journals Clostridium difficile free medical journals Clostridium difficile famous journals Clostridium difficile Google Scholar indexed journals
Article Details
Overview/Introduction
Gastroparesis is a common complication in poorly controlled diabetic patients, characterized by delayed gastric emptying without apparent mechanical obstruction. Clinical presentation includes upper abdominal pain, nausea, vomiting, postprandial fullness, and early satiety due to the increased sensitivity caused by hyperglycemia in the gastrointestinal tract. Diabetic Gastroparesis (DG) diagnosis, according to the American College of Gastroenterology guidelines, require gastrointestinal symptoms and gastroparesis criteria. [1,9,10,12]. The stomach plays a fundamental role in digestion by producing hydrochloric acid and pepsinogen and performing digestion first steps. As part of the stomach's normal function, food is mixed, stored, and delivered through chemical and mechanical processes. The stomach expands to accommodate food, triggering digestion by delivering or storing food according to need, followed by trituration and emptying of chyme towards the duodenum. The ability to perform any of the previous tasks requires adequate gastric motility. In patients with impaired muscular contractions or relaxation of the smooth muscular layers of the stomach, gastrointestinal symptoms and gastroparesis may be present [1,4].
The physiopathology of hyperglycemia in neuropathy supports the main theories about delayed gastric emptying secondary to diabetes. During diabetic gastroparesis, the major motility control centers (the autonomic and enteric nervous systems) malfunction, causing altered emptying patterns. A coordinated fundal tone and antral contraction, with inhibitions of the duodenum and pyloric contractions, are necessary for gastric emptying. The exchange of nerve signals between the enteric and autonomic nervous systems allows synchronization of the stomach's smooth muscle layers and specialized pacemakers (Interstitial Cells of Cajal). Also, the vagus nerve regulates the accommodation of the fundus, along with antral contraction and pyloric relaxation. DG high glucose levels in the serum cause a proinflammatory state, resulting in neuronal injury (neuropathy) and improper vagus nerve neurotransmission with defective pacemakers and smooth muscle cells. When nerves are damaged, fewer antral contractions are visible, and pyloric spasms accompany uncoordinated antro-duodenal contractions, causing delayed gastric emptying [1,8,11,12]. The treatment options vary from patient to patient. Dietary changes for glycemic control and prokinetic drugs are the first line of treatment. However, surgical management is necessary in some cases, especially in patients with refractory gastroparesis [8]. Antrectomy with reconstruction is one of the surgical options for gastroparesis treatment; this procedure removes the lower third of the stomach, the antrum, followed by an anastomosis that controls the flow of chyme from the stomach to the duodenum or jejunum [3,5,7]. Antrectomy complications include insufficient perfusion and leakage of the gastric remnant to be anasromosed. The use of Indocyanine green helps reduce the risk of this complication. Indocyanine green is a tricarbocyanine molecule with water-soluble properties and high molecular weight, allowing it to bind to plasma proteins quickly and leak as minimally as possible. The method involves a non-invasive image study in which Indocyanine green becomes fluorescent and allows a time-varying recording of blood dilation. Results show a clearly defined vasculature, which helps spot low blood perfusion or leakage into the interstitial space, in this case, after an antrectomy [2,6,13].
Case report
A 33-year-old female was admitted to the hospital after suffering from stomach pain and vomiting over a period of 3 days. Symptoms are similar to those seen during previous admissions. Our patient had a prior medical history of type 1 diabetes mellitus treated with insulin Lantus, for more than 15 years, with bilateral retinal detachment, and finally requiring renal transplantation 5 years ago. 4 years before admission she became infected with Clostridium difficile and treated with fecal transplantation. 3 years prior to admission, our team performed a laparoscopic cholecystectomy on her with atypical upper GI symptoms and biliary sludge, with poor resolution of her symptoms, which prompted further studies until an official diagnosis of diabetic gastroparesis was achieved. In her admission through the Emergency Room, she weighed 92 kilograms with 1.56 meters height (BMI 37.8). The physical examination showed abdominal distention with normal peristalsis and tympanic percussions. According to a 99m Tc-Sulfur colloid nuclear MRI scan, gastric emptying was calculated at 831.92 minutes and 3% excretion in 60 minutes, leading to Severely Prolonged Gastric Emptying (figure 1). Endoscopy revealed biliary content in the stomach, and biopsies indicate reactive/chemical gastropathy (figure 2).
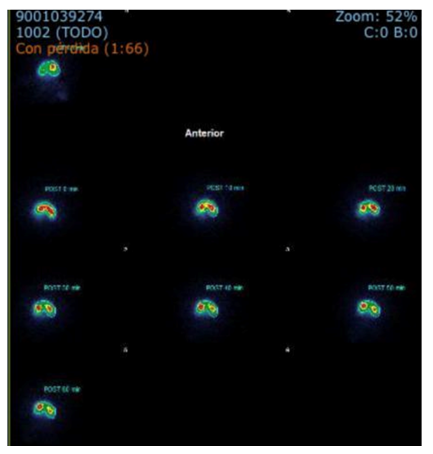
Figure 1: Gastric Emptying Nuclear Scan
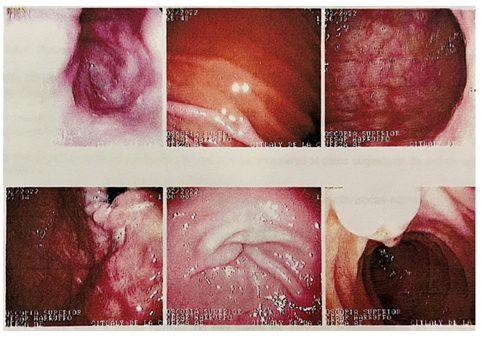
Figure 2: Endoscopy showing erosive gastritis as well as biliary reflux.
Surgical procedure
We performed a laparoscopic antrectomy with Gastrojejunal Billroth 2 reconstruction. Once the antrum was removed, and the loop of bowel was carefully measured using a 10 cm mark on our intestinal clamps, the patient received 2.5 mg of IV Indocyanine Green, to verify the optimal irrigation of both the gastric border of resection and the jejunal segment that was ascended in the loop configuration (figure 3). The gastric resection level was above the incisura angularis, resecting the antrum and segment of the body, leaving a horizontal gastric stump line (figure 4). We decided to perform the anastomosis bypassing 1.80 mts of jejunum, to help her achieve weight loss, after counting the distal small bowel in 470 cms distally to the anastomotic site. After optimal perfusion was verified, the G-J was performed using a stapled posterior anastomosis and a blue 40 mm load, closing the stapler defect with running 2-0 V-Loc suture. Total surgical time was 105 minutes, with minimal bleeding and no other findings reported. The procedure was well tolerated, starting clear liquids on PO day 1, and progressing slowly through 5 more days until discharged with a soft diet, with strict multidisciplinary management involving her Nephrologist, Gastroenterologist, and Registered Dietitian. She was seen a month later with good food intake and without abdominal pain and vomit. She underwent follow up with our RD and Psychologist according to our center standards. After 6 months she was asymptomatic regarding her gastric emptying, and lost 20 kilograms, making her metabolic control easier.
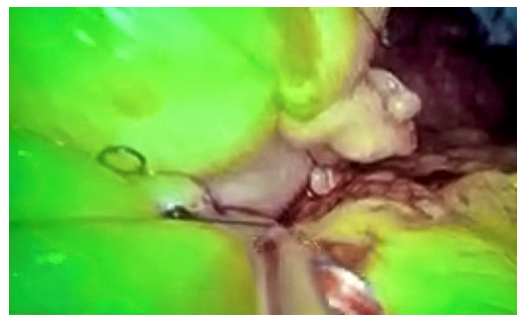
Figure 3: ICG injection with gastric stump in the upper segment, and jejunal loop on the bottom, a 2-0 silk suture can be seen between both segments.
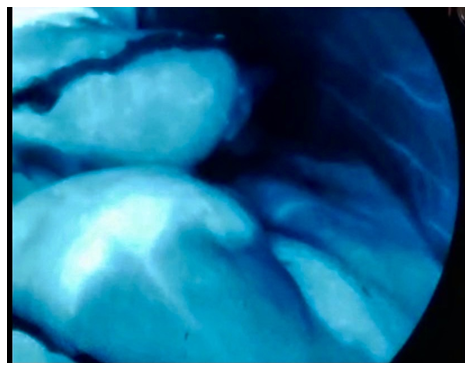
Figure 4: Final ICG with the gastric stump (staple line of gastric resection visible as a black horizontal line) and jejunal stump perfectly perfused after completing the anastomosis.
Discussion
Gastroparesis is a challenging disease, both diagnosis and treatment are difficult to determine in the majority of the cases. Here we have the case of a young diabetic female who was initially operated on for a laparoscopic cholecystectomy years before being diagnosed officially with gastroparesis. The atypical symptoms persisted and she was evaluated deeply until we concluded her diagnosis. Considering the patient’s weight, we considered performing an antrectomy with small bowel reconstruction bypassing enough distance to help her achieve weight loss as well. Gastric bypass with or without gastric resection has been used and has resulted in both symptom reduction and decreased use of prokinetics [14]. Both nausea and vomiting have been improved in series of patients using gastric bypass in these patients [15,16]. The use of Indocyanine green angiography in bariatric operations has been reported to asses insufficient blood flow and hence increased risk of leakage [17]. In this patient we assessed optimal perfusion both from the gastric stump to be anastomosed and from the intestinal loop that was ascended. We had no evidence of leaks and the patient had a favorable resolution of her symptoms.
sectors.
References
- Aswath GS, Foris LA, Ashwath AK, et al.(2022). Diabetic Gastroparesis. StatPearls.
- Boni L, David G, Mangano A, et al. Clinical applications of indocyanine green (ICG) enhanced fluorescence in laparoscopic surgery. Surg Endosc 29 (2015): 2046-2055.
- Dozois RR., Kelly KA, Code CF. Effect of Distal Antrectomy on Gastric Emptying of Liquids and Solids. In Gastroenterology 61 (1971): 675-681.
- Fehnel S, Fiedorek FT, Nelson L, et al. Development and psychometric evaluation of the Diabetic Gastroparesis Symptom Severity Diary. In Clinical and Experimental Gastroenterology 12 (1971): 93-103.
- Mishra RK. Antrectomy. World Laparoscopy Hospital (2022).
- Ozkaya A, Alagoz C, Garip R. et al. The role of indocyanine green angiography imaging in further differential diagnosis of patients with nAMD who are morphologically poor responders to ranibizumab in a real-life setting. Eye 30 (2016) 958-965.
- Palumbo LT, Sharpe WS. Distal antrectomy with vagectomy for duodenal ulcer: results in 611 cases. Annals of surgery 182 (1975): 610-616.
- Parkman HP, Hasler WL, Fisher RS, American Gastroenterological Association. American Gastroenterological Association technical review on the diagnosis and treatment of gastroparesis. Gastroenterology 127 (2004):1592.
- Parkman HP, Wilson LA, Hasler WL, et al. Abdominal Pain in Patients with Gastroparesis: Associations with Gastroparesis Symptoms, Etiology of Gastroparesis, Gastric Emptying, Somatization, and Quality of Life. Digestive Diseases and Sciences (2019).
- Petri M, Singh I, Baker C, et al. Diabetic gastroparesis: An overview of pathogenesis, clinical presentation and novel therapies, with a focus on ghrelin receptor agonists. Journal of Diabetes and Its Complications (2020): 107733.
- Sensoy I. A review on the food digestion in the digestive tract and the used in vitro models. Current research in food science 4 (2021): 308-319.
- Usai-Satta P, Bellini M, Morelli O, et al. Gastroparesis: New insights into an old disease. World journal of gastroenterology 26 (2020): 2333-2348.
- Yannuzzi LA. Indocyanine Green Angiography: A perspective on use in the clinical setting. American Journal of Ophthalmology 151 (2011): 745-751.
- Sun Z. Surgical treatment of medically refractory gastroparesis in the morbidly obese. Surg Endosc 29 (2015): 2683-2689.
- Watkins PJ, Buxton-Thomas MS, Howard ER. Long-term outcome after gastrectomy for intractable diabetic gastroparesis. Diabet Med 20 (2003): 58-63.
- Wakamatsu K. Laparoscopic treatment of gastroparesis: a single center experience. Surg Obes Relat Dis 14 (2018): 200-205.
- Helmut B. A550 Indocyanine green mesenteric angiography as an intraoperative assessment of bowel perfusion in revisional and primary bariatric operations. assessment of 50 cases, operative findings and surgical interventions taken surg obes relat dis 15 (2019): S228.


 Impact Factor: * 4.2
Impact Factor: * 4.2 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 